Neonatal jaundice N Hyperbilirubinemia Bilirubin metabolism RBCs destructions

Neonatal jaundice (N. Hyperbilirubinemia)
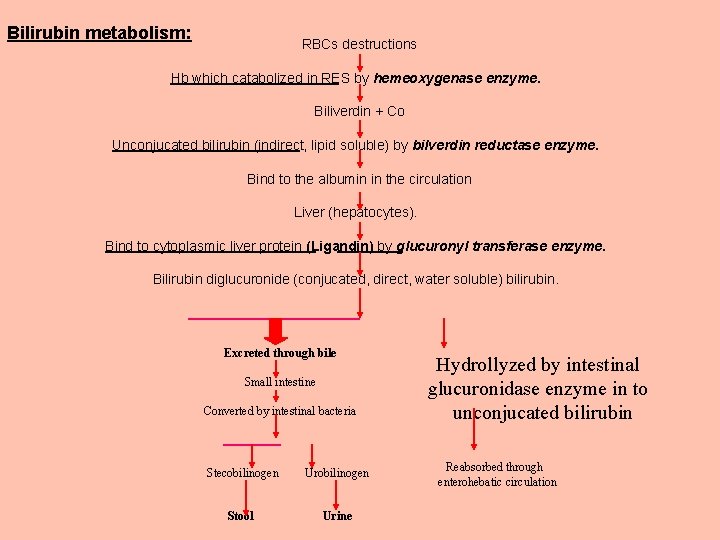
Bilirubin metabolism: RBCs destructions Hb which catabolized in RES by hemeoxygenase enzyme. Biliverdin + Co Unconjucated bilirubin (indirect, lipid soluble) by bilverdin reductase enzyme. Bind to the albumin in the circulation Liver (hepatocytes). Bind to cytoplasmic liver protein (Ligandin) by glucuronyl transferase enzyme. Bilirubin diglucuronide (conjucated, direct, water soluble) bilirubin. Excreted through bile Small intestine Converted by intestinal bacteria Stecobilinogen Urobilinogen Stool Urine Hydrollyzed by intestinal glucuronidase enzyme in to unconjucated bilirubin Reabsorbed through enterohebatic circulation

**One gram of Hb produces 35 mg of bilirubin. Newborn infant have a 2 to 3 folds greater rate of bilirubin production than in adults 24 hr in newborn while 3 mg/kg/24 hr in adult), this is due to: 1. Increased RBC mass (higher Hb concentration). ed RBC life span (70 -90 -days, compared with the 120 days in the adults.

One gram of albumin binds 8. 5 mg of bilirubin in wborns, if the binding sites become rated, the free unconjucated bilirubin will enter the CNS causing neurological damage

Etiological classification of jaundice: A. Unconjucated jaundice: s incompatibility: ABO patibility, Rh incompatibility, or minor roup incompatibility (Kell). enzymes defects: G 6 PD deficiency, pyruvate kinase deficiency. 3. RBC membrane defects: spherocytosis, ovalocytosis. 4. Physiological jaundice. 5. Breast milk jaundice.

6. Internal hemorrhage. 7. Polycythemia. 8. Infants of diabetic mothers. ajjar syndrome (deficiency of glucuronyl transferase enzyme). 10 Gilbert disease.

B. Conjugated jaundice: 1. Cholestasis. 2. CMV and other perinatal congenital infections (TORCH). 3. Neonatal hepatitis. 4. Neonatal sepsis. 5. Inborn error of metabolism (e. g. galactosemia). 6. Cystic fibrosis. 7. Biliary atresia. 8. Alpha-1 -antitrypsin deficiency.

Physiological jaundice: It’s the most common cause of neonatal jaundice, its occurs in the most newborn infants, and characterized by: 1. Clinical jaundice appears at 3 rd day of life. 2. Peak unconjucated bilirubin level no more than 12 mg/dl. ce decrease at 5 th-7 th day of life unconjucated bilirubin<2 mg/dl).

Causes: ncrease bilirubin production due to increased RBCs mass and shortened RBC life span. 2. Hepatic immaturity of ligandin and glucuronyl transferase. Diagnosis: 1. Clinical pattern of jaundice. 2. Exclusion of pathological causes of jaundice.

Pathological (nonphysiological) jaundice: It's considered if: 1. Jaundice appears during first 24 hr of life. 2. Serum bilirubin rising at rate greater than 5 mg/dl/24 hr. um bilirubin greater than 12 mg/dl in full term infants or 10 -14 mg/dl in preterm infants. 4. Jaundice persists after 10 -14 days of life. 5. Direct bilirubin is greater than 2 mg/dl at any time. 6. Presence of anemia or hepatosplenomegaly.

Breast milk jaundice: Its unconjucated hyperbilirubinemia occur in 2% of breast-feed term infants after 1 st week of life, reaching beak bilirubin concentration of 1030 mg/dl during the 2 nd or 3 rd week of life.

If the breast milk discontinued for 1 -2 days and replaced by battle feeding, it will result in rapid decline in bilirubin level, after which the breast feeding can be resumed without return of hyperbilirubinemia to its previous high levels. Kernicterus (bilirubin encephalopathy) has been reported in some cases. The cause of breast milk jaundice is unclear, but the breast milk may contain inhibitors to bilirubin conjugation or the breast milk contain glucuronidase which increase the enterohepatic recirculation of bilirubin.

Breast feeding associated jaundice: Its occur in 13% of breast-feed infants in the 1 st week of life, its unconjucated type of jaundice (unconjucated bilirubin >12 mg/dl), and its due to: 1. Decreased milk intake with dehydration. 2. Reduced caloric intake. glucose water to the baby which decrease intake of high caloric breast milk. Treatment: 1. Frequent breast feeding (>10 times/24 hr). 2. Rooming-in with night feeding. 3. Prevent 5% glucose water supplementation.

Prolong jaundice: Its jaundice that persists during 1 st month of life. Causes: Inspissated bile syndrome (following hemolytic disease of newborn). 2. Cholestasis. 3. CMV and STORCH infections. 4. Familial nonhemolytic jaundice. 5. Hepatitis. 6. Congenital biliary atrasia. 7. Galactosemia. 8. Cystic fibrosis. 9. Physiological jaundice (rarely).

Approach to diagnosis of prolong jaundice: A. Detailed history and physical examination. B. Investigations: 1. CBC and blood film morphology. 2. Bacterial and viral cultures. 3. Hepatic ultrasonography. 4. Metabolic screening tests. 5. Sweat chloride test. 6. Liver biopsy. Treatment of prolong jaundice: According to the underlying cause.

Bilirubin encephalopathy (kernicterus): Its neurological syndrome resulting from the deposition of unconjucated bilirubin in the brain cells, the unconjucated bilirubin cross the blood brain barrier (BBB) because its lipid solubility especially during the 1 st week of life when the BBB is not fully mature. The risk is directly related to the serum bilirubin concentration, its occurs in full term neonate when the serum bilirubin is >25 mg/dl, but its may occurs at bilirubin levels below 20 mg/dl in the presence of following risk factors:

1. Neonatal sepsis and meningitis. 2. Hemolytic disease of newborn. 3. Asphyxia or hypoxia. 4. Hypothermia. 5. Hypoglycemia. ematurity: very immature infants weighing than 1000 g may develop Kernicterus at bilirubin levels less than 10 mg/dl.
Clinical features: A. Early: Noted after 4 th day of life and includes lethargy, hypotonia, irritability, poor Moro reflex, poor feeding vomiting, and high-pitched cry. B. Late: Noted during the 1 st year of life, including bulging fontanels, opisthotonic posturing, pulmonary hemorrhage, fever, hypertonia, and seizures.

C. severely affected infants died in neonatal period. D. Complete neurological syndrome: Its appear at age of 3 years and consist of nerve deafness, choreoathetoid cerebral palsy, mental retardation, and teeth discoloration.

Prevention of kernicterus: 1. Avoiding excessively high indirect bilirubin levels. ns or drugs g. sulphonamides) that may display bilirubin from albumin. mmediate exchange transfusion which might reverse the very early signs of kernicterus.
- Slides: 20