Neonatal Jaundice Dr Abdul Rahman Al Nemri MD

Neonatal Jaundice Dr. Abdul. Rahman Al Nemri, MD Chairman of Pediatric Department Associate Professor Senior Consultant Neonatologist

Introduction ØYellow-orange pigment Icterus – ikteros - bilirubin in the skin and sclerae. It affects 60% of neonates. ØJaundice = galbus (it appears when TSB is more than 34 umol/l in adults Vs >86 in neonates) ØIt is one of the most common clinical phenomena encountered in newborns.

Bilirubin Production Ø Bilirubin is obtained by degrading heme from hemoglobin-containing RBCs (80% of bilirubin is from Hb). Ø RBC life in adults is 120 days. In children, it is shorter (90 days) giving them higher turnover rates specially in premature infants. Ø It functions as an antioxidant against free radicals, and an emulsion to lipids. Ø 20% from ineffective erythropoiesis and turnover of non-hemoglobin hemoproteins (eg, myoglobin, catalase, nitric oxide synthase, peroxidases, and cytochromes).
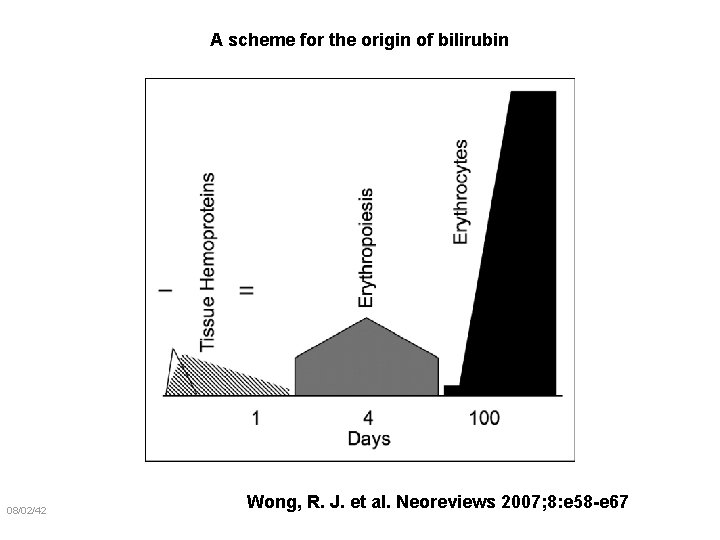
A scheme for the origin of bilirubin 08/02/42 Wong, R. J. et al. Neoreviews 2007; 8: e 58 -e 67
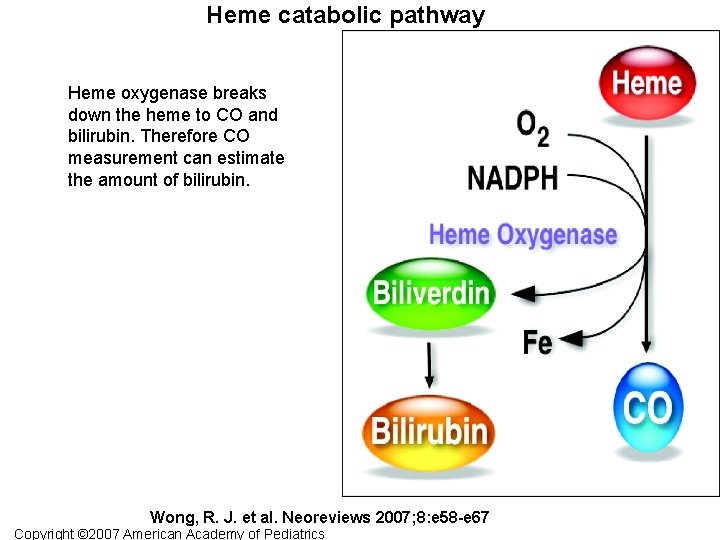
Heme catabolic pathway Heme oxygenase breaks down the heme to CO and bilirubin. Therefore CO measurement can estimate the amount of bilirubin. Wong, R. J. et al. Neoreviews 2007; 8: e 58 -e 67 Copyright © 2007 American Academy of Pediatrics

Bilirubin Transport • Free Bilirubin is lipid soluble (hydrophobic), crosses the BBB and is toxic to the brain, therefore it binds to albumin. • It binds reversibly to albumin (bilirubin: albumin) • (about 0. 8 - 7 mg of bilirubin per gram of albumin- ) • Low Albumin level and affinity binding sites • Aqueous diffusion • The movement of bilirubin from the circulation into tissue cross BBB. • Albumin-bilirubin conjugate is transports to hepatocytes.

Conjugation • Conjugation of bilirubin (in the hepatocytes) with glucuronic acid (water-soluble, nonneurotoxic bilirubin) by the enzyme UGT. • uridine diphospho- glucuronosyltransferase (UGT), lack of this enzyme in neonates will increase its toxicity. • Decrease conjugation by: 1. Slower rate of hepatic uptake of free bilirubin from the blood 2. Decreased concentrations of (UGT) +

Bilirubin Excretion • Conjugated bilirubin enter the bile ducts and are excreted with the bile into the intestinal tract. • Mono Or Diglucuronide > unconjugated Bili • In the colon, bacterial flora in older neonates hydrogenate bilirubin to urobilinogen, urobilins, and stercobilins. • Part of the urobilinogen is absorbed into the portal circulation and excreted by the kidney.
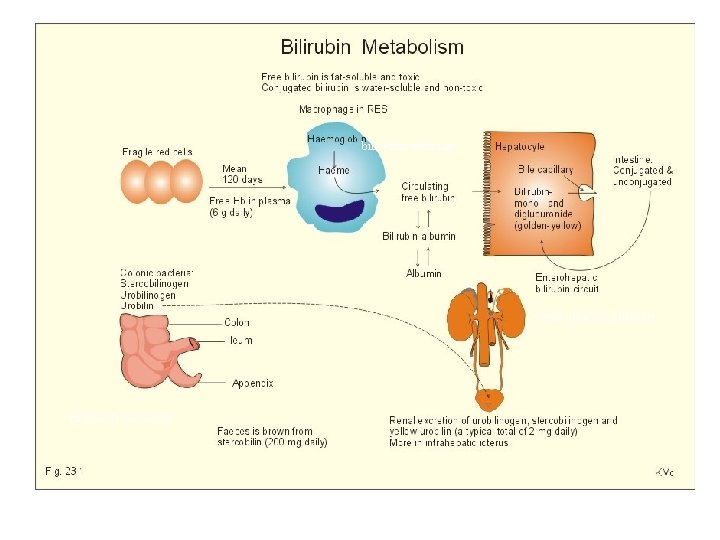
biliverdin reductase beta-glucuronidase Bilirubin oxidase
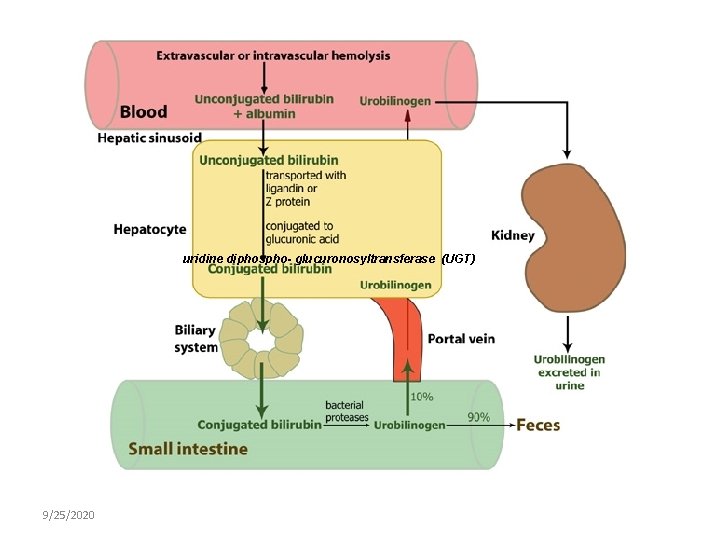
uridine diphospho- glucuronosyltransferase (UGT) 9/25/2020

RISK FACTORS FOR SIGNIFICANT JAUNDICE • • Gestational Age more in premature Race (Genetic @ environmental Maternal illness DM & Blood group (ABO or Rhs) Family history of jaundice requiring phototherapy • Hemolysis (G 6 PD, Spherocytosis) • Severe bruising • Breastfeeding

History • • • Origin of the infant Blood group Autoimmune diseases. Hemoglobinopathies. Onset and associated symptoms (lethargy, poor suckling and crying). • Color of the stool and urine. • Color of the skin: if pale then hemolytic anemia. Jaundiced. • Check for hepato-spleenomegaly. 9/25/2020

Etiological Classification 1. Increased bilirubin load • I. Hemolytic causes Coombs' test positive: Rh factor incompatibility, ABO II. incompatibility, minor antigens, autoimmune as lupus and RA because antibodies are already there. Which one is common ? Coombs' test negative: red blood cell membrane defects (spherocytosis, elliptocytosis), red blood cell enzyme defects (G 6 PD deficiency, pyruvate kinase deficiency) Ø Why not thalasemia or SCD? SCA and thalasemia beta are never a DDx because they are a beta chain abnormality while the neonate Hb. F which consists of alfa and gamma chains, while thalasemia alfa (there will be in utero hemolysis) and G 6 PD are imp DDx.
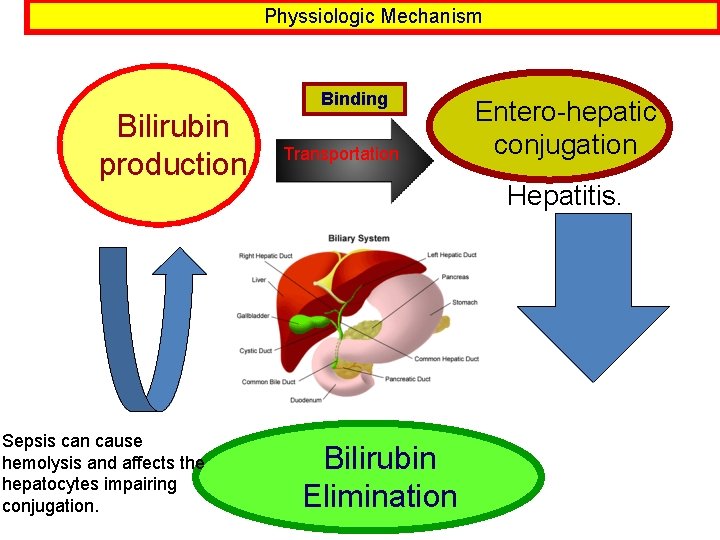
Physsiologic Mechanism Bilirubin production Sepsis can cause hemolysis and affects the hepatocytes impairing conjugation. Binding Transportation Entero-hepatic conjugation Hepatitis. Bilirubin Elimination

Nonhemolytic causes • Increased unconjugated bilirubin level, normal percentage of reticulocytes ØPhysiologic jaundice ØExtravascular sources ØPolycythemia ØExaggerated enterohepatic circulation

2 - Decreased bilirubin conjugation Ø Ø Ø Ø Ø Physiologic jaundice Crigler-Najjar syndrome: deficiency of UGT enzyme. Gilbert syndrome. Hypothyroidism. Cystic fibrosis. Metabolic in-born illness. Alfa one antitrypsin deficiency. Breast milk jaundice Hep B or C TORCH or any bacterial infection to the liver. affects the liver and impairs the conjugation. Ø Hepatomegaly and hepatits.

3 - Impaired bilirubin excretion • Conjugated bilirubin level of >2 mg per d. L (34 μmol per L) or >20% of total serum bilirubin level Ø Biliary obstruction e. g. biliary atresia can be extra-hepatic (they come with distinctive features) or intra-hepatic. Or obstruction outside the biliary system e. g. hematoma, hemangioma, choledecal cyst, pancreatic or duodenal mass. Ø Infection Ø Metabolic disorder Ø Chromosomal abnormality e. g. dobbin Johnson and Rotters syndrome.

Physiologic jaundice • increased breakdown of fetal erythrocytes. shortened lifespan of fetal erythrocytes and the higher erythrocyte mass in neonates • The commonest cause of jaundice in term babies. • Hepatic excretory capacity is slow because hepatocytes are still not mature. • low activity of glucuronyl transferase • Typically, presentation is on the second or third day of life. • Jaundice that is visible during the first 24 hours of life is likely to be non-physiologic

What is the commonest cause of non hemolytic hyperbilirubineamia? Physiological jaundice. What are the other D/D?

What are the criteria of physiological Jaundice ? 1. Onset more than 24 hours but less than 2 weeks. 2. Rate of TSB increment not more than 5 mg. 3. Level of TSB less than 25 mmol/l. 4. Type of Bili: un-conjugated, if conjugated its pathological. 5. Duration 08/02/42

Infants with multiple risk factors may develop an exaggerated form of physiologic jaundice in which the total serum bilirubin level may rise as high as 17 mg per d. L (291 μ mol per L)

JAUNDICE AND BREAST FEEDING • Early-Onset Breast feeding associated Jaundice or B Feeding failure J. • Decreased volume and frequency of feedings may result in mild dehydration and the delayed passage of meconium • Breast milk jaundice occurs later in the newborn period usually peaking in the sixth to 14 th days of life. • B Milk Metabolites ( progestrin, pregnane 3α, 20β)

PATHOLOGIC JAUNDICE All etiologies of jaundice beyond 1) Physiologic 2) Breastfeeding (the baby does not feed and becomes dehydrated) or 3) breast milk jaundice (milk content causing jaundice) are considered pathologic.

Un-Conugated Hyperbilirubinemia 1. Excessive Bilirubin Production 2. Impaired Conjugation 3. Excretion

Hemolytic Disease Blood group incompatibility Red cell enzyme deficiency Red blood cell membrane defect Extravascular Blood Polycythemia Sepsis

ABO Incompatibility • ABO Incompatibility is the most common cause of hemolytic jaundice • Only 10 -20% of infants with ABO mismatch develop significant jaundice • Coombs positive ABO is more likely to cause hemolysis • Conversely, Coombs negative ABO mismatch does occasionally cause significant hemolysis, but this is rather rare.
Diagnosis • HISTORY • PHYSICAL EXAMINATION
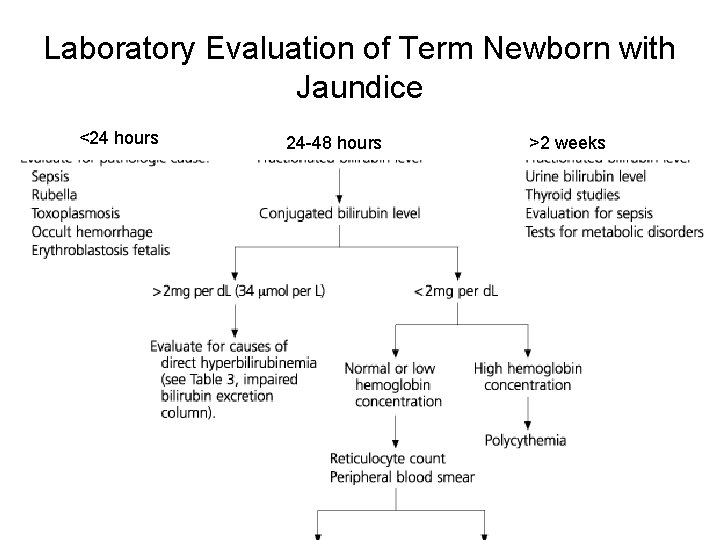
Laboratory Evaluation of Term Newborn with Jaundice <24 hours 24 -48 hours >2 weeks

Management • 1. 2. 3. 4. An increased incidence of kernicterus (mostly in the basal ganglia, cranial nerves mainly auditory) was found to be associated with total serum bilirubin levels above 20 mg per d. L in the presence of hemolysis Hydration And Supportive measures Management guidelines now focus primarily on phototherapy (anti-oxidant) as initial treatment. Aggressive guidelines recommending the use of exchange transfusion in all infants with significant hyperbilirubinemia. Albumin can be given when there is an increase in the level of free bilirubin (>25 mg/dl).

Conjugated hyperbilirubinemia is never physiologic, and it may indicate the presence of a potentially serious underlying disorder HOWEVER ELEVATED CONJUGATED BILIRUBIN LEVELS ARE NOT DIRECTLY TOXIC TO BRAIN CELLS IN THE NEONATE.
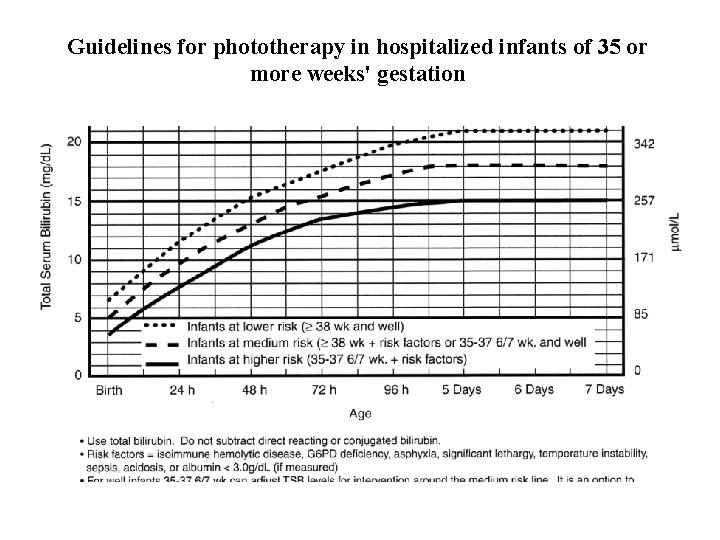
Guidelines for phototherapy in hospitalized infants of 35 or more weeks' gestation
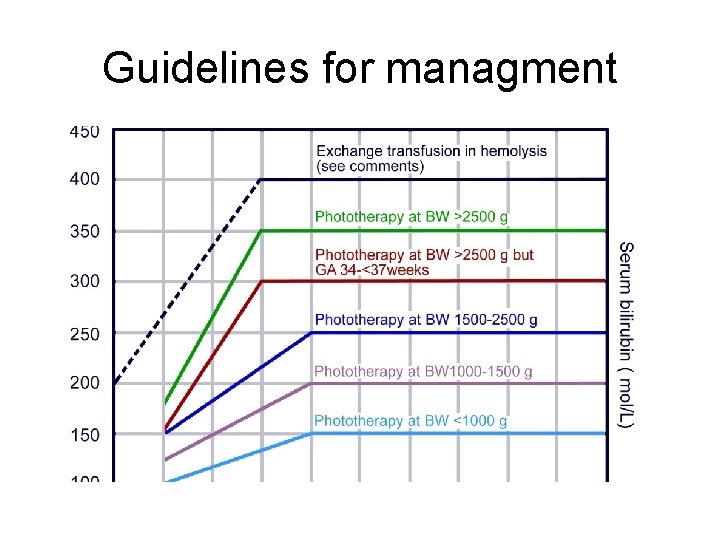
Guidelines for managment

Management • Depending on the chart: Either assure or conservatively hydrate if still not responding or in the phototherapy zone do phototherapy, and finally exchange transfusion. 9/25/2020
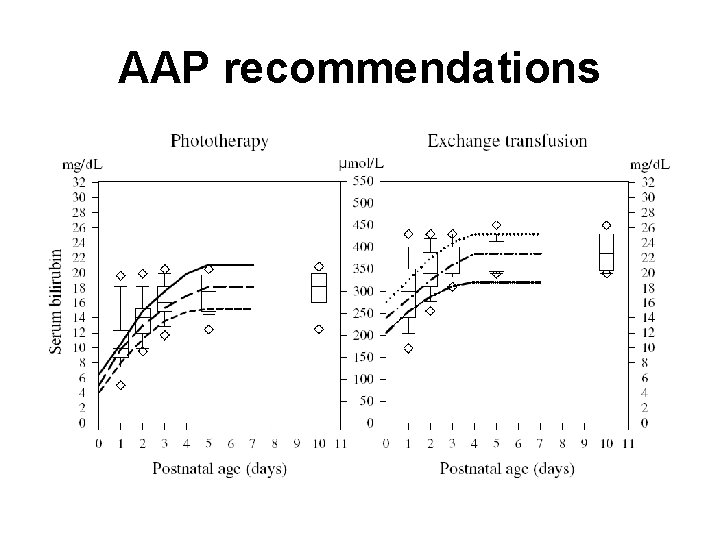
AAP recommendations

PHOTOTHERAPY Any baby with jaundice must be investigated. We do CBC to check the levels of bilirubin, whether its in the phototherapy zone or not. (if less than 8 and its in an unconjugated type then just reassure. ) light at blue or blue-green wavelengths converts the bilirubin molecule into a form that is either easier to excrete or is less toxic to the neonate The effective spectrum for this process has been identified in vitro to peak at around 450 nm (blue light)
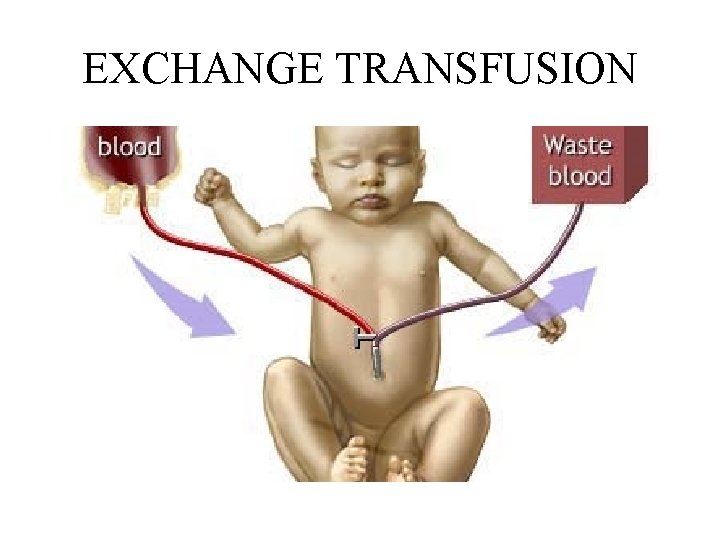
EXCHANGE TRANSFUSION

OTHER • Mesoporphyrin Still under investigation • Albumin trnsafusion • Antibiotics • Fluid and Electrolytes • D 5% water NO it’s a wrong practice just give the baby milk. • Phenobarbiton ?
basal ganglia hippocampus kernicterus geniculate bodies cranial nerve nuclei Especially the vestibulocochlear nerve.

Pathophysiology • Bilirubin staining in the regions of the basal ganglia, hippocampus, substantia nigra, and brainstem nuclei • Staining can occur in the absence of severe hyperbilirubinemia • Characteristic patterns of neuronal necrosis
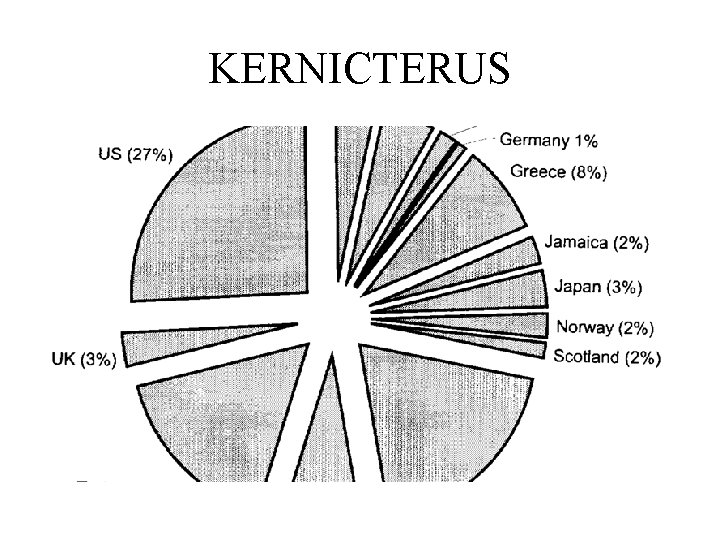
KERNICTERUS

Causes • Severe hemolytic processes were identified in 19 out of 80 babies (24%) • glucose-6 -phosphate dehydrogenase (G 6 PD) deficiency was diagnosed in 18 out of 80. • galactosemia occurred in 2 out of 80 • Crigler-Najjar syndrome type I occurred in 1 • NO etiology for the severe hyperbilirubinemia was discovered in 73% of cases • In SA its more commonly due to G 6 PD and crigler Najjar.

Incidence • Do we have any registry in Saudi Arabia? ? • All reported cases from Saudi literatures were secondary to Crigler Najjarr syndrome Am J Med. Genet. 1998 Aug 27; 79(1): 12 -5

Term Infant with Jaundice and üHigh pitched cry üArching of the baby's body into a bow üWeakness, limpness, floppiness ü Difficulty nursing and/or sucking üWHAT IS THE TREATMENT ?

KERNICTERUS DIAGNOSIS • Early symptoms-acute bilirubin encephalopathy-poor feeding, abnormal cry, hypotonia, • Intermediate phase- stupor, irritability, hypertonia • Late phase shrill cry, no feeding, opisthotonus, apnea, seizures, coma, death
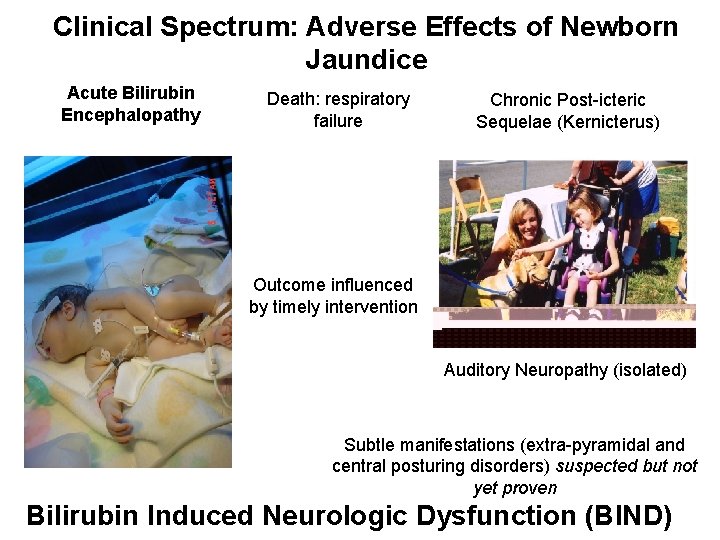
Clinical Spectrum: Adverse Effects of Newborn Jaundice Acute Bilirubin Encephalopathy Death: respiratory failure Chronic Post-icteric Sequelae (Kernicterus) Outcome influenced by timely intervention Auditory Neuropathy (isolated) Subtle manifestations (extra-pyramidal and central posturing disorders) suspected but not yet proven Bilirubin Induced Neurologic Dysfunction (BIND)

KERNICTERUS • Late sequelae can include Ø gaze abnormalities Ø feeding difficulties Ø dystonia Ø incoordination Ø choreoathetosis Ø sensorineural hearing loss Ø painful muscle spasms

KERNICTERUS • Incidence of bilirubin levels >30 1/10, 000 • Over 120 cases kernicterus documented since 1990 • majority term, breastfed • Majority of those had levels in high 30 s to 40 s. • Lowest level recorded in case series of 111 from 1991 -2002 was 20. 7, but the mean was 38. • Many cases had no planned follow up and had been discharged early (<48 hours).

Risk Factors 1. 2. 3. 4. 5. 6. 7. 8. ASPHYXIA ACIDOSIS SEPSIS HYPOALBUMINEMIA YOUNG GESTATIONAL AGE LOW BIRTH WT HYPERTHERMIA RESPIRATORY DISTRESS
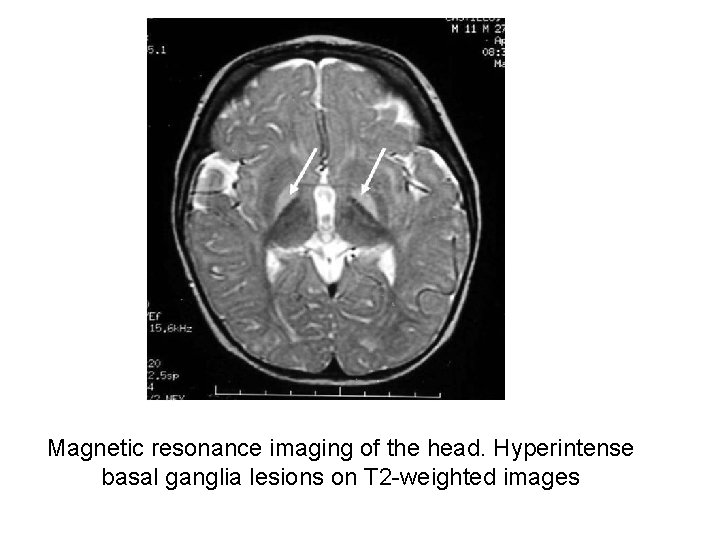
Magnetic resonance imaging of the head. Hyperintense basal ganglia lesions on T 2 -weighted images

Management of Hyperbilirubinemia AAP Alerts: l Clinical Overview: l Usually benign; but potential of bilirubin toxicity l Focus: l Reduce incidence of severe hyperbilirubinemia

Prevention l. Recommend: Ø Ø Promote and support successful breastfeeding. Universal systematic pre-discharge assessment. Provide targeted follow-up based on the risk. Track outcome for timely treatment to prevent excessive hyperbilirubinemia and possibly, kernicterus.

AAP 2004: Recommendations I. III. IV. V. VII. Primary Prevention: lactation support Risk assessment for severe hyperbilirubinemia: Interpretation of TSB values Cause of jaundice/hyperbilirubinemia. Pre-discharge risk assessment Hospital policies and procedures Treatment

Summary • Bilirubin physiology • Prevent neurotoxicity • Identify and treat illness associated with excess production, impaired conjugation or inadequate elimination • Combination of therapy

A 3 -day old full term infant with hemolytic disease of the newborn due to Rh incompatibility has a serum indirect bilirubin concentration of 33 mg/d. L. You perform an exchange transfusion with no further elevations of bilirubin above 19 mg/d. L. Among the following, the MOST appropriate study to use to follow up on this infant is: A. B. C. D. E. Another Coomb’s test Brainstem auditory evoked response Computed tomography of the head Hemoglobin electrophoresis Indirect retinoscopy

7 -day old breastfeed infant born at term has had decreased appetite, irritability and vomiting for 24 hours. On Physical examination, the infant appears listless. Respiratory Rate: 40/min, Heart Rate : 160/min, and blood pressure: 68/38 mm Hg. The skin and sclera are icteric but no other abnormalities noted. Laboratory studies reveal: Hemoglobin: 12 gm/d. L. Urinalysis is negative for reducing substances. Of the following, the MOST likely diagnosis is: A. B. C. D. E. Bacterial sepsis Blood group incompatibility Breast milk jaundice Hypothyroidism Intrauterine infection

A 3 -day old , breast fed infant develops jaundice. The serum bilirubin level is 12 mg/d. L with a direct bilirubin component of 0. 5 mg/d. L. The infant’s mother asks whether the jaundice might be associated with breastfeeding. Which of the following statements regarding hyperbilirubinaemia associated with breast feeding is TRUE: A. Indirect hyperbilirubinaemia associated with breast feeding may occur as early as the first day of life. B. Water supplementation in breast-fed infants will significantly reduce serum concentrations of indirect bilirubin C. Hyperbilirubinemia associated with breast feeding may persist for 8 to 12 weeks D. Decreased clearance of bilirubin may play a role in breast feeding jaundice, breast milk jaundice.

Of the following conditions, which is the MOST consistent with findings of mild cholestasis without evidence of billiary atresia? A. B. C. D. E. Lead intoxication Chronic hemolytic disease Alpha – antitrypsin deficiency Breast milk jaundice Crigler-Najjar Syndrome

A 4 -week old, breast-fed boy has had mild jaundice since birth. Weight gain has been poor. The urine is light yellow-brown, and the stools are pale yellowgreen in color. At this point, the MOST appropriate next step in management is to: A. Observe the child clinically for 2 to 4 weeks B. Stop breastfeeding and re-examine the child in 7 to 10 days C. Obtain a cholecystogram D. Obtain a total and direct serum bilirubin levels and studies of liver function

The following statement is correct regarding bilirubin A. Is normally excreted in the urine following its conjugation to glucuronic acid B. May achieve high blood levels due to haemolysis associated with glucose-6 -phosphate dehydrogenase deficiency C. Must be prevented from reaching 340 umol/L in well term babies by use of exchange transfusion if necessary D. Results from the oxidation of haemoglobin by the enzyme glucuronyl transferase E. Is normally about 50% bound to albumin and 50% as the unbound

-Neonatal jaundice is associated with all of the following except : A. prematurity B. cystic fibrosis C. Gilbert’s syndrome D. breast milk feeding E. neonatal thyrotoxicosis 60

A Term Baby Is Found to Have Serum bilirubin of 250 umol/l at 18 Hours of Age. Which of the Following Is True? A. Physiological jaundice is the most likely cause B. An urgent conjugated bilirubin level is indicated C. It is unlikely to be due to haemolysis D. The infants blood group and Coombs test are the most important investigations E. There is no indication to start phototherapy

Un-conjugated (indirect) hyperbilirubinaemia occurs in the followings Except: A. on transfusion of incompatible ABO/Rh blood B. Sepsis neonatorum C. in glucose-6 -phosphate dehydrogenase (G 6 PD) deficiency D. in type I Crigler-Najjar syndrome E. Rotter, s syndrome 62

In an infant who appeared healthy at birth, vomiting and diarrhea developed at 1 week of age. She gained weight poorly despite a change from breast milk to infant formula feeding at 2 weeks of age. At 3 weeks of age, she is brought to the emergency department where she is found to be lethargic and to have hepatomegaly. Of the following, the most likely diagnosis is A) Inspissated bile syndrome B) Crigler-Najjar Syndrome C) Galactosemia D) Gilbert Syndrome E) Dubin-Johnson Syndrome
- Slides: 63