Neonatal Hyperbilirubinemia CHO NICU Lecture Prepared by A

Neonatal Hyperbilirubinemia CHO NICU Lecture Prepared by A D’Harlingue MD 12 -13 -10

Objectives • Identify risk factors for severe hyperbilirubinemia • Understand the relationship between hyperbilirubinemia and the risk for neurologic or developmental injury • Discuss ways to screen for infants who might develop severe hyperbilirubinemia • Discuss guidelines for treatment • Identify common pitfalls and best practices in bilirubin management

Bilirubin production • Heme is released from hemoglobin with RBC breakdown • Heme is converted to bilirubin by the action of heme oxygenase • Hyperbilirubinemia results from excessive production or decreased elimination of bilirubin

Epidemiology: increased risk for neonatal jaundice • Race/gender: – Increased risk in males – Increased bilirubin production: East Asian, Native American – G 6 PD: Greek, East Asian, African • Genetic: history of sibling with jaundice – G 6 PD deficiency – gene for Gilbert’s syndrome – Spherocytosis, hexokinase, pyruvate kinase

Epidemiology: increased risk for neonatal jaundice • Maternal: diabetes mellitus – Increased bilirubin production rate – Correlation with macrosomia and polycythemia – Elevated beta-glucuronidase in breastmilk • Maternal drugs: epidural anesthesia (bupivacaine), oxytocin • Delayed cord clamping (polycythemia)

Epidemiology: increased risk for neonatal jaundice: infant factors • Prematurity – Near term infant particularly at risk • Polycythemia • Breast feeding • Caloric deprivation, postnatal weight loss – increased enterohepatic circulation • Delayed passage of meconium

Epidemiology: increased risk for neonatal jaundice: infant factors • Isoimmune hemolysis: Rh , ABO, others • Non-isoimmune hemolysis: infection, drugs, Tantigen exposure, coagulopathy, RBC enzyme deficiencies (G 6 PD, PK, HK) • Hemorrhage: cephalohematomas, intracranial bleeding, bruising • Infection: sepsis, UTI • Endocrine: hypothyroidism, hypopituitarism, adrenal insufficiency

Epidemiology: increased risk for neonatal jaundice • Environmental factors: – Phenolic detergents – Naphthaline (moth balls) • Short hospital stay – Failure to detect significant jaundice – Failure to establish breastfeeding

What is a normal physiologic serum bilirubin? • Dennery et al. NEJM 2001: average peak bilirubin in term newborn, 5 -6 mg/d. L • Breast fed infants are on average about 2 mg/d. L higher than bottle fed infants in the first days of life. • Racial differences – Greek, Asian, Navajo at higher risk

How should non-physiologic jaundice be defined? • Collaborative Perinatal Project (1955 -61) and Maisels (1986): upper limit of physiologic jaundice (95%) 12. 9 mg/d. L • Kaiser (1997): 95%-ile 17. 5 mg/d. L • Multicentered international study (Natus, 1998): 95%-ile 15. 5 mg/d. L, 2 SD 17 mg/d. L at 96 hours • Bhutani. Pediatrics 1999; 103: 6 – Post discharge: 95 th percentile 17. 5 mg/d. L – predictive curves for severe hyperbilirubinemia

Why worry about bilirubin? • Vast majority of patients are asymptomatic except for jaundice • Classic kernicterus is relatively infrequent • Aggressive approach to bilirubin management in the 1970 s was followed by a less aggressive approach in the 1980 s • Bilirubin 20 mg/d. L = Vigintiphobia – Watchko JF, Oski FA. Pediatrics 1983; 71: 660

Why the increase in kernicterus in the late 80 s-90 s? • Increase in breastfeeding • Trend towards earlier discharge of mothers and newborns • Less aggressive approach to jaundice led to an increase in severe hyperbilirubinemia • Increase in bilirubin encephalopathy and kernicterus

Bilirubin injury to the brain • Bilirubin encephalopathy: – Acute reversible changes – Acute irreversible changes • Kernicterus (yellow staining of the brain) • Neurodevelopmental sequelae

Clinical features of kernicterus • Acute form: – Phase 1 (first 1 -2 days): poor suck, stupor, hypotonia, seizures – Phase 2 (mid 1 st week): hypertonia of extensor muscles, opisthotonus, retrocollis, fever – Phase 3 (after 1 st week): hypertonia • Chronic form: – First year: hypertonia, active DTRs, obligatory tonic neck reflexes, delayed motor skills – After first year: movement disorders (choreoathetosis, ballismus, tremor), upward gaze, sensorineural hearing loss Adapted from Dennery, et al. NEJM 2001; 344: 584

Pathology of kernicterus • Orth: described bilirubin pigmentation of the brain of infants with severe jaundice in 1875 • Kernicterus: German word meaning jaundice of the nuclei – Term was coined by Christian Schmorl in 1904 • • Yellow staining of the brain (basal ganglia) Neuronal swelling Programmed death of neurons Gliosis

Pathophysiology of bilirubin encephalopathy • Blood brain barrier – Hyperosmolarity opens the barrier – Hypercarbia increases bilirubin deposition in the brain • Bilirubin binding to albumin: 1: 1 at the first binding site • Displacement of bilirubin from albumin: sulfa drugs, benzyl alcohol, FFA, ceftriaxone • Free bilirubin hypothesis

Cellular mechanisms of bilirubin toxicity • • Formation of bilirubin crystals in cells binding to cellular membranes Decreased Na-K exchange Cellular accumulation of water Axonal swelling Lowers membrane potentials, decreased action potential Decreased amplitude and longer intervals in auditory response • Decreased phosphorylation of protein kinase

Cellular mechanisms of bilirubin toxicity • Decreased phosphorylation of synapsone 1 • Decreased tyrosine uptake and dopamine synthesis in dopaminergic striatal synaptosomes • Bilirubin induced changes in energy metabolism: 31 P nuclear magnetic resonance

Clinical factors which increase the risk for kernicterus or bilirubin encephalopathy • • • Displacement of bilirubin from albumin Duration of severe hyperbilirubinemia Hemolysis Prematurity Hyperosmolarity Hypoxemia, hyperoxemia Hypercarbia Acidosis Sepsis

What is a safe bilirubin level? • 1 g/100 ml of albumin binds 8. 3 mg /100 ml of bilirubin – Free bilirubin increases when the binding capacity to albumin is exceeded • Safe free bilirubin level (Alfors): 1. 3 mcg/d. L to a max of 4 mcg/d. L. – This test generally not available for clinical use

Recent clinical reports of bilirubin encephalopathy • Penn, Stevenson, 1994: TB 50 mg/d. L, E. coli sepsis, abnormal neuro exam (acutely and 4 mo), EEG and MRI. • Maisels, 1995: 6 “healthy infants” with bilirubin injury; range peak bilirubin 39. 0 -49. 7 mg/d. L • Mac. Donald, 1995: 4 term infants with G 6 PD, TB 37 -49 mg/d. L, abnormal neuro exam and seizures • Johnson, 1999: kernicterus registry (125 cases reported) • Estimated incidence of kernicterus in USA: 1: 27, 00055, 000 • Unknown incidence of mild injury

Recent clinical reports of bilirubin encephalopathy • Ebbesen, 2000: 6 cases of kernicterus in Denmark. Peak TB 531 -745 micromole/L (31 -44 mg/d. L) – 1 spherocytosis, 1 galactosemia, 2 ABO incompatibility • Harris, 2001: 6 term and near term infants, TB 26. 4 -36. 9 mg/d. L (5/6 >30). 5/6 presented with abnormal neuro exam. 3/4 had abnormal MRI (increase T 1 signal in basal ganglia). 5/6 had normal neurodevelopmental followup. One infant had CP, MR, encephalomalacia. • Ahlfors, 2003: term, TB 31. 7 at 4 days, unbound bili 7. 7 mcg/d. L, seizures, G 6 PD deficiency, kernicterus at autopsy

Outcome of severe hyperbilirubinemia • Newman, 2003: Kaiser, Northern CA – 11 newborns (1: 10, 000 incidence) of TB > 30 mg/d. L (mean 34. 9, range 30. 7 -45. 5). All treated with phototherapy; 5 XTX. – Normal neurologic outcome in all infants. – One infant died of SIDS, no evidence of kernicterus on autopsy. • Newman, 2006: – 130 newborns: TB 25 -29. 9; 10 newborns TB >= 30 mg/d. L – Outcome at >= 2 yr in 132 bili patients compared to 419 controls – 17% vs. 29% questionable or abnormal neuro findings in hyperbilirubinemia vs. control, P = 0. 04 – Lower cognitive scores for hyperbili pts, if direct Coombs +

JCAHO Sentinel Alert: April 2001 • Risk factors for severe hyperbilirubinemia – – – – Jaundice in the first 24 hours Inadequate PO intake due to suboptimal breastfeeding Mild prematurity: 35 -37 weeks Bruising and cephalohematomas Unrecognized hemolysis: ABO G 6 PD deficiency Genetic/ethnic factors: siblings with jaundice, East. Asian or Mediterranean descent

JCAHO Sentinel Alert: April 2001 • Root causes identified: – Unreliability of visual assessment of jaundice – Failure to measure bilirubin before discharge or in an infant with visible jaundice in the first 24 hours – Early discharge: especially in <38 weeks GA infant – Failure to provide early f/u assessment post discharge – Failure to provide lactation support, information to parents about jaundice or poor feeding – Failure to treat appropriately

AAP clinical practice guideline • Management of hyperbilirubinemia in the newborn infant 35 or more weeks gestation – Pediatrics 2004; 114: 297 • Committee consensus revision of 1994 CPG • Evidence based recommendations

AAP 2004 CPG: Summary recommendations • Promote breastfeeding • Nursery protocols to identify/evaluate jaundice • Jaundice in 1 st 24 hr: serum or transcutaneous bilirubin • Recognize inaccuracy of visual bilirubin assessment • Interpret bilirubin based on infant age (hr)

AAP 2004 CPG: Summary recommendations • Higher risk: < 38 weeks and breastfed • Assessment of risk for severe hyperbilirubinemia at discharge • Parental education • Appropriate follow up based on age at discharge and risk assessment • Appropriate treatment

Strategies to diagnose severe hyperbilirubinemia • Predischarge assessment (bilirubinometer, serum bilirubin) with use of nomogram to predict risk • Identify risk factors: breastfeeding, <38 weeks, h/o jaundice in sib, jaundice prior to discharge home • Standardized hospital policies for screening • Procedures for followup of all newborns 24 -48 hr • Informational materials for parents about jaundice • Lactation support
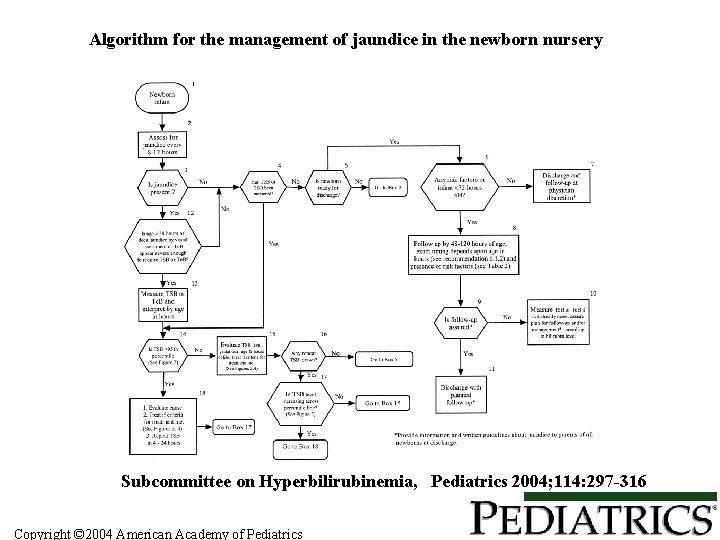
Algorithm for the management of jaundice in the newborn nursery Subcommittee on Hyperbilirubinemia, Pediatrics 2004; 114: 297 -316 Copyright © 2004 American Academy of Pediatrics

Common pitfalls in recognition of at risk infants • Treating the near term infant (35 -37 wk) like a full term infant – Poor feeding – Failure to establish breast feeding – Risk for dehydration – More prolonged jaundice with higher peak in the preterm infant

Best practices • • Promotion of breast feeding Lactation support Weight checks Parental education re: expected feeding, voiding, stooling patterns

Bilirubin measurement and interpretation: common pitfalls • Failure to measure bilirubin in a jaundiced patient, especially in the 1 st 24 hr • Cephalad to caudad progression of skin color used alone to assess jaundice • Failure to interpret the bilirubin level with respect to age in hours
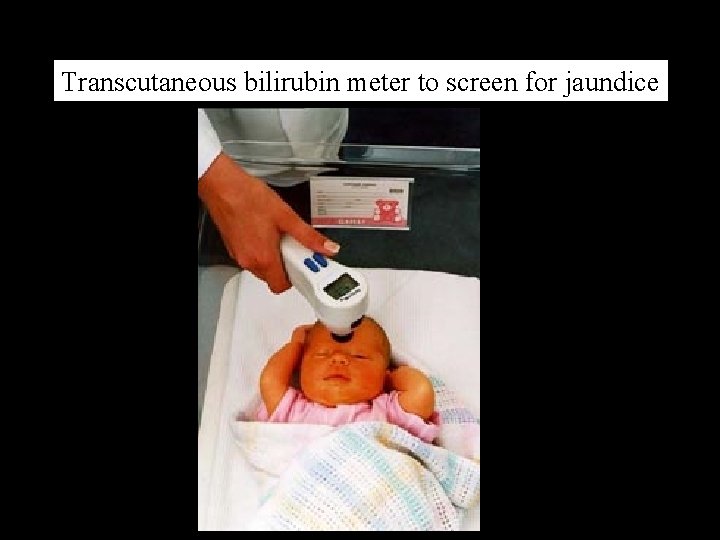
Transcutaneous bilirubin meter to screen for jaundice
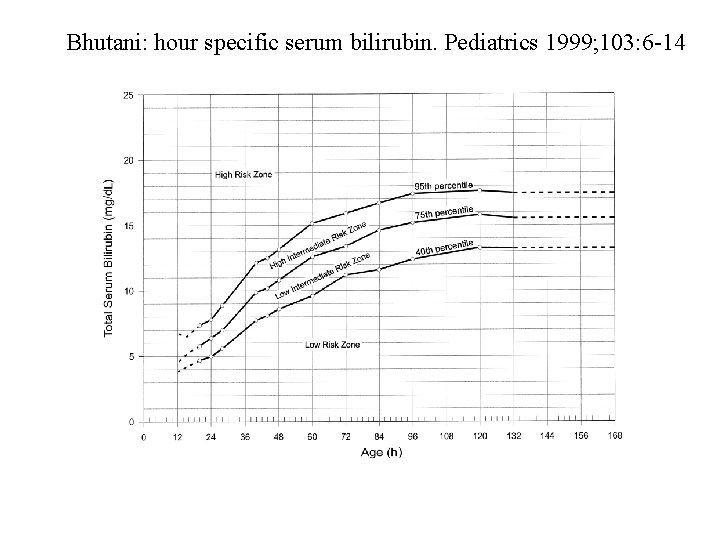
Bhutani: hour specific serum bilirubin. Pediatrics 1999; 103: 6 -14

Predictive nomograms for severe hyperbilirubinemia: Bhutani 1999 • Risk for severe hyperbilirubinemia? (any subsequent bilirubin in the high risk zone, 95%) • Above 95%: 39. 5% • 75 -95%: 21. 6% • 40 -75%: 11. 6% • Below 40%: very low (0)

Use of Bhutani curves to determine timing of follow up visit and/or bilirubin test (one approach) • Compare serum bilirubin or transcutaneous photometer to Bhutani curves • Above 95%: bilirubin within 24 hours • 75 -95%: bilirubin within 48 hours • 40 -75%: if risk factors present, bilirubin within 48 hours • Below 40%: usually no followup bili needed

Risk factors for severe hyperbilirubinemia for consideration with hour specific bilirubin • Exclusive breastfeeding: poor feeding, weight loss • Isoimmune or other hemolytic disease • Previous sibling with jaundice • Cephalohematomas or bruising • East Asian race • Lower gestational age
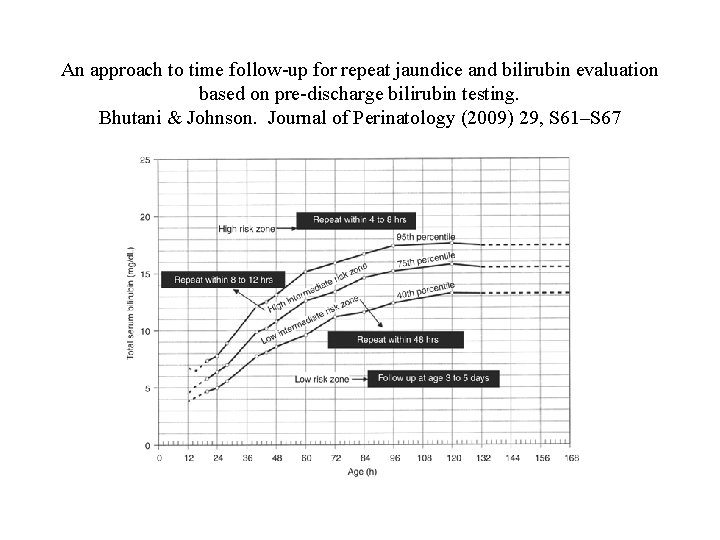
An approach to time follow-up for repeat jaundice and bilirubin evaluation based on pre-discharge bilirubin testing. Bhutani & Johnson. Journal of Perinatology (2009) 29, S 61–S 67

Laboratory evaluation of hyperbilirubinemia • • • Blood type and Coombs CBC and smear, reticulocyte count Direct bilirubin Albumin level G 6 PD Blood culture UA and urine culture Check results of state screen Thyroid studies

Acute management of severe hyperbilirubinemia • Phototherapy with fluorescent blue lights: maximal surface exposure and dose • Correct dehydration: no need to give extra fluids if hydration is normal • Correct acidosis (respiratory and metabolic), and hypotension • Correct hypoalbuminemia (1 g/d. L of albumin binds 8. 3 mg/d. L bilirubin) – Augments removal of bilirubin with exchange transfusion

Acute management of severe hyperbilirubinemia • Avoid drugs which displace bilirubin from albumin – Sulfa drugs, ceftriaxone • IVIG for Rh or ABO isoimmunization – Reduces need for exchange transfusion by blocking Fc receptor of the hemolytic antibody – Dose: 0. 5 -1 g/kg, repeat q 12 -24 hr as needed – May increase risk of NEC • Reduce enterohepatic circulation of bilirubin: – – limited restriction of breast milk feedings use formula feedings Stimulate stooling: frequent feeds, glycerin suppositories Agar, charcoal use has been reported

Phototherapy: pitfalls in its use • Inadequate light source – White vs. blue light – Inadequate output • Non-optimal use of lights – Amount of skin exposure – Distance of the light from the patient • Delays in starting treatment – Referral to ED vs. direct admission

Factors that Determine “Dose” of Phototherapy • • • Spectrum of light Irradiance of light source Design of phototherapy device Surface area exposed to light Distance of infant from light Maisels: N Engl J Med 2008; 358: 920 -8
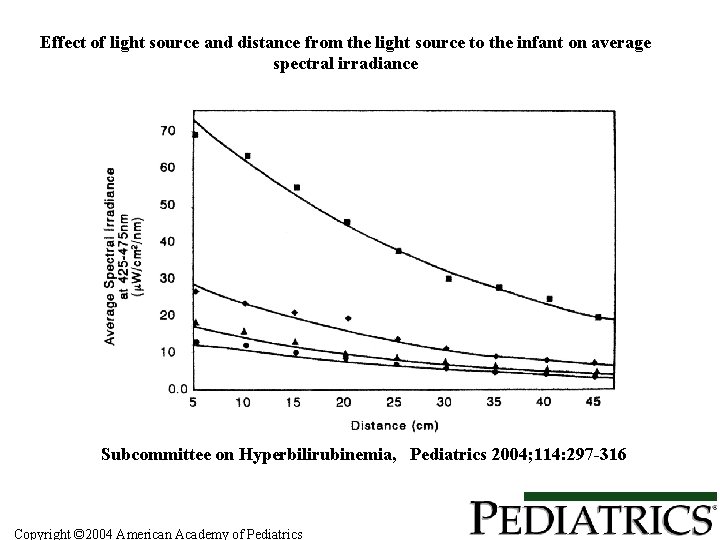
Effect of light source and distance from the light source to the infant on average spectral irradiance Subcommittee on Hyperbilirubinemia, Pediatrics 2004; 114: 297 -316 Copyright © 2004 American Academy of Pediatrics
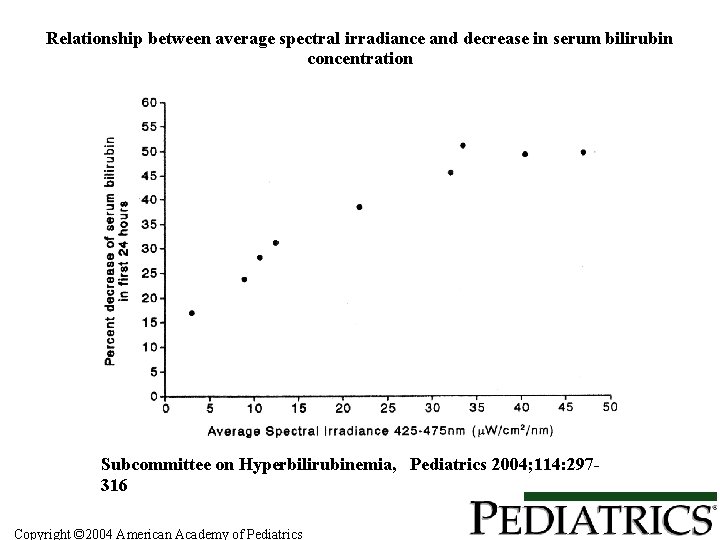
Relationship between average spectral irradiance and decrease in serum bilirubin concentration Subcommittee on Hyperbilirubinemia, Pediatrics 2004; 114: 297316 Copyright © 2004 American Academy of Pediatrics
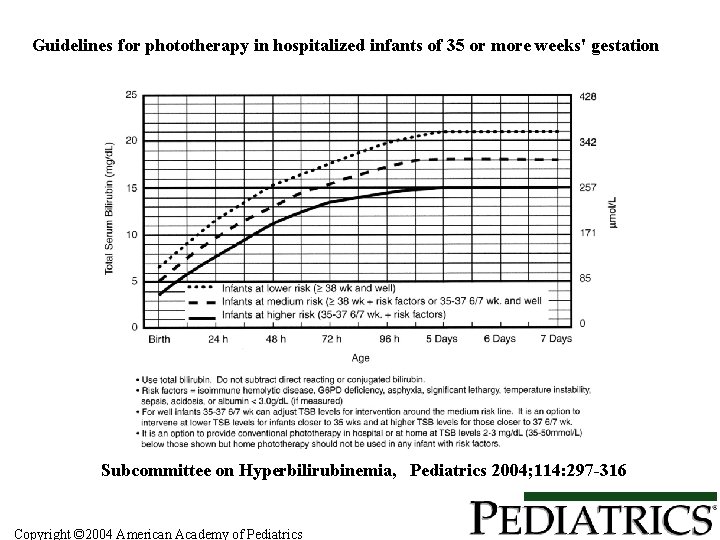
Guidelines for phototherapy in hospitalized infants of 35 or more weeks' gestation Subcommittee on Hyperbilirubinemia, Pediatrics 2004; 114: 297 -316 Copyright © 2004 American Academy of Pediatrics

Risk factors for neurotoxicity affecting bilirubin level to start phototherapy • • • Immune hemolytic disease G 6 PD deficiency Asphyxia Sepsis Acidosis Albumin < 3. 0
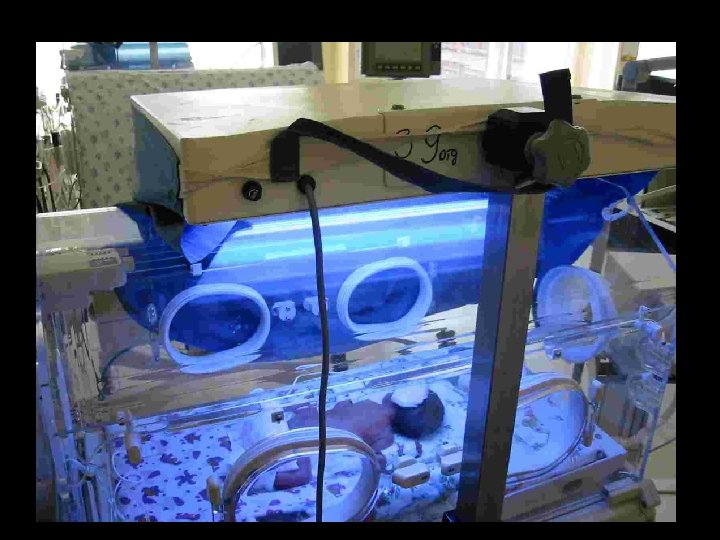
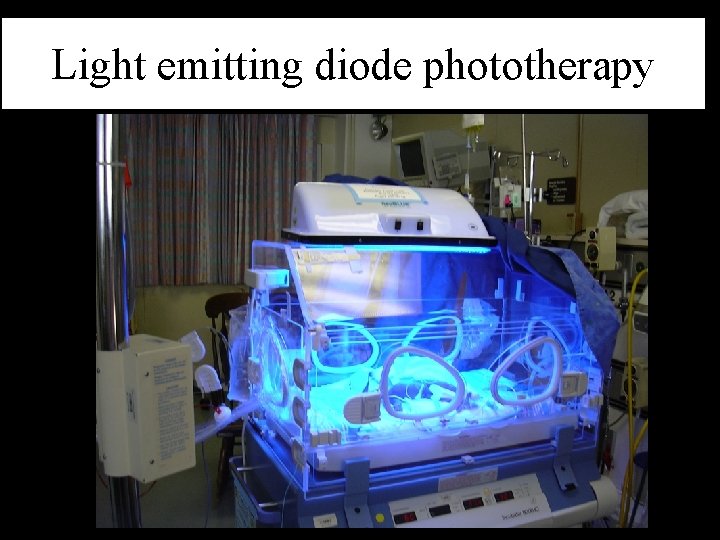
Light emitting diode phototherapy

When to stop phototherapy? • Term and near term infants: TB < 13 -14 mg/d. L – Lower levels if high risk or early severe jaundice • Premature infants <35 weeks: TB <6 -10 mg/d. L • Cholestasis: elevated direct bilirubin • Most infants need not remain in hospital for measurement of “rebound” bilirubin – High risk infants may need f/u outpatient testing

Complications of phototherapy • Increase in stool water loss • Change in skin water loss is minimal • Thermal burns with inappropriate use of halogen lamps • Abrasive injuries with bili blankets in premature infants • Rare skin eruptions • Bronze baby syndrome
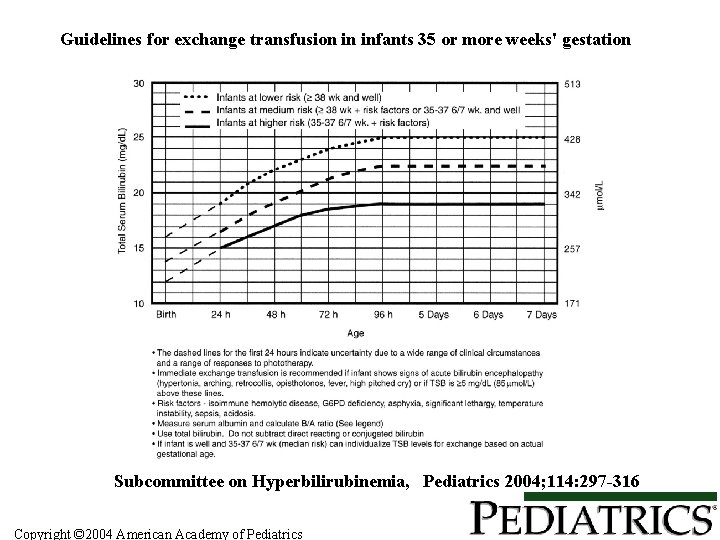
Guidelines for exchange transfusion in infants 35 or more weeks' gestation Subcommittee on Hyperbilirubinemia, Pediatrics 2004; 114: 297 -316 Copyright © 2004 American Academy of Pediatrics

Prematures: observation studies, bilirubin encephalopathy or kernicterus Study Crosse, 1955 Meyer, 1956 Crosse, 1958 Crosse, 1961 Koch, 1959 Hugh-Jones, 1960 bilirubin, mg/d. L >18 >22 >20 >30 adapted from Watchko, Pediatrics 1992; 90: 707

Randomized study of exchange transfusion for hyperbilirubinemia, prematures Patients with indirect bilirubin >18 mg/d. L at >36 hours of age were randomized to exchange transfusion or observation. Study group #kernicterus/total Exchange, bilirubin >18 mg/d. L 0/50 No exchange, bilirubin >18 mg/d. L 1*/50 Not randomized, bilirubin <15 mg/d. L 0/87 *peak indirect bilirubin 27. 6, clinical symptoms noted at 17. 7, seizures at 22. 8, kernicterus noted at autopsy Wishingrad, Pediatrics 1965; 36: 162

Exchange transfusion: criteria • Term: >= 25 mg/d. L >= 20 mg/d. L, Rh disease • 35 -36 weeks: > 25 mg/d. L • 30 -34 weeks: > 20 mg/d. L • < 30 weeks: 15 -20 mg/d. L • Reduce exchange level 3 -5 mg/d. L for seriously ill infants: sepsis, acidosis, respiratory failure • Acute symptoms of bilirubin encephalopathy
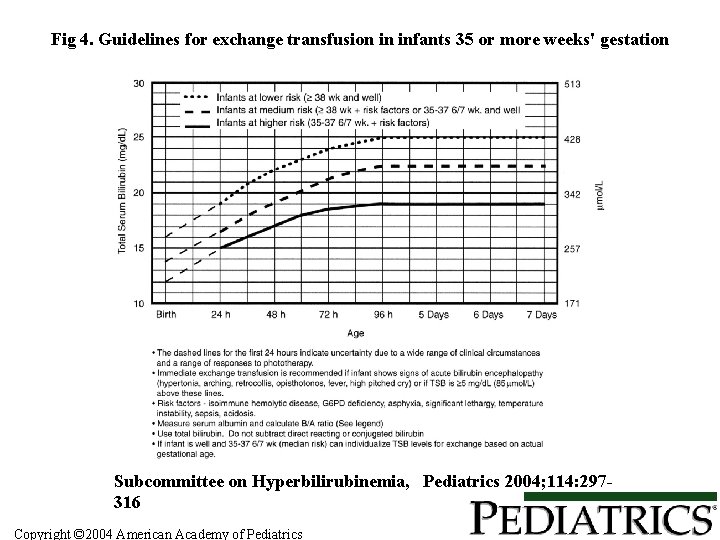
Fig 4. Guidelines for exchange transfusion in infants 35 or more weeks' gestation Subcommittee on Hyperbilirubinemia, Pediatrics 2004; 114: 297316 Copyright © 2004 American Academy of Pediatrics

Exchange transfusion (XTX): criteria • Immediate XTX for patients with acute bilirubin encephalopathy or TB >= 5 mg/d. L above exchange level • Hospitalized patients on intensive phototherapy who cross XTX threshold • Readmitted patients who remain above XTX threshold despite 6 hours of phototherapy

Pitfalls with respect to patients near or above exchange level • Failure to provide intensive phototherapy • Exchange transfusion performed by inexperienced personnel • Failure to recognize the risks and complications of exchange transfusion
Complications of exchange transfusion • Vascular: thrombi, air embolism • Metabolic: hypocalcemia, hypoglycemia • Hematologic: hemolysis, thrombocytopenia, anemia, coagulopathy • Infectious: blood exposure and vascular device related • Mortality: <= 1% • Other: NEC

Patients who might need XTX: Best Practices • Prompt recognition of severe hyperbilirubinemia • Intensive phototherapy • Expanded laboratory evaluation: serum albumin, G 6 PD, blood gas • Blood bank sets up blood for exchange transfusion • Vascular access • Timely referral to a NICU with experienced staff in XTX

Discharge and follow up issues • “Rebound” bilirubin testing • Hearing testing

Final take home messages • Screen all newborns prior to discharge – Bilirubin photometer vs. measured bilirubin in lab – Risk assessment • Appropriate outpatient bilirubin assessment of at risk infants • Beware of the mildly premature infant (35 -37 wk) • Use effective (intensive) phototherapy (blue light) • Parental education about bilirubin • Lactation support
- Slides: 64