Neonatal Fever SHABNAM ZARGAR MD FAAP ASSISTANT CLINICAL

Neonatal Fever SHABNAM ZARGAR, MD, FAAP ASSISTANT CLINICAL PROFESSOR PEDIATRICS UCR SCHOOL OF MEDICINE
Neonatal Fever A 15 day old infant presents to the ED with a temperature of 38. 4 degrees Celsius (101. 4 Fahrenheit). What to do next and why?

Neonatal fever What is neonatal fever? Temperature of 38 degrees Celsius (100. 4 Fahrenheit) in infants 0 -28 days of life. Rectal temperature recommended

Neonatal Fever Why is neonatal fever important? Febrile neonates are at high risk for serious infection (SI) or serious bacterial infection (SBI) because of increased susceptibility to infections, difficulty with clinical examination, and poor outcomes if not diagnosed or treated properly
Neonatal Fever Differential Diagnoses: Meningitis � bacterial or viral Bacterial – GBS, E. coli, Listeria Viral – Enterovirus HSV infections � localized or disseminated infections UTI � E. coli, Enterococcus Bacteremia Sepsis Cellulitis Abscess Osteomyelitis Septic arthritis Viral

Neonatal Fever Most common etiology Viral illness Viral Bacterial etiologies: Most common – UTI Followed by: Meningitis Sepsis or bacteremia Abscess or cellulitis Pneumonia Bacteremia/Sepsis Meningitis Approximately 12%-28% of neonates presenting to a pediatric ED with fever have a SBI - bacteremia, gastroenteritis, cellulitis, osteomyelitis, septic arthritis, meningitis, pneumonia, and UTI (Cincinnati)

Neonatal Fever Febrile infants may have few symptoms to guide diagnosis and management History to obtain: Fever? How high? How was temperature measured? Last anti-pyretic use? Change in feeding? Irritability or lethargy? Seizures? Change in cry? URI symptoms? Difficulty breathing? Swelling of joints or skin changes? Sick contacts? Vomiting or diarrhea?
Neonatal Fever Physical exam Gen: Mentation? HEENT: Anterior fontanelle – bulging? Eyes – Cellulitis/conjunctivitis? Ears – otitis? Nose – congestion? Rhinorrhea? Throat – weak/high pitched cry? Cough? Neck: Swelling? Neck stiffness is a sign in older children Lungs: Retractions? Crackles? Ronchi? CVS: Murmur? Tachycardia? Capillary refill? Pulses? Abdomen: Omphalitis? GU: Circumcised? Skin: Cellulitis/Abscess? Rash? MSK: Joint swelling? Neuro: Mentation? Irritable? Lethargic?
Neonatal Fever Diagnosis Laboratory: Full sepsis workup CBC with manual differential Blood culture UA with microanalysis (urethral catheterization) Urine Culture CSF studies – tube 1 culture, tube 2 protein and glucose, tube 3 cell count and differential, tube 4 – HSV PCR if HSV encephalomengitis suggested If CSF pleocytosis, add enterovirus PCR CXR if symptomatic Stool culture if diarrhea present *Ok to delay LP if patient unstable, do administer antibiotics! *Full septic workup still recommended in neonates with symptoms of bronchiolitis

Neonatal Fever Values CBC with manual differential: Normal WBC 5, 000 -15, 000 per mm 3 WBC < 5, 000 or >15, 000 per mm 3 or ANC >10, 000 per mm 3 have increased risk of SBI CSF: Low risk of meningitis: <20 WBC/mm 3 High risk of meningitis: >20 WBC/mm 3 Other values: High protein >120 mg/d. L and low glucose <40 mg/d. L Urinalysis: WBC < 10/mm 3, negative LE and nitrites

Neonatal Fever Management � Admit to inpatient pending culture results � IV antibiotics to cover common organisms – empirical treatment should be given immediately after cultures obtained Ampicillin and gentamicin Ampicillin and 3 rd generation cephalosporin -Cefotaxime preferred over ceftriaxone *All neonates should be given a single dose of ampicillin and cefotaxime immediately after cultures are obtained � IV antiviral Acyclovir should be started on all neonates who have pending CSF HSV PCR studies Clinical prediction models have not been able to accurately predict SBIs in neonates so common practice remains for hospitalization for sepsis evaluation and IV antibiotics (Fielding-Singh et al. )
Neonatal fever Antibiotics Ampicillin covers Enterococcus and Listeria, also Streptococcus/gram positives Gentamicin covers gram negatives, crosses blood brain barrier Cefotaxime covers gram negatives (rising resistance of E. coli to Ampicillin), crosses blood brain barrier

Neonatal Fever All febrile neonates ≤ 28 days of age should be hospitalized, undergo a full sepsis evaluation, and receive empirical IV antibiotics

Neonatal fever Pre-treated CSF: Can add real time PCR and DNA sequencing for bacterial r. RNA if pleocytosis is present and there is a concern for meningitis
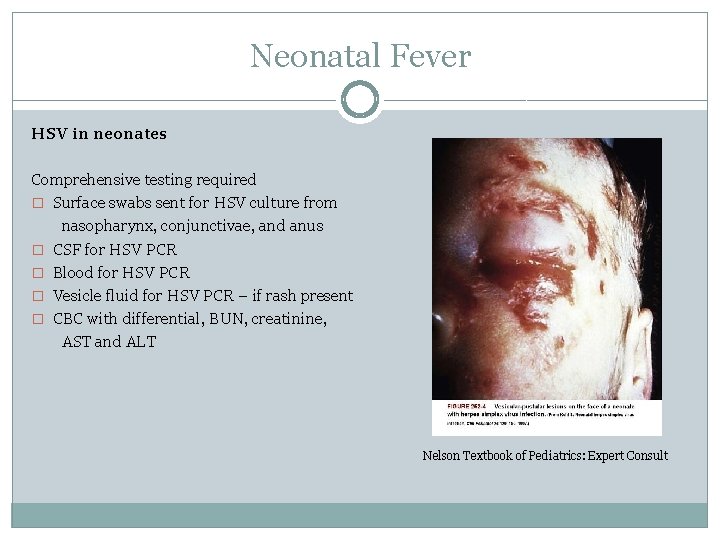
Neonatal Fever HSV in neonates Comprehensive testing required � Surface swabs sent for HSV culture from nasopharynx, conjunctivae, and anus � CSF for HSV PCR � Blood for HSV PCR � Vesicle fluid for HSV PCR – if rash present � CBC with differential, BUN, creatinine, AST and ALT Nelson Textbook of Pediatrics: Expert Consult
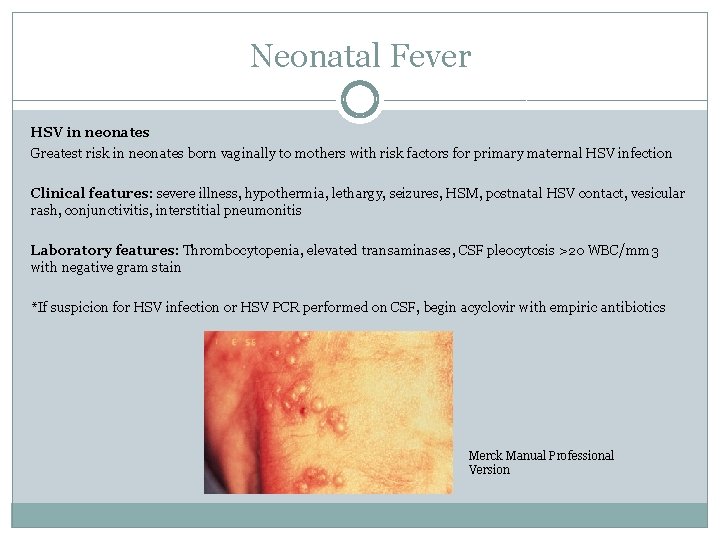
Neonatal Fever HSV in neonates Greatest risk in neonates born vaginally to mothers with risk factors for primary maternal HSV infection Clinical features: severe illness, hypothermia, lethargy, seizures, HSM, postnatal HSV contact, vesicular rash, conjunctivitis, interstitial pneumonitis Laboratory features: Thrombocytopenia, elevated transaminases, CSF pleocytosis >20 WBC/mm 3 with negative gram stain *If suspicion for HSV infection or HSV PCR performed on CSF, begin acyclovir with empiric antibiotics Merck Manual Professional Version

Neonatal Fever How long to admit for? Standard length of hospitalization: 48 hours – “ 48 hour rule out sepsis” Studies are being performed to determine if 48 hours of hospitalization is really needed Recent studies have also looked at low risk criteria for treating febrile neonates less conservatively but concluded that low risk criteria are not sufficiently reliable to exclude SBIs in febrile neonates

Neonatal Fever One study from Hospital Pediatrics (Fielding-Singh et al. ): Objective: To determine the risk of a positive, pathogenic bacterial culture of blood or CSF in infants ≤ 30 days beyond 24 hours after collection Methods: retrospective review of 1, 145 infants ≤ 30 days with blood or CSF cultures drawn at Santa Clara Valley Medical Center in San Jose, CA from 19992010. High risk infants had WBC <5, 000 or >15, 000 per microliter, bands >1, 500 per microliter, or abnormal UA Results: 1, 876 blood and CSF cultures were identified. 79% were hospitalized and of those hospitalized, 45% were for fever without a source. 2. 7% had pathogenic cultures and 0. 5% had a time to notification >24 hours (not statistically significant), of those 0. 5%, all had fever without source and highrisk criteria. No low-risk criteria patient had a time to notification >24 hours. 1. 8% of high risk patients had growth 24 -48 hours. Conclusion: Low-risk infants hospitalized for fever without source may not need hospitalization for 48 hours to rule out bacteremia or meningitis

Neonatal fever Study continued: Mean and median time to notification 24. 5 ± 17. 1 and 19 hours for pathogens and 45. 3 ± 30. 7 and 35. 8 hours for contaminants, respectively

Neonatal Fever Previous studies: Time to positivity of blood and CSF cultures in neonates suggest that 48 hours is necessary to identify >95% of cases, however, these studies included infants in the ICU where Co. NS and yeast cultured from central lines take time to grow (Fielding et al. )

Neonatal Fever Approximately 90% of bacterial pathogens are identified within the first 24 hours of incubation (Byington et al. ) Infants 0 -6 months of age: Blood cultures: Mean time to positivity for true pathogens is ~17. 5 hours Urine and CSF: Median time to positivity are 16 and 18 hours, respectively

Neonatal Fever Consider discharge at 24 hours if bacterial cultures negative and viral studies positive (excluding HSV) AND well-appearing Patients with bronchiolitis or other viral infections are at lower risk of SBI Seattle Children’s recommends this

Neonatal Fever Discharge criteria: �Well-appearing �Tolerating PO �Follow up available within 48 -72 hours �Family and primary care team agree with plan �Cultures negative

Neonatal Fever If a neonate presents with fever to your clinic -Send to the ED If you receive a call from a mom stating her neonate has a fever -Send to the ED If you are working in the ED and have a neonate with fever -Perform full septic workup, give first dose of ampicillin and cefotaxime, and admit to inpatient If you are the admitting inpatient team – continue/begin empirical antibiotics, making sure urine, blood, and CSF cultures have been drawn (if LP not successful and patient appears meningitic – do not delay antibiotics), and observe 48 hours pending cultures

Neonatal Fever Side note: Neonates with meningitis need to be admitted to a hospital with pediatrics ID and PICU -Complications – seizures, empyema, elevated ICP -BAER and ophthalmology exam

Neonatal Fever Possible QI project? Develop a standardization pathway of management of neonatal fever in our institution based on clinical evidence Standardization improves medical care!

References Bishop, Julianne, and S. Heath Ackley. Clinical Standard Pathway: Neonatal Fever. Project Owners, Aug. 2013. Web. 20 July 2015. https: //www. seattlechildrens. org/pdf/neonatal-fever-learning-module. pdf. Byington, Carrie L. , F. Rene Enriquez, Charles Hoff, Richard Tuohy, E. William Taggart, David R. Hillyard, Karen C. Carroll, and John C. Christenson. "Serious Bacterial Infections in Febrile Infants 1 to 90 Days Old With and Without Viral Infections. " Pediatrics 113. 6 (2004): 1662 -666. Caserta, Mary T. "Neonatal Herpes Simplex Virus (HSV) Infection - Pediatrics. " Merck Manuals Professional Edition. Merck Sharp & Dohme Corp, May 2013. http: //www. merckmanuals. com/professional/pediatrics/infections-inneonates/neonatal-herpes-simplex-virus-hsv-infection. Accessed 24 July 2015. Cincinnati Children's Hospital Medical Center. Evidence-based care guideline for fever of uncertain source in infants 60 days of age or less. October 27, 2010. http: //www. cincinnatichildrens. org/svc/alpha/h/health-policy/evbased/default. htm. Accessed July 20, 2015 Fielding-Singh, Vikram, David K. Hong, Stephen J. Harris, John R. Hamilton, and Alan R. Schroeder. "Ruling Out Bacteremia and Bacterial Meningitis in Infants Less Than One Month Of Age: Is 48 Hours of Hospitalization Necessary? " Hospital Pediatrics 3. 4 (2013): 355 -61. Web. Hamilton, Jennifer L. , and Sony P. John. "Evaluation of Fever in Infants and Young Children. " American Family Physician (2013): http: //www. aafp. org/afp/2013/0215/p 254. html. Accessed July 20, 2015. Kliegman, Robert M. , Bonita M. D. Stanton, Joseph St. Geme, and Nina F. Schor. Nelson's Textbook of Pediatrics: Expert Consult. 20 th ed. Philadelphia: Elsevier, 2016. Jain, Shabnam, John Cheng, Elizabeth R. Alpern, Cary Thurm, Lisa Schroeder, Kelly Black, Angela M. Ellison, Kimberly Stone, and Evaline A. Alessandrini. "Management of Febrile Neonates in US Pediatric Emergency Departments. " Pediatrics 133. 2 (2014): 187 -95.
- Slides: 27