Neonatal Emergencies After Discharge Robert Englert M D

Neonatal Emergencies (After Discharge) Robert Englert, M. D. Dept Neonatology Bethesda Naval Hospital

Most Interesting ED Chief Complaints Drank the dog’s milk - from the dog’s nipple l Needs a circumcision because his tonsils are so big l Can’t find baby’s birthmark l Piece of bologna string hanging from anus l Baby is afraid of his hands l

Case Presentation 10 day old male presents to ED with 1 day history poor feeding, lethargy and, over last 1 -2 hours, increasing work of breathing. Pre- and postnatal history are unremarkable.

ABC’s of Neonatal Resuscitation Airway l

Initial Management l IV access l monitor l oxygen

Initial Management - Therapy l Respiratory Support l Volume l Antibiotics

Diagnostic Tests ABG l CBC l Lytes l Cultures l Radiography l

Categories l Infectious l Cardiac l Endocrine

Late-Onset Infections Group B Streptococcus l E. coli l Listeria l H. influenza, S. Pneumonia, N. meningitis l Viral l – RSV, HSV, Enterovirus

Group B Streptococcus 1 -3/1000 live births l Up to 1/3 women colonized l Early and late onset disease l Antibiotics around delivery affect early onset not late onset l Late onset highly associated with meningitis l

Listeria monocytogenes Early and late onset disease l Early onset often associated with meconium staining even in preterms l Late onset disease is primarily meningitic l

Escherichia coli K 1 capsular antigen uniquely associated with neonatal meningitis l K 1 related not only to invasive disease, but to more severe outcomes l Significant association with galactosemia likely due to depressed PMN function caused by elevated serum galactose levels l Urosepsis/posterior urethral valves l

Case Presentation l 4 day old infant African American male presents to ER because of decreased feeding, lethargy, poor color, increased work of breathing, prenatal history unremarkable, spent 2 days in hospital, no reported problems, discharged 48 hours ago
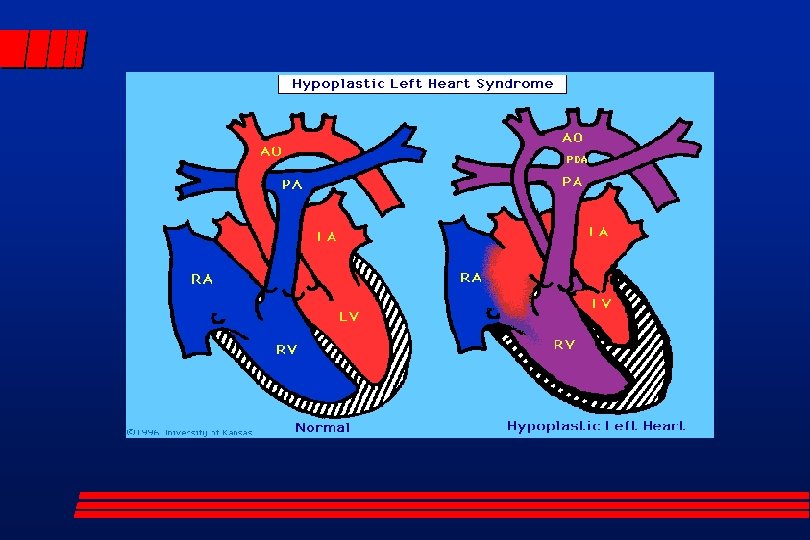
Ductal Dependent Cardiac Lesions l Left sided heart lesions – Systemic blood flow is dependent upon ductal patency » coarctation of the aorta » interrupted aortic arch » hypoplastic left heart

Ductal Dependent Cardiac Lesions Left Sided shock l cardiac failure - hepatosplenomegaly, large heart, gallop l Pressor support l prostaglandin E 1 l – side effects: » Flushing, Hypotension, Pyrexia (fever) » idiosyncratic apnea

Case Presentation 3 d old caucasian male presents to ER because of poor feeding, lethargy, comfortable tachypnea, “color not right”, harsh murmur l Pre-natal Hx unremarkable, no U/S done during pregnancy l D/C to home at 26 hol l

Ductal Dependent Cardiac Lesions l Right sided heart lesions – pulmonary blood flow is dependent on ductal patency » tetralogy of Fallot » transposition of great vessels » tricuspid atresia » pulmonary stenosis/atresia
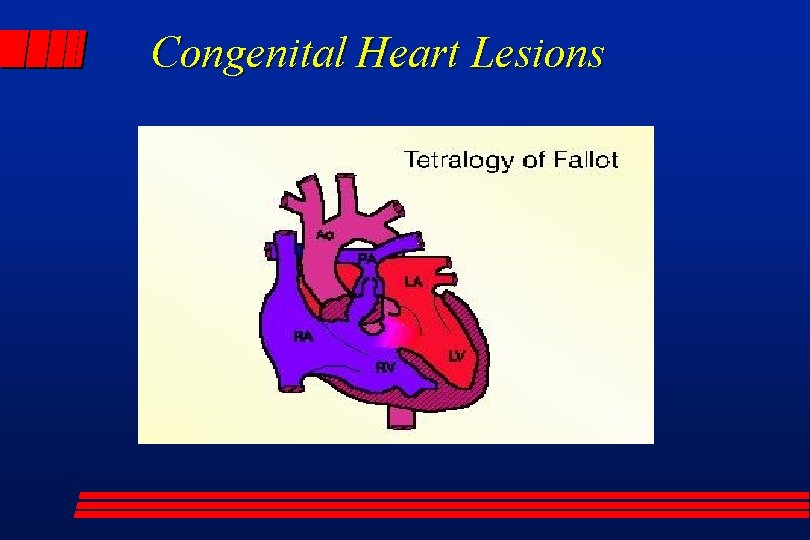
Congenital Heart Lesions
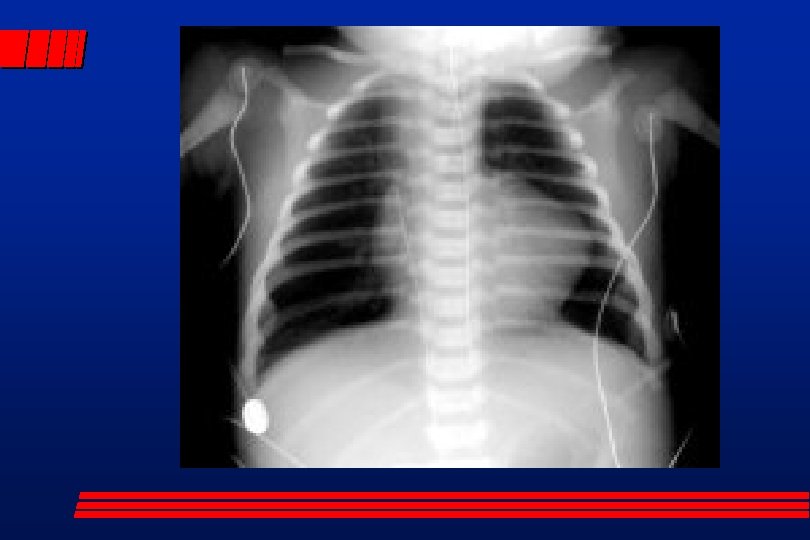

Case Presentation Infant is tachycardic, 200 -220/min, mottled with poor perfusion. Poor feeding, Respirations are labo with rate of 80/min.

Neonatal Rhythm Disturbances l Fast l Slow l In between


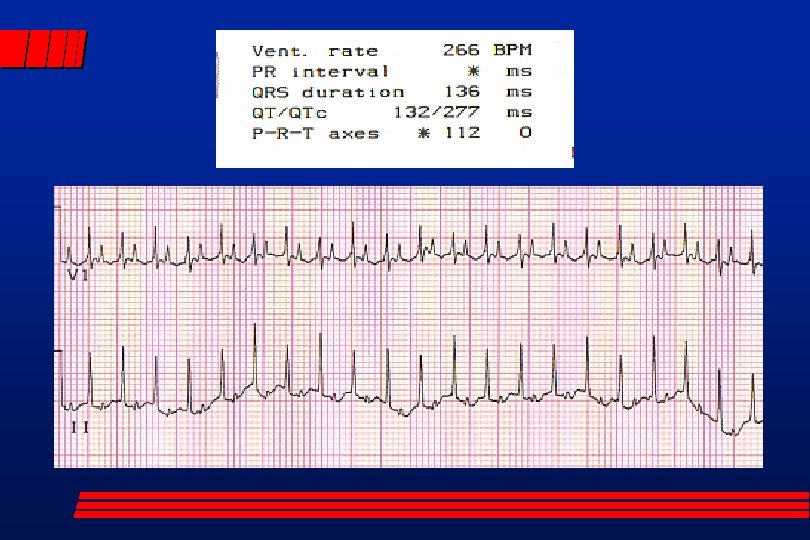
Supraventricular Tachycardia persistent ventricular rate of > 200/min l fixed RR interval l abnormal P wave shape or axis, abnormal PR interval, or absence of P waves l little change in rate with activity, crying, etc. l

Supraventricular Tachycardia most common symptomatic arrhythmia in children l may be associated with WPW syndrome or Ebstein’s anomaly l CHF rare in first 24 hrs; 50% after 48 hrs l

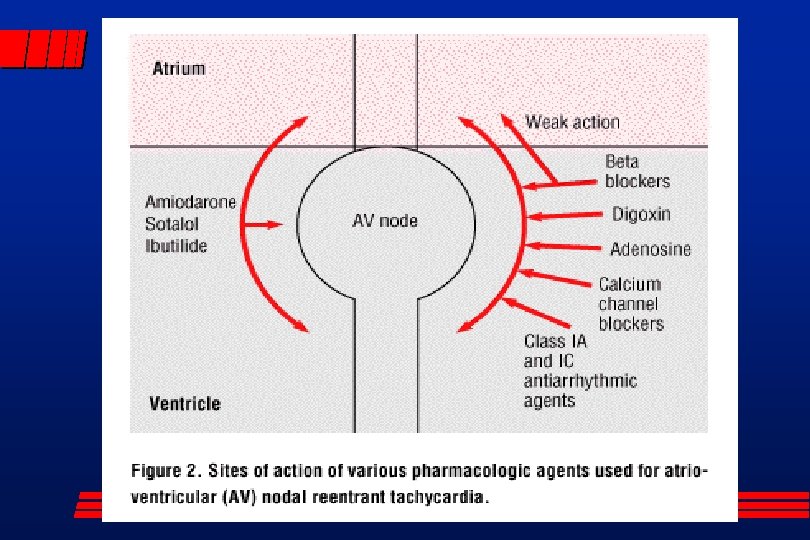
Supraventricular Tachycardia unstable vs stable l synchronized cardioversion in unstable patient l vagal stimulation (ice to face) l adenosine l side effect of all cardioversion methods: l – asystole – death

Case Presentation 29 yo Black female G 4 P 0 presents at 35 +2 weeks with swollen ankles l No Ctx, normal cervical exam, labs pending l FHR noted to be 280, U/S otherwise normal l BPP 4/10, Delivered via LTCS l
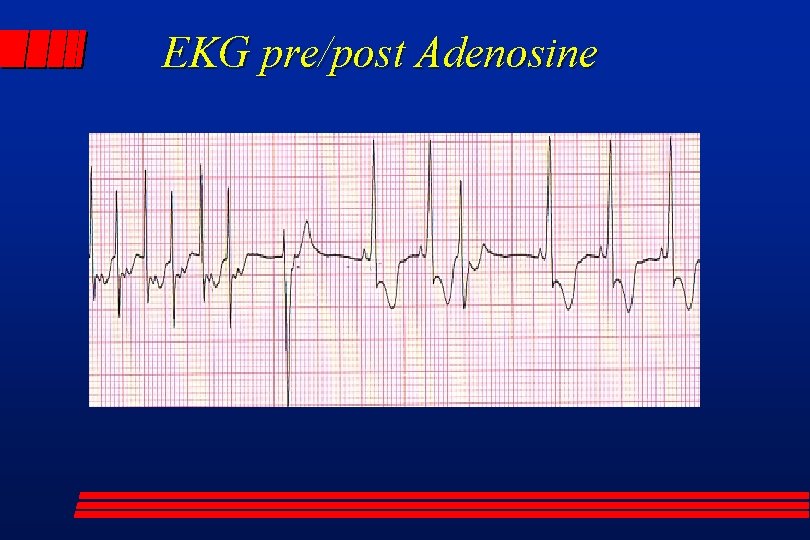
EKG pre/post Adenosine


Neonatal Hyperthyroidism Maternal Graves disease - 1/2000 pregnancies l Thyroid-stimulating immunoglobulins cross the placenta l Mothers with symptomatic disease may be treated with PTU l

Neonatal Hyperthyroidism l Infants of mothers with Graves disease may be: – goitrous and hypothyroid – euthyroid due to maternal PTU which crosses the placenta – hyperthyroid due to maternal thyroidstimulating Ig

Neonatal Hyperthyroidism Transplacentally acquired thyroidstimulating Ig may exert effects for up to 12 weeks postnatally l Thyroid storm l – Irritibility – Respiratory distress – Severe tachycardia – Cardiac failure

Neonatal Thyrotoxicosis Treatment l Suppress excess secretion of hormone and conversion of T 4 >>T 3 l – PTU and/or Potassium Iodide (Lugol’s) l Adrenergic Blockade – Propranolol

Case Presentation A 7 lb male newborn has bilateral cryptorchidism and hypospadius. At 7 days of age infant presents to the ER with a history of vomiting. The baby is pale, tachycardic, hypotensive. l Believe it or not it happens…. . l

Congenital Adrenal Hyperplasia group of enzyme defects which impair steroid hormone production l 21 -hydroxylase - 90% of cases l two forms l – partial: simple virilizing – more complete deficiency: salt losing

Congenital Adrenal Hyperplasia females are virilized; males usually appear normal l salt losing - adrenal insufficiency occurs under basal conditions l – significant impairment of cortisol and aldosterone synthesis – most have onset of symptoms at 6 -14 days – shock with hypoglycemia, hyponatremia, hyperkalemia, acidemia

Congenital Adrenal Hyperplasia Treatment treat hypovolemia l correct sodium and potassium if necessary l hydrocortisone is steroid of choice l mineralocorticoid replacement may be necessary l

Inborn Errors of Metabolism Alteration in mental status l acidosis l hypoglycemia l electrolyte abnormalities l ketosis l hyperbilirubinemia l

Inborn Errors of Metabolism Hepatomegaly l Seizures l Hyperammonemia l Reducing substances in urine l

Inborn Errors of Metabolism The Smell Test l l l l Maple Syrup Urine Dz maple syrup Isovaleric acidemia sweaty feet Tyrosinemia rancid butter Beta-methylcrotonylcoenzyme A def. tomcat’s urine phenylketonuria mousy/musty methionine malabsorption cabbage trimethylaminuria rotting fish

Conclusions ABC’s l Monitor, IV, Oxygen, Antibiotics l Diagnostic tests l Know the differential l
- Slides: 43