Neighbourhood deprivation and Stop Smoking Service outcomes Leonie

Neighbourhood deprivation and Stop Smoking Service outcomes Leonie Brose 1, Volker Behrends 2 1 Addictions, UK Centre for Tobacco and Alcohol Studies, Institute of Psychiatry, KCL 2 Department of Surgery and Cancer, Imperial College

Acknowledgements Professor Robert West Dr Andy Mc. Ewen Everyone at the NCSCT who helped with the data provision North 51 All service managers who agreed to share data My post is funded by the UK Centre for Tobacco and Alcohol Studies. Funding from the Medical Research Council, British Heart Foundation, Cancer Research UK, Economic and Social Research Council and the National Institute for Health Research under the auspices of the UK Clinical Research Collaboration, is gratefully acknowledged (MR/K 023195/1).

• Social injustice kills • England: Gap in life expectancy 17 years • Other negative effects, unaffordable to ignore Approaches – Universal health care – Address health behaviours • Smoking particular determinant of inequality

Deprivation and smoking Smoking and cessation England 1 Most deprived Least deprived Smoking men % 33 14 Smoking women % 26 10 Ever smokers who quit % 50 75 • Not less likely to attempt to stop, but attempts less successful e. g. 2, 3 • In stop smoking services (2001 -03): ‘Rather than quitting smoking, disadvantaged smokers quit treatment’ 4 1 Office for National Statistics, 2014. 2 Kotz et al, 2009. 3 Reid et al, 2010. 4 Hiscock et al, 2011

Questions 1. To what extent is neighbourhood deprivation associated with – loss to follow-up – success of quit attempts while taking into account other demographic or treatment characteristics? 2. Can difference in success be explained by loss to follow-up? 3. Does neighbourhood deprivation add anything above and beyond other indicators of deprivation?

How we measured deprivation • Index of multiple deprivation, IMD • 38 indicators in seven domains – – – – Income Employment Health and disability Education and Training Barriers to housing & services Living environment Crime • Available across England for Lower Super Output Areas – LSOAs: neighbourhoods consisting of about 1500 residents • Other indicators – Occupation (NS-SEC) – Education – IMDs for larger areas, e. g. service

Sample • 555, 744 treatment episodes from 2009 to 2012 – Excludes 14% of initial sample: ongoing treatment, telephone support, prisoners, incomplete postcodes • Linked to Index of Multiple Deprivation for neighbourhood (LSOA) using postcode • Split into 10 groups of different levels of deprivation relative to all English LSOAs

Measures – associations? Deprivation • Index of Multiple Deprivation, 10 groups • Occupation NS-SEC: employed v not employed • Exemption from prescription charges Demographics • Age • Gender • Heaviness of smoking (18%) Outcomes • Loss to 4 -week follow-up • Self-reported 4 -week success • 4 -week CO-validated success rates (lost=no) Intervention • Medication • Type • Setting • First or later attempt with stop smoking service
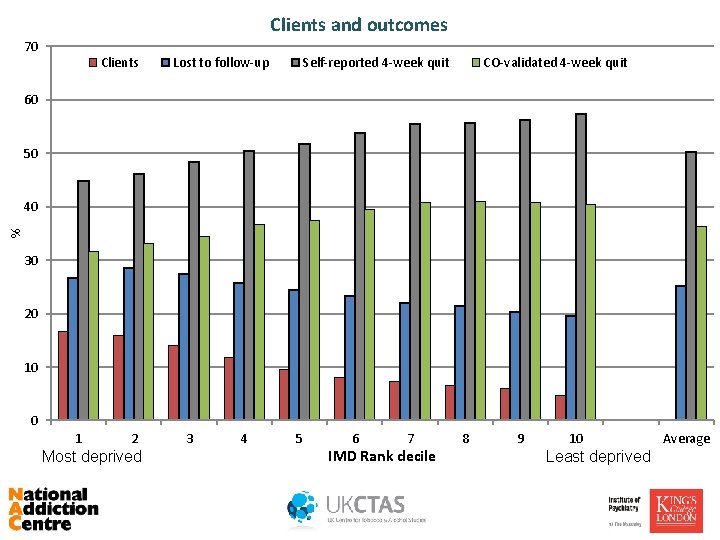
Clients and outcomes 70 Clients Lost to follow-up Self-reported 4 -week quit CO-validated 4 -week quit 60 50 % 40 30 20 10 0 1 2 Most deprived 3 4 5 6 7 IMD Rank decile 8 9 10 Least deprived Average
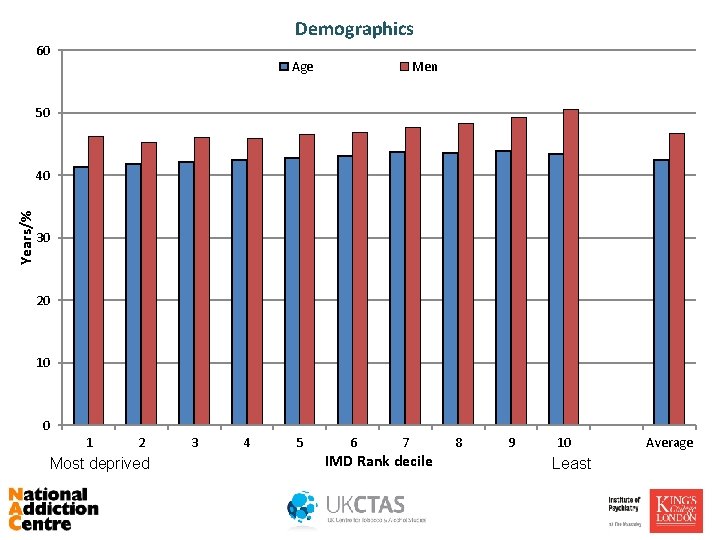
Demographics 60 Age Men 50 Years/% 40 30 20 10 0 1 2 Most deprived 3 4 5 6 7 IMD Rank decile 8 9 10 Least Average
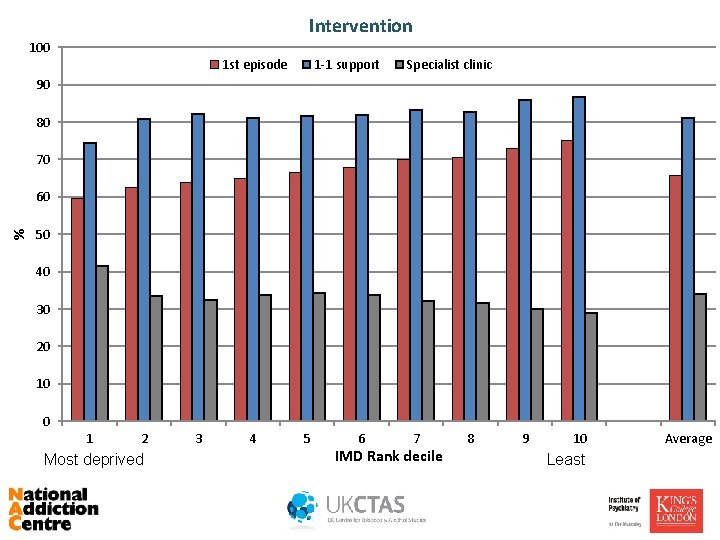
Intervention 100 1 st episode 1 -1 support Specialist clinic 90 80 70 % 60 50 40 30 20 10 0 1 2 Most deprived 3 4 5 6 7 IMD Rank decile 8 9 10 Least Average
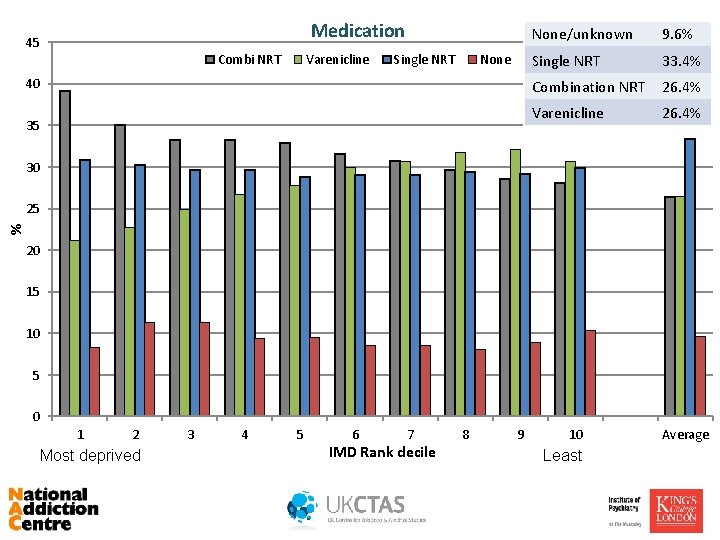
Medication 45 Combi NRT Varenicline Single NRT None 40 35 None/unknown 9. 6% Single NRT 33. 4% Combination NRT 26. 4% Varenicline 26. 4% 30 % 25 20 15 10 5 0 1 2 Most deprived 3 4 5 6 7 IMD Rank decile 8 9 10 Least Average
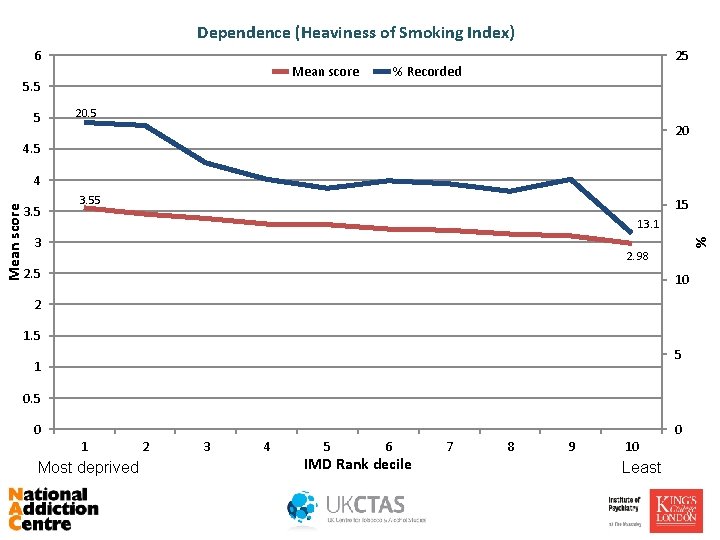
Dependence (Heaviness of Smoking Index) 6 Mean score 5. 5 5 25 % Recorded 20. 5 20 4. 5 3. 55 15 13. 1 3 % Mean score 4 2. 98 2. 5 10 2 1. 5 5 1 0. 5 0 0 1 Most deprived 2 3 4 5 6 IMD Rank decile 7 8 9 10 Least

Each step from more to less deprivation vs 1 st time vs 1 -1 vs specialist clinic

Does loss explain differences in success? • Lost usually treated as not successful - Loss to follow-up closely linked to success rates • Only completed episodes (416, 436 episodes): – Association success and deprivation only very slightly smaller (OR=1. 03, 95% CI: 1. 03 to 1. 03, p<0. 001) Ø No
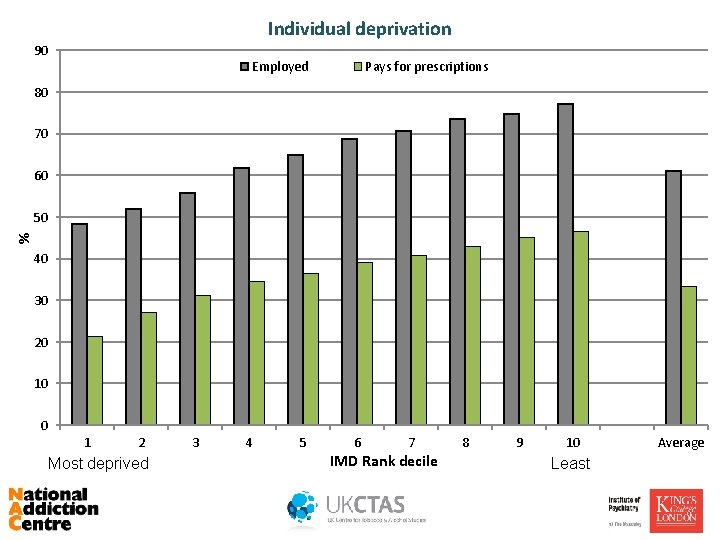
Individual deprivation 90 Employed Pays for prescriptions 80 70 60 % 50 40 30 20 10 0 1 2 Most deprived 3 4 5 6 7 IMD Rank decile 8 9 10 Least Average
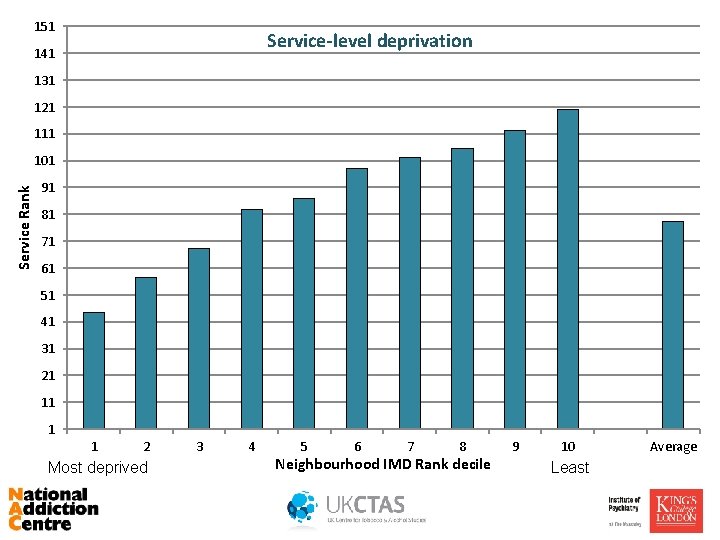
151 Service-level deprivation 141 131 121 111 Service Rank 101 91 81 71 61 51 41 31 21 11 1 1 2 Most deprived 3 4 5 6 7 8 Neighbourhood IMD Rank decile 9 10 Least Average

Does neighbourhood deprivation add anything to other indicators? • Added individual indicators of deprivation and service-level deprivation to model • All closely related, but – Neighbourhood deprivation remained associated with reduced follow-up and quit success – Unemployment, exemption and service-level deprivation also associated with worse outcomes Ø Yes

Conclusions • Services continue to support many disadvantaged smokers • Follow-up rates and success rates decrease with deprivation • Some characteristics that are associated with reduced success also associated with deprivation – Additional hurdles to stopping – Do not explain difference in outcomes • Limitations – Data collected prior to 2013 – Repeated recording of the same individual

Some remaining questions Why? Background quit rates? Those returning may need more/different support What is the full picture on dependence? What causes difference in medication use across deprivation? • Recording practice pharmacies? • • • Thank you Leonie. brose@kcl. ac. uk
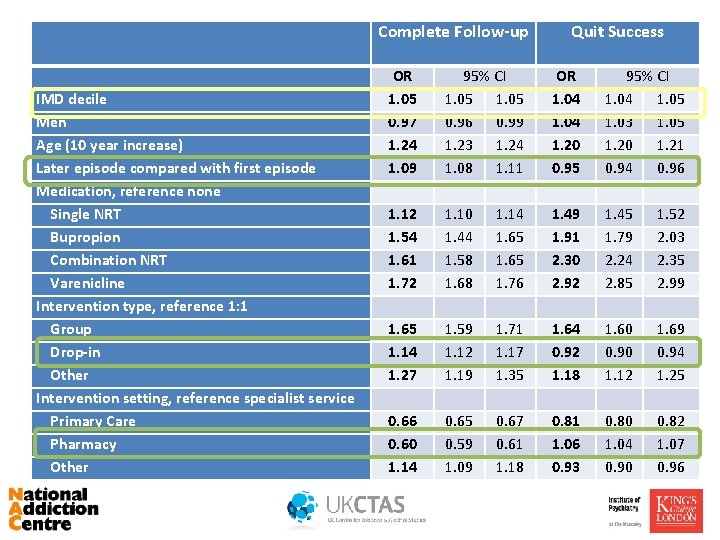
IMD decile Men Age (10 year increase) Later episode compared with first episode Medication, reference none Single NRT Bupropion Combination NRT Varenicline Intervention type, reference 1: 1 Group Drop-in Other Intervention setting, reference specialist service Primary Care Pharmacy Other Complete Follow-up OR 1. 05 0. 97 1. 24 1. 09 95% CI 1. 05 0. 96 0. 99 1. 23 1. 24 1. 08 1. 11 1. 12 1. 54 1. 61 1. 72 1. 10 1. 44 1. 58 1. 68 1. 14 1. 65 1. 76 1. 65 1. 14 1. 27 1. 59 1. 12 1. 19 1. 71 1. 17 1. 35 0. 66 0. 60 1. 14 0. 65 0. 59 1. 09 0. 67 0. 61 1. 18 Quit Success OR 1. 04 1. 20 0. 95 1. 49 1. 91 2. 30 2. 92 1. 64 0. 92 1. 18 0. 81 1. 06 0. 93 95% CI 1. 04 1. 05 1. 03 1. 05 1. 20 1. 21 0. 94 0. 96 1. 45 1. 52 1. 79 2. 03 2. 24 2. 35 2. 85 2. 99 1. 60 1. 69 0. 90 0. 94 1. 12 1. 25 0. 80 0. 82 1. 04 1. 07 0. 90 0. 96
- Slides: 21