NECROTIZING ENTEROCOLITIS NEC Disease of premature low birth
NECROTIZING ENTEROCOLITIS
NEC Disease of premature & low birth weight infant. Difficult to define. Epidemiology Unclear risk factors. 2. 3 -11% of infant with less than 1500 kg. What are the best treatment strategies ? B. W. Incidence &Pathophysiologic fatality inversely associated with factors What are the optimal prevention ? race. 1 -BLACK intestinal motility. Considerable mortality & morbidity. infant. digestion. 2 -Male intestinal Overlooked long term sequelae. of 15 -30%. 3 -Mortality mucous coat. increased to 50% when surgery is necessary. 4 -Mortality tight junctions. n. NOS long-term outcomes. 5 -Worse intestinal regeneration. cases in full-term. 6 -90% NO. of cases are preterm. Occasional e. NOS have the same clinical & patho. Findings but 7 -Term endotoxin (LPS). i. NOS 8 -different PAF-AH. initiating factors. economic burden. 9 -considerable EGF (HB-EGF). 10 - balance between constrictor ET-1 & dilator NO. 11 - balance between commensal & pathologic Bactria.

Work-up for NEC History Abdominal examination Ø Symptoms & signs. Ø Exclude extra -abd. Problems Ø Feeding regimen. Ø Medications Ø Abd. Wall discoloration. Ø Abd. distention. Ø Pain, tenderness. Ø Palpable mass. Ø Scrotum. Ø Ø Ø Lab. Test Imaging WBC. Platelet. Hb. ABG. Lactic acid. Ø Erect abd film. Ø Lat. decubitus film. Ø Serial X-rays. Ø Finding ? • Ileus. • Fixed loop. • Pneumatosis. • Portal V. gas. • pneumoperit.


Medical management for NEC Q/ For how long to continue on medical treatment ? • Stop all feeds. Gastric • decompression 7 – 10 days. • Insert NG Q/ If patient shows clinical improvement ? • Specificfeeds. AB • Broad Startspectrum slowly advancing AB • Anti-fungal ? Q /If patient not tolerate feeds ? Serial abd. exam, • Clinical deterioration • Repeat episode of NEC. lab. Test & • Frequency of serial tests & imaging. • Post-NEC stricture. imaging

Post-NEC stricture Most commonly occur in : the left colon near splenic flexure. But may occur anywhere. What investigation you should consider ? Contrast enema & UGI study. Which is first to perform? & why ?


When to operate on NEC ? I- Absolute indications: Free air. II- Relative indications: “best” • 1 - Portal venous gas. • 2 - positive paracentesis. • 3 - clinical deterioration. “good” • 1 - fixed loop. • 2 - erythema. • 3 - palpable mass. “fair” • Severe pneumatosis. Do not decide to operate after one assessment but after serial examinations.

Surgical management Peritoneal drain Vs laparotomy ! Ø Mortality ? Ø Early results ? Ø Delayed result ? Patients with peritoneal drain may have Howneurological to decide between drain & years laparotomy worse outcomes 1 -2 after ? • Currently is better. patients. NEC recovery unknown comparedwhich to laparotomy • Neurological outcomes. Why ? ? ? • Focal area of perforation. (drain , laparotomy). NEST (necrotizing enterocolitis surgery trial) • Discuss with family. • RCT study. • 300 patients. • Follow up 18 -22 months after NEC recovery • Results are expected in 2016.

Peritoneal drain Technique: 1 - bedmanagement: side. Drain 2 • L. A Irrigate the drain regularly to keep it patent. When to feed ? 3 incision. • transverse Start to remove it after 7 -10 days. If patient doing well, start feeds. 4 RIF. • If continued of stool ? If there is feedingleakage intolerance, contrast study 5 - penrose drain. 6 - avoid too large incision. Hernia. 7 - enter abdominal cavity with hemostate. 8 - place the drain carefully. 9 - install normal saline to wash abd. Cavity. 9 - secure the drain in place.
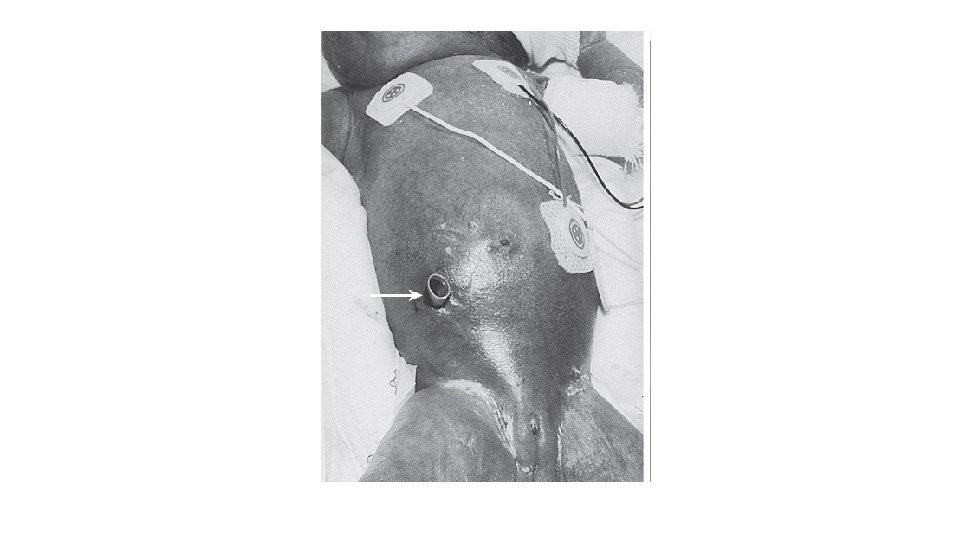

Operative management Pre-operative: 1 - resuscitate the patient & correct any coagulopathy. 2 - set up packed RBC, FFP, platelets for OR. Surgical technique: In the OR or bedside in NICU. Supra-umbilical transverse incision. Abd. Wall is very thin bowel, liver, spleen injury. Assess the integrity of intestine, ischemia, necrosis, perforation. Segmental necrosis resection & primary anastomosis. proximal stoma & mucous fistula. stoma creation: Bring the stoma out through the same incision. Bring out the functional stoma & mucous fistula next to each other. Proper fixation of both ends to the fascia. Leave more length of the distal end. It is not necessary to mature the stoma.

Management of diffuse NEC Usually see diffuse pneumatosis, unhealthy bowel but not necrotic. ofgoskip This. Management is usually occur if you to OR lesions too early. Need to decide if there is something to with resect. Consider resecting all lesions together one anastomosis. Management of NEC totalis If unsure, it is better to leave intestine for second look. If you not, are resect individual lesions, multiple anastomosis, proximal Currently no technique can manage such problem. Consider leaving the abdomen open of if there are dilated bowel. diverting stoma. Likelhood of survival through years TPN to reach liver & Management of extremely friable bowel Clipping &transplant dropping: intestine is zero Result from being forced to%. operate when the inflammatory Management of tension pneumoperitoneum Usually for unstable patient with no time for anastomosis. Just close the abdomen & pursue comfort caremultiple for the patient. process in the abdomen is at the peak. Abdominal compartement syndrome may occure free air. Only resect necrotic &realistic return another dayfrom to complete Discuss withthe family & give them explanations. The smartest decision a bowel surgeon can make is know when to stop Decompress using angiocath as a temporizing maneuvuer as the anastomosis when the patient is more stable. the operation & return another day. patient may not be stable enough to go to OR. Continuing the operation will result in more serosal tears & bowel injuries & worse outcome to patient. If possible, identify the proximal bowel & create a diverting stoma.

Post - operative management Reversing the stoma: Consider after the patient is stable & tolerating feeds. Wait until the patient is at least 2 kg. Consider re-feeding through mucous fistula if the patient has high output stoma. If there are signs of TPN- induced cholestasis or you cannot nourish the patient because of high output stoma, then consider closing the stoma sooner. Re-feeding through mucous fistula: Recent article shows a substantial decrease in TPN use. Be careful when creating the mucous fistula as they often retracted or get stenosis. Consider leaving a soft catheter in the fistula postoperatively to keep it open. Thank you
- Slides: 14