NCMB opioid prescribing update and guidance on recognizing

NCMB opioid prescribing update and guidance on recognizing opioid misuse and abuse Debra A. Bolick, MD Board Member North Carolina Medical Board 1203 Front Street | Raleigh, NC 27609 www. ncmedboard. org | info@ncmedboard. org North Carolina Medical Board 800. 253. 9653 www. ncmedboard. org | info@ncmedboard. org

NCMB mission The North Carolina Medical Board was established in 1859 by the General Assembly "in order to properly regulate the practice of medicine and surgery for the benefit and protection of the people of North Carolina. " North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

2017 Medical Board North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Board composition Eight physicians NP and PA (one each) Three public members North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Objectives • Review of new CME requirement • Review the Safe Opioid Prescribing Initiative • Strategies for recognizing and responding to abuse/diversion • Tools for monitoring opioid patients • Resources • Q&A North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

New CME requirement • 2015 -2016 state budget provision called on boards to adopt CS CME requirements • Requires physicians and PAs who prescribe controlled substances to earn relevant CME during each CME cycle Primary objectives: • Reduce inappropriate opioid prescribing and associated patients deaths and harm • Improve quality of care North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

New CME requirement Effective July 1, 2017 Who must comply? Physicians and PAs who prescribe ANY controlled substances (even nonopioids). Residents are exempt. MDs/DOs: Three hours of relevant CME during each three year CME cycle PAs/NPs: Two hours of relevant CME in each two year CME cycle North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

How will this affect you? • If you prescribe controlled substances you must earn relevant CME by end of current CME cycle • NCMB sent emails late Feb – early March to all physicians and PAs; Physicians were told what CME cycle year they are in. • About 9 percent of physicians are currently in Year 3 and must complete CME this calendar year • PAs who maintain NCCPA certification may use their current NCCPA two-year cycle North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

What are qualifying education topics? Best practices in prescribing controlled substances Chronic pain management Recognizing signs of misuse and abuse North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Enforcing the new requirement • Licensees are NOT required to submit documentation of each course completed • NCMB will continue its established practice of random CME audits to determine compliance • Licensees are advised to keep records for 6 years, in the event they are audited North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

How do I let NCMB know I complied? • Annual license renewal questionnaire includes a new section about the CS CME requirement • Controlled substances prescribers will check a box to indicate that they prescribe CS and that they understand they are responsible for completing the necessary CME • Licensees who do not prescribe CS will check a box to indicate this North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Where to find courses • Many existing CME courses meet requirement • NCMB does not approve or certify courses – if the education topic is covered and the course is appropriately certified, it will count • Multiple free/low cost courses on website: www. ncmedboard. org/prescribing. CME North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

NCMB/ Wake. AHEC course • NCMB and Wake AHEC received grant to develop one hour opioid CME Webinar – this is available online on NCMB website • Webinar complemented by live opioid panel discussions offered at different locations across the state. • Sessions for fall 2017 and beyond are being added regularly North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

What value to nonopioid prescribers? • NCMB believes all controlled substances prescribers benefit from a good understanding of opioid overdose epidemic • Example: Psychiatrists rarely prescribe opioids but most prescribe benzodiazepines – concomitant use of opioids and benzos greatly increases risk of opioid overdose • Non-opioid prescribers need to screen patients for opioid use before prescribing benzos North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Objectives • Review of new CME requirement • Review the Safe Opioid Prescribing Initiative • Strategies for recognizing and responding to abuse/diversion • Tools for monitoring opioid patients • Resources • Q&A North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Safe Opioid Prescribing Initiative • Launched April 2016 • Typical Board investigations are reactive – e. g. case is opened in response to information received; patient harm often has already occurred • SOPI is proactive – cases are opened based on criteria developed by the Board, using data provided by NCCSRS • NCMB can potentially ID prescribing of concern before harm occurs North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Safe Opioid Prescribing Initiative • NCMB is expected to take a leadership role in addressing opioid overdose crisis • Being selected for investigation is NOT an assumption of substandard practice • Program goals: identify licensees of concern and reduce inappropriate opioid prescribing • NCMB hopes to ID licensees of concern not previously known to the Board North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Who is investigated? • Physicians and PAs who managing large numbers of patients at high doses of opioids • Physicians and PAs with multiple patient deaths due to opioid overdose • As of Sept. 2017, SOPI has directly impacted (e. g. a case has been opened) 82 licensees – 0. 2 percent of all active physicians and physician assistants North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

SOPI investigative criteria (eff. July 1) • Top two percent prescribing 100 milligrams of morphine equivalents (MME) per patient per day. • Top two percent prescribing 100 MMEs per patient per day in combination with any benzodiazepine • CS prescribers with two+ patient deaths within a 12–month period due to opioid poisoning AND who prescribed 30+ tablets of opioids within 60 days of patient death North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
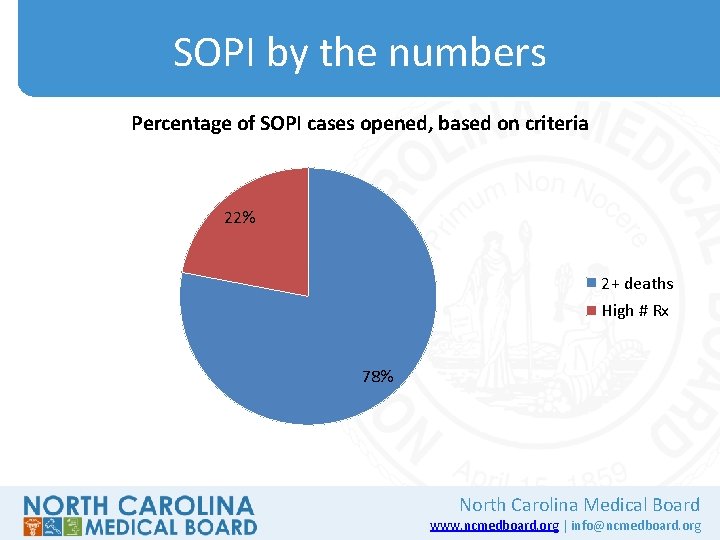
SOPI by the numbers Percentage of SOPI cases opened, based on criteria 22% 2+ deaths High # Rx 78% North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Areas of practice represented • More than half of licensee cases opened involve prescribers who practice either pain management OR physical medicine & rehab • Most other cases involve licensees practicing family/internal medicine, emergency medicine or psychiatry • No cases involved hospice or palliative medicine providers (cause of death = cancer, not opioid overdose) North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
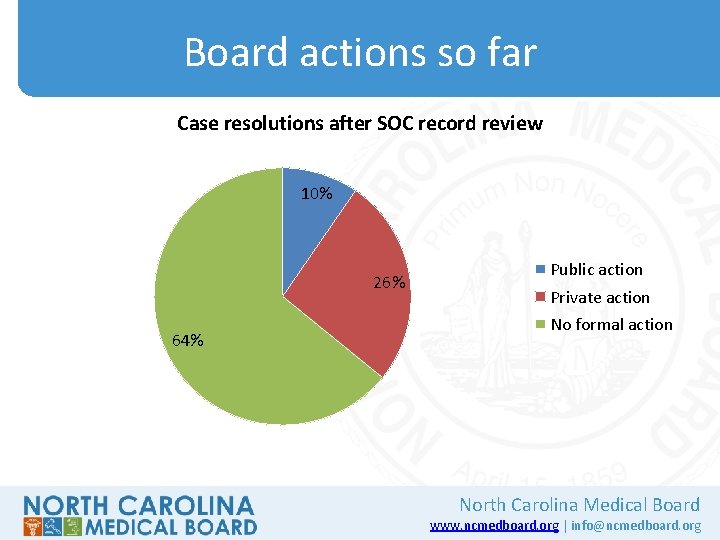
Board actions so far Case resolutions after SOC record review 10% 26% 64% Public action Private action No formal action North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Some final points • NCMB recognizes that chronic pain is a legitimate medical issue and that patients deserve appropriate care • NCMB has not established a limit on opioid prescribing for chronic pain – use professional judgment to determine treatment • Whatever treatment plan is established, clearly document rationale North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Objectives • Review of new CME requirement • Review the Safe Opioid Prescribing Initiative • Strategies for recognizing and responding to abuse/diversion • Tools for monitoring opioid patients • Resources • Q&A North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Misuse and diversion Systematic review from 38 studies (26% primary care settings, 53% pain clinics) Source: Vowles, et al 2015 Misuse rates: 21 -29% Misuse = Opioid use contrary to the directed or prescribed pattern of use, regardless of the presence or absence of harm or adverse effects. Addiction rates: 8 -12% Addiction = Pattern of continued use with experience of, or demonstrated potential for, harm North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Risk assessment • Opioid Risk Tool (ORT) • Screener and Opioid Assessment for Patients with Pain-Revised (SOAPP-R) • Adequate family history, physical exam, and information from prior/current providers • CSRS prescription medication history • Initial urine drug screen prior to prescribing, at least annually thereafter • Consider offering naloxone for increased risk factors North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Increased risk of misuse • History of Substance Use Disorder (SUD) or illicit drug use • Psychiatric conditions, specifically unstable or untreated conditions • Few supports or resources at home/in community • Multiple prescribers of opioids, high doses of opioids, and/or in combination with benzos North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Aberrant medication-taking behaviors In order of severity (lower to higher): • Requests for increased opioid dose • Requests for specific opioids, brand name, many allergies • Non-adherence with other recommended therapies (e. g. PT) • Running out early (unsanctioned dose escalation) • Deterioration in function at home or work (talk to family) • Non-adherence w/monitoring (pill counts, urine drug screen) • Multiple “lost” or “stolen” scripts • Illegal activities (forging scripts, selling opioid prescriptions) North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Discussing possible abuse/diversion • Stay 100% in “Benefits/Risk” mindset • Address patient behaviors which raise concerns about abuse (running out, “lost” scripts, etc. ) • Remember that patients may suffer from both chronic pain and addiction • Intervention based on level of risk and concern for safety: “I cannot responsibly continuing prescribing opioids because I feel it would cause more harm than good” • Always offer referral to treatment • May need to abandon risky treatment, but not patient. North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Opioid tapering – general approach • Speed of taper depends on level of concern vs. apparent risk of harm • Individualize tapering plans based on patient goals and concerns • First reduce dose to smallest dosage unit • Then, increase time between doses o An IR/SA opioid may be started after tapering to lowest dose of ER/LA opioids o May use α 2 - adrenergic agonist to treat withdrawal North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

For best results • Use shared decision making as much as possible in planned taper • Build up alternative pain treatment modalities • Consider treatment for substance use disorder if present • Communicate clearly with patient and set expectations • Document, document North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Opioid use disorder (DSM-V) • • • Taken in larger amounts or for longer periods Persistent desire/unsuccessful efforts to reduce usage Great deal of time spent obtaining/using opioids Craving, or strong desire to use opioids Failure to fulfill work/home obligations due to opioid use Lack of concern for problems due to recurrent opioid use Lack of interest in activities that used to be important Recurrent use of opioids despite hazards Continued use despite known problems due to opioid use North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Opioid use disorder (DSM-V) • Tolerance (except for those under medical supervision) o Markedly increased amounts to achieve desired effect o Markedly diminished effect with continued use at same amount • Withdrawal (except for those under medical supervision) o Characteristic opioid withdrawal syndrome o Opioids are taken to relieve or avoid withdrawal syndrome Mild OUD: 2 -3 Criteria Moderate OUD: 4 -5 Criteria Severe OUD: >6 Criteria Taken from American Psychiatric Association North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

SUD treatment options • Substance Abuse and Mental Health Services Administration (SAMHSA) treatment locator: www. samhsa. gov/treatment • AA or NA – free, widely available • State resources (NC DHHS) o Acute treatment services (detoxes), residential treatment o Methadone maintenance treatment programs North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Buprenorphine treatment • Office-based opioid treatment • Clinicians must complete training and obtain a DATA waiver to lawfully treat patients with buprenorphine • PAs must complete 8 hours, plus an additional 16 hours of training to obtain waiver North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Objectives • Review of new CME requirement • Review the Safe Opioid Prescribing Initiative • Strategies for recognizing and responding to abuse/diversion • Tools for monitoring opioid patients • Resources • Q&A North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Monitoring methods • Pain contracts-single prescriber, single pharmacy • Pill counts • Use of prescription drug database (CSRS, SC-PMP Aware) • Periodic urine drug screening • Whatever methods used, be consistent and follow up – i. e. pill counts are off, contract is violated, scripts are filled consistently but drug is NOT in system, or additional drugs are in system North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Thoughts on UDS • Urine drug screening can be a helpful tool if used and interpreted correctly o Know common false positives, know your lab o Understand the pharmacology of opioid prescriptions and what to look for o Have a plan for responding to unexpected results North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Thoughts on UDS • Immunoassay-POC test, qualitative. GS/MSmore sensitive and specific, confirmatory • No established criteria for frequency, but every visit is not indicated for stable, compliant patients-use clinical judgment • Insurance companies will not cover “excessive” UDS, leaving patients to foot the bill for costly tests North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

UDS resource • NC Governor’s Institute has established a page with UDS guidance information • Incorporates content from NCMB about common issues with UDS Find it here: http: //governorsinstitute. org/opioid/clinicaltools/uds/ North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

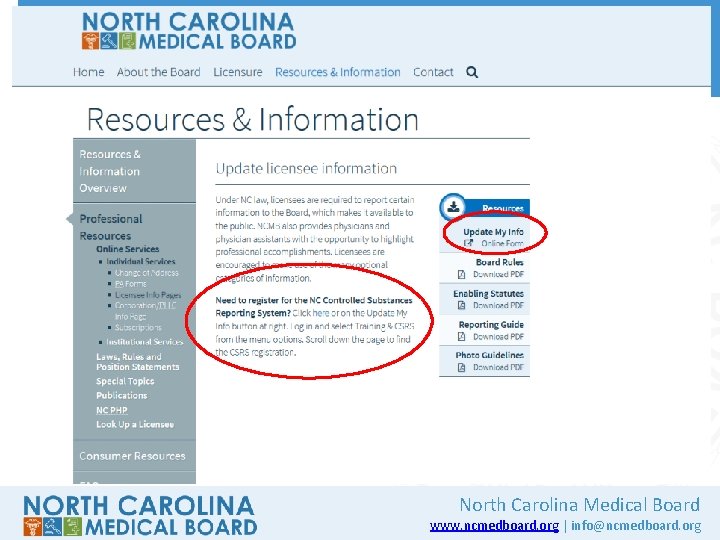
NC CSRS • 2016 NC General Assembly passed a bill that makes NC CSRS registration mandatory • STOP Act of 2017 requires mandatory NCCSRS use before prescribing • All DEA registration holders are subject • Requirement does not take effect until NC CSRS completes technical upgrades • NCMB encourages timely registration. Why wait? North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
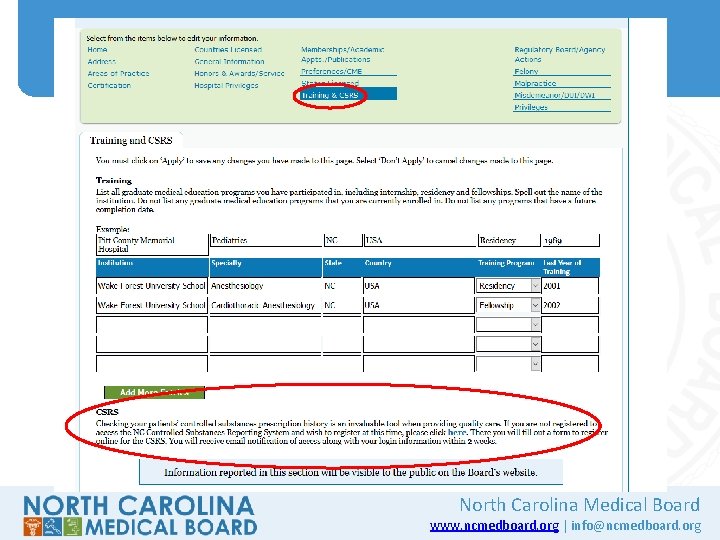
North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

STOP Act: NC CSRS Utilization • The STOP Act (signed into law June 2017) would require mandatory use of NC CSRS for many prescribers • Review of patient’s 12 -month prescription history required before issuing initial prescription for a Schedule II or Schedule III opioid • Subsequent 12 -month reviews required every three months for as long as patient remains on the opioid North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

STOP Act: NC CSRS Utilization • NC CSRS review NOT required if medication is: o administered in a health care setting, hospital, nursing home, outpatient dialysis facility or residential care facility o prescribed for the treatment of cancer or another condition associated with cancer OR o prescribed to patients in hospice care or palliative care North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

If using NC CSRS, don’t ignore data • Most common problem NCMB sees with NC CSRS (and UDS) is failure by the clinician to respond to aberrant results • If results suggest misuse or abuse, prescriber is expected to consider information, act and document! • Continuing or escalating opioids in the face of evidence of aberrant use is not consistent with accepted standards of care and could result in discipline North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Objectives • Review of new CME requirement • Review the Safe Opioid Prescribing Initiative • Strategies for recognizing and responding to abuse/diversion • Tools for monitoring opioid patients • Resources • Q&A North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Resources • NCMB voted in January 2017 to adopt the CDC Guideline for Prescribing Opioids for Chronic Pain – this replaces NCMB’s previous opioid position statement. • CDC policy is guidance, not rule – recommendations may not be appropriate for all patients. Use your professional judgment. • Opioid guidelines developed by other reputable organizations may be useful, as well. North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

STOP Act resources • STOP Act summaries available in flyer and text only format • NCMB has developed STOP Act FAQs and is adding to the collection as needed • CDC resources on tapering opioids; condensed version of CDC Guideline for patient education All available at: www. ncmedboard. org/safeopioids North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org

Thank you! Questions? Evelyn Contre, Chief Communications Officer 919 -326 -1109 x 235 or econtre@ncmedboard. org Jean Fisher Brinkley, Communications Director 919 -326 -1109 x 230 jean. brinkley@ncmedboard. org North Carolina Medical Board www. ncmedboard. org | info@ncmedboard. org
- Slides: 55