NBT guidelines for management of patients presenting with
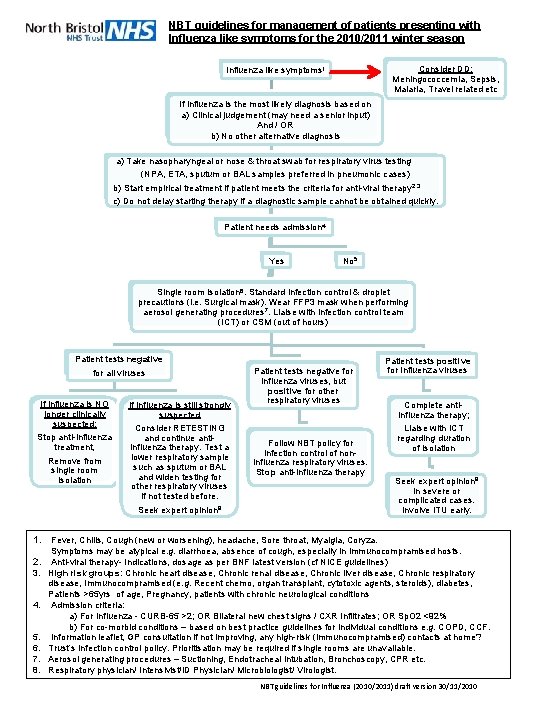
NBT guidelines for management of patients presenting with Influenza like symptoms for the 2010/2011 winter season Consider DD: Meningococcemia, Sepsis, Malaria, Travel related etc Influenza like symptoms 1 If influenza is the most likely diagnosis based on a) Clinical judgement (may need a senior input) And / OR b) No other alternative diagnosis a) Take nasopharyngeal or nose & throat swab for respiratory virus testing (NPA, ETA, sputum or BAL samples preferred in pneumonic cases) b) Start empirical treatment if patient meets the criteria for anti-viral therapy 2, 3 c) Do not delay starting therapy if a diagnostic sample cannot be obtained quickly. Patient needs admission 4 Yes No 5 Single room isolation 6. Standard infection control & droplet precautions (i. e. Surgical mask). Wear FFP 3 mask when performing aerosol generating procedures 7. Liaise with infection control team (ICT) or CSM (out of hours) Patient tests negative for all viruses If influenza is NO longer clinically suspected: Stop anti-influenza treatment, Remove from single room isolation 1. 2. 3. 4. 5. 6. 7. 8. If influenza is still strongly suspected Consider RETESTING and continue antiinfluenza therapy. Test a lower respiratory sample such as sputum or BAL and widen testing for other respiratory viruses if not tested before. Seek expert opinion 8 Patient tests negative for Influenza viruses, but positive for other respiratory viruses Follow NBT policy for infection control of noninfluenza respiratory viruses. Stop anti-influenza therapy Patient tests positive for Influenza viruses Complete antiinfluenza therapy; Liaise with ICT regarding duration of isolation Seek expert opinion 8 in severe or complicated cases. Involve ITU early. Fever, Chills, Cough (new or worsening), headache, Sore throat, Myalgia, Coryza. Symptoms may be atypical e. g. diarrhoea, absence of cough, especially in immunocompramised hosts. Anti-viral therapy- Indications, dosage as per BNF latest version (cf NICE guidelines) High risk groups: Chronic heart disease, Chronic renal disease, Chronic liver disease, Chronic respiratory disease, Immunocompramised (e. g. Recent chemo, organ transplant, cytotoxic agents, steroids), diabetes, Patients >65 yrs of age, Pregnancy, patients with chronic neurological conditions Admission criteria: a) For Influenza - CURB-65 >2; OR Bilateral new chest signs / CXR Infiltrates; OR Sp. O 2 <92% b) For co-morbid conditions – based on best practice guidelines for individual conditions e. g. COPD, CCF. Information leaflet, GP consultation if not improving, any high-risk (immunocompramised) contacts at home? Trust’s Infection control policy. Prioritisation may be required if single rooms are unavailable. Aerosol generating procedures – Suctioning, Endotracheal intubation, Bronchoscopy, CPR etc. Respiratory physician/ Intensivist/ID Physician/ Microbiologist/ Virologist. NBT guidelines for Influenza (2010/2011) draft version 30/11/2010
- Slides: 1