National Prescribing Indicators 2017 2018 National Prescribing Indicators

National Prescribing Indicators 2017– 2018

National Prescribing Indicators (NPIs) development process Developed by the All Wales Prescribing Advisory Group (AWPAG): • July 2016: Task and Finish Group review and develop NPIs. • September 2016: Document discussed at AWPAG. • November 2016: Consultation with industry and stakeholders. • February 2017: Final document endorsed by the All Wales Medicines Strategy Group (AWMSG).

Prescribing measures – volume measures Items • • Single item prescribed by a prescriber on a prescription form. Number of items is a measure of how often a prescriber has decided to write a prescription. For vaccines and acute treatment such as antibiotics it can be used as a volume measure. However, a single item can be any quantity or duration (e. g. 1 item = lansoprazole 15 mg od 28 tablets). Defined daily doses (DDDs) • • • Developed and maintained by WHO based on international prescribing habits. Each medicine is given a value, within its recognised dosage range, that represents the assumed average maintenance dose per day when used for its main indication in adults (DDD lansoprazole = 30 mg). Unit of measurement – not a recommended dose and may not be a real dose. DDD of one medicine is assumed to be functionally equivalent to DDD of any other medicine used for a similar indication; therefore the number of DDDs for two or more such medicines can be added together. Average daily quantities (ADQs) • • • Work undertaken in England showed that prescribing in primary care can differ from the international standard. Measure of prescribing volume that accurately reflects primary care prescribing behaviour in England. Assumed average maintenance dose/day for a medicine used for its main indication in adults. Not a recommended dose, but an analytical unit to compare prescribing activity of primary care practitioners (ADQ lansoprazole = 20 mg). Many ADQs are the same as the corresponding DDD; however, values may differ e. g. when DDD is influenced by use of higher doses in hospital setting.

Prescribing measures – denominators To allow comparison between health boards, clusters and practices of different sizes, there needs to be a way of weighting prescribing data. • • • Patients - Data can be presented per 1, 000 patients. - Only useful if monitoring something that is not influenced by age and gender. Prescribing units (PUs) - Introduced in 1983 to take into account the greater need of the elderly population. - Age < 65 years weighted as 1; age 65 and over weighted as 3. Specific therapeutic group age-sex related prescribing units (STAR-PUs) - Introduced in England in 1995. - Designed to weight individual health board or practice populations based on the age and sex distribution of their practice, for specific therapeutic group for which a particular medicine/group of medicines is prescribed. - Reviewed regularly (most recently 2013) to take into account changes in prescribing practice: some are cost based, some item based, and ADQ based prescribing units now being introduced. Analysis has been undertaken to ensure correlation between PUs and STAR-PUs to determine that these measures are relevant to the Welsh population. Advantage that comparison can also be undertaken with English Clinical Commissioning Groups (CCGs).

Primary Care National Prescribing Indicators (NPIs)
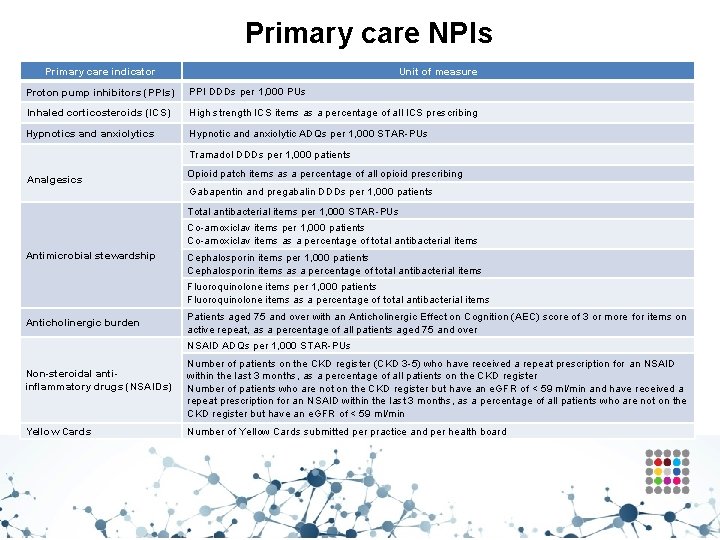
Primary care NPIs Primary care indicator Unit of measure Proton pump inhibitors (PPIs) PPI DDDs per 1, 000 PUs Inhaled corticosteroids (ICS) High strength ICS items as a percentage of all ICS prescribing Hypnotics and anxiolytics Hypnotic and anxiolytic ADQs per 1, 000 STAR-PUs Tramadol DDDs per 1, 000 patients Analgesics Opioid patch items as a percentage of all opioid prescribing Gabapentin and pregabalin DDDs per 1, 000 patients Total antibacterial items per 1, 000 STAR-PUs Co-amoxiclav items per 1, 000 patients Co-amoxiclav items as a percentage of total antibacterial items Antimicrobial stewardship Cephalosporin items per 1, 000 patients Cephalosporin items as a percentage of total antibacterial items Fluoroquinolone items per 1, 000 patients Fluoroquinolone items as a percentage of total antibacterial items Anticholinergic burden Patients aged 75 and over with an Anticholinergic Effect on Cognition (AEC) score of 3 or more for items on active repeat, as a percentage of all patients aged 75 and over NSAID ADQs per 1, 000 STAR-PUs Non-steroidal antiinflammatory drugs (NSAIDs) Yellow Cards Number of patients on the CKD register (CKD 3 -5) who have received a repeat prescription for an NSAID within the last 3 months, as a percentage of all patients on the CKD register Number of patients who are not on the CKD register but have an e. GFR of < 59 ml/min and have received a repeat prescription for an NSAID within the last 3 months, as a percentage of all patients who are not on the CKD register but have an e. GFR of < 59 ml/min Number of Yellow Cards submitted per practice and per health board

Proton pump inhibitors (PPIs) • PPI use continues to increase across Wales at a rate of almost 4% per year. • This NPI aims to encourage a reduction in PPI prescribing due to safety concerns regarding long-term use e. g. – Clostridium difficile infection, – Increased risk of bone fractures, – Increased risk of mortality in older people. • People with dyspepsia should initially be offered lifestyle advice and medications should be reviewed for possible causes of dyspepsia. • If medication is required, first line treatment should be with an alginate. • PPIs should only be considered for short courses (4 weeks) where needed. • If symptoms continue or recur, a PPI can be continued at the lowest possible dose or on an ‘as required’ basis. • Offer annual review to patients receiving PPIs and step down from treatment doses where appropriate. • Taper the dose of PPIs in patients who have been taking them for a long time to reduce the risk of rebound hypersecretion.
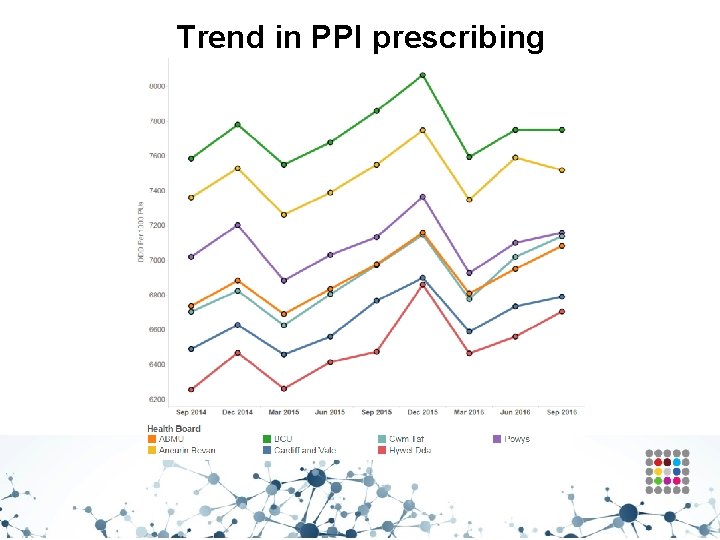
Trend in PPI prescribing
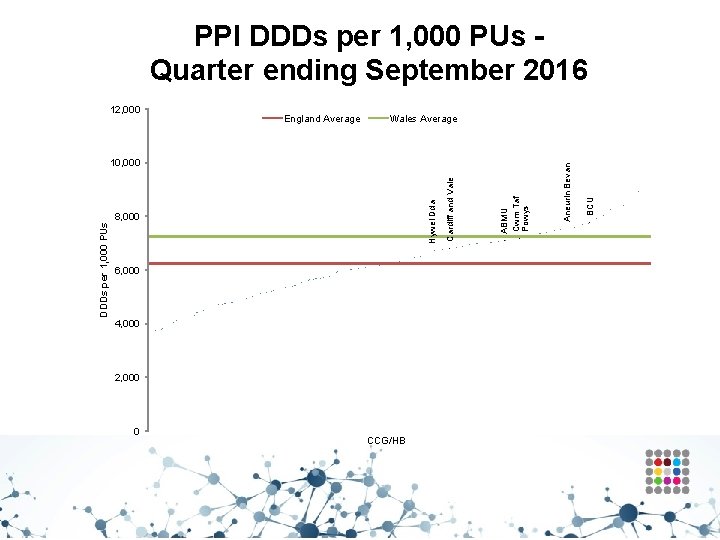
PPI DDDs per 1, 000 PUs Quarter ending September 2016 Wales Average 6, 000 4, 000 2, 000 0 CCG/HB ABMU Cwm Taf Powys 8, 000 Cardiff and Vale Hywel Dda DDDs per 1, 000 PUs 10, 000 BCU England Average Aneurin Bevan 12, 000

Inhaled corticosteroids (ICS) • Aims to encourage the routine review of ICS in people with asthma, particularly those on high doses, encouraging step down of the dose when clinically appropriate. • ICS (particularly at high doses) are associated with a number of side effects including adrenal suppression, growth failure, decrease in bone mineral density, cataracts and glaucoma. • To minimise side effects, the BTS/SIGN British guideline on the management of asthma recommends: - ICS should be titrated to the lowest dose at which effective control of asthma is maintained. - ICS dose reduction should be considered every three months, decreasing the dose by approximately 25– 50% each time.
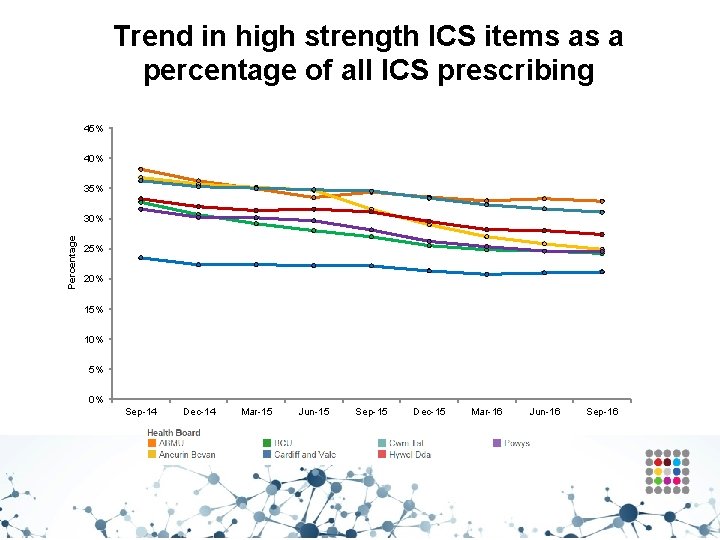
Trend in high strength ICS items as a percentage of all ICS prescribing 45% 40% 35% Percentage 30% 25% 20% 15% 10% 5% 0% Sep-14 Dec-14 Mar-15 Jun-15 Sep-15 Dec-15 Mar-16 Jun-16 Sep-16
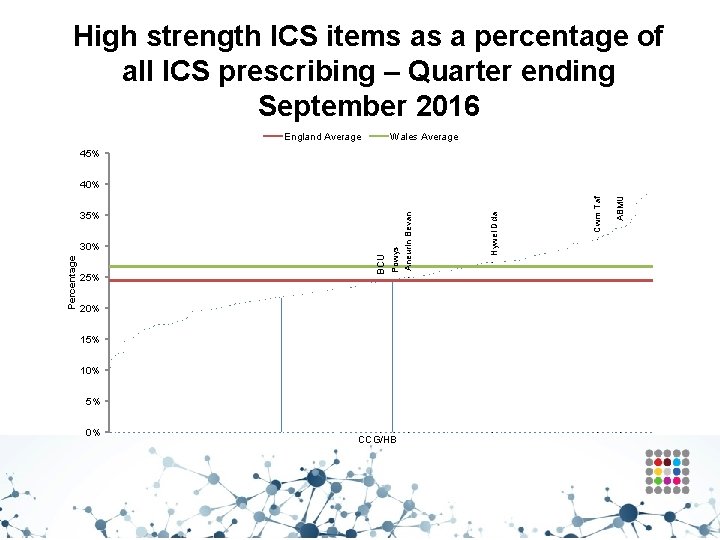
High strength ICS items as a percentage of all ICS prescribing – Quarter ending September 2016 England Average Wales Average 45% 25% BCU Percentage 30% 20% 15% 10% 5% 0% CCG/HB ABMU Cwm Taf Hywel Dda 35% Powys Aneurin Bevan 40%

Hypnotics and anxiolytics • Aims to encourage a reduction in the inappropriate prescribing of hypnotics and anxiolytics in Wales. • There is a high level of prescribing within Wales, in comparison to England. • Hypnotics and anxiolytics are known to significantly increase the risk of falls. • Hypnotics should only be considered after non-drug therapies have been explored, and should be used at the lowest dose possible, for the shortest duration possible and for no more than 4 weeks. • Benzodiazepines should not be offered for the treatment of GAD, except as a short-term measure during crises. • AWMSG Material to Support Appropriate Prescribing of Hypnotics and Anxiolytics provides: - examples of practice protocols to allow clinicians to agree a consistent approach for the prescribing and review of hypnotics and anxiolytics. - materials to support the review and discontinuation of hypnotic and anxiolytic treatment.
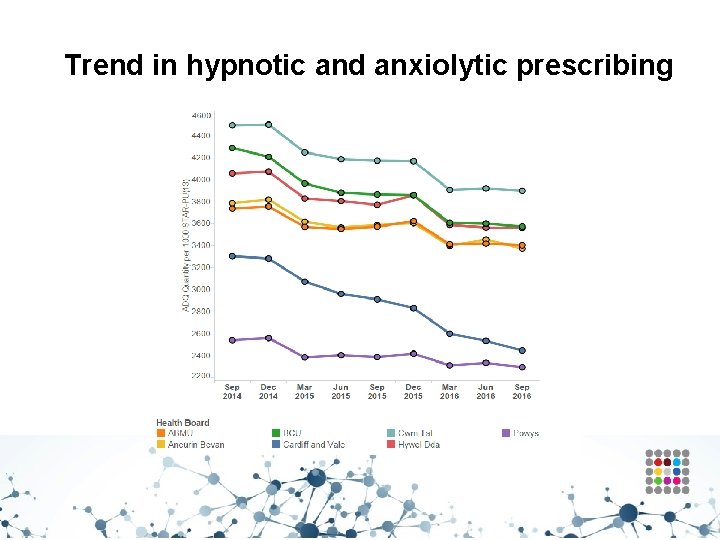
Trend in hypnotic and anxiolytic prescribing
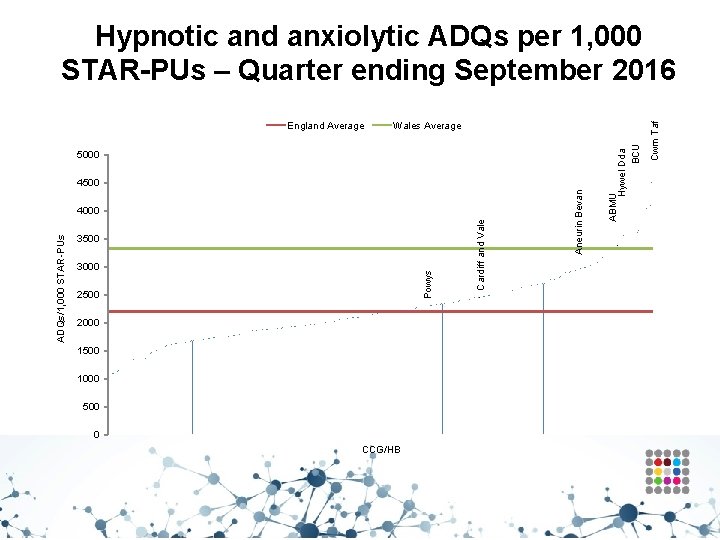
Wales Average 5000 3000 2500 2000 1500 1000 500 0 CCG/HB Cardiff and Vale 3500 Powys ADQs/1, 000 STAR-PUs 4000 Aneurin Bevan 4500 ABMU Hywel Dda BCU England Average Cwm Taf Hypnotic and anxiolytic ADQs per 1, 000 STAR-PUs – Quarter ending September 2016

Analgesics – Tramadol • Aims to encourage the appropriate use and review of tramadol, minimising the potential for diversion and misuse. • There are concerns regarding abuse, dependence and deaths involving tramadol. • Side effects include hallucinations, confusion and convulsions. Rare cases of dependence and withdrawal symptoms have been reported with tramadol at therapeutic doses. • Tramadol should be used with caution in patients taking concomitant medicines that can lower the seizure threshold, such as TCAs and SSRIs. • Where appropriate, consider stepping down or stopping, reducing the dose slowly to minimise the risk of withdrawal symptoms and/or adverse reactions.
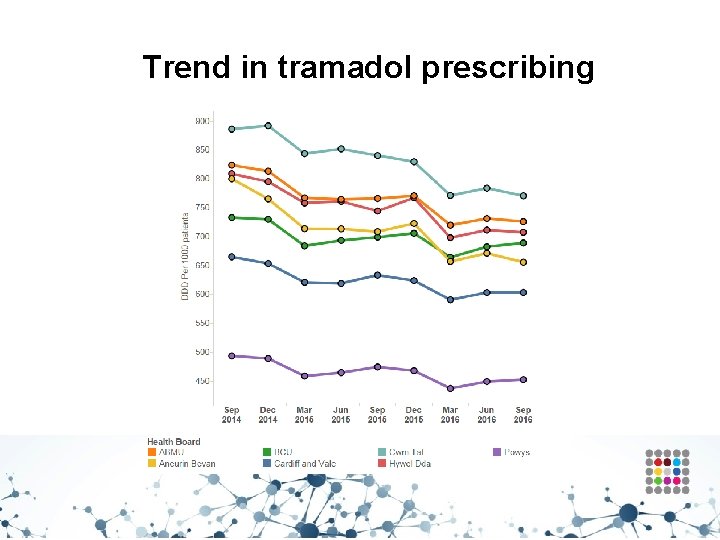
Trend in tramadol prescribing
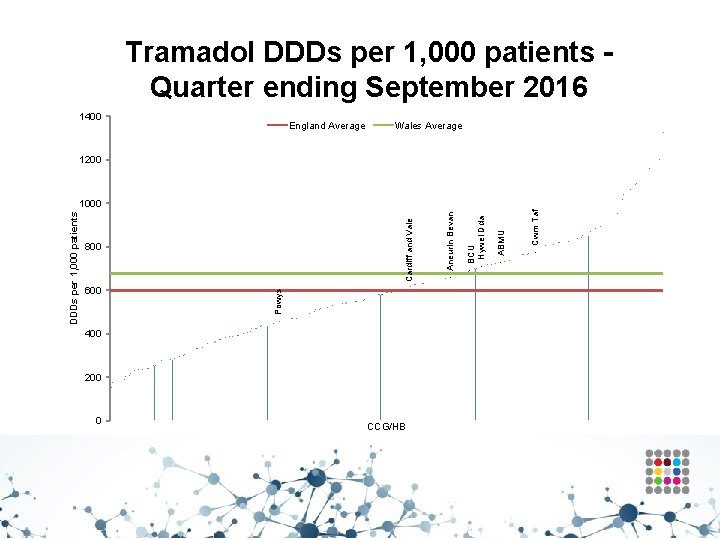
Tramadol DDDs per 1, 000 patients Quarter ending September 2016 1400 England Average Wales Average 1200 600 400 200 0 CCG/HB Cwm Taf ABMU BCU Hywel Dda Aneurin Bevan Cardiff and Vale 800 Powys DDDs per 1, 000 patients 1000

Analgesics – Opioid patches • Aims to encourage the appropriate use and review of opioid patches. • Fentanyl patches have been associated with a number of lifethreatening reactions and fatalities occurring as a result of inappropriate strength of fentanyl prescribed in opioid naive patients. • Fentanyl and buprenorphine patches are not suitable for acute pain, or for patients whose analgesic requirements are changing rapidly. • Reserve the use of opioid patches for patients in whom oral opioids are unsuitable and whose analgesic requirements are stable. • Fentanyl patches should only be used in patients who have previously tolerated opioids because of the risk of significant respiratory depression in opioid naive patients. • Ensure the initial dose of opioid patch is based on a patient’s opioid history.
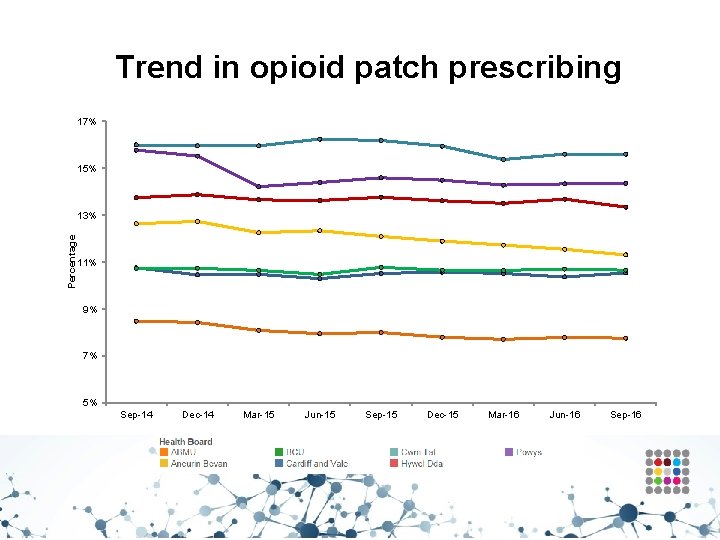
Trend in opioid patch prescribing 17% 15% Percentage 13% 11% 9% 7% 5% Sep-14 Dec-14 Mar-15 Jun-15 Sep-15 Dec-15 Mar-16 Jun-16 Sep-16
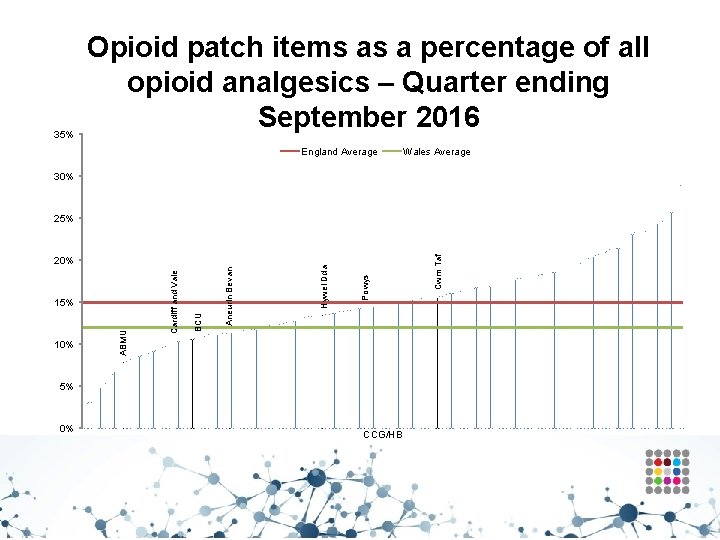
35% Opioid patch items as a percentage of all opioid analgesics – Quarter ending September 2016 England Average Wales Average 30% 10% 5% 0% CCG/HB Cwm Taf Powys Aneurin Bevan BCU ABMU 15% Cardiff and Vale 20% Hywel Dda 25%

Analgesics – Gabapentin and pregabalin • • Aims to encourage the appropriate use and review of gabapentin and pregabalin, minimising the potential for diversion and misuse. The number of deaths involving gabapentin and pregabalin is increasing, from 48 deaths in 2013 to 137 deaths in 2015. If the patient has not shown sufficient benefit within eight weeks of reaching the maximum tolerated dose, gabapentin/ pregabalin should be gradually reduced over a minimum of one week and then stopped. Caution should be exercised in prescribing pregabalin for patients with a history of substance abuse.
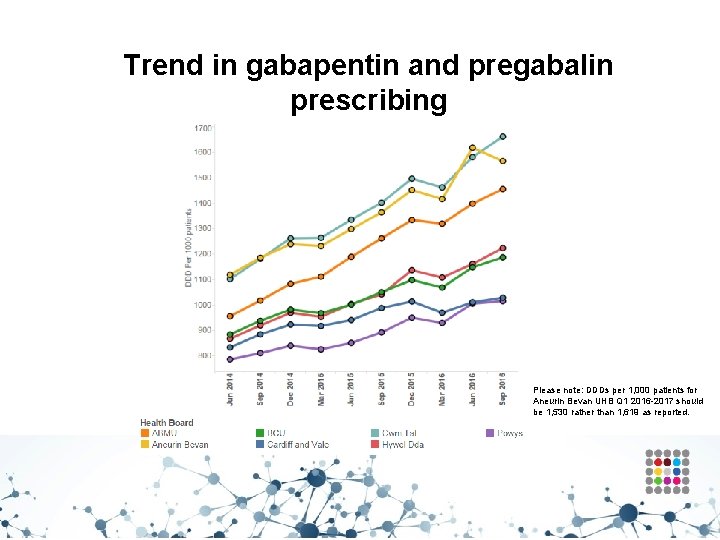
Trend in gabapentin and pregabalin prescribing Please note: DDDs per 1, 000 patients for Aneurin Bevan UHB Q 1 2016 -2017 should be 1, 530 rather than 1, 619 as reported.
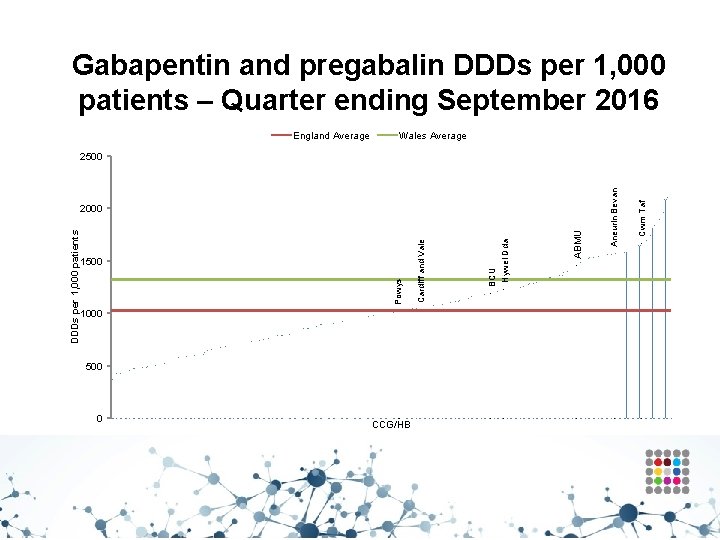
Gabapentin and pregabalin DDDs per 1, 000 patients – Quarter ending September 2016 England Average Wales Average 1000 500 0 CCG/HB Cwm Taf ABMU BCU Hywel Dda Cardiff and Vale 1500 Powys DDDs per 1, 000 patients 2000 Aneurin Bevan 2500

Antimicrobial Stewardship • • • Aims to encourage the appropriate prescribing of antibiotics. Overprescribing of antibiotics leads to resistance. The use of simple generic antibiotics and the avoidance of broad-spectrum antibiotics preserve these from resistance and reduce the risk of C. difficile, MRSA and resistant UTIs. If there is evidence of bacterial infection, prescribe according to national or local guidelines. Where an antibiotic is indicated, prescribe the shortest effective course at the most appropriate dose. Document the clinical diagnosis with the reason for prescribing, or not prescribing, an antimicrobial.
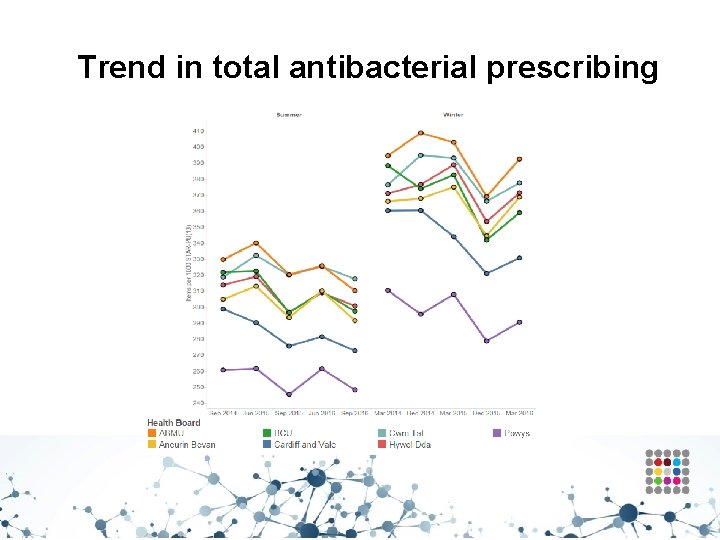
Trend in total antibacterial prescribing
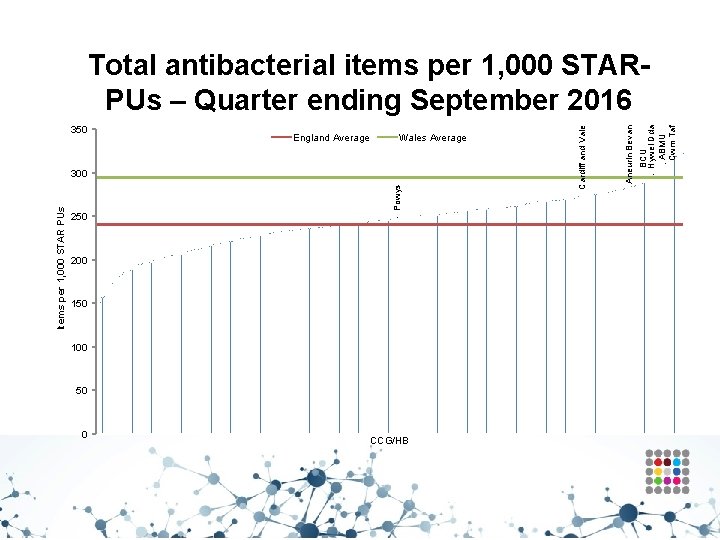
Wales Average Powys Items per 1, 000 STAR PUs 300 250 200 150 100 50 0 CCG/HB BCU Hywel Dda ABMU Cwm Taf England Average Aneurin Bevan 350 Cardiff and Vale Total antibacterial items per 1, 000 STARPUs – Quarter ending September 2016
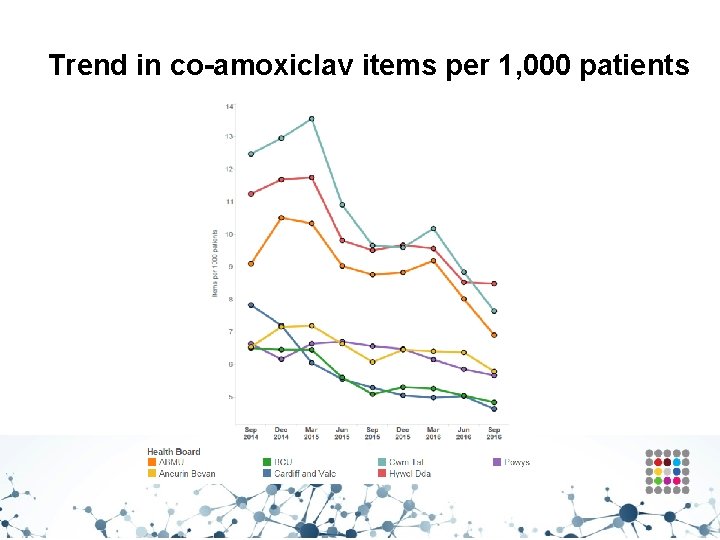
Trend in co-amoxiclav items per 1, 000 patients
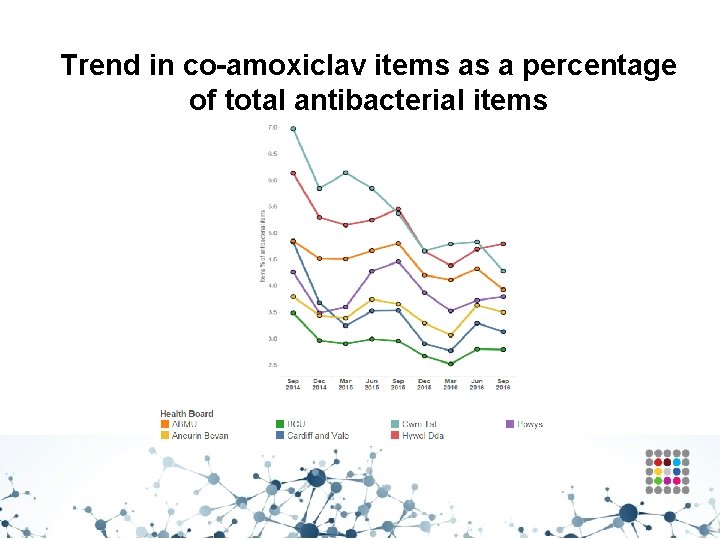
Trend in co-amoxiclav items as a percentage of total antibacterial items
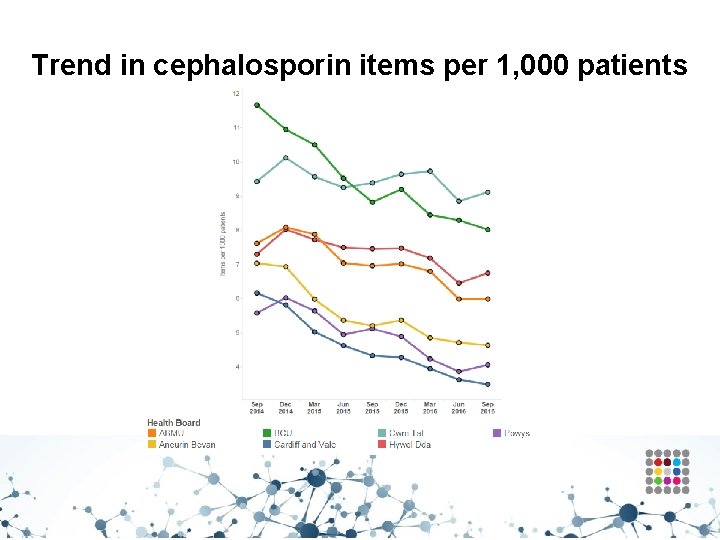
Trend in cephalosporin items per 1, 000 patients
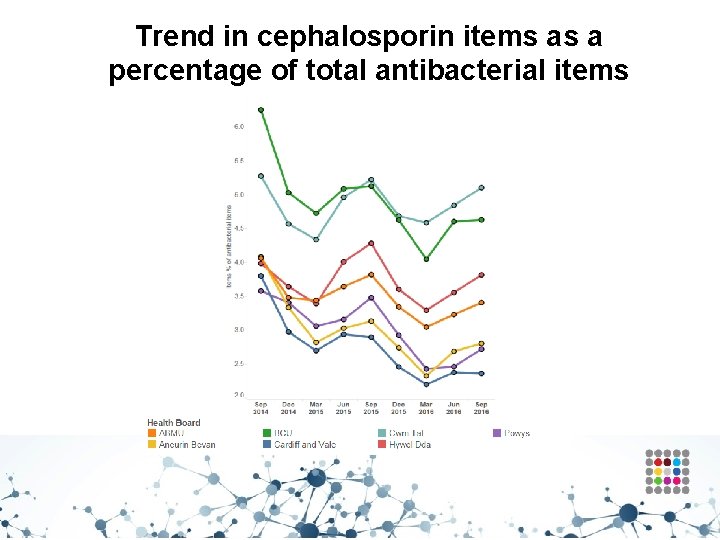
Trend in cephalosporin items as a percentage of total antibacterial items
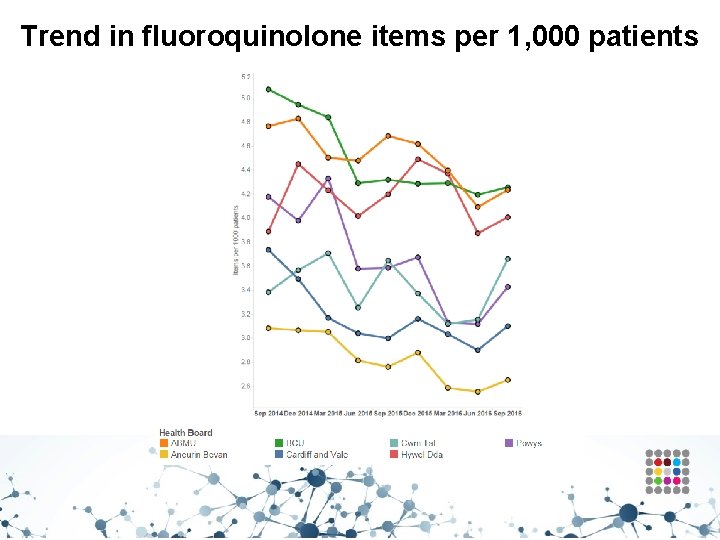
Trend in fluoroquinolone items per 1, 000 patients
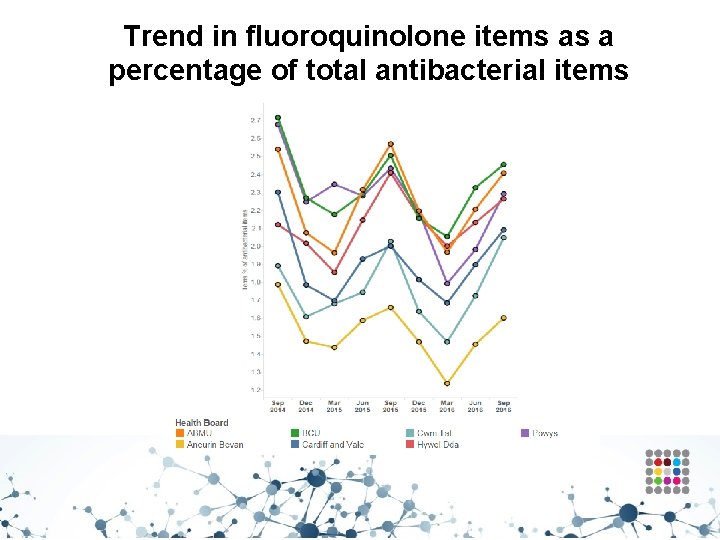
Trend in fluoroquinolone items as a percentage of total antibacterial items

Anticholinergic Burden • • • Aims to encourage a review of patients with an Anticholinergic Effect on Cognition (AEC) score of 3 or more, to reduce anticholinergic use where appropriate. An increasing number of studies report that medicines with anticholinergic effects are associated with an increased risk of cognitive impairment, dementia and falls in older people. Research suggests a link to increased mortality with the number and potency of anticholinergic agents prescribed. Many medicines commonly prescribed to older people are not routinely recognised as having anticholinergic activity, and are prescribed based on their anticipated therapeutic benefits, overlooking the risk of cumulative burden. During medication review, consider anticholinergic burden with the aim of avoiding, reducing doses and deprescribing medicine with anticholinergic activity, where clinically possible.
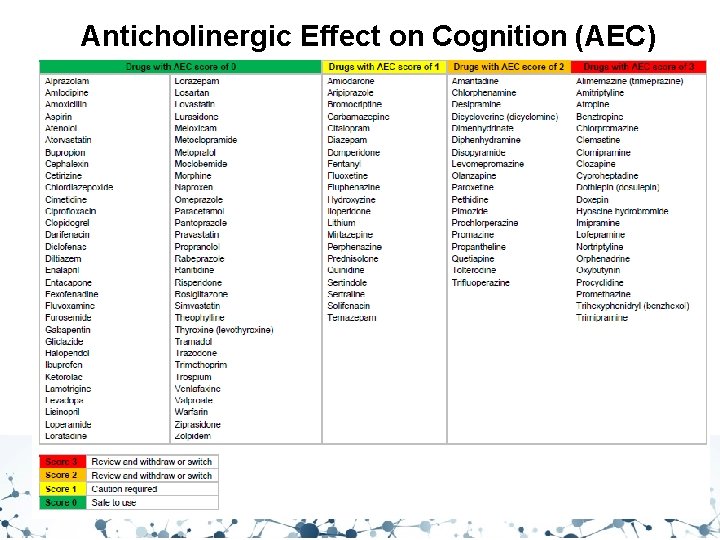
Anticholinergic Effect on Cognition (AEC)
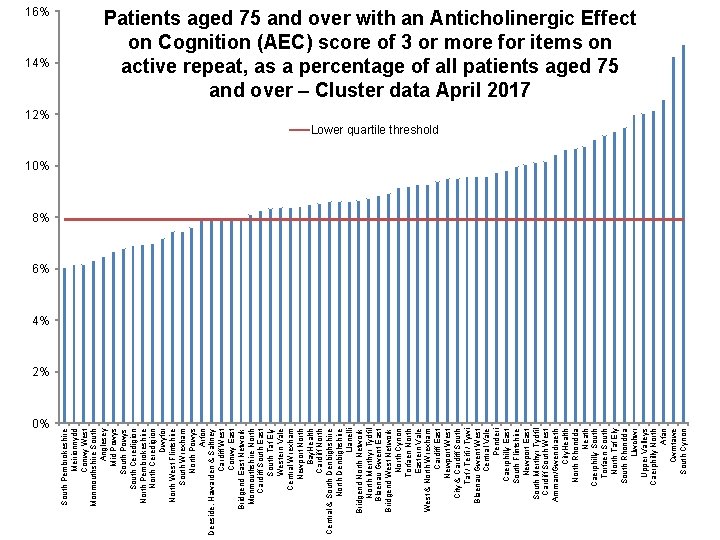
14% 0% South Pembrokeshire Meirionnydd Conwy West Monmouthshire South Anglesey Mid Powys South Ceredigion North Pembrokeshire North Ceredigion Dwyfor North West Flintshire South Wrexham North Powys Arfon Deeside, Hawarden & Saltney Cardiff West Conwy East Bridgend East Network Monmouthshire North Cardiff South East South Taf Ely Western Vale Central Wrexham Newport North Bay. Health Cardiff North Central & South Denbighshire North Denbighshire Llanelli Bridgend North Network North Merthyr Tydfil Blaenau Gwent East Bridgend West Network North Cynon Torfaen North Eastern Vale West & North Wrexham Cardiff East Newport West City & Cardiff South Taf / Teifi / Tywi Blaenau Gwent West Central Vale Penderi Caerphilly East South Flintshire Newport East South Merthyr Tydfil Cardiff South West Amman/Gwendraeth City. Health North Rhondda Neath Caerphilly South Torfaen South North Taf Ely South Rhondda Llwchwr Upper Valleys Caerphilly North Afan Cwmtawe South Cynon 16% Patients aged 75 and over with an Anticholinergic Effect on Cognition (AEC) score of 3 or more for items on active repeat, as a percentage of all patients aged 75 and over – Cluster data April 2017 12% Lower quartile threshold 10% 8% 6% 4% 2%

NSAIDs – Overall use • • • Aims to ensure that the risks associated with NSAIDs are minimised by appropriate use. There are long-standing and well recognised safety concerns with all NSAIDs. If an oral NSAID is indicated, prescribing should be based on the safety profiles of individual NSAIDs and on an individual patient risk profile. Patients should be prescribed the lowest effective dose, for the shortest duration necessary to control symptoms, in order to minimise adverse effects. A patient's need for symptomatic relief and response to treatment should be re-evaluated periodically.
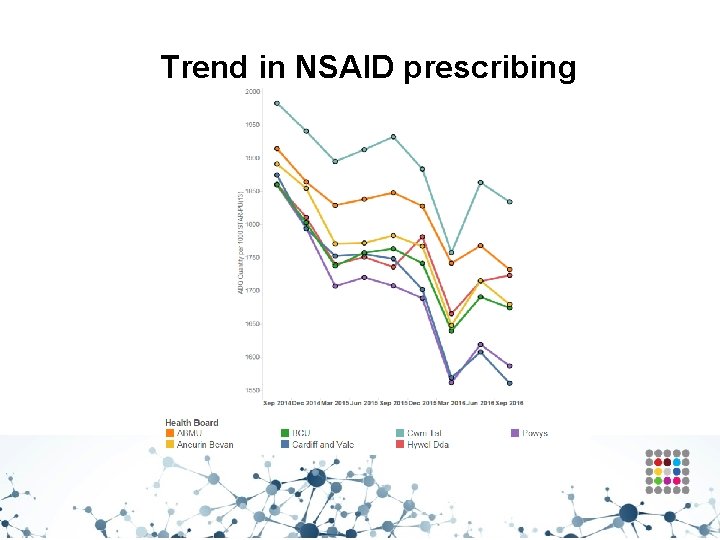
Trend in NSAID prescribing
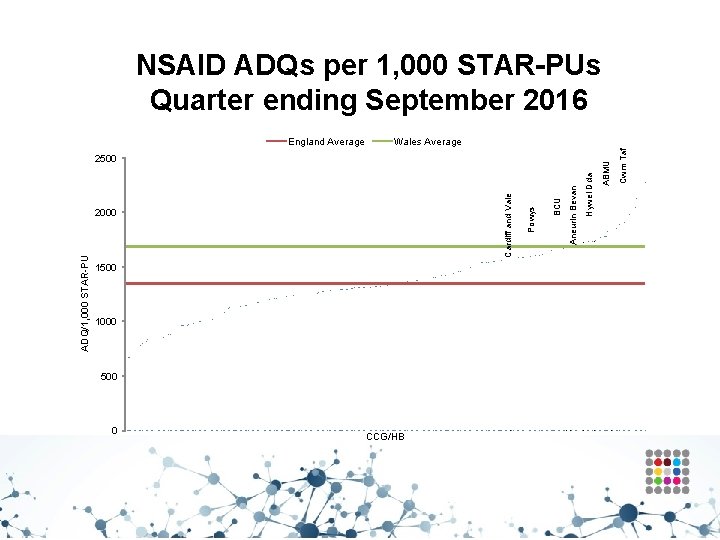
NSAID ADQs per 1, 000 STAR-PUs Quarter ending September 2016 ADQ/1, 000 STAR-PU 1500 1000 500 0 CCG/HB Hywel Dda Aneurin Bevan BCU 2000 Powys Cardiff and Vale 2500 Cwm Taf Wales Average ABMU England Average

NSAIDs and CKD • • Aims to encourage appropriate use and review of NSAIDs for patients with CKD. The chronic use of NSAIDs in patients with CKD may be associated with disease progression. Acute use of NSAIDs in CKD is associated with a reversible decrease in GFR. For patients with CKD, regular review of the ongoing need for an NSAID and reassessment of the risk versus benefit is appropriate.
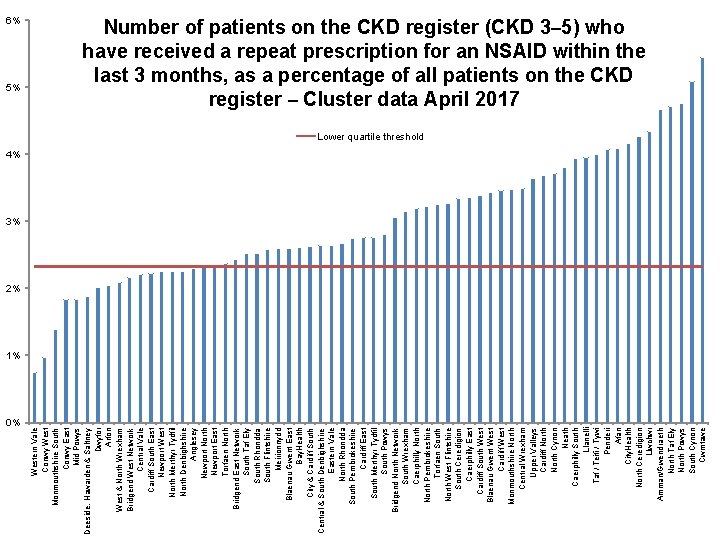
5% 0% Western Vale Conwy West Monmouthshire South Conwy East Mid Powys Deeside, Hawarden & Saltney Dwyfor Arfon West & North Wrexham Bridgend West Network Central Vale Cardiff South East Newport West North Merthyr Tydfil North Denbighshire Anglesey Newport North Newport East Torfaen North Bridgend East Network South Taf Ely South Rhondda South Flintshire Meirionnydd Blaenau Gwent East Bay. Health City & Cardiff South Central & South Denbighshire Eastern Vale North Rhondda South Pembrokeshire Cardiff East South Merthyr Tydfil South Powys Bridgend North Network South Wrexham Caerphilly North Pembrokeshire Torfaen South North West Flintshire South Ceredigion Caerphilly East Cardiff South West Blaenau Gwent West Cardiff West Monmouthshire North Central Wrexham Upper Valleys Cardiff North Cynon Neath Caerphilly South Llanelli Taf / Teifi / Tywi Penderi Afan City. Health North Ceredigion Llwchwr Amman/Gwendraeth North Taf Ely North Powys South Cynon Cwmtawe 6% Number of patients on the CKD register (CKD 3– 5) who have received a repeat prescription for an NSAID within the last 3 months, as a percentage of all patients on the CKD register – Cluster data April 2017 Lower quartile threshold 4% 3% 2% 1%
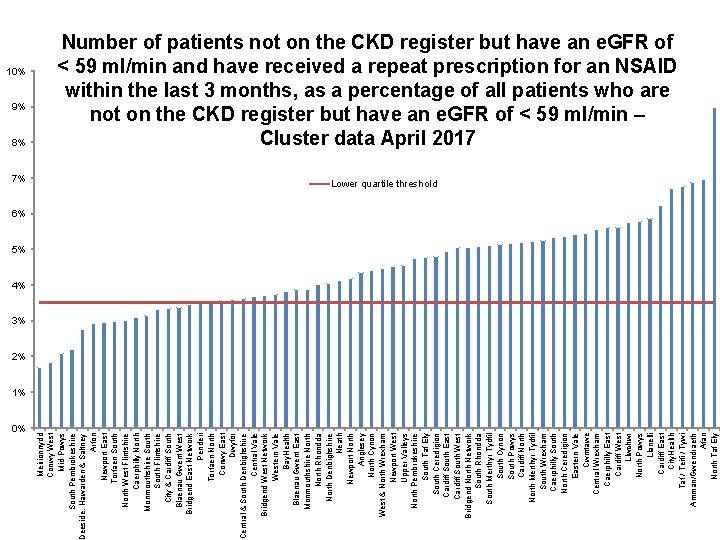
9% 8% 7% 0% Meirionnydd Conwy West Mid Powys South Pembrokeshire eeside, Hawarden & Saltney Arfon Newport East Torfaen South North West Flintshire Caerphilly North Monmouthshire South Flintshire City & Cardiff South Blaenau Gwent West Bridgend East Network Penderi Torfaen North Conwy East Dwyfor Central & South Denbighshire Central Vale Bridgend West Network Western Vale Bay. Health Blaenau Gwent East Monmouthshire North Rhondda North Denbighshire Neath Newport North Anglesey North Cynon West & North Wrexham Newport West Upper Valleys North Pembrokeshire South Taf Ely South Ceredigion Cardiff South East Cardiff South West Bridgend North Network South Rhondda South Merthyr Tydfil South Cynon South Powys Cardiff North Merthyr Tydfil South Wrexham Caerphilly South North Ceredigion Eastern Vale Cwmtawe Central Wrexham Caerphilly East Cardiff West Llwchwr North Powys Llanelli Cardiff East City. Health Taf / Teifi / Tywi Amman/Gwendraeth Afan North Taf Ely 10% Number of patients not on the CKD register but have an e. GFR of < 59 ml/min and have received a repeat prescription for an NSAID within the last 3 months, as a percentage of all patients who are not on the CKD register but have an e. GFR of < 59 ml/min – Cluster data April 2017 Lower quartile threshold 6% 5% 4% 3% 2% 1%

Yellow Cards • • • Aims to encourage an increase in the number of Yellow Cards submitted by GP practices in Wales. ADRs are a significant clinical problem, increasing morbidity and mortality. The Yellow Card Scheme is vital in helping the MHRA monitor the safety of all healthcare products in the UK to ensure they are acceptably safe for those that use them. Yellow Card reporting supports the identification and collation of ADRs, which might not have been known about before. A strong safety culture requires good reporting of adverse events from all healthcare professionals and patients.
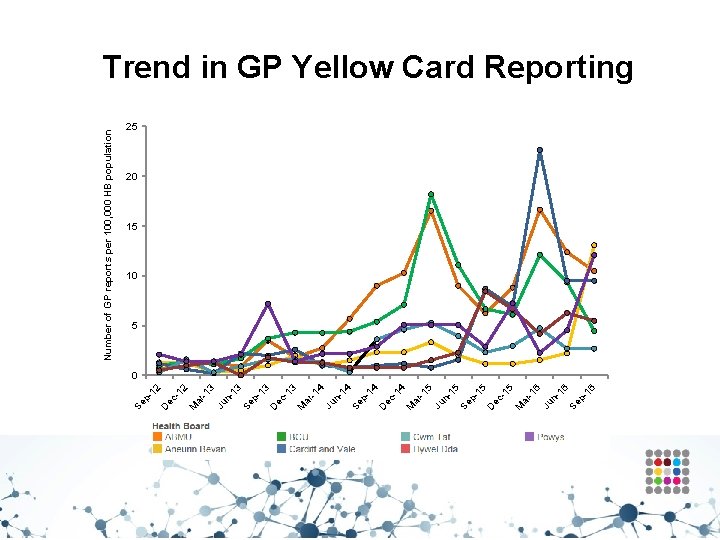
3 n 13 Se p 13 D ec -1 3 M ar -1 4 Ju n 14 Se p 14 D ec -1 4 M ar -1 5 Ju n 15 Se p 15 D ec -1 5 M ar -1 6 Ju n 16 Se p 16 Ju 12 12 -1 ar M ec - D p- Se Number of GP reports per 100, 000 HB population Trend in GP Yellow Card Reporting 25 20 15 10 5 0

Secondary Care National Prescribing Indicators (NPIs)

Secondary care NPIs Secondary care indicator Unit of measure Insulin prescribing Items/number of long-acting insulin analogues expressed as a percentage of total insulin prescribed within primary and secondary care. Prescribing of biosimilars Quantity of biosimilar medicines prescribed as a percentage of total ‘reference’ product plus biosimilar. Antibiotic surgical prophylaxis Proportion of elective colorectal patients receiving surgical prophylaxis for more than 24 hours.

Insulin prescribing • Aims to reduce prescribing of long-acting insulin analogues and to achieve prescribing levels below the Welsh average for prescribing within secondary care • There is an absence of evidence to suggest the superiority of the long-acting insulin analogues versus NPH insulin (Cochrane Centre/NICE, 2011) • NICE recommends NPH as first choice regimen before long -acting insulin analogues (CG 87, 2009; NG 28, 2015)
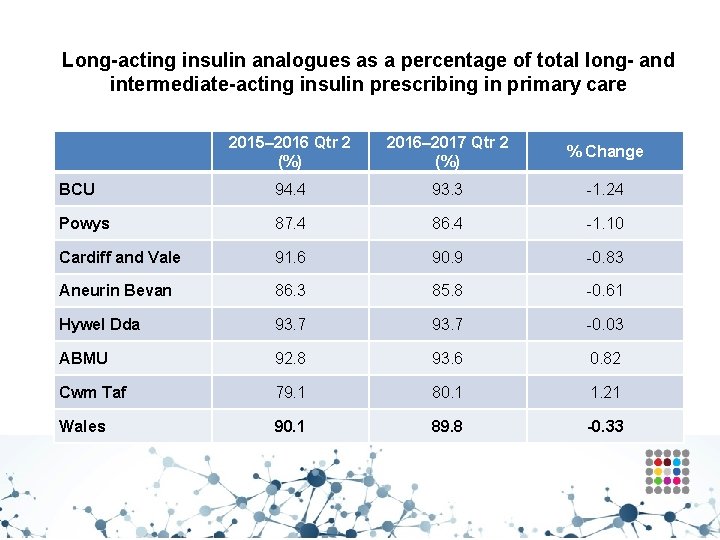
Long-acting insulin analogues as a percentage of total long- and intermediate-acting insulin prescribing in primary care 2015– 2016 Qtr 2 (%) 2016– 2017 Qtr 2 (%) % Change BCU 94. 4 93. 3 -1. 24 Powys 87. 4 86. 4 -1. 10 Cardiff and Vale 91. 6 90. 9 -0. 83 Aneurin Bevan 86. 3 85. 8 -0. 61 Hywel Dda 93. 7 -0. 03 ABMU 92. 8 93. 6 0. 82 Cwm Taf 79. 1 80. 1 1. 21 Wales 90. 1 89. 8 -0. 33
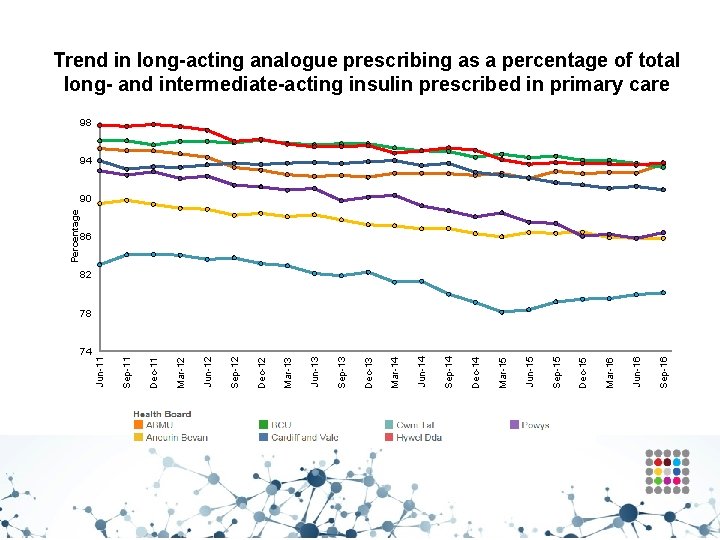
Trend in long-acting analogue prescribing as a percentage of total long- and intermediate-acting insulin prescribed in primary care 98 94 86 82 Sep-16 Jun-16 Mar-16 Dec-15 Sep-15 Jun-15 Mar-15 Dec-14 Sep-14 Jun-14 Mar-14 Dec-13 Sep-13 Jun-13 Mar-13 Dec-12 Sep-12 Jun-12 Mar-12 Dec-11 74 Sep-11 78 Jun-11 Percentage 90
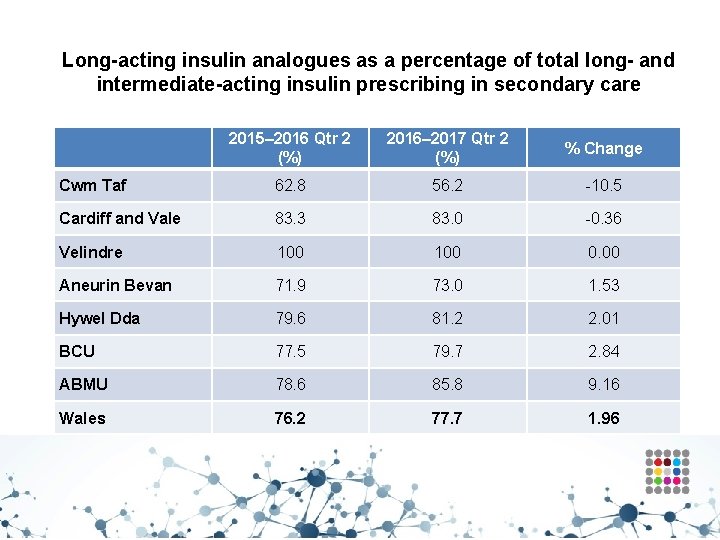
Long-acting insulin analogues as a percentage of total long- and intermediate-acting insulin prescribing in secondary care 2015– 2016 Qtr 2 (%) 2016– 2017 Qtr 2 (%) % Change Cwm Taf 62. 8 56. 2 -10. 5 Cardiff and Vale 83. 3 83. 0 -0. 36 Velindre 100 0. 00 Aneurin Bevan 71. 9 73. 0 1. 53 Hywel Dda 79. 6 81. 2 2. 01 BCU 77. 5 79. 7 2. 84 ABMU 78. 6 85. 8 9. 16 Wales 76. 2 77. 7 1. 96

Prescribing of biosimilars • Aim is to increase the appropriate use of biosimilar medicines in line with guidance and increase commercial competition. • A biosimilar medicine is “a biological medicine that is developed to be highly similar and clinically equivalent to an existing biological medicine”. • Biological medicines including all biosimilars must be prescribed by brand name. • Within the next five years a number of biological medicines will lose their patent protection thus increasing the potential opportunity of prescribing biosimilar medicines. • There a number of biosimilar medicines available within NHS Wales; those currently being monitored are filgrastim - Nivestim®, Zarzio®, infliximab - Inflectra® and insulin glargine – Abasaglar®

Prescribing of biosimilars – Filgrastim • Use of filgrastim biosimilars as a percentage of all filgrastim within NHS Wales for quarter ending September 2016 was 98. 8%. • When comparing to the equivalent quarter of 2015: - Within secondary care there was a decrease from 98. 98% to 98. 92%. - Within primary care there was an increase from 48. 0% to 90. 8%.
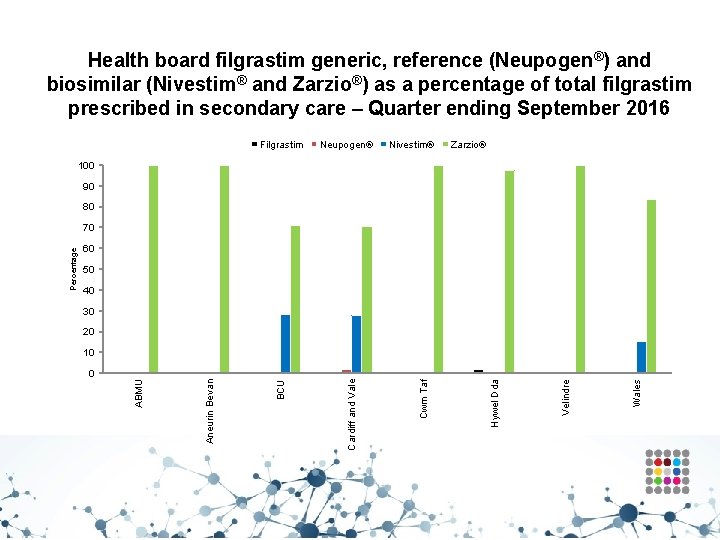
Health board filgrastim generic, reference (Neupogen®) and biosimilar (Nivestim® and Zarzio®) as a percentage of total filgrastim prescribed in secondary care – Quarter ending September 2016 Filgrastim Neupogen® Nivestim® Zarzio® 100 90 80 60 50 40 30 20 Wales Velindre Hywel Dda Cwm Taf Cardiff and Vale BCU 0 Aneurin Bevan 10 ABMU Percentage 70
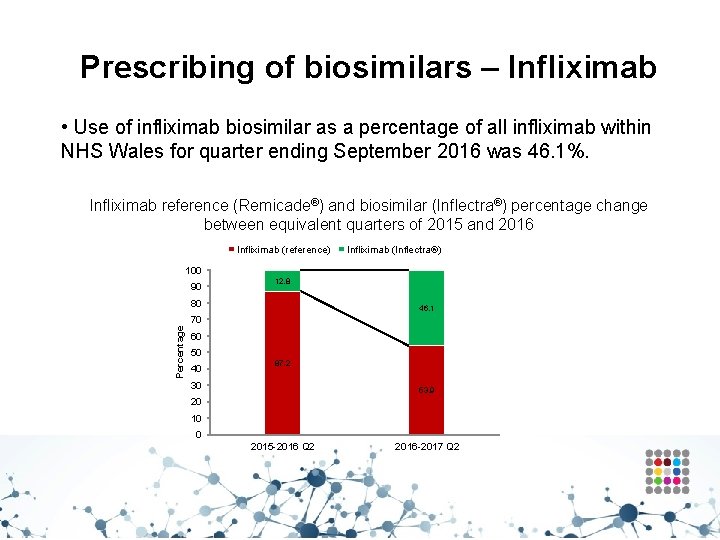
Prescribing of biosimilars – Infliximab • Use of infliximab biosimilar as a percentage of all infliximab within NHS Wales for quarter ending September 2016 was 46. 1%. Infliximab reference (Remicade®) and biosimilar (Inflectra®) percentage change between equivalent quarters of 2015 and 2016 Infliximab (reference) Infliximab (Inflectra®) 100 90 12. 8 80 46. 1 Percentage 70 60 50 40 87. 2 30 53. 9 20 10 0 2015 -2016 Q 2 2016 -2017 Q 2

Antibiotic prophylaxis for surgical patients • Aim is to encourage the appropriate prescribing of antibiotics by reducing the proportion of elective colorectal patients receiving surgical prophylaxis for more than 24 hours. • Antibiotic prophylaxis should be given to patients before: - Clean surgery involving the placement of a prosthesis or implant - Clean-contaminated surgery - Contaminated surgery • Antibiotic prophylaxis is not routinely recommended for clean non-prosthetic uncomplicated surgery • Single therapeutic dose of intravenous antibiotics should be used, unless: - Operation is longer than antibiotic half-life so a repeat dose is needed - Certain circumstances requiring a longer course up to 24 hours • Antibiotic choice should take into account: - Expected pathogens - Clostridium difficile risk - Local antimicrobial susceptibility and resistance information - Narrow versus broad spectrum - Cost
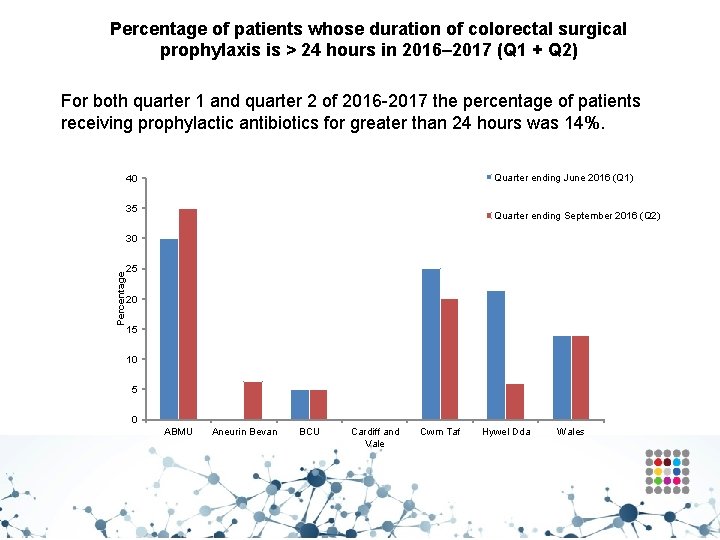
Percentage of patients whose duration of colorectal surgical prophylaxis is > 24 hours in 2016– 2017 (Q 1 + Q 2) For both quarter 1 and quarter 2 of 2016 -2017 the percentage of patients receiving prophylactic antibiotics for greater than 24 hours was 14%. Quarter ending June 2016 (Q 1) 40 35 Quarter ending September 2016 (Q 2) Percentage 30 25 20 15 10 5 0 ABMU Aneurin Bevan BCU Cardiff and Vale Cwm Taf Hywel Dda Wales

Thank you
- Slides: 57