National Prescribing Indicators 2016 2017 National Prescribing Indicators

National Prescribing Indicators 2016– 2017

National Prescribing Indicators (NPIs) development process Developed by the All Wales Prescribing Advisory Group (AWPAG): • July 2015: Task and Finish Group review and develop NPIs. • September 2015: Document discussed at AWPAG. • November 2015: Consultation with industry and stakeholders. • February 2016: Final document endorsed by the All Wales Medicines Strategy Group (AWMSG).

Prescribing measures – volume measures • Items – single item prescribed by a prescriber on a prescription form – – – • DDDs – defined daily doses – – • The number of items is a measure of how often a prescriber has decided to write a prescription. For vaccines and acute treatment such as antibiotics it can be used as a volume measure. However, a single item can be any quantity or duration (e. g. 1 item = lansoprazole 15 mg od 28 tablets). Developed and maintained by WHO based on international prescribing habits. Each medicine is given a value, within its recognised dosage range, that represents the assumed average maintenance dose per day when used for its main indication in adults (DDD lansoprazole = 30 mg). A DDD is a unit of measurement; it is not a recommended dose and may not be a real dose. A DDD of one medicine is assumed to be functionally equivalent to the DDD of any other medicine used for a similar indication; therefore the number of DDDs for two or more such medicines can be added together. ADQs – average daily quantities – – – Work undertaken in England showed that prescribing in primary care can differ from the international standard. ADQs provide a measure of prescribing volume that accurately reflects primary care prescribing behaviour in England. ADQs represent the assumed average maintenance dose/day for a medicine used for its main indication in adults. An ADQ is not a recommended dose, but an analytical unit to compare prescribing activity of primary care practitioners (ADQ lansoprazole = 20 mg). Many ADQs are the same as the corresponding DDD; however, the values may differ e. g. when a DDD value is influenced by use of higher doses in a hospital setting.

Prescribing measures – denominators To allow comparison between health boards, clusters and practices of different sizes, there needs to be a way of weighting prescribing data. • • • Patients – Data can be presented per 1, 000 patients. – Only useful if monitoring something that is not influenced by age and gender. PUs – Prescribing Units – Introduced in 1983 to take into account the greater need of the elderly population. – Age < 65 years weighted as 1; age 65 and over weighted as 3. STAR-PUs – Specific Therapeutic group Age-sex Related Prescribing Units – Introduced in England in 1995. – Designed to weight individual health board or practice populations based on the age and sex distribution of their practice, for specific therapeutic group for which a particular medicine/group of medicines is prescribed. – Reviewed regularly (most recently 2013) to take into account changes in prescribing practice: some are cost based, some item based, and ADQ based prescribing units now being introduced. • Analysis has been undertaken to ensure correlation between PUs and STAR-PUs to determine that these measures are relevant to the Welsh population. • Advantage that comparison can also be undertaken with English Clinical Commissioning Groups (CCGs).
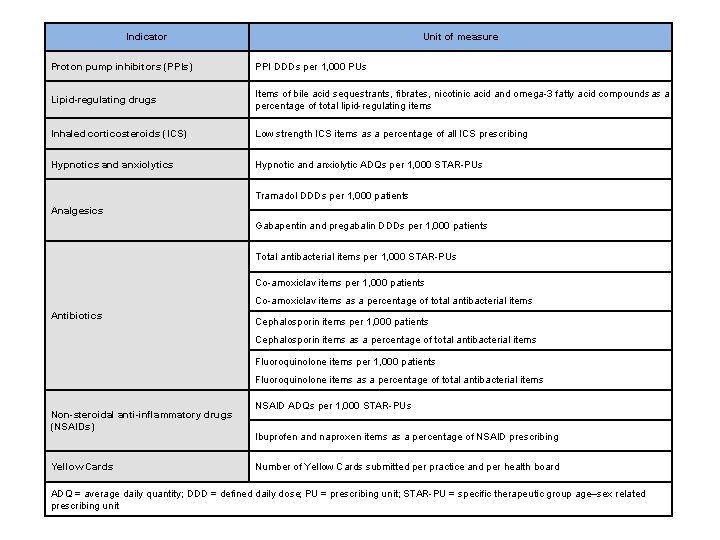
Indicator Unit of measure Proton pump inhibitors (PPIs) PPI DDDs per 1, 000 PUs Lipid-regulating drugs Items of bile acid sequestrants, fibrates, nicotinic acid and omega-3 fatty acid compounds as a percentage of total lipid-regulating items Inhaled corticosteroids (ICS) Low strength ICS items as a percentage of all ICS prescribing Hypnotics and anxiolytics Hypnotic and anxiolytic ADQs per 1, 000 STAR-PUs Tramadol DDDs per 1, 000 patients Analgesics Gabapentin and pregabalin DDDs per 1, 000 patients Total antibacterial items per 1, 000 STAR-PUs Co-amoxiclav items per 1, 000 patients Co-amoxiclav items as a percentage of total antibacterial items Antibiotics Cephalosporin items per 1, 000 patients Cephalosporin items as a percentage of total antibacterial items Fluoroquinolone items per 1, 000 patients Fluoroquinolone items as a percentage of total antibacterial items Non-steroidal anti-inflammatory drugs (NSAIDs) Yellow Cards NSAID ADQs per 1, 000 STAR-PUs Ibuprofen and naproxen items as a percentage of NSAID prescribing Number of Yellow Cards submitted per practice and per health board ADQ = average daily quantity; DDD = defined daily dose; PU = prescribing unit; STAR-PU = specific therapeutic group age–sex related prescribing unit
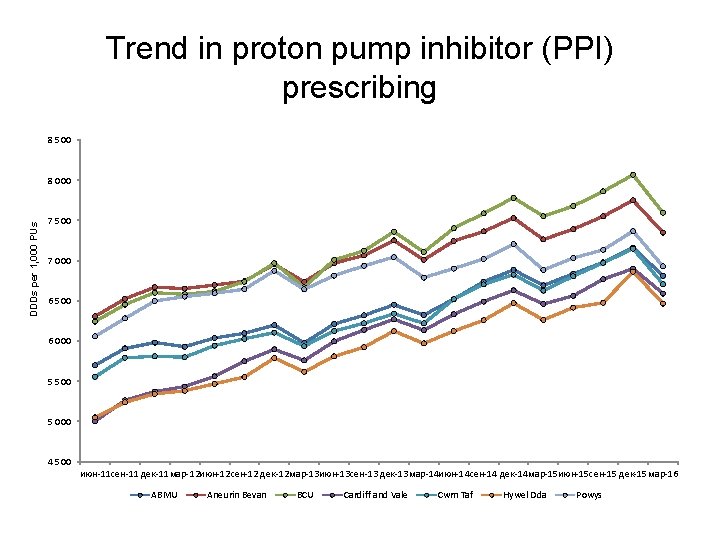
Trend in proton pump inhibitor (PPI) prescribing 8 500 DDDs per 1, 000 PUs 8 000 7 500 7 000 6 500 6 000 5 500 5 000 4 500 июн-11 сен-11 дек-11 мар-12 июн-12 сен-12 дек-12 мар-13 июн-13 сен-13 дек-13 мар-14 июн-14 сен-14 дек-14 мар-15 июн-15 сен-15 дек-15 мар-16 ABMU Aneurin Bevan BCU Cardiff and Vale Cwm Taf Hywel Dda Powys
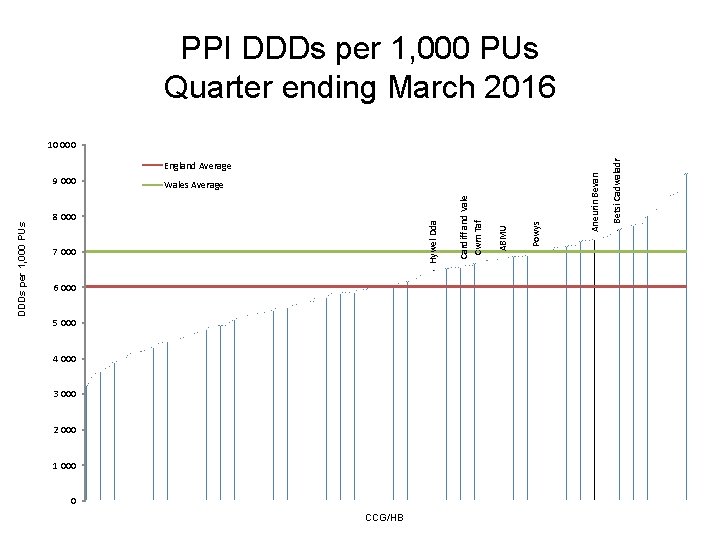
PPI DDDs per 1, 000 PUs Quarter ending March 2016 6 000 5 000 4 000 3 000 2 000 1 000 0 CCG/HB Powys ABMU 7 000 Cardiff and Vale Cwm Taf 8 000 Hywel Dda DDDs per 1, 000 PUs Wales Average Aneurin Bevan England Average 9 000 Betsi Cadwaladr 10 000

Proton pump inhibitors (PPIs) • PPI use continues to increase across Wales at a rate of 4% per year. • Aims to encourage a reduction in PPI prescribing due to potentially serious adverse effects linked to long-term use e. g. – Clostridium difficile infection, – Hospital- and community-acquired pneumonia, – Hypomagnesaemia, – Fractures of the hip, wrist and spine. • NICE CG 184 recommends offering people requiring long-term management of dyspepsia symptoms an annual review: – Review medicines which may cause dyspepsia (e. g. calcium channel blockers, nitrates, theophyllines, bisphonates, corticosteroids and NSAIDs). – Encourage people requiring long-term management of dyspepsia symptoms to reduce their use of prescribed medication stepwise: by using the lowest effective dose, by trying 'asneeded' use when appropriate, and by returning to self-treatment with antacid and/or alginate therapy. • Gastro-protection should be considered for people taking high-risk medicines e. g. NSAIDs in osteoarthritis and rheumatoid arthritis.
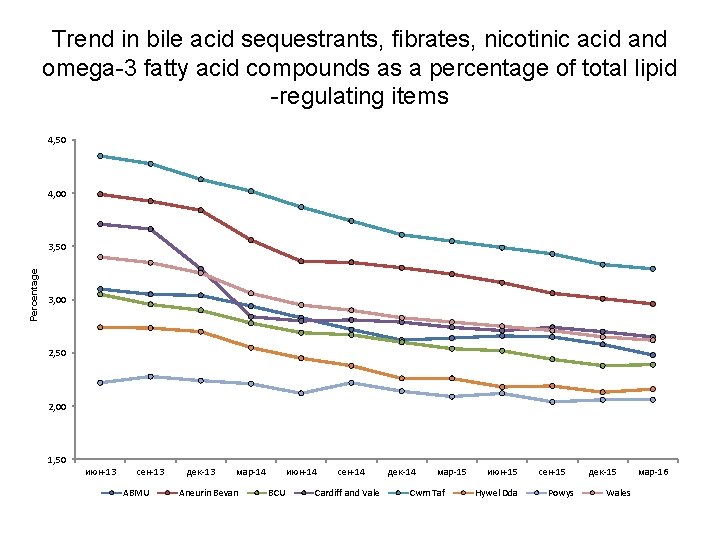
Trend in bile acid sequestrants, fibrates, nicotinic acid and omega-3 fatty acid compounds as a percentage of total lipid -regulating items 4, 50 4, 00 Percentage 3, 50 3, 00 2, 50 2, 00 1, 50 июн-13 сен-13 ABMU дек-13 мар-14 Aneurin Bevan июн-14 BCU сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 Wales мар-16
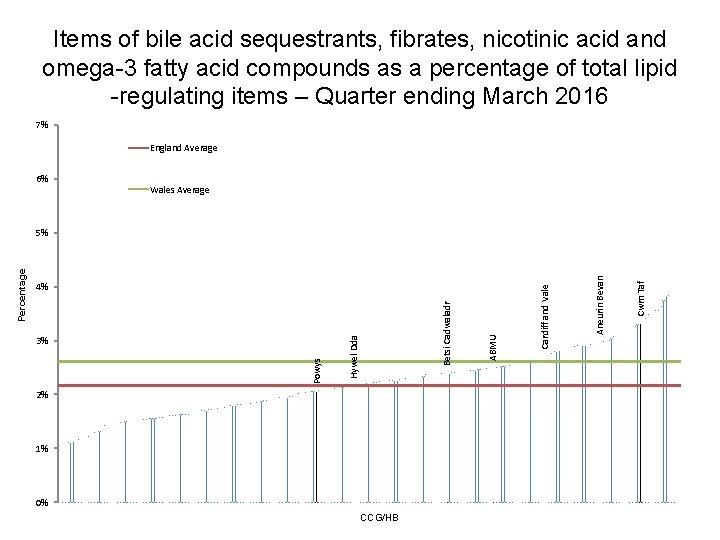
Items of bile acid sequestrants, fibrates, nicotinic acid and omega-3 fatty acid compounds as a percentage of total lipid -regulating items – Quarter ending March 2016 7% England Average 6% Wales Average 2% 1% 0% CCG/HB Cwm Taf Aneurin Bevan Cardiff and Vale ABMU Hywel Dda 3% Betsi Cadwaladr 4% Powys Percentage 5%

Lipid regulating drugs • Aims to encourage prescribers to review and, if appropriate, revise prescribing of the lipid-regulating medicines – bile acid sequestrants, fibrates, nicotinic acid and omega-3 fatty acid compounds – to ensure it is in line with NICE guidance. • NICE CG 181 was published in July 2014, and recommends against the routine prescribing of fibrates, and against offering nicotinic acid, bile acid sequestrants and omega-3 fatty acid compounds, for the prevention of cardiovascular disease in the following people, either as monotherapy, or in combination with a statin: • People who are being treated for primary prevention • People who are being treated for secondary prevention • People with chronic kidney disease (CKD) • People with Type 1 diabetes • People with Type 2 diabetes
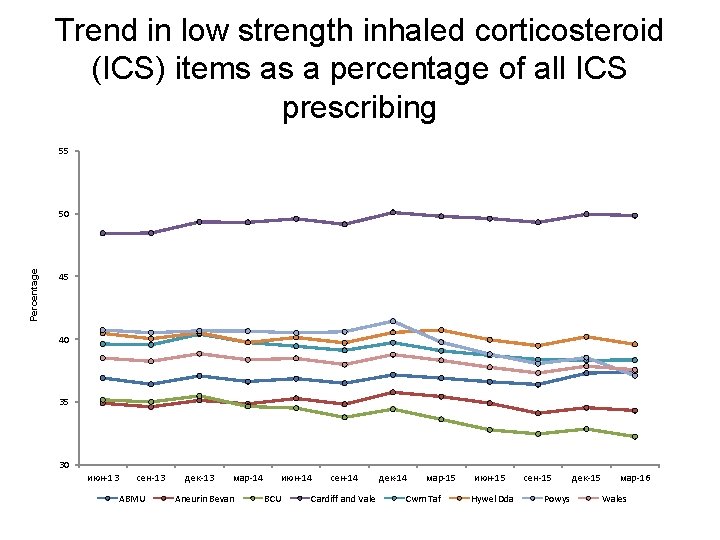
Trend in low strength inhaled corticosteroid (ICS) items as a percentage of all ICS prescribing 55 Percentage 50 45 40 35 30 июн-13 сен-13 ABMU дек-13 мар-14 Aneurin Bevan июн-14 BCU сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 мар-16 Wales
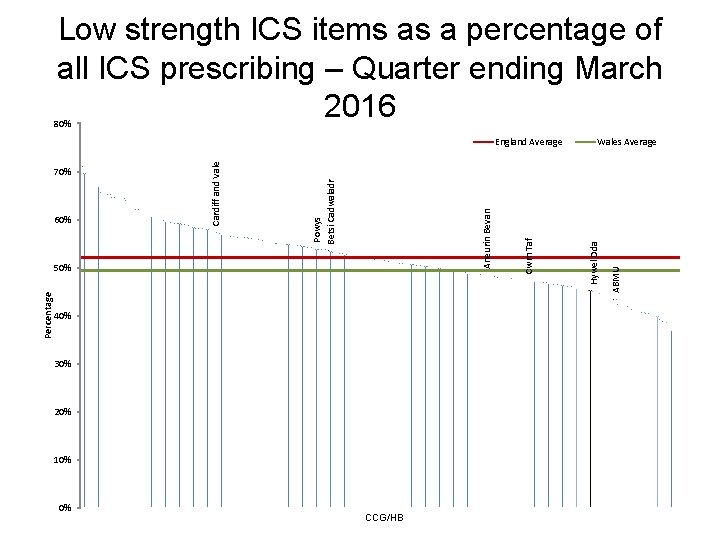
Low strength ICS items as a percentage of all ICS prescribing – Quarter ending March 2016 80% 40% 30% 20% 10% 0% CCG/HB Hywel Dda Wales Average ABMU Percentage 50% Cwm Taf Aneurin Bevan 60% Powys Betsi Cadwaladr 70% Cardiff and Vale England Average

Inhaled corticosteroids (ICS) • Aims to encourage the routine review of ICS in people with asthma, particularly those on high doses, encouraging step down of the dose when clinically appropriate. • ICS (particularly at high doses) are associated with side effects: adrenal suppression, growth failure, decrease in bone mineral density, cataracts and glaucoma. • The British guideline on the management of asthma recommends: – a stepwise approach for the treatment of asthma with ICS as the first-choice regular preventer therapy for adults and children with asthma. – dose of ICS should be titrated to the lowest dose at which effective control of asthma is maintained. – ICS dose reduction should be considered every three months, decreasing the dose by approximately 25– 50% each time.
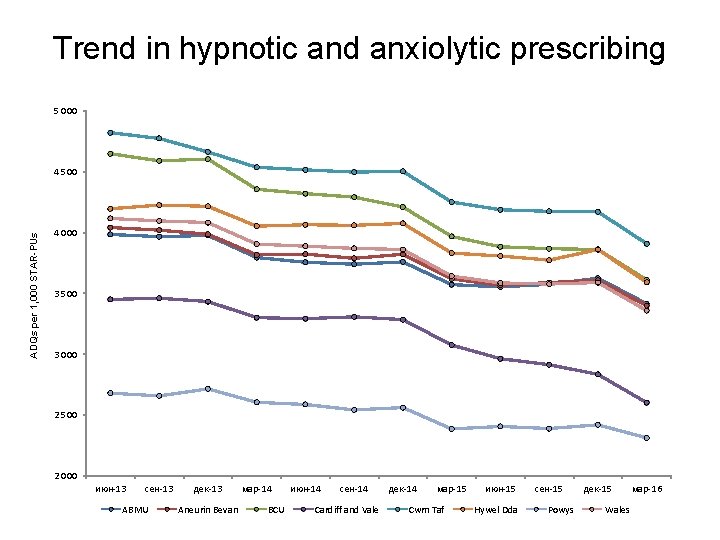
Trend in hypnotic and anxiolytic prescribing 5 000 ADQs per 1, 000 STAR-PUs 4 500 4 000 3 500 3 000 2 500 2 000 июн-13 сен-13 ABMU дек-13 Aneurin Bevan мар-14 BCU июн-14 сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 Wales мар-16
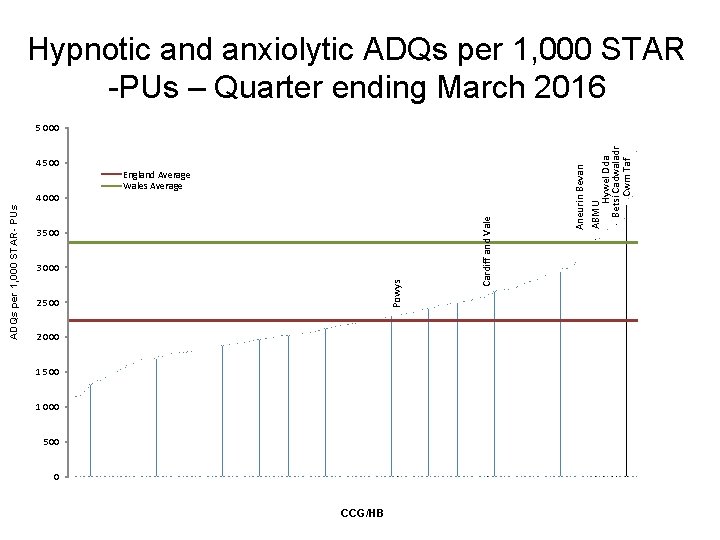
Hypnotic and anxiolytic ADQs per 1, 000 STAR -PUs – Quarter ending March 2016 3 500 3 000 Powys ADQs per 1, 000 STAR- PUs 4 000 England Average Wales Average 2 500 2 000 1 500 1 000 500 0 CCG/HB Cardiff and Vale 4 500 Aneurin Bevan ABMU Hywel Dda Betsi Cadwaladr Cwm Taf 5 000

Hypnotics and anxiolytics • Aims to encourage a reduction in the inappropriate prescribing of hypnotics and anxiolytics in Wales. • Variation in prescribing rates across health boards in Wales. • Prescribing in Wales is still high compared to England: six health boards in Wales within the highest prescribing quartile when compared to CCGs in England. • Long-term use of benzodiazepine hypnotics and anxiolytics is associated with increased risk of Alzheimer’s disease and falls. • AWMSG hypnotics and anxiolytic educational pack provides: – examples of practice protocols to allow clinicians to agree a consistent approach for the prescribing and review of hypnotics and anxiolytics. – materials to support the review and discontinuation of hypnotic and anxiolytic treatment.
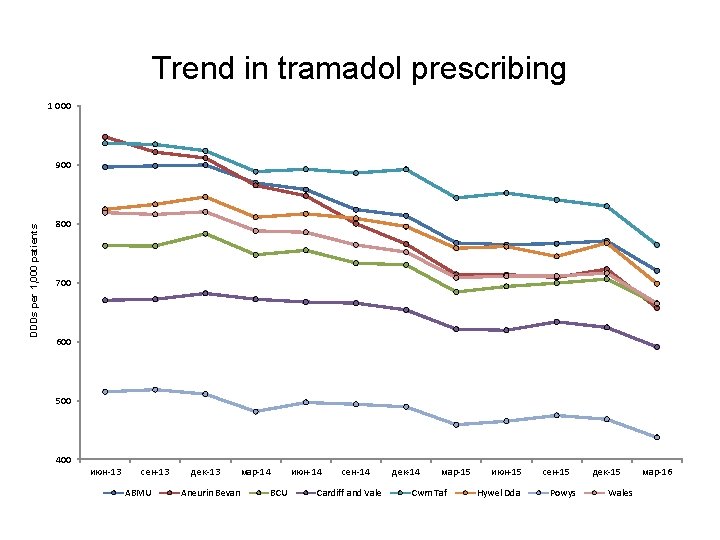
Trend in tramadol prescribing 1 000 DDDs per 1, 000 patients 900 800 700 600 500 400 июн-13 сен-13 ABMU дек-13 Aneurin Bevan мар-14 BCU июн-14 сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 Wales мар-16
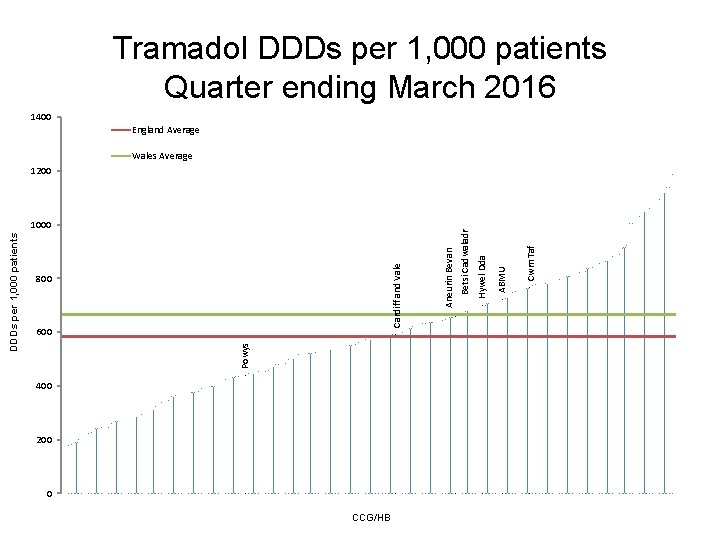
Tramadol DDDs per 1, 000 patients Quarter ending March 2016 1400 England Average Wales Average 600 400 200 0 CCG/HB Cwm Taf ABMU Hywel Dda Aneurin Bevan Cardiff and Vale 800 Powys DDDs per 1, 000 patients 1000 Betsi Cadwaladr 1200

Opioid analgesics – Tramadol • Aims to encourage the appropriate use and review of tramadol, minimising the potential for diversion and misuse. • Deaths related to tramadol misuse in England Wales increased from 83 in 2008 to 240 in 2014. • In June 2014, tramadol was placed within Schedule III to the Misuse of Drugs Regulations, requiring prescriptions to be written as for other controlled drugs, including a maximum supply of 28 days. • Avoid abrupt withdrawal after long-term tramadol treatment. • Tramadol reduces seizure threshold. • Side effects include: dizziness, constipation, hallucinations, confusion and convulsions. Drug dependence and withdrawal have been reported at therapeutic doses. • Multiple drug interactions: warfarin, antidepressants (SSRIs, SNRIs, TCAs)
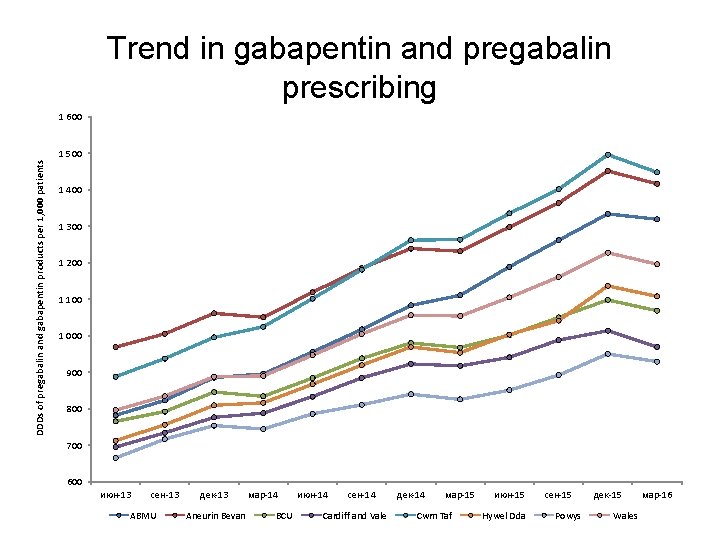
Trend in gabapentin and pregabalin prescribing 1 600 DDDs of pregabalin and gabapentin products per 1, 000 patients 1 500 1 400 1 300 1 200 1 100 1 000 900 800 700 600 июн-13 сен-13 ABMU дек-13 Aneurin Bevan мар-14 BCU июн-14 сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 Wales мар-16
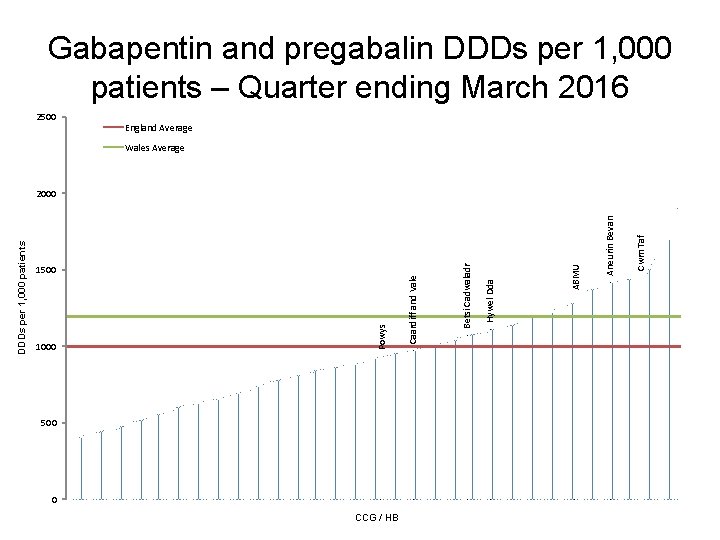
Gabapentin and pregabalin DDDs per 1, 000 patients – Quarter ending March 2016 2500 England Average Wales Average 1000 500 0 CCG / HB Cwm Taf Aneurin Bevan ABMU Hywel Dda Betsi Cadwaladr Caardiff and Vale 1500 Powys DDDs per 1, 000 patients 2000

Gabapentin and pregabalin • Aims to encourage the appropriate use and review of gabapentin and pregabalin, minimising the potential for diversion and misuse. • Neuropathic pain is common and can have a significant impact on quality of life. NICE CG 173 recommends amitriptyline, duloxetine, gabapentin and pregabalin as first line treatment options; however, it does not recommend one particular medicine as superior to the others. • Advice published by the Advisory Council on the Misuse of Drugs (ACMD) in January 2016 highlighted the potential risk of dependence, misuse and diversion of gabapentin and pregabalin and the importance of appropriate prescribing to minimise these risks. • If the patient has not shown sufficient benefit within eight weeks of reaching maximum tolerated dose, gabapentin and pregabalin should be reduced gradually over a minimum of one week, and stopped. • Neuropathic pain management is often complex and prescribers need to make evidence-based, informed decisions based on the individual needs of the patient.
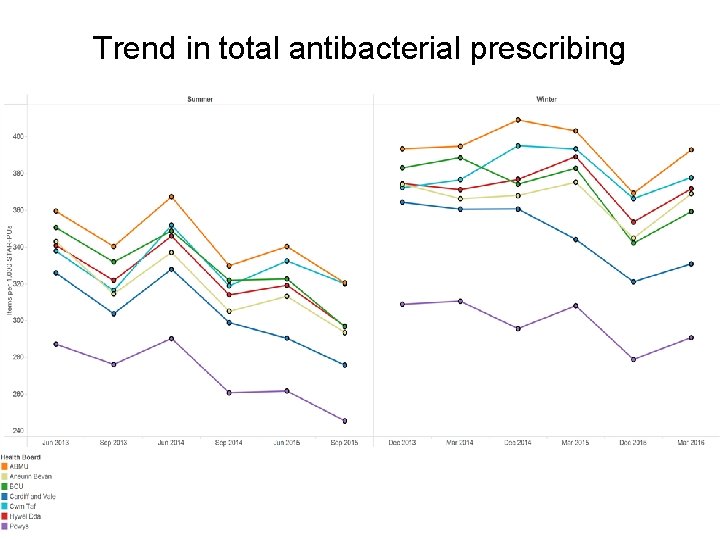
Trend in total antibacterial prescribing
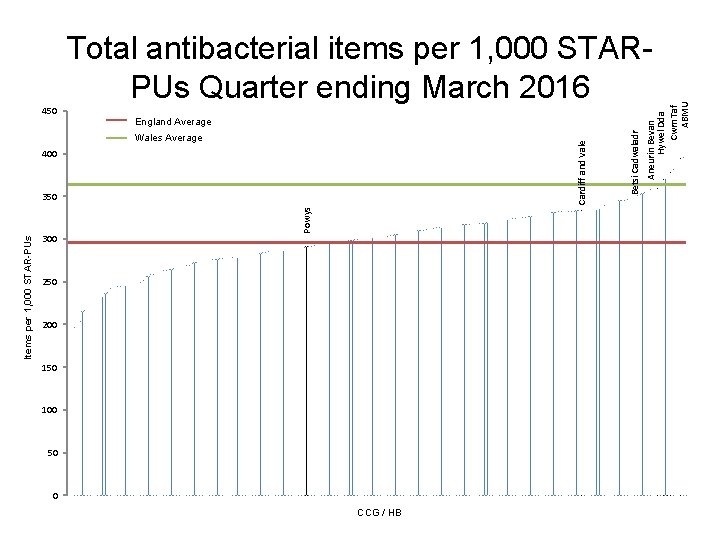
Series 2 England Average Cardiff and Vale England Average Wales Average Series 3 400 Items per 1, 000 STAR-PUs 300 Powys 350 200 150 100 50 0 CCG / HB Betsi Cadwaladr 450 Aneurin Bevan Hywel Dda Cwm Taf ABMU Total antibacterial items per 1, 000 STARPUs Quarter ending March 2016
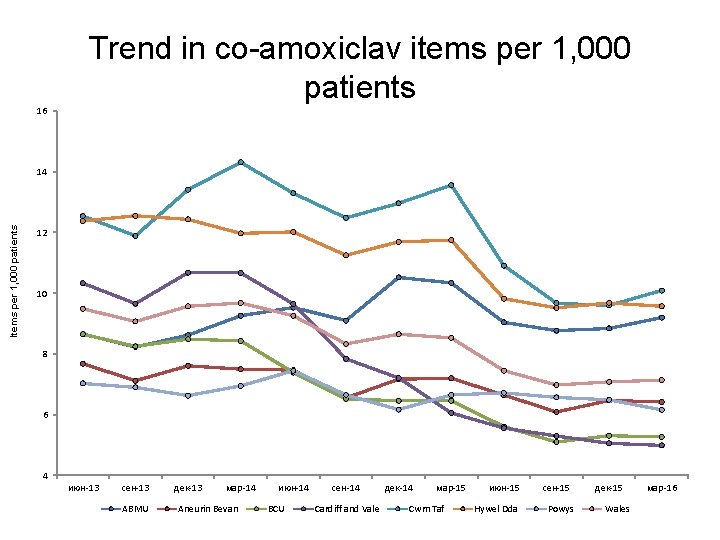
Trend in co-amoxiclav items per 1, 000 patients 16 Items per 1, 000 patients 14 12 10 8 6 4 июн-13 сен-13 ABMU дек-13 мар-14 Aneurin Bevan июн-14 BCU сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 Wales мар-16
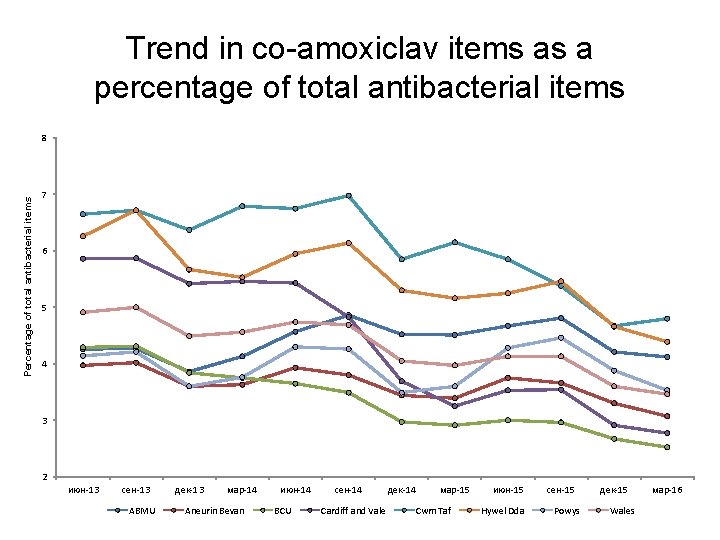
Trend in co-amoxiclav items as a percentage of total antibacterial items Percentage of total antibacterial items 8 7 6 5 4 3 2 июн-13 сен-13 ABMU дек-13 мар-14 Aneurin Bevan июн-14 BCU сен-14 Cardiff and Vale дек-14 мар-15 Cwm Taf июн-15 Hywel Dda сен-15 Powys дек-15 Wales мар-16
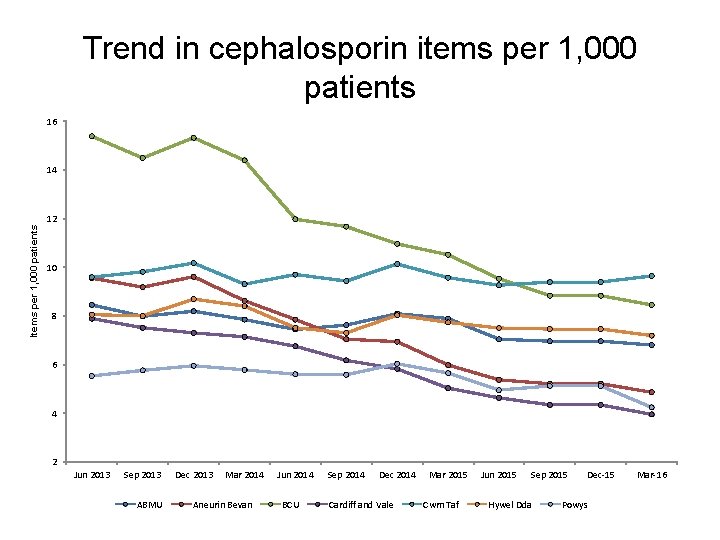
Trend in cephalosporin items per 1, 000 patients 16 Items per 1, 000 patients 14 12 10 8 6 4 2 Jun 2013 Sep 2013 ABMU Dec 2013 Mar 2014 Aneurin Bevan Jun 2014 BCU Sep 2014 Dec 2014 Cardiff and Vale Mar 2015 Cwm Taf Jun 2015 Sep 2015 Hywel Dda Dec-15 Powys Mar-16
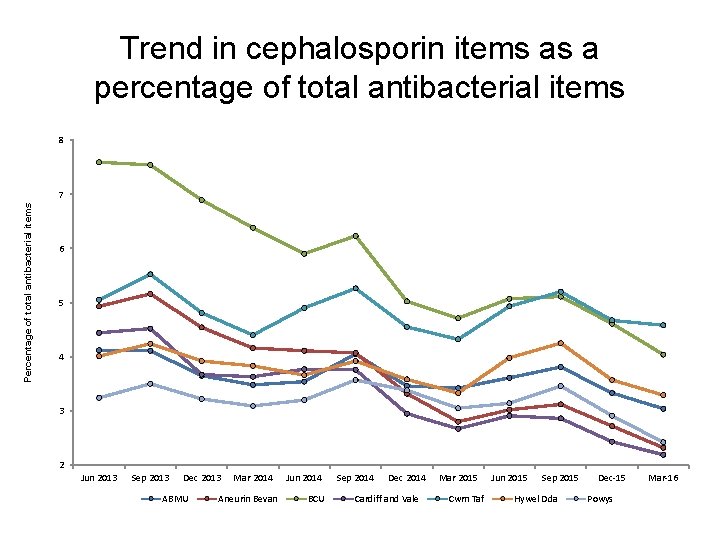
Trend in cephalosporin items as a percentage of total antibacterial items 8 Percentage of total antibacterial items 7 6 5 4 3 2 Jun 2013 Sep 2013 Dec 2013 ABMU Mar 2014 Aneurin Bevan Jun 2014 BCU Sep 2014 Dec 2014 Cardiff and Vale Mar 2015 Cwm Taf Jun 2015 Sep 2015 Hywel Dda Dec-15 Powys Mar-16
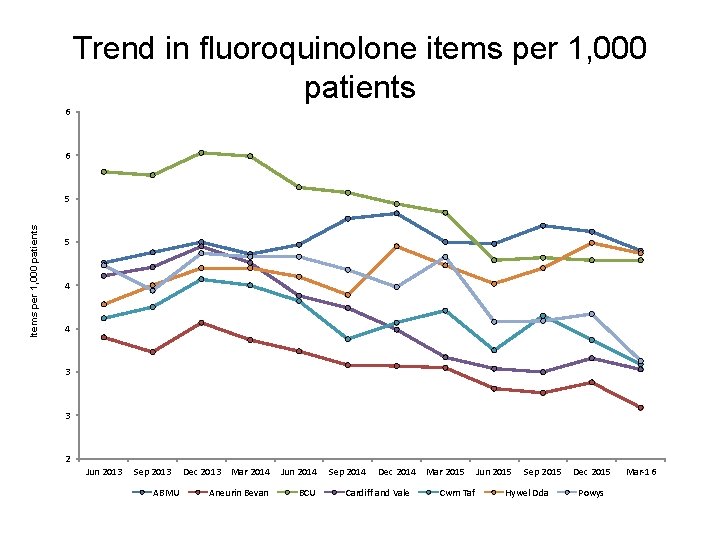
Trend in fluoroquinolone items per 1, 000 patients 6 6 Items per 1, 000 patients 5 5 4 4 3 3 2 Jun 2013 Sep 2013 ABMU Dec 2013 Mar 2014 Jun 2014 Aneurin Bevan BCU Sep 2014 Dec 2014 Cardiff and Vale Mar 2015 Cwm Taf Jun 2015 Sep 2015 Hywel Dda Dec 2015 Powys Mar-16
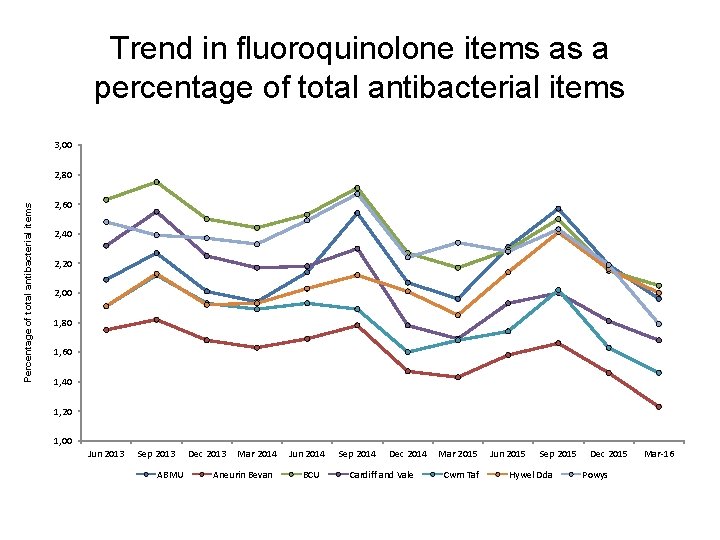
Trend in fluoroquinolone items as a percentage of total antibacterial items 3, 00 Percentage of total antibacterial items 2, 80 2, 60 2, 40 2, 20 2, 00 1, 80 1, 60 1, 40 1, 20 1, 00 Jun 2013 Sep 2013 ABMU Dec 2013 Mar 2014 Aneurin Bevan Jun 2014 BCU Sep 2014 Dec 2014 Cardiff and Vale Mar 2015 Cwm Taf Jun 2015 Sep 2015 Hywel Dda Dec 2015 Powys Mar-16

Antibiotics • These indicators support one of the core elements of the Welsh Antimicrobial Resistance Programme: to inform, support and promote the prudent use of antimicrobials. They also aim to reduce the prescribing of medicines associated with an increased risk of C. difficile, MRSA and resistant UTIs. • AWMSG CEPP National Audit: Focus on antibiotic prescribing – consists of stand-alone bite-size components • sore throat, • acute rhinosinusitis, • UTI in females, • acute cough or bronchitis, • fluoroquinolone prescribing, • cephalosporin prescribing, • co-amoxiclav prescribing, • hospital prescribing of antibiotics, • delayed prescriptions, • read coding to identify healthcare-acquired infections.
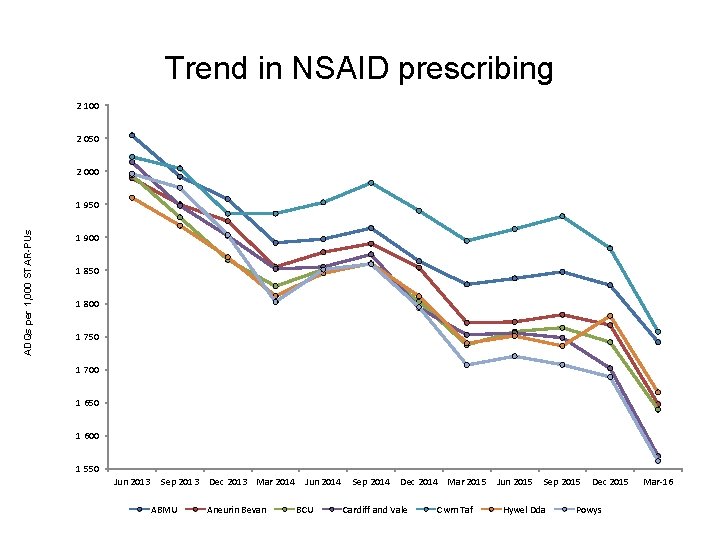
Trend in NSAID prescribing 2 100 2 050 2 000 ADQs per 1, 000 STAR-PUs 1 950 1 900 1 850 1 800 1 750 1 700 1 650 1 600 1 550 Jun 2013 Sep 2013 ABMU Dec 2013 Mar 2014 Aneurin Bevan Jun 2014 BCU Sep 2014 Dec 2014 Mar 2015 Cardiff and Vale Cwm Taf Jun 2015 Sep 2015 Hywel Dda Dec 2015 Powys Mar-16
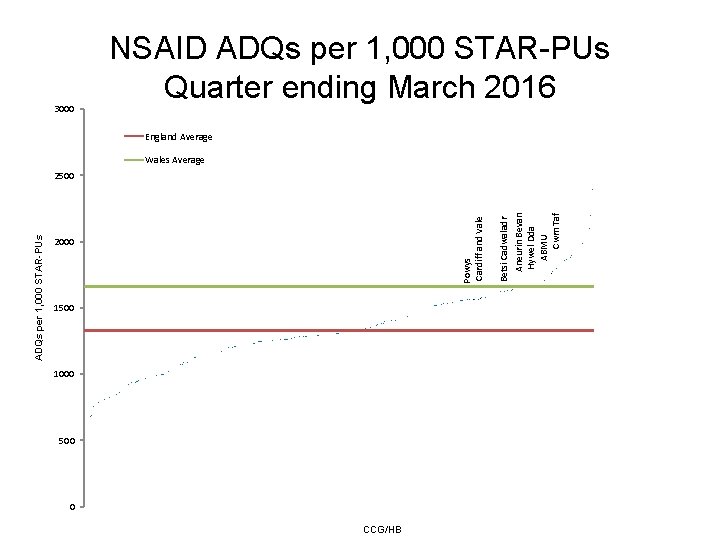
3000 NSAID ADQs per 1, 000 STAR-PUs Quarter ending March 2016 England Average Wales Average 2000 1500 1000 500 0 CCG/HB Betsi Cadwaladr Aneurin Bevan Hywel Dda ABMU Cwm Taf Powys Cardiff and Vale ADQs per 1, 000 STAR-PUs 2500
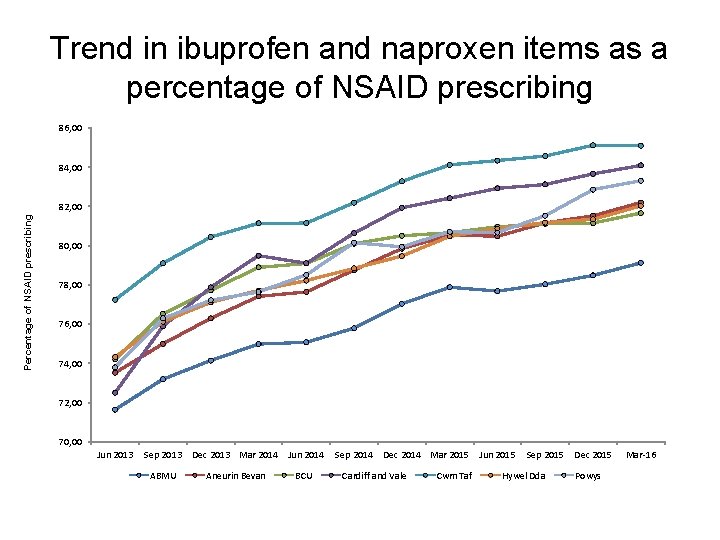
Trend in ibuprofen and naproxen items as a percentage of NSAID prescribing 86, 00 84, 00 Percentage of NSAID prescribing 82, 00 80, 00 78, 00 76, 00 74, 00 72, 00 70, 00 Jun 2013 Sep 2013 ABMU Dec 2013 Mar 2014 Jun 2014 Aneurin Bevan BCU Sep 2014 Dec 2014 Mar 2015 Jun 2015 Cardiff and Vale Cwm Taf Sep 2015 Hywel Dda Dec 2015 Powys Mar-16
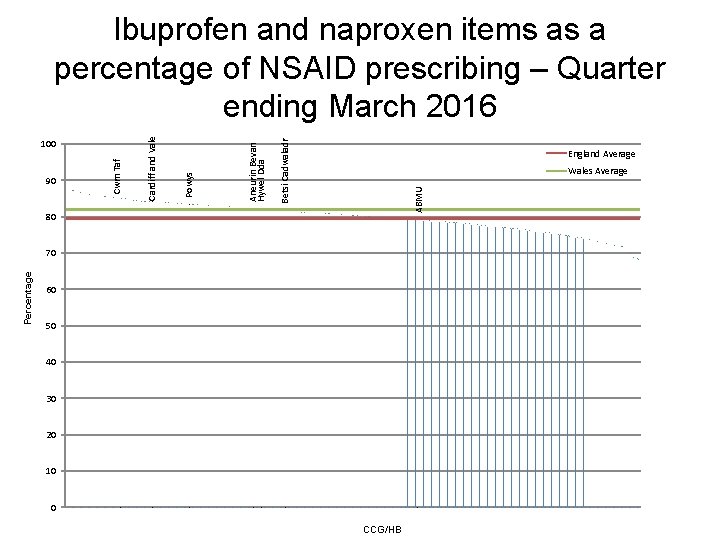
Betsi Cadwaladr England Average Wales Average ABMU Aneurin Bevan Hywel Dda Powys 90 Cwm Taf 100 Cardiff and Vale Ibuprofen and naproxen items as a percentage of NSAID prescribing – Quarter ending March 2016 80 Percentage 70 60 50 40 30 20 10 0 CCG/HB

NSAIDs • Aims – to encourage a reduction in total NSAID prescribing, which is consistently higher than in England, – to increase the proportion of ibuprofen and naproxen prescribing, because these drugs are associated with a lower risk of cardiovascular adverse events than other NSAIDs. • It is recommended that prescribers should: – Review their NSAID prescribing using the AWMSG CEPP National Audit: Towards Appropriate NSAID Prescribing. – Use acute rather than repeat prescriptions for NSAIDs. – Set the default to small quantities (e. g. 1– 2 weeks supply) per script. – Prescribe naproxen 250 mg rather than 500 mg to allow patients to make dose adjustments.

Yellow Cards • Aim to increase the number of Yellow Cards submitted by GP practices. • The Yellow Card Scheme is vital in helping the Medicines and Healthcare Products Regulatory Agency monitor the safety of medicines and vaccines and supports the identification and collation of adverse drug reactions (ADRs), which might not have been known about before. • What to report – Established medicines and vaccines: report all suspected ADRs considered to be serious (i. e. fatal, life-threatening, congenital abnormality, disabling or incapacitating, or resulting in prolonged hospitalisation). – New medicines and vaccines (black triangle): report all suspected ADRs. • Yellow Card reporting can be used to report suspected ADRs to medicines, vaccines, homeopathic or herbal remedies, medical device incidents, defective or suspected counterfeit medicines. • A strong safety culture requires good reporting of adverse events and critical incidents from across all professions and healthcare settings as well as from patients.
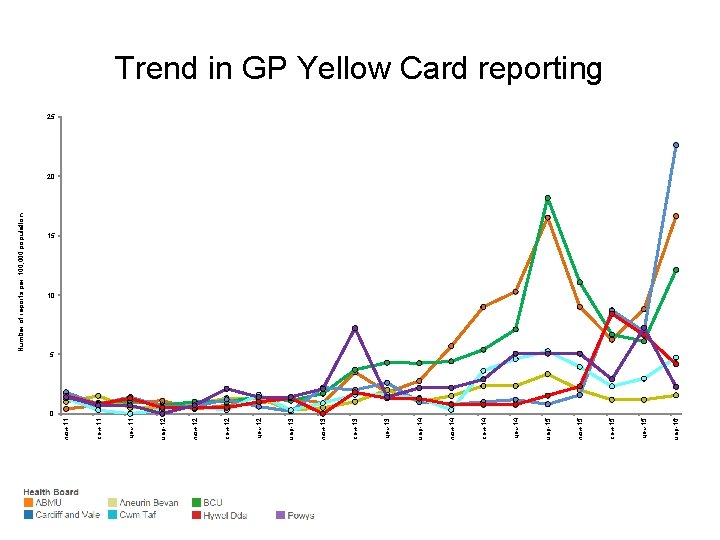
мар-16 дек-15 сен-15 июн-15 мар-15 дек-14 сен-14 июн-14 мар-14 дек-13 сен-13 июн-13 мар-13 дек-12 сен-12 июн-12 мар-12 дек-11 сен-11 июн-11 Number of reports per 100, 000 population Trend in GP Yellow Card reporting 25 20 15 10 5 0

. For more information on the National Prescribing Indicators for 2016– 2017, please visit the AWMSG website at www. awmsg. org or contact AWTTC on awttc@wales. nhs. uk
- Slides: 40