Nanofibrous scaffolds for Wound Healing Mohamad Javad MirzaeiParsa

Nanofibrous scaffolds for Wound Healing Mohamad Javad Mirzaei-Parsa 1 Department of Medical Nanotechnology, Faculty of Allied Medical Sciences, Kerman University of Medical Sciences, Kerman, Iran

2 Introduction and statistics According to the National Center for Health Statistics, there about 41 million trauma cases each year in the USA with an economic burden of >$670 billion annually. Fire- and heat-induced burns result in 35 million injuries each year worldwide, with 2. 9 million hospitalizations and 238, 000 deaths. Chronic wounds are a global healthcare problem. In the USA, 6. 5 million patients endure chronic skin ulcers with >$25 billion spent annually on their treatment. Human skin wounds are a major, rapidly growing threat for public health and the economy

3 Advantages of nanofibers as a wound dressing v Fiber structures: ECM analog, porosity , diameter, and fiber alignment v Pyhsical parameters: Mechanical properties, degradation rate v Delivery of materials (drug, metal, gene, growth factor)
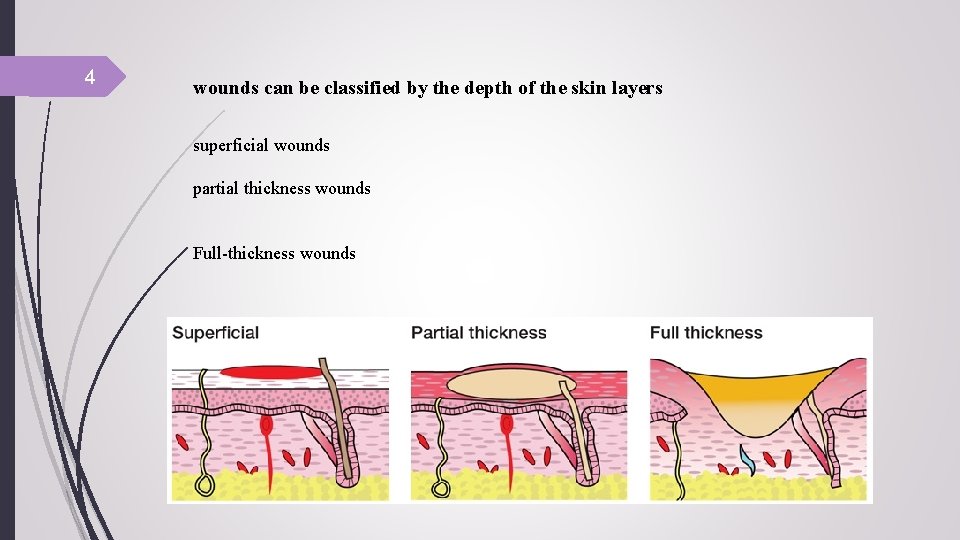
4 wounds can be classified by the depth of the skin layers superficial wounds partial thickness wounds Full-thickness wounds
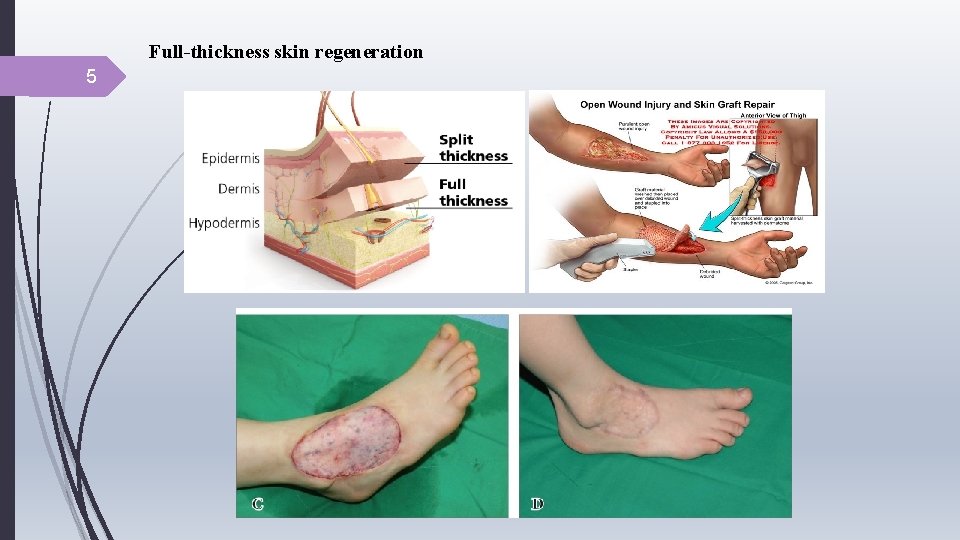
Full-thickness skin regeneration 5

6 Bioengineered skin equivalents are largely grouped into three groups. v Epidermal components (Epicel, Myskin) v Dermal components which are mainly based on chemical analogues of extracellular matrix (ECM). (Dermagraft, Alloderm, Integra, Matriderm). Numerous studies have proven that efficient wound closure requires the interaction of both dermal and epidermal components. v Combination of both dermal and epidermal components such as (Apligraf)
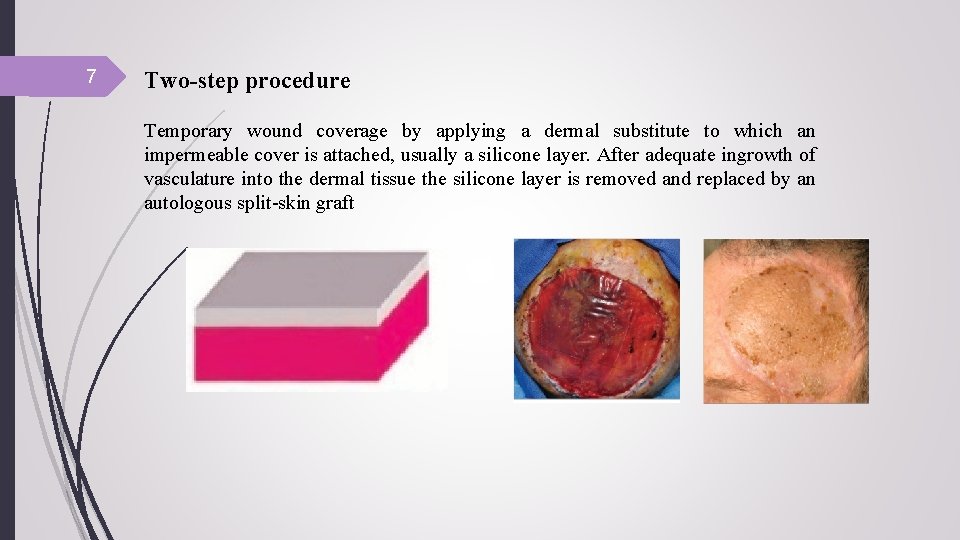
7 Two-step procedure Temporary wound coverage by applying a dermal substitute to which an impermeable cover is attached, usually a silicone layer. After adequate ingrowth of vasculature into the dermal tissue the silicone layer is removed and replaced by an autologous split-skin graft
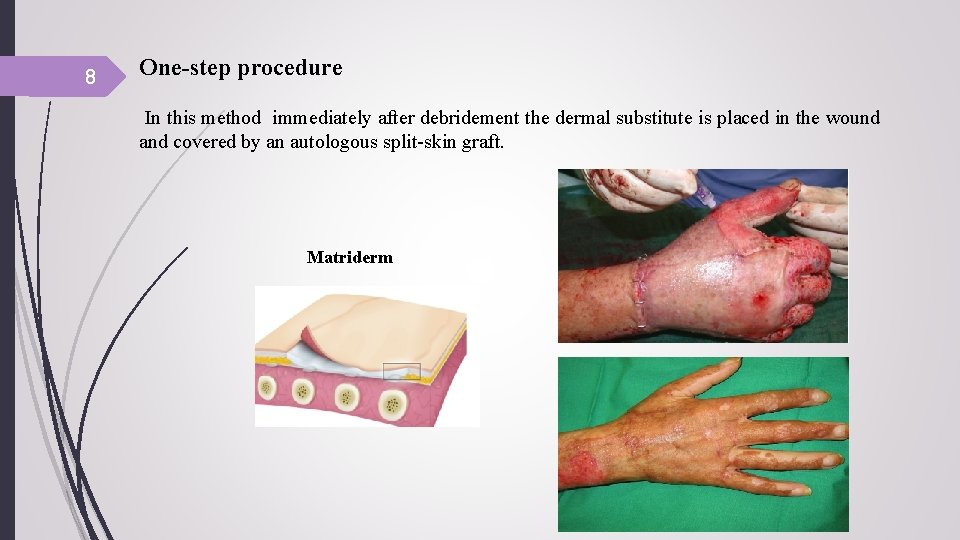
8 One-step procedure In this method immediately after debridement the dermal substitute is placed in the wound and covered by an autologous split-skin graft. Matriderm

9 Aim of our study The aim of this study was to evaluate the feasibility of combining acellular dermal matrix (ADM) with nanofiber as a bilayer scaffold for treatment of full-thickness wounds in a single step procedure.
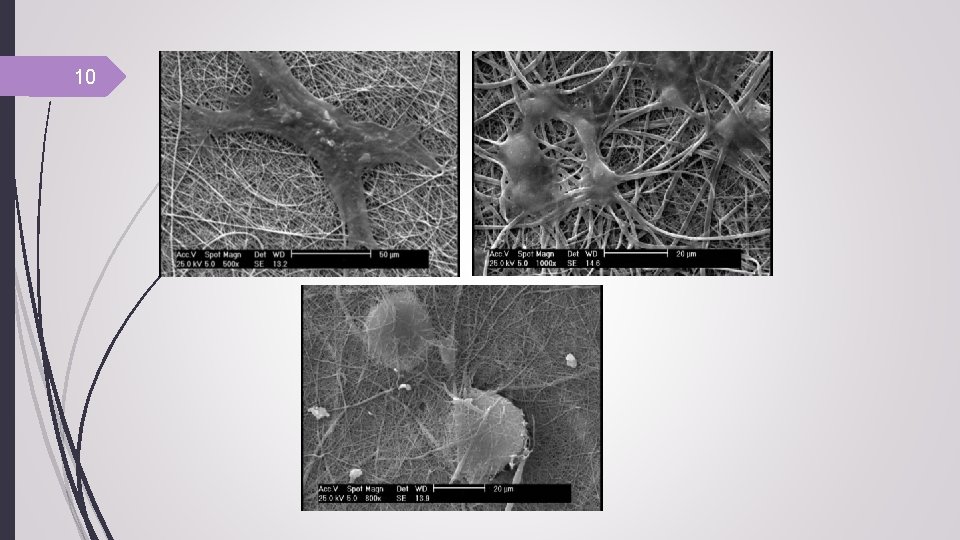
10

11 Preparation of Acellular dermal matrix (ADM) Acellular dermal matrix from rat was donated by tissue processing unit of Iranian Tissue Bank (Imam Khomeini Hospital, Tehran, Iran). Preparation of ADM-nanofiber scaffolds (bilayer scaffold) For bilayer scaffolds, the nanofibers were attached to ADM with collagen (2 wt%). After freeze - drying , the bilayer scaffolds fixed with absorbable surgical sutures for in vivo transplantation.
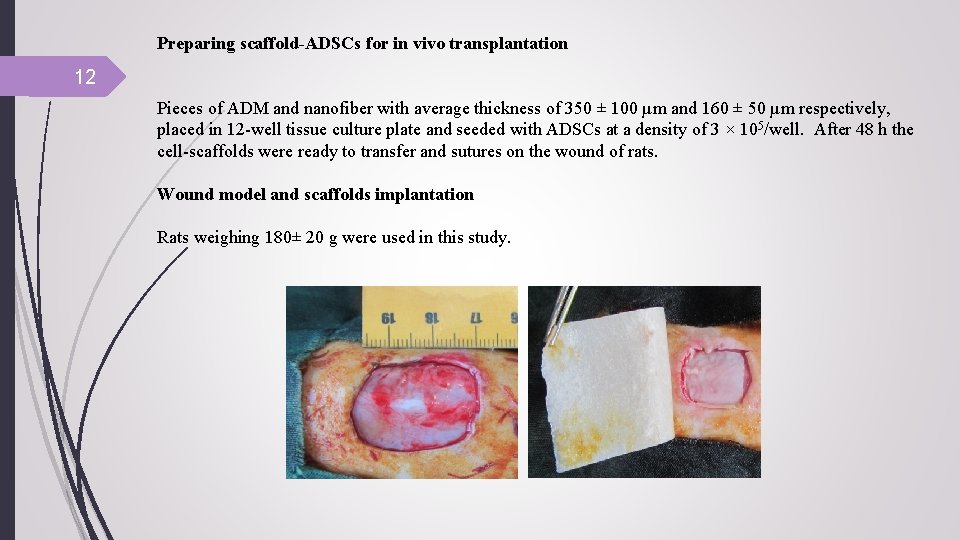
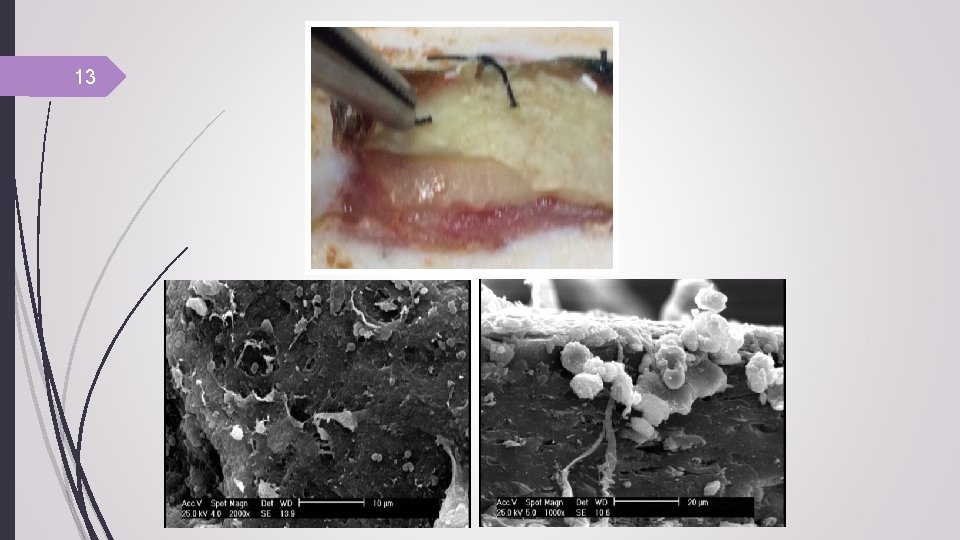
Preparing scaffold-ADSCs for in vivo transplantation 12 Pieces of ADM and nanofiber with average thickness of 350 ± 100 µm and 160 ± 50 µm respectively, placed in 12 -well tissue culture plate and seeded with ADSCs at a density of 3 × 105/well. After 48 h the cell-scaffolds were ready to transfer and sutures on the wound of rats. Wound model and scaffolds implantation Rats weighing 180± 20 g were used in this study.
13
14
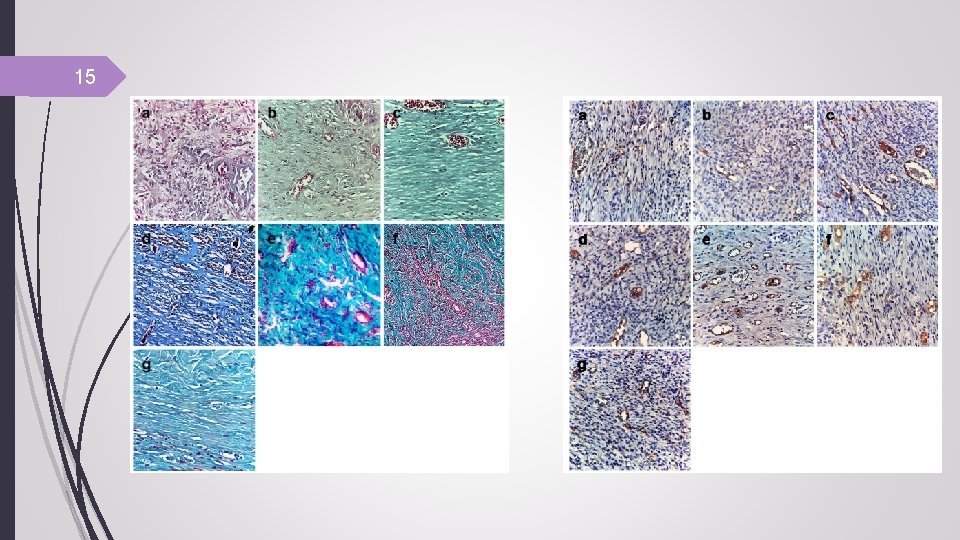
15
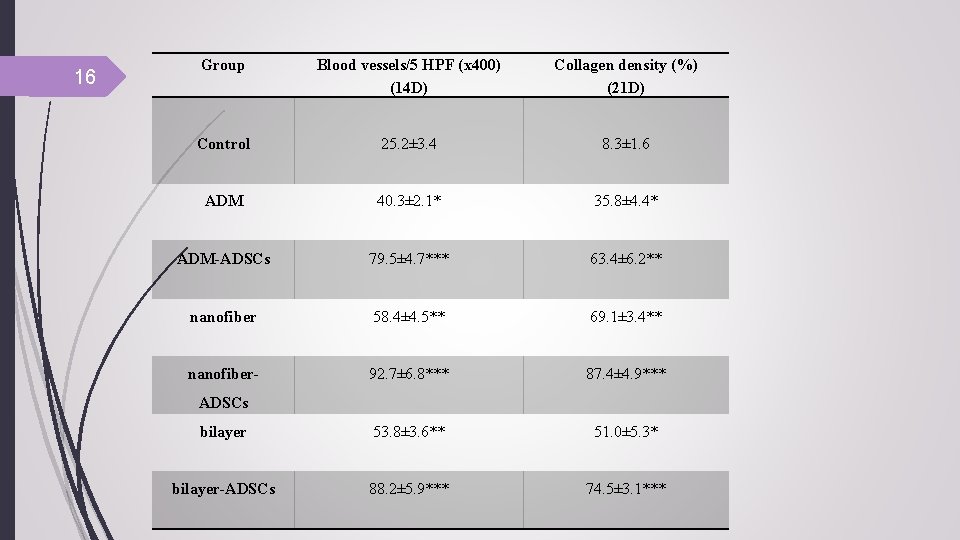
16 Group Blood vessels/5 HPF (x 400) (14 D) Collagen density (%) (21 D) Control 25. 2± 3. 4 8. 3± 1. 6 ADM 40. 3± 2. 1* 35. 8± 4. 4* ADM-ADSCs 79. 5± 4. 7*** 63. 4± 6. 2** nanofiber 58. 4± 4. 5** 69. 1± 3. 4** nanofiber- 92. 7± 6. 8*** 87. 4± 4. 9*** bilayer 53. 8± 3. 6** 51. 0± 5. 3* bilayer-ADSCs 88. 2± 5. 9*** 74. 5± 3. 1*** ADSCs

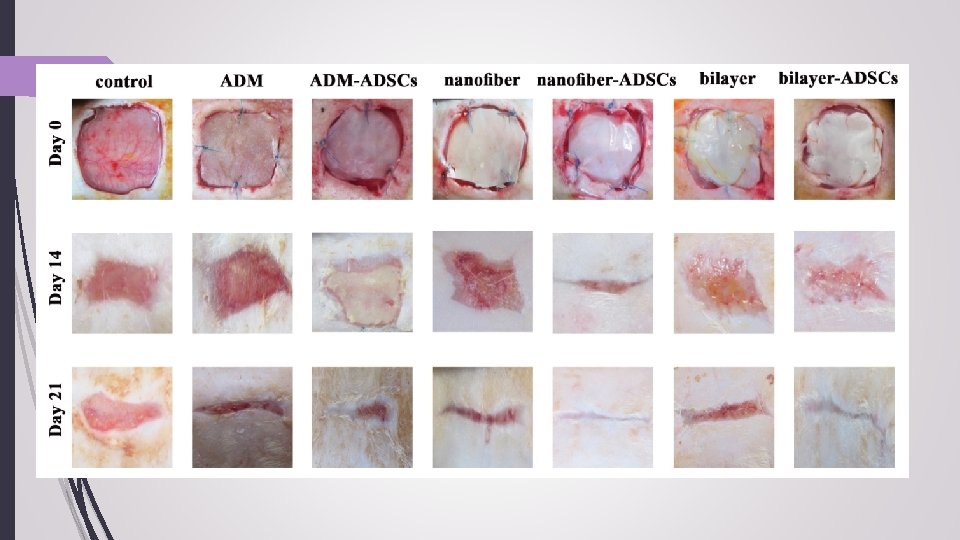
17 Conclusion The feasibility of combining nanofiber-ADM as a bilayer scaffold for treatment of fullthickness wounds in a single-step procedure. ADM can be integrated into wound bed or enhanced wound healing when covered with nanofibers seeded with ADSCs This study revealed that ADSCs seeded onto bilayer scaffolds can promote regeneration, reepithelialization, angiogenesis, and collagen remodeling in comparison to the cell-free scaffolds and control. Further investigations are needed in order to optimize this technique to produce bilayer scaffolds as an alternative for splitthickness grafts.
- Slides: 17