n n n n 26 Basophils and mast

n n n n 26. Basophils and mast cells- types, function. 27. Immune mechanisms of the inflammation (local and systemic reaction) 28. Cytokines (overview, disposal according their function) 29. Physiological mechanisms of regulation of the immune system. 30. HLA system, 1 st class molecules, their structure and function 31. HLA system, 2 nd class molecules, their structure and function 32. HLA system, genetic background. HLA typing.

26. Basophils and mast cells - types, function.
Basophils n n n A type of bone marrow derived circulating granulocyte Ability to migrate into the tissue Structural and functional similarities to mast cells = granules are containing inflammatory mediators; express a high- afinity receptor for Fc fragment of Ig. E on the cell surface Participate in immediate hypersensitivity reactions Produce cytokines (IL-4, 13)


Basophils surface markers n FcεRI – high-affinity receptor for Fc fragment of Ig. E n CD 123 – receptor for IL- 3 63 – activating marker – expressed after degranulation
Mast cells n Derived from bone marrow precursor n Reside in tissues adjacent to blood vessels n Express a high-affinity receptor for Fc fragment of Ig. E n Contain numerous mediator-filled granules
Mast cells surface markers n FcεRI n CD – high-affinity receptor for Ig. E 117 - membrane gp – mediates interaction necessary for mast cells proliferation

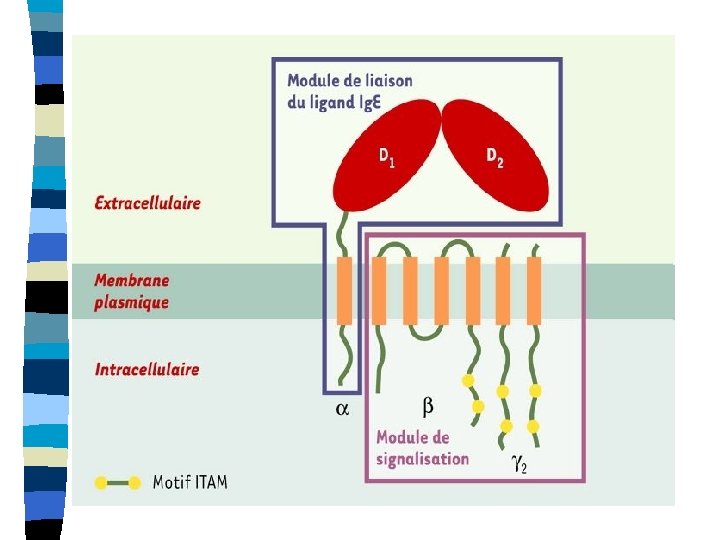
FcεRI complex consists: - α- chains with two extracellular immunoglobulin domains - β- chains – four times cross the membrane – both their ends are inserted to the cytoplasm - γ- chain = homodimer - β and γ chains – contain activating motives ITAM (mediate transport of activating signal from mast cell surface after binding of Ig. E) in their cytoplasmic part n

Cytoplasmic granules Histamin (dilation of small blood vessels, increase of vascular permeability, contraction of smooth muscles), proteases (cause a damage to the tissues) n Cytokines: IL- 4 ( stimulates Ig. E production by B cells), 5 (activates eosinophils), 13 (stimulates mucus secretion by airway epithelial cells), TNF α, IL-1 n Growth factors: TGF- β, VEGF (vascular endothelial growth factor) n Synthetize: PAF (platelet activation factor), LTC 4 - leukotrienes (stimulate prolonged smooth muscle contraction), PGD 2 prostaglandins (cause vascular dilation) n

Mast cells function Participate on defence against bacterial and parasites infection n Develop immediate hypersensitivity reactions (production of Ig. E antibodies in response to an antigen, binding of Ig. E to Fc receptors of mast cells, cross-linking of the bound Ig. E by the antigen and release of mast cell mediators) n Take part in reparation of tissues angiogenesis, production of intercellular substances n
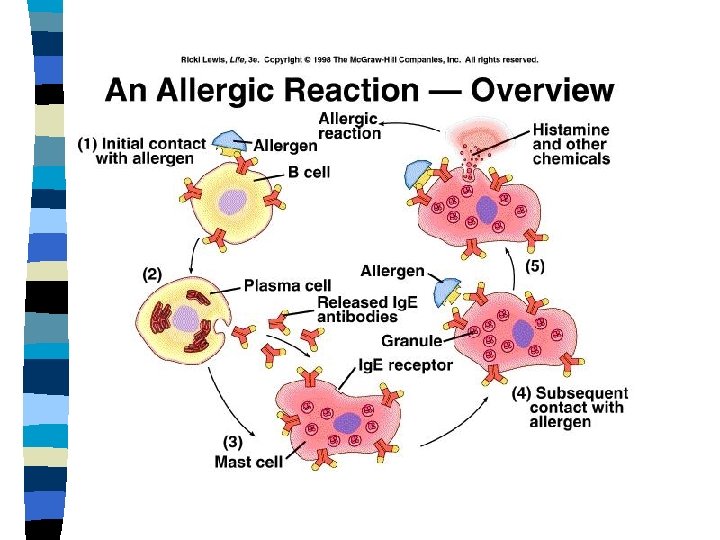

27. Immune mechanisms of the inflammation (local and systemic reaction)

Inflammation = a complex reaction of the innate immune system in vascularized tissues that involves accumulation and activation of leukocytes and plasma proteins at a site of infection, toxin exposure or cell injury n Iniciated by changes in blood vessels that promote leukocyte recruitment and movement of fluid and plasma proteins into tissue n Inflammation serves a protective function in controlling infections and promoting tissue repair
Inflammatory response n Local - signs: redness, swelling, pain, heat n Systemic n Acute – sings: fever or chronic process

Inflammation - iniciation n 1. signal: phagocytes and degranulated mast cells, substances released from damaged cells, parts of intercellular substance exposed by injury

Local inflamation n n Increase of vessels permeability – plasma fluid passes through the blood vesselsswelling Increase of endothelial adhesivity (expression of cell adhesion molecules)phagocytes and lymphocytes adhere to endothelial cells – pass to the tissues The coagulation, fibrinolytic, kinin and complement systems are activated Local nerve endings are influenced (pain) changes in temperature regulation

Local inflamation phagocytes- accumulate in a site of injury, produce cytokines n Ag + APC home to LN (lymph nodes) activate T cells and induce their terminal differentiation, activation of B cells and their changes into plasma cells with production of antibodies n Mature Th 1 lymphocytes migrate from LN to the site of infection and stimulate macrophages n

Systemic response (SR) to inflammation Development of SR depends on: - range of damage - duration of local inflammation n SR can arise also without local inflammation: - after massive enter of microorganisms into the blood = septic shock - after intravascular antigen impulse of noninfection character = anaphylactic shock n Massive release of mediators (cytokines, complement, histamin)- leads to a massive vasodilatation- hypotensis- vascular collapse n

Sings of systemic inflammation n Fever- caused by stimulation of hyppothalamic center of termoregulation (by proinflammatory cytokines –TNF, IL-1, INF-gama) n Caused also by increase of proteosynthesis, increase of Hsp production (hot shock protein)

Mediators of inflammation Cytokines produced in the site of inflammation - come through the blood into the liverstimulate production of plasma proteins of acute inflammation phase (CRP, amyloid P, complement C 3, C 4), transport proteins (ceruloplasmin, transferin) and inhibitors of proteases (alfa 2 -macroglobulin) n Proteins of acute phase – function opsonisation, activation of complement n Cytokines and mediators cause bone marrow to release and produce leukocytesleukocytosis n

Reparation of damaged tissues Activation of reparation process: - occurs during later phases of inflammation - phagocytes- eliminate damaged cells - activation of fibroplastic mechanisms - activation of angiogenesis - start regeneration and remodelation of tissues n Control by cytokines, hormons, enzymes n Chronic inflammation – accompane by fibrotic process n

28. Cytokines (overview, disposal according their function)

Cytokines n n n Humoral factors - provide intercellular communication between immune cells + communication between immune system and other body systems Proteins secreted by leukocytes (and by other cells of immune system) Influence different cells of immune system through specific receptors Forms- secreted or membrane Effects - pleiotropic (1 cytokine has a several fysiological effects)

Function of cytokines n n n Activating signals for cells – activate, regulate cell cycle, mitotic activity Cause changes of the cell membranes – increase of cytokine receptors expression Participate in reparation of tissues in the terminal phase of inflammation Regulate immune cells proliferation and differentiation in the immune organs Influence migration of the immune cells

Classification of cytokines n Pro-inflammatory n Anti-inflammatory n With growth activity factor n Participating in humoral response IS n Participating in cell response IS n With antiviral effect
Proinflammatory cytokines IL-1 – produced by macrophages and T cells; activates neutrophils, endothelial cells and T cells, induces synthesis of acute phase proteins in liver, causes fever n IL-6 – produced by T and B cells, monocytes; regulates B cell differentiation and proliferation, synthesis antibodies; stimulates hepatocytes to produce acute phase proteins n IL-8 – produced by monocytes, macrophages, endothelial cells; chemotactic factor for neutrophils n IL-12, IL-18, TNF n

TNF α – produced by macrophages (+T a B cells, NK cells, neutrophiles, . . ) after activation by lipopolysacharids binded to plasma protein- complex binds to CD 14 on the macrophage surface – causes releasing of TNF α n TNF α – participates on early phase of inflammation, induces expression of adhesive molecules on endothelial cells and leukocytes; stimulates proinflammatory protein production; stimulates catabolic processes n TNF β- produced by T and B cells; similar n

Antiinflammatory cytokines IL-10 – produced by Th 2 cells, monocytes, macrophages, activated B cells; inhibition of cytokine Th 1, Tc and NK cells production; inhibition of synthesis proinflammatory cytokines by macrophages n TGF-β – growth activator but also inhibitor of different cell types n Regulates damaged tissues reparation by stimulation of intercellular substances synthesis, modulate expression of tissue metaloproteases and tissue inhibitors of proteolytic enzymes; regulates cell adhesion; chemoatractant of fibroblasts; can inhibite T and B cell proliferation n IL-4 n

CYTOKINES with activity of growth factors n n n IL-2, IL-4, IL-5, IL-6, IL-9, IL-14 SCF- stimulates stem cell proliferation, their release to the peripheral blood IL-3 – influences maturation of all cell lines IL-7 – growth factor of T cells IL-11 – growth factor of megakaryocytes IL-15 – induces proliferation of mast cells, Th and Tc cells

CYTOKINES with activity of growth factors n G-CSF, M-CSF, GM-CSF – stimulate granulocytes and/or monocytes/macrophages proliferation and differentiation, prolongate their survival and increase their functional capacity during inflammation n EPO = erythropoetin- stimulates red cells differentiation
CYTOKINE participating in humoral response of IS IL-4 – produced by Th 2 cells, mast cells and basophils; stimulates B cell proliferation, production of Ig. M, G 1, E; stimulates T cell proliferation; activates macrophages; growth factor of mast cells (antiinflammatory effect) n IL-13 – see IL-4 + chemotactic factor for monocytes and macrophages n IL-5 – produced by Th 2 cells, lymphocytes and mast cells; activates and stimulates B cells and eosinophils proliferation, stimulates Tc cells n IL-9 – produced by Th 2 cells; co-stimulating factor - amplifies Th cells and mast cells proliferation n
CYTOKINES participating in cell mediated response IL-2 – produced by Th cells after stimulation by antigen, autocrine effect to Th cells; activating signal for Tc cells and NK cells; 2. signal for activation and differentiation of B cells n IL-12 – produced by monocytes, macrophages; stimulates maturation Th 0 into Th 1 cells; activates NK cells; stimulates INFγ production by Th 1 cells; inhibites Ig. E secretion n IFN-γ, GM-CSF n

CYTOKINE with antiviral effect Interferons- anti-inflammatory, anti-prolifferative n IFN-α, IFN-β - produced by cells with nucleus after stimulation – viruses - IFN (after binding to the receptor) induces in noninfected cell status of non-permisivity = decomposition of viral nucleus acids and influence into translation of viral proteins n IFN- α = represents 20 cytokines – differ by glycosylation of general protein structure; produced by leukocytes - in recombinant form – therapy of chronic active hepatitis B, hepatitis C n

Receptors for cytokines Consist of 2 -3 subunits n 1 - binds cytokine n Others mediate contact with intracellular signaling molecules n Results of signalisation: stimulation of cell mitosis, differentiation, initiation of effector functions (degranulation, secretion of cytokines, activation of membrane enzymes, chemotaxis), inhibition of cell mitosis and induction of apoptosis n

Signaling process n RECEPTORS of CYTOKINES are associated with: Protein-kinases- phosphorylate intracellular substances (after activation )- influence transcription of genes, structure of cytoskelet n G-proteins – iniciate phosphorylation (after cytokine binding to the receptor) – catalyze the replacement of GDP (guanyl diphosphate) to GTP and can activate a variety of cytoplasmic enzymes n Calcium ions – open Ca channels (after cytokine binding to the receptor) – increase of Ca ions concentration in the cytoplasma - activation of proteins by ca ions binding n
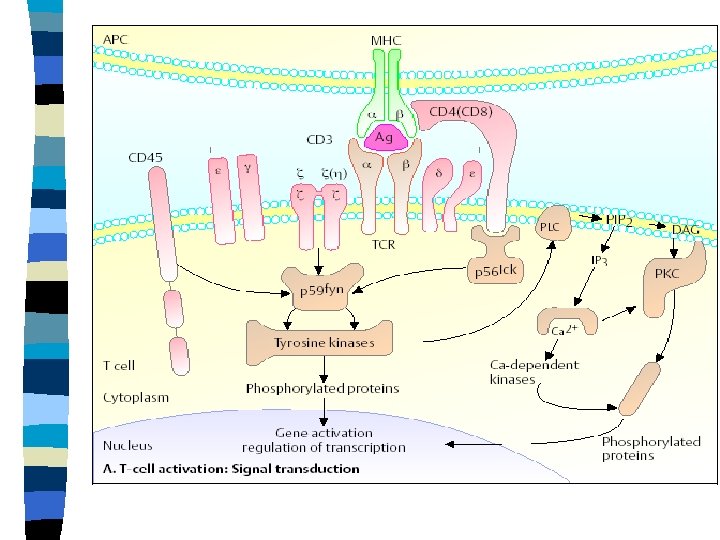

Regulation of local concentration of cytokines n Biological effects are neutralized by binding to nature inhibitors and soluble forms of receptors for cytokines n MMP (matrix metaloproteases) release cytokines from molecules of intercellular substance n Elastases release binded cytokines

29. Physiological mechanisms of regulation of the immune system.

Immune mechanisms of regulation Immune system is regulated by: n Antigen n Antagonistic peptid n Antibodies n Cytokines and intercellular contact n T lymphocytes n Neuroendocrine regulation

REGULATION BY ANTIGEN Antigen competition – peptides from different antigens compete for binding-sites on the MHC gp = antigen is able to suppress expression of other antigen IMPORTANT IS : n the binding strenght of peptide to MHC gp II n density of peptid-MHC gp II complex on the surface of APC Immune response finishes after extinction of antigen – due to a short life-span of effector lymphocytes n

ANTAGONISTIC PEPTIDES Agonists - peptide fragments of antigen with adequate binding to MHC gp, recognition by T cells with sufficient affinity – induce full response of T cells n Partial agonists – induce a qualitative different response of T cells - peptides have a similar structure, bind adequately to MHC gp, but make too weak or too strong interaction with T cells n Antagonists – induce anergy of T cells n

REGULATION MEDIATED BY ANTIBODIES Antibodies have an effector and regulatory functions n Secreted antibodies – compete with BCR for antigen = negative regulators of B cells stimulation n Immune complexes of antibody and antigen – bind to the surface of B cells – interaction of signaling molecules (proteinkinases, protein-phosphatases) = inhibit B cells activation (= antibody feedback) n

REGULATION MEDIATED BY CYTOKINES AND INTERCELLULAR CONTACT Inhibition of cytokine effect by endocytosis of their receptors or by binding of inhibitors to their receptors n Inhibitory receptors – protection against too easy T cells activation n Apoptotic receptor (Fas) mediates a negative regulation after binding to ligand Fas. L on activated T cells – causes – lysis of cell n

NEGATIVE REGULATION mediated by T lymphocytes Th 2 cells produce IL-4, IL-10 - suppress immune response of Th 1 cells n Suppression of T cells occurs after recognition an antigen on cells different from APC (missing of co-stimulating signals) n CD 8+ T cells – secrete soluble forms of TCR - compete with TCR on the surface of other cells- inhibition n Regulatory Tr 1 cells (CD 4+)- secrete IL-10 anti-inflammatory effect, induce tolerance to autoantigens n

NEUROENDOCRINE REGULATION n n n Neurotrasmiters influence leukocytes by binding to the specific receptors (noradrenalin) CS, growth hormons, thyroxin, endorfins – influence the leukocytes by binding to the specific receptors Leukocytes produce endorfins, TSH, growth hormon, vitamin D 3, ACTH Cytokines influence nerve system (IL-1, IL-6) Stress influences immune systemcortocosteroids-activity of phagocytes, NK cells

OTHER FACTORS n n n The same antigen can induce active immune response or active tolerance – depends on: Condition of immune system Character of antigen (size, structure of molecule) Dose of antigen (too low or too high dosesinduce tolerance) Route of antigen administration (s. c. induce immune response, p. o. or i. v. - induce tolerance)

32. HLA system, genetic background. HLA typing.

MHC (major histocompatibility complex) n human MHC = HLA (human leukocyte antigens) n Genes of MHC complex – are codominantly expressed = alleles inherited from both parents are expressed equally; are polymorphic – many different alleles are present

Contain of MHC complex n MHC gp = are encoded by genes localized on short arm of human 6. chromosome n The MHC locus- contains 4 single blocks of loci - HLA Ags I are encoded by loci A, B, C - HLA Ags II – locus D - HLA Ags III – locus between HLA I a II (contains genes with nondirected participation in histocompatibility- genes for complement, TNF…)

Polymorphism of MHC gp A lot of different forms of alleles (of each isotype) exist in the population n Forms of alleles differ in 1 or more amino acids in their binding-site for peptide n Importance of polymorphism: - positive – allows to bind a lot of types of peptides - negative – complicates transplantation n

MHC gp The MHC was discovered as the genetic locus that is the principal determinant of acceptance or rejection of tissue grafts exchanged between individuals. n Individuals that are identical at their MHC locus will accept grafts from one another n Individuals that differ at their MHC loci will reject such grafts n

Function of MHC gp n Physiologic function of MHC molecules is to display peptides derived from protein antigens to antigen- specific T lymphocytes: n bind peptides n transport peptides to the cell surface n display peptides to T lymphocytes

Classification of MHC gp n MHC gps class I - display intracellular proteins to CD 8+ T lymphocytes n MHC gps class II - display extracellular proteins to CD 4+ T lymphocytes

HLA typing The combination of class I and class II antigens expressed by a person is called his/her HLA phenotype. n The combination of class I and class II alleles is the HLA genotype. In most cases, the genotype reflects the phenotype. n

HLA typing n HLA typing identifies a person's HLA type and, therefore, helps to characterize the immune function of that person. n Different loci and different levels of resolution are required for different clinical applications

HLA typing is routinely used for : n matching donors and recipients in solid organ or hematopoietic stem cell transplantation n helping in the diagnosis of certain autoimmune or anti-inflammatory diseases n determining eligibility of patients to tumor vaccination protocols when the vaccine is HLA-allele dependent

HLA typing The peripheral blood lymphocytes from the indiviual are incubated with antibodies that are known to react with specific HLA molecules and complement. n If there is lysis of the cells, that individual carries the HLA protein recognized by that specific antibody. n

HLA typing n Molecular techniques can now be used to type HLA molecules. n PCR using primers that amplify only certain HLA sequences allow accurate identification of HLA types. n This has the advantage of not requiring the preparation of live cells from the individual to be typed.

30. HLA system, 1 st class molecules, their structure andfunction

MHC gps Ist class Expressed on all nucleated cells n Display intracellular proteins n isotypes of clasic HLA Ist class: HLA- A, - B, - C n isotypes of nonclasic HLA Ist class: HLA- E, - F, G n molecules at structure similar to MHC gp Ist class : CD 1 n

Structure of MHC gp Ist class n 2 polypeptide chains (noncovalent association): - transmembrane chain alfa: subunits alfa -1, -2, -3 - ß 2 - microglobulin (noncovalent binding) n binding site for peptides: N-terminal domain between subunits alfa 1 and 2
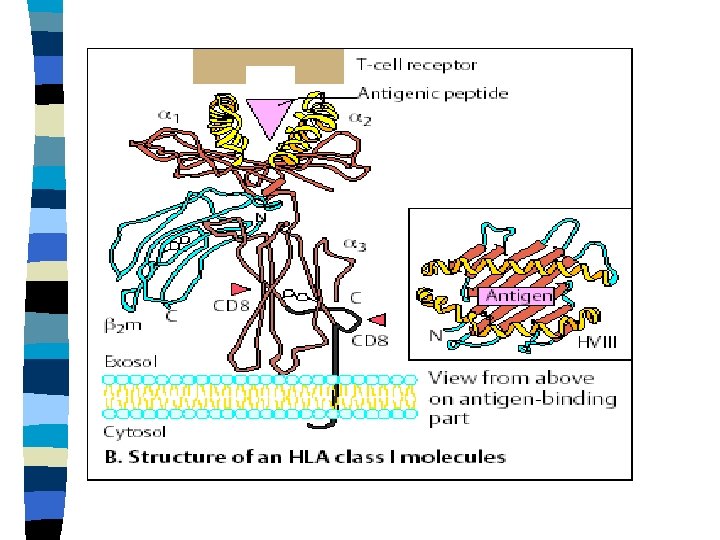
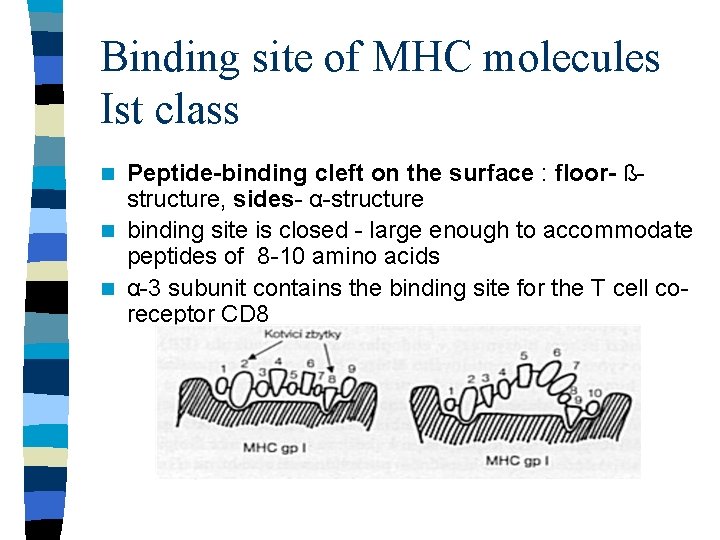
Binding site of MHC molecules Ist class Peptide-binding cleft on the surface : floor- ßstructure, sides- α-structure n binding site is closed - large enough to accommodate peptides of 8 -10 amino acids n α-3 subunit contains the binding site for the T cell coreceptor CD 8 n

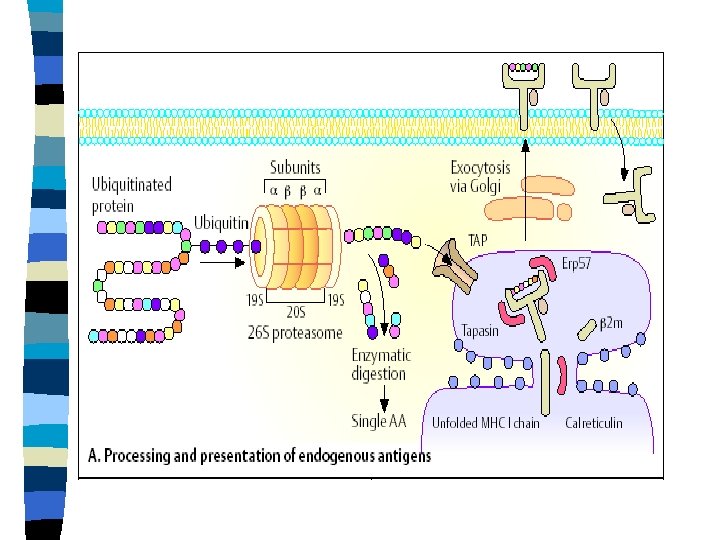
Processing of internalized antigens (MHC gp Ist class) n n n MHC gps Ist class are synthesized in the ER Proteins can be produced in the cytoplasm from viruses inside infected cells, from mutated or altered host genes, as in tumors- all targeted for destruction by proteolysis Proteins are covalently tagged with small peptide called ubiquintin in proteasome- proteins are degraded TAP = transporters associated with antigen processing binds peptides, enters the ER, binds to MHC gps class I Complex is transported to the Golgi complex- TAP dissociates and complex of MHC gp class I + peptide is transported to the cell surface and recognized by CD 8+ T lymphocytes

31. HLA system, 2 nd class molecules, their structure and function
MHC gps II class n Expressed on APC (dendritic cells, monocytes, macrophages, B lymphocytes) n Isotypes HLA-DR, -DQ, -DP n Display extracellular peptides to T lymphocytes

Structure of MHC gp IInd class n 2 transmembrane subunits: - transmembrane chain alfa consists of 2 subunits (alfa 1 a 2) - transmembrane chain beta consists of 2 subunits (beta 1 a 2) - binding-site for peptides: N- terminal domain between subunits alfa 1 and beta 1
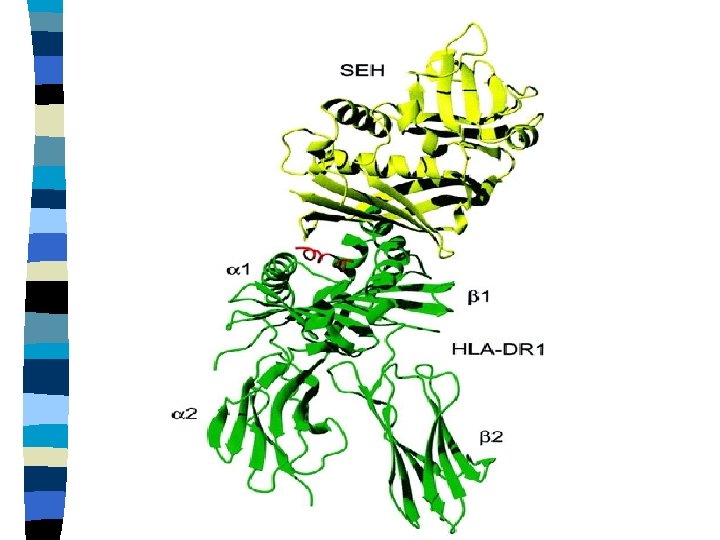

Binding-site of MHC gp IInd class Binding-site is opened n Cleft is large enough to accommodate peptides of 15 -35 - amino acids n β- 2 domain contains binding-site for the T cell coreceptor CD 4 n

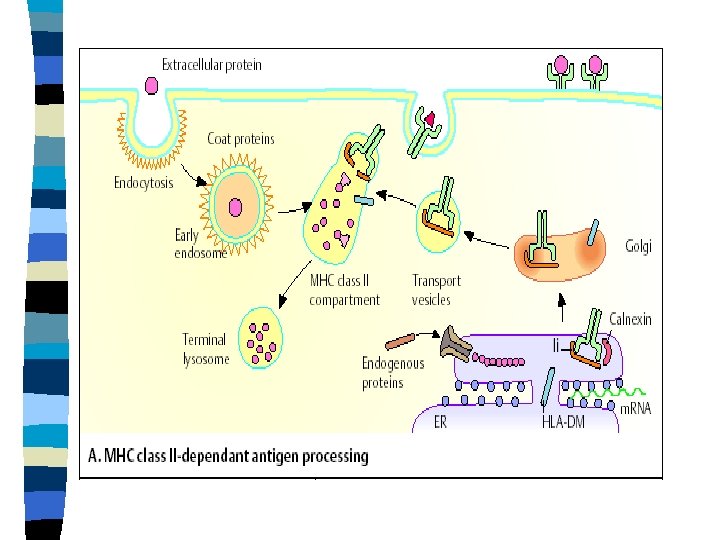
Processing of internalized antigens (MHC gp IInd class) MHC gps II are synthesized in endoplasmic reticulum – carry with invariant chain that contains a sequence – CLIP = binds to the peptide binding cleft- transport vesicle n The microbial proteins enter intracellular vesicles (endosomes) – proteins are broken down by enzymes n Endosome fuses with transport vesicle – CLIP is removed – the cleft accepts the peptide, MHC gps IInd class and peptide are transported to the cell surface where are recognized by CD 4+ T cells n

MHC restriction n. T lymphocytes recognize a foreign peptide antigen only when it is bound to MHC gp

Nonclasic MHC gps I class n expressed only on some cells n Specialize to binding of specific ligands n HLA-G is expressed on the surface of trophoblast cells n complexes HLA-E, -G with peptides are recognized by inhibitory receptors of NK cells – induce tolerance of fetus in uterus
- Slides: 75