n Lymphoma Malignancy of Lymphocytes n Lymphocytes Bcells

n Lymphoma : Malignancy of Lymphocytes n Lymphocytes B-cells T-cells NK-cells (Natural Killer Cells)

Definition The term "malignancy" refers to cancerous cells that have the ability to invade and destroy tissues, and / or to metastasize to other sites in the body. There may also be changes to the physiology of the organism. n Malignant cells tend to have fast, uncontrolled growth due to changes in their genetic makeup. n

n A malignant clone is a clone of cell that have genomic changes that leads to the malignant state. n However not all genomic changes result in malignant clones.

n Clonal evolution is the further changes in the genome which may result in progression of disease relapse after treatment resistence to standard therapy.

Lymphomas n 10 -20 new case per 100, 000 per year n Deaths 8 per 100, 000 per year Commonest: Diffuse Large B-cell lymphoma Follicular lymphoma CLL Mantle cell lymphoma

Rappaport Lymphoma Classification n 1966 Well-differentiated diffuse lymphocytic lymphoma Poorly differentiated diffuse lymphocytic lymphoma Well differentiated nodular lymphocytic lymphoma Poorly differentiated nodular lymphocytic lymphoma Nodular Histiocytic lymphoma (= large cell lymphoma) Diffuse Histiocytic lymphoma (=large cell lymphoma) Mixed cell lymphoma MORPHOLOGY ONLY

Non-Hodgkin’s lymphoma USA n Lukes and Collins Dorfman n Kiel (Lennert) Germany n WHO Geneva UK n Hodgkin’s lymphoma n Lukes-Butler n Rye Nodular sclerotic Lymphocyte predominent Mixed cellularity Lymphocyte depleted

Lukes and Collins (1974) I. Unidentified Cell Type II. T-cells Mycosis fungoides and Sezary, convoluted lymphocyte Immunoblastic sarcoma of T-cells. III. B-cells Small lymphocytic Plasmacytoid lymphocyte Follicular center cell (FCC types; follicular, diffuse, follicular and diffuse, sclerotic) small cleaved large cleaved small non-cleaved Large non-cleaved Immunoblastic IV Histiocytic type V Unclassifiable

Updated Kiel B- cell Low Grade n n Lymphocytic. CLL, prolymphocytic, hairy cell lymphoma Lymphoplasmacytic/lymphoplasmactoid Medium Grade n n n Plasmacytic Centroblastic/centroblastic T-cell n n n Lymphocytic CLL, prolymphocytic Lymphoepitheloid Angioimmunoblastic T-zone Pleomorphic small cell Pleomorphic medium and large High Grade n Centroblastic Immunoblastic Large cell anaplastic Burkitt’s lymphoma Lymphoblastic n Rare types n n n Immunoblastic Large cell naplastic n Lymphoblastic n n Rare types

Working Formulation n Low Grade ¨ ¨ ¨ n Intermediate grade ¨ ¨ n Malignant Lymphoma, follicular, predominantly large cell Malignant Lymphoma, diffuse, small cleaved cell Malignant Lymphoma, diffuse, mixed small and large cell Malignant Lymphoma, diffuse, large cell High grade ¨ ¨ ¨ n Malignant Lymphoma, small lymphocytic (chronic lymphocytic leukemia) Malignant Lymphoma, follicular, predominantly small cleaved cell Malignant Lymphoma, follicular, mixed (small cleaved and large cell) Malignant Lymphoma, large cell, immunoblastic Malignant Lymphoma, lymphoblastic Malignant Lymphoma, small non-cleaved cells (Burkitt's lymphoma) Miscellaneous ¨ ¨ ¨ Composite Mycosis fungoides Histiocytic Extramedullary plasmacytoma Unclassifiable
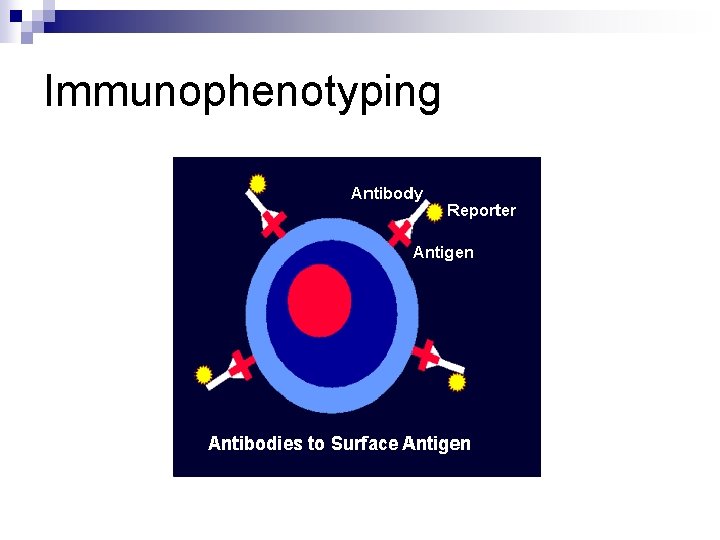
Immunophenotyping


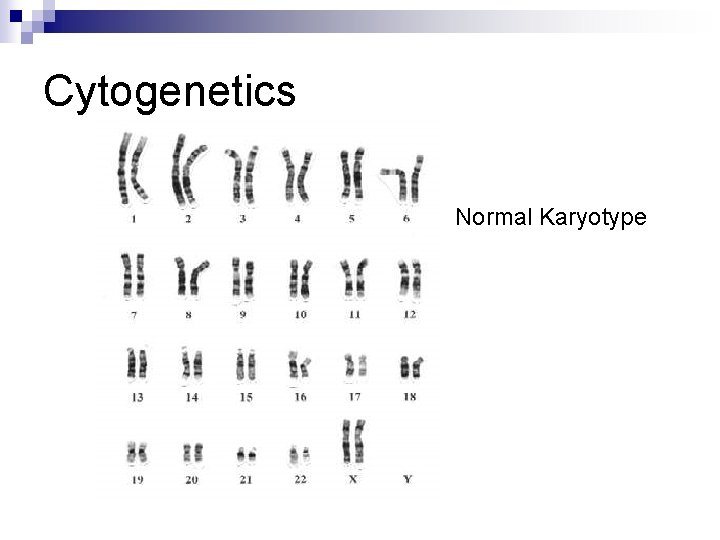
Cytogenetics Normal Karyotype
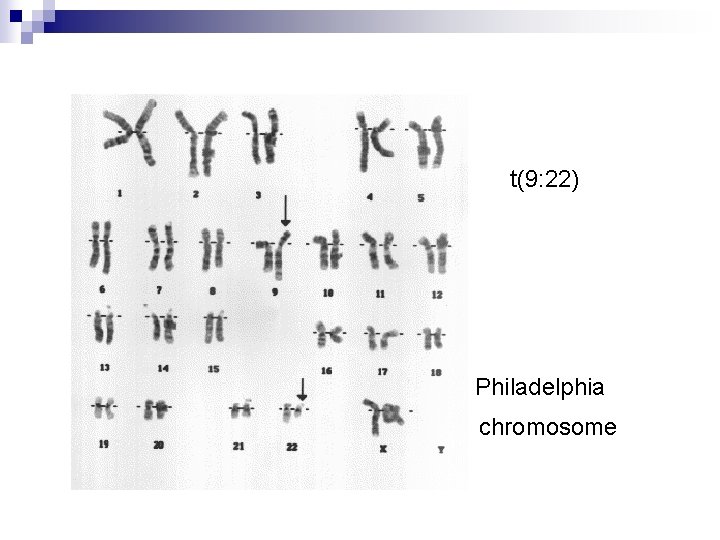
t(9: 22) Philadelphia chromosome
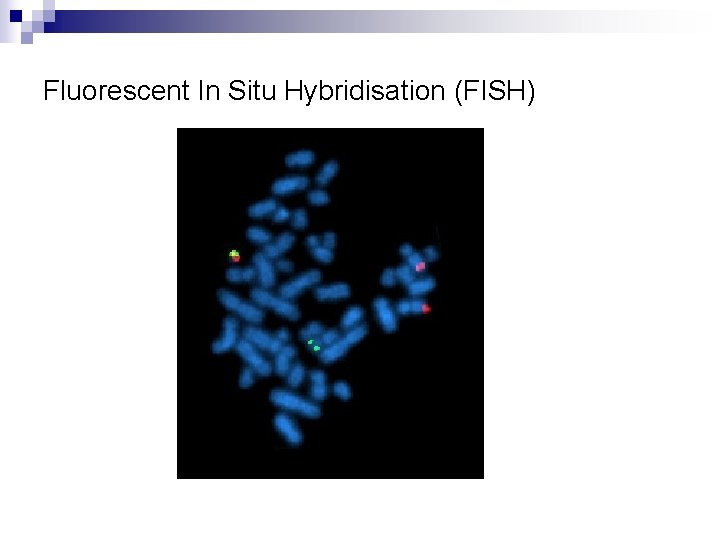
Fluorescent In Situ Hybridisation (FISH)

The Revised European American Lymphoma Classification (REAL) 1994 n I. Precursor B-cell neoplasm: n Precursor B-lymphoblastic leukemia/lymphoma n n n n B-cell chronic lymphocytic leukemia / small lymphocytic lymphoma B-cell prolymphocytic leukemia Lymphoplasmacytic lymphoma Splenic marginal zone B-cell lymphoma (+/- villous lymphocytes) Hairy cell leuekmia Plasma cell myeloma/plasmacytoma Extranodal marginal zone B-cell lymphoma of mucosa-associated lymphoid tissue type Nodal marginal zone lymphoma (+/- monocytoid B-cells) Follicle center lymphoma, follicular, Mantle cell lymphoma Diffuse large cell B-cell lymphoma Mediastinal large B-cell lymphoma Primary effusion lymphoma Burkitt's lymphoma/Burkitt's cell leukemia n n II. Mature (peripheral) B-cell neoplasms ¨ T-Cell and Natural I. Precursor T cell neoplasm: Killer Cell Neoplasms n Precursor T-lymphoblastic lymphoma/leukemia n n n n T-cell prolymphocytic leukemia T-cell granular lymphocytic leukemia Aggressive NK-Cell leukemia Adult T cell lymphoma/leukemia (HTLV 1+) Extranodal NK/T-cell lymphoma, nasal type Enteropathy-type T-cell lymphoma Hepatosplenic gamma-delta T-cell lymphoma Subcutaneous panniculitis-like T-cell lymphoma Mycosis fungoides/Sézary's syndrome Anaplastic large cell lymphoma, T/null cell, primary cutaneous type Peripheral T cell lymphoma, not otherwise characterized Angioimmunoblastic T cell lymphoma Anaplastic large cell lymphoma, T/null cell, primary systemic type n n n Nodular lymphocyte predominance Hodgkin's lymphoma Classical Hodgkin's lymphoma Nodular sclerosis Hodgkin's lymphoma Lymphocyte-rich classical Hodgkin's lymphoma Mixed cellularity Hodgkin's lymphoma Lymphocyte depletion Hodgkin's lymphoma n II. Mature (peripheral) T cell and NK-cell neoplasms ¨ Hodgkin lymphoma (Hodgkin Lymphoma)
WHO classification 2002 ¨ Mature B cell neoplasms n n n n Chronic lymphocytic leukemia/Small lymphocytic lymphoma B-cell prolymphocytic leukemia Lymphoplasmacytic lymphoma (such as Waldenström macroglobulinemia) Hairy cell leukemia Splenic marginal zone lymphoma Extranodal marginal zone B cell lymphoma , also called MALT lymphoma Nodal marginal zone B cell lymphoma (NMZL) Follicular lymphoma Mantle cell lymphoma Diffuse large B cell lymphoma Mediastinal (thymic) large B cell lymphoma Intravascular large B cell lymphoma Primary effusion lymphoma Burkitt lymphoma/leukemia n n n n T cell prolymphocytic leukemia T cell large granular lymphocytic leukemia Aggressive NK cell leukemia Adult T cell leukemia/lymphoma Extranodal NK/T cell lymphoma, nasal type Enteropathy-type T cell lymphoma Hepatosplenic T cell lymphoma Blastic NK cell lymphoma Mycosis fungoides / Sezary syndrome Primary cutaneous CD 30 -positive T cell lymphoproliferative disorders Primary cutaneous anaplastic large cell lymphoma Lymphomatoid papulosis Angioimmunoblastic T cell lymphoma Peripheral T cell lymphoma, unspecified Anaplastic large cell lymphoma n n n Classical Hodgkin lymphomas: Nodular sclerosis Mixed cellularity Lymphocyte-rich Lymphocyte depleted or not depleted Nodular lymphocyte-predominant Hodgkin lymphoma n n n Associated with a primary immune disorder Associated with the Human Immunodeficiency Virus ( HIV) Post-transplant Associated with methotrexate therapy Primary central nervous system lymphoma occurs most often in immuno-compromised patients, in particular those with AIDS, but it can occur in the immunocompetent as well. It has a poor prognosis, particularly in those with AIDS. Treatment can consist of corticosteroids, radiotherapy, and chemotherapy, often with methotrexate. ¨ ¨ ¨ Mature T cell and natural killer (NK) cell neoplasms Hodgkin lymphoma Immunodeficiency-associated lymphoproliferative disorders

WHO Classification 2008 n 98 lymphoma entities
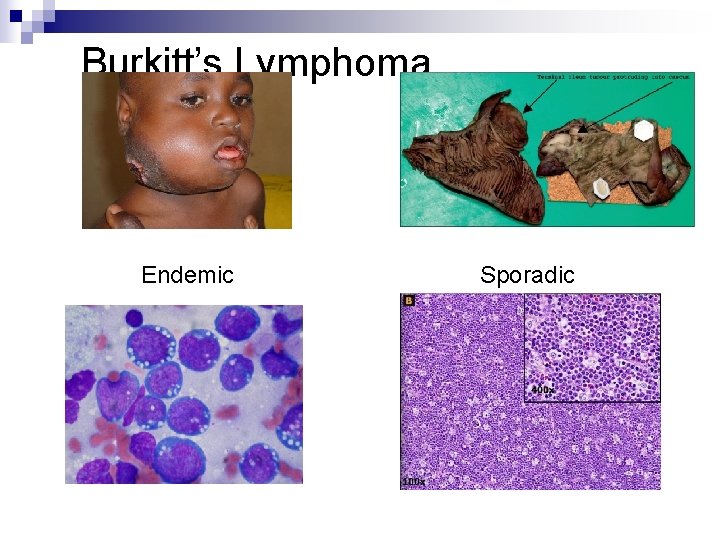
Burkitt’s Lymphoma Endemic Sporadic
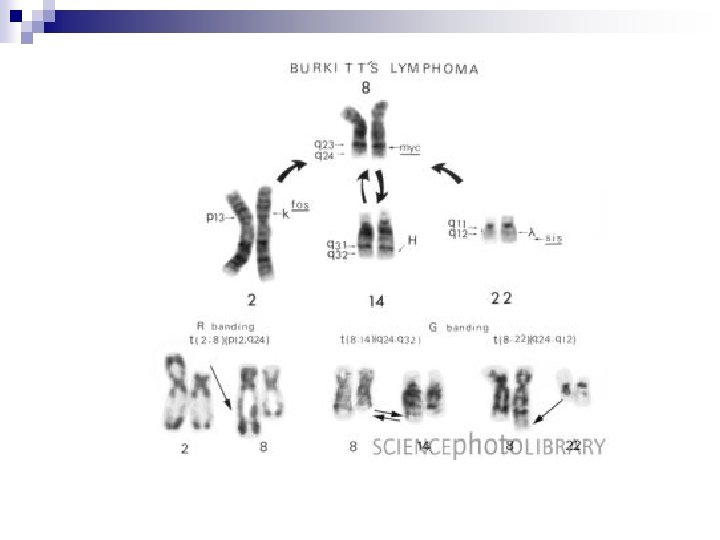

c-myc oncogene Regulator of 15% of genes, some of which are involved in cell replication.
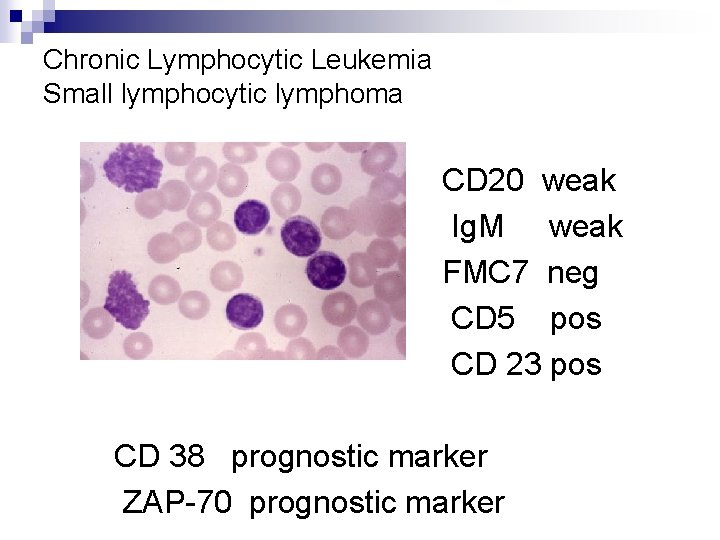
Chronic Lymphocytic Leukemia Small lymphocytic lymphoma CD 20 weak Ig. M weak FMC 7 neg CD 5 pos CD 23 pos CD 38 prognostic marker ZAP-70 prognostic marker

CLL Staging n n Stage 0 (LOW RISK) Lymphocytosis >5, 000/mm 3 without adenopathy (enlarged lymph nodes), hepatosplenomegaly (enlarged spleen), anemia (low red blood cells), or thrombocytopenia (low platelets). n Stage I (INTERMEDIATE RISK) lymphadenopathy n Stage II (INTERMEDIATE RISK) hepatomegaly or splenomegaly with or without lymphadenopathy n Stage III (HIGH RISK) Hb < 11. 0 g/d. L, n Stage IV (HIGH RISK) low platelets < 100, 00/mc. L

FISH 17 pn 11 qn Normal n Trisomy 12 n 13 qn 6 qn 14 q 32 n 32 mths 79 mths 111 mths 114 mths 133 mths Good prognosis Poor prognosis

n Low-risk CLL People in this group are often diagnosed based on a high lymphocyte count in the blood but otherwise have normal blood counts and do not have enlarged lymph nodes or organs. The prognosis (outlook) for people in this group is often very good, with long survival expected. n Most people can be observed with careful and frequent follow-up exams. Treatment is considered if there are signs that the leukemia is progressing or if a person develops bothersome symptoms. When needed, initial treatment is usually chemotherapy (chemo) often combined with a monoclonal antibody targeting CD 20 like rituximab (Rituxan).

n Patients with high-risk CLL (stages III and IV) are more likely to need immediate treatment. n When treatment is needed, there are many options. What treatment is used will depend on factors like the patient's health, possible side effects, the reason treatment is needed, and any need for a rapid response. Commonly used treatments include: ■FCR: fludarabine (Fludara), cyclophosphamide (Cytoxan), and rituximab ■Bendamustine (sometimes with rituximab) ■FR: fludarabine and rituximab ■CVP: cyclophosphamide, vincristine, and prednisone (sometimes with rituximab) ■CHOP: cyclophosphamide, doxorubicin, vincristine (Oncovin), and prednisone ■Chlorambucil ■PCR: pentostatin (Nipent), cyclophosphamide, and rituximab ■Alemtuzumab (Campath) Anti-CD 52 ■Fludarabine (alone)
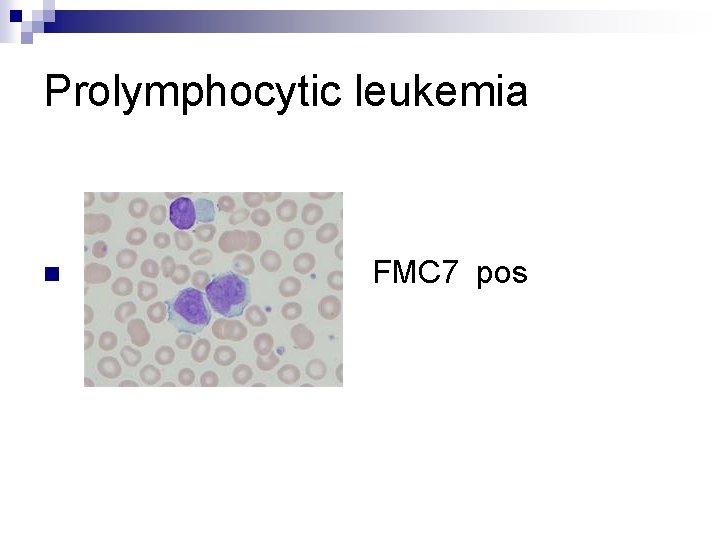
Prolymphocytic leukemia n FMC 7 pos
Lymph node
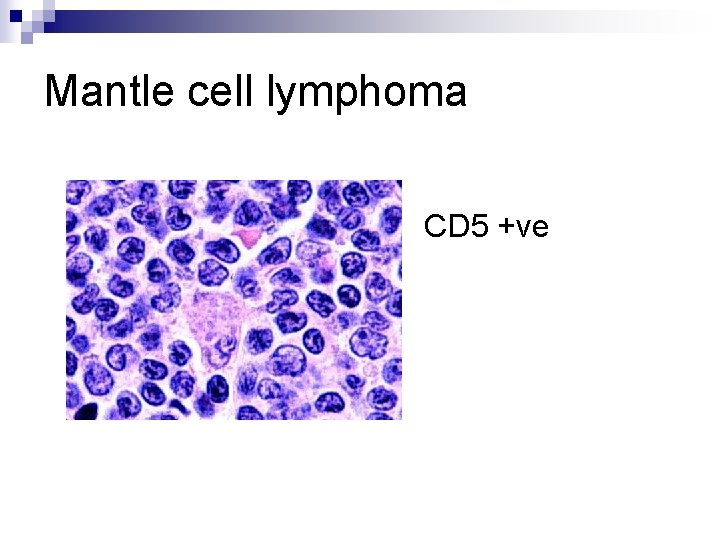
Mantle cell lymphoma CD 5 +ve
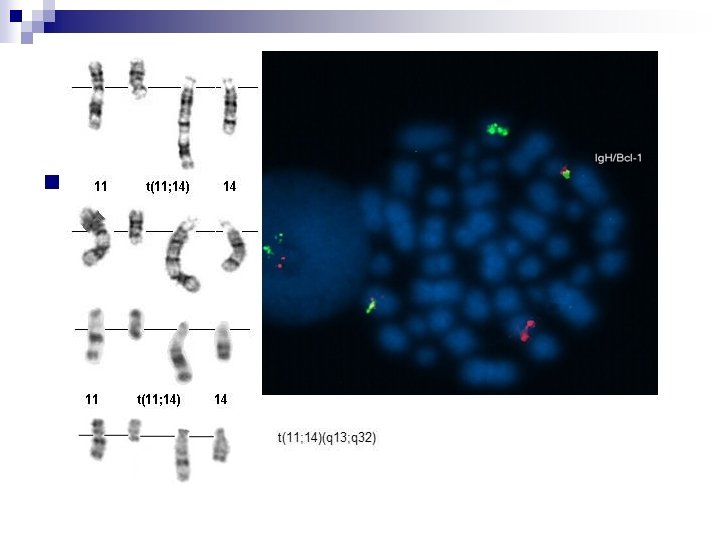
n
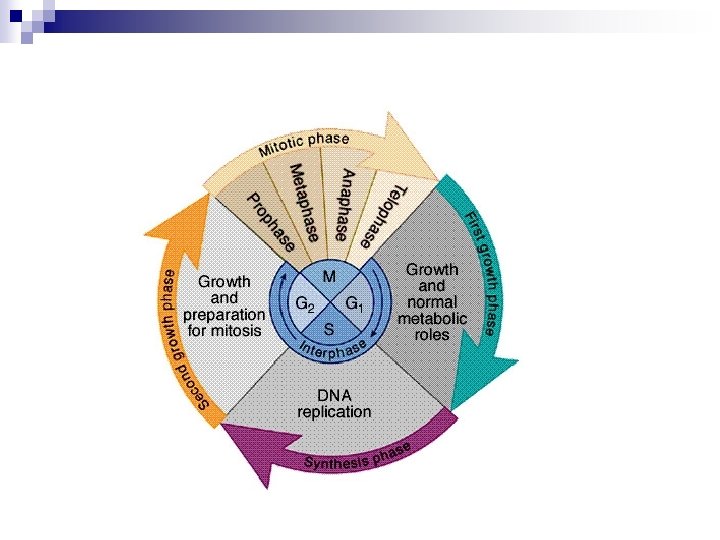
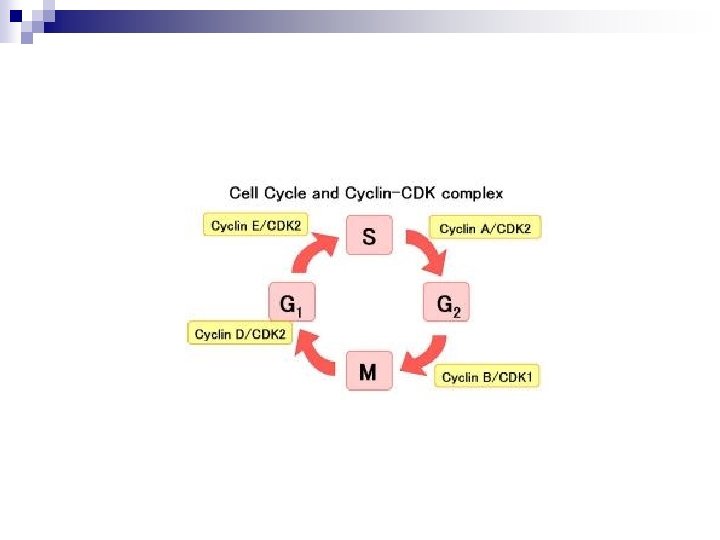
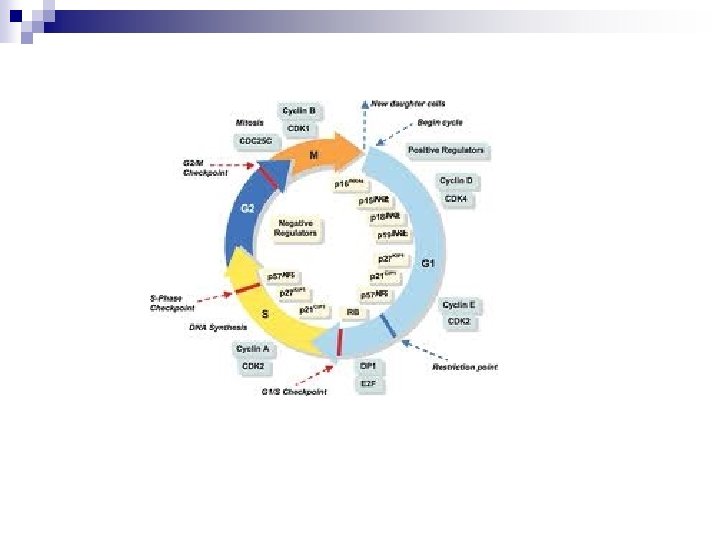

MC treatment n CHOP (hyper VCAD) n Proteosome inhibitors n Stem cll transplant
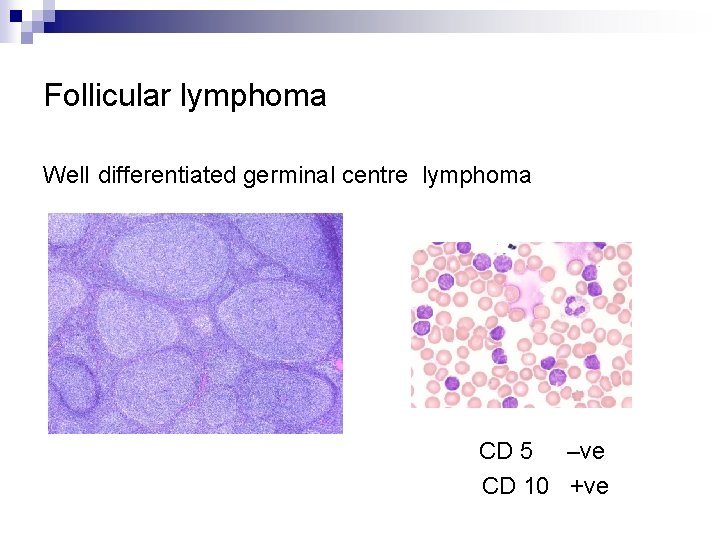
Follicular lymphoma Wel. I differentiated germinal centre lymphoma CD 5 –ve CD 10 +ve

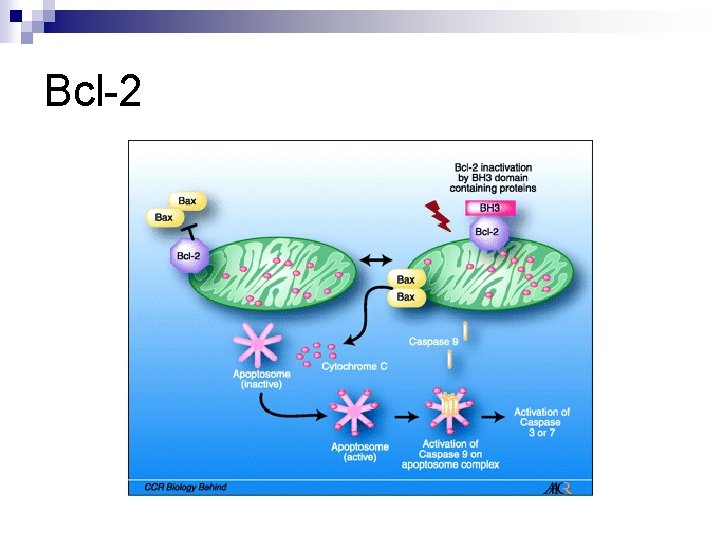
Bcl-2
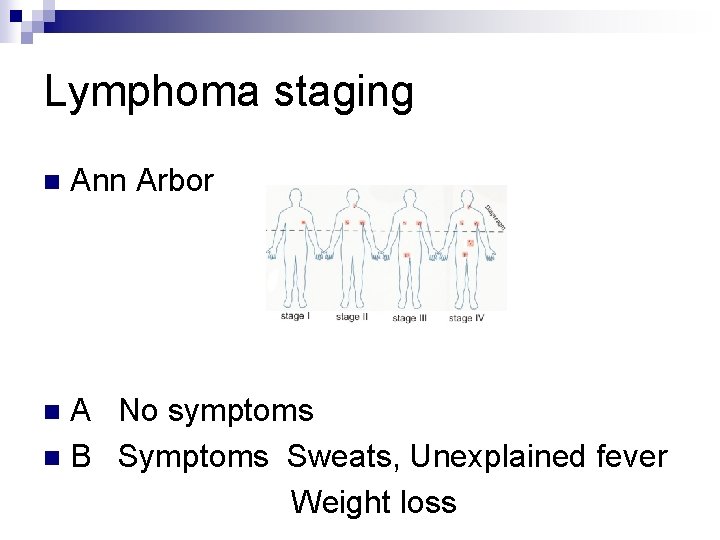
Lymphoma staging n Ann Arbor A No symptoms n B Symptoms Sweats, Unexplained fever Weight loss n

FL treatment n CLL type combinations n FMDR Fludarabine Mitoxanthrone Dexamethasone Rituxamab
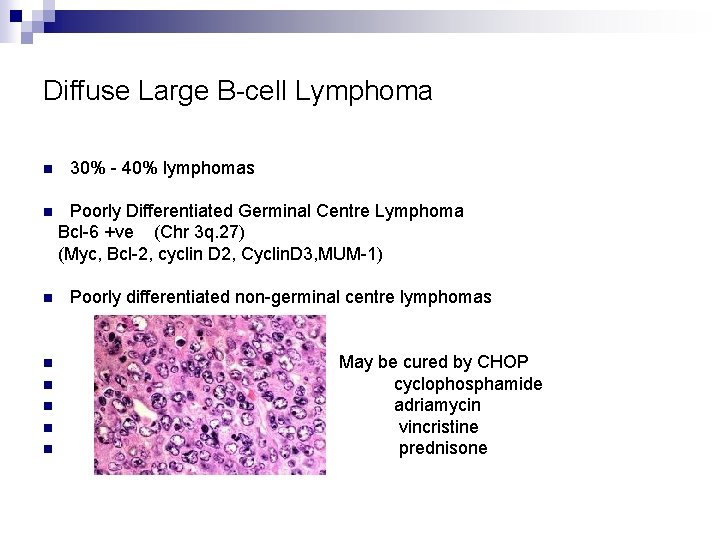
Diffuse Large B-cell Lymphoma n n n n 30% - 40% lymphomas Poorly Differentiated Germinal Centre Lymphoma Bcl-6 +ve (Chr 3 q. 27) (Myc, Bcl-2, cyclin D 2, Cyclin. D 3, MUM-1) Poorly differentiated non-germinal centre lymphomas May be cured by CHOP cyclophosphamide adriamycin vincristine prednisone
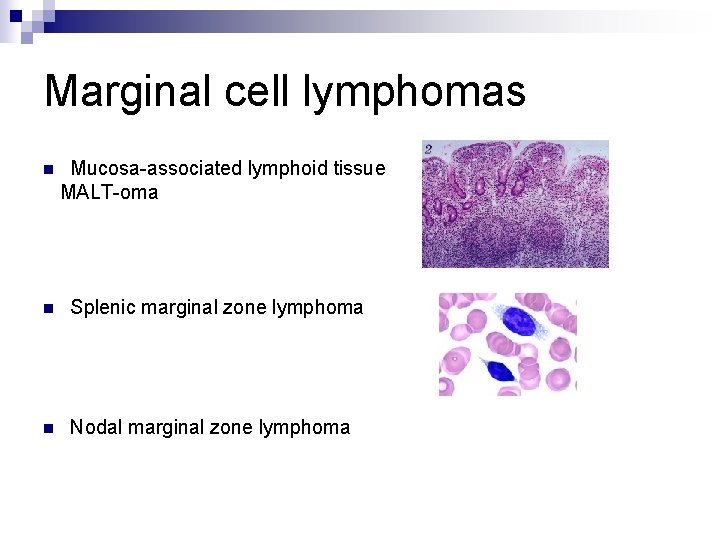
Marginal cell lymphomas n Mucosa-associated lymphoid tissue MALT-oma n Splenic marginal zone lymphoma n Nodal marginal zone lymphoma

Gastric MALTOMA Helicobactor pylori nearly always present. Virulence factor Cag. A may be required for the continued growth of the lymphoma Japanese have shown triple antibiotic therapy for H. pylori will result in regression of the lymphoma. (amoxicillin, clarithromycin, omeprazole)

Other Maltomas n Associated with Autoimmune Disease n Thyroid Maltoma with Hashimoto’s thyroiditis n Lacrimal and Salivary gland Maltoma associated with Sjrogen’s disease.

MALT FISH PANEL n t(11; 18) in gastric Maltoma n t(14, 18) in lacrimal/salivary gland Maltoma n t(3; 14) in thyroid Maltoma n t(1; 14) in lymph node marginal zone lymphomas
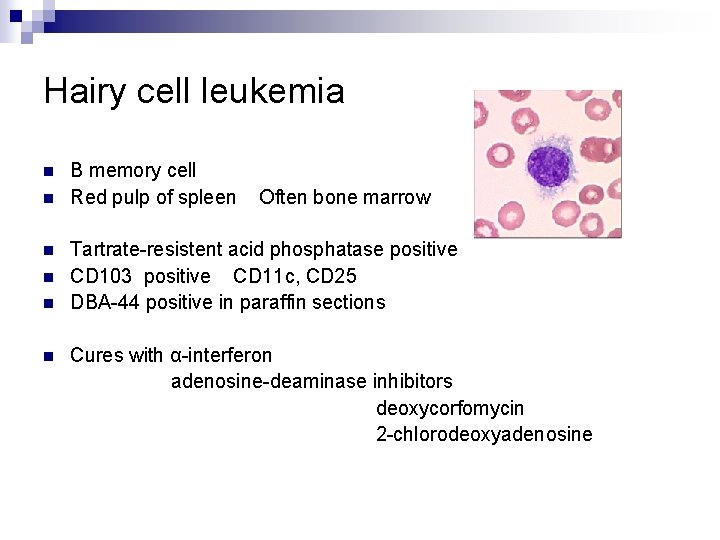
Hairy cell leukemia n n n B memory cell Red pulp of spleen Often bone marrow Tartrate-resistent acid phosphatase positive CD 103 positive CD 11 c, CD 25 DBA-44 positive in paraffin sections Cures with α-interferon adenosine-deaminase inhibitors deoxycorfomycin 2 -chlorodeoxyadenosine
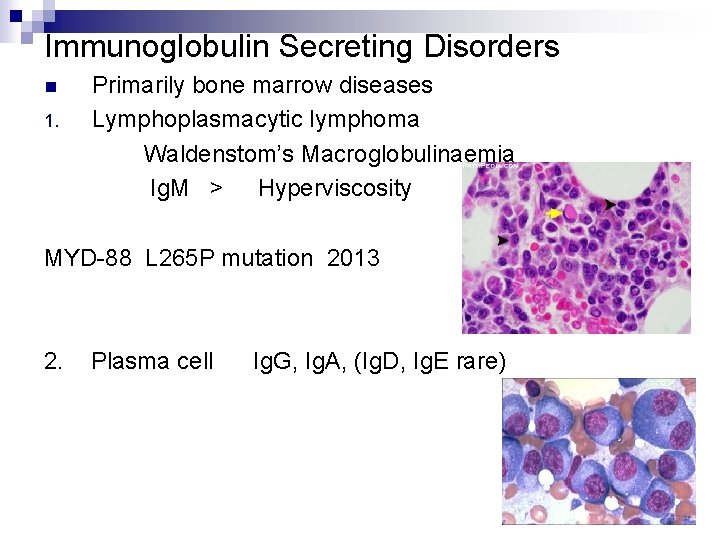
Immunoglobulin Secreting Disorders n 1. Primarily bone marrow diseases Lymphoplasmacytic lymphoma Waldenstom’s Macroglobulinaemia Ig. M > Hyperviscosity MYD-88 L 265 P mutation 2013 2. Plasma cell Ig. G, Ig. A, (Ig. D, Ig. E rare)
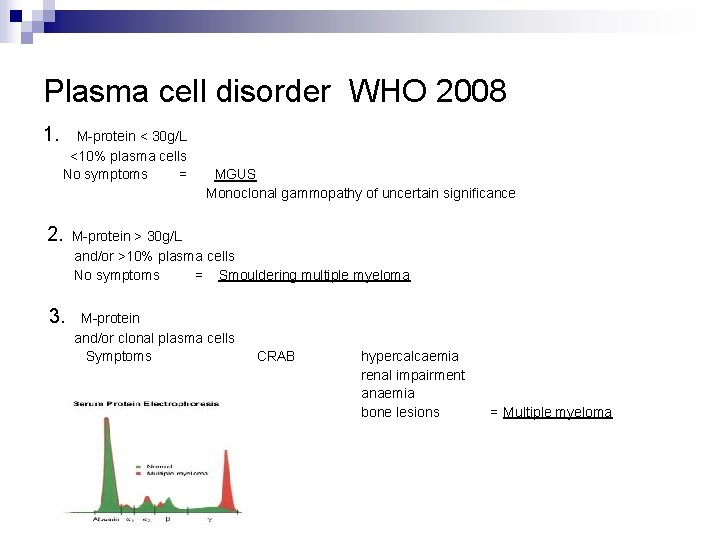
Plasma cell disorder WHO 2008 1. M-protein < 30 g/L <10% plasma cells No symptoms = MGUS Monoclonal gammopathy of uncertain significance 2. M-protein > 30 g/L and/or >10% plasma cells No symptoms = Smouldering multiple myeloma 3. M-protein and/or clonal plasma cells Symptoms CRAB hypercalcaemia renal impairment anaemia bone lesions = Multiple myeloma
Cytogenetics n n Hyperdiploid or not hyperdiploid Translocations Cyclin D 1 and Cyclin D 3 Good Cyclin D 2 Poor

Treatment of Myeloma n Bortezomib, cyclophosphamide, dexamethasone n Thalidomide n PSCT
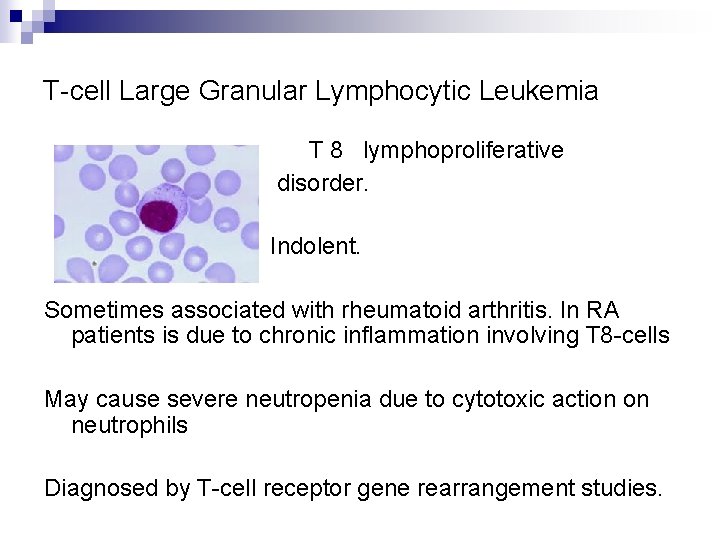
T-cell Large Granular Lymphocytic Leukemia T 8 lymphoproliferative disorder. Indolent. Sometimes associated with rheumatoid arthritis. In RA patients is due to chronic inflammation involving T 8 -cells May cause severe neutropenia due to cytotoxic action on neutrophils Diagnosed by T-cell receptor gene rearrangement studies.
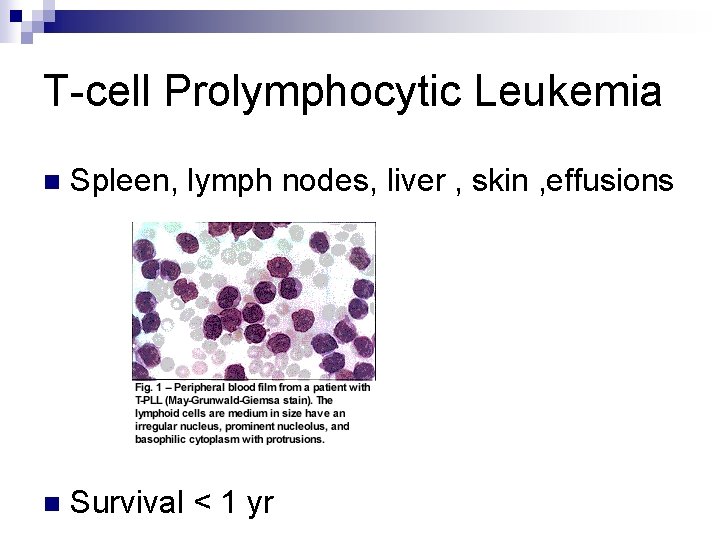
T-cell Prolymphocytic Leukemia n Spleen, lymph nodes, liver , skin , effusions n Survival < 1 yr
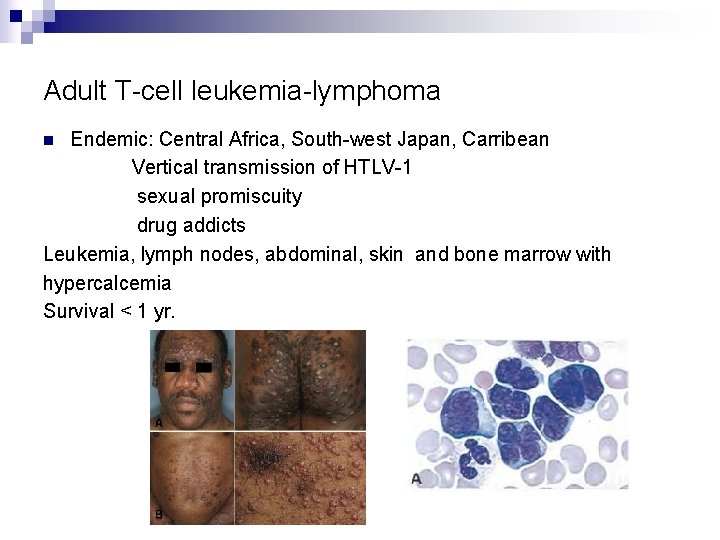
Adult T-cell leukemia-lymphoma Endemic: Central Africa, South-west Japan, Carribean Vertical transmission of HTLV-1 sexual promiscuity drug addicts Leukemia, lymph nodes, abdominal, skin and bone marrow with hypercalcemia Survival < 1 yr. n
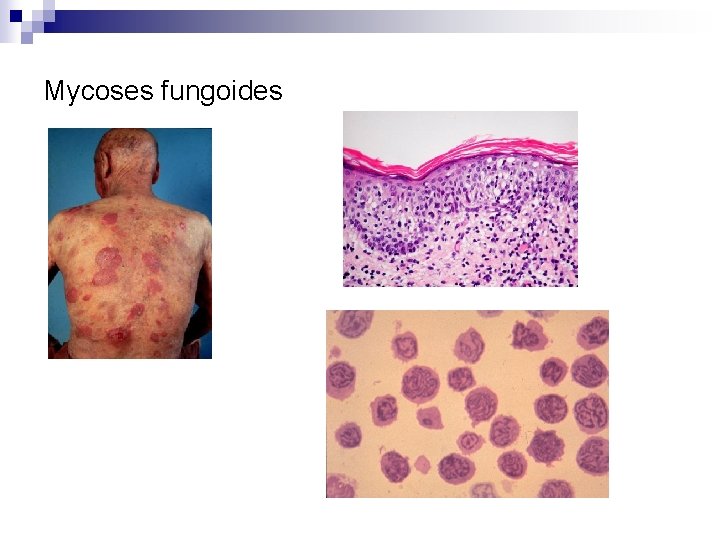
Mycoses fungoides

Enteropathy-associated T-cell lymphoma Associated with refractory coeliac disease n Patient is positive for HLA-DQ 2 or DQ 8 n Associated dermatitis herpatiformis and hyposplenism. n n Aggressive T lymphoma with poor prognosis

Peripheral T-cell lymphomas (NOS) Lymph node , bone marrow, liver, spleen, Other organs n Low 5 year survival rate
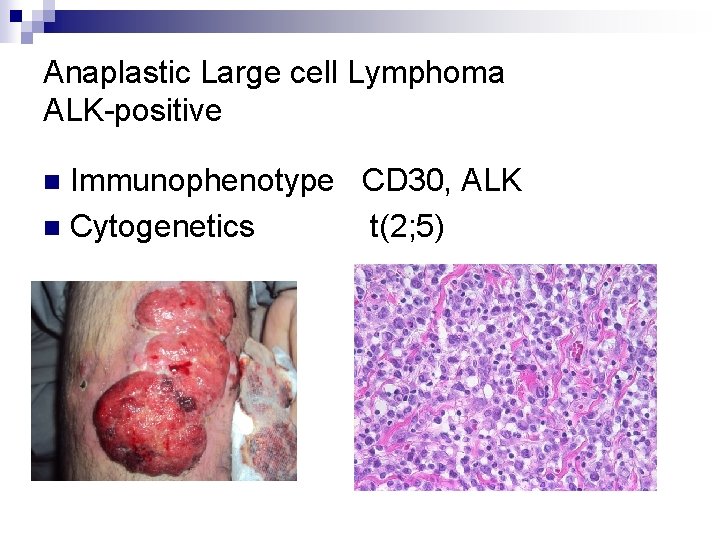
Anaplastic Large cell Lymphoma ALK-positive Immunophenotype CD 30, ALK n Cytogenetics t(2; 5) n
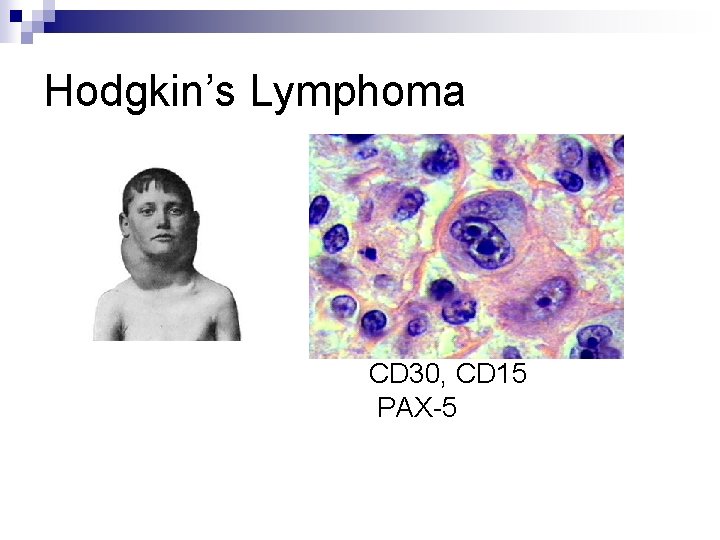
Hodgkin’s Lymphoma CD 30, CD 15 PAX-5

Virus associated Lymphomas n EBV Burkitt’s lymphoma Nasal type NK cell lymphoma Post-transplant lymphoproliferative disorders AIDS associated lymphomas Some classical type Hodgkin’s disease n HTLV-1 n HHV-8 Causes multicentric Castleman’s disease

Case Studies n Mr. JC 67 yrs Kaitaia 1 month of feeling tired. Hb 139 WCC 156 Pl 77 March 2009 Bone marrow : high grade lymphoma cells CSF: Clear
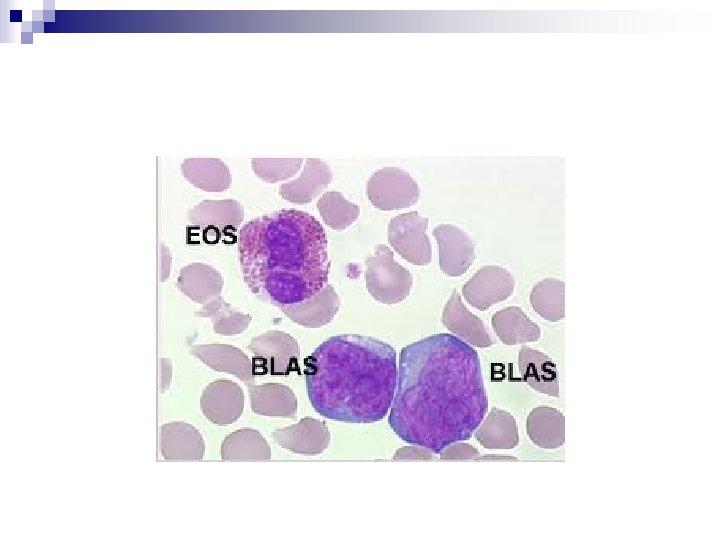
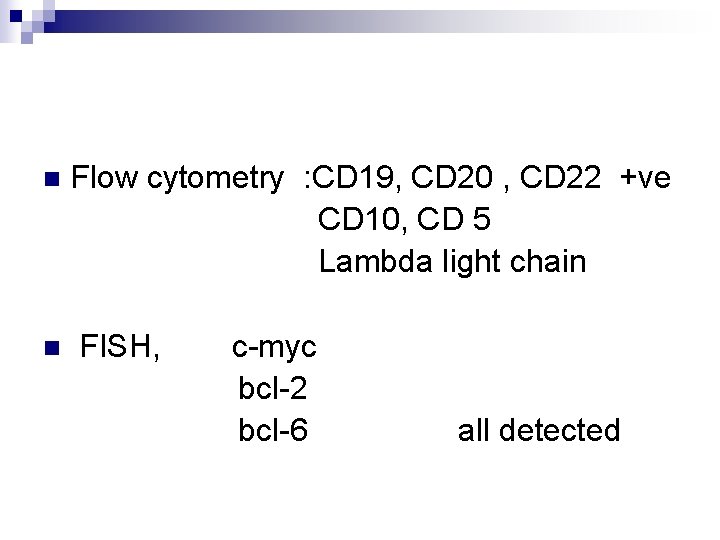
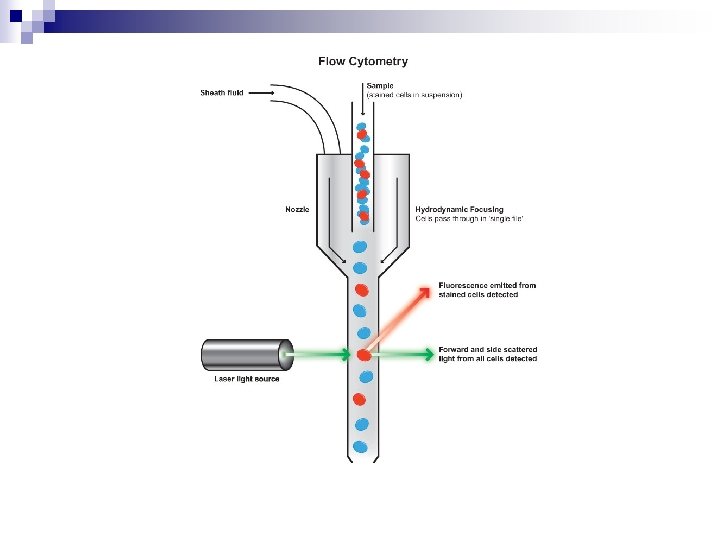
n n Flow cytometry : CD 19, CD 20 , CD 22 +ve CD 10, CD 5 Lambda light chain FISH, c-myc bcl-2 bcl-6 all detected

n Received CHOP, methotrexate, etopiside n Remission in June 2009 n September 2009 Headache, drowsiness CSF relapse Died

“Burkitt-like Lymphoma” n Heterogenous population of large cells n New Classification 2008 “B-cell lymphoma, unclassifiable, with features between DLBCL and Burkitt lymphoma”
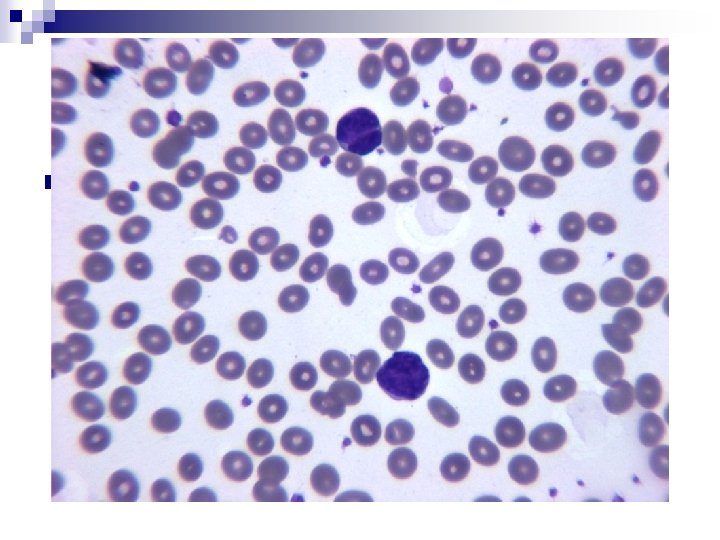
n AH. From Kaitaia Long standing CLL. Blood film changes

n 55 yr old man presents with cervical lymphadenopathy n Hb 149 WCC 12. 9 Pl 166 7. 0 x 109 /L Cervical lymph node biopsy June 2012

n Lymphocytes CD 19 CD 20 weak CD 5, CD 23 pos Lamba light chain weak CD 38 pos n FISH Trisomy 12
- Slides: 71