N 106 Nursing Care of the Newborn Immediate

N 106 Nursing Care of the Newborn

Immediate Baby Care • • Airway - Clean mouth and nose Thermoregulation - Warmth APGAR Gross assessment Identification Bonding – safety against infection Medications

Fetus to Newborn: Respiratory Changes • Initiation of respirations • Chemical surfactant reduces surface tension 34 -36 wks decrease in oxygen concentration • Thermal sudden chilling of moist infant • Mechanical compression of fetal chest during delivery normal handling

Nursing Process for Respirations • Assess for respiratory distress • Plan: Maintain patent airway • Interventions - Positioning infant – head lower - Suction secretions – bulb, keep near head, mouth first, avoid trauma to membranes • Evaluation – rate 30 -60, no distress

Fetus to Newborn: Neurological adaptation: Thermoregulation Methods of heat loss Evaporation – wet surface exposed to air Conduction – direct contact with cool objects Convection- surrounding cool air - drafts Radiation – transfer of heat to cooler objects not in direct contact with infant
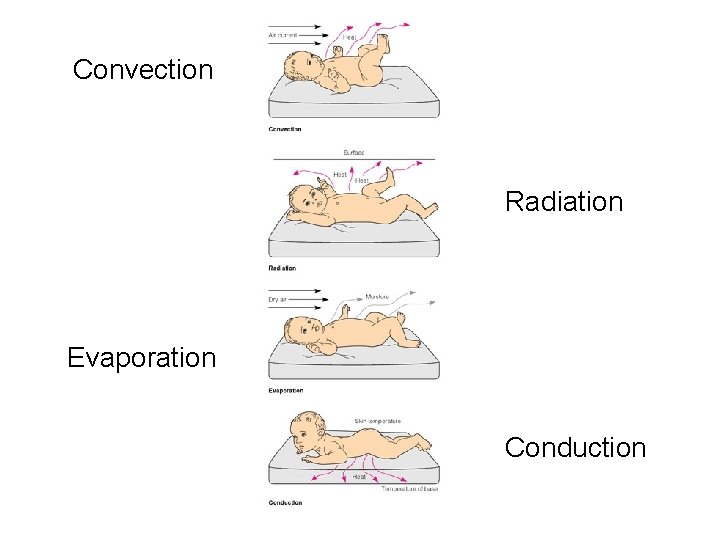
Convection Radiation Evaporation Conduction
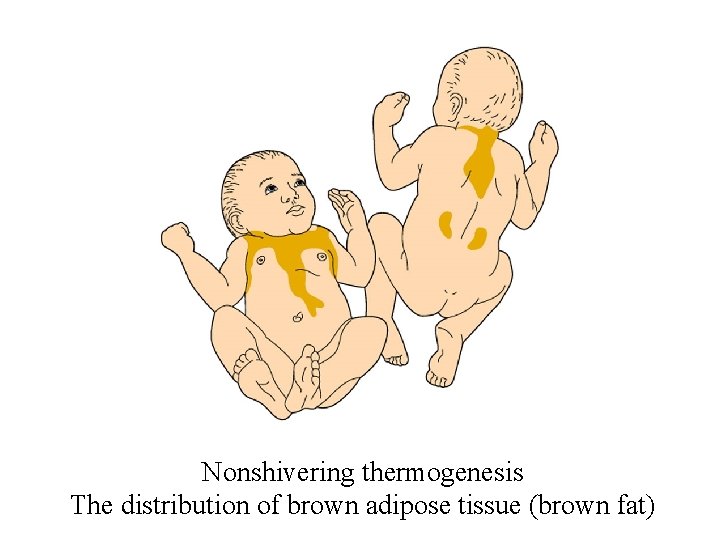
Nonshivering thermogenesis The distribution of brown adipose tissue (brown fat)

Nursing Care – Cold Stress • Preventing heat loss – radiant warmer • Providing immediate care - dry quickly, cover head with cap, replace wet blankets • Providing on going prevention - safety • Restoring thermoregulation – if becoming chilled - intervene

Effects of Cold Stress • • • Increased oxygen need Decreased surfactant production Respiratory distress Hypoglycemia Metabolic acidosis Jaundice

APGAR • • • Heart rate – above 100 Respiratory Effort – spontaneous with cry Muscle tone – flexed with movement Reflex response – active, prompt cry Color – pink or acrocyanosis • 0 -3 infant needs resuscitation • 4 -7 Gentle stimulation – Narcan • 8 -10 – no action needed

Early Assessments • Assess for anomalies • Head – anterior fontanelle closes 12 -18 mo posterior fontanelle closes 2 -3 months • Neck and clavicles fracture of clavicle – large infant, lump, tenderness, crepitus, decreased movement • Cord • Extremities flexed and resist extension assess fractures, clubfeet hips vertebral column
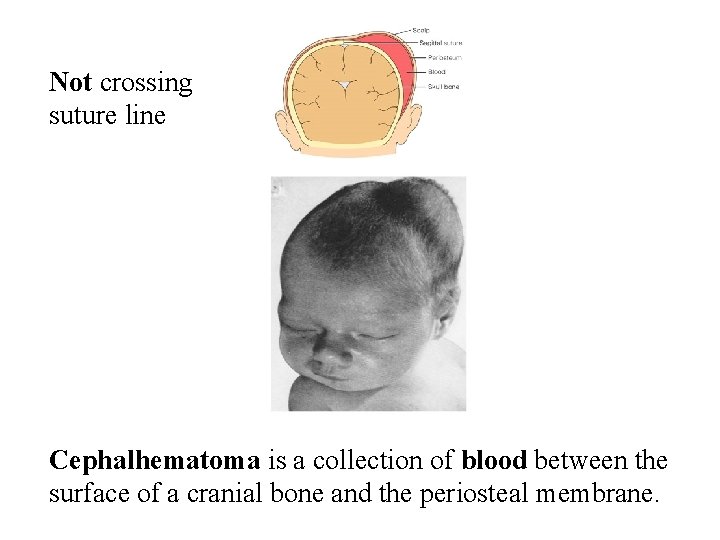
Not crossing suture line Cephalhematoma is a collection of blood between the surface of a cranial bone and the periosteal membrane.
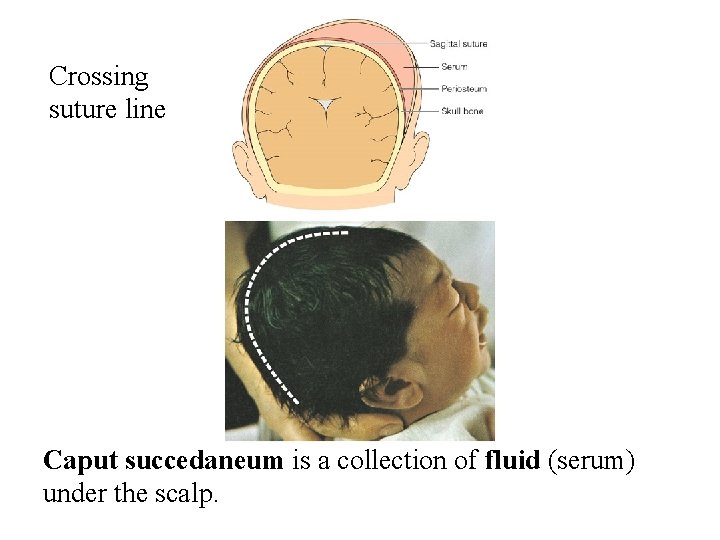
Crossing suture line Caput succedaneum is a collection of fluid (serum) under the scalp.
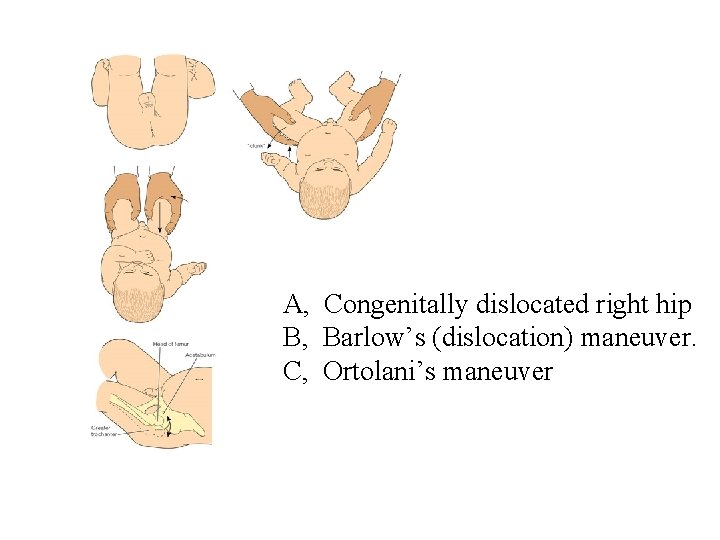
A, Congenitally dislocated right hip B, Barlow’s (dislocation) maneuver. C, Ortolani’s maneuver

Measurements • • Weight – loss of 10% normal Length Head and chest circumference Normal VS temp 97. 7 -99. 5 F axillary apical pulse 120 -160 bpm respirations 30 -60/min
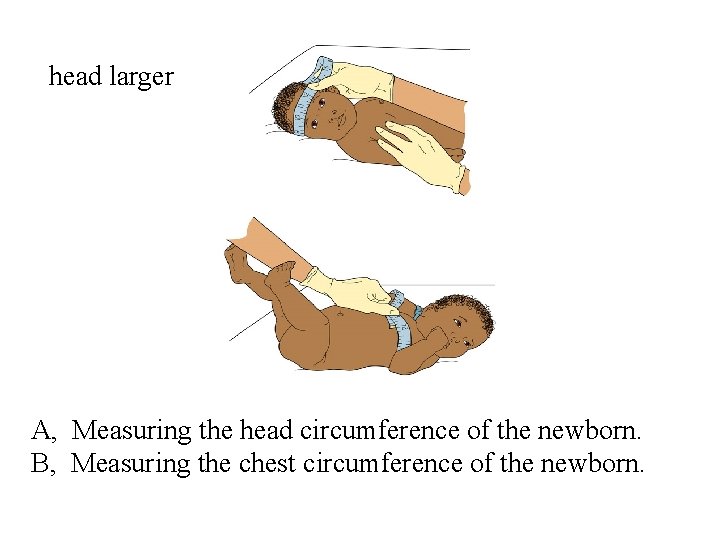
head larger A, Measuring the head circumference of the newborn. B, Measuring the chest circumference of the newborn.
Assessment of Cardio-respiratory Status • History • Airway • Assess rate q 30 min. X 2 hrs symmetry breath sounds - moisture for 1 -2 hrs

Assessment of Thermoregulation • • • Check soon after birth Set warmer controls Take temp q 30 min until stable Rectal for first temp Insert only 0. 5 inch Axillary route rest of time
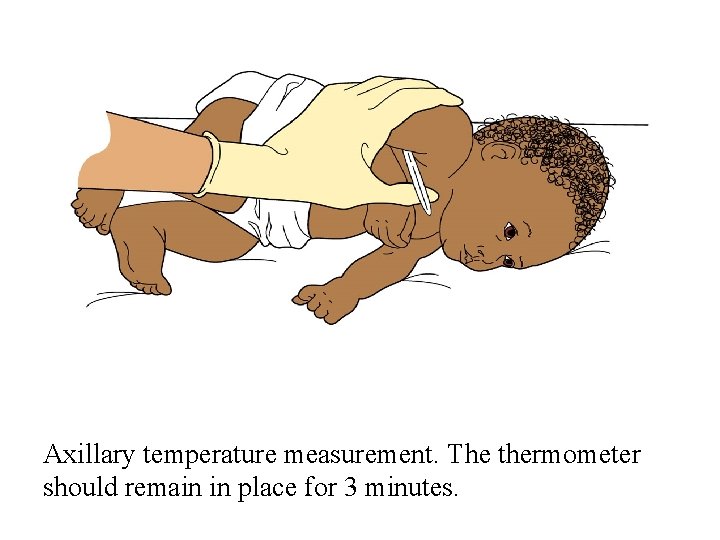
Axillary temperature measurement. The thermometer should remain in place for 3 minutes.

Assessment of Hepatic Function • Blood Glucose Signs of hypoglycemia jitteriness respiratory difficulties drop in temp poor sucking Tx- feed infant if glucose below 40 -45 mg/dl • Bilirubin physiologic jaundice peaks 2 -4 days of life early onset may be pathologic

Jaundice • • • Hemolysis of excessive erythrocytes Short red blood cell life Liver immaturity Lack of intestinal flora Delayed feeding Trauma resulting in bruising or cephalhematoma • Cold stress or asphyxia
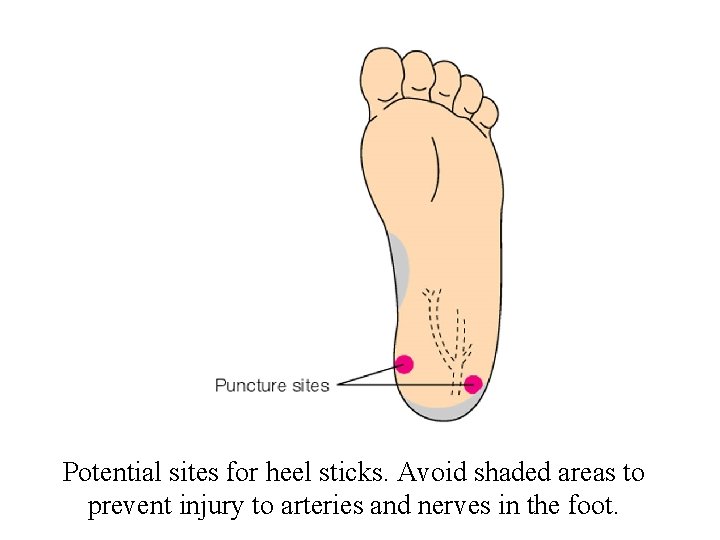
Potential sites for heel sticks. Avoid shaded areas to prevent injury to arteries and nerves in the foot.

Assessment of Neuro System • Reflexes • Babinski Grasp Moro Rooting Stepping Sucking Tonic neck reflex “fencing” • Cry • Infant response to soothing

Assessment of Gastrointestinal System • • • Mouth Suck Abdomen Initial feeding Stools meconium – within 12 -48 hours of birth dark greenish black breastfed – soft, seedy, mustard yellow formula-fed – solid, pale yellow

Assessment of Genitourinary System • • Umbilical cord vessels Urine – within 24 hours of birth Voiding – 6 to 10 times a day after 2 days Genitalia female – edema normal, majora covers minora, pseudomenstruation male – pendulous scrotum, descended testes by 36 wks gest. , placement of meatus

Assessment of Integumentary System • • • Vernix – white covering Lanugo – fine hair Milia Erythema toxicum – red blotchy with white Birthmarks Mongolian spots – sacral area Telangiectatic nevus “stork Bite” - blanches Nevus flammeus “port wine stain” - no blanching Nevus vasculosus “strawberry hemangioma” usually on head, disappears by school age
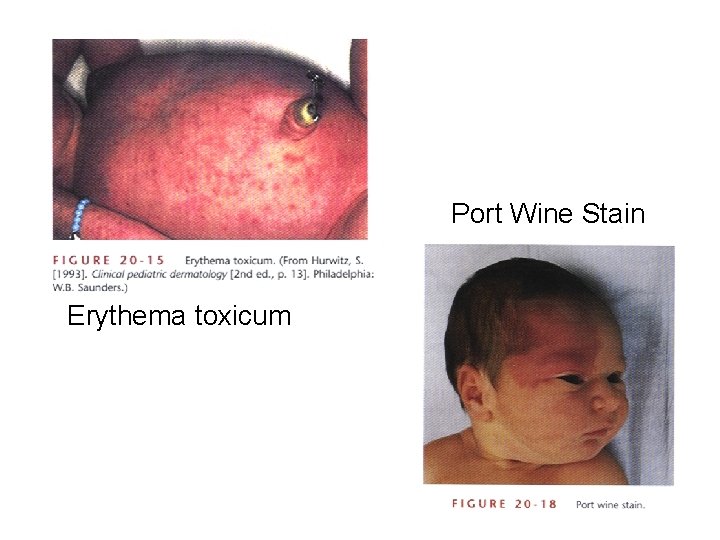
Port Wine Stain Erythema toxicum

Fetus to Newborn: Psychosocial adaptation • Periods of Reactivity active – 30 -60 min sleep – 2 -4 hours alert – 4 -6 hours • Behavioral States quiet sleep active sleep drowsy state quiet alert – best for bonding active alert crying state

Gestational Age Assessment • • Assessment tool – Dubowitz, Ballard Weeks from conception to birth Used to identify high risk infants Neuromuscular characteristics Posture – more flexion Square window – more pliable Arm recoil - active Popliteal angle - less Scarf Sign – less crossing Heel to ear – most resistance
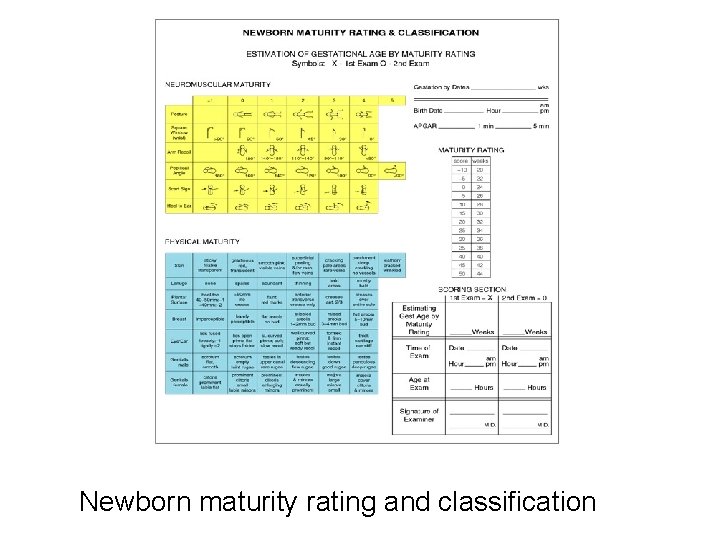
Newborn maturity rating and classification

Gestational Age Assessment • Physical characteristics Skin- deep cracking, no vessels seen, post-leathery Lanugo – less as age Plantar creases – more with age Breasts – larger areola Eyes and Ears – stiff with instant recoil Genitals – deep rugae, pendulous, covers minora • Gestational Age & Size – may not correspond small SGA <10% for weight large LGA >90% for weight appropriate AGA between 10 -90%
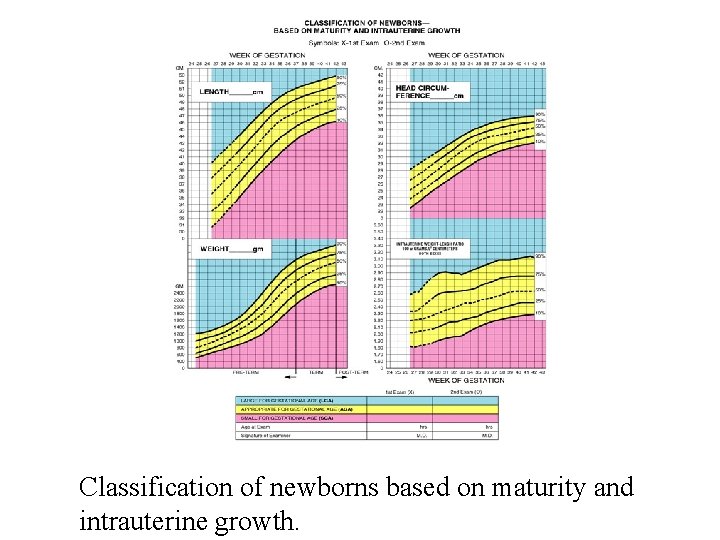
Classification of newborns based on maturity and intrauterine growth.
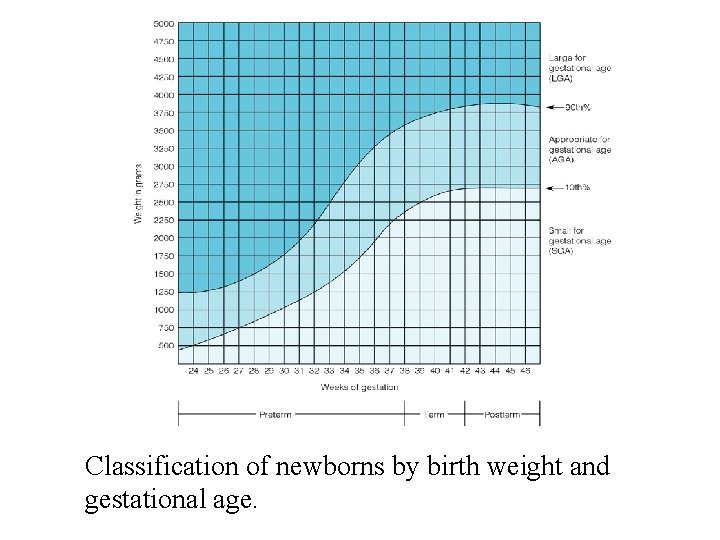
Classification of newborns by birth weight and gestational age.

Ongoing Assessment and Care • • • Bathing Cord care Cleansing diaper area Assisting with feedings Protecting infant identifying infant preventing infant abduction – alert to unusual preventing infection • Review beige cue cards in center of book for teach
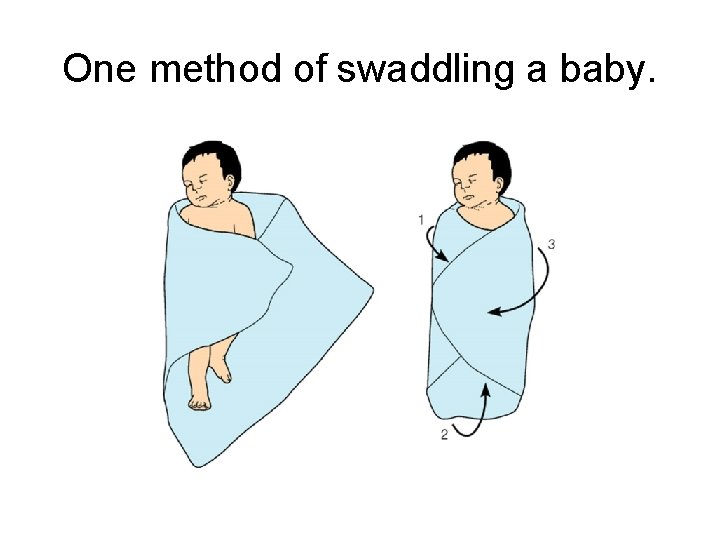
One method of swaddling a baby.
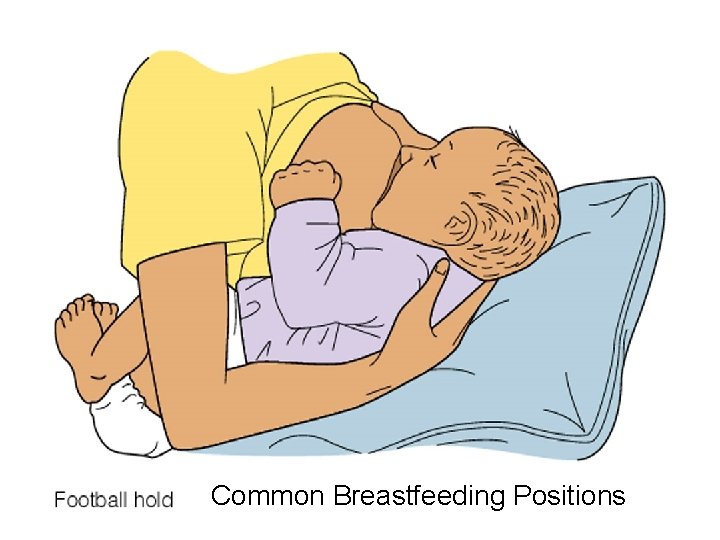
Common Breastfeeding Positions
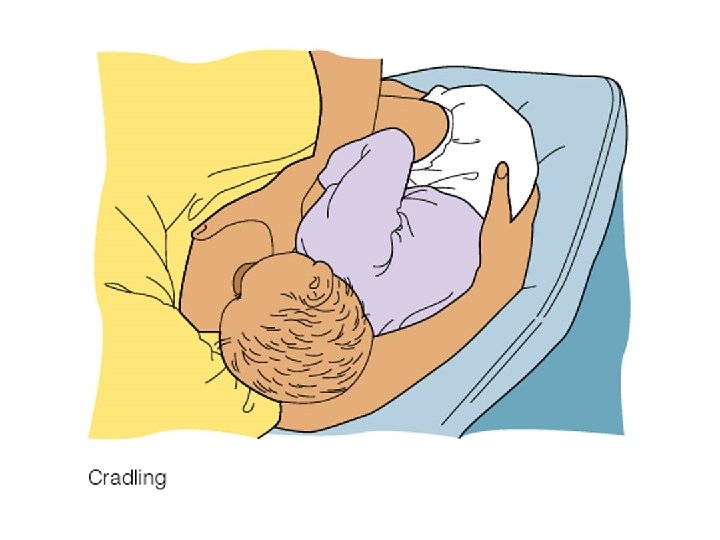
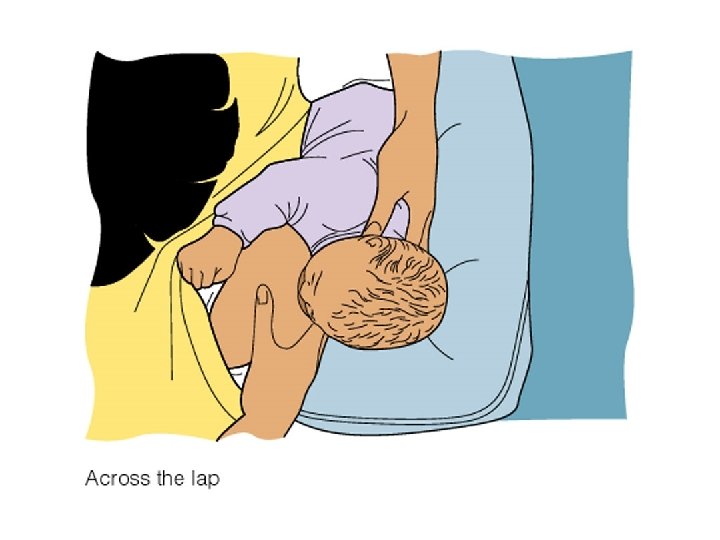
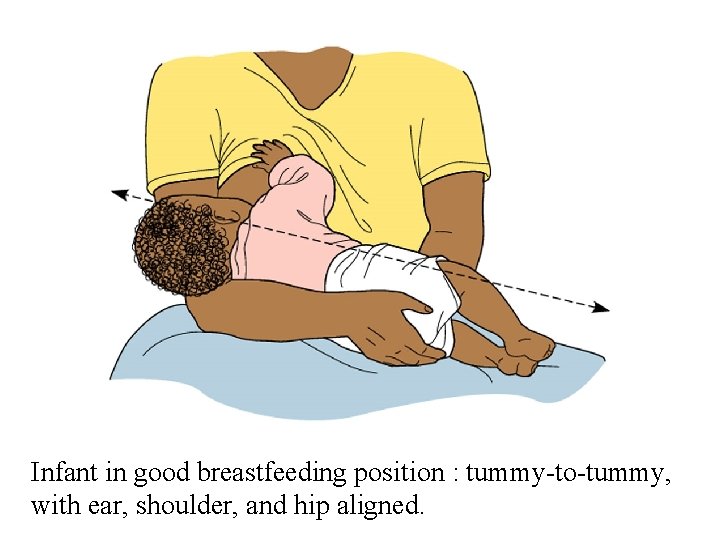
Infant in good breastfeeding position : tummy-to-tummy, with ear, shoulder, and hip aligned.
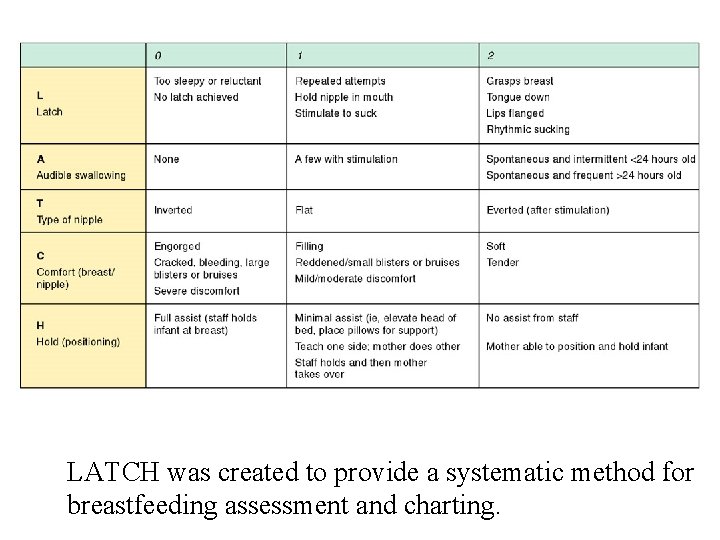
LATCH was created to provide a systematic method for breastfeeding assessment and charting.
Infant teaching checklist is completed by the time of discharge.

Circumcision • Most common neonatal surgical procedure • Reasons for choosing • Reasons for rejecting – hypospadias, epispadias • Pain relief • Methods • Nursing care
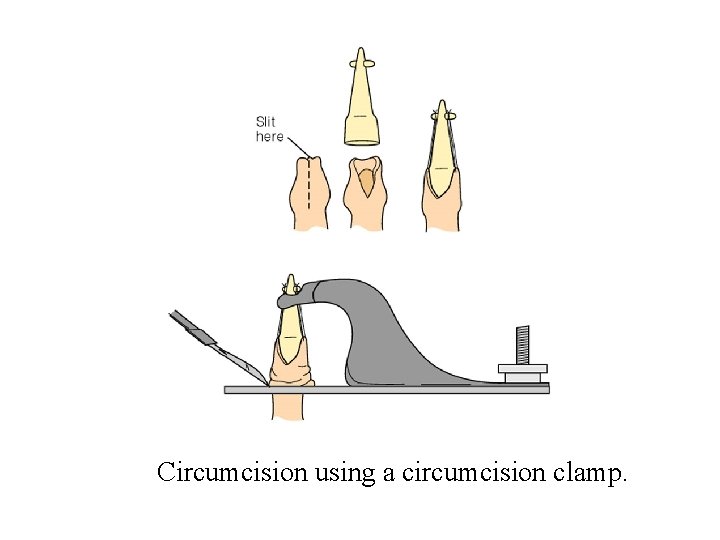
Circumcision using a circumcision clamp.
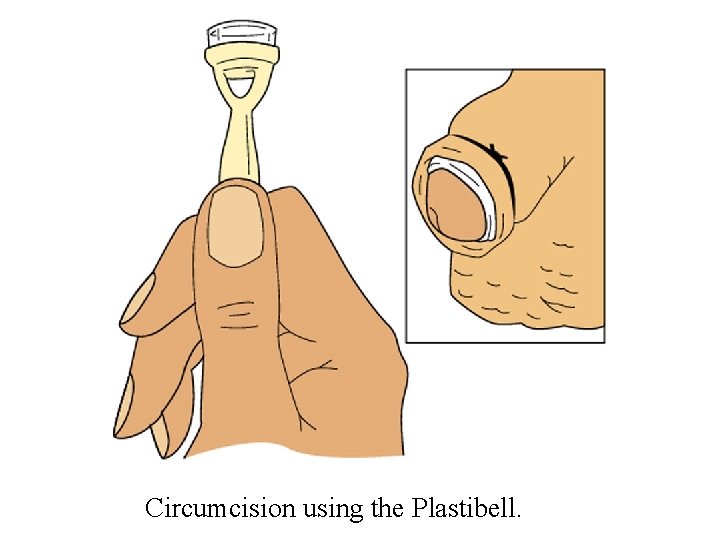
Circumcision using the Plastibell.

Other Concerns • Immunizations Hepatitis B – begin vaccine at birth • Screening tests Hearing Phenylketonuria – by law

Further Assessments • Complications r/t poorly functioning placenta hypoglycemia hypothermia respiratory problems • Complications r/t LGA infant hypoglycemia birth injury due to size

Shoulder Dystocia • Risk factors diabetes; macrosomic infant obesity prolonged second stage previous shoulder dystocia • Morbidity- fracture of clavicle or humerus, brachial plexus injury • Management – generous episiotomy
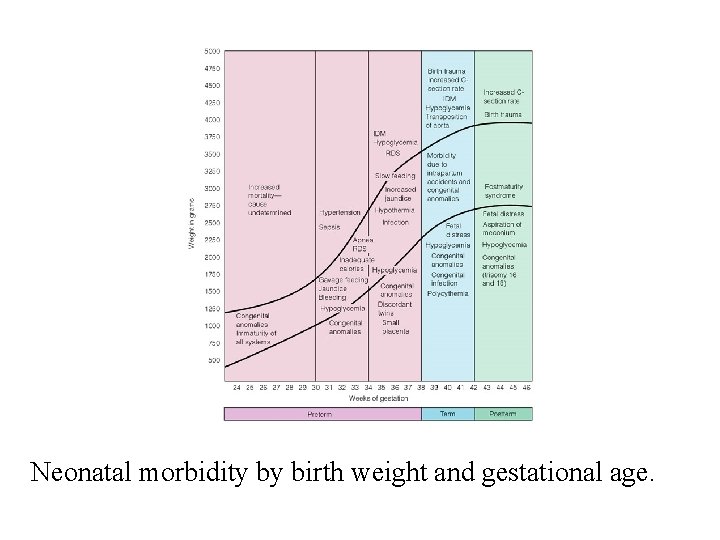
Neonatal morbidity by birth weight and gestational age.

High Risk Infants • • Preterm – before 38 weeks gestation IUGR – full term but failed to grow normally SGA LGA Infants of Diabetic mothers Post mature babies Drug exposed

Preterm infants • Survive - Weight 1250 g -1500 g – 85 -90% 500 -600 g at birth 20% survive • Ethical questions • Characteristics – frail, weak, limp, skin translucent, abundant vernix & lanugo • Behavior – easily exhausted, from noise and routine activities, feeble cry

Nursing Care of Preterm Infants • Inadequate respirations • Inadequate thermoregulation • Fluid and electrolyte imbalance – dehydration sunken fontanels <1 ml/kg/hr or over hydration bulging, edema and urine output >3 ml/kg/hr • Signs of pain – high-pitched cry, >VS • Signs of over stimulation - >P, >RR, stiff extended extremities, turning face away • Nutrition – signs of readiness to nipple resp <60/m, rooting, sucking, gag reflex
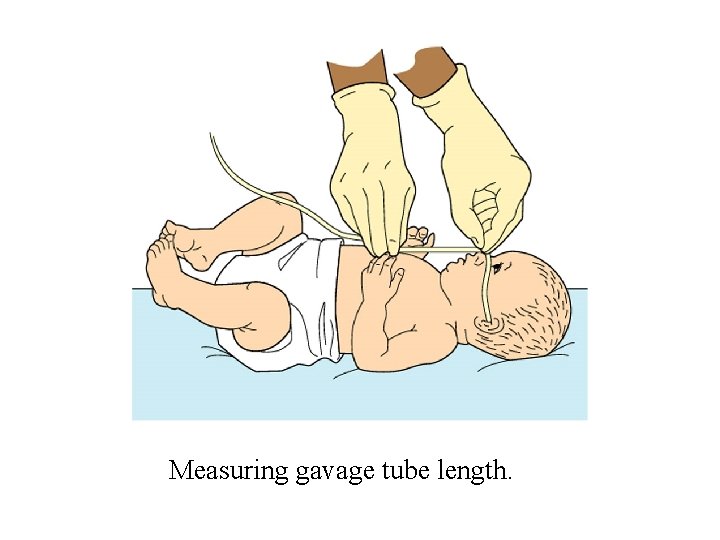
Measuring gavage tube length.
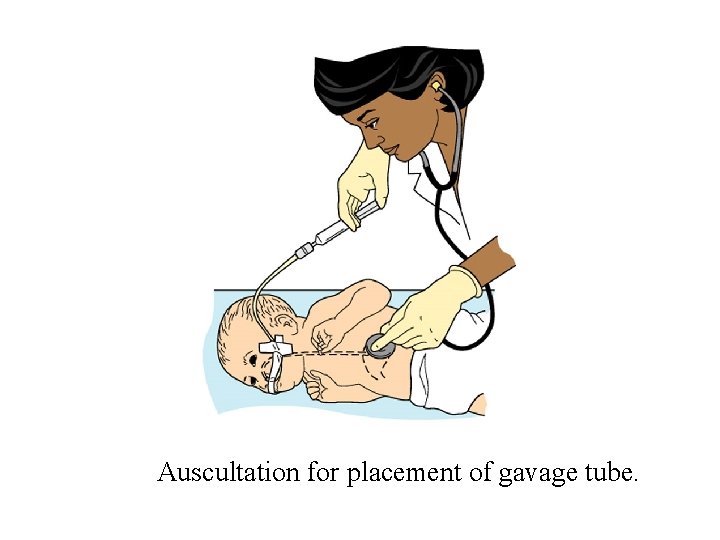
Auscultation for placement of gavage tube.

Complications of Preterm Infants • Respiratory Distress Syndrome -RDS • Bronchopulmonary dysplasia – chronic lung disease • Periventricular-Intraventricular Hemorrhage 30% infants <32 wk gest or <1500 g • Retrolenthal fibroplasia – visual impairment or blindness from O 2 & ventilator • Necrotizing Enterocolitis (NEC) – distention, increased residual, Tx - rest bowel

Respiratory Distress Syndrome • RDS also know as “hyaline membrane disease” • Cause – besides preemie, C/S, diabetic mothers birth asphyxia – interfere with surfactant • S&S tachypnea - over 60/min retractions- sternal or intercostal nasal flaring cyanosis- central grunting- expiratory seesaw respirations asymmetry
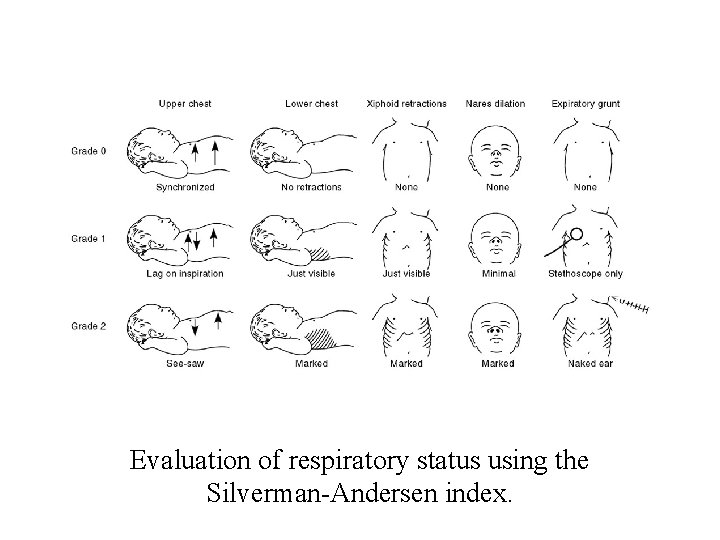
Evaluation of respiratory status using the Silverman-Andersen index.

Therapeutic Management of RDS • • • Surfactant replacement therapy Installed into the infant’s trachea Improvement in breathing occurs in minutes Doses repeated prn Other treatment mechanical ventilation correction of acidosis IV fluids

Post Term Infants • • • Born after 42 weeks Increase risk of meconium aspiration Hypoglycemia Loss of subcutaneous fat Skin –peeling, vernix sparse, lanugo absent, fingernails long • Focus on prevention – “due date” • Attention to thermoregulation & feeding

Meconium Aspiration Syndrome • Occurs most often post term infants, decreased amniotic fluid /cord compression • Meconium enters lung – obstruction • S & S vary from mild to severe respiratory distress: tachypnea, cyanosis, retractions, nasal flaring, grunting • Tx – suction at birth, may need warmed, humidified oxygen, or ventilators

Hyperbilirubinemia • Pathologic jaundice – occurs within first 24 hours • Bilirubin levels >12 in term or 10 -14 preterm • May lead to kernicterus – brain damage • Most common cause – blood incompatibility of mother and fetus, Rh or ABO – only occurs with mother negative Rh or O blood • Treatment focus on prevention, assess coombs, monitor bilirubin levels, most common treatment is phototherapy, blood transfusions
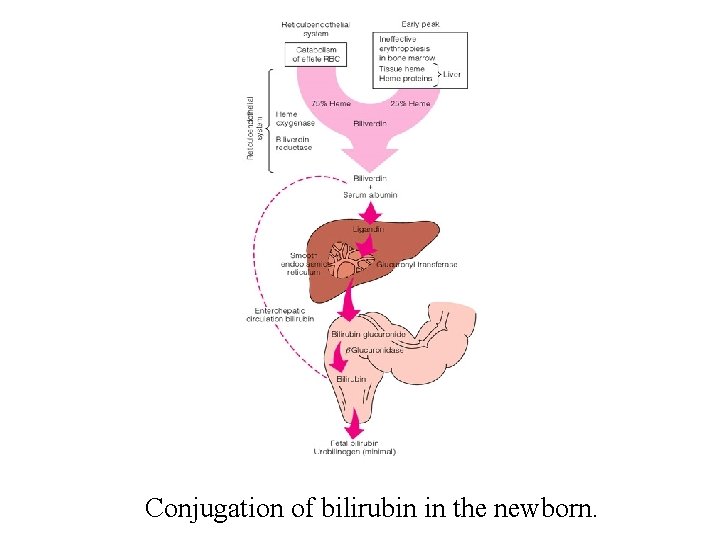
Conjugation of bilirubin in the newborn.

Phototherapy for Hyperbilirubinemia • Phototherapy – bilirubin on skin changes into water-soluble excreted in bile & urine • “Bili” lights placed inside warmer, need patches over eyes, infant wearing only diaper or fiberoptic phototherapy blanket against skin • Side effects of phototherapy: freq, loose, green stools, skin changes • Can use at home

Other interventions for hyperbilirubinemia • Exchange transfusions – if lights not working • Maintain neutral thermal environment – not too hot or too cold • Provide optimal nutrition – hydrate • Protecting the eyes from retinal damage • Enhance therapy by expose as much skin as possible to light, remove all clothing except diaper, turn frequently

Infant of a Diabetic Mother • Macrosomia – face round, red, body obese, poor muscle tone, irritable, tremors • High risk for – trauma during birth, congenital anomalies, RDS, hypocalcemia • Hypoglycemia occurs 15 -50% of time <40 -45 mg/dl, test right after birth, q 2 h. X 4, then q 4 hr. X 6 until stable • Most frequent symptom: jitteriness or tremors • Tx – fed, gavage or IV if needed

Hypoglycemia • Serum glucose is below 40 mg/d. L • Tx: feed infant formula or breast milk and retest until glucose stable • S & S: jitteriness, lethargy, poor feeding, high -pitched cry, irregular respirations, cyanosis, seizures • Risk factors: DM, PIH, preterm, post term, LGA, cold stress, maternal intake of ritodrine or terbutaline

Large for Gestational Age • Infants weight is in the 90 th % for neonates same gestational age, may be pre, post, or full term infants • LGA does not mean post term • Most common cause – maternal diabetes • Infant at risk: birth injuries, hypoglycemia, and polycythemia - macrosomia

Small for Gestational Age • • • Infant whose wt is at or below the 10 th % Results from failure to thrive Is a high risk condition SGA does not mean “premature. ” Causes: anything restricting uteroplacental blood flow, smoking, DM, PIH, infections • Complications: hypoglycemia, meconium aspiration, hypothermia, polycythemia

Mother with Substance Abuse • Use of alcohol or illicit drugs • Tobacco and alcohol are most frequent • Prenatal alcohol exposure is the most commons preventable cause of mental retardation • Signs of maternal addition: wt loss, mood swings, constricted pupils, poor hygiene, anorexia, no prenatal care

Drug Withdrawal in Infants • Signs of drug exposure opiates – 48 -72 hours cocaine – 2 -3 days alcohol – within 3 -12 hours • Symptoms: irritable, hyperactive muscle tone, high-pitched cry • High risk for SGA, preterm, RDS, jaundice • Obtain infant mec and urine sample for test

Nursing Care of Drug-Exposed Infant • Feeding – more difficult may need to gavage • Rest – keep stimulation to minimum, reduce noise and lights, calm, slow approach • Promote bonding • Teach measures for frantic crying: rock, coo, dark room, avoid stimulation

Phenylketonuria - PKU • Genetic disorder causes CNS damage from toxic levels of amino acid phenylalanine • caused by deficiency of the enzyme phenylalanine hydroxylase • Signs- digestive problems, vomiting, seizures, musty odor to urine, mental retardation • Tx – low phenylalanine diet – start within 2 months • Screening before 24 -48 hours needs to be repeated for accuracy

Signs Bonding Delayed • • Using negative terms describing infant Discussing infant in impersonal terms Failing to give name – check culture Visiting or calling infrequently Decreasing length of visit Refusing to hold infant Lack of eye contact with infant
- Slides: 72