Myelography Dr Malith Kumarasinghe MBBS Colombo What is
Myelography Dr Malith Kumarasinghe MBBS (Colombo)

What is it? � Injection of intra-thecal contrast material to visualize disease or injury within the spinal column using CT and fluoroscopy � Invasive test with associated risks � Has been largely replaced by MR, which is non-invasive and therefore safer

Why Is Myelography Still Used? � 10 -20% of patients are unable to tolerated MR secondary to claustrophobia or the inability to remain still • Post-op metallic hardware (e. g. pedicle screws) and pacemakers cause distortion of MR images

Indications Still considered the “gold standard” for degenerative disease � Confirmation of equivocal MR findings particularly in the cervical spine (such as small tumor nodules on nerve roots) � Used to visualize nerve roots in direct coronal plane to better assess degree of compression seen on MR � Often surgeons request myelography because they are more familiar with this technique �

Indications (cont. ) � Osteophytic disease is accurately identified owing to exquisite bone detail The left side of the spinal cord is compressed by an osteophyte

Indications (cont. ) � Subarachnoid spread of tumor and small tumor implants on nerve roots � Arachnoiditis � Nerve root compression, extradural impressions, and disc protrusion � Visualization of dilated veins in patients with spinal A-V malformations Note: MR is the test of choice for visualizing the spinal cord and soft tissues if there is no contraindication

Contraindications � Patient with known severe hypersensitivity to contrast � Significant local or systemic infection where bacteremia is likely � Very recent prior myelogram (concern for contrast overdosage)

Pre-Procedure � Explain procedure to patient Ø Typically a lumbar approach is used to access thecal sac since this is easier and has a lower complication rate Ø If patient has a complete block or lumbar access cannot be obtained it may be necessary to perform a cervical tap to analyze the cervical spine Inform patient of risks (bleeding, HA, infection, pain, and seizure) and obtain consent � Stop all meds that lower seizure threshold (e. g. phenothiazines, antipschotics, tricyclic antidepressants, MAOIs, lithium, INH) 24 to 48 hrs prior to the procedure �

Procedure Follow lumbar puncture protocol (see appropriate section) � Once in thecal sac CSF should be collected if it is needed for examination � Administer contrast (typically Omnipaque 300, 240, 210, or 180) � Ø Generally, 3. 06 g of iodinated contrast instilled intrathecally is the limit in adults (2. 94 g in children) Ø This corresponds to 10 ml of contrast with a concentration of 300 mg/ml or 12 ml at 240 mg/ml Ø Concentration in children should be less than 210 mg/ml

Procedure – Lumbar myelogram Contrast should be instilled with intermittent fluoroscopy to determine the correct amount to be administered (amount will vary depending on size of thecal sac) � AP, lateral and oblique films are obtained with patient in the prone position within 30 minutes after contrast injection (standing views may accentuate disk herniation) � Postmyelogram CT (several hours after administration of contrast) � Ø Sections angled through the disks Ø Contiguous straight transaxial sections allow high-quality sagittal and coronal reconstruction
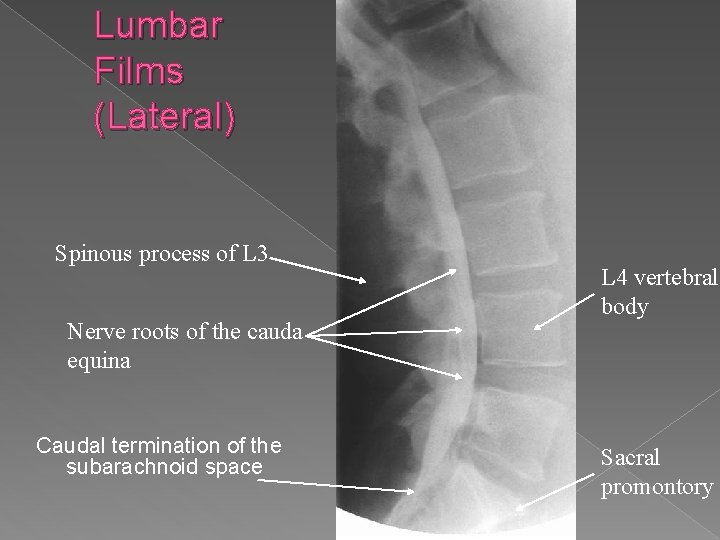
Lumbar Films (Lateral) Spinous process of L 3 Nerve roots of the cauda equina Caudal termination of the subarachnoid space L 4 vertebral body Sacral promontory
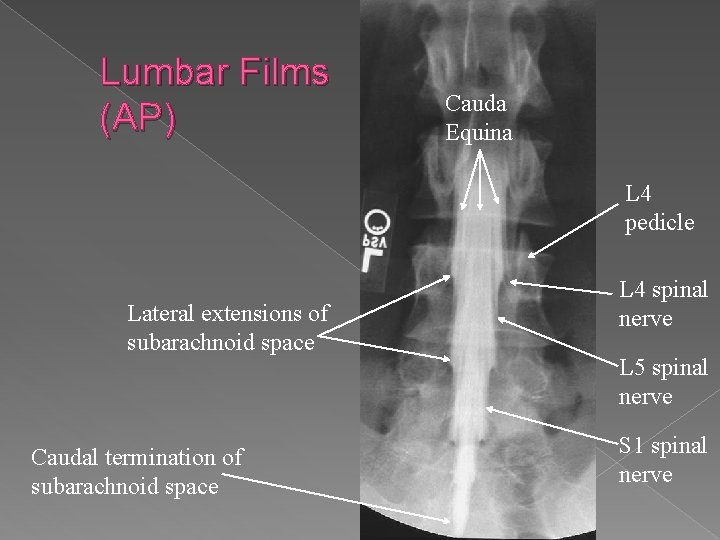
Lumbar Films (AP) � Cauda sd Equina L 4 pedicle Lateral extensions of subarachnoid space Caudal termination of subarachnoid space L 4 spinal nerve L 5 spinal nerve S 1 spinal nerve
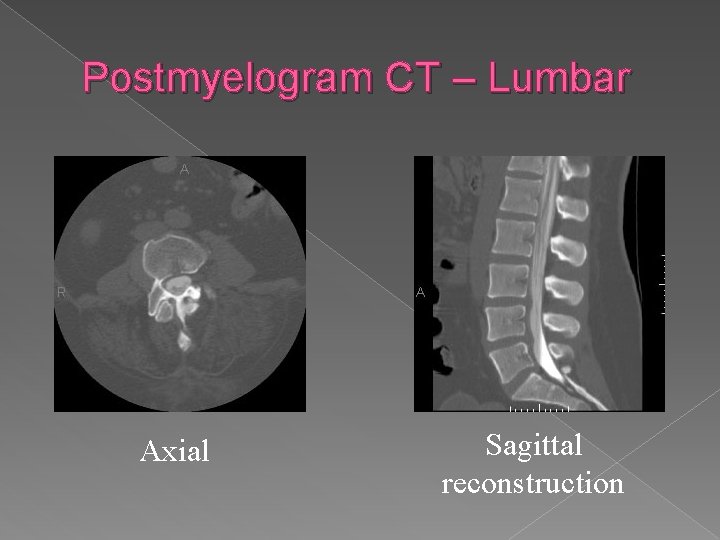
Postmyelogram CT – Lumbar Axial Sagittal reconstruction

Procedure – Cervical Myelogram � Lumbar Approach Ø Easier, less patient anxiety, and lower complication rate when compared to cervical approach Ø Contrast is inserted as a bolus in the lumbar region of the spine and maintained as a bolus as the patient is tilted downward Ø Patient’s head is maintained in a hyperflexed fashion to prevent contrast from entering the intracranial sac Ø Once contrast is in the cervical region, the patient is flattened and the contrast pools in the natural lordosis of the cervical spine

Procedure – Cervical Myelogram � Cervical Approach Ø Reserved for patients with complete block or severe degenerative changes, scoliosis, or infection that prevent lumbar tap Ø Risk is increased (still low at. 17 percent) owing to the presence of the spinal cord and vertebral arteries Ø Needle is inserted just anterior to the spinal lamina line at C 1 -C 2 using cross-table lateral and AP fluoro Ø Needle is inched forward using lateral fluoro to ensure that the needle does not puncture the spinal cord Ø Permanent damage from puncturing the spinal cord is very rare unless contrast is injected into the cord itself. Ø Low dose contrast should be instilled into thecal sac for cervical examination

Procedure – Cervical Myelogram � Obtain AP, lateral, and oblique films � Postmyelogram CT scans are obtained through suspicious levels seen on plain films ØSections angled through the disks ØContiguous straight transaxial sections allow highquality sagittal and coronal reconstruction
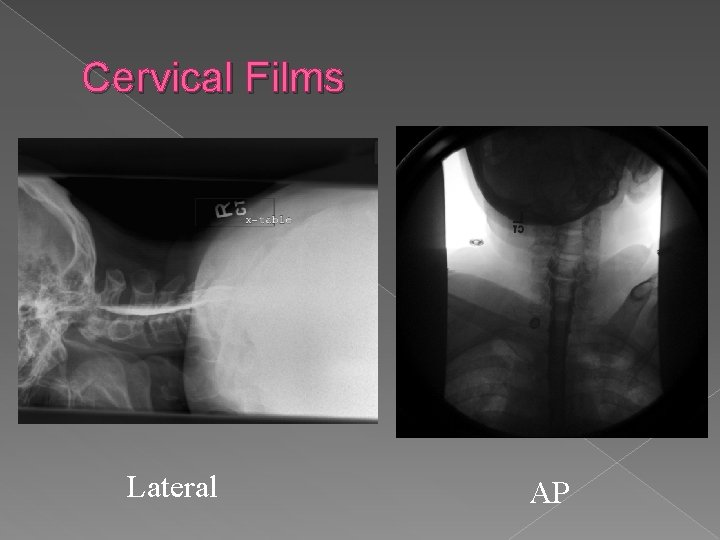
Cervical Films Lateral AP
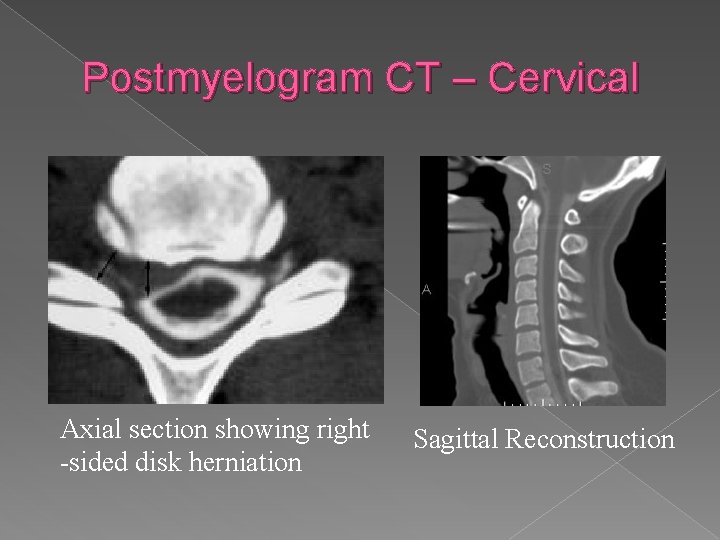
Postmyelogram CT – Cervical Axial section showing right -sided disk herniation Sagittal Reconstruction

Post-Procedure � Bed rest for 4 hrs � No heavy lifting or bending for 24 hrs � Keep head elevated to limit contrast flowing intracranially � Ibuprofen or Acetaminophen prn pain and HA � Resume restricted meds after 24 hrs
- Slides: 19