Myelodysplastic Syndromes MDS Authors Lao Zhentang MBBS Academic

Myelodysplastic Syndromes (MDS) Author(s): Lao Zhentang, MBBS Academic Affiliation: Singapore General Hospital, Registrar Level: Intermediate Version No: 1. 0 Submitted: April 2012 Editors’ Review:

2 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

3 Financial Disclosures (past 3 years) No Disclosures
4 Definition • Heterogeneous group of haematopoietic stem cell disorders • Characterized by: – – Bone marrow dysplasia Ineffective haematopoiesis Peripheral blood cytopenias Risk of transformation to acute leukemia (AML)

5 Risk factors • Old age (median age at diagnosis = 72 years) • Radiation – high dose radiotherapy (median time interval = 12 years) • Cytotoxic drugs – classically alkylating agents and topoisomerase inhibitors (median time interval = 5 years) • Occupational exposure to organic solvents e. g. benzene • Congenital factors – Down's syndrome and Bone marrow failure syndromes such as Fanconi's Anemia

6 WHO 2008 Classification • Refractory Cytopenia with Unilineage Dysplasia (RCUD) • Refractory Anemia with Ringed Sideroblasts (RARS) • Refractory Cytopenia with Multilineage Dysplasia (RCMD) • Refractory Anemia with Excess Blast (RAEB) RAEB - 1 (5 – 9% blasts) RAEB - 2 (10 – 19% blasts) • New cutoff of 20% blast for definition of acute myeloid leukemia • Shown to have prognostic significance, with RCUD having the best prognosis and RAEB -2 having the worst

7 Prognosis – IPSS 1997 • Bone marrow myeloblast percentage • Cytogenetics • Number of cytopenias – Hb <10 g/d. L – Platelets <100, 000/mm 3 – Neutrophils <1, 800/mm 3 • IPSS risk groups – Lower risk (Low, Int-1) and higher risk (Int-2 and High)
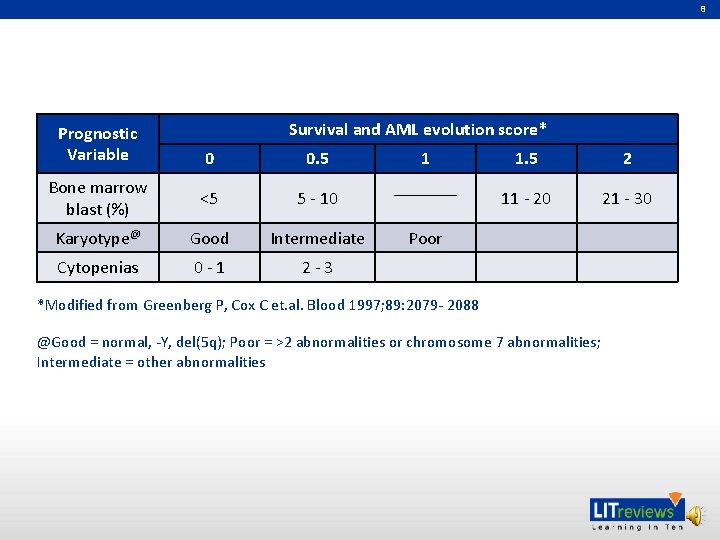
8 Prognostic Variable Survival and AML evolution score* 0 0. 5 Bone marrow blast (%) <5 5 - 10 Karyotype@ Good Intermediate Cytopenias 0 - 1 2 - 3 1 _______ 1. 5 2 11 - 20 21 - 30 Poor *Modified from Greenberg P, Cox C et. al. Blood 1997; 89: 2079 - 2088 @Good = normal, -Y, del(5 q); Poor = >2 abnormalities or chromosome 7 abnormalities; Intermediate = other abnormalities
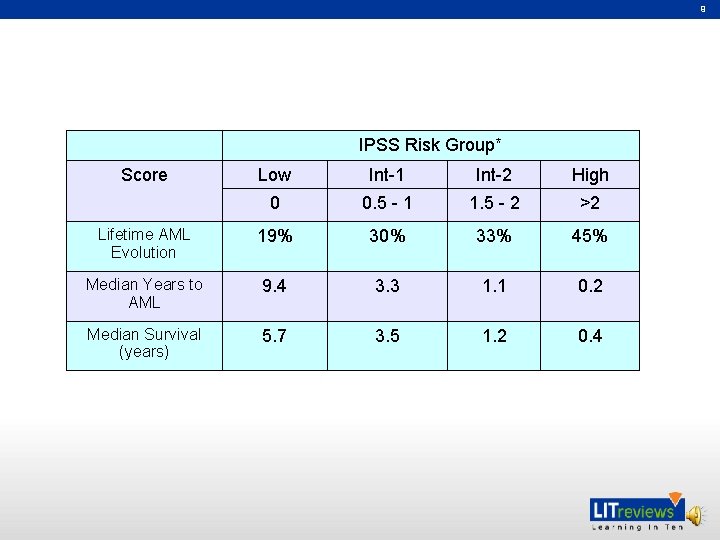
9 IPSS Risk Group* Score Low Int-1 Int-2 High 0 0. 5 - 1 1. 5 - 2 >2 Lifetime AML Evolution 19% 30% 33% 45% Median Years to AML 9. 4 3. 3 1. 1 0. 2 Median Survival (years) 5. 7 3. 5 1. 2 0. 4

10 Treatment modalities • Supportive care (BSC), transfusion support • Treatment for iron overload in transfusion dependent MDS • Hematopoietic growth factors • Low dose chemotherapy • Intensive chemotherapy • Stem cell transplantation (SCT) • Immunosuppressive therapy (IST) • Novel therapies

11 Supportive Treatment • Aim to manage patient’s symptoms and the problems related to cytopenias • RBC transfusion – Threshold depends on patient’s symptom and local guideline (e. g. Hb <8. 0 g/d. L) • Platelet transfusion – Threshold depends on whethere is any bleeding complication and local guideline (e. g. plt <10, 000/mm 3) • Antibiotics for infective complications • Haemopoietic growth factors

12 Intensive chemotherapy • Generally offered to relatively younger and higher risk MDS patients who are fit for intensive therapy and for reducing disease burden prior to stem cell transplantation • There is no standard induction regimens for elderly with MDS/AML • Lower induction CR rate 40 -50% and shorter remission duration in high risk MDS when compared to de novo AML • Induction mortality ~30% • Without consolidation with stem cell transplantation, 2 year survival is <20%

13 Stem cell transplantation • Majority of MDS patients are not eligible • Allogeneic stem cell transplantation using standard myeloablative conditioning regimen from HLA-identical sibling donor • 3 -year overall survival ~40% • The use of reduced intensity conditioning (RIC) regimen allows more older patients to be eligible for allograft • RIC is sssociated with higher relapse rate but lower treatment related mortality

14 Novel therapies • Lenalidomide (Revlimid®) for 5 q- syndrome • DNA methyl transferase (DNMT) inhibitors – 5 -Azacytidine (Vidaza®) – Decitabine (Dacogen®) • Histone deacetylase (HDAC) inhibitors – Valporic acid, Vorinostat, Panobinostat, Entinostat, Romidepsin etc. • Combination therapies

Partners in Academic Medicine
- Slides: 15