Myasthenia Gravis Terri Kueber CRNA MS Objectives Explain

Myasthenia Gravis Terri Kueber, CRNA, MS

Objectives �Explain the pathophysiology and classification of Myasthenia Gravis (MG) �List the signs and symptoms and clinical manifestation �Describe the various treatments available for Myasthenia Gravis �Discuss the anesthetic considerations for patients with Myasthenia Gravis


Introduction �Myasthenia Gravis is an autoimmune neuromuscular �Consider a “Snowflake Disease” �Cause is still unknown �No known cure �History �Incident and prevalence is increasing with 5 -10 per 100, 000 25, 000 cases in US �Still considered sporadic �Women versus men �Often associated with other autoimmune disorders
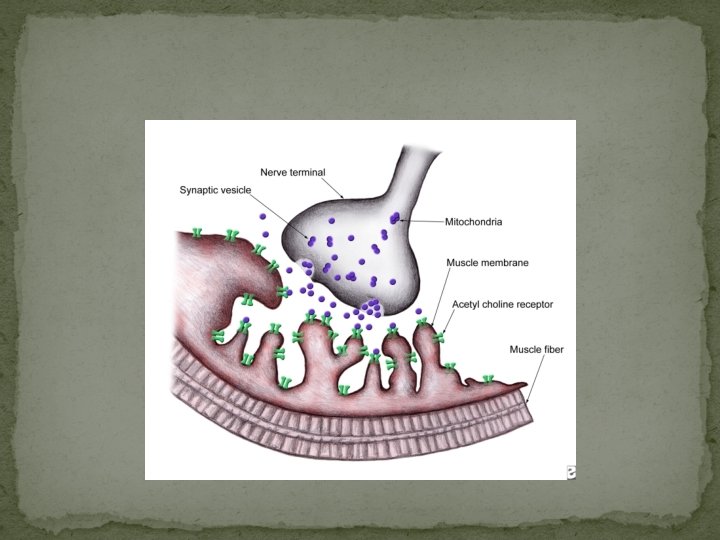
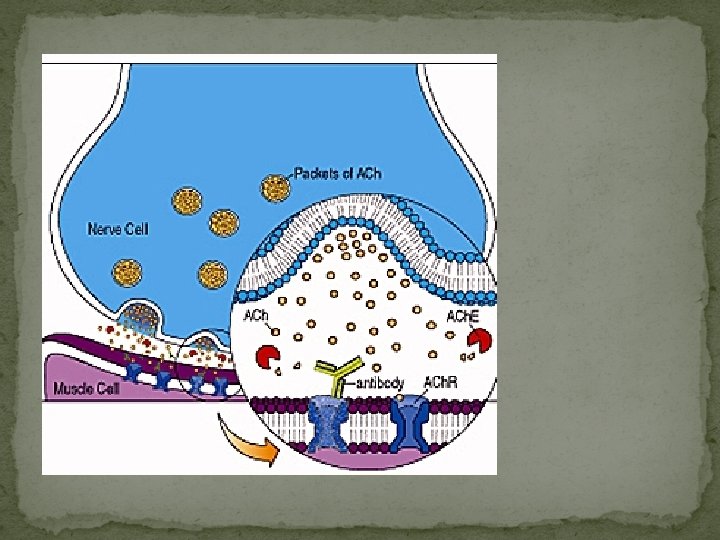

MGFA/Osserman Classification �Class I: Ocular weakness, other muscle are normal �Class II: Mild weakness affecting other muscle �Class IIa: Muscles weakness affecting limbs and possibly oropharyngeal muscles �Class III: Moderate weakness/severe ocular weakness �Class IV: Severe weakness affecting limb muscle �Class V: Defined by intubation

Pathophysiologic Type �Ocular Myasthenia Gravis �Classic General Myasthenia Gravis �Transient Neonatal Myasthenia Gravis �Juvenile Myasthenia Gravis �Congenital Types �Drug-induced (Pencillamine, NDMR, aminoglycosides, procainamide)

Presenting Symptoms �Bilateral or Unilateral Ptosis �Diplopia �Hoarseness �Altered Speech �Problems chewing �Dysphagia �Limited Facial Expressions

Diagnostic Procedures �Endrophonium (tensilon) Chloride Test � 2. 6 -3. 3 mg initial dose Neostigmine may be used in patients who do not respond to tensilon �Auto-antibodies in MG – receptor binding antibodies are present in 80% of patients �Thymic hyperplasia is present in 70%

Diagnostic Procedures (continue) �Electromyography (EMG) Testing �Repetitive Nerve Stimulation (RNS) �Single Fiber EMG (SFEMG) �Ocular Cooling �Other Testing

Differential Diagnosis �Congenital Myasthenia Syndromes (not autoimmune) �Drug induced MG �Eaton-Lambert Syndrome (related to Small cell carcinoma of the lung) �Hyperthyroidism (increases MG symptoms) �Graves disease �Botulism �Ophthalmoplegia �Intracranial pathology

Factors that Worsen MG � Fatigue or insufficient sleep � Stress, anxiety, illness � Overexertion, repetitive motion � Pain or depression � Low potassium or thyroid levels � Alcoholic beverages � Sudden fear, or extreme anger � Extreme temperatures � Humidity � Sunlight or bright lights � Hot foods or beverages � Medications (beta blockers, antibiotics, calcium blockers) � Chemicals such as household cleaner, insecticides, pet sprays, lawn chemicals

Treatment for Myasthenia Gravis �Cholinesterase inhibitor � Pyridostigmine – most commonly used � Neostigmine – used less frequently �Thymectomy �Plasmapheresis �Corticoid Steroid Therapy �Immunosuppressive therapy (azathioprine, cyclosporine, etc. ) �Short-term Immunotherapy (IV immunoglobulin)

Anesthetic Comsiderations �Current health and symptoms �PMH/PSH �NMBA – Monitoring �Post operative plan �Pain control �Induction and Extubation criteria

Case Discussion #1 � 46 year old male diagnosis with MG in 6/2006 � Presenting symptoms: fatigue and weakness after working out with intermittent dipoplia � At time of diagnosis weakness lead to respiratory failure leading ventilation and respiratory support x 3 days � Residual symptoms: weakness, pain and left ptosis � Refractory to medical support under went a thymectomy in October 2009

Case Discussion (Continued) �Height/Weight: 75”/95=4. 7 �PFT’s FVC=65%, FEV 1/FVC=61% �Did not take his Pyridostigmine this am as he was instructed not to take it (not by anesthesia department)

What did we do? ? �Gave Pyridostigmine 90 mg preoperatively IV �Additional dose give at 1400 in recovery room �Induction included: slow induction no neuromuscular blocking agents Total Agents included: Propofol 400 mg Fentanyl 300 Morphine 4 mg Midazolam 3 mg Intubation with glidescope secondary to NIM’s tube placement.

Patient Outcome �Successfully extubated at end of case �Received pyridostigmine in recovery room �ICU overnight �Discharge next day.

Case Discussion #2 � 63 year old male �Diagnosis between 12/05 and 2/06 �Schedule for Laparoscopic Nissen Fundoplication �Multiple drug allergies �Ex-smoker (2 PPD x 30 years) �H/O: MG controlled with medications, HTN, diet controlled, AST – normal with EF 55 -65% �Hiatal Hernia/Barrett’s Esophagus �Previous surgery included: Brow lift, Laparoscopic Cholecystectomy

How did the case finish? ? � Previous anesthetic records � Surgeons desire muscle relaxation � We did: � Propofol 350 mg � Fentanyl 400 mcg � Midazolam 2 mg � Zofran/Decadron � Ephedrine 15 mg � Vasopressin 2 units Patient’s was successfully extubated in OR and discharge home the next day



Thank you for your attention Questions? ?

- Slides: 25