Musculoskeletal fractures Nancy Lin RN MS Adapted from



















































- Slides: 78

Musculoskeletal- fractures Nancy Lin, RN, MS Adapted from Kara Potter

SLO’s ¡ Compare and contrast clinical manifestations, pathophysiology, clinical treatments and management of pediatric clients with congenital and acquired musculoskeletal conditions

SLO’s ¡ ¡ Compare and contrast clinical manifestations, pathophysiology, clinical treatment and nursing management of pediatric and adult clients with acquired musculoskeletal conditions. Analyze the nursing process for clients with musculoskeletal conditions.

FUNCTIONS OF THE SKELETAL SYSTEM ¡ ¡ ¡ SUPPORT PROTECTION MOVEMENT HEMATOPORESIS MINERAL STORAGE

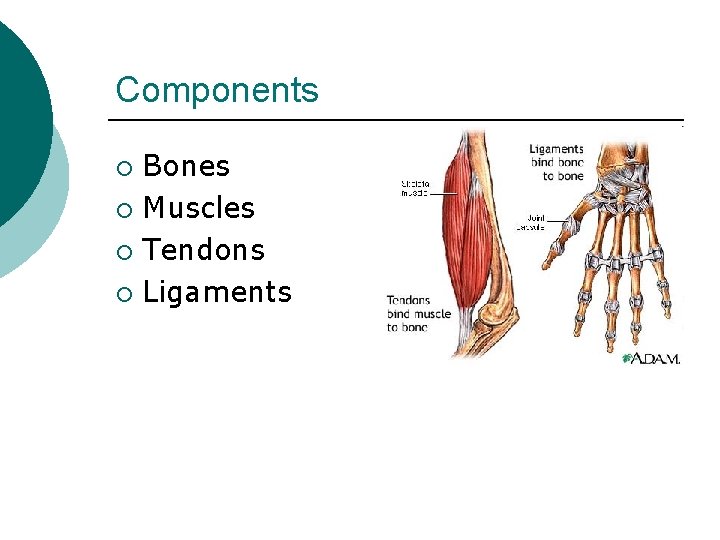
Components Bones ¡ Muscles ¡ Tendons ¡ Ligaments ¡

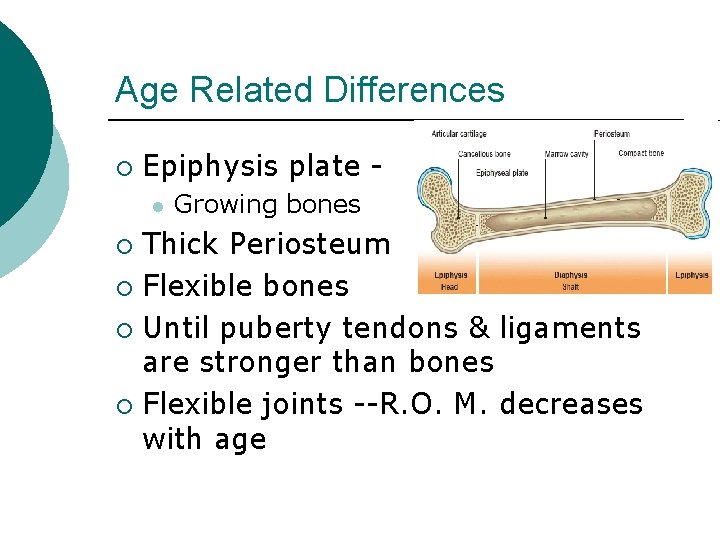
Age Related Differences ¡ Epiphysis plate l Growing bones Thick Periosteum ¡ Flexible bones ¡ Until puberty tendons & ligaments are stronger than bones ¡ Flexible joints --R. O. M. decreases with age ¡

Diagnostic Tests X-rays ¡ Arthrography - dye injected into joint ¡ l l l under local anesthetic rest joint for 12 hours compression bandage to reduce swelling

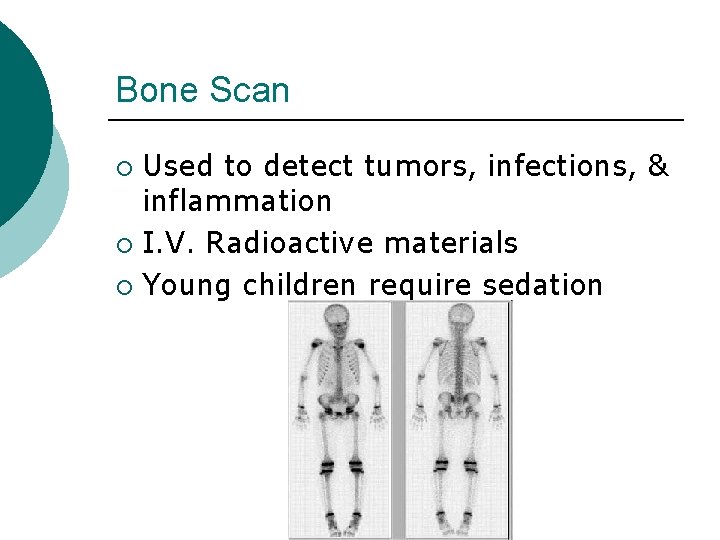
Bone Scan Used to detect tumors, infections, & inflammation ¡ I. V. Radioactive materials ¡ Young children require sedation ¡

Computed Tomography Scan (CAT) Used to visualize anatomic details ¡ Narrow x ray beam - 3 D cross section ¡ Contrast dye may be used ¡ Painless but frightening ¡ Youngsters may require sedation ¡

MRI Organ structures clearly defined ¡ Often used to diagnose ligament and muscle tears ¡ Unrestricted food & fluid ¡ Length of test - one hour or more ¡ Sedation may be needed ¡

Fractures Disruption or break in continuity of the structure of bone ¡ Majority of fractures from traumatic injuries ¡ Some fractures secondary to disease process ¡ l Cancer or osteoporosis

Classification ¡ Fractures are described and classified according to l l l Type Comminution Anatomic location of fracture on involved bone

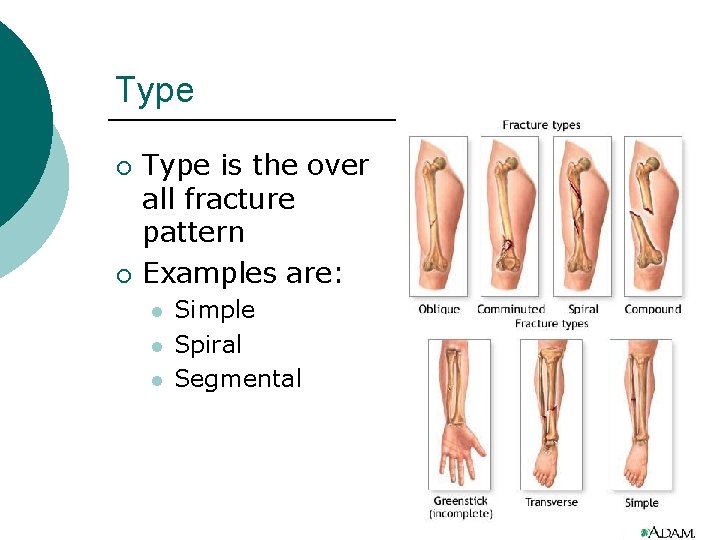
Type ¡ ¡ Type is the over all fracture pattern Examples are: l l l Simple Spiral Segmental

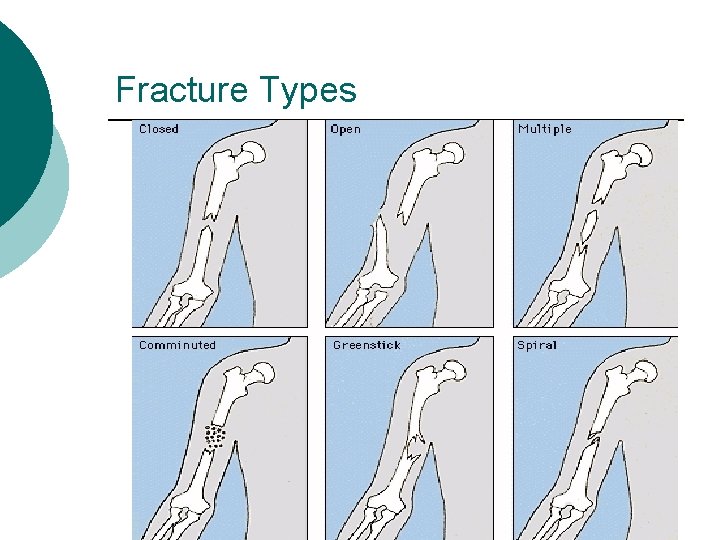
Fracture Types

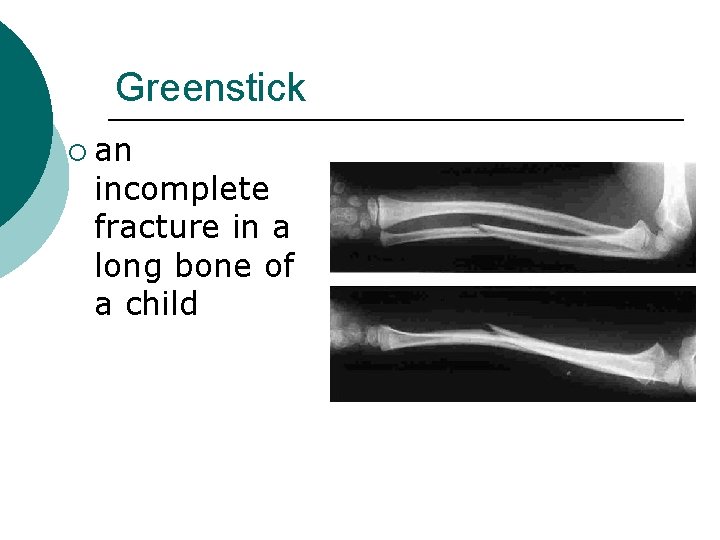
Greenstick ¡ an incomplete fracture in a long bone of a child

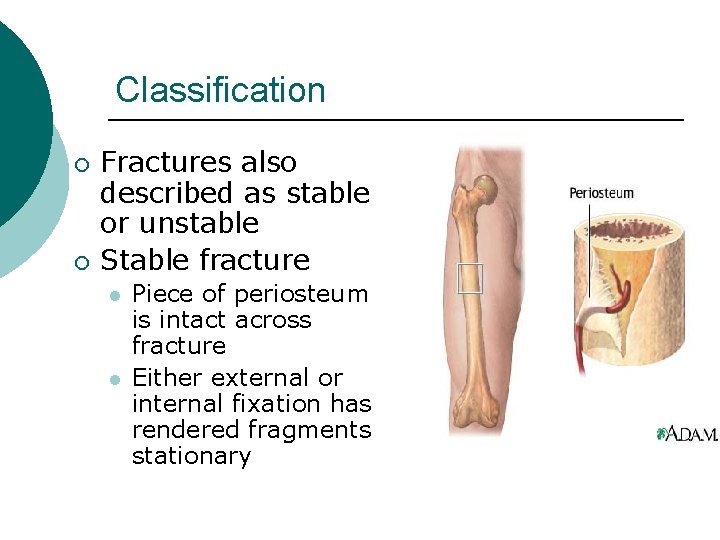
Classification ¡ ¡ Fractures also described as stable or unstable Stable fracture l l Piece of periosteum is intact across fracture Either external or internal fixation has rendered fragments stationary

Classification ¡ Unstable fracture Grossly displaced during injury l Site of poor fixation l Usually comminuted or oblique l

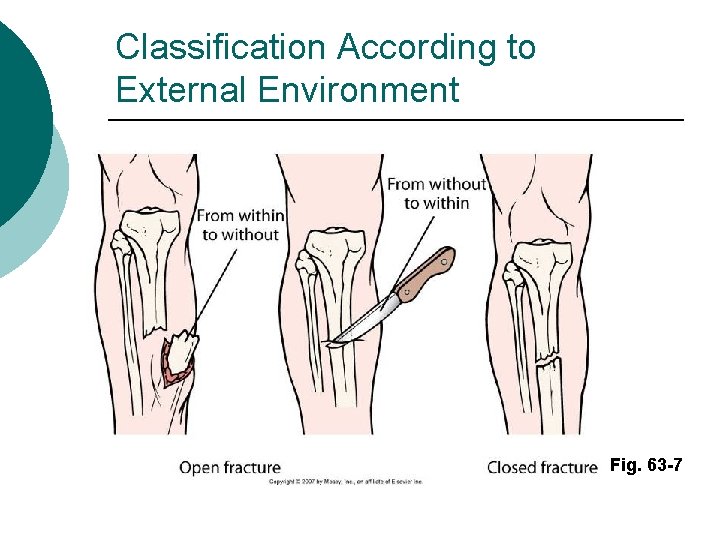
Classification According to External Environment Fig. 63 -7

Anatomic description Comminution is the measure of the number of pieces of broken bone that there are. ¡ Examples: ¡ l l l non-comminuted mildly comminuted severely comminuted

Anatomic description - Location Anatomic location of fracture usually described by giving the bone involved and location on the bone ¡ Examples: distal radial shaft, proximal 1/3 humeral shaft, intraarticular distal tibial ¡

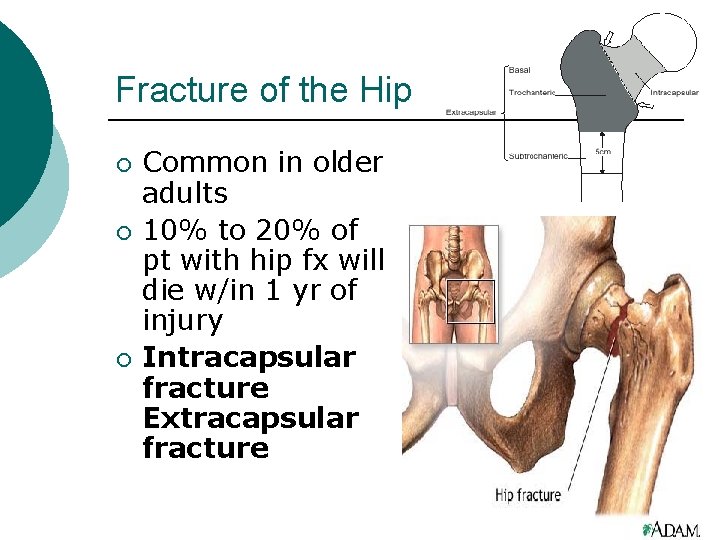
Fracture of the Hip ¡ ¡ ¡ Common in older adults 10% to 20% of pt with hip fx will die w/in 1 yr of injury Intracapsular fracture Extracapsular fracture

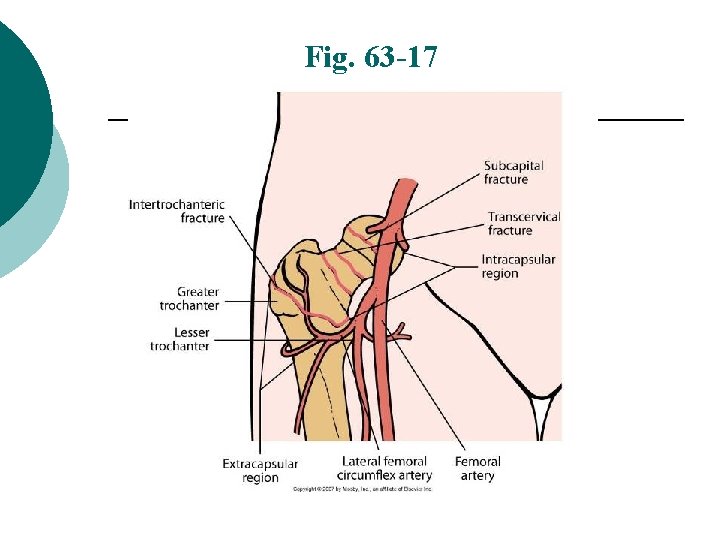
Fig. 63 -17

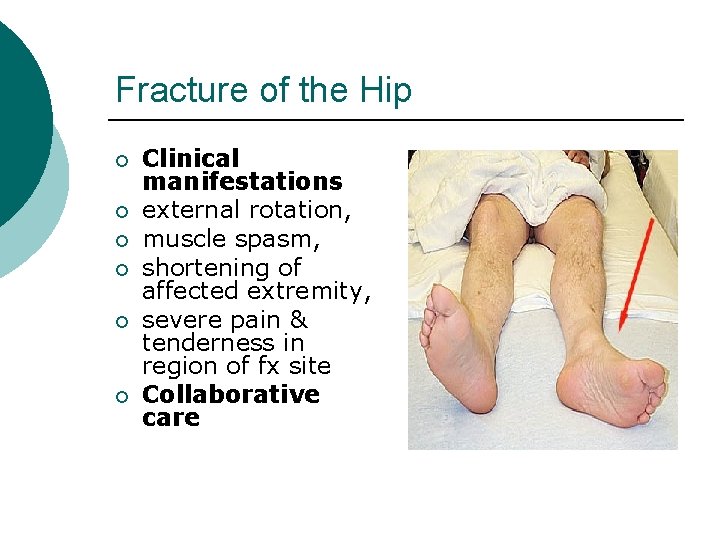
Fracture of the Hip ¡ ¡ ¡ Clinical manifestations external rotation, muscle spasm, shortening of affected extremity, severe pain & tenderness in region of fx site Collaborative care

Gerontology Considerations Hip Fracture ¡ ¡ ¡ Inadequacy of local tissue shock absorbers Underlying skeletal strength Interventions to reduce hip fx in elderly: - Calcium & Vit D supplementation - estrogen replacement - bisphonate drug therapy

Hip Fx Treatment ORIF ¡ Preoperative management ¡ Postoperative management ¡

Colles’ Fracture ¡ ¡ Fx of distal radius One of most common fx in adults Usually occurs when pt attempts to break a fall with an outstretched arm & hand Most often occur in women >age 50 whose bones are osteoporotic

Colles’ Fracture ¡ Clinical Manifestations: • Complications: - vascular insufficiency - carpal tunnel syndrome • Management:

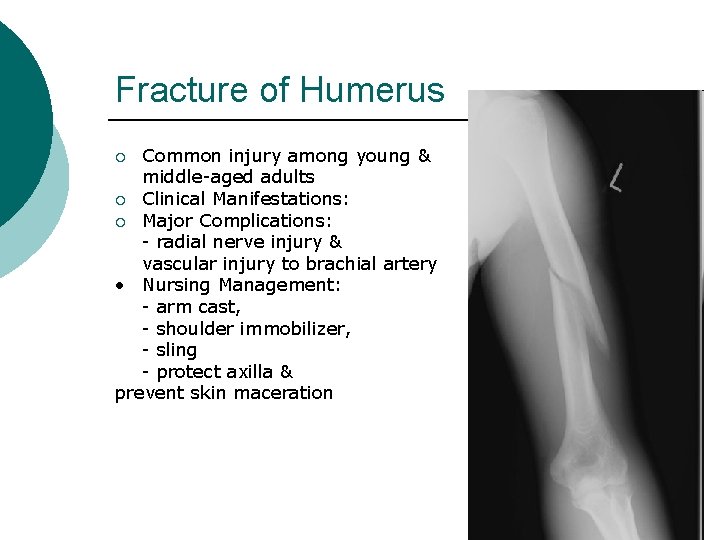
Fracture of Humerus Common injury among young & middle-aged adults ¡ Clinical Manifestations: ¡ Major Complications: - radial nerve injury & vascular injury to brachial artery • Nursing Management: - arm cast, - shoulder immobilizer, - sling - protect axilla & prevent skin maceration ¡

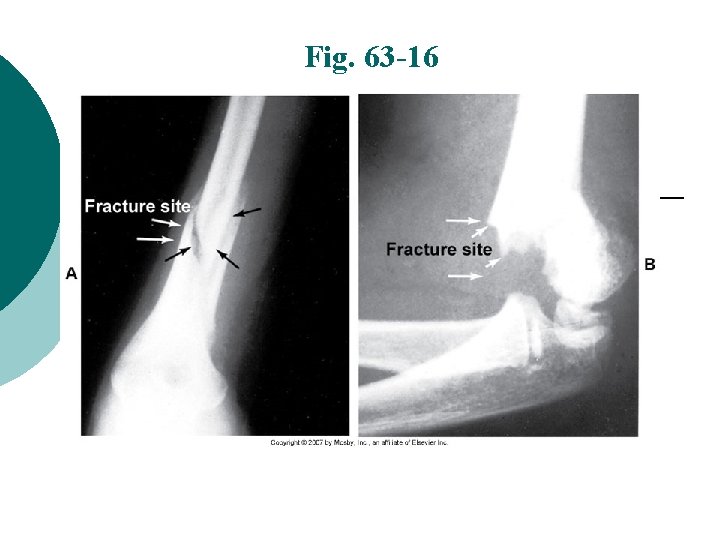
Fig. 63 -16

Pelvis Fracture ¡ ¡ Pelvic fx range from benign to life threatening Small percentage of all fx are pelvic fractures, associated with highest mortality rate May cause serious intraabdominal inj Patients may survive initial pelvic injury, only to die from sepsis, FES, or DVT complications

Pelvis Fracture ¡ Clinical Manifestations ¡ Treatment

Stable Vertebral Fractures ¡ Fracture or fragment not likely to move or cause spinal cord damage l ¡ ¡ Often in lumbar regions Vertebral bodies usually protected from displacement by intact spinal ligaments All spinal injuries should initially be considered unstable & potentially serious until tests are performed & fx is determined to be stable

Facial Fractures ¡ Primary concern: - establish & maintain patent airway - provide adequate ventilation by removal of foreign material & blood - alternative airway may be needed if patent airway cannot be maintained - all patients with facial injuries should be ruled out for cervical injury

Fracture Clinical Manifestations ¡ Mechanism of injury associated with numerous signs and symptoms Edema & Swelling l Pain & Tenderness l Muscle Spasm l Deformity l Ecchymosis/Contusion l Loss of Function l Crepitation l

Fracture Clinical Manifestations Fracture may not be accompanied by obvious bone deformity ¡ Immobilize extremity if fracture is suspected ¡ Unnecessary movement l Increases soft tissue damage l May convert a closed fracture to open ¡

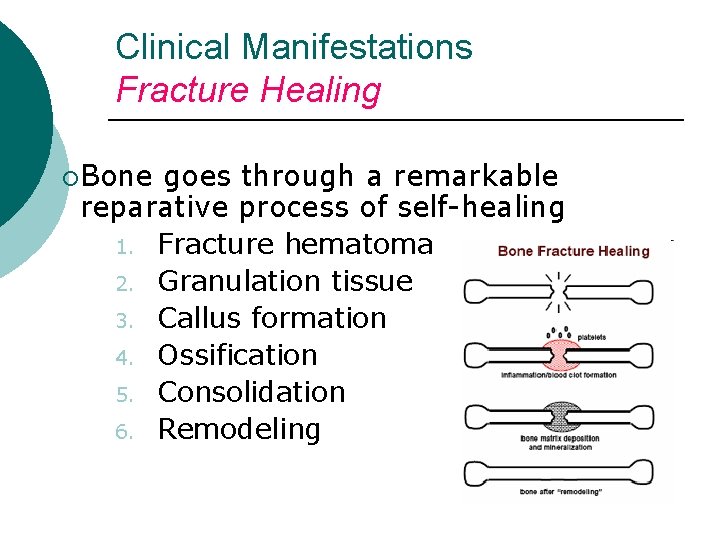
Clinical Manifestations Fracture Healing ¡Bone goes through a remarkable reparative process of self-healing 1. Fracture hematoma 2. Granulation tissue 3. Callus formation 4. Ossification 5. Consolidation 6. Remodeling

Clinical Manifestations Fracture Healing ¡ Factors influencing healing ¡Age ¡Initial displacement ¡Immobilization ¡Implants ¡Site ¡Infection ¡Hormones ¡Blood supply to area

Clinical Manifestations Fracture Healing ¡ ¡ Fracture healing may l Not occur in the expected time ¡ Delayed union l Not occur at all ¡ Nonunion Healing time of fractures increases with age

Collaborative Care ¡ Overall goals of fracture treatment Anatomic realignment of bone fragments l Immobilization to maintain realignment l Restoration of normal or nearnormal function of injured parts l

Nursing Management Nursing Assessment ¡ Initial treatment Splint joints l Check neurovascular status l Elevate l Do not attempt to straighten fractured or dislocated joint l Do not manipulate protruding bone ends l

Nursing Management Nursing Assessment ¡ ¡ ¡ ¡ ¡ Monitor for 5 P’s Deformity of affected limb Edema and ecchymoses Muscle spasm Tenderness and pain Loss of function Numbness, tingling, loss of distal pulse Grating (crepitus) Open wound over injured site, exposure of bone

Nursing Management Nursing Assessment ¡ Initial treatment ice packs l x-rays l Mark location of pulses l Splint fracture site l Elevate l

Initial Care ¡ Immobilize +Maintain alignment l l ¡ Splints Slings Cast Manual Traction Elevate

Splint

Sling

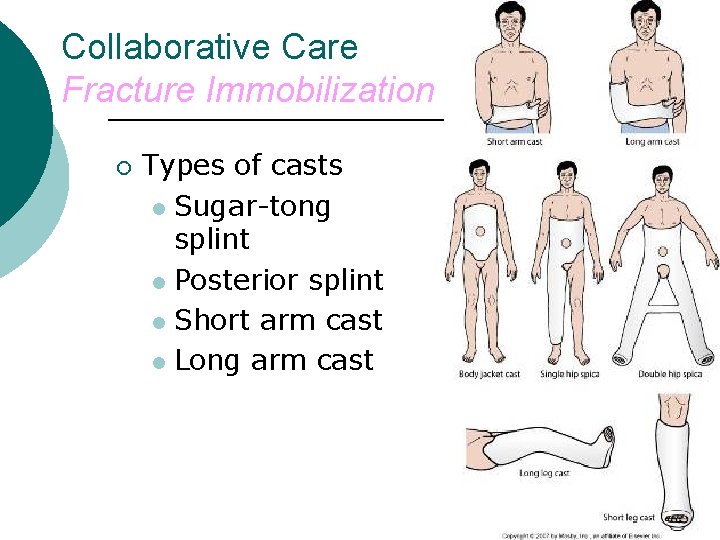
Collaborative Care Fracture Immobilization ¡ Types of casts l Sugar-tong splint l Posterior splint l Short arm cast l Long arm cast

Collaborative Care Traction Application of a pulling force to an injured part of body or extremity while counter traction pulls in opposite direction ¡ Purpose of any traction ¡ l l Prevent or ↓ muscle spasm Immobilize joint or part of body ↓ a fracture or dislocation Treat a pathologic joint condition

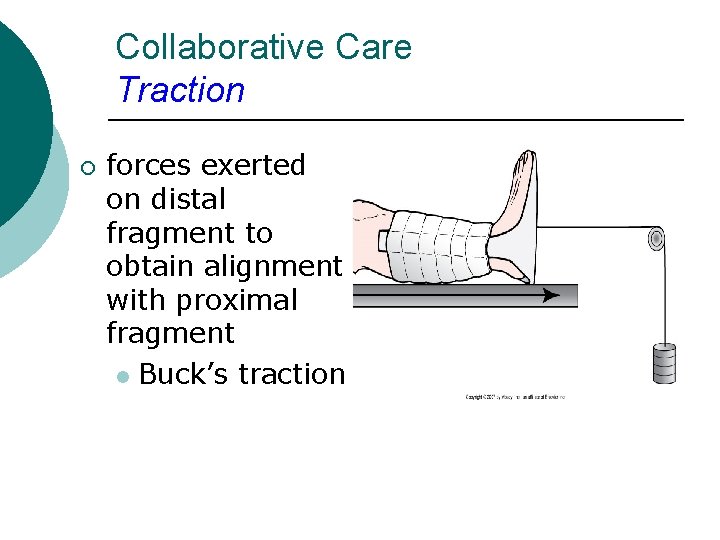
Collaborative Care Traction ¡ forces exerted on distal fragment to obtain alignment with proximal fragment l Buck’s traction

Traction

Collaborative Care Traction ¡ Traction also indicated to l l l Provide immobilization Reduce muscle spasm Expand a joint space During arthroscopic procedures ¡ Before major joint reconstruction ¡

Collaborative Care Traction ¡ Two most common types of traction l l Skin traction Skeletal traction

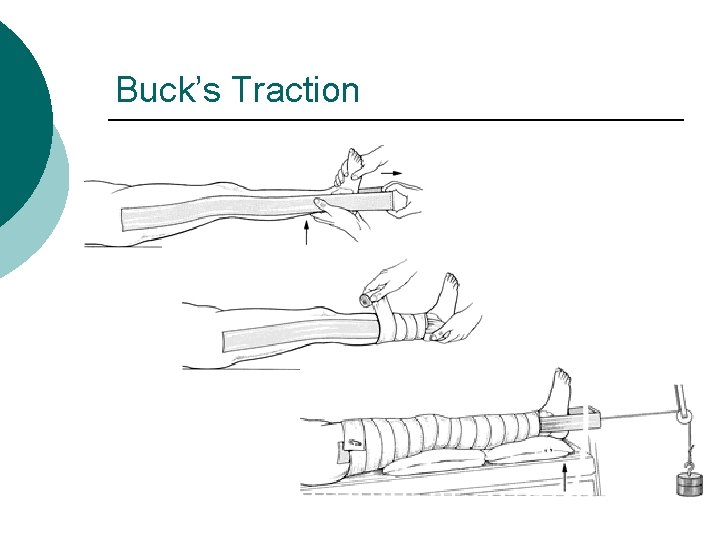
Buck’s Traction

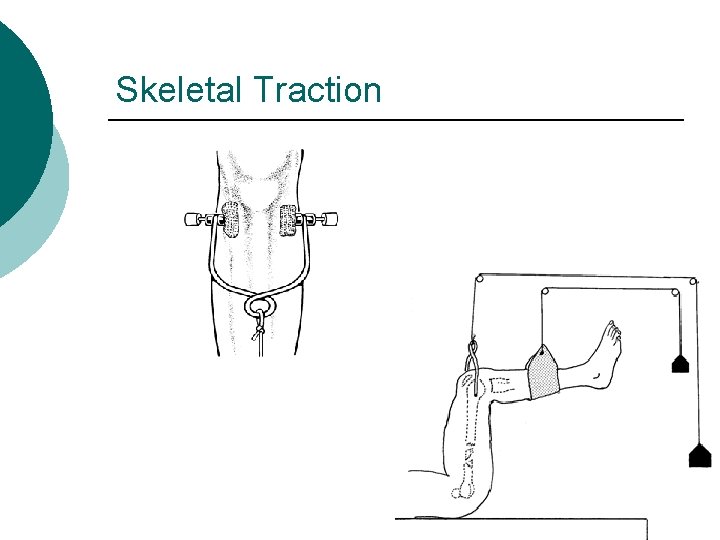
Skeletal Traction

Application of Skin Traction ¡ http: //www. youtube. com/watch? v= 2 ZEWz_Ps 7 vo&feature=related

Collaborative Care Fracture Reduction ¡ Closed l l reduction manual realignment of bone without surgery Traction and counter-traction Performed while patient is under local or general anesthesia Need to be splinted or casted after

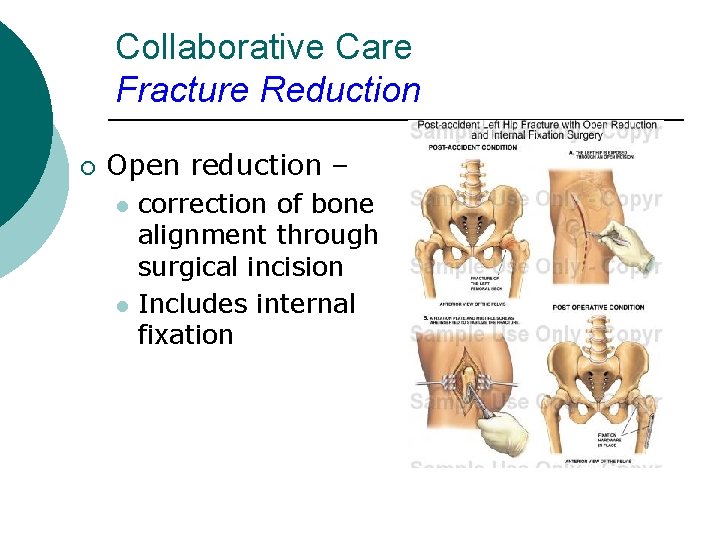
Collaborative Care Fracture Reduction ¡ Open reduction – l l correction of bone alignment through surgical incision Includes internal fixation

Collaborative Care Fracture Immobilization ¡ Internal fixation devices: surgically inserted at time of realignment l l l Pins Plates Screws Wires Rods Nails

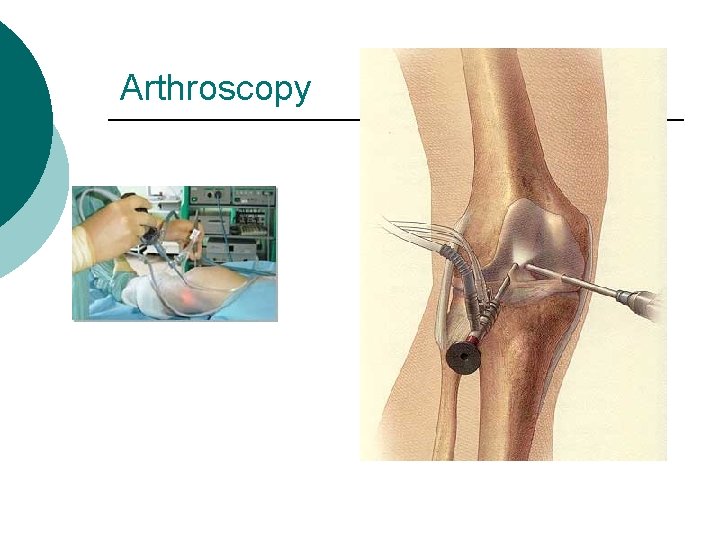
Arthroscopy For visualization inside the joint ¡ Dx or repair ¡ Local or may be general anesthesia ¡ NPO 8 hours pre op ¡ Antibiotics - prn ¡

Arthroscopy

Nursing Assessments Fracture ¡ CSMT’s l l l ¡ AKA neurovascular checks Circulation Sensation Motion temperature Pin sites with traction

Collaborative Care Nutritional Therapy ¡ ¡ ¡ Patient’s dietary requirements must include l Ample protein l Vitamins l Calcium, Phosphorus, Magnesium Adequate fluid intake: 2000 to 3000 ml/day High-fiber diet with fruits and vegetables

Collaborative Care Drug Therapy up to date with Tetanus ¡ Open fracture need bonepenetrating abx: ¡ cephalosporins – ¡ l kefzol, ancef

Complications of Fractures Majority heal without complication ¡ If death occurs, usually result of ¡ l l ¡ Damage to underlying organs and vascular structures Complications of fracture or immobility May be either direct or indirect

Complications of Fractures ¡ Direct complications l Problems with bone infection l Bone union l Avascular necrosis ¡ Fat embolism ¡ Traumatic or hypovolemic shock ¡ Indirect complications l Blood vessels and nerve damage ¡ Compartment syndrome ¡ Deep vein thrombosis

Complications of Fractures ¡ Infection l l l High incidence in open fractures and soft tissue injuries Massive or blunt soft tissue injury often has more serious consequences than fractures Devitalized and contaminated tissue: ideal medium for pathogens Costly Treatment Osteomyelitis may become chronic

Collaborative Care Open fractures require aggressive surgical debridement ¡ Extent of soft tissue damage determines whether ¡ l l l Wound will be closed at time of surgery Drainage may be necessary Skin grafting may be needed

Compartment Syndrome ¡ http: //www. youtube. com/watch? v= 4 l. KKBWWEr. HM

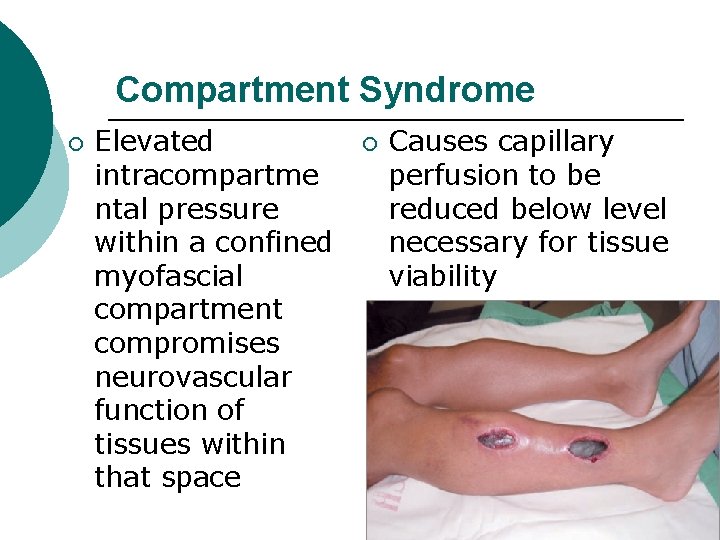
Compartment Syndrome ¡ Elevated intracompartme ntal pressure within a confined myofascial compartment compromises neurovascular function of tissues within that space ¡ Causes capillary perfusion to be reduced below level necessary for tissue viability

Compartment Syndrome ¡ Two types include: - ↓ compartment size resulting from restrictive dressings, splints, casts, excessive traction, or premature closure of fascia - ↑ compartment content related to bleeding, edema, chemical response to snakebite, or IV infiltration

Compartment Syndrome ¡ Associated with trauma - fractures - extensive soft tissue damage - crush injury - reperfusion syndrome - severe burns - venomous snakebite - following knee or leg surgery - prolonged pressure on a muscle compartment - massive infiltration of IV fluids -

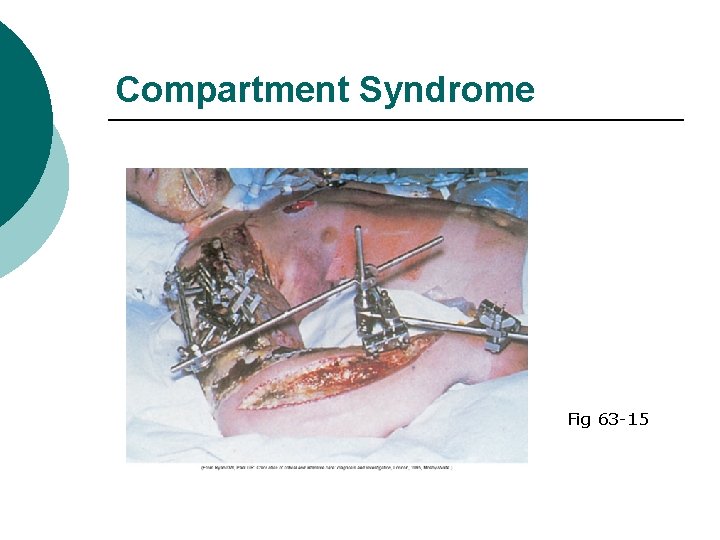
Compartment Syndrome Fig 63 -15

Compartment Syndrome Clinical Manifestations & Nsg Management Early recognition and treatment essential ¡ Ischemia can occur within 4 to 12 hours after onset ¡ Regular neurovascular assessments ¡

Compartment Syndrome Clinical Manifestations ¡ Six Ps are characteristic of impending compartment syndrome 1. 2. 3. 4. 5. 6. P P P

Compartment Syndrome Clinical Manifestations & Nsg Mgt Assess urine output ¡ Acute renal failure ¡ Myoglobin released can obstruct renal tubules ¡ Common signs of myoglobinuria ¡ l l Dark reddish brown urine Clinical manifestations associated with acute renal failure

Compartment Syndrome Collaborative Care ¡ ¡ ¡ Extremity SHOULD NOT be elevated above heart level DO NOT apply cold compresses Remove or loosen bandage or bivalve cast Reduction in traction weight may ↓ external circumferential pressures Surgical decompression may be necessary Severe compartment syndrome may require amputation

Venous Thrombosis ¡ Precipitating factors l ¡ ¡ Venous stasis Aggravated by inactivity of muscles that normally assist in pumping action of venous blood Instruct patient to l l Wear compression gradient stockings Move fingers or toes of affected extremity against resistance and perform ROM exercises

Venous Thrombosis Prophylactic anticoagulant drugs may be ordered ¡ Low-molecular-weight heparin (lovenox) frequently used ¡ Newer class of antithrombotic drugs - fondaparinux (arixtra) ¡

References Hockenberry, M. J. & Wilson, D. (2015). Wong’s Nursing care of infants and children (10 th ed. ). St. Louis, MO: Mosby. Lewis, S. , Heitkemper, M. & Dirksen, S. (2014). Medical Surgical Nursing: Assessment and Management of Clinical Problems (9 th ed. ). St. Louis, MO: Mosby Potter, K (2009) Musculoskeletal. Presented at Evergreen Valley College Touhy, T. & Jett, K. (2014). Ebersole & Hess’ Gerontological Nursing Healthy Aging (4 th Ed. ) St. Louis: Mosby/Elsevier