Muscle Relaxants 4 th year Anaesthesia MBCh B

Muscle Relaxants 4 th year Anaesthesia MBCh. B
Triad of Anaesthesia Hypnosis Muscle Relaxation Analgesia

Physiology of the NMJ (neuromuscular junction) • Excitation-contraction coupling – Nervous impulse is converted into a skeletal muscle contraction at the NMJ • Acetylcholine (Ach) – Key neurotransmitter at the NMJ – Formed from ACETYL Co. A + CHOLINE – Stored in pre-synaptic vesicles – Binds to NICOTINIC cholinergic receptors on postjunctional membrane – Broken down by Acetylcholinesterase (ACh. E)
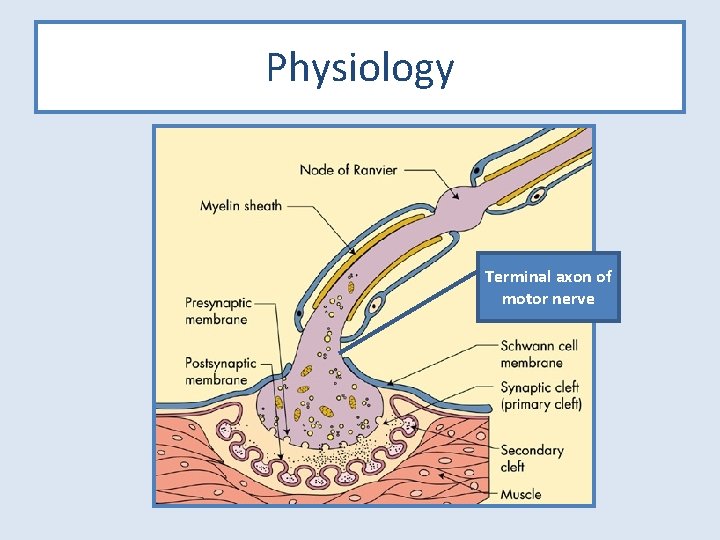
Physiology Terminal axon of motor nerve
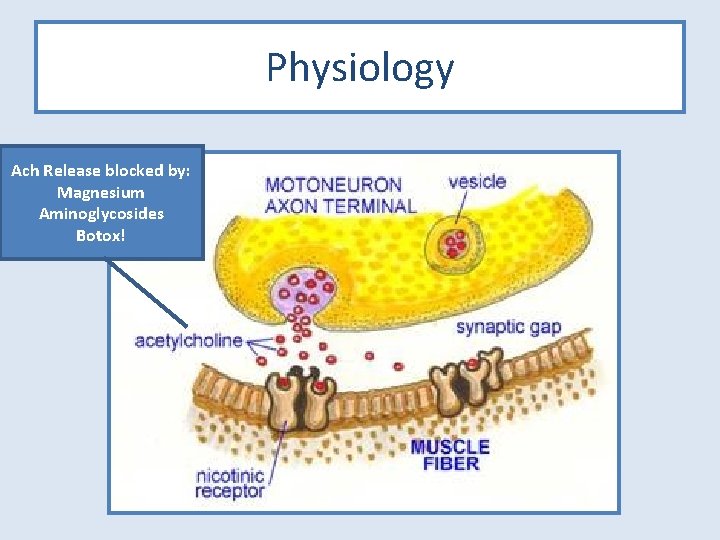
Physiology Ach Release blocked by: Magnesium Aminoglycosides Botox!

Pharmacology • 3 ways to achieve muscle relaxation • Blocking the. . . 1. nerve (local anaesthetics) 2. NMJ (muscle relaxants) 3. muscle (dantrolene)

History • Dates back to the 16 th century • European explorers encountered the Amazonians in South America using poison arrows that produced death by skeletal muscle paralysis! • This poison, known today as curare – active ingredient, tubocurarine

History • By 1943, neuromuscular blocking drugs became established as muscle relaxants in the practice of anaesthesia and surgery

Neuromuscular Blockers • 2 types – Depolarisers – Non-depolarisers

Mechanism of Action Depolarisers • Non-competitive • Cannot be reversed Non-depolarisers • Competitive • Compete with Ach for nicotinic receptors • Require reversal

ED 95 • Dose of muscle relaxant that will paralyse 95% of normal people • Usual intubating does: 2 x ED 95

Total paralysis • Adequate does of muscle relaxant will result in: – Inability to breath – Inability to maintain an airway – Loss of protective reflexes Consciousness is completely unimpaired!!!
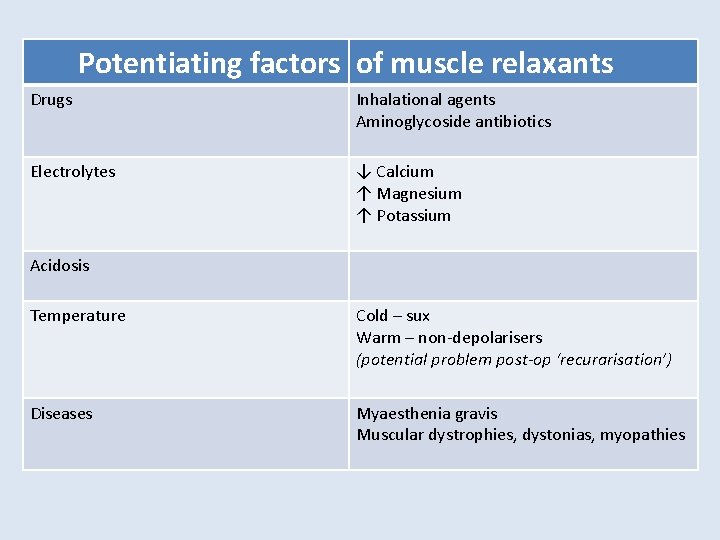
Potentiating factors of muscle relaxants Drugs Inhalational agents Aminoglycoside antibiotics Electrolytes ↓ Calcium ↑ Magnesium ↑ Potassium Acidosis Temperature Cold – sux Warm – non-depolarisers (potential problem post-op ‘recurarisation’) Diseases Myaesthenia gravis Muscular dystrophies, dystonias, myopathies

Indications • Improved surgical access • Facilitate intubation or bronchoscopy • Prevention of movement in microsurgery – Unconscious patients can still move! • Manipulation of fractures • Prevention of / treatment of convulsions • ICU – – Tetanus Severe lung disease Severe uncontrolled shivering Severe ↑ ICP

Precautions • So, Must ventilate a patient who you paralyse the person administering the – IPPV with the mechanical ventilator muscle – Reservoir bag relaxant must. . . – Self-inflating bag (ambubag) 1) assess the airway Via. . . 2) be competent in maintenance – Facemask of a patent airway – LMA – ETT 3) have necessary equipment

Specific Muscle Relaxants

Suxamethonium • Chemical structure: – 2 Ach molecules • Amp: 100 mg (2 mls) • Dose: 1 -2 mg / kg • Effects: – Profound paralysis in 60 sec – Ultra-shortacting – fasciculations – Lasts 5 minutes • Excretion: – Metabolised by pseudocholinesterase or plasma cholinesterase • Synthesised in liver • Found in plasma • Markedly ↓ed in SCOLINE APNOEA – Inherited homozygous or heterozygous – Prolonged paralysis – Supportive treatment with ventilation + sedation – FFPs

Suxamethonium • Side-effects: – Scoline pains – Bradycardias – Hyperkalaemia and arrhythmias, even cardiac arrest – Triggers Malignant Hyperthermia – Scoline Apnoea – Histamine release – Anaphylaxis • Contra-indications: – – – Drug allergy Scoline apnoea MH Unknown myopathies Risk of hyperkalaemia • Renal failure • Paralysis • Crush / Burn injury

Non-depolarisers • Types: – Benzolisoquinolinium compounds • Curare, alcuronium, atracurium, cisatracurium, mivacurium – Aminosteroids • Rocuronium, vecuronium, pancuronium • Doses: based on lean body mass • Physical properties: – 2 – 5 ml ampoules – May require refrigeration

Non-depolarisers • Clinical effects: – Marked paralysis in 1 – 5 minutes – No fasciculations – Duration is variable • Short-acting • Intermediate-acting • Long-acting • Metabolism: – Hepatic – Hoffman degradation • Excretion: – Renal – Hepatobiliary – Pseudocholinesterase

Reversal of neuromuscular blockade • Neostigmine – Acetylcholinesterase inhibitor – Increase Ach concentration in synaptic cleft – Ach COMPETES with NDMR – Others: pyridostigmine, edrophonium, organophosphates – But Ach ↑es at nicotinic and muscarinic receptors • Anticholinergic – ANTI-MUSCARINIC – Atropine or glycopyrrolate – Bad muscarinic effects (the B’s) • • Bronchial secretions Bronchospasm Bradycardia Beristalsis (peristalsis) Dose: Neostigmine 2. 5 mg Glycopyrrolate 0. 4 -0. 6 mg
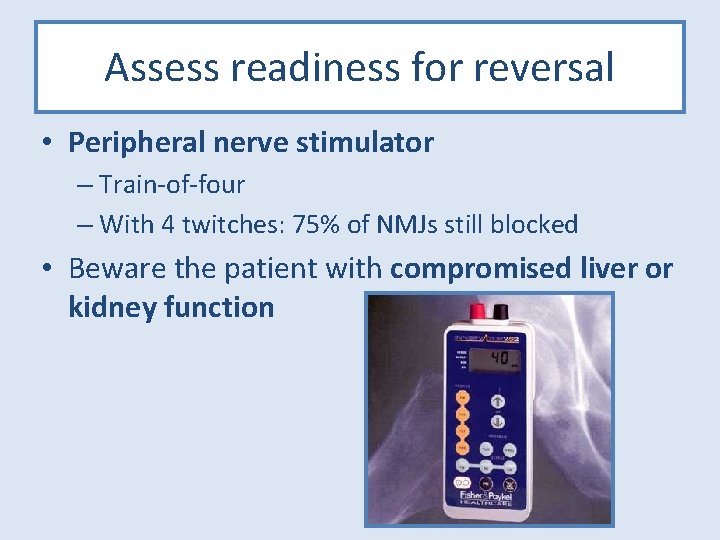
Assess readiness for reversal • Peripheral nerve stimulator – Train-of-four – With 4 twitches: 75% of NMJs still blocked • Beware the patient with compromised liver or kidney function

Inadequate Reversal ü Jerky respiration ü Reduced VT ü Tracheal tug ü Restlessness, may be worsened by hypoxia ü Inability to raise head from pillow ü Weak hand grip “fish out of water” ü Poor ability to cough ü ptosis

This is how our patients feel when they are partially reversed

Management of Inadequate Reversal • Exclude another cause – Anaesthetic agents, analgesia, hypo or hypercarbia, CVA • Maintain ventilation • Reverse any potentiators – Warm patient – Check Mg, K, Ca • Use PNS • Repeat dose neostigmine (max: 5 mg) – Neostigmine in bigger doses can may cause weakness

Pancuronium • • Kept in fridge Vagolytic – tachycardia No histamine release Long-acting

Vecuronium • • • Kept in fridge Cardiovascularly stable No histamine release Intermediate-acting Largely hepato-biliary excretion therefore safe in renal failure

Rocuronium • Kept in fridge • Cardiovascularly stable • High dose: 1 mg/kg can provide intubating conditions within 1 minute – Modified RSI • Intermediate duration of action

Atracurium • Fridge • Histamine releasing – Increased risk of anaphylaxis • Hoffman degradation – Spontaneous – Dependent on p. H and temperature • Side-effect: laudanosine • Safe in renal failure • Intermediate duration of action

Cisatracurium • • Fridge No histamine release Safe in renal failure (Hoffmann Degradation) Intermediate-acting
- Slides: 31