Muscarinic Antagonists and other bronchodilators Ch 7 1

Muscarinic Antagonists and other bronchodilators Ch. 7 1
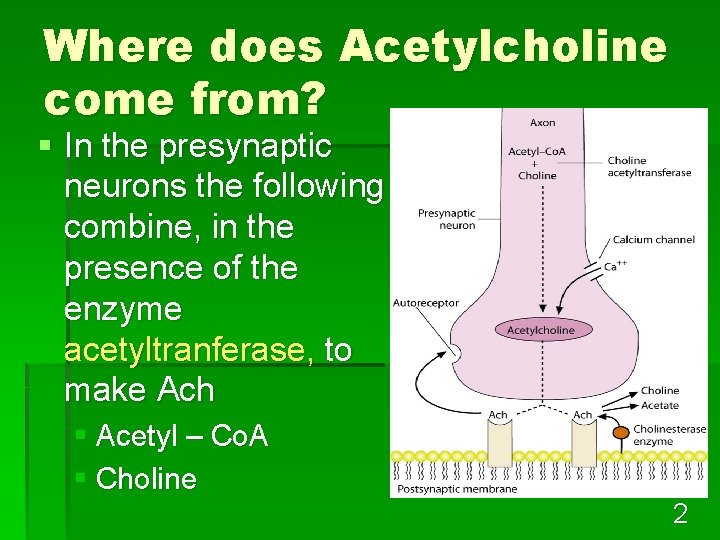
Where does Acetylcholine come from? § In the presynaptic neurons the following combine, in the presence of the enzyme acetyltranferase, to make Ach § Acetyl – Co. A § Choline 2

Where does Acetylcholine come from? § When the nerve impulse reaches the ganglion, there is an influx of Ca++ § 1000 to 50, 000 molecules of Ach per vesicle are released into the junction 3

Parasympathetic Receptors NTs and Termination § Acetylcholine (ACh) stimulates Muscarinic 3 (M 3) receptors § Action of ACh is terminated primarily by the enzyme acetylcholinesterase § Secondarily, ACh activates M 2 receptors on the presynaptic ganglion, which inhibits the release of ACh 4
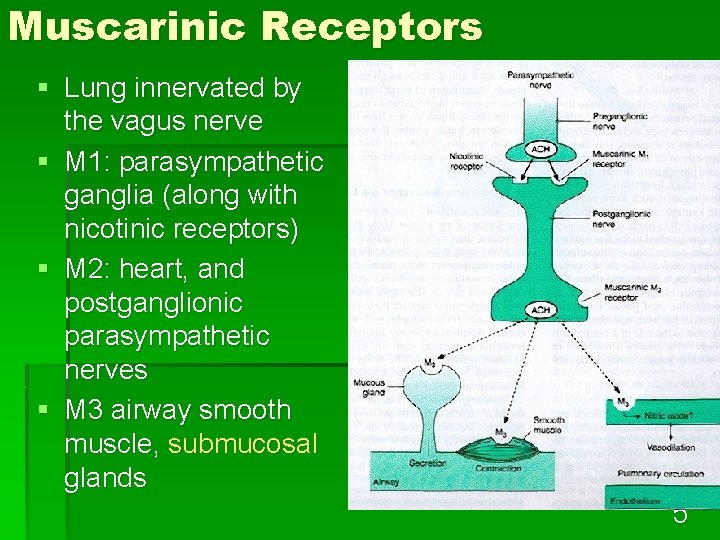
Muscarinic Receptors § Lung innervated by the vagus nerve § M 1: parasympathetic ganglia (along with nicotinic receptors) § M 2: heart, and postganglionic parasympathetic nerves § M 3 airway smooth muscle, submucosal glands § scan page 100 here 5

Blocking Muscarinic Receptors § Blocking… § M 3 receptors on smooth muscle and mucous glands § M 1 receptors on the postganglionic nerve § M 2 receptors on the end of the postganglionic nerve § All of our bronchodilators currently blockade all 3, including M 2 6
Remember the Cholinergic Effects § SLUG or SLUD 7

Remember the Cholinergic Effects § For us in the lung: § Increase in secretion production (exocytosis) § Bronchial smooth muscle contraction § M 3 receptor stimulation produces chain effect, end result of which is an influx of Ca++ into the cell causing muscle contraction 8

Anticholinergic Advantage § Parasympatholytics have shown long term improvement in baseline FEV 1 in COPD patients § No such improvement found using adrenergics, although still used § Unknown etiology, although may be from blocking Vagally mediated bronchoconstriction 9

Combination Therapy § Ventolin and Atrovent, when taken together, have a greater effect than either alone. § AKA = synergism § Why? § No one knows for sure, may be related to different time of onset, or times of peak effect 10

Xanthines – 2 nd or 3 rd line agents? Theories of action 1. inhibition of phosphodiesterase? § this is what breaks down c. AMP (we’ll talk about this later) § but it is not that good at it 2. antagonism of adenosine? § adenosine can agonize A 1 and A 2 receptors § but they don’t have that much to do with bronchodilation 11

Xanthines – 2 nd or 3 rd line agents? Theories of action 3. catecholamine release? § no conclusive evidence 4. move calcium so it can’t be used in muscle contraction? 12

What does Phosphodiesterase do? A bit of a review § When beta two receptor is activated by an agonist… § Stimulates Adenyl Cyclase § Adenyl Cyclase helps to convert adenosine triphosphate (ATP) into cyclic adenosine 3’, 5’ monophosphate (c. AMP); § phosphodiesterase breaks down the “good” c. AMP 13

What does Phosphodiesterase do? Continued § Cyclic AMP § increases the inactivation of protein kinase A, which leads to less myosin + actin interaction § lowers intracellular calcium (Ca) § Ultimately causing smooth muscle relaxation § Also results in inhibition of mast cell degranulation 14

Categorized a bronchodilator, but… § Bronchodilating effects are weak § Not a first line drug for asthma or COPD § Minimal to no improvement in pulmonary function studies § But may show clinical improvement § True benefit may come from other effects 15

Non-Bronchodilatory Benefits § Increased diaphragm strength-from improved muscle contractility § CNS Stimulationincreased ventilatory drive 16

More Non-Bronchodilatory Benefits § Anti-Inflammatory Effects § Improved Cardiac function (common comorbidity) § Diuresis (think caffeine but more potent) 17

Side effects: think Caffeine and more § neonates previously given theophylline for apnea of prematurity, now given caffeine (safer xanthine) § Side effects of theophylline… § § § headache, vertigo, diarrhea, nausea, vomiting anorexia nervousness, insomnia, irritability, tremor, hyperglycemia low electrolytes (hypokalemia, hypercalcemia, hypomagnesemia, hypophosphatemia) § cardiac arrhythmias leading to hypotension, § seizures, death 18

End of Show 19

Stop Here if this is Friday 20

What happens at the Muscarinic Three Receptor When Activated § Activation of phospholipase § Phospholipase helps to breakdown phosphoinositides to 1. inositol triphosphate (IP 3) 2. diacylglycerol (DAG) § This increases intracellular calcium (Ca++) § Ultimately causing smooth muscle contraction § Also results in gland exocytocis - submucosal gland produces secretions 21

Anticholinergics § Atropine is the naturally occurring alkaloid found in the Atropa Belladona (nightshade plant) and the Datura species § Dantura plants burned and inhaled as early as the 17 century in India § Atropine used as an adjunct to sympathomimetics in the 1980 s § Q. What’s another way to inhale a drug besides burning? § A. The Atropine was nebulized 22

ipratropium (Atrovent) § Available for use in a nebulized formula in 1987 § Short-acting (4 to 6 to 8 hrs) anti-cholinergic (antimuscarinic) § non-selectively blocks the M 1, M 2, and M 3 receptors § Q. Which one of these is the worst to antagonize if you’re goal is to help an an Asthmatic? § A. M 2 § indications: bronchoconstriction due to COPD and also to Asthma, etc 23

Revised-Eric Lau (slide 10 Beta 2) Bronchodilation: the hypothetical Nonadrenergic, noncholinergic (NANC) (continued) 1. (from the last slide) 2. Brochoconstriction may be caused by afferent C-fibers leading back to the CNS § § § C-fibers stimulated by a noxious substances (causes bronchoconstriction) C-fibers release a neuropeptide (a tachykinin) known as substance P Results in more bronchoconstriction and cough As well as vasodilation, increased vascular permeability, mucous gland secretion, mucocilliary activity Currently no pharmacological agents targeted toward NANC 24
![ipratropium inhaled Inhaled dosages and [ ]s § MDI 20 mcg/puff, 1 -2 puffs ipratropium inhaled Inhaled dosages and [ ]s § MDI 20 mcg/puff, 1 -2 puffs](http://slidetodoc.com/presentation_image_h2/79b0615db9ca2720310020cfb542b187/image-25.jpg)
ipratropium inhaled Inhaled dosages and [ ]s § MDI 20 mcg/puff, 1 -2 puffs § soln 0. 25 mg/m. L § nebules (many) § § § 0. 25 mg/ml in 1 m. L of drug 0. 125 mg/ml in 2 m. L “ “ 0. 25 mg/ml in 2 mls “ “ 25

ipratropium; dosages and routes § Dosage Frequencies (three examples) § Taken at same times as salbutamol (i. e. q 4 h, qid, prn) § Taken tid (when salbutamol taken qid) § Taken as “maintenance” bronchodilator on its own, with salbutamol as a “rescue” (COPD) § Other formulations § nasal spray 26

Atrovent (ipratropium): side effects § less side effects (cardiac, vasoactive) as it is fully ionized limiting systemic absorption § dry mouth § cough, pharyngitis § nervousness, irritation, § hypersensitivity reactions (laryngospasm, uticaria, etc) § headache, vertigo, diarrhea, nausea and vomiting § worsening of narrow angle glaucoma when it gets into the eyes (intraoccular pressure can rise) § should use t-piece when nebulizing to older 27 patients

Atrovent (ipratropium): drug times § § § Onset 5 - 15 min; CPS = ______ Peak 60 - 90 min; CPS = ______ Duration 4 to 6 to 8 hrs; CPS = ______ 28

Ventolin and Atrovent together: Combivent § Indicated for COPD maintenance § salbutamol and ipratropium combined § § § *MDI 100 or 120 mcg (sulfate) with 20 mcg Nebules 2. 5 mg with 0. 5 mg all in a 2. 5 ml soln bromide? sulphate? “Salts” or “formulations” § not synonymous § * discontinued in 2007 29

Spiriva (tiotropium) § Mode of action: § More selective for M 3 receptors dissociates from M 2 faster § 6 – 20 X more affinity for M 3 than ipratropium § Concentrations and Dosages § 18 mcg qday § Form and Delivery § “Handihaler” (DPI) capsules are crushed and inhaled § Repeat inhalation (of the single capsule) 2 or 3 times with reduced IC § http: //www. spiriva. com/consumer/taking-spiriva/spirivacapsules-and-handihaler. jsp § Action Times (onset, and duration) § 30 min, 3 hrs (peak) § Half life of 35 hrs – improves FEV 1 to max peak at one-week 30

4 Steps for the “HH” 31

Theophylline (a xanthine) § As a anti-inflammatory drug § Very small therapeutic index, therefore target the following blood levels § 55 -65 mmol/L § 10 -12 mcg/m. L § Salts of theophylline § § pure (100% theophylline) e. g. Theodur given orally aminophylline (85%) given IV oxtriphylline (Choledyl) (65%) given orally regular tabs or extended release capsules 32
- Slides: 32