Multiple Chronic Conditions MCC electronic Care Plan Project
















































- Slides: 59

Multiple Chronic Conditions (MCC) electronic Care Plan Project Overview: Jenna Norton Gay Dolin Evelyn Gallego Jerry Goodnough Katiya Shell

Agenda • • • Background Project Scope Approach Project Status Next Steps

BACKGROUND

https: //www. cdc. gov/chronicdisease/pdf/infographics/chronic-disease-H. pdf

The Multiple Chronic Condition (MCC) Patient • Accumulates a large team of care providers to manage their conditions • Has complex mixes of medical, social, behavioral, and functional issues • Has a large burden of chronic illness and functional impairment, complicated by changes in mood and cognition, and exacerbated by social determinants of health (SDOH) • Requires a team effort to achieve the goals they value

MCC Care Coordination for Patients & Clinicians Clinician Patient Clinician

Why Use e. Care Plans to Enable Care Coordination? 1. Give the person direct access to his or her information. 2. Put the person’s goals at the center of decision-making. 3. Are holistic, including clinical and non-clinical (e. g. , home. and community-based) needs and services. 4. Follow the person through both high-need episodes (e. g. , acute illness) and periods of health improvement and maintenance. 5. Allow clinicians to 1) view information relevant to their role in caring for the person, 2) identify which clinician is doing what, and 3) update other members of an interdisciplinary team. Baker, et al. Making the Comprehensive Shared Care Plan a Reality. NEJM Catalyst. 2016: https: //catalyst. nejm. org/making-the-comprehensive-shared-care-plan-a-reality/

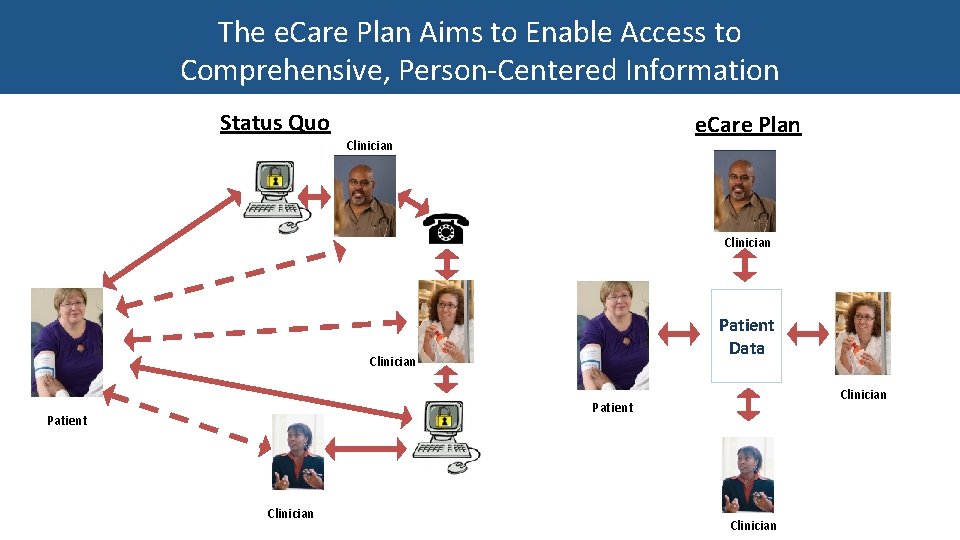
The e. Care Plan Aims to Enable Access to Comprehensive, Person-Centered Information Status Quo e. Care Plan Clinician Patient Data Clinician Patient Clinician

SCOPE

AHRQ-NIDDK MCC e. Care Plan Project Scope • Identify use cases to support the documentation and exchange of MCC e. Care Plan data within EHRs and other health technology systems; • Identify, develop, and prioritize the necessary MCC data elements, clinical information models (CIM), and FHIR mappings to enable the standardized transfer of data across health settings; • Develop and test an open-source clinician facing SMART on FHIR e. Care Plan application for managing persons with MCC; and • Develop, test, and ballot an HL 7® Fast Health Interoperability Resource (FHIR®) Implementation Guide based on the defined use cases and MCC data elements.

AHRQ-NIDDK MCC e. Care Plan Project Goals • Promote the interoperable collection, use, and sharing of comprehensive, person-centered health and social data across settings; • Facilitate coordinated, person-centered care planning approaches that integrate the full care team (including the patient) across settings; and • Build data capacity to conduct pragmatic Patient Centered Outcomes Research (PCOR). Chroni c Kidney Diseas e Diabet es Cardio vascul ar Diseas e Chronic Pain

APPROACH

AHRQ – NIDDK Project Approach 1. Develop & Test FHIR IG & SMART on FHIR e-care plan application – Identify existing or build new clinical information models (CIM)/FHIR profiles building on existing CKD data elements & standards – Develop e-care plan application and implementation guide (IG) for point of care data review/entry – Implement & evaluate the e-care plan application in diverse clinical settings in patients with MCC, including CKD 2. Establish an e-care plan repository and development collaborative 3. Expand the draft e-care plan application & IG to include cardiovascular disease (CVD), type 2 diabetes & chronic pain – Expand the CKD data elements & CIMs to consider additional conditions – Revise e-care plan application & IG to incorporate expanded DESS and pilot test feedback. 4. Disseminate all project deliverable through open source channels

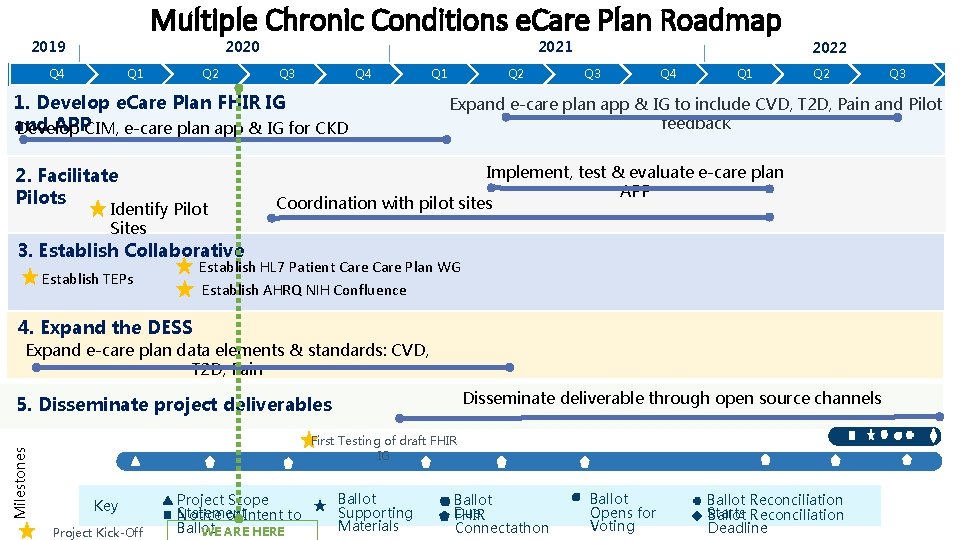
Multiple Chronic Conditions e. Care Plan Roadmap 2021 2020 2019 Q 4 Q 1 Q 2 Q 3 Q 4 1. Develop e. Care Plan FHIR IG and APPCIM, e-care plan app & IG for CKD Develop 2. Facilitate Pilots Identify Pilot Sites Q 1 Q 2 2022 Q 3 Q 4 Q 1 Q 2 Expand e-care plan app & IG to include CVD, T 2 D, Pain and Pilot feedback Implement, test & evaluate e-care plan APP Coordination with pilot sites 3. Establish Collaborative Establish HL 7 Patient Care Plan WG Establish AHRQ NIH Confluence Establish TEPs 4. Expand the DESS Expand e-care plan data elements & standards: CVD, T 2 D, Pain Disseminate deliverable through open source channels Milestones 5. Disseminate project deliverables First Testing of draft FHIR IG Key Project Kick-Off Project Scope Statement Notice of Intent to Ballot WE ARE HERE Ballot Supporting Materials Q 3 Ballot Due FHIR Connectathon Ballot Opens for Voting Ballot Reconciliation Starts Ballot Reconciliation Deadline

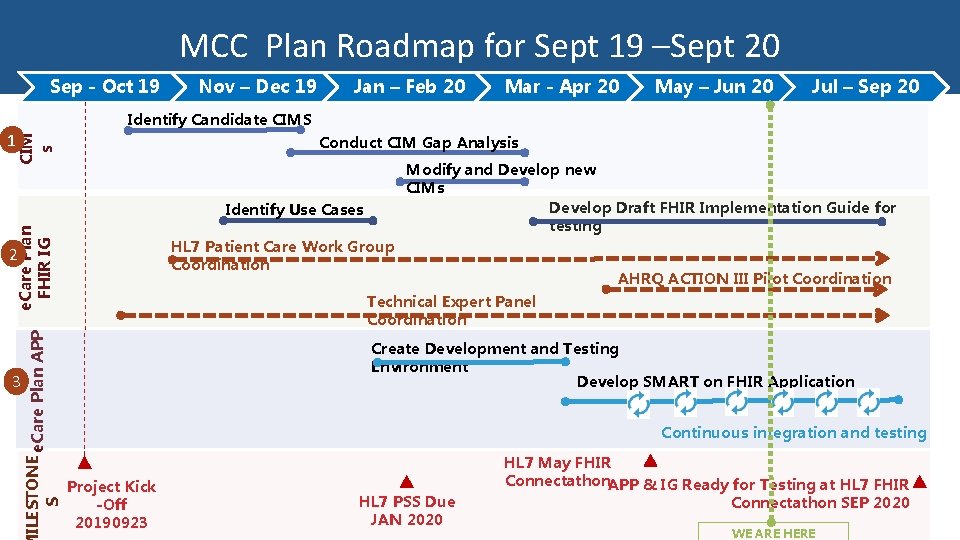
MCC Plan Roadmap for Sept 19 –Sept 20 Sep - Oct 19 Nov – Dec 19 Jan – Feb 20 May – Jun 20 Jul – Sep 20 Identify Candidate CIMS Conduct CIM Gap Analysis CIM s 1 Modify and Develop new CIMs Develop Draft FHIR Implementation Guide for testing e. Care Plan FHIR IG Identify Use Cases HL 7 Patient Care Work Group Coordination ILESTONE e. Care Plan APP S 2 3 Mar - Apr 20 AHRQ ACTION III Pilot Coordination Technical Expert Panel Coordination Create Development and Testing Environment Develop SMART on FHIR Application Continuous integration and testing Project Kick -Off 20190923 HL 7 PSS Due JAN 2020 HL 7 May FHIR Connectathon. APP & IG Ready for Testing at HL 7 FHIR Connectathon SEP 2020 WE ARE HERE

September 2020 and Beyond Care Planning, Plan Definition, Care Team, Care June 2020 Coordination and Clinical Guidelines Framework for MCC e. Care Plan Draft IG (non -balloted, ready for testing) September 2020 SMART on FHIR App v 1. 0 (ready for testing) September 2020 Connectathon 1 -6 September 2020 – May 2022 Real world testing implementation and testing January 2021 – September 2021 Expansion of conditions and values sets in IG from CKD to include MCC Round 1 January 2021 – September 2021 Expansion of conditions in IG from CKD to include MCC Round 2 September 2021 – September 2022 Submit for STU Ballot September 2022

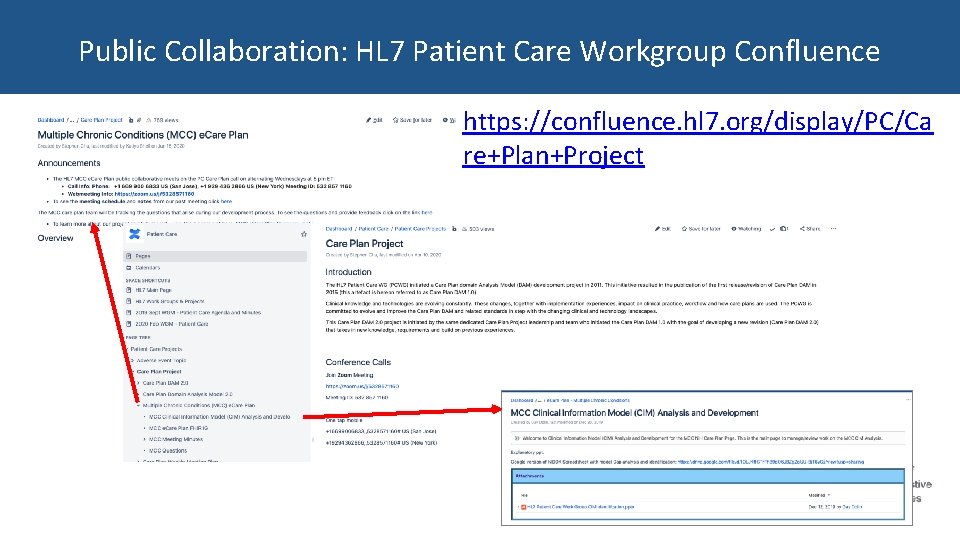
Public Collaboration: HL 7 Patient Care Workgroup Confluence https: //confluence. hl 7. org/display/PC/Ca re+Plan+Project

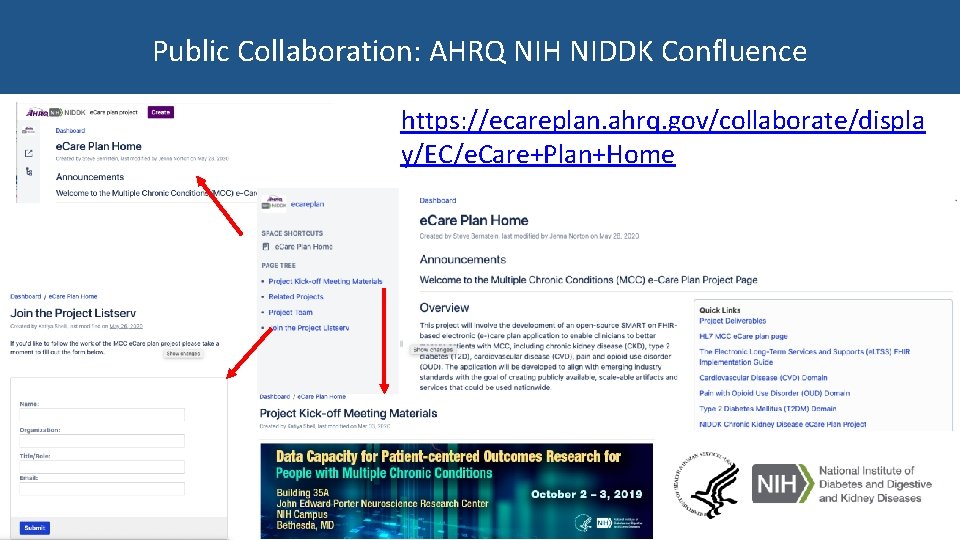
Public Collaboration: AHRQ NIH NIDDK Confluence https: //ecareplan. ahrq. gov/collaborate/displa y/EC/e. Care+Plan+Home

PROJECT STATUS

1 Clinical Information Modeling (CIM) • CIM Definition (for this project): – CIMs are a representation of a clinical concept with identified and specified data elements, attributes, and vocabularies • CIM Development: CKD data elements were mapped to HL 7 Fast Healthcare Interoperability Resources (FHIR) for direct re-use or constraint. • Some Examples: § § US Core Questionnaire/Questionaire. Response Clinical Information Modeling Initiative (CIMI) models Etc.

CIM Gap Analysis & Development • Phase 1 a: Benchmarking & Gap Analysis (completed Dec 2019) – Review and modify NIDDK Chronic Kidney Disease (CKD) spreadsheet where data elements will be assigned • Phase 1 b: Modify Candidate CIMS (Completed March 2020) – Modify CKD spreadsheet with: § Single value term bindings § New or existing value sets § Cardinalities of attribute and elements • Phase 1 c: Develop New CIMs (Completed March 2020) – Continue to modify CKD spreadsheet and include: § Proposed Model Name § FHIR Resources that will be used to create new model

2 e. Care Plan FHIR IG Components • Content: CKD Data Elements (CIMs) represented in FHIR Profiles (target End of June 2020) • Care Plan Workflow and Profile Relationship Diagrams (target Mid July 2020 • MCC e. Care Plan FHIR Profile Build (target Mid-end July 2020)

2 e. Care Plan FHIR IG Components • Introductory Material (target August 2020): – Uses Cases – Personas § Patient Story § Use Cases represented using Actor-Transaction Diagrams – Implementation and Conformance Guidance – Pictures and Diagrams

e. Care Plan Use Cases • • • Attribute Care Team Members Subscribe to updates to e. Care Plan Generate and share (push/publish) e. Care Plan Query and pull e. Care Plan Consent to share e. Care Plan information for research (e. g. S 4 S) Consent to share e. Care Plan sensitive information with specific team members

Relevant Initiatives for Use Case Development § § § § § HL 7 Care Plan Domain Analysis Model 2. 0 (DAM) HL 7 CDA R 2 Pharmacist Care Plan Document R 1 HL 7 Pharmacist Care Plan FHIR Implementation Guide HL 7 electronic Long-Term Services and Supports (e. LTSS) Implementation Guide SAMSHA Omnibus Care Plan FHIR Profiles HL 7 Nutrition Care Plan Supplemental Templates HL 7 Gravity Project ONC FAST Shared Care Planning Use Case IHE Dynamic Care Planning Profile

Candidate e. Care Plan Personas • • Patricia Noelle (Patient) Rose Noelle (Caregiver) John Carlson (Primary Care Physician) Julie Smith (Care Coordinator) Vince Jones (Nephrologist) Sam Johnson (Social Worker) Wilson Odunbaku (Cardiologist) Barbara Wojcicki (Pain Specialist)

Candidate Patient Persona About Patricia • Patricia is a retired school teacher. • Her husband passed away a few years ago, and she currently lives with her daughter, Rose. • Patricia feels nervous and overwhelmed managing her MCCs. This also impacts her depression. • Patricia relies on Rose to drive her to the doctor and thereby can only schedule appointments when Rose is not working. § Meet Patricia Noelle § 65 years old § Clinical Health Concern: CKD, Patricia's Typical Routine & Interactions Diabetes, CHF, Chronic Low Back Pain, Depression • Patricia spends her days: watching TV, walking around the house, § Social risks: food insecurity, sometimes having a meal with friends. transportation • She finds certain activities like reading more difficult now due to § 1 child (Rose who is her care giver) decreased vision. § Location TBD • Currently she follows a carbohydrate controlled, heart healthy diet.

Candidate Patient Persona Challenges & Goals • Patricia is finding it hard to schedule appointments with her physician and specialists because of frequent time conflicts. • Patricia is stressed because she does not know which of her many doctors to listen to, what she should be eating, which medications to take. • Over the past month, Patricia has become increasingly anxious and depressed regarding her progressive CKD and what course of action she needs to take should her kidneys fail. • She is also concerned about tapering off the opioids she is currently on to manage lower back pain. What Patricia’ wants from a Care Plan • • • A way for all her different providers to communicate with each other. A summary of her goals and plans reviewed by all her providers Ability to talk to a nurse about her MCC Education materials on living with MCC An easier way to schedule appointments Contact information for a counselor

Draft Implementation Guide Development – Sept 2020 • IG Framework Begun (Build is in Trifolia) – MCC Care Plan Resource Profile started – “Content” profiles 75% Built - Specific to CKD and related: § Conditions § Procedures § Lab Results – https: //trifolia-fhir. lantanagroup. com/igs/lantana_hapi_r 4/MCC-IG/index. html • Next: – Complete Content Profiles – Develop workflow and Resource relationship diagrams – Constrain content profiles into MCC Care Plan Profile • Look and feel will align where appropriate with Gravity IG – https: //trifolia-fhir. lantanagroup. com/igs/lantana_hapi_r 4/SDOH-CC/index. html

FHIR Specifications for IG Development – First § Reuse/Reference: • US Core: Patient, Practitioner. Role, Organization, Goal, Procedure, Care Team, Condition, Laboratory Result Observation, Profile. Diagnosticreportlab, Diagnostic report-note, Smoking Status, Medicationrequest, Medication • FHIR Resources: Care. Plan, Risk Assessment, Family. Member. History, Observation, Questionnaire. Response, Coverage, Consent, Communication • IHE Profiles: Dynamic Care Planning • CIMI: Vital Signs • BSe. R Bidirectional Service e. Referral

FHIR Specifications for IG Development – Second § Reuse or Reference: • CDS Hooks SMART on FHIR integration • Gravity Project: FHIR R 4 Profiles for SDOH Content • Da Vinci: CDex (Clinical Data Exchange) • Future: • FHIR Plan Definition and FHIR Clinical Guidelines

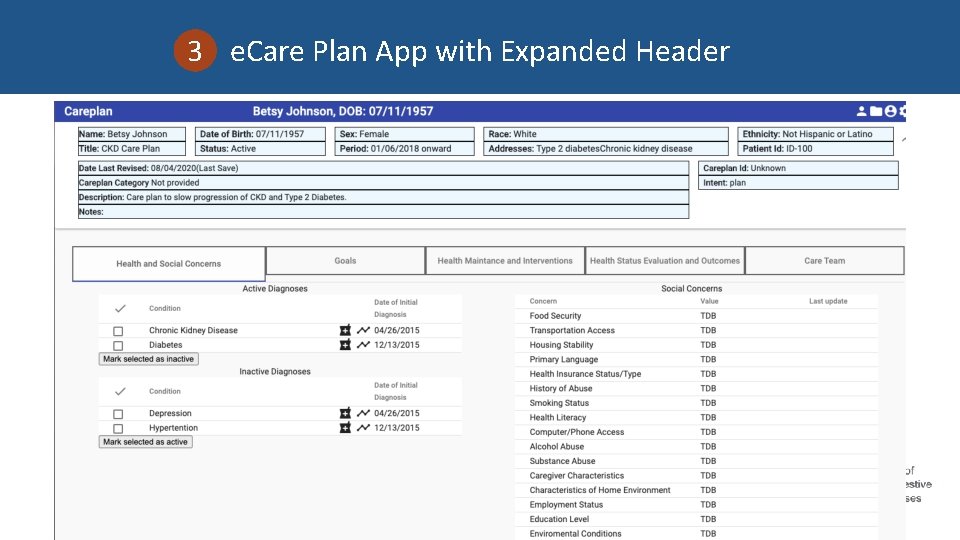
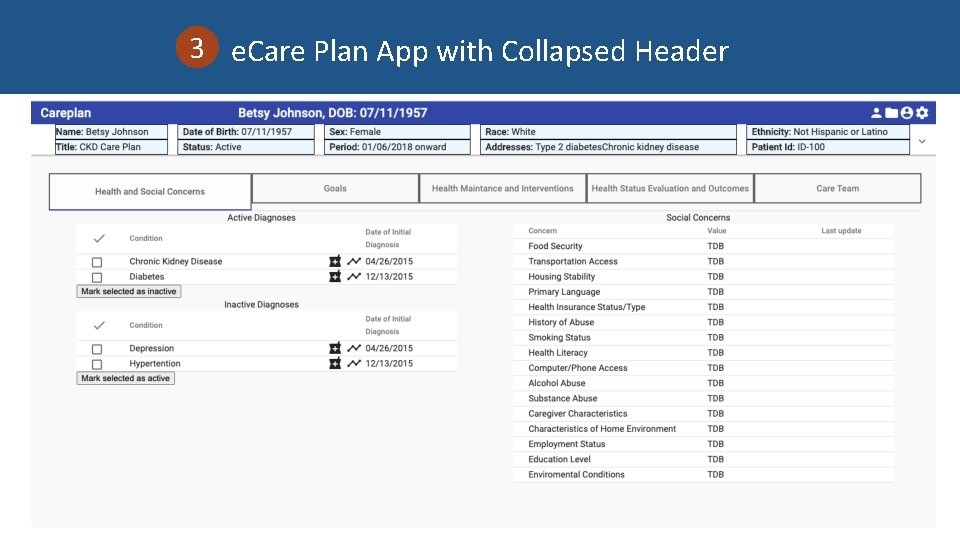
3 e. Care Plan SMART on FHIR App • Pilot version of SMART on FHIR e. Care Plan app focused on CKD care planning • App will support following capabilities: – Retrieve patient data and related resources from EHR and other health IT systems for aggregation, analysis, and sharing – Incorporate priority CKD data elements finalized in task 1 activities – Incorporate draft NIDDK e. Care Plan wireframe and ongoing testing

3 e. Care Plan SMART on FHIR App • Current Status: – Currently integrated with Logical Health Servers – Using existing FHIR Connectathon R 4 resources • Near Term work – – Additional tabs (Goals, Interventions, Outcome etc. ) Integration with VSAC values sets SMART on FHIR full integration Graphing in Health Status and Outcomes

3 e. Care Plan App with Expanded Header

3 e. Care Plan App with Collapsed Header

3 e. Care Plan App Health Status Evaluation & Outcomes Tab

Connectathon Testing • Draft IG will be used as foundation for: – Connectathons – Pilot Testing – Project Discussions and Design Changes – TEP input – SMART on FHIR App Build • First Round of Testing: September 2020 – Plan to test at subsequent testing events • First Ballot: September 2022

May HL 7 FHIR Connectathon Care Coordination Track § Members of the MCC e. Care Plan Project led the Care Coordination track during the May 13 th to 15 th 2020 Virtual HL 7 Connectathon § Care Coordination Track: Tested multiple IGs specific to patient/person level data across the continuum of care: SDOH screening, functional assessments, care planning, and e. Referrals § The 2020 -05 Care Coordination track page includes the report out, video recorded demonstration and lessons learned § Track details available here Target FHIR Specifications for Testing: • • • HL 7 FHIR Gravity Social Determinants of Health in the Clinical Care Setting (sdoh-cc) PACIO Functional Status Assessment IG and Cognitive Status Assessment IG HL 7 FHIR Electronic Long-Term Services and Supports (e. LTSS) IHE Dynamic Care Planning Da Vinci CDex, FAST HL 7 FHIR Bidirectional Service Request (BSe. R) IG Clinical Practice Guidelines (CPG) CDS Hooks, on-patient-view SMART on FHIR C-CDA on FHIR US Core

May HL 7 FHIR Connectathon Lessons Learned • Lack of implementer readiness to generate, query, and exchange e. Referrals • Limited testing of provider workflow to complete multiple patient assessments within EHR system • No EHR or HIE system readiness to test FHIR based exchange • Roadmap for “push transactions” not clear § Push for referral events vs. Polling for referrals • Dependency and interdependency on low maturity FHIR Resources and WIP IGs increases project risks

May HL 7 FHIR Connectathon Recommendations • The two priority items that need to be addressed to successfully test the MCC FHIR IG in the September 2020 HL 7 Connectathon: – Recruit EHR and HIE vendors to participate as system actors across the care coordination transactions: SDOH screening, patient assessments, e. Referrals, and care planning. – Consider providing a mechanism to enable HIEs and care coordination platforms that are not yet FHIR enabled to query and pull C-CDA based exchange documents. E. g. CDA Companion Guides

NEXT STEPS

Upcoming Meeting Schedule Week Call Date PCWG Meeting Topic 1 6/24 Discuss: Project Background, Scope, Approach and Status 2 7/8 Discuss: IHE Dynamic Care Planning (DCP) Profile and Care Plan DAM 2. 0 informing diagrams, workflow and IG development 3 7/22 Discuss: Relationship diagrams, use cases, and personas Introduce Sept HL 7 Care Coordination Track 4 8/05 Discuss: Integration Questionnaires and e. Referrals 5 8/19 Discuss: Overview of FHIR IG build Round 1 constraints and patient app design Update: Care Coordination Track Participants 6 9/2 Overview of FHIR IG build Round 2 constraints and Connectathon planning 7 9/9 HL 7 FHIR Connectathon!

Next Steps for the Project • Facilitate Bi-weekly calls on the patient care work group meeting June to September 2020: • Next Meeting is July 8, 2020 – Meeting schedule: https: //confluence. hl 7. org/display/PC/MCC+Meeting+Minutes • • • Identify Connectathon participants Initiate HL 7 Virtual Connectathon planning Complete Draft FHIR IG Complete pilot version of the SMART on FHIR APP Test at the September HL 7 FHIR Virtual Connectathon

Next Steps for Stakeholders • Join the Patient Care Work Group Calls • Visit the two MCC e. Care Plan confluence pages – AHRQ/NIDDK: https: //confluence. hl 7. org/display/PC/Care+Plan+Project – HL 7: https: //ecareplan. ahrq. gov/collaborate/display/EC/e. Care+Plan+Home • Email the Evelyn Gallego evelyn. gallego@emiadvisors. net or Katiya Shell katiya. shell@emiadvisors. net if you are an EHR or HIE vendor interested in participating in the September 9 -11 Connectathon

Questions? e. Care Plan Project Contacts § Federal Leadership § Jenna Norton (NIDDK): jenna. norton@nih. gov § Arlene Bierman (AHRQ): arlene. bierman@ahrq. hhs. gov § Project Manager § Tom Hicke: thicke@cognitivemedicine. com § Technical Architect § Jerry Goodnough: jgoodnough@saperi. io § CIM Technical Leads § Gay Dolin: gdolin@namasteinformatics. com § Joe Bormel: jbormel@cognitivemedicine. com § SDO Liaison & Coordination § Evelyn Gallego: evelyn. gallego@emiadvisors. net § Katiya Shell: katiya. shell@emiadvisors. net

Back-Up

Defining Person-Centered Care “Person-centered care” means that individuals’ values and preferences are elicited and, once expressed, guide all aspects of their health care, supporting their realistic health and life goals. Person-centered care is achieved through a dynamic relationship among individuals, others who are important to them, and all relevant providers. This collaboration informs decision-making to the extent that the individual desires. “Person-Centered Care: A Definition and Essential Elements” The American Geriatrics Society Expert Panel on Person-Centered Care, December 2015 https: //www. ncbi. nlm. nih. gov/pubmed/26626262

Care Plans in the US: A Long Road Ahead Surveys and interviews with staff from 17 technically savvy US institutions: • Care plans were infrequently used in practice • Care plans were often free-text or paper documents shared by fax, providing limited support for care coordination • Little consistency of and interoperability in care plans existed across settings, or across disciplines within settings. • Most acute hospital sites sent electronic clinical data (e. g. , problems, orders, allergies, medications) but none sent patient preference/goals data • Patient involvement in care plan development was limited and peripheral Dykes, at al. JAMIA 2014: 21(6): 1082 -90.

Role of Standardized e. Care Plans § Standards provide the fundamental definitions for and structures of the data that can be communicated electronically across a wide variety of healthcare use cases § Interoperable care planning involves standardization across three layers: – how care plan information is sent and received (transport) – the structure and format of the information (syntax) – the terms or meaning of the information within the care plan (semantics) STANDARDS EXIST TO SUPPORT ALL THREE LAYERS

Two Fundamental Standards Care Plan Document Template (constrained within C-CDA R 2. 1 Implementation Guide) http: //www. hl 7. org/implement/standards/product_brief. cf m? product_id=492 • More mature standard • Document exchange focused • Trust from document context & obligations • Independent of system integration • Import data from documents Care Plan Resource (constrained by FHIR Standard for Trial Use) https: //www. hl 7. org/fhir/careplan. html Evolving standard Granular data exchange focused System-based trust framework Tightly integrated IT and business systems • Export data from APIs • • Both standards share common syntax and set of resources Source: https: //www. slideshare. net/Furore_com/01 -b-from-ccda-to-fhir-grahame

NIH NIDDK CKD Patient Persona for Betsy Johnson NIDDK Electronic CKD Care Plan Initiative: https: //bit. ly/2 QFY 4 zb

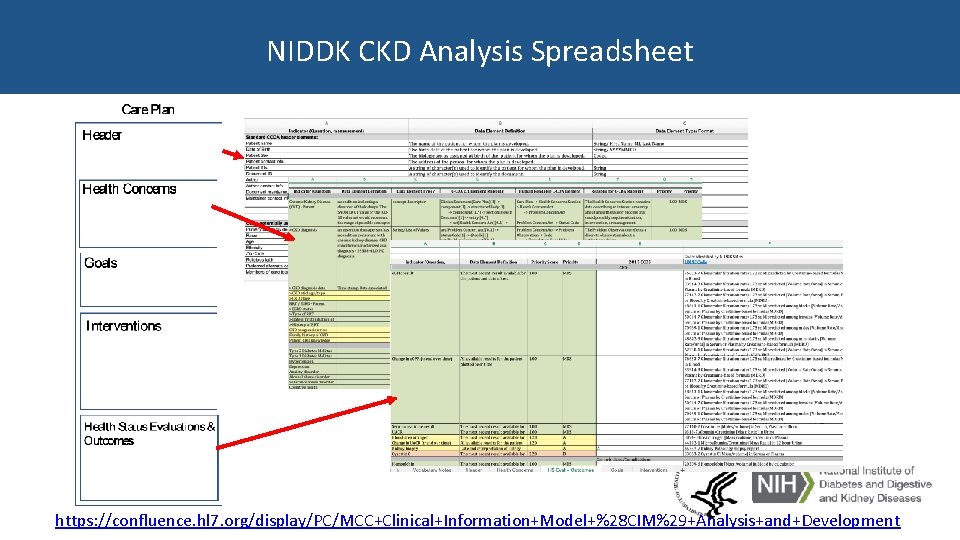
NIDDK CKD Analysis Spreadsheet https: //confluence. hl 7. org/display/PC/MCC+Clinical+Information+Model+%28 CIM%29+Analysis+and+Development

SMART on FHIR Standards and Specifications https: //docs. smarthealthit. org/

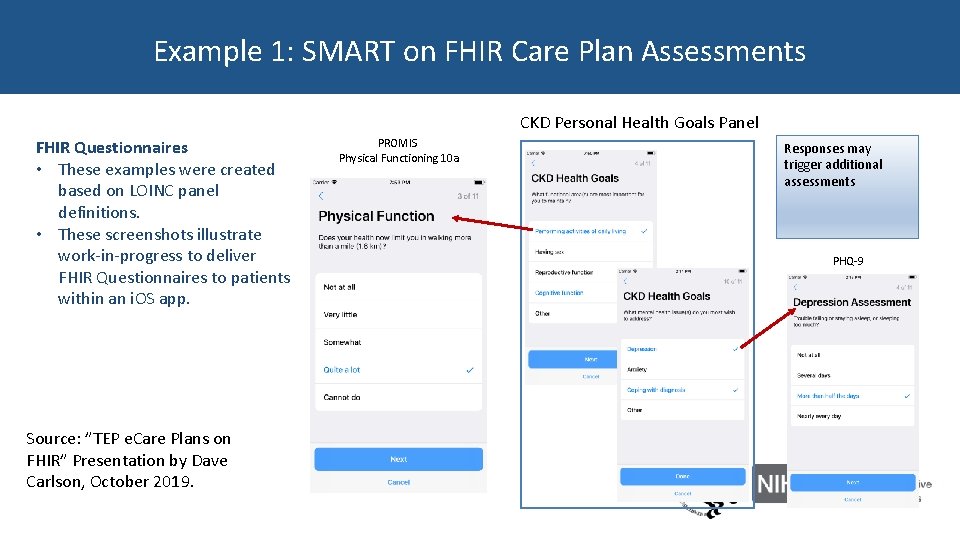
Example 1: SMART on FHIR Care Plan Assessments CKD Personal Health Goals Panel FHIR Questionnaires • These examples were created based on LOINC panel definitions. • These screenshots illustrate work-in-progress to deliver FHIR Questionnaires to patients within an i. OS app. Source: ”TEP e. Care Plans on FHIR” Presentation by Dave Carlson, October 2019. PROMIS Physical Functioning 10 a Proposed Solution Responses may trigger additional assessments PHQ-9

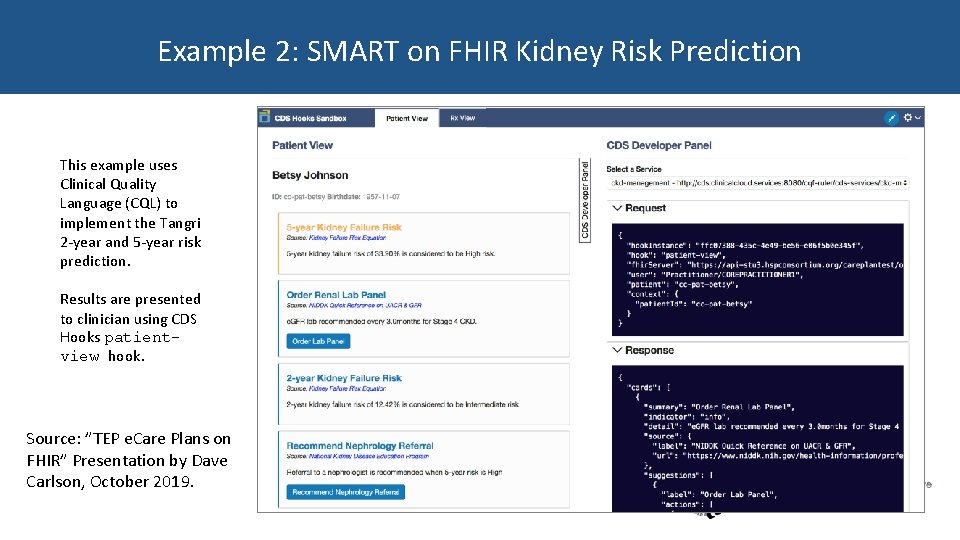
Example 2: SMART on FHIR Kidney Risk Prediction This example uses Clinical Quality Language (CQL) to implement the Tangri 2 -year and 5 -year risk prediction. Results are presented to clinician using CDS Hooks patientview hook. Source: ”TEP e. Care Plans on FHIR” Presentation by Dave Carlson, October 2019.

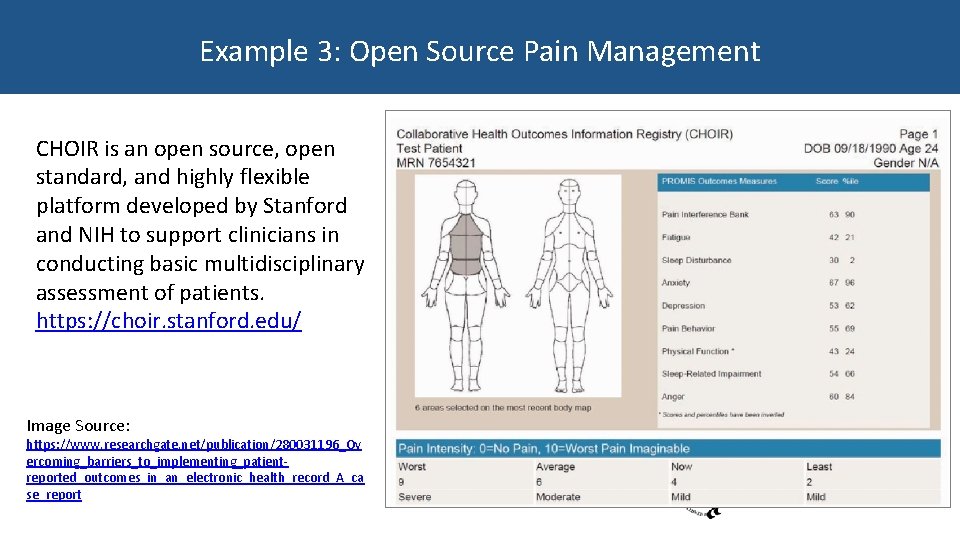
Example 3: Open Source Pain Management CHOIR is an open source, open standard, and highly flexible platform developed by Stanford and NIH to support clinicians in conducting basic multidisciplinary assessment of patients. https: //choir. stanford. edu/ Image Source: https: //www. researchgate. net/publication/280031196_Ov ercoming_barriers_to_implementing_patientreported_outcomes_in_an_electronic_health_record_A_ca se_report

e. Care Plan Use Case Components • Personas. Commonly used in user-centered design to describe the fictional character who would represent a user type that might use a site, brand, or product in a similar way. Describe in terms of a person’s behaviors, skills, preferences, and needs. • Patient Story. Describes Personas engaging with a service, technology, or setting over a period of time to accomplish a specific goal. • Use Cases. Technical narratives of the interactions between the Personas and the systems they use.

e. Care Plan Persona Descriptors • About Persona. Introduces the name of the persona, their occupation, their current health concerns, and their person-centered goals. • Typical Routine and Interactions. Describes key activities in the Persona’s day. • Clinical Information (for Patient Persona only). Snapshot of Patient Care Summary including Social History. • Challenges and Goals. For the Patient Persona, lists key questions the Persona has around their current health concerns. For the Provider Persona, lists key challenges the Provider has around addressing their care delivery needs of their patients with MCC. • What Persona Wants from a Care Plan. Summarizes key attributes and outcomes of the ideal care plan that the persona is seeking.

Candidate e. Care Plan Patient Story for TEP Review • Personas (see previous slide) • Settings: – – – Primary Care Practice Patient home Nephrologist Office Cardiologist Office Pain Specialist Office • Activities: – Screening/Assessment, Diagnosis, Care Coordination (care planning, referral, consultation), and Treatment/Interventions