Multidisciplinary Team Working in PD Nin Bajaj Consultant

Multidisciplinary Team Working in PD Nin Bajaj Consultant Neurologist, Nottingham Fiona Lindop, Specialist Physiotherapist, Derby

Setting up a PD service • Nuts and Bolts • You can’t do this alone • You need “mates” or at the very least people you can work with on a professional level • The days of the “solo” practitioner really should be over

The team- the minimum requirement • A neurologist • A Care of the Elderly Physician • A PD specialist nurse

The extended team • • • PD physiotherapy OT SALT Community PD nurses Neurorehab specialist

The fantasy football team • • • Pharmacist Dietician PD service management Psychiatrist Palliative Care Parkinson’s UK/Care PD patient representative

PD Steering Group • The Fantasy Football team • Meet 4 x a year • Allows managed expansion and cohesive lobbying • Allows access to “pots” from Cancer and Medicine • Allows unified drug, pharmacovigilance and audit policy

How do you create a profile for the service • Playing at Home • Playing Away • International fixtures

Playing at Home • The local community with PD has to have a voice in the local service • This might be best done by co-opting local patient representatives from the charities • Having a local rep man the information stand at clinics • Holding education groups and facilitating special groups locally e. g. young persons with PD

Playing Away- National Level • • • Endorsement of the service Hospital Doctor Award Guardian Public Sector Awards HS awards Research Profiles

Hospital Doctor Award

Research Profiles • • • De. NDRo. N CLRN The De. NDRo. N PD Director (region) Non-portfolio work Refereeing Working for and with the Charities
Research Profiles- National • De. NDRo. N working parties • National grants

Co-operative Working with Pharma • Educational Events • IIT research grants • Portfolio Adoption

Playing Away from Home. International • International Endorsement • The national Parkinson Foundation Programme • Research
NPF

NPF Centres of Excellence

Research- International • Present at conferences • Lecture • Faculty Boards

How to build a world class PD service: Business cases in Derby • Specialist Physiotherapist & OT Posts (appointed 2009, but already working as specialists for several years) • Dedicated SALT (appointed 2009) – LSVT training 2010 (one patient, 4 weeks / 4 x 40 mins at present) • Dietician – appointed 2010

Impact of Specialist Therapy Posts: in-reach and out-reach • Potential for reduced length of stay • Specialist support for in-patients • Outpatients reduced waiting list & improved follow up availability • Provision of emergency therapy appointments • Specialist MDT may be able to support patients while waiting longer for consultant/PDNS clinic appointments

Further aspects of the roles • Education for patient and carer – Including exercise, relaxation • Education and support for ward staff • Education for AHP’s on a national level – NCORE courses – annual PD or Parkinson’s Plus courses • Signposting to other support agencies e. g. Parkinson’s UK

Specialist Physiotherapy Role • Promote best practice- evidence-based models of therapy • Assessment and Management • Outcome measures – including LPAS, • Importance of exercise • Teach compensatory cues and strategies • Ultrasound for Apo-nodules
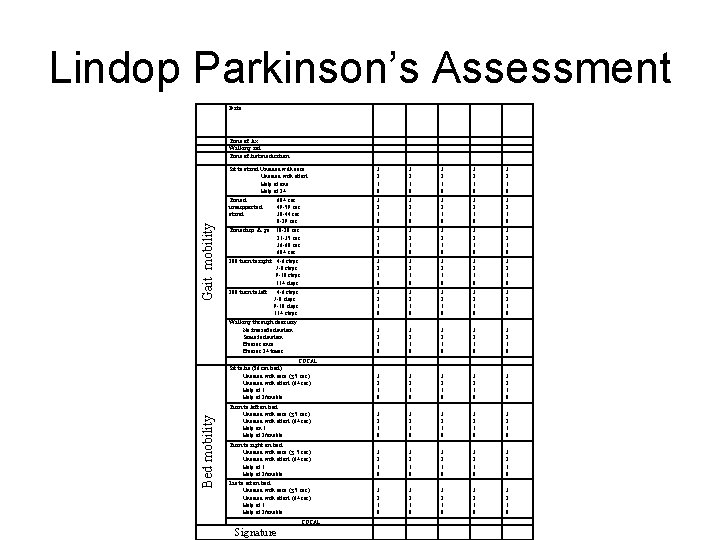
Lindop Parkinson’s Assessment Date Bed mobility Gait mobility Time of Ax Walking aid Time of last medication Sit to stand: Unaided with ease Unaided with effort Help of one Help of 2+ 3 2 1 0 3 2 1 0 Timed unsupported stand: 60+ sec 49 -59 sec 30 -44 sec 0 -29 sec 3 2 1 0 3 2 1 0 Timed up & go: 10 -20 sec 21 -35 sec 36 -60 sec 60+ sec 3 2 1 0 3 2 1 0 180 turn to right: 4 -6 steps 7 -8 steps 9 -10 steps 11+ steps 3 2 1 0 3 2 1 0 180 turn to left: 4 -6 steps 7 -8 steps 9 -10 steps 11+ steps 3 2 1 0 3 2 1 0 Walking through doorway: No freeze/festination Some festination Freezes once Freezes 2+ times 3 2 1 0 3 2 1 0 TOTAL Sit to lie (56 cm bed): Unaided with ease (≤ 5 sec) Unaided with effort (6+ sec) Help of 1 Help of 2/unable 3 2 1 0 3 2 1 0 Turn to left on bed: Unaided with ease (≤ 5 sec) Unaided with effort (6+ sec) Help on 1 Help of 2/unable 3 2 1 0 3 2 1 0 Turn to right on bed: Unaided with ease (≤ 5 sec) Unaided with effort (6+ sec) Help of 1 Help of 2/unable 3 2 1 0 3 2 1 0 Lie to sit on bed: Unaided with ease (≤ 5 sec) Unaided with effort (6+ sec) Help of 1 Help of 2/unable 3 2 1 0 3 2 1 0 TOTAL Signature

Specialist Occupational Therapy Role • Functional Assessment – all aspects of ADL including self-care, domestic, leisure, work • Assessment of cognition – ACER, MOCA • Assessment of Mood – HAD Scale, Becks. • Information regarding mood disorders - anxiety or depression • CBT/Anxiety management group • Relaxation/ fatigue management • Sleep hygiene

Future Dreams • • • Second PDNS More SALT hours Education framework Palliative Care Training for Care home staff Outreach to people with Parkinson's in care homes

Basal Ganglia Dysfunction • Impaired performance of well-learned motor skills and movement sequences – Preparation, Initiation, Sequencing, Timing • Difficulty in performing 2 or more welllearned tasks simultaneously • Difficulty in shifting motor and cognitive sets • Increased time required for mental processing

Enhancing function in PD – whole team approach Principles • Engage conscious attention • Avoid dual tasking • Use of cues • Use of strategies Cues Internal • Attention/concentration • Mental rehearsal • Visualisation • Cognitive • Weight transference External • Facilitation of attention • Visual • Auditory

Whole team approach: Freezing of Gait • “Inability to initiate walking sequences, a sudden cessation of stepping, part-way through a locomotor task, or difficulty igniting subsequent steps in the sequence once the motor block has occurred” (Morris et al 2008; Bloem at al 2004) • Reduces activity

Intervention for Freezing • Freezing: auditory cues to slow step frequency; visual cues to maintain momentum of step • Gait initiation: visual cue, rhythmic weight transference strategy • Step length: visual cue, attention cue, strategy • Relaxation techniques • Training for or avoidance of dual tasking
Turning Safe turn requires: Intervention for turning: • • • Avoid dramatic change of direction • Avoid dual tasking • Cues • Physiotherapy to improve balance and rigidity Independent mobility Ground clearance Good stability Continuity of movement • Good posture

Intervention for falls • • • Balance re-education Teach to recognise festination in time Cues for freezing Environment – inside and outside Strategies for dyskinesia (compression & resistance) and dystonia (stretches) • Teach how to get up from the floor backward chaining

To Summarise. . . Team Approach!
- Slides: 31