Mucolytics Module E Mucolysis Mucolysis is the breakdown

Mucolytics Module E

Mucolysis • Mucolysis is the breakdown of mucus. • Mucolysis is needed in diseases in which there is increased mucus production: • • Cystic Fibrosis COPD Bronchiectasis Respiratory Infections • Turberculosis

Mucolysis • These diseases result in a marked slowing of mucus transport • Changes in properties of the mucus • Decreased ciliary activity • Both

Mucolytics • acetylcysteine • sodium bicarbonate (Na. HCO 3) • dornase alfa • Pulmozyme

Airway Anatomy

Mucus Layer • Gel (1 to 2 mm): Gelatinous and sticky (flypaper) • Sol (4 to 8 mm): Watery, Cilia in this layer • Total layer thickness: 5 to 10 mm thick • Surface Epithelial Cells • • Pseudostratified ciliated columnar Surface goblet cells (6, 800/mm 2) Serous cells – Sol layer Clara cells – Unknown function (enzymes? ) • Submucosal Gland • Bronchial Gland

Mucus Layer • Bronchial Gland • • • Found in submucosa Found down to terminal bronchioles Parasympathetic control (Vagus nerve) Provide the majority of mucus secretion Total volume 40 times greater than goblet cells

Mucus vs. Sputum • Mucus is the total secretion from mucous membranes including the surface goblet cell and the bronchial glands. • Sputum is the expectorated secretions that contains mucus, as well as oropharyngeal and nasopharyngeal secretions (saliva).

Mucociliary Escalator • Mucosal Blanket • Sol layer • Gel layer • Cilia • • • 200 per cell 6 mm in length Beat 1000/min Move mucus 2 cm/min Paralyzed by cigarette smoke

Viscosity and Elasticity • Rheology • Viscosity: Property of a liquid that measures the resistance to movement when a force is applied. • Increased viscosity, increased resistance to flow • Olive oil vs. Water • Elasticity: Property of solid whereby a solid changes shape (deforms) when a force is applied. • Ideally, a solid is totally elastic, and returns to its original shape when force is released. • The mucus layer is ideally very elastic and has a very low viscosity.

Function of Mucociliary Escalator • Protective function • Remove trapped or inhaled particles and dead or aging cells. • Antimicrobial (enzymes in sol/gel) • Humidification • Insulation (prevents heat and moisture loss) • NOTE: No cilia or mucus in lower airways (respiratory bronchioles on down) • Mucus also protects the epithelium from toxic materials.

Structure and Composition of Mucus • Composition • 95% water • Need for water intake to replenish • Mucus doesn’t easily absorb water once created • 3% protein and carbohydrates • 1% lipids • Less than 0. 3% DNA

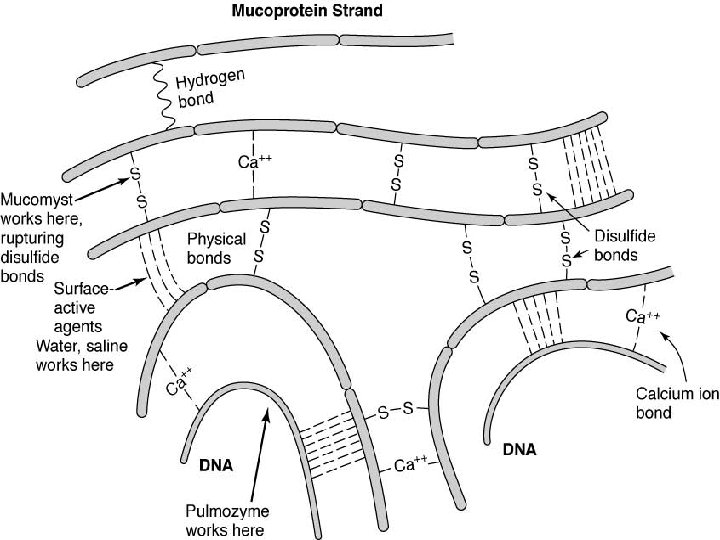
Structure and Composition of Mucus • Glycoprotein • Large (macro)molecules • Strands of polypeptides (protein) that make up the backbone of the molecule • String of amino acids • Carbohydrate side chains • Chemical bonds “hold” mucus together • Intramolecular: Dipeptide links • Connect amino acids • Intermolecular: Disulfide and Hydrogen bonds • Connect adjacent macromolecules

Mucus Production • Normal person produces 100 m. L of mucus per 24 hour period • Most is reabsorbed back in the bronchial mucosa • 10 m. L reaches the glottis • Most of this is swallowed • Mucus production increases with lung disease

Increased Mucus Production • • • Smoking Environmental irritants Allergy Infections Genetic predisposition Foreign bodies

Increased Mucus Production § § § Viscosity of mucus ¯ Ciliary effectiveness Mucus plugs Airway Resistance Infections Obstructed bronchioles leads to atelectasis

Diseases that Increase Mucus Production • • • Chronic Bronchitis Asthma Cystic Fibrosis Acute Bronchitis Pneumonia • Also some drugs (anticholinergics, antimuscarinics)

Factors that Impair Ciliary Activity • • Endotracheal tubes Temperature extremes High Fi. O 2 levels Dust, Fumes, Smoke Dehydration Thick Mucus Infections

Facilitation of Mucus Clearance • Provide adequate hydration • Increase fluid intake orally or IV • Remove causative factors • Smoking, pollution, allergens • Optimize tracheobronchial clearance • Use Mucolytics • Reduce Inflammation

Dairy Intake • No evidence to support the common belief that drinking milk increases the production of mucus or phlegm and congestion in the respiratory tract • There is a loose cough associated with milk intake

Secretion Management • Increase the depth of the sol layer • Water • Saline • Expectorants • Alter the consistency of the gel layer • Mucolytics • Improve ciliary activity • Sympathomimetic bronchodilators • Corticosteroids

Bland Aerosols • “Dilutes” mucus molecule • Also known as wetting agents • Function may be more of an irritant than a wetter • Types • Sterile & Distilled Water • Humectant • Dense aerosols and asthmatics • Normal (isotonic) Saline • Hypertonic Saline • Increase mucus production • Hypotonic Saline

Expectorants • Iodides • Unclear function • SSKI (Saturated Solution of Potassium Iodide) • Guifenesin • At high doses, stimulates bronchial gland secretion • Robitussin

Cough Suppressants • Vagal stimulation causes a cough. • Irritation of pharynx, larynx, and bronchi lead to a reflex cough impulse. • If the cough is dry and non-productive, it may be desirable to suppress its activity. • Cough suppressants depress the cough center in medulla (? ). • Narcotic preparations (codeine) • Non-Narcotic preparations (dextromethorphan) • Caution in patients with thick secretions.

Function of Mucolytics • Weakening of intermolecular forces binding adjacent glycoprotein chains • Disruption of Disulfide Bonds • Alteration of p. H to weaken sugar side chains of glycoproteins • Destruction of protein (Proteolysis) contained in the glycoprotein core of proteolytic enzymes • Breaking down of DNA in mucus
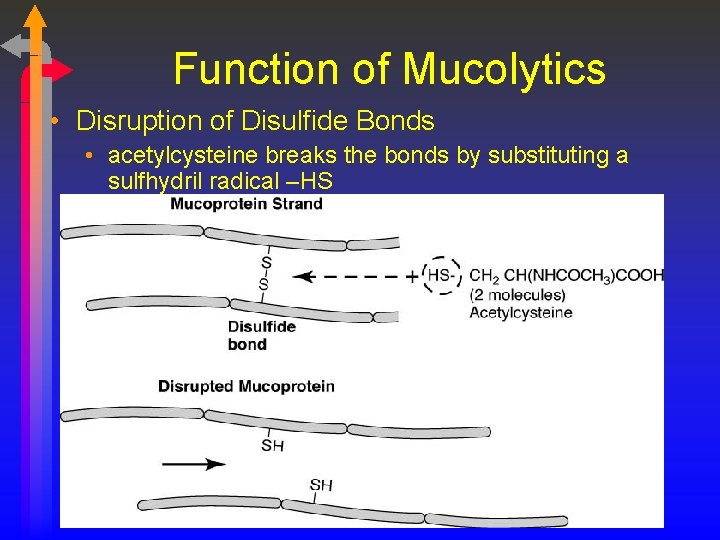
Function of Mucolytics • Disruption of Disulfide Bonds • acetylcysteine breaks the bonds by substituting a sulfhydril radical –HS

Function of Mucolytics • Alteration of p. H • 2% Na. HCO 3 solutions are used to increase the p. H of mucus by weakening carbohydrate side chains • Can be injected directly into the trachea or aerosolized (2 -5 m. L)

Function of Mucolytics • Proteolysis • Dornase alfa (Pulmozyme) • Attacks the protein component of the mucus

Hazard of Mucolytics • The problem with all three mucolytics is that they destroy the elasticity of mucus while reducing the viscosity. • Elasticity is crucial for mucociliary transport. • The patient must be able to cough adequately to remove the mucus.

acetylcysteine • Indications • Mucolytic by aerosol or direct instillation into the ET tube. • Given orally to reduce liver injury with acetaminophen (Tylenol) overdose. • Mix with cola or given by NG tube.

Dosage of acetylcysteine • Concentration • 10% or 20% • Dosage • 3 -5 m. L of a 20% solution TID or QID • Maximum dose 10 m. L • 6 -10 m. L of a 10% solution TID or QID • Maximum dose 20 m. L • 1 -2 m. L of a 10% or 20% for direct instillation

Hazards of acetylcysteine • Bronchospasm • Asthma – may be a problem during an acute asthma attack. • Anecdotal; lack of evidence • If used with asthma, use 10% and mix with a bronchodilator (preferably a short-acting agent). • Increase mucus production • Be prepared to suction a patient who cannot cough or who is intubated.

Hazards of acetylcysteine • Do not mix with antibiotics in the same nebulizer (incompatible). • Nausea & Vomiting • Disagreeable odor (smells like rotten eggs) due to the hydrogen sulfide. • Open vials should be used within 96 hours to prevent contamination.

sodium bicarbonate • Weak base. • Increasing the p. H of mucus weakens the polysaccharide chains. • Available as 1. 4%, 5%, and 7. 5% solutions. • Dosage: 2 -5 m. L of a 2. 5% solution Q 4 -Q 8. • Mix 5% solution with equal volume of sterile water. • Can be irritating (especially the 5 & 7. 5% solutions).

dornase alfa • Pulmozyme • Clone of the natural human pancreatic DNase enzyme which digests extracellular DNA. • Dornase alfa is a solution of recombinant human deoxyribonuclease (rh. DNase) • Approved by FDA in 1994

dornase alfa – Pulmozyme • Indications • Reduce viscosity of secretions during an infection by breaking down extracellular DNA. • Used in cystic fibrosis, chronic bronchitis or bronchiectasis. • Maintenance therapy in CF • Has no effect on non-infected sputum.

Infection • Increased WBCs – neutrophils • WBCs contain DNA • WBCs release DNA when they die which increases the viscosity of secretions • Decreases the effectiveness of antibiotics • Pancreas produces an enzyme called deoxyribonuclease (DNase) which breaks down the DNA •
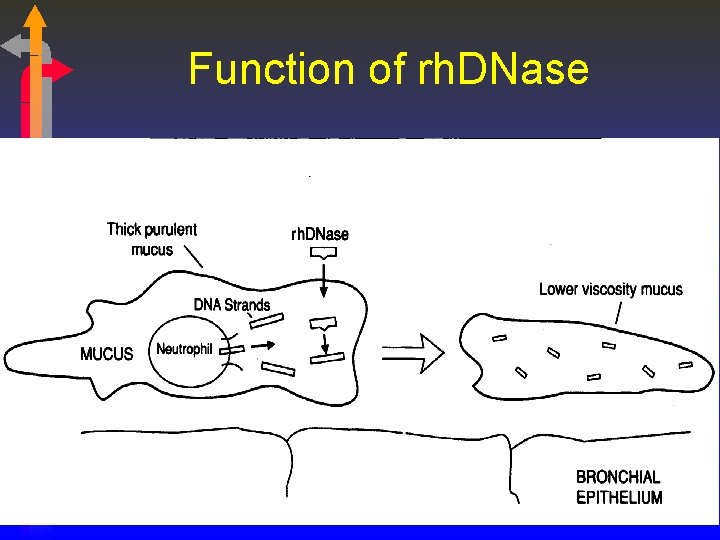
Function of rh. DNase

Concentration and Dosage • • Supplied in single dose vials (unit dose). Concentration is 1 mg/m. L (0. 1% solution). Each vial contains 2. 5 mg /2. 5 m. L. Administer one unit dose vial (2. 5 m. L) daily. • Some patients may benefit from BID administration. • Do not mix or dilute with other drugs. • Nebulizer specific (per manufacturer).

Common Side Effect of Pulmozyme • • • Voice Alteration Pharyngitis/Laryngitis Rash Chest pain Conjunctivitis • Contraindicated in patients hypersensitive to Chinese Hamster Ovary cell products.

amiloride • Midamor • Diuretic that can be given by aerosol for patients with cystic fibrosis. • It is a sodium channel blocker. • In Cystic Fibrosis, Na+ is absorbed into the epithelium along with H 2 O, leaving the mucus thick and dehydrated. • By blocking sodium absorption, dehydration of the mucus is prevented. • Drug is dissolved in 0. 3% Na. Cl solution and nebulized. • Bronchial Asthma (? )
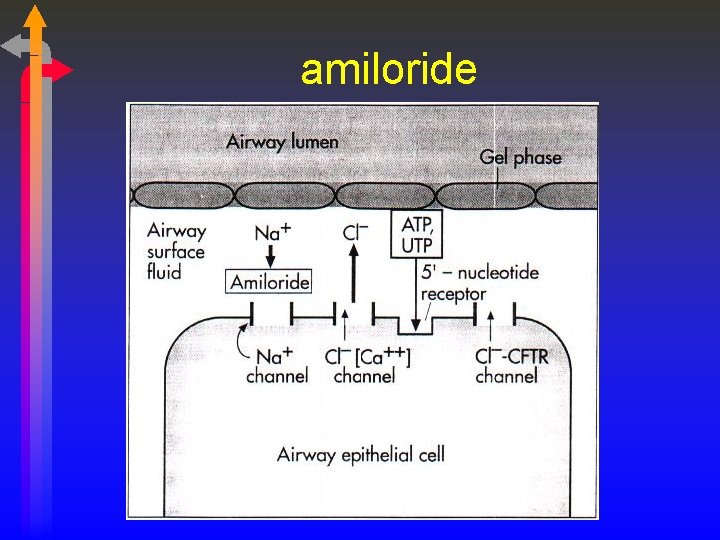
amiloride

denusfosol tetrasodium • Experimental drug in CF research • Phase II as of 8/07 • Enhances mucosal hydration and mucus clearance by activating Cl- secretion and inhibiting epithelial Na+ transport. • 28 days of treatment
- Slides: 44