MRSA Prescreening and Eradication New England Baptist Hospital

MRSA Prescreening and Eradication: New England Baptist Hospital Experience David H. Kim, MD Director of Medical Education New England Baptist Hospital Boston, MA

New England Baptist Hospital n n 150 -bed adult medical/surgical hospital located in Mission Hill area of Boston Orthopaedic subspecialty hospital & “Center of Excellence” – Acute inpatient discharges: n n 75% Orthopedic 8% General Surgery 17% Medical Orthopaedic Surgery ~ 10, 000/cases a year
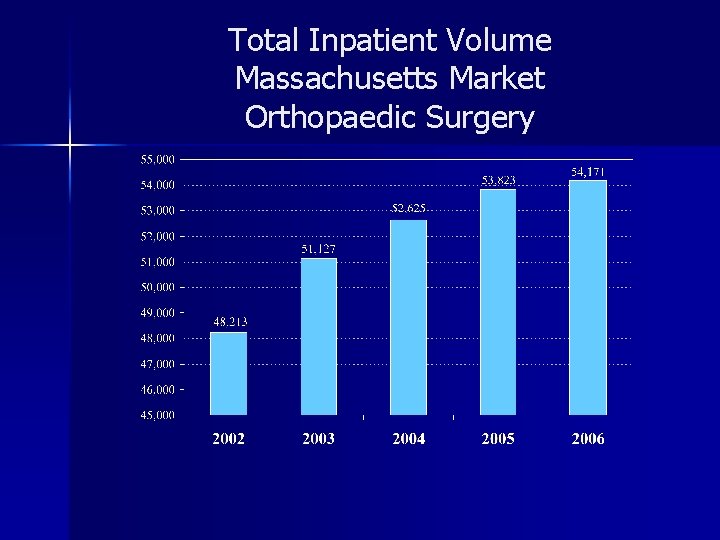
Total Inpatient Volume Massachusetts Market Orthopaedic Surgery
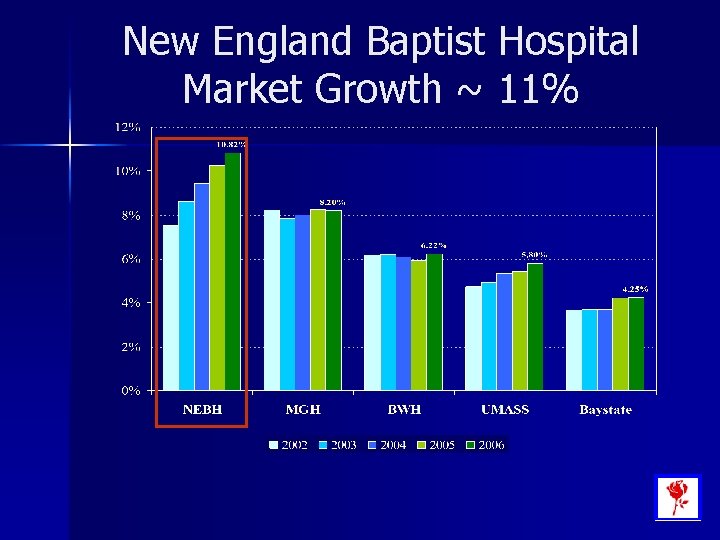
New England Baptist Hospital Market Growth ~ 11%

Methicillin-resistant Staphylococcus Aureus

S. Aureus n n Most important pathogen in SSI Most SSI caused by strains carried by patient into hospital Anterior nares main niche Nasal carriage of S. aureus is risk factor for SSI [Kluytmans et al, Clin Microbiol Rev 1997]

MRSA vs. MSSA Infection associated with higher mortality [Melzer et al, Clin Infect Dis 2003] n Survive in dry conditions & on inanimate surfaces up to 20 days [Clarke n et al, Ir Med J 2001] n Prevalence increasing

History of MRSA n Resistance to PCN within 1 yr – By 1950’s, 3/4 of S. aureus strains PCN-resistant – Today, 90 -95% clinical strains PCN-resistant n 1959—methicillin (1 st antistaph PCN) introduced – 1 st MRSA strain within 2 yrs – 60% of clinical S. aureus strains isolated from ICU’s are MRSA

Linezolid n Introduced in 2000 for MRSA –Resistant strain reported within 1 year [Tsiodras et al, Lancet 2001]

Daptomycin n Introduced in 2003 for MRSA • Resistant strain reported within 2 years [Mangili et al, Clin Infect Dis 2005]

Vancomycin Resistance n Recognized after almost 40 yrs – 1 st glycopeptide-intermediate S. aureus (GISA) isolated in Japan in 1996 [Hiramatsu et al, J Antimicrob Chemother 1997] n High level resistance appeared in Detroit in 2002 – van. A gene complex acquired from VRE [Centers for Disease Control and Prevention, MMWR Morb Mortal Wkly Rep 2002] n 2 nd strain in Philadelphia n 3 rd strain in New York

MIC Creep n n Increases in vancomycin MIC in both MRSA & MSSA over time [Rhee et al, Clin Infect Dis 2005] Largest study of >6000 S. aureus isolates over 5 yrs in California university hospital – Drift towards reduced susceptibility – ing percentage of isolates with MIC ≥ 1. 0 μg/m. L n n 19. 9% in 2000 70. 4% in 2004 [Wang et al, J Clin Microbiol 2006]

MIC Creep n ’d vancomycin failure rate in MRSA infections in setting of ’d MICs – [Sakoulas et al, J Clin Microbiol 2005]

Surgical Site Infection (SSI) n Increased costs – Median hospital stay increased 2 wks – Rehospitalization rates doubled – Overall costs tripled [Whitehouse et al, Infect Control Hosp Epidemiol 2002]

SSI Costs n Capitation – DRGs do not cover cost of treating nosocomial infection (considered “preventable”)

Risk of SSI Increased in Nasal Carriers n Nasal carriage only independent risk factor for S. aureus SSI in orthopaedic implant surgery – Kalmeijer et al, Infect Control Hosp Epidemiol 2000 n SSI rate 2 -9 x higher in carriers – Kluytmans et al, Clin Microbiol Rev 1997 – Perl et al, Ann Pharmacother 1998 – Wenzel et al, J Hosp Infect 1995 n In S. aureus SSI, S. aureus isolates from wound match nares 85% of time – Perl et al, N Engl J Med 2002

Risk Factors for S. Aureus SSI n Observational study of 357 cardiac surgery patients 27% nasal carriers SSI rate 6. 4% n Independent risk factors n n – S. aureus in 64% – 8/16 infections in nasal carriers – Diabetes (RR 5. 9) – Reoperation (RR 3. 1) – S. aureus nasal carriage (RR 3. 1) [Munoz et al, J Hosp Infect 2008]
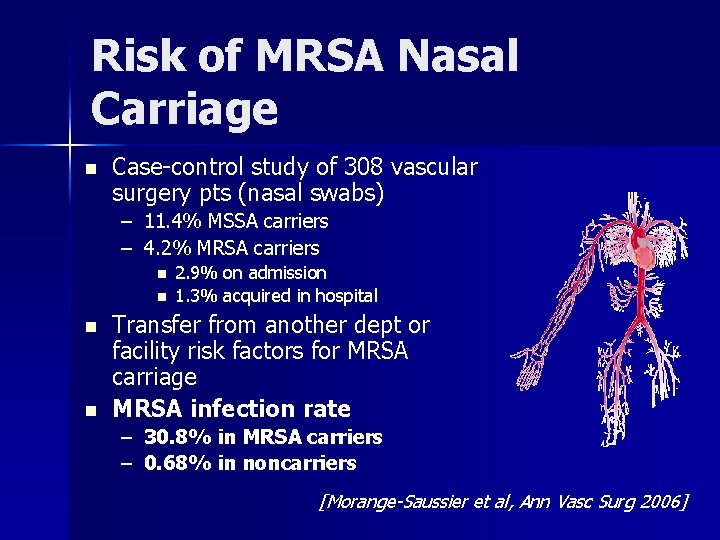
Risk of MRSA Nasal Carriage n Case-control study of 308 vascular surgery pts (nasal swabs) – 11. 4% MSSA carriers – 4. 2% MRSA carriers n n 2. 9% on admission 1. 3% acquired in hospital Transfer from another dept or facility risk factors for MRSA carriage MRSA infection rate – 30. 8% in MRSA carriers – 0. 68% in noncarriers [Morange-Saussier et al, Ann Vasc Surg 2006]

Environmental Reservoirs n n MRSA infected/colonized pts contaminate rooms, contribute to endemic MRSA Prospective study of 25 MRSA pts Sampling of isolation rooms – 53. 6% of surface samples positive – 28% of air samples – 40. 6% of settle plates Isolates identical or closely related in 70% of patients [Sexton et al, J Hosp Infect 2006]
![Environmental Reservoirs [Sexton et al, J Hosp Infect 2006] Environmental Reservoirs [Sexton et al, J Hosp Infect 2006]](http://slidetodoc.com/presentation_image/236c6af7efc27b403a390f2117a3bc0f/image-20.jpg)
Environmental Reservoirs [Sexton et al, J Hosp Infect 2006]
![Potential Airborne Transmission [Sexton et al, J Hosp Infect 2006] Potential Airborne Transmission [Sexton et al, J Hosp Infect 2006]](http://slidetodoc.com/presentation_image/236c6af7efc27b403a390f2117a3bc0f/image-21.jpg)
Potential Airborne Transmission [Sexton et al, J Hosp Infect 2006]

Airborne Transmission n MRSA counts remain elevated for up to 15 minutes after bed making Consider air ventilation & filtration Keep doors closed [Shiomori et al, J Hosp Infect 2002]

Inadequate Patient Space n n n 18 -month prospective study Addition of fifth bed to four-bed bay ’d relative risk of MRSA colonization 315% [Kibbler et al, J Hosp Infect 1998]

Long-term Care Facilities n 44% of environmental surfaces tested positive for MRSA [Asoh et al, Intern Med 2005]

Decolonization of Carriers Intranasal mupirocin (Bactroban) n Eradicates nasal colonization in most patients n Reduces S. aureus infections n – Herwaldt, J Hosp Infect 1998; Kluytmans et al, Infect Control Hosp Epidemiol 1996; Tacconelli et al, Clin Infect Dis 2003 (dialysis) – Cimochowski et al, Ann Thorac Surg 2001; Kluytmans et al, Infect Control Hosp Epidemiol 1996 (Cardiovasc) – Gernaat-van der Sluis et al, Acta Orthop Scand 1998 (ortho) – Perl et al, N Engl J Med 2002 (mixed)

Mupirocin and the Risk of S. Aureus (MARS) Study n n n University of Iowa Prospective randomized double-blind placebo-controlled 4020 enrolled, 3864 analyzed – Elective cardiothoracic, general, oncologic, gyn, neuro surgery n Rate of S. aureus SSI (primary endpoint) – 2. 3% in mupirocin pts – 2. 4% in placebo pts n No reduction in rate of S. aureus SSI – Among nasal carriers, risk of nosocomial S. aureus infection decreased by half (7. 7% to 4. 0%) [Perl et al, N Engl J Med 2002]

MARS Study n n n Mupirocin nasal swab for up to 5 days Chlorhexidine shower for cardiothoracic pts night before & morning of surgery Power analysis – 4046 pts to detect 50% in S. aureus SSI (estimated reduction of 2. 8% (57 pts) to 1. 4% (28 pts) with 85% power n 4030 enrolled, 3551 completed study – 82. 6% received at least 3 mupirocin doses [Perl et al, N Engl J Med 2002]
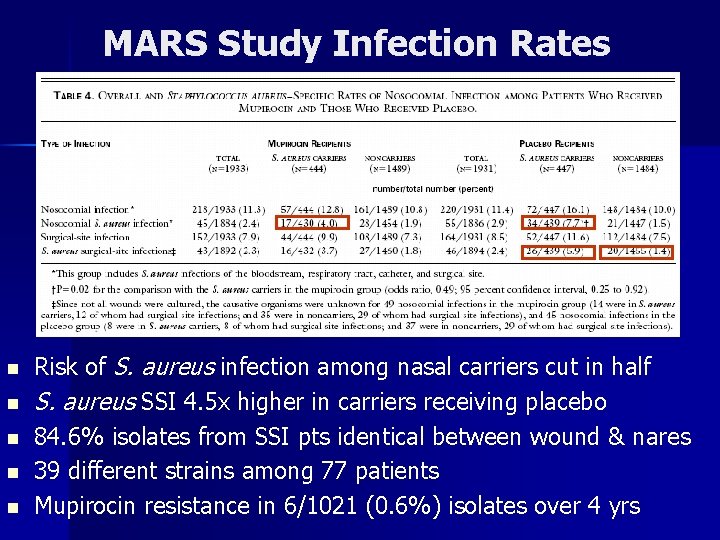
MARS Study Infection Rates n n n Risk of S. aureus infection among nasal carriers cut in half S. aureus SSI 4. 5 x higher in carriers receiving placebo 84. 6% isolates from SSI pts identical between wound & nares 39 different strains among 77 patients Mupirocin resistance in 6/1021 (0. 6%) isolates over 4 yrs
![Effect of Universal Screening: University of Geneva Hospital [Harbarth et al, JAMA 2008] n Effect of Universal Screening: University of Geneva Hospital [Harbarth et al, JAMA 2008] n](http://slidetodoc.com/presentation_image/236c6af7efc27b403a390f2117a3bc0f/image-29.jpg)
Effect of Universal Screening: University of Geneva Hospital [Harbarth et al, JAMA 2008] n n n Prospective interventional cohort with crossover 21, 754 pts (multiple surgical subspecialty wards) Rapid screening + standard infection control measures vs. standard measures alone MRSA Screening before or on admission by PCR Standard infection control for MRSA carriers – – n Contact isolation Gown, mask, gloves Adjusted perioperative abx Mupirocin & chlorhexidine x 5 days Universal rapid MRSA admission screening did not reduce nosocomial MRSA infection
![Incidence of MRSA Infections [Harbarth et al, JAMA 2008] Incidence of MRSA Infections [Harbarth et al, JAMA 2008]](http://slidetodoc.com/presentation_image/236c6af7efc27b403a390f2117a3bc0f/image-30.jpg)
Incidence of MRSA Infections [Harbarth et al, JAMA 2008]

Harbarth et al: Results n 94% (10, 193/10, 844) screened – 21, 754 pts--70% power to detect reduction in MRSA infection rate from 0. 9% to 0. 6% n n 5. 1% (515 pts) MRSA-positive No difference in MRSA SSI rate – 0. 99% (76 pts) without screening – 1. 14% (93 pts) with screening n 57% (53/93 pts) with nosocomial MRSA infection during screening period were MRSA -free on admission – 31% of MRSA carriers identified after surgery – 43% of MRSA carriers identified before surgery rec’d appropriate abx prophylaxis

Harbarth et al n None of MRSA carriers detected during outpatient preop visits developed MRSA infection – all received decolonization treatment & appropriate antibiotic prophylaxis n 57% of infections hospital-acquired

Preoperative Decolonization n n University of Pittsburgh Prospective observational study Total joint arthroplasty 1966 patients – 636 screened (nasal) n n n 26% positive for S. aureus (164/636) 23% MSSA (147/636) 3% MRSA (17/636) – 1330 control (not screened) [Rao et al, Clin Orthop Relat Res 2008]

Pittsburgh Protocol n Decolonization – Pts educated 1 wk preop – Mupirocin nasal ointment BID x 5 days – Chlorhexidine bath QD x 5 days
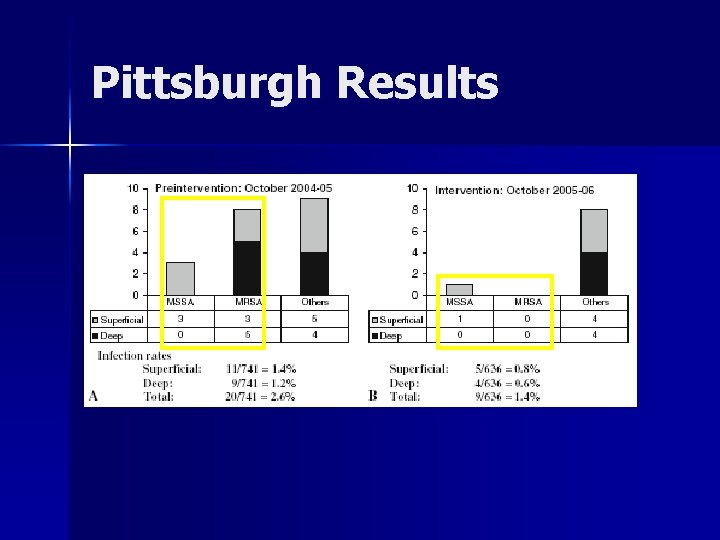
Pittsburgh Results
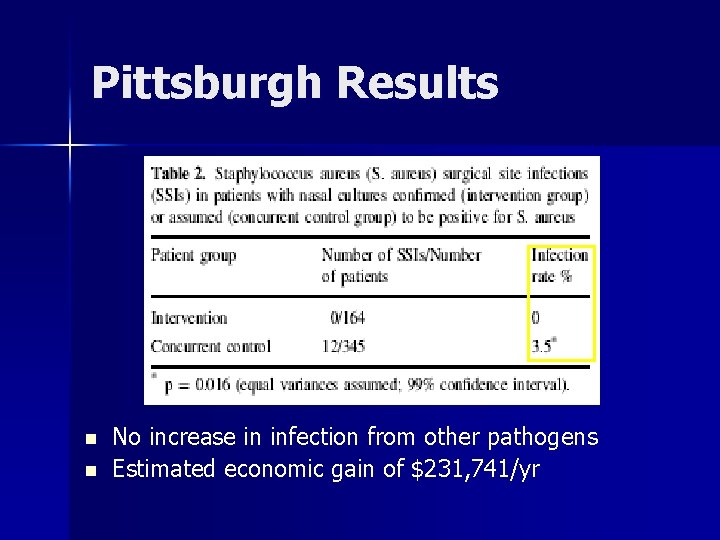

Pittsburgh Results n n No increase in infection from other pathogens Estimated economic gain of $231, 741/yr

NEBH Experience: Background n FY 06 - 46 SSI in 8986 surgical pts (0. 5%) – National rate for orthopedic SSI ~ 1. 5% n 57% SSI due to S. aureus – 16 (35%) MSSA – 10 (22%) MRSA n PFGE of isolates documented community acquired strains

Anonymous Nasal Surveillance Cultures February 2006 --133 anonymous nares cultures after patient anesthetized Results: 38 – S. aureus (29%) *5 - MRSA ( 4%) • all previously undiagnosed *no precautions used in OR, PACU or nursing units *Cefazolin used for antibiotic prophylaxis

Screening Proposals n February 2006 – prepared three screening proposals with costs 1) Traditional nasal cultures - 3 day results $245, 000. 00 2) Purchase rapid PCR equipment $337, 338. 00 3) Lease rapid PCR equipment $259, 990. 00 n March 2006 –Board approval of equipment purchase

Implementation – 8 Months n March – October 2006 – Weekly meetings: n – – surgical services, infection control, micro, administration, & medical staff members July 2006 – letter to surgeons July 17, 2006 – initiated pilot on Spine Service August 2006 – letter to medical staff September 2006 – initiated universal program for all inpatient surgery

Policy & Procedure Formalization n Protocol developed for all departments & units affected – – – – – OR Scheduling Patient Access Prescreening Unit Pre-surgical unit OR PACU Nursing Units Microbiology Lab Ancillary Departments: Housekeeping, Central Transport, Radiology, etc.

NEBH Program: Preoperative Outpatient Screening n n Nasal swabs during prescreening Microbiology Laboratory PCR detects presence of bacteria-specific DNA – Cepheid Gene. Xpert – Results within 24 hrs for S. aureus, 2 hrs for MRSA n Topical decolonization protocol for patients found to be carriers of S. aureus or MRSA

Topical Decolonization Protocol n n n n Intranasal 2% mupirocin ointment (Bactroban) BID x 5 days Shower with 2% chlorhexidine (Hibiclens) daily x 5 days Patients called by PASU to initiate treatment protocol Repeat call to document compliance MRSA carriers re-screened prior to surgery Contact precautions if 2 nd MRSA screen positive Vancomycin preop antibiotic prophylaxis for all patients with history of MRSA carrier status

Results n Study group (7/17/06 to 9/30/07) – 7019 patients screened n 5122 n 1588 n 309 (73. 0%) non-carriers (22. 6%) S. aureus positive ( 4. 4%) MRSA positive

S. aureus & MRSA SSI Rate n 13/7019 (0. 18%) SSI cases in screened patients – 7/5122 (0. 14%) in noncarriers (0. 14%) n n 1/5122 MRSA 6/5122 S. aureus – 6/1897 (0. 31%) in carriers n n n 3/309 + MRSA 3/1588 + S. aureus (0. 02%) (0. 11%) (0. 97%) (0. 19%) SSI rate higher in carriers, highest in MRSA carriers
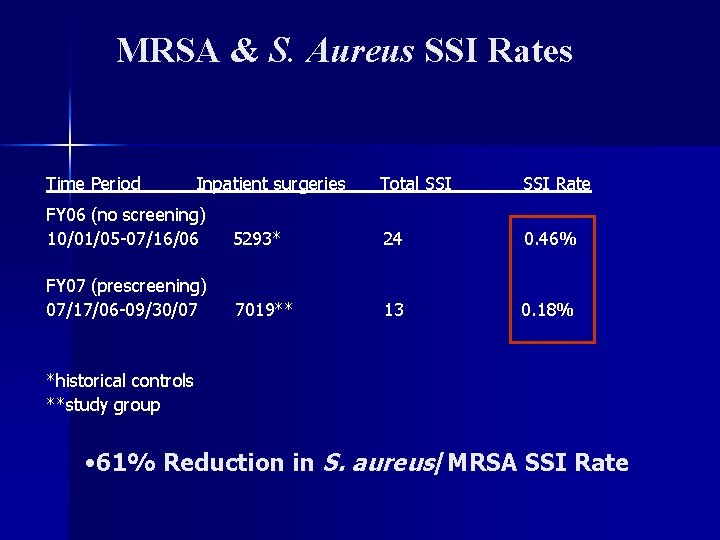
MRSA & S. Aureus SSI Rates Time Period Inpatient surgeries Total SSI Rate FY 06 (no screening) 10/01/05 -07/16/06 5293* 24 0. 46% FY 07 (prescreening) 07/17/06 -09/30/07 7019** 13 0. 18% *historical controls **study group • 61% Reduction in S. aureus/MRSA SSI Rate

50% Reduction in MSSA SSI 60% Reduction in MRSA SSI Rate MSSA SSI Rate 0. 26% 0. 18% 0. 13% 0. 06% 10/01/05 -07/16/06 07/17/06 -09/30/07

Study Limitations – Use of historical controls

Problem with Historical Controls n n n University of Amsterdam, The Netherlands Prospective double-blind, placebo-controlled 614 pts – Elective ortho surgery with implants (hip, knee, spine) n n Eradication rate 83. 5% mupirocin, 27. 8% placebo No reduction in SSI rate (primary outcome) – Rate of endogenous S. aureus infection 5 x lower [Kalmeijer et al, Clin Infect Dis 2002]
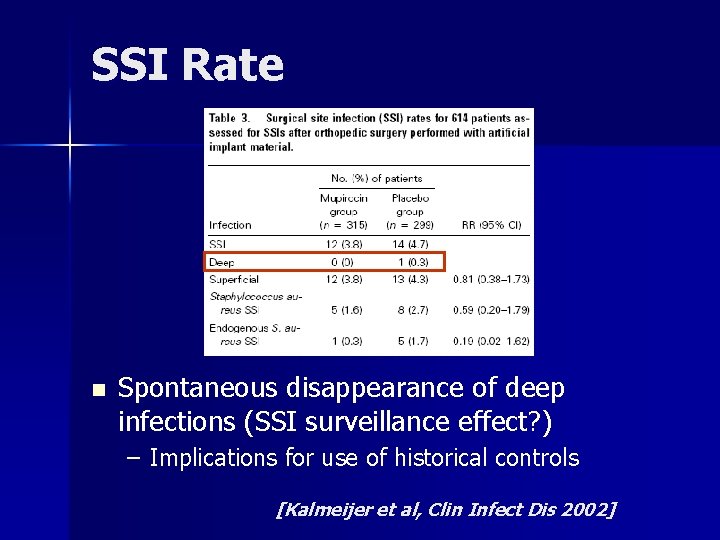

SSI Rate n Spontaneous disappearance of deep infections (SSI surveillance effect? ) – Implications for use of historical controls [Kalmeijer et al, Clin Infect Dis 2002]
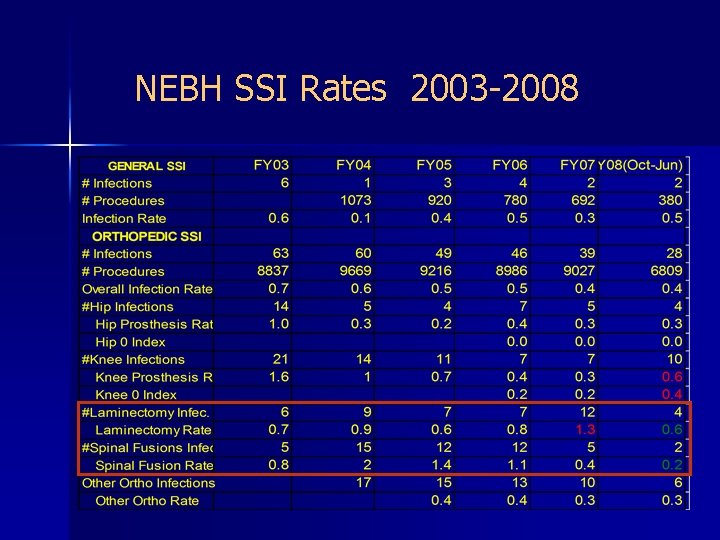
NEBH SSI Rates 2003 -2008

Conclusions: n n Program for comprehensive prescreening/treatment of S. aureus & MRSA prior to elective surgery is readily established & well-received Program allows early identification of colonized patients, treatment, & adjustment of antibiotic prophylaxis, early isolation & contact precautions for MRSA Associated with significant reduction in infections due to S. aureus & MRSA colonized patients continue to have higher rate of SSI

NEBH Program Cost First year costs ~$400, 000 ~$100, 000 for 2 full-time positions: • Microbiologist & PASU Medical Technician ~$60, 000 PCR rapid test equipment ~Lab cost for PCR $40. 00/test (compared to routine culture ~ $20. 00) ~ 6, 000 inpatient surgeries = $240, 000

Cost-effectiveness Analyses n Compared 3 strategies n n n Screen & treat Treat all Nothing – Assumptions n n S. aureus carrier rate 23. 1% Mupirocin efficacy 51%, cost $48. 36 Costs: septicemia $25, 128, pneumonia $18, 366, SSI $16, 256 Both treatment strategies cost-saving – Treat all: prevents 1 infection/116 pts; 1 death/10, 000 pts; save $88/pt – Screen & treat: prevents 1 infection/27 pts; 1 death/2500 pts; save $102/pt [Young and Winston, Infect Control Hosp Epidemiol 2006]

Cost-effectiveness n Budget impact model of rapid testing & decolonization – 7, 181, 484 elective surgeries in US (2003) – Rapid test cost $25/pt n n sensitivity 52% Specificity 85% – Decolonization cost $72. 50/pt n 56. 5% effective – 7. 5% SSI rate n n n 7. 5% in carriers 1. 5% in noncarriers $231, 538, 400 cost saving, 364, 919 fewer hospital days, 935 fewer in-hospital deaths [Noskin et al, Infect Control Hosp Epidemiol 2008]

Intangible Benefits n n NEBH S. aureus/MRSA prescreening & eradication program viewed very favorably as positive proactive infection control measure by staff, patients, family members & media Allows additional patient education on importance of hand hygiene, prevention of SSI, & infection control measures in home to reduce transmission of MRSA & S. aureus

Concerns

NEBH Screening Results n 7/17/06 to 9/30/07 – 7019 patients screened n n n 1588 (22. 6%) S. aureus positive 309 ( 4. 4%) MRSA positive through April 30, 2008 – 10, 815 patients screened n n 2712 ( 25%) S. aureus positive 507 ( 5%) MRSA positive Repeat nasal screens of MRSA carriers reveal 78% eradication rate Prevalence of carriers increasing

New England Baptist Hospital MRSA/MSSA Infection Rates Time Period Inpatient surgeries Surgical Infections Infec. Rate FY 06 10/01/05 -07/16/06 5293 24 0. 46% 7019 13 0. 18% 4770 4 0. 08% FY 07 07/17/06 -09/30/07 FY 08 10/01/07 -06/30/08

Conclusions n Targeted active surveillance useful – In outbreaks – In high-risk populations, e. g. ICU’s n Efficacy of universal surveillance & eradication remains unproven – Depends on regional variations in MRSA/MSSA epidemiology – Depends on hospital surveillance data n Stanford vs. UCSF

Acknowledgements Maureen Spencer, RN Brian Kwon, MD NEBH Board of Trustees Joseph Dionisio, NEBH President and CEO Ling Li, Ph. D David Hunter, MD, Ph. D

Thank You
- Slides: 62