MRSA MRS BRITT HEALTH SCIENCE I OBJECTIVES In

MRSA MRS. BRITT HEALTH SCIENCE I

OBJECTIVES • In this lesson you can expect to learn the following objectives. • Origin of Methicillin Resistant Staphylococcus Aureus. • Signs of MRSA infection. • Nosocomial transmission of MRSA. • Treatment of MRSA infection. • Your part in MRSA transmission prevention.

METHICILLIN RESISTANT STAPHYLOCOCCUS AUREUS • You have probably heard of a superbug that is causing illness to patients in the facility where you work. • MRSA causes skin infections and wound infections which are highly visible. • It also causes infections you can’t outright see all the time, like pneumonia or urinary tract infections. • MRSA infections can be deadly or lead to serious and chronic complications with a patient.

THE EVOLUTION • S. aureus is a bacteria that lives naturally on our bodies. • It is part of the normal flora that maintains a natural balance. Staphylococcus Aureus is a spherical bacteria that is found in clusters. • S. aureus is found in the nares and on the skin. • It does not automatically cause infection. www. cdc. gov
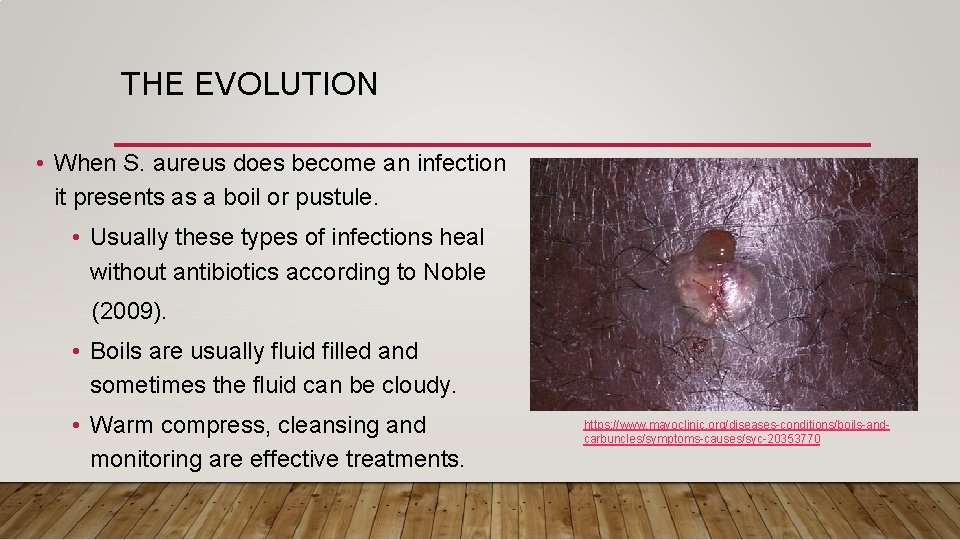
THE EVOLUTION • When S. aureus does become an infection it presents as a boil or pustule. • Usually these types of infections heal without antibiotics according to Noble (2009). • Boils are usually fluid filled and sometimes the fluid can be cloudy. • Warm compress, cleansing and monitoring are effective treatments. https: //www. mayoclinic. org/diseases-conditions/boils-andcarbuncles/symptoms-causes/syc-20353770

THE EVOLUTION • When S. aureus enters the blood stream through a cut or otherwise it can cause a serious infection called Sepsis. • Sepsis is a serious blood infection. • This does require antibiotics for treatment. • S. aureus is treated with methicillin antibiotics.

THE EVOLUTION • The evolution of S. aureus to MRSA occurred with misuse of antibiotics. • Whose fault was it? • Doctors were ordering antibiotics even if not needed. • Patients were not completing the antibiotic prescription. • Doctors ordered antibiotics without checking a culture & sensitivity test first. • MRSA is S. aureus with a protective armor that shield antibiotic treatment.
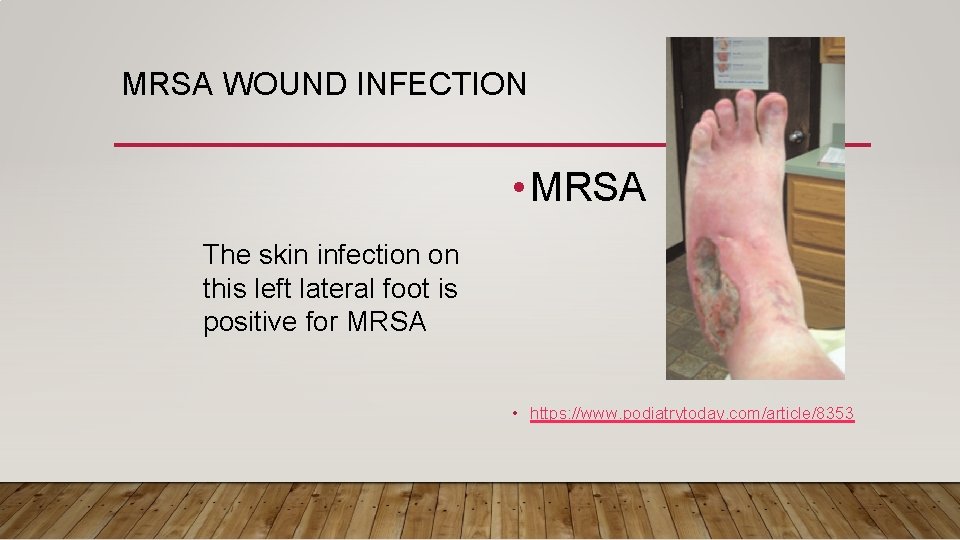
MRSA WOUND INFECTION • MRSA The skin infection on this left lateral foot is positive for MRSA • https: //www. podiatrytoday. com/article/8353

TRANSMISSION COMMUNITY ACQUIRED • Infection is contracted while living in the community. NOSOCOMIAL • Infection is contracted during a hospital stay. According to the CDC, MRSA can survive on a surface without a host for months in the right environment.

TRANSMISSION COMMUNITY ACQUIRED INFECTIONS • “MRSA is most frequently found on the patient or athlete-contact surfaces of athletic training room facilities. ” (Montomery, Ryan, Krause & Starkey, , 2010. para. 14). • MRSA can also be found on shopping carts, in locker rooms, chairs, or desks in schools. https: //gettysburgsports. com/facilities/athletic-training-and-sports-therapy/71

TRANSMISSION NOSOCOMIAL • MRSA can be carried from room infected patient to susceptible patient by: • Equipment • Staff uniforms • Dirty linens • Shoes • Cracked nail polish or jewelry Q. HOW CAN WE PREVENT THE TRANSMISSION? A. By breaking the chain of infection, maintaining aseptic technique and following protocol at ALL times.

TREATMENT • MRSA has an enzyme property that prevents penicillin from killing it. ØTherefore, Vancomycin is the effective treatment for MRSA infections. • Vancomycin is delivered intravenously (IV). ØIt is highly irritating to the vessel where the IV is inserted ØFrequently given through a Peripherally Inserted Central Catheter (PICC) line to maintain health of the blood vessels. (pictured above) www. my. IV. com

TREATMENT Vancomycin is usually effective to treat MRSA, but it can cause complications. • Clostridium Difficile (C. difficile) infection of the bowel • Redman’s Syndrome These are two of the main complications related to vancomycin treatment.

TREATMENT • Vancomycin is a very strong antibiotic. • It is a broad-spectrum antibiotic also, this means it kills many different types of bacteria. Due to it’s strong nature vancomycin wipes out the normal flora of the body allowing some unwanted bacterial infections. • C. diff is one of those infections • C. diff creates chronic and severe colitis in the patient creating a whole new condition to battle.

https: //casereports. bmj. com/content/2009/bcr. 03. 2009. 17 TREATMENT • Redman’s Syndrome is a various serious complication of vancomycin treatment. v Redman’s Syndrome occurs when the IV antibiotic is infused too quickly. Ø Redman’s Syndrome has the following signs and symptoms: • • Red, hot and inflamed skin Leathery skin Severe shortness of breath Dizziness These signs are very important to recognize as Redman’s Syndrome could lead to Organ failure and death. Always report any suspected sign or symptom of Redman’s Syndrome to the charge nurse immediately.
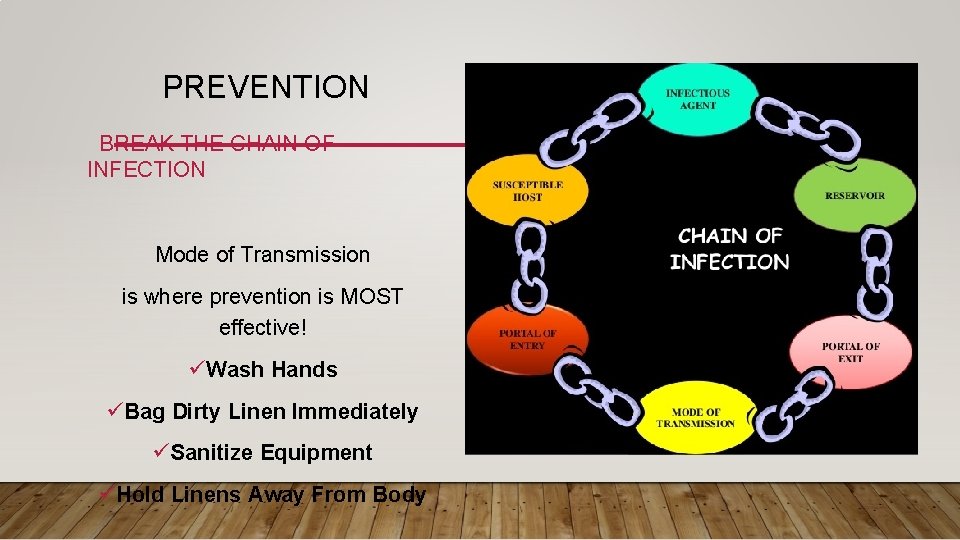
PREVENTION BREAK THE CHAIN OF INFECTION Mode of Transmission is where prevention is MOST effective! üWash Hands üBag Dirty Linen Immediately üSanitize Equipment üHold Linens Away From Body

PREVENTION FOLLOW ASEPTIC TECHNIQUE üWash Hands üWear Gloves or other PPE üBag Dirty Linen Immediately üSanitize Equipment üHold Linens Away From Body üUse Isolation Precautions as Directed PPE = PERSONAL PROTECTIVE EQUIPMENT

PREVENTION The MOST effective way to break the Mode of Transmission is by WASHING HANDS. This student created video demonstrates the proper method of washing hands.
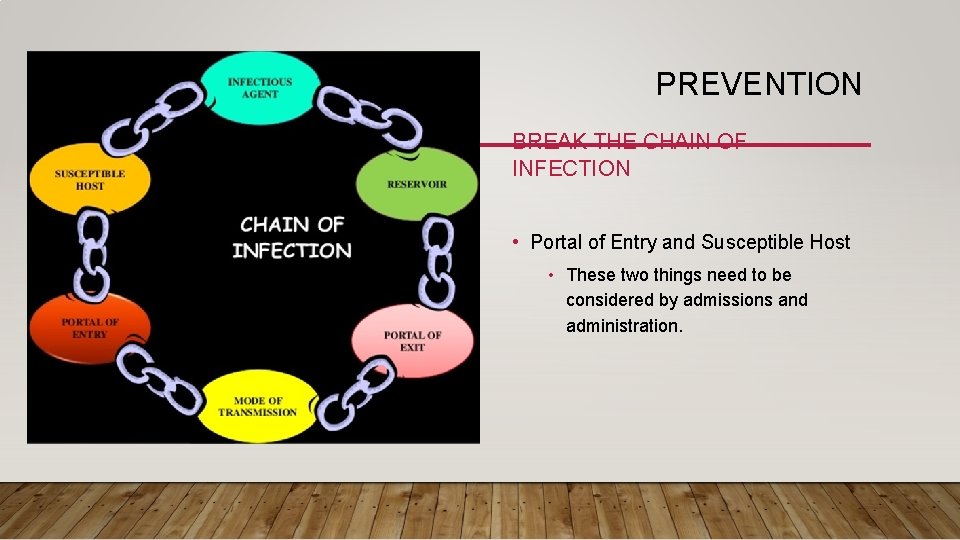
PREVENTION BREAK THE CHAIN OF INFECTION • Portal of Entry and Susceptible Host • These two things need to be considered by admissions and administration.

PREVENTION • Patient with MRSA can only have specific roommates. • The roommate must be free from: • Wounds • Surgical Incisions • Tube Feeding • IV • Indwelling Foley Catheter • A disorder that compromises the immune system * This rules also accounts for a patient with MRSA colonized or old resolve MRSA infections.

SUMMARY • It is important that you are aware of MRSA infections within your patient schedule. • Always wash hands, follow aseptic technique, and consider roommate placements. • WASHING HANDS IS THE NUMBER ONE WAY TO PREVENT THE SPREAD OF MRSA. • Monitor those who receive vancomycin treatment for signs of Redman’s Syndrome. • Report your findings to the charge nurse. • Remember, if you are unsure about something you see, or how to address a

References Buckingham, S. C. (2008, December). Prevention of recurrent MRSA skin infections: What you need to know. Consultant, 48(13), 1031. Retrieved from https: //link. gale. com/apps/doc/A 192589337/AONE? u=lom_ferrissu&sid=AONE&xid=e d 107799 Carikas, K. , & Matthews, S. (2019). Hospital privacy curtains –What’s hanging around? . The Dissector: Journal of the Perioperative Nurse College of the New Zealand Nurses Organisation, 47(1), 20+. Retrieved from https: //link. gale. com/apps/doc/A 588342216/AONE? u=lom_ferrissu&sid=AONE&xid=2 5 e 0 e 519 Enright, M. , Robinson, A. , Randle, G. , Feil, E. , Grundmann, H. , Spratt, B. (2002). The evolutionary history of methicillin-resistant Staphylococcus aureus (MRSA). Proceedings of the National Academy of Sciences of the United States of America, 99(11). doi. org/10. 1073/pnas. 122108599

Harrison, S. (2005). How to stay on the right side of the infection control code: Nurses who spread MRSA are as culpable as nurses who give patients the wrong drug, say lawyers. Nursing Standard, 19(38), 14+. Retrieved from https: //link. gale. com/apps/doc/A 133569471/AONE? u=lom_ferrissu&sid=AONE&xid =1 e 9566 c 5 Mc. Namara, D. (2007, May). MRSA treatment begins at the skin. Skin & Allergy News, 38(5), 21. Retrieved from https: //link. gale. com/apps/doc/A 163738259/AONE? u=lom_ferrissu&sid=AONE&xid =9 ccc 0159 Montgomery, K. , Ryan, T. J. , Krause, A. , Starkey, C. (2010). Assessment of athletic health care facility surfaces for MRSA in the secondary school setting. Journal of Environmental Health, 72(6), 8+. Retrieved October 12, 2019, https: //link. gale. com/apps/doc/A 215481007/AONE? u=lom_ferrissu&sid=AONE&xid=b 3 da 337 a Noble, D. B. (2009, November-December). Patient education on MRSA prevention and management: the nurse’s vital role. Med. Surg Nursing, 18(6), 375+. Retrieved from https: //link. gale. com/apps/doc/A 215481570/AONE? u=lom_ferrissu&sid=AONE&xid=5 e 5 c 1 a 2 a

Sadsad, R. Sintchenko, V. , Mc. Donnell, G. D. , & Gilbert, G. L. (2013). Effectiveness of hospitalwide methicillin-resistant staphylococcus aureus (RSA) infection control policies differs by ward specialty. PLo. SONE, 8(12). Retrieved from http: //dx. doi. org. ferris. idm. oclc. org/10. 1371/journal. pone. 0083099 Thompson, C. A. (2007). Community-acquired skin infections remain treatable. American Journal of Health-System Pharmacy, 64(24), 2524+. Retrieved October 13, 2019, from https: //link. gale. com/apps/doc/A 176818978/AONE? u=lom_ferrissu&sid=AONE&xid=d e 01 c 4 d 8 Trueland, J. (2011). A stick to beat MRSA: nurses at one trust are celebrating after two years without MRSA infection. Nursing Standard, 26(2), 23. Retrieved from https: //link. gale. com/apps/doc/A 269027727/AONE? u=lom_ferrissu&sid=ao. NE&xid=26 b 7 f 54

Vogel, C. (2008, May). Stopping MRSA: consistent simple procedures can keep this communicable disease at bay. District Administration, 44(6), and 42+. Retrieved from https: //link. gale. com/apps/doc/A 179159647/AONE? u=lom_ferrissu&sid=AONE&xid=3 2 bf 71 a 1 Welsh, J (2015, March). Reconsidering contact precautions for MRSA and VRE. The American Journal of Nursing, 115(3), 14+. Retrieved from https: //journals. lww. com/ajnonline/fulltext/2015/03000/Reconsidering_Contact_Precauti ons_for_MRSA_and_VRE. 8. aspx

Visual Art (Pictures had links to further informational articles) www. my. IV. com https: //www. mayoclinic. org/diseases-conditions/boils-andcarbuncles/symptoms-causes/syc-20353770
- Slides: 26