Moving into Family Inclusive Practice Sian Kennedy Bridging

Moving into Family Inclusive Practice Sian Kennedy - Bridging the Divide project officer, Family Drug Support 1

Overview Introductions Family systems theory Assessment skills Assisting families to understand drug use Coping strategies for families 2

Family Drug Support MISSION STATEMENT To assist families throughout Australia to deal with drug issues in a way that strengthens relationships and achieves positive outcomes PHILOSOPHY Our energies are given in primarily supporting families struggling as a result of drug use. We aim to assist in any way possible to empower families to cope with the realisation of their situation and survive intact 3

FDS continued CEO - Tony Trimingham AOM Established in 1997 Largely peer-based with some professional staff 24/7 support line: 1300 368 186 Support meetings held in NSW, QLD, ACT & VIC Stepping Stones to Success course for families 4

Bridging the Divide Bridging The Divide funded by Department of Health & Ageing (Do. HA) Increasing treatment opportunities and resources for families affected by AOD issues Providing resources for workers within the AOD Sector Increase capacity of AOD treatment services to respond to the needs of families 5

And me. . . 10 years experience in the alcohol & other drug sector in Victoria Worked in a variety of roles: detox units, residential rehab, supported accommodation, counselling as well as specialist consulting roles within child protection, psychiatric services & homelessness services Particular interest in training & education - taught certificate IV in AOD work for years through Odyssey House & Victoria University & currently teach Bachelor of Social work at RMIT (in my spare time ; -) 6

Is it my job? • • ‘core role only’ (‘it’s not my concern’) ‘core role plus assessment of ‘other needs’, leading to referral’ (‘it’s a concern but someone else’s job – refer on’) ‘other needs incidental but unavoidable’ (‘not my core role but I have to do it’) ‘other needs’ intrinsic part of core role (‘it’s part and parcel of my job’) (Mc. Caughey et al 1977) 7

Family Systems Theory “But I’m not a family therapist”. . . 8

What is family? Family is a basic unit of understanding ourselves in society Many people, not just our clients, spend much time trying to make sense of their own family experience In Australia, two parent households with dependent children makes up about 1/3 of Australia’s families (ABS 2008) 9

Families often subject their own members to discrimination & oppression, and that families in turn, particularly those you are likely to encounter in your services, experience discrimination & oppression, in a pattern of oft repeated cycles. 10

Overwhelmingly, though not exclusively, being in a lower socio-economic bracket makes families more likely to have intervention from services & workers. The experience of ‘family’ is often challenging for most of us. 11

What are some of these factors? 12

Systems Theory Systems theory focuses on individuals as part of a system Incorporates the social with the psychological elements of practice Systems interact with each other Families are their own discreet system, operating as part of much larger societal systems 13

Types of systems • Natural systems: families, colleagues, friendship circles • Formal systems: trade unions, self-help groups • Societal systems: hospitals, schools 14
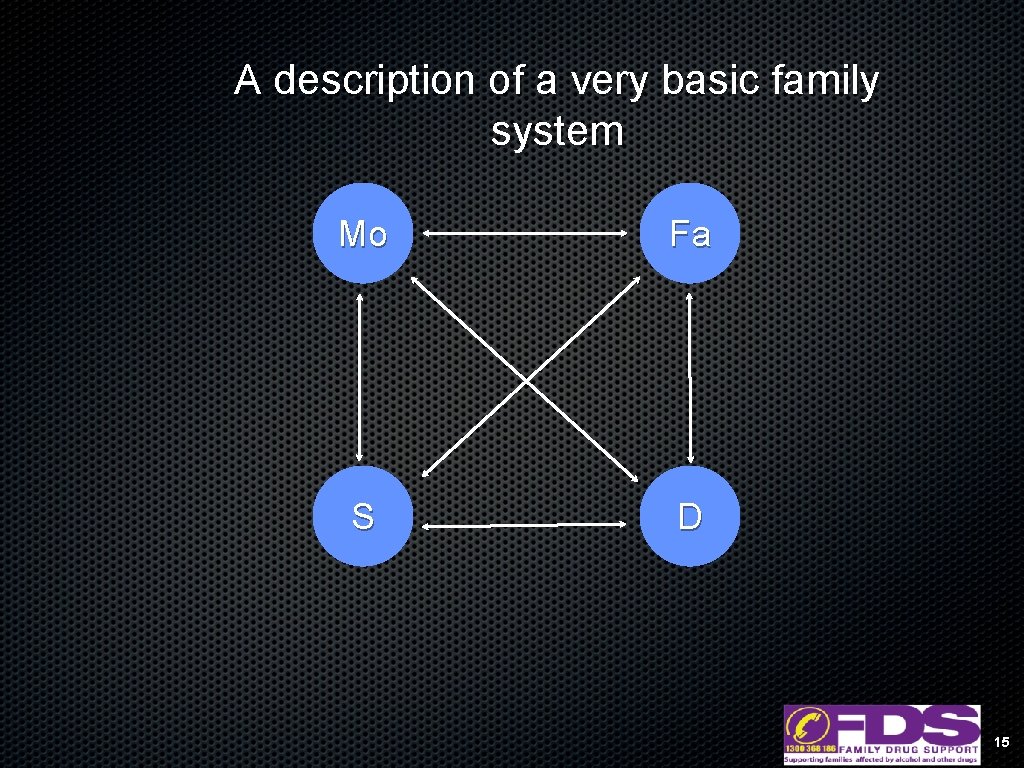
A description of a very basic family system Mo Fa S D 15

Systems have structure • • Systems are entities with definable boundaries & resources are more often shared within than across those boundaries Closed & open systems – as workers/women/Aboriginal/non-Aboriginal/family members etc some systems will be closed or open to us, depending on our own roles 16

Steady state: can incorporate change without changing its fundamental identity 17

Homeostasis: ability to maintain fundamental identity, even though external resources will alter us 18

Differentiation: that systems will grow more complex over time as new components are added 19

Non-summativity: systems are worth more than the sum of their parts 20

Reciprocity: if one integral part of the system changes, that change affects all the other components. Hence, they all change. 21

Some psychological theories Ones which apply to how we relate to others 22

Trauma Theory Attributed to witnessing disasters, violence, assault, destruction, near-miss incidents & other mayhem Creates a lasting sense of helplessness, vulnerability, loss of safety & trust Lasting neurological impact , particularly in children Intergenerational impact is poorly understood, often re -victimising survivor’s children (Stolen Generations & subsequent generation) 23

Evidence exists that parental trauma impacts on the ability to parent, despite a parents’ often best attempts to mask it Trauma theory is not merely the diagnosis of PTSD as we are concerned with how trauma impacts on social interaction 24

An important distinction PTSD is the description of a cluster of symptoms arising from exposure to a terrible event PTSD is more common after an event caused by other people PTSD is an Anxiety Disorder Despite high probability of exposure to some form of trauma, PTSD is a low-prevalence disorder (~8% population) 25

All that said, people who have been in out of home care have higher rates of PTSD diagnoses than returned soldiers 26

Attachment theory John Bowlby (1951) Describes the relationship between caregivers & dependents, most commonly parents & children First described during WWII & the experiences of children orphaned Secure, avoidant, anxious & disorganised attachment 27

• Attachment basically means a secure bond of affection between people • Important to understand that humans are interdependent – our social adaptability is one of our strongest evolutionary traits • Humans are one of the slowest mammals to mature • Secure attachment builds the confidence to be independent 28
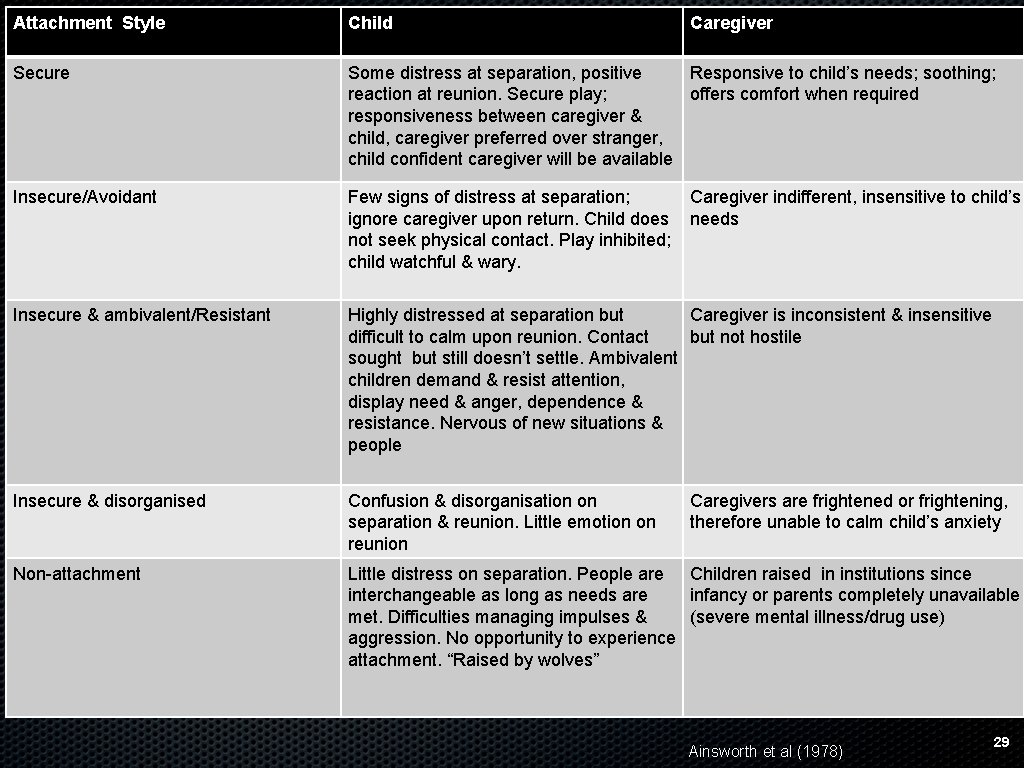
Attachment Style Child Caregiver Secure Some distress at separation, positive Responsive to child’s needs; soothing; reaction at reunion. Secure play; offers comfort when required responsiveness between caregiver & child, caregiver preferred over stranger, child confident caregiver will be available Insecure/Avoidant Few signs of distress at separation; ignore caregiver upon return. Child does not seek physical contact. Play inhibited; child watchful & wary. Insecure & ambivalent/Resistant Highly distressed at separation but Caregiver is inconsistent & insensitive difficult to calm upon reunion. Contact but not hostile sought but still doesn’t settle. Ambivalent children demand & resist attention, display need & anger, dependence & resistance. Nervous of new situations & people Insecure & disorganised Confusion & disorganisation on separation & reunion. Little emotion on reunion Non-attachment Little distress on separation. People are Children raised in institutions since interchangeable as long as needs are infancy or parents completely unavailable met. Difficulties managing impulses & (severe mental illness/drug use) aggression. No opportunity to experience attachment. “Raised by wolves” Caregiver indifferent, insensitive to child’s needs Caregivers are frightened or frightening, therefore unable to calm child’s anxiety Ainsworth et al (1978) 29

Attachment theories are important when understanding our adult clients • • • Attachment types are reasonably stable, unless adult relationships heal earlier attachment issues We understand ourselves largely through our social interactions & we understand others through our understanding of ourselves In assessment, we use attachment to explore current relationships, family of origin & environmental stressors 30
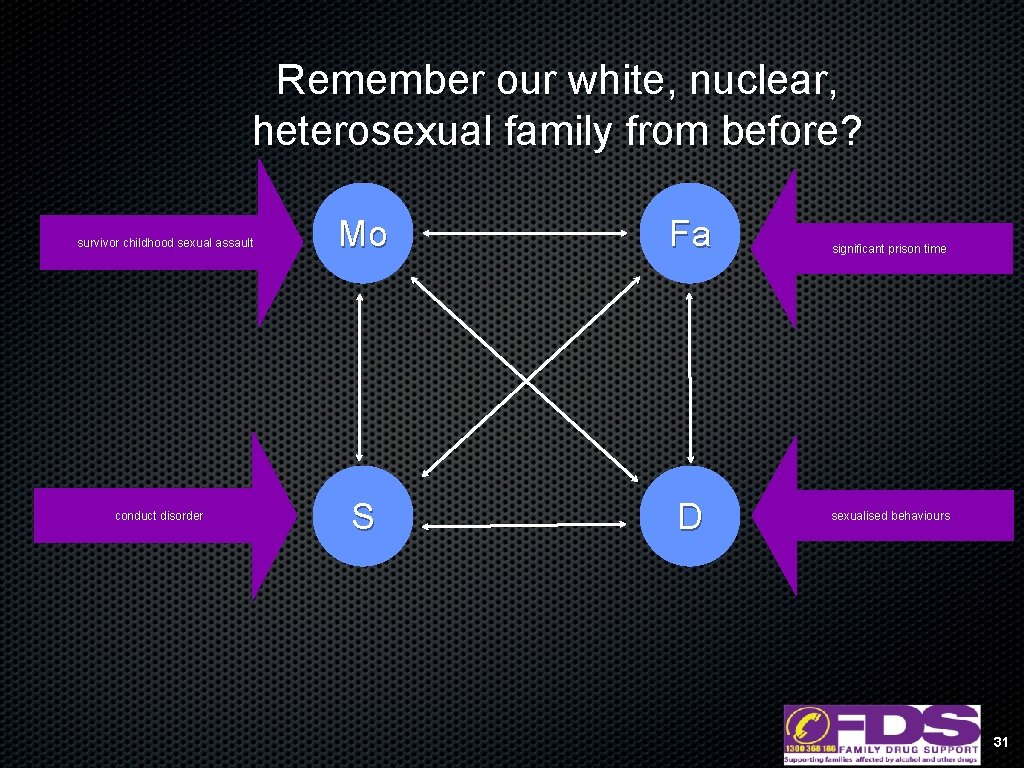
Remember our white, nuclear, heterosexual family from before? survivor childhood sexual assault conduct disorder Mo Fa S D significant prison time sexualised behaviours 31
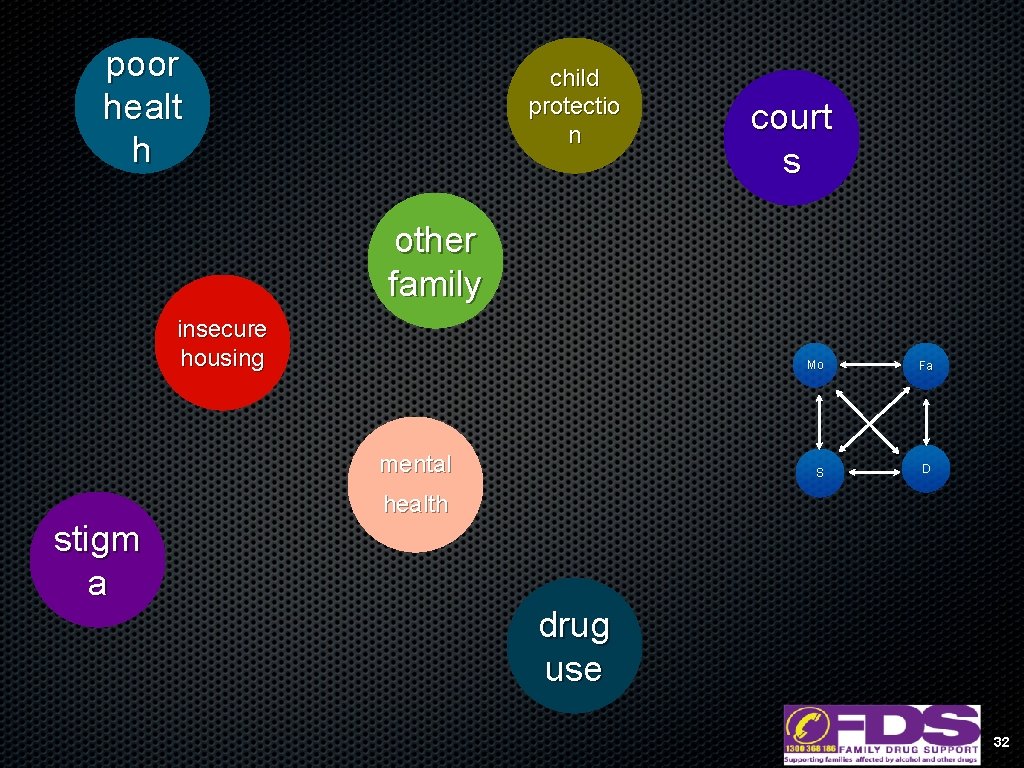
poor healt h child protectio n court s other family insecure housing mental Mo Fa S D health stigm a drug use 32

It’s important as workers to understand the systems context when we are dealing with families 33

Some musings on power by Foucault Power is exercised, not possessed Power is both oppressive & productive: power over & power to Power comes from the bottom up & we all have the ability to create it 34

“But our assessment tool is already soooo long” INTAKE & ASSESSMENT 35

How routine is assessment in your service? • Telephone screening • Initial screening • Specialist assessment • Full psycho-social assessment & history • Ongoing assessment & case planning 36

Here are some I prepared earlier. . . 37

Issues to be alert for during assessment • Drug use & • Problematic alcohol use • Family Violence • Child abuse – emotional/physical/sexual & environmental neglect issues 38

“they’re never going to get better. . . ” ASSISTING FAMILIES TO UNDERSTAND DRUG USE 39

Common experiences • Shame & guilt • Blame • Fear • Isolation & loneliness • Grief & loss • Despair that there is no solution • Profound sadness • Trauma • Judgement • • High level conflict Ignorance/misinformation about drugs/mental illness 40

To start with • • Explain that people use drugs for lots of different reasons There aren’t a clear set of vulnerability criteria, ie: apportioning blame is difficult • We live in a drug taking society • Not everyone who uses drugs will become an “addict” • Mental illness affects 1 in 5 Australians during lifetime 41

If a history of drug/alcohol use/mental illness in the family was an accurate predictor, we would nearly all have a “problem” 42

But if the situation is further advanced than that. . . • • • Families won’t necessarily know what people are using, quantities, frequencies etcetera, so general drug information is useful but don’t frighten them unnecessarily Preferably give written information as families coming to a service are likely to be in a period of high stress Help families understand that only drug users can change their own behaviour 43
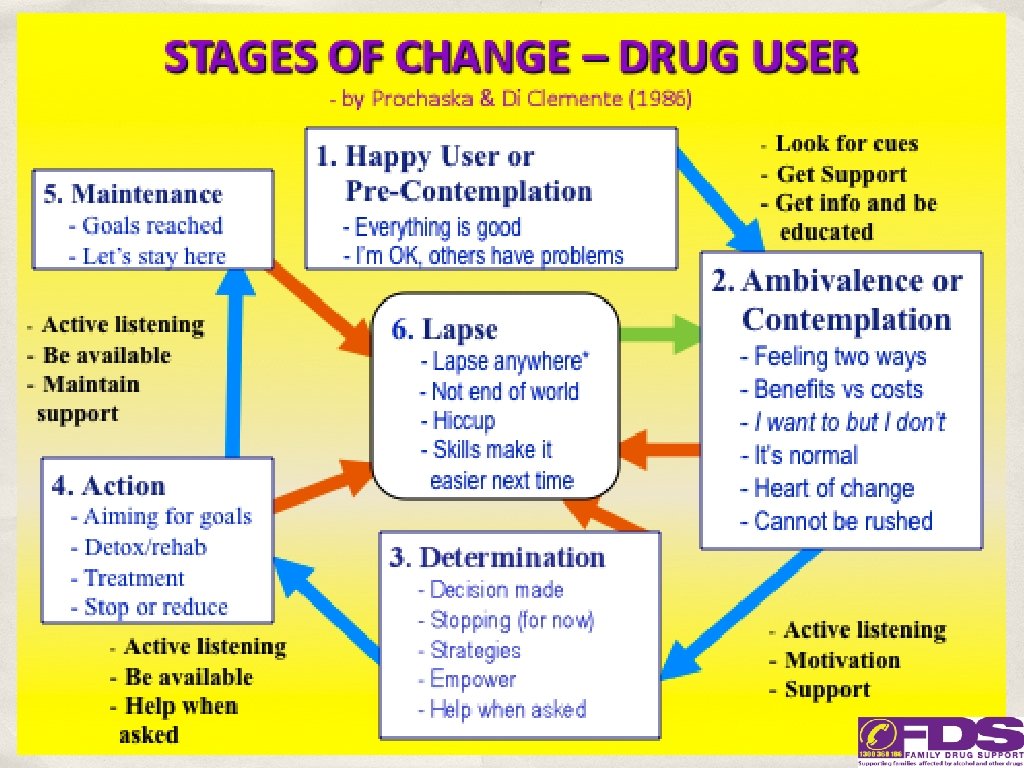

Understanding where the family is at with the drug use 45
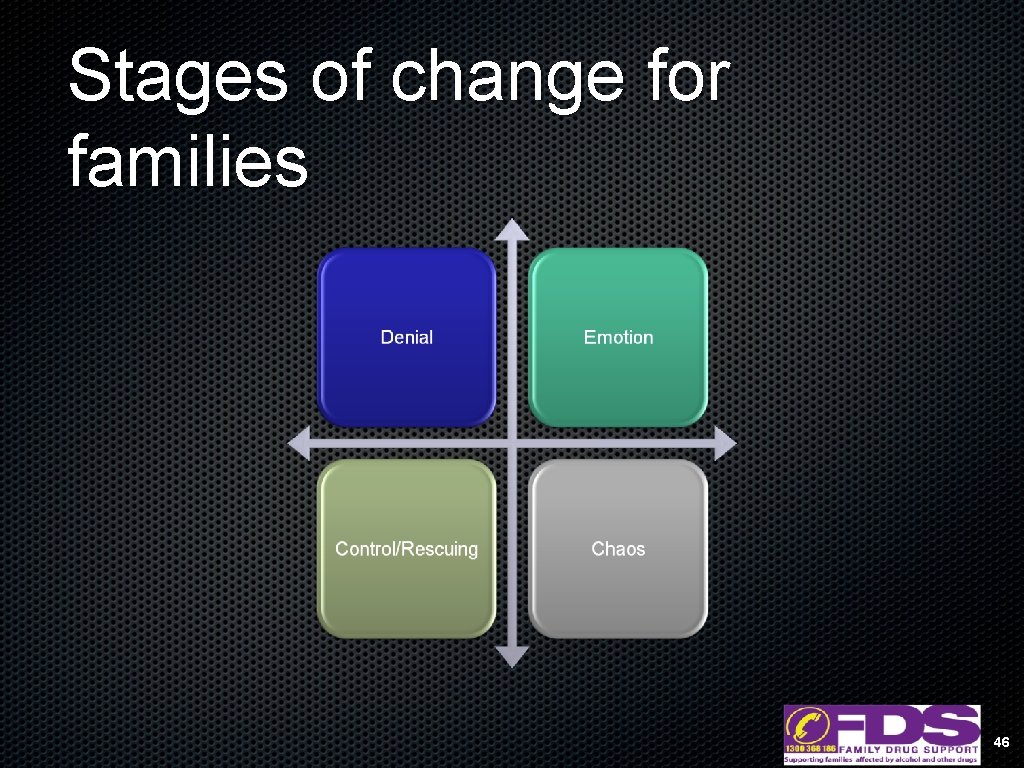
Stages of change for families 46

Denial • Feelings of shock • Isolating from other friends/family networks • Uncertain about own role in other person’s drug use • Covering up for the drug user • Unlikely to seek help 47

Emotion • Reactive • Starting to understand the enormity of the problem • Strong shame/guilt/stigma/stress/anger • Feeling torn in multiple directions • Overwhelmed • Recognise the need for help, but still unlikely to seek it out 48

Control/Rescue • Acknowledge the drug use, think the solution is simple • “Do what I say” to fix the problem • Expect trust but are afraid to give it • You ‘know’ who and/or what is responsible • Trying to get help for the drug user 49

Chaos • • Confidence is depleted Family relationships are often falling apart by this stage Exhaustion Feel that everything has been tried & that nothing will work 50

At this stage, a couple of things are possible 51

Talk to families about the idea that their ability to cope is separate from whether the drug user stops using/gets better 52

Target approach to where family member is at in the stages of change 53

Practical tips to help families during each stage 54

Pre-contemplation TIPS TO HELP THEM • • Be patient Tell them you are there for them if they need it TIPS TO HELP FAMILIES • Get information • Get support for yourself • • • Be open & honest in your communication with them Listen • Look for cues – when they want to talk to you, make time to listen Encourage them to be honest about their drug use 55

Contemplation TIPS TO HELP THEM • • • Provide information to reinforce the good & bad aspects of drug use TIPS TO HELP FAMILIES • • Be willing to listen & continue to be patient • Remind them of their good qualities & talents • Talk things over with others Try to understand the process & the stage they are at Communicate what you will & won’t accept, in a positive way Keep listening & don’t push the ‘give up’ message too hard 56

Preparation TIPS TO HELP THEM • TIPS TO HELP YOU Keep LISTENING • • • Help them get information Stay in touch, particularly if they aren’t at home. • • • Reinforce their plan for change • Be positive with them Develop agreements with them now Look after yourself Don’t always rescue them when things get tough for them (learn to let go) 57

Action TIPS TO HELP THEM • • • Be positive about the steps they’ve taken so far TIPS TO HELP YOU • • Continue to be patient & listen Acknowledge & celebrate their successes, no matter how small • Be available If asked, help them get reestablished in the community Now is a good stage to invest your resources in them 58

Maintenance TIPS TO HELP THEM • • • Don’t test them (eg. Leaving money around to see if they take it) Encourage them, letting them know that you know how far they’ve come. TIPS TO HELP YOU • • Feel pleased in the supportive role you have played in their recovery Acknowledge the relief you feel, but know that this too shall pass Provide practical support 59

Lapse TIPS TO HELP THEM • • TIPS TO HELP YOU Be encouraging & positive Let them know you haven’t lost faith in their capacity to maintain recovery Reinforce what they have achieved so far Reinforce that lapse is part of the journey & that it’s part of the learning process • • All is not lost: relapse is almost certainly past of any journey of recovery Seek out the support networks you have cultivated throughout 60

“Will it ever stop? ” HELPING FAMILIES COPE 61

It’s ok for them to feel however they feel about the drug user Love/hate is common, even for parents & siblings It’s possible to love the person but hate the behaviour 62

Common dilemmas for families • Violence or the threat of violence • Impact on non-using family members • Stealing • Allowing people to remain at home 63

“Should I tell them not to come home drug affected? ” FOR • • • AGAINST A quick solution to possible conflict • What if something happens to them? • Anxiety ++ Problem is less visible if you can’t see it Protects the rest of the family • • Your disapproval is obvious Your relationship with them might be affected 64

“Should I give them money? ” FOR • • • Their need to commit crime for their drug use is reduced Alleviate the immediate symptoms of withdrawal Makes life easier for you in the short term AGAINST • • • It might become more expensive than you can afford You might feel resentful about your decision or manipulated into it Creates a pattern whereby they will ask again 65

“What if they steal from us – should we call the police? ” FOR AGAINST • • Keeps you & your family safe Sets up a cycle of boundaries & consequences Might help them reach their “rock bottom” • • Your relationship with the drug user is likely to deteriorate Involvement in the criminal justice system is not good for their prognosis: the further entrenched in drug use they become, the harder it is to get out You might not actually be able to follow through 66

Violence is never acceptable But apart from that, there are no clearly right or wrong answers Families are frequently confused by the conflicting “advice” they receive from health professionals 67

Families need to be supported to make the best decisions they can in the circumstances they are in, with the resources they have available 68

Boundaries • • • The same ones that we all learn about & how to implement them Consequences for behaviour are important so that families (particularly parents) retain some semblance of control & authority Understanding & establishing your bottom line, both with self & with the drug user 69

Communication • The same things we all learn about & how to do it effectively • “I” statements • Talking about feelings, not acting on them • Listen • Be as informed as you can be • Listen for signs of change 70

Strategies • • Focus on self (or rest of the family) rather than the drug user Accept the reality of the situation, for now. Don’t exhaust yourself on a family member who “hasn’t turned up” for the process Offer support, not rescue Adopt a problem-solving approach, not a problem saturated one 71

Great resources ✤ www. strongbonds. jss. org. au ✤ www. crcnsw. org. au ✤ www. siblingsupport. com. au ✤ www. edas. org. au/family_resources ✤ www. copmi. net. au ✤ www. eddiegallagher. id. au/ 72

References Allen, J. , Briskman, L. & Pease, B. (eds) 2009 Critical Social Work: theories & practices for a socially just world. Allen & Unwin; Crows Nest Ainsworth, M. , Blehar, M. C. , Waters, E. & Wall, S. (1978) Patterns of attachment. Earlbaum: New Jersey Clausen. M. (2009) Audit of Family Inclusive Practice in Alcohol & Other Drugs Services in the EMR, Springboard Social Planning Dawe S, Harnett P, Frye S. (2008). Improving outcomes for children living in families with parental substance misuse: what do we know and what should we do. Australian Institute of Family Studies, National Child Protection Clearing House, Child Abuse Prevention Issues, Paper No 29 Department of Human Services & Turning Point Alcohol & Drug Services (2000) Specialist Assessment Form (For General Client Population) Eastern Drug & Alcohol Service, (2010) The Family Focus Toolkit’, EDAS Family Focus Project Family Drug Support & Qu. IHN (2007) A guide to coping: support for families faced with problematic drug use. Family Drug Support (2009) Stepping stones workbook: guiding families through a journey of coping with drug & alcohol use. Australian Drug Foundation: Melbourne Payne, M. (2005) Modern Social Work Theory. Palgrave Macmillan: New York Weeks, W. & Quinn, M. (eds) (2000) Issues facing Australian Families 3 rd edition. Pearsons Education: Frenchs Forest 73
- Slides: 73