Mount Auburn Practice Improvement Program MAPIP Community Learning

Mount Auburn Practice Improvement Program (MA-PIP) Community Learning Session #3 Improving Communication: To Improve Care and Patient Satisfaction While Reducing Malpractice Risk Yvonne Cheung, MD, MPH, CPPS Chair, Department of Quality and Patient Safety Mount Auburn Hospital December 4, 2015 This project is funded through a Commonwealth of Massachusetts - Health Care Workforce Transformation Fund Grant (#54038)

Learning Objectives As a result of participating in this activity, learners will be able to: § Describe strategies and tools that improve communication with patients and patient safety § Use small tests of change to make it feasible to improve care while providing care § Identify and employ strategies for engaging patients in improvement work.

Disclosure Statement All Presenters and Content Developers have no significant financial interest/arrangement with any organization(s) that could be perceived as a real or apparent conflict of interest with the subject matter of the presentation.

Mount Auburn Practice Improvement Program (MA-PIP): Why now? § Purpose: Improving patient safety in office practice/ambulatory care § § § Enabling your practice to improve your work while you do your work- “see problems and solve problems” Build on a proven model – federally funded PROMISES program Build infrastructure, integrate with current ambulatory patient safety program

Key Concepts For Safety § Focus on systems, not people § Work on a culture of safety For improvement: § Define a clear aim § Use measurement and data for decision making § Remember that improvement requires change § Keep testing using PDSA cycles – keep tests small For everything: § Remember that customers are key

Science of Patient Safety § § Systems thinking § Most problems do not result from individual workers; but from the design of work processes/system Safety culture § Leadership & values § Teamwork & communication § Trust, psychological safety What if you started your staff meetings with the question: “Do you have any patient safety concerns we can talk about? ”
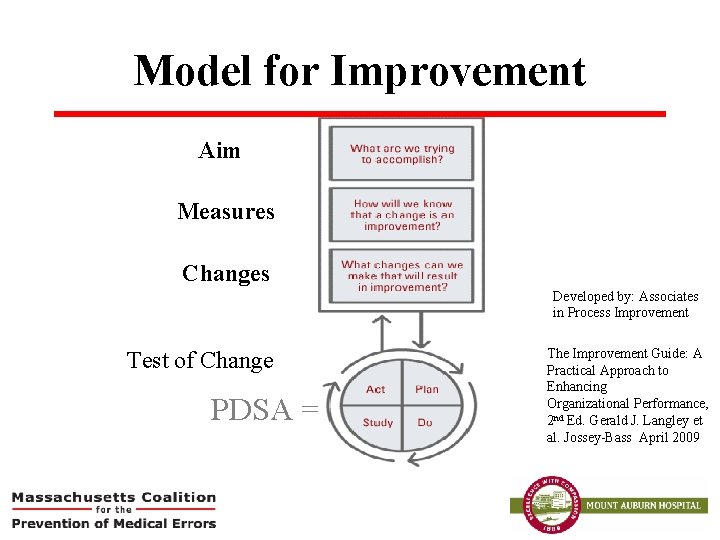
Model for Improvement Aim Measures Changes Developed by: Associates in Process Improvement Test of Change PDSA = The Improvement Guide: A Practical Approach to Enhancing Organizational Performance, 2 nd Ed. Gerald J. Langley et al. Jossey-Bass April 2009

Patient Safety Priorities in Ambulatory Care Reliable processes - 3 key areas: -Test result management -Referral Management -Medication Management Communication – With patient, among staff, across settings What keeps you up at night? 8

Why Focus on Communication Physician-Patient Communication: The Relationship with Malpractice Claims Among Primary Care Physicians and Surgeons § Study identified specific communication behaviors among Primary Care physicians with no malpractice claims vs. those who had experienced malpractice claims Levinson, et al. , JAMA 1997 277(7): 553 -339 9

Those Without Claims: § Used statements of orientation (educating the patient about what to expect/flow of the visit) § Used more facilitation (soliciting patient’s opinion, checking understanding, encouraging patient to talk) § Spent longer in routine visit – 18. 3 vs. 15. 0 minutes (independent effect in predicting claims status) Summary question: Did it build a positive relationship, or lead to fewer errors, or both?

From latest IOM Report: To Improve Diagnosis and Reduce Diagnostic Error Goal 1 - Facilitate more effective teamwork in the diagnostic process among health care professions, patients and their families Recommendation 1 B: § Partner with patients and families as diagnostic team members § Facilitate patient and family engagement in the diagnostic process § Align with their needs values and preferences

Communication Issues for Today’s Discussion § For today’s discussion – not focused on patients with “additional” communication challenges § health literacy, § language barriers, § cultural literacy etc. § Focus is communication with patients without barriers, but still have symptoms not addressed, unanswered questions, unclear understanding, concerns with the treatment etc.

Brief Small Group Discussion What are some examples in office practice of how poor communication results in harm to a patient?

Feedback and large group discussion

Examples of Suboptimal Communication That Can Lead to Safety Risk: With the clinician: - Interrupting the patient and not hearing all the symptoms - Not asking about concerns with the treatment plan - Not assuring correct understanding of instructions - Not acknowledging uncertainty about diagnosis - Incomplete communication about danger signs

Examples of Suboptimal Communication That Can Lead to Safety Risk: § § § Not checking to see that all issues were addressed Not making it safe to admit lack of adherence to prior treatment plans Not using structured communication formats (missing new information on family history)

Examples of Suboptimal Communication That Can Lead to Safety Risk: With other office staff § Front desk didn’t get information to assess urgency of the need § Not checking at the front desk – do they understand the next steps, have barriers or concerns § Not checking to make sure they got all their questions answered

Overlap With Those Working on Patient-Centered Medical Home § Patient Safety brings added dimensions and focus on communication. § Moving beyond non-compliance (“Why don’t they do what I tell them to? ”) § Some similar issues – shared decision making, motivational interviewing, effective teaching § Some additional nuances - missed diagnosis, safety issues in other staff communications
- Slides: 18