Motivational Interviewing Basics for Coaching Cris Cannon D

Motivational Interviewing: Basics for Coaching Cris Cannon, D. Min. , LPC/MHSP, CCMHC, ACS

Learning Objectives Ø What Motivational Interviewing is and is not Ø The Philosophy and Spirit of Motivational Interviewing Ø The Role of Ambivalence Ø The Purpose: Change Talk, Commitment Language, and Behavior Change Ø An Example of Motivational Interviewing Ø MI: Just Another Theory? Ø Encouraging Motivation to Change: Am I Doing It Right? 2

Motivational Interviewing What it IS NOT: What it IS: Patient education Confrontation “Expert” based Telling Solving the patient’s problem § Developing a plan § “Wrestling” – correcting § the patient’s behavior § § § Relationship based Empathy Collaboration Evoking Focusing on ambivalence Majoring on “change talk” “Dancing” – with the patient’s fears about attempting change 3

Motivational Interviewing is NOT Based on the Stages of Change (Miller, Ten Things that Motivational Interviewing Is Not, 2009. ) v William Miller – “MI was never based on the TTM. ” v “They are, in essence, kissing cousins who never married. ” v Not important to explain the stages of change when delivering MI v Not necessary to assign people to a stage of change as part of MI v “In the second edition of Motivational Interviewing, we intentionally removed all reference to TTM in the front of the book, precisely because of the extent the two were being confused. ” 4

MI and the Stages of Change • Stages of Change – conceptual model of how and why changes occur • Motivational Interviewing - is a specific clinical method to enhance personal motivation for change The Stage of Change that a patient presents suggests the type of Motivational Interviewing technique that is utilized. 5

Philosophy of MI “People are generally better persuaded by the reasons which they themselves discovered than by those which have come in to the mind of others. ” - Blaise Pascal, French mathematician, physicist, and philosopher 6

MI Defined “Motivational Interviewing is a collaborative, person-centered form of guiding to elicit and strengthen motivation for change. ” (Miller and Rollnick, 2009, p. 137) “It is not a bag of tricks for getting people to do what they don’t want to do; rather, it is a fundamental way of being with and for people – a facilitative approach to communication that evokes change. ” (Miller and Rollnick, 2002) “MI is primarily concerned with helping clients to make a decision to change. It is intended to address the question of why change should occur now. ” (Moyers, 2014) 7

It’s All About Ambivalence noun 1. uncertainty or fluctuation, especially when caused by inability to make a choice or by a simultaneous desire to say or do two opposite or conflicting things. The possibility of change creates ambivalence! Life changes we know we need to make • The fear of failing. . . which creates. . . • The fear of trying • And leaves us exactly where we are • Ambivalence = “stuck” 8

Typical Health Care Response to Ambivalence Explain why the person should change - Insight Give benefits resulting from making the change Knowledge Tell the person how they could make the change - Skills Persuade the person to do it If you meet resistance, repeat the process Supposedly. . . Insight + Knowledge + Skills = Behavior Change This is NOT Motivational Interviewing 9

Ambivalence is the Heart of MI It is a normal aspect of human nature It is a natural phase in the process of change It is not denial It is not a lack of motivation, therefore. . . It is not helpful to conceive of patients as “unmotivated” “I want to but I don’t want to. ” Ambivalence is the dilemma of change 10

Let’s Experience Some Ambivalence! 11

On a Piece of Paper. . . 1. A behavior or habit you want to change 2. What are the positive things about this behavior or habit? 3. What are the “not so positive” things about this behavior or habit? 4. Please state a goal you want to work towards that supports your sense of meaning and purpose. How you want to leave your mark in this world. 5. How will this behavior or habit affect your ability to reach this goal? 12

You Have Just Performed Motivational Interviewing with Yourself. . . Are you aware of what you have just done? The major topic is not the behavior or habit you wanted to change. It is considering the effect of the behavior or habit on the larger issues of your life. Instead of trying to get you to change the behavior or habit, we were examining and addressing the issue of change itself. . . MI creates cognitive dissonance between where one is now and where one wants to be. We want to allow patients to experience the tipping point for change and then utilize information and momentum towards the implementation of change. 13

The Spirit of Motivational Interviewing (Rollnick, Miller, & Butler, 2008) Evocative vs. Educational – Drawing things out of the patient rather than putting them in • Patient is responsible for change. - “What would you gain if you lost weight? ” vs. getting our point across - “You really do need to change your eating habits. ” Honoring Autonomy vs. Authority – It’s not my job to make the patient change • Allow the freedom not to change. - “How ready are you to change? ” vs. push for commitment - “Unmanaged stress leads to many health problems and you don’t want to get sick. ” Collaborative vs. Confrontational – “dancing vs. wrestling” • Work in partnership - “How about we discuss some options together? ” vs. confrontation - “I urge you to take your medications regularly. ” 14

Four Key Principles of MI: Building Relationship with the Ambivalent Patient v Express empathy – Thinking about things as the patient does; perceiving the patient’s feelings. The coach’s accurate understanding of the client’s experience facilitates change. v Develop discrepancy – Motivation for change results when a patient perceives the discrepancy between where they are and where they want to be. v Roll with resistance – Don’t fight a patient’s resistance, use it to explore the patient’s views. v Support self-efficacy – Focus on the patient’s ability to make change and support that belief. 15

Core MI Strategies: OARS and Their Purpose Open-ended Questions: • “What concerns you the most about your weight? ” • “How have you tried to deal with stress in the past? ” Affirmations: • “I know it’s difficult to think about change, I’m really pleased that you are willing to talk about it. ” • “You have done a great job in keeping that food journal. ” Reflective Listening: • Restating to the client what he/she has shared with you. • “You know you need to make change, but you aren’t quite sure how and if you can maintain it. ” Summaries: • Reflective listening reflecting back on what the patient has told you. • “Let me stop and summarize what we’ve just talked about. . . ” 16

The Purpose: Eliciting Change Talk (Miller and Rose, 2009) Statements made by a patient indicating the possibility for change. Goals Regarding Change Talk: • Identify – know it when you hear it • Elicit – seek more • Strengthen – by encouragement • Limit “sustain talk” – keeping everything as it is 17

Categories of Change Talk Desire: “I want things to be different, to do things differently. ” Ability: “I can manage to make this change. ” Reason: “These are three reasons it would be beneficial for me to change. ” Need: “I need to do this; I know I should. ” Change talk leads to. . . 18

Commitment Language Commitment: “I will work toward this change. ” Activation: “I am ready to do this. ” Taking Steps: “These are the steps I will take. ” 19

Change Talk, Commitment Language, and Behavior Change Ø Change Talk ØCommitment Language ØBehavior Change 20

City of Westminster Patient: “Susan” Coach: “Susan, how can I help you today? Susan: “I don’t know; I am failing at exercise and I don’t know what to do, so I have stopped doing anything! I’m just not motivated at all anymore. I’m helpless!” Coach: “And when you feel negatively about something, it’s just so easy to give up. ” Susan: “Exactly! I just don’t even want to try to exercise anymore. I feel so badly when I don’t do it. If I’m a failure at something as easy as exercise, I feel like I’m a failure at everything!” Coach: “On the other hand, when you do exercise, I bet you feel pretty good about yourself. ” Susan: “Oh yeah; I feel like I’m in control of myself when I do exercise. It’s like I feel whole because I make every minute count from my day and I am trying to stay healthy, as well. Not wasting time. That sort of thing. ” 21

City of Westminster Patient: “Susan” Coach: “So it sounds like having control of your life is as important to you as exercise itself. ” Susan: “When I don’t exercise, I feel guilty that this is another area of my life where I am a failure and then I feel totally bad about myself as a person. ” Coach: “May I ask you a question about your motivation for exercise? ” Susan: “Sure. Ask away!” Coach: “On a one to ten scale, just how motivated are you to exercise right now? ” Susan: “”Hmm. . . let me think about that. (long pause) About a two. ” Coach: “Thanks for your honesty! Not easy to admit when you don’t feel the best about yourself. May I ask: what would it take to move yourself from two to an eight? ” Susan: “Hmmm. . . (long pause). I guess if I could figure out how to get back into exercise. I don’t really know. I just don’t want to feel like a failure. It might be easier just to give up altogether!” (nervous laughter) 22

City of Westminster Patient: “Susan” Coach: “Tell me about a time when you were successful with exercise. ” Susan: “I have a stretching DVD that I really like. My husband I were doing it every morning until I hurt my back and had to go to the chiropractor. I haven’t tried stretching since and he won’t get up with me to do it anyway now. ” Coach: “May I summarize? You feel better about yourself as a person overall when you exercise, and you stopped because of an injury, but if you can find a positive way to get back into exercise, your motivation goes from a two to an eight. ” Susan: (pause) “That pretty much sums up how I’m feeling. So how do I go from the two to the eight without feeling like a loser? ” Coach: “Let’s talk about stretching, because of your past success with it. Are you healed and cleared to exercise again? ” Susan: “My back is fine and the doctor told me I was free to do anything I want. I just can’t get stretching back into my morning routine again. ” 23

City of Westminster Patient: “Susan” Coach: “Would you tell me about your morning routine? ” Susan: ” I wake up around five, but lay in bed until about six, have my coffee and quiet time and start my day. ” Coach: “So when you were stretching, where did that fit into your morning routine? ” Susan: “I made myself get up at 5: 15 am. I just don’t know if I’m willing to do that again. ” Coach: “I understand! Sleeping late really feels good! At the same time, you’re willing to move from a two to an eight if you can find a way to do so. ” Susan: “Yes, but I don’t want to give up my morning quiet time, which I did sometimes when I exercised. I’ve had my morning quiet time for many years, ever since I was in high school. ” 24

City of Westminster Patient: “Susan” Coach: “Your quiet time is very important to you. On the other hand, must it be a choice between exercise and quiet time? ” Susan: (long silence) “I wonder if I could make myself get up and exercise and then have my quiet time? But I don’t know. I’ve gotten used to sleeping in and it feels really good. . . ” Coach: “What time would you have to get up for exercise and quiet time? ” Susan: “About 5: 15, I guess. (silence) Coach: “So I guess it’s a choice between feeling better about yourself from exercising vs. sleeping longer and not feeling as positive about yourself. ” Susan: “The one thing I can say is that I am tired of feeling crappy because I can’t make myself exercise! I feel like such a loser! I don’t know which is worse; feeling bad from no exercise or feeling like I can’t make myself do what I need to do. ” 25

City of Westminster Patient: “Susan” Coach: “Susan, how do you want to feel about yourself a year from now? ” Susan: “I want to feel. . . like I have control over myself and my health is better from exercising. I want to stop feeling like a wimp!” Coach: “Great! You know your ultimate goal! If the first step is getting up at 5: 15, brainstorm some other steps that will move you towards self-control. ” Susan: “Hmm. . . (long pause). I guess I could get the Keurig ready the night before to go right to my coffee and quiet time. ” Coach: “An excellent idea, Susan! What are other possibilities? ” Susan: “I need to place my shoes and workout clothes closer to the bed to make it easier to get myself up and going. Having the clothes close removes an excuse for me. ” 26

City of Westminster Patient: “Susan” Coach: “So let’s review: the night before, you can get your coffee ready, put your clothes and shoes by the bed, and get up at 5: 15. ” Susan: “That’s the size of it. I’m not sure I’m ready to start this five days a week. I always take weekends off. ” Coach: “Let’s keep it simple, then. How many days of exercise would it take to assist you in reaching your goal of feeling better about yourself? ” Susan: “Good point. If I want to feel better, I have to start somewhere. (pause) Okay; three days a week. Monday, Wednesday, and Friday!” Coach: “Susan, you’ve done it! Your exercise goal supports your desire for selfcontrol! You know what you want to do, how to get ready to do it, and why you want to exercise. Are you ready to set the start date? ” Susan: “Monday morning! I’m starting next Monday! And I just realized that my quiet time is how I reward myself for getting out of bed and exercising!” 27

Two Dynamics with “Susan” 1. Engaged Susan in “change talk” that included feelings about her life, not just about exercise. 2. Moved to Preparation and Action only after Susan clearly was in favor of pursuing change. 28

29

NOTE: MI is NOT for Every Patient! “MI was developed specifically for the purpose of helping people resolve ambivalence and strengthen motivation for change. Not everyone needs the evoking process of MI. When motivation for change is already strong, move ahead with planning and implementation. ” (Miller & Rollnick, 2012, p. 35). 30

How Patients Feel About Change. . . 31

Our Motivational Interviewing Message. . . 32

Motivational Interviewing: Just Another Theory? Ewing, S. W. , Yezhuvah, U. , Houck, J. , Filbey, F. (2014). Brain-based origins of change language: A beginning. Addictive Behaviors, 39, 1904 -1910. “Client change talk (CT), a critical component of MI, has been associated with differential brain activation. The goal of this study was to begin to deconstruct how and why CT may affect the brain. ” While placed in a “functional MRI”, subjects listened to recorded messages for Change Talk and Sustain Talk (ST). One group selfgenerated their statements during an MI session; the second group listened to a pre-established list of messages. Findings: Both types of client language, CT and ST, elicited greater blood oxygenation level dependent (BOLD) responses in the self-generated group vs. the pre-established group. 33
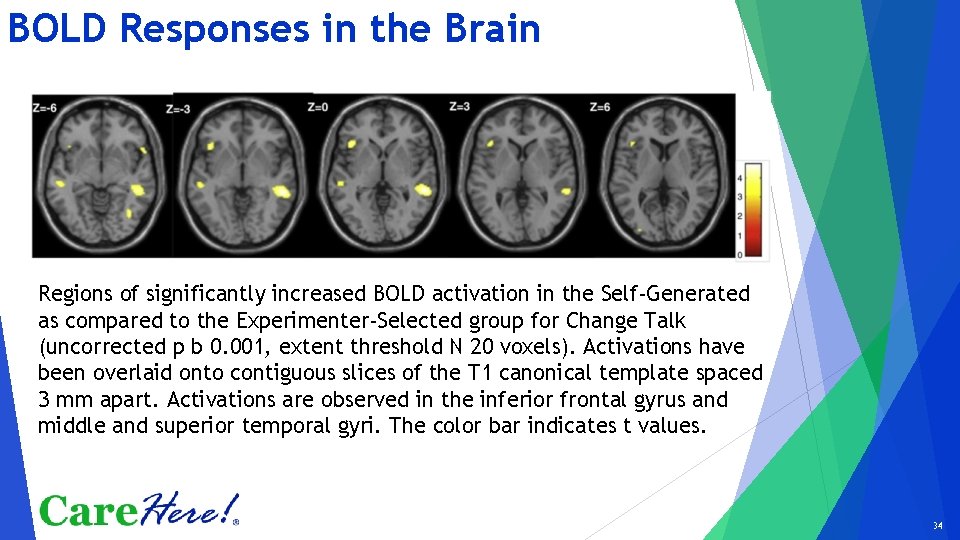
BOLD Responses in the Brain Regions of significantly increased BOLD activation in the Self-Generated as compared to the Experimenter-Selected group for Change Talk (uncorrected p b 0. 001, extent threshold N 20 voxels). Activations have been overlaid onto contiguous slices of the T 1 canonical template spaced 3 mm apart. Activations are observed in the inferior frontal gyrus and middle and superior temporal gyri. The color bar indicates t values. 34

“These findings indicate that the nature of client language matters. ” This suggests “. . . that it is not simply Change Talk, but spontaneous, personally-relevant Change Talk made in the context of a therapeutic exchange that is critical in client change language. ” 35

How Will You Know When You’re Doing MI Right? Patient is doing most of the talking Patient is using a great deal of “change talk” Resistance Patient is minimized is exploring avenues toward change 36

Encouraging Motivation to Change: Am I Doing this Right? Center for Evidence-Based Practices, Case Western Reserve University www. centerforebp. case. edu 1. Do I listen more than talk? 2. Do I keep myself sensitive and open to this person’s issues, whatever they may be? 2. Or am I talking more than I listen? Or am I talking about what I think the problem is? Do I invite this person to talk about and explore his/her own ideas for change? Or am I jumping to conclusions an possible solutions? 37

Encouraging Motivation to Change: Am I Doing this Right? 4. Do I encourage this person to talk about his/her reasons for not changing? Or am I forcing him/her to talk only about change? 5. Do I ask permission to give my feedback? Or am I presuming that my ideas are what he/she really wants to hear? 6. Do I reassure this person that ambivalence to change is normal? Or am I telling him/her to take action and push ahead for a solution? 38

Encouraging Motivation to Change: Am I Doing this Right? 7. Do I help this person identify successes and challenges from his/her past and relate them to present change efforts? Or am I encouraging him/her to ignore or get stuck on old stories? 8. Do I seek to understand this person? Or am I spending a lot of time trying to convince him/her to understand me and my ideas? 9. Do I summarize for this person what I am hearing? Or am I just summarizing what I think? 39

Encouraging Motivation to Change: Am I Doing this Right? 10. Do I value this person’s opinion more than my own? 11. Or am I giving more value to my viewpoint? Do I remind myself that this person is capable of making his/her own choices? Or am I assuming that he/she is not capable of making good choices? 40

References Arkowitz, H, Westra, HA, Miller, WR, Rollnick, S (Eds. ) (2008). Motivational interviewing in the treatment of psychological problems. New York: Guilford Press. Dunn, C & Stephens, K. (2010). Motivational Interviewing. Retrieved from: http: //uwaims. org/webinars/slides/AIMS_MHIP_Motivational. Interviewing. Slides_050510. pdf Di. Clemente, C. C. , Prochaska, J. O. , Fairhurst, S. K. , Velicer, W. F. , Velasquez, M. M. and Rossi, J. S. (1991) The process of smoking cessation: an analysis of precontemplation, contemplation and preparation stages of change. Journal of Consulting and Clinical Psychology, 59, 295– 304. Miller, WR & Rollnick, S (1991). Motivational interviewing: Preparing people to change addictive behavior. New York: Guilford Press. Miller, WR & Rollnick, S (2002). Motivational interviewing: Preparing people for change (2 nd ed. ). New York: Guilford Press. Miller, WR. (2009). Ten things that motivational interviewing is not. Behavioural and Cognitive Psychotherapy, 2009, 37, 129– 140. Miller, W. R. , & Rollnick, S. (2012). Motivational interviewing: Helping people change. Guilford Press. Moyers, T. (2014). The relationship in motivational interviewing. Psychotherapy, 2014, 51, 358 -363. Rollnick, S, Miller, WR & Butler, CC (2007). Motivational Interviewing in Health Care. New York: Guilford Press. Rollnick, S, Miller, WR & Butler, CC (2008). Motivational interviewing in health care. New York: Guilford Press. Rosengren, D. B. (2009). Building Motivational Interviewing Skills: A practitioner workbook. New York: Guilford Press. 41
- Slides: 41