MotherBaby Project 201011 Year 3 Group 13 to

Mother-Baby Project 2010/11 (Year 3) Group 13 to 15 THEME 5: MINOR AILMENTS IN NEWBORN AND INFANCY

DEFINITIONS � Newborn: an infant in the first 28 days of life (from birth up to 4 weeks after birth, less than a month old) � Infancy: children between the ages of 1 month and 12 months Source: Merriam-Webster online dictionary http: //www. merriam-webster. com/

PRESENTATION OUTLINE I. Gastrointestinal system � Neonatal jaundice � Vomiting and regurgitation � Diarrrhoea � Gastroenteritis � Constipation II. Respiratory system � Flu � Pharyngitis � Acute otitis media (AOM)

PRESENTATION OUTLINE III. Urinary system � Urinary tract infection (UTI) IV. Integumentary system � Atopic dermatitis/ Infantile eczema � Contact dermatitis � Seborrhoeic dermatitis � Diaper dermatitis/ Nappy rash � Heat rash / Prickly heat � Others

I. GASTROINTESTINAL (GI) SYSTEM
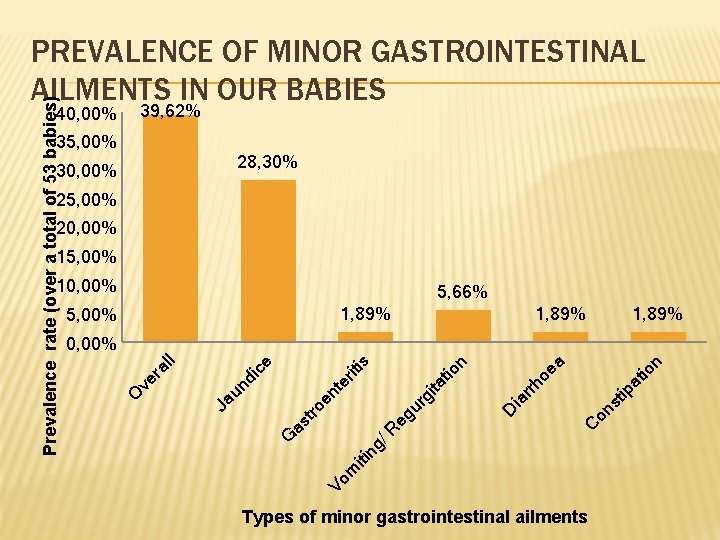
Prevalence rate (over a total of 53 babies) PREVALENCE OF MINOR GASTROINTESTINAL AILMENTS IN OUR BABIES 39, 62% 40, 00% 35, 00% 28, 30% 30, 00% 25, 00% 20, 00% 15, 00% 10, 00% 5, 66% 1, 89% 5, 00% 1, 89% n io on st ip at C oe a rrh Vo m iti ng /R ia eg u ro en as t G D te r iti rg ita tio n s di ce Ja un O ve r al l 0, 00% Types of minor gastrointestinal ailments
1. NEONATAL JAUNDICE

1. NEONATAL JAUNDICE - OVERVIEW Yellowish discoloration of skins and sclera in the newborn due to accumulation of unconjugated bilirubin. � Among the most common condition requiring medical attention in newborns. � Mostly reflects a normal transitional phenomenon. � However, excessive rise of unconjugated bilirubin would result in neurotoxicity �
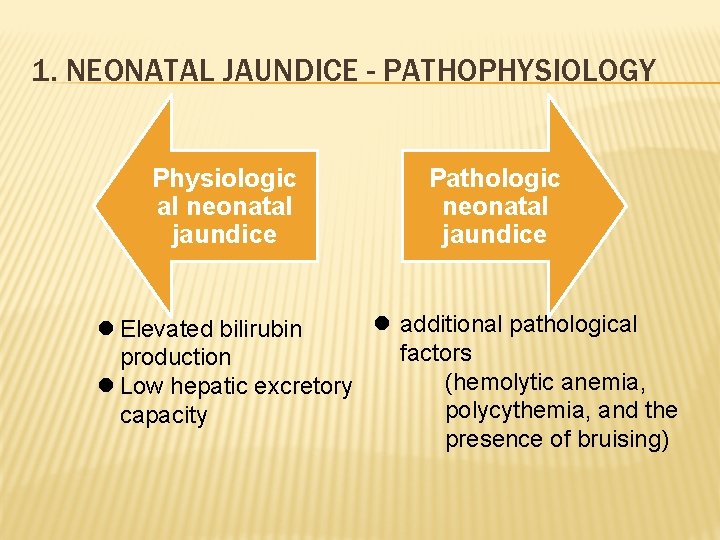
1. NEONATAL JAUNDICE - PATHOPHYSIOLOGY Physiologic al neonatal jaundice Pathologic neonatal jaundice l additional pathological l Elevated bilirubin factors production (hemolytic anemia, l Low hepatic excretory polycythemia, and the capacity presence of bruising)

1. NEONATAL JAUNDICE - COMPLICATIONS In severe cases, � neonatal deaths, or � lifelong neurological sequelae in surviving infants (kernicterus). **Kernicterus: Damage to brain centers of infants due to increased levels of unconjugated bilirubin.

1. NEONATAL JAUNDICE – RISK FACTORS � Race � More common in infants of East Asian, American Indian, and Greek descent born in Greece. � Black infants are affected less often than white infants. � Gender � More in male than in female (not related to bilirubin production rate which is similar in both genders) � Gestational � Risk Age inversely proportional to the gestational age

1. NEONATAL JAUNDICE AMONG OUR BABIES � Race � All of them are Chinese so we cannot compare its effect � Gender � We cannot have meaningful analysis of the data ∵a lot of our fellow classmates have input the gender of the mothers instead of that of the babies � Gestation age

1. NEONATAL JAUNDICE AMONG OUR BABIES � Does gestational age cause neonatal jaundice? Jaundice No Jaundice 6, 67% 13, 51% 20, 00% 10, 81% Pre-term Full-term Post-term 73, 33% 75, 68%

1. NEONATAL JAUNDICE AMONG OUR BABIES � Is the difference statistically significant? Observed values Expected values Pre-term Full-term Post-term TOTALS Jaundice 1 11 3 15 No Jaundice 4 28 5 TOTALS 5 39 8 � � Pre-term Full-term Post-term TOTALS Jaundice 1. 4423 11. 25 2. 3077 15 37 No Jaundice 3. 5577 27. 75 5. 6923 37 52 TOTALS 5 39 8 52 Chi-square = 0. 4903 Degrees of freedom = 5 p-value = 0. 99 The result is NOT statistically significant.

1. NEONATAL JAUNDICE - TREATMENT � Phototherapy � Exchange transfusion � Other strategies � Phenobarbital � Intravenous immunoglobulin (IVIG)

2. VOMITING AND REGURGITATION

2. VOMITING AND REGURGITATION � Vomiting ≠ Regurgitation!!!! Vomiting Coordinated, sequential series of events, leading to forceful oral emptying of gastric contents Usually preceded by nausea Regurgitation Non-forceful return of contents from stomach into esophagus No nausea

2. VOMITING – COMMON CAUSES � Feeding problems e. g. force-feeding, overfeeding � Regurgitation (Infantile GERD) � Allergic reactions to formula � Gastroenteritis

2. VOMITING – OTHER DDX � Need to exclude � Congenital � e. g. obstructive lesions intestinal atresia, midgut malrotation � Pyloric stenosis � Metabolic disorders � e. g. galactosemia � Infections � viral, bacterial � e. g. pharyngitis, otitis media, UTI � CNS causes – increased intracanial pressure

2. VOMITING - TREATMENT � Monitor for dehydration � If exclusive breastfeeding continue; oral rehydration solution NOT NEEDED � If formula feeding oral rehydration solution � Specific treatments if underlying causes present

2. REGURGITATION - OVERVIEW � Infantile gastro-esophageal reflux (GERD), spitting up � Non-forceful return of contents from stomach into esophagus � Functional reflux is normal, common in infants � 40% experienced reflux during first 3 mons of life, without major clinical significance � 0. 3% significant reflux, with potential complications

2. REGURGITATION – COMMON CAUSES � Loss of normal gastro-esophageal pressure gradient due to: � Functional immaturity of lower esophageal sphincter � Diminished esophageal clearance � Short length of intra-abdominal esophagus � Increased abdominal pressure by crying

2. REGURGITATION – TREATMENT AND PREVENTION � Add inert thickening agents to feeds � e. g. Nestargel, Carobel � Smaller volume feeds � 30° head-up prone position after feeding � Medications in severe reflux � Domperidone � Omeprazole
3. DIARRHEA IN NEWBORN

3. DIARRHEA IN NEWBORN - OVERVIEW � Diarrhea is defined by increase frequency or change in consistency � Normally: � frequency : newborn passes stool about 8 -10 times per day � consistency: small, watery stools mixed with yellow, seedy pieces

3. DIARRHEA IN NEWBORN – COMMON CAUSES � Intestinal infections � Food intolerance or sensitivity � Food allergy e. g. milk � Normal intestinal variations

4. CONSTIPATION

4. CONSTIPATION – COMMON CAUSES � Change in Diet i. e. from breast milk to formula milk � Hirschsprung’s Disease � Hypothyrodism

4. CONSTIPATION - MANAGEMENT � Change the feeding schedule � For babies that have formula try, adding an extra bottle of water each day � Mix a teaspoon of the flax oil with formula, or insert a suppository when the baby shows sign of constipating.
5. GASTROENTERITIS

5. GASTROENTERITIS - OVERVIEW � Can cause both vomiting and diarrhoea � common

5. GASTROENTERITIS - CAUSES � The commonest cause: Rotavirus infection � 60% of cases in children < 2 yr � esp during winter � Other viral causes: � Adenovirus � Coronovirus � Bacterial causes less common in developed countries; common pathogens include: � Campylobacter � Shigella � Salmonellae � Vibrio cholera � E. Coli jejuni
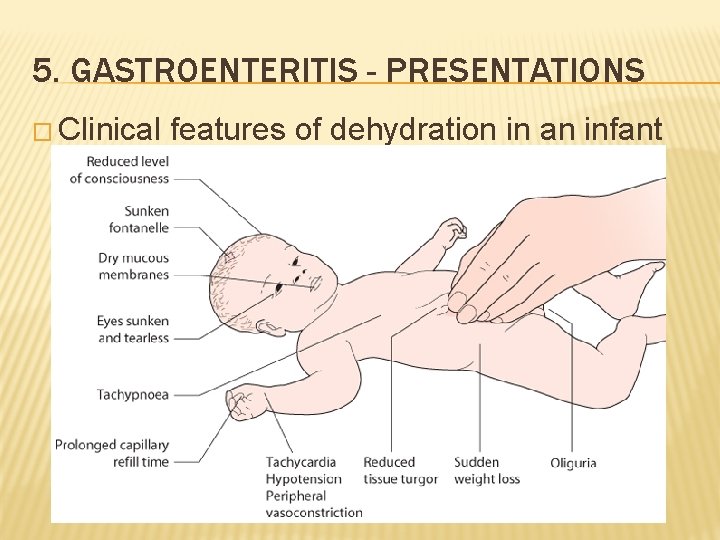
5. GASTROENTERITIS - PRESENTATIONS � Clinical features of dehydration in an infant

5. GASTROENTERITIS - MANAGEMENT � For rotavirus � effective � In vaccine available general � Correction of dehydration is THE MOST IMPORTANT!

5. GASTROENTERITIS - MANAGEMENT � For mild dehydration (<5% body weight loss) �A short-term substitution of normal feeds with maintenance type of glucose-electrolyte solution � to enhance sodium and water absorption � given till vomiting and profuse diarrhoea subside � usually �a lasts <24 hrs normal diet can then be given

5. GASTROENTERITIS - MANAGEMENT � For moderate dehydration (5 -10% body weight loss) � Oral rehydration � aiming to give 100 m. L/kg in 6 hours � can be given orally or by nasogastric tube � If no improvement, IV rehydration

5. GASTROENTERITIS - MANAGEMENT � Severe dehydration (>10% body weight loss) � IV rehydration is ALWAYS indicated � If in shock: immediate resuscitation � Fluid balance monitored closely renal failure may rarely complicate severe dehydration � Failure to recognise continuing oliguria overhydration and pulmonary edema � Acute

II. RESPIRATORY SYSTEM
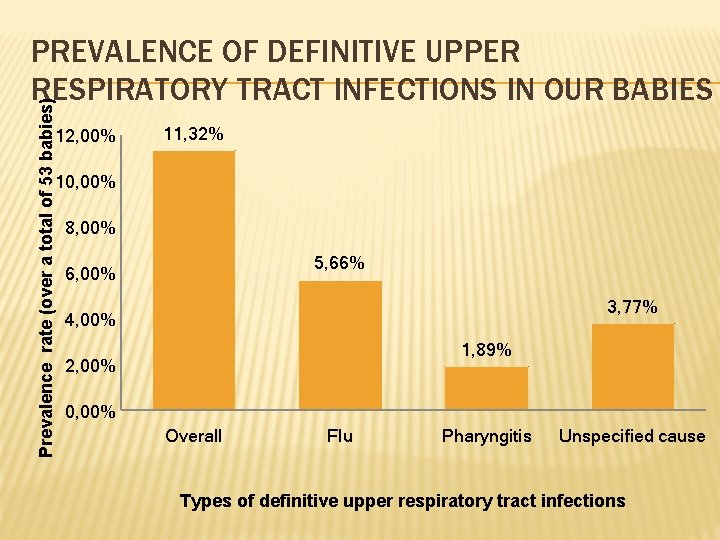
Prevalence rate (over a total of 53 babies) PREVALENCE OF DEFINITIVE UPPER RESPIRATORY TRACT INFECTIONS IN OUR BABIES 12, 00% 11, 32% 10, 00% 8, 00% 5, 66% 6, 00% 3, 77% 4, 00% 1, 89% 2, 00% 0, 00% Overall Flu Pharyngitis Unspecified cause Types of definitive upper respiratory tract infections
1. FLU/ 2. PHARYNGITIS

1. FLU – CLINICAL PRESENTATION � Dry cough � Nasal discharge � Fever

1. FLU – AETIOLOGY � Influenza virus � Orthomyxoviridae � RNA virus � Enveloped � Usually due to influenza A or B

1. FLU – MANAGEMENT � Symptomatic treatment � Analgesics/anti-pyretic, e. g. paracetamol � Avoid aspirin if suspecting Reye’s Syndrome!!! � Anti-viral � e. g. drugs oseltamivir, zanamivir

1. FLU - PREVENTION � Contact precaution e. g. face mask, hand hygiene � Annual vaccination

2. PHARYNGITIS – CLINICAL PRESENTATIONS � Sore throat � Inflamed tonsils � +/- fever, watery eyes, running nose, enlarged cervical lymph nodes

2. PHARYNGITIS – AETIOLOGY � Mostly viral � Sometimes GAS

2. PHARYNGITIS – MANAGEMENT � Symptomatic if viral � Penicillin if bacterial � Throat swab for culture if uncertain

2. PHARYNGITIS - PREVENTION � Contact precaution � Avoid overcrowding
1. FLU/ 2. PHARYNGITIS AMONG OUR BABIES � Does the choice of feeding affect the chance of having URTI?
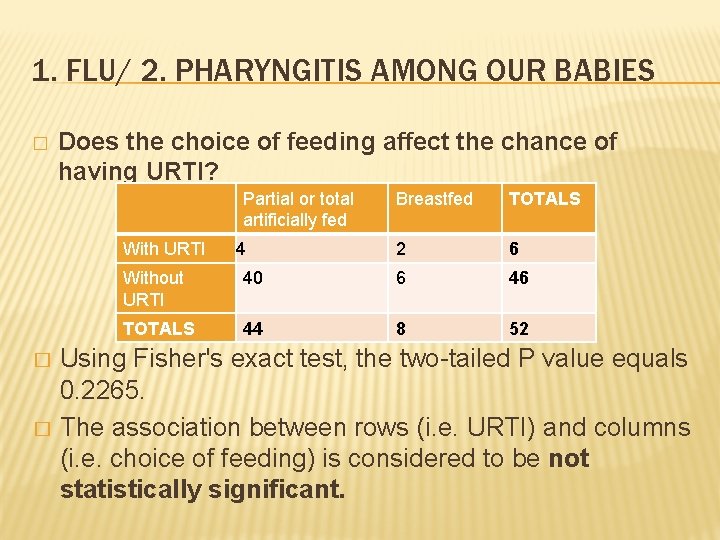
1. FLU/ 2. PHARYNGITIS AMONG OUR BABIES � Does the choice of feeding affect the chance of having URTI? Partial or total artificially fed With URTI � � 4 Breastfed TOTALS 2 6 Without URTI 40 6 46 TOTALS 44 8 52 Using Fisher's exact test, the two-tailed P value equals 0. 2265. The association between rows (i. e. URTI) and columns (i. e. choice of feeding) is considered to be not statistically significant.

3. AOM - OVERVIEW � Inflammation of the middle ear with an acute onset but no reference to etiology or pathogensis � Might develop into otitis media with effusion or chronic suppurative otitis media � High prevalence of recurrence � More than one third of children experience 6 or more episodes of AOM by age 7 years

3. AOM – CLINICAL PRESENTATIONS � Otalgia � Irritability � Fever � Lethargy � Concurrent or recent URI symptoms (eg, cough, rhinorrhea, sinus congestion) � Anorexia, nausea, vomiting, and diarrhea
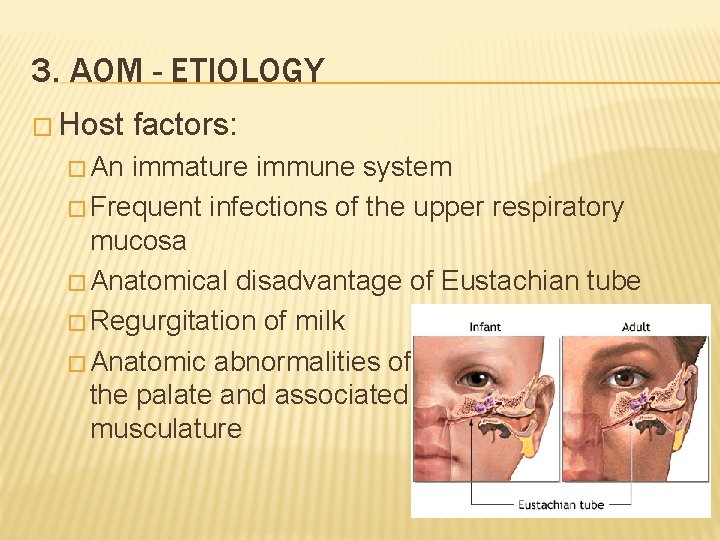
3. AOM - ETIOLOGY � Host � An factors: immature immune system � Frequent infections of the upper respiratory mucosa � Anatomical disadvantage of Eustachian tube � Regurgitation of milk � Anatomic abnormalities of the palate and associated musculature

3. AOM - ETIOLOGY � Infectious � The factors: most common bacterial pathogen in AOM is Streptococcus pneumoniae, followed by nontypeable Haemophilus influenzae and Moraxella catarrhalis. � These 3 organisms are responsible for more than 95% of all AOM cases with a bacterial etiology.

3. AOM - TREATMENT � Medical � Analgesics and antipyretics e. g. paracetamol, ibuprofen � Antibiotics if � The child is under 2 years old � The infection is severe � The infection does not settle within 2 -3 days � Complications develop e. g. temporary hearing loss, perforated eardrum, mastoiditis

3. AOM - TREATMENT � Surgical � Tympanocentesis if � Unsatisfactory response to antimicrobial therapy � OM associated with a confirmed or potential suppurative complication � OM in a newborn, sick neonate, or patient who is immunologically deficient, any of whom may harbor an unusual organism � Myringotomy insertion if � Recurrent with tympanostomy tube (TT) AOM/ OME � Chronic OME � Eustachian tube dysfunction

III. URINARY SYSTEM

Prevalence rate (over a total of 53 babies) PREVALENCE OF DEFINITIVE URINARY TRACT INFECTION IN OUR BABIES 2, 00% 1, 89% 1, 80% 1, 60% 1, 40% 1, 20% 1, 00% 0, 80% 0, 60% 0, 40% 0, 20% 0, 00% Urinary tract infection
1. URINARY TRACT INFECTION (UTI)

1. UTI - PRESENTATION � Foul odor urine � Suprapubic tenderness � Can present without fever � Voiding symptoms; dysuria, urgency, frequency, hesitancy, incontinence

1. UTI - PATHOPHYSIOLOGY � Ascending � Normal infection! defense mechanism: � Flushing effect

1. UTI – RISK FACTORS � Under broad-spectrum antibiotics � Uncomplete/ infrequent bladder emptying � Anatomical/ neurogenic voiding abnormalities � Catheterization � Sepsis

1. UTI - MANAGEMENT � Infants < 8 weeks, initially with fever � Hospitalized � Parenteral antibiotic therapy � Parenteral antibiotics may be used with daily follow-up until the patient is afebrile for 24 hours. � Complete 10 -14 days of therapy with an oral antibiotic active against the infecting bacteria.

1. UTI - MANAGEMENT � Antibiotic agents for parenteral treatment Drug Comment Ceftriaxone *Do not use in infants <6 wk of age; (∵parenteral antibiotic with long half-life; may displace bilirubin from albumin) Cefotaxime *Safe to use in infants <6 wk of age Ampicillin Used with gentamicin in neonates <2 wk of age; for enterococci and patients allergic to cephalosporins Gentamicin Monitor blood levels and kidney function if therapy extends >48 h

1. UTI - MANAGEMENT � For Infants and children aged 2 months to 2 years, initially with fever � Parenteral antibiotics OR � Oral antibiotics AND � Symptomatic relief if necessary; fluids and NSAIDs

1. UTI - PREVENTION � Antibiotic prophylaxis with low-dose daily therapy to prevent recurrent infections in children with vesicoureteral reflux (VUR) � In patients with pyelonephritis, reinfection is common, with a high incidence in the first 6 months after the initial infection. Therefore, 612 months of suppressive treatment is recommended.

1. UTI - COMPLICATIONS � Allergic reaction to antibiotic therapy. � Pyelonephritis � lobar inflammation of the kidney or renal abscess. � scar formation. � Long-term complications of pyelonephritis are : � Hypertension � Impaired renal function � End-stage renal disease (ESRD)

IV. INTEGUMENTARY SYSTEM
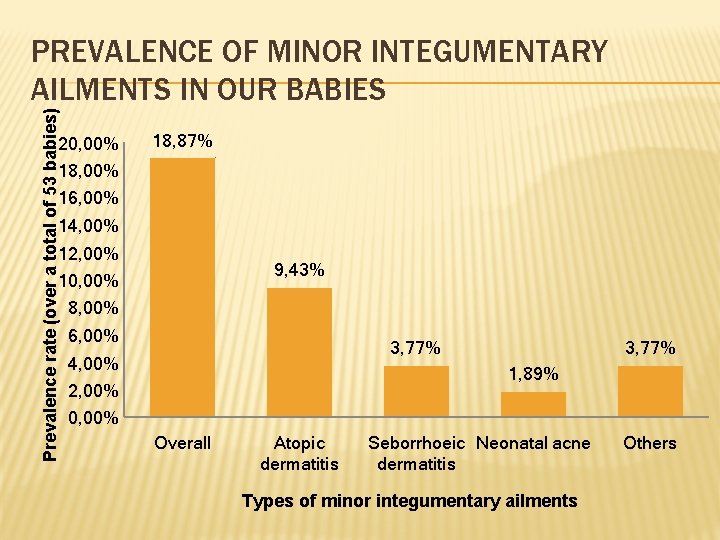
Prevalence rate (over a total of 53 babies) PREVALENCE OF MINOR INTEGUMENTARY AILMENTS IN OUR BABIES 20, 00% 18, 00% 16, 00% 18, 87% 14, 00% 12, 00% 10, 00% 8, 00% 9, 43% 6, 00% 3, 77% 4, 00% 2, 00% 0, 00% 3, 77% 1, 89% Overall Atopic dermatitis Seborrhoeic Neonatal acne dermatitis Types of minor integumentary ailments Others
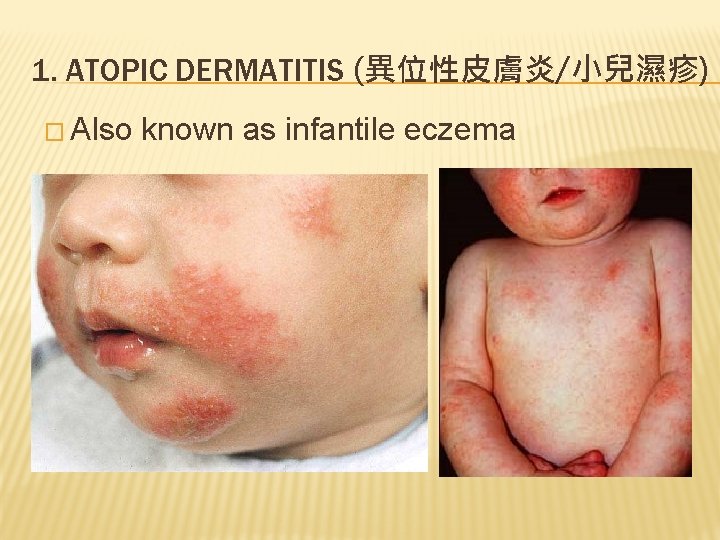
1. ATOPIC DERMATITIS (異位性皮膚炎/小兒濕疹) � Also known as infantile eczema

1. ATOPIC DERMATITIS – CLINICAL FEATURES � Red, dry skin, +/- small blisters and scabs � Extremely itchy! � Usually on cheeks, elbows, knees and trunk � First appears at 2 to 3 months old, and condition will wax and wane � Fades away at adolesence; some may persist into adulthood

1. ATOPIC DERMATITIS - CAUSES � Genetic predisposition � Other family members may suffer from allergic diseases like rhinitis and asthma, or are allergic to certain substances like detergents, pollen, dust or food

1. ATOPIC DERMATITIS - TREATMENT � Steroids or antibiotic cream

1. ATOPIC DERMATITIS – PREVENTION AND CARE � Skin care � Bathing � Moisturizer � Baby’s nails � Avoid exposure to cold wind and strong sunlight � Wipe baby’s sweat � Cotton clothing; gentle laundry detergent � Household environment � Diet (breastfeeding)
1. ATOPIC DERMATITIS AMONG OUR BABIES � Does maternal smoking affect the chance of having atopic dermatitis in the offspring?

1. ATOPIC DERMATITIS AMONG OUR BABIES � � � Does maternal smoking affect the chance of having atopic dermatitis in the offspring? Maternal smoking Maternal nonsmoking TOTALS With atopic dermatitis 0 5 5 Without atopic dermatitis 2 45 47 TOTALS 7 45 52 Using Fisher’s exact test, the two-tailed P value equals 1. 0000. The association between rows (groups) and columns (outcomes) is considered to be not statistically significant.
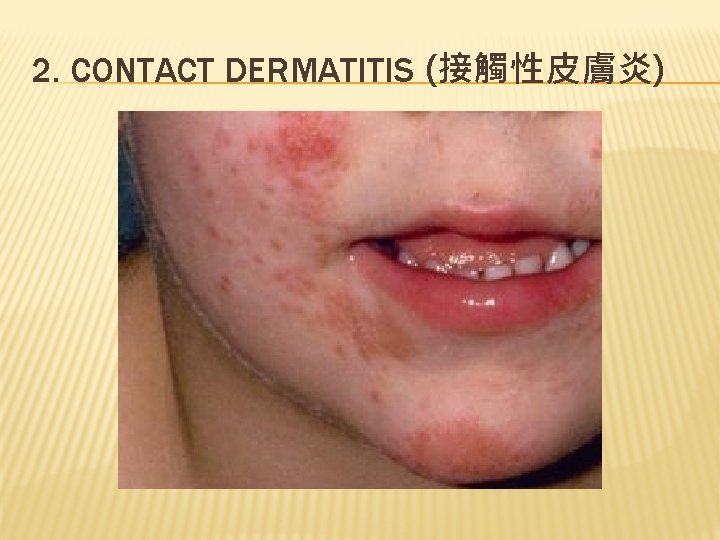
2. CONTACT DERMATITIS (接觸性皮膚炎)

2. CONTACT DERMATITIS – TYPES � Irritant � Allergic

2. CONTACT DERMATITIS – CLINICAL FEATURES � Red and itchy skin � +/-small blisters � In sites of contact with irritants/allergens

2. CONTACT DERMATITIS - CAUSES � Inflammatory reactions due to repeated contact with irritants, e. g. baby’s saliva, detergents, foods or medicines � Allergic responses after contact with allergens, e. g. certain metals like silver, dye

2. CONTACT DERMATITIS - TREATMENT � mid-potency topical corticosteroids (e. g. triamcinolone 0. 1% ointment or betamethasone valerate cream 0. 1%). � Skin allergy test to identify allergen(s)

2. CONTACT DERMATITIS – PREVENTION � Avoid contact with irritants and allergens
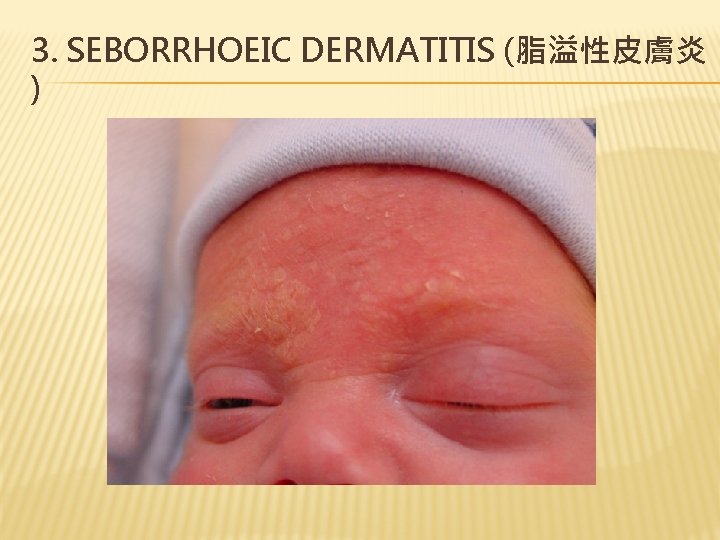
3. SEBORRHOEIC DERMATITIS (脂溢性皮膚炎 )

3. SEBORRHOEIC DERMATITIS – CLINICAL FEATURES � Slightly red skin with lumps of small oily flakes � Or yellowish, thick scales adhering to form a layer of scab � Mostly in areas of numerous sebaceous glands, e. g. head, forehead, cheeks, eyebrows, ears, armpits, abdomen and folds between thighs In scalp, it is known as ‘cradle cap’

3. SEBORRHOEIC DERMATITIS – CAUSE � Unclear

3. SEBORRHOEIC DERMATITIS – TREATMENT � Baby shampoo + 1% hydrocortisone cream � For thick lesions on scalp, 2% salicylic acid in olive oil or a corticosteroid gel

3. SEBORRHOEIC DERMATITIS – CARE � Clean with water � use of soap not advisable � Apply moisturizing cream after cleaning
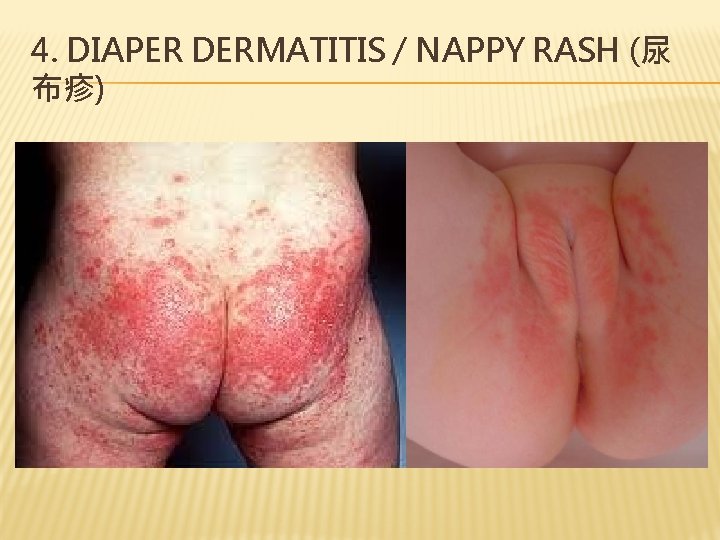
4. DIAPER DERMATITIS / NAPPY RASH (尿 布疹)

4. DIAPER DERMATITIS / NAPPY RASH – CLINICAL FEATURES � Red macules small, raised reddish rash � On areas covered with diaper

4. DIAPER DERMATITIS / NAPPY RASH – CAUSES � Wet skin ↑ penetration of irritant substances � Lipases and proteases in faeces mix with urine on non-intact skin, causing an alkaline surface p. H � Bile salts in the stools enhance the activity of fecal enzymes

4. DIAPER DERMATITIS / NAPPY RASH – PREVENTION AND CARE � Breastfeeding (? ) � Change diaper frequently; allow baby’s skin to air dry fully before putting on a clean diaper � Avoid using diaper wipes; use lukewarm water and with soap if needed, e. g. when soiled with feces � Apply a thin layer of moisturizer � Apply barrier cream like zinc oxide cream on red raw skin � Do not use baby powder
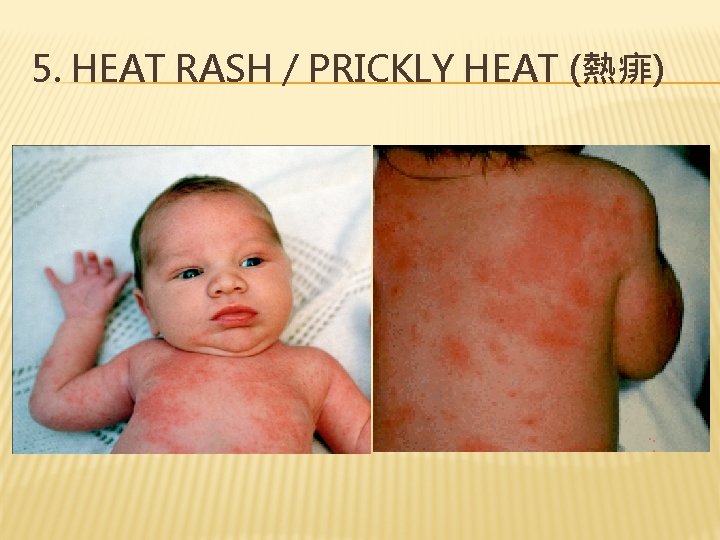
5. HEAT RASH / PRICKLY HEAT (熱痱)

5. HEAT RASH / PRICKLY HEAT – CLINICAL FEATURES � Small red papules � Mostly on the baby’s neck, back and chest � Usually occurs in hot weather / if baby is wrapped by excessive clothing in cool weather

5. HEAT RASH / PRICKLY HEAT – CAUSE � Irritation of skin due to sweat

5. HEAT RASH / PRICKLY HEAT – PREVENTION AND CARE � Appropriate clothing � Keep skin cool and dry to reduce sweating � Clean baby’s skin with cool water
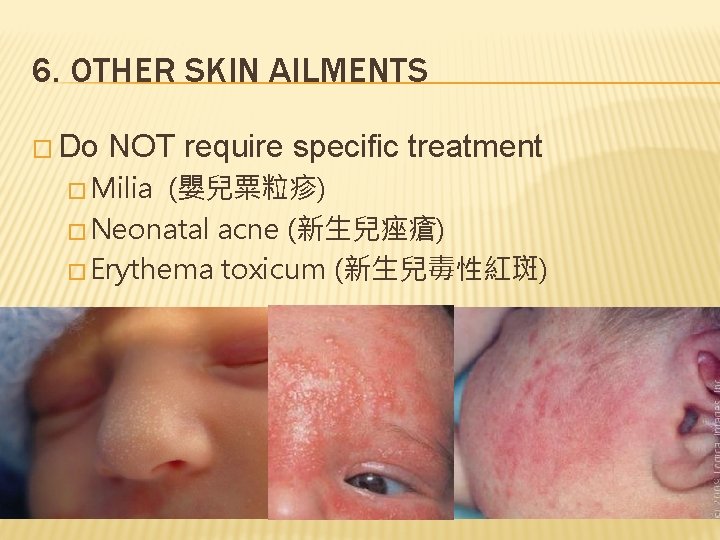
6. OTHER SKIN AILMENTS � Do NOT require specific treatment � Milia (嬰兒粟粒疹) � Neonatal acne (新生兒痤瘡) � Erythema toxicum (新生兒毒性紅斑)

6. OTHER SKIN AILMENTS - MANAGEMENT �Do � The NOT worry!!! above 3 conditions usually resolve spontaneously. � Avoid squeezing � No specific treatment needed

REFERENCES � GI system � � � Nelson Essentials of Pediatrics Illustrated Textbook of Paediatrics MD Consult http: //www. mdconsult. com/php/2201513783/homepage Ask. Dr. Sears. com http: //www. askdrsears. com/html/11/T 081500. asp Respiratory system � � Lars A Hanson MD. Breastfeeding Provides Passive and Likely Long-Lasting Active Immunity. Annals of Allergy, Asthma & Immunology. Volume 81, Issue 6, December 1998, Pages 523 -534, 537. Emedicine http: //emedicine. medscape. com/article/994656 overview Patient UK http: //www. patient. co. uk/health/Ear-Infection-(Otitis -Media). htm Primary Children's Medical Center 2010 https: //kr. ihc. com/ext/Dcmnt? ncid=520407540

REFERENCES (CONT’D) � Urinary � � system Urinary Tract Infection- Author: Donna J Fisher, MD, Assistant Professor of Pediatrics, Tufts University School of Medicine; Consulting Staff, Division of Pediatric Infectious Diseases, Children's Hospital, Baystate Medical Center http: //emedicine. medscape. com/article/969643 -overview Emedicine http: //emedicine. medscape. com

REFERENCES (CONT’D) � Integumentary system � � Pediatric Dermatology Vol 21 No. 2 109 -112, 2004. Kam Lun Hon, et al. Skin Diseases in Chinese Children at a Pediatric Dermatology Center. Illustrated Textbook of Paediatrics, 3 rd edition. Tom Lissauer, Graham Clayden. T. Schäfer MD, MPHa, P. Dirschedlb, B. Kunz MDc, J. Ring MDa and K. Überla MD. Maternal smoking during pregnancy and lactation increases the risk for atopic eczema in the offspring. Journal of the American Academy of Dermatology. Volume 36, Issue 4, April 1997, Pages 550 -556. Family Health Service, Department of Health. http: //www. fhs. gov. hk/english/health_info/class_topic/ct_child_he alth/ch_newborn. html Common skin problems in Newborns.

End of presentation. THANK YOU!
- Slides: 101