MORTALITY MORBIDITY CONFERENCE CASE SERIES FUO NERISSA ANG

MORTALITY & MORBIDITY CONFERENCE CASE SERIES - FUO NERISSA ANG SORRAH FIEL BRIONES ERICK VERANO February 15, 2007 Ledesma Hall

Objectives l To present two distinct cases of patients presenting with prolonged fever l To be able to discuss the step by step approach in the management of patients’ with fever of unknown origin
FEVER OF UNKNOWN ORIGIN Case Presentation

General Data l l l I. S. 29 year old male single

Chief Complaint l l Work up for on and off Fever 1 month duration
History of Present Illness 6 weeks PTA (+) intermittent fever Tmax: 39. 5ºC (-) associated signs and symptoms Temporary relief by paracetamol 500 mg PO
History of Present Illness 5 weeks PTA (+) intermittent fever Tmax 39ºC (+) 3 episodes LBM Admitted at a local hospital Dx Typhoid fever (+) Typhidot Ig. G + Ig. M Rx Chloramphenicol x 7 days (+) fever episodes Discharged for holiday season
History of Present Illness 3 weeks PTA (+) intermittent fever Tmax 39ºC Self medicate l l l Paracetamol Cotrimoxazole Amoxicillin No relief Readmitted again

Diagnostics A. B. C. D. E. F. G. Malarial Smear – NEGATIVE Peripheral Smear – NORMAL Blood GS – NO GROWTH HIV ELISA – NON REACTIVE ANA – 1. 054 – WEARLY POSITIVE Thyroid Fxm Test – NORMAL UTZ of the abdomen – NORMAL SONOGRAPHICS

Diagnostics H. I. J. Fecalysis – NO OVA / PARASITE SEEN Urinalysis – NORMAL CT of the Abdomen – RENAL CORTICAL CYST (R)

History of Present Illness l l l He was given ceftriaxone 3 G IV OD x 3 days but developed HPS rxn Shifted to cefixime 200 mg BID x 7 days Patient remained to have intermittent fever Tmax 38. 5º despite of antibiotic coverage Opted to be discharged Consult Admission

Past Medical History l l (-) HPN (-) diabetes mellitus (-) asthma (-) Hs of other hospitalization in the past

Family History l l (+) HPN mother (-) heredofamilial diseases l e. g. CA, mumps, leukemia

Personal and Social History l l l Non smoker Non alcoholic beverage drinker (-) history of travel

Review of System l l l l (-) anorexia (-) weight loss (-) cough and colds (-) rashes (-) photophobia (-) alopecia (-) oral ulcers (-) bleeding tendencus

Physical Examination l l l Conscious, coherent not in cardiorespiratory distress BP: 120/80 mm. Hg, CR: 82, RR: 19, Tº: 38. 9ºC Pink palpebral conjunctive, anicteric sclerae (-) TPC, (-) CLAD ECE, (-) Retraction, Clear breath sounds (-) crackles Adynamic precordium, normal rate regular rhythm, ( -) murmur

Physical Examination l l Flat, soft abdomen, NABS, (-) masses, (-) tenderness (-) gross deformities, full equal pulses, (-) cyanosis (-)edema

Salient Features l l 29 y/o male 1 month history of intermittent fever Normal physical examination Came in for work-up

Admitting Impression l Fever of unknown origin

Course in the Ward l Upon admission l l l l l CBC, ESR, CRP Blood CS x 2 sites Monospot test Spec 16 Urinalysis ANA, LE panel CT of the Chest Transesophageal echocardiography Hematology referral for BMA

Laboratory Results CBC Hgb – 12. 5 WBC – 4690 Lymphos – 23 HCT – 39. 6 Seg – 60 Platelet – 223, 000 ESR – 77 (N- 0. 15) CRP – Positive up to 1. 0 serum dilution Bun – 5. 0 Alb – 3. 0 Spec 15 Na – 139 K – 4. 5 Monospot test – Normal Crea – 0. 9

LE Panel l l l ANA – weakly positive Anti DNA (-) Anti SM (-) Anti RNP (-) Anti SSA (-) Anti SSB (-) Anti JO-1 (-)

Transesophageal Echocardiography l l l There is no echocardiography evidence of endocardial vegetation on all four cardiac valves Thickened anterior mitral valve with mild systolic proplase Mild posterolaterally-directed mitral regurgitation Mild tricuspid regurgitation Normal ventricular size and systolic function Ejection fraction 64%

1 st Hospital Day l l Patient was scheduled for BMA CT Scan of the chest l l l Result: INH 300 mg 1 tab OD Rif – 400 mg 1 tab OD PZA – 500 mg 3 tabs OD Ethambutol – 400 mg 3 tabs OD

2 nd Hospital Day l CXR PA Lateral view l l l Result CD 4 CD 8 Post Bone marrow aspiration biopsy
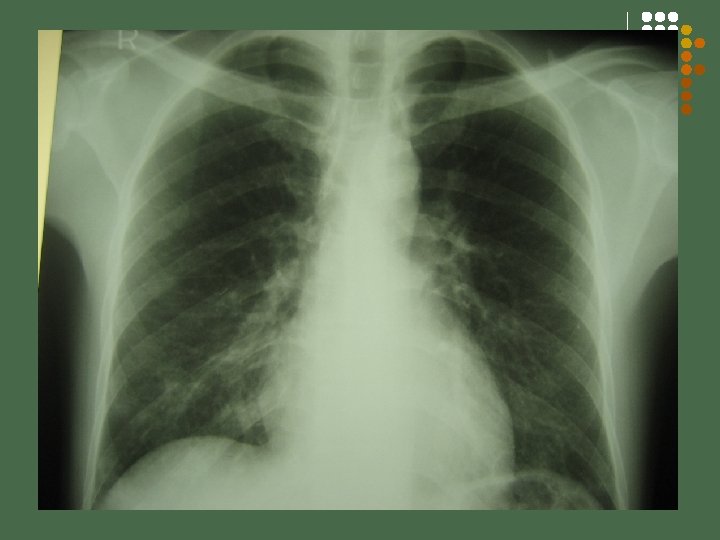

3 rd Hospital Day l Vit A 2500 ml 2 tabs 4 x a day x 8 doses

4 th Hospital Day l l Bone marrow aspiration GS – No growth Bone marrow aspiration biopsy – normal l Normal cellular component Normal megakaryocytes, erythroid and myeloid cells No abnormal tumor cells

5 th – 7 th Hospital Day l Afebrile

8 th Hospital Day l l Discharged Take home medications c/o DOTS

FINAL DIAGNOSIS Miliary Tuberculosis
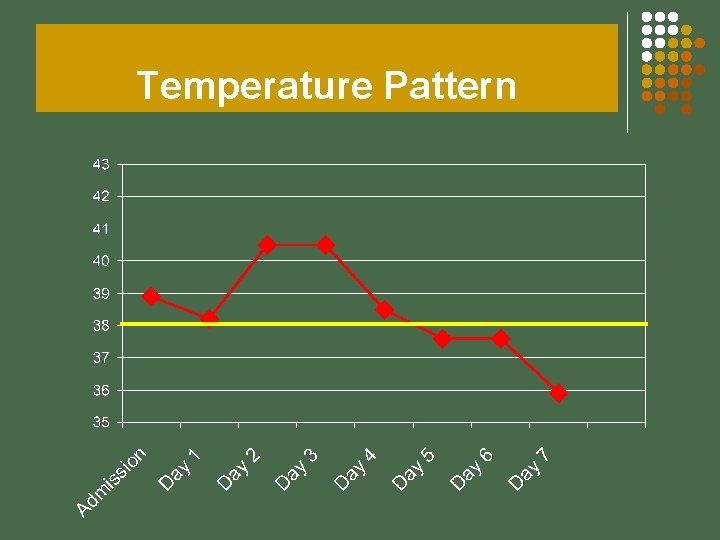
Temperature Pattern

CASE NO. 2 G. F. , a 64 year-old female Chief complaint: fever

HISTORY OF PRESENT ILLNESS 3 weeks PTA intermittent fever (Tmax 38. 8 0 C) (+) loose watery stools x 5 days after taking Dulcolax generalized crampy abdominal pain

HISTORY OF PRESENT ILLNESS admitted at Asian Hospital Dx: Diverticulitis, sigmoid, (confirmed by CT- scan), Infectious diarrhea and UTI given Metronidazole and Ciprofloxacin x 10 days pending urine C/S

HISTORY OF PRESENT ILLNESS 1 week PTA recurrence of fever (Tmax 39 0 C), chills (+) hypogastric pain, dysuria CBC: Hgb 11. 8 Hct 0. 35 wbc 9. 3 seg 80 lym 11 mon 8 plt 533, 000

HISTORY OF PRESENT ILLNESS Urinalysis: rbc: 3 -5 wbc: >150 bacteria: +1 fecalysis: color: greenish brown consistency: semi-formed rbc: 1 -2/hpf wbc: 2 -4/hpf ova/parasites: none
HISTORY OF PRESENT ILLNESS 3 days PTA persistence of symptoms ID consult Dx: Diverticulitis vs UTI given Cotrimoxazole urine C/S: 1. E. coli 25, 000 cfu/m. L resistant to Ciprofloxacin 2. Klebsiella pneumonia 15, 000 sensitive to Ciprofloxacin 2 days PTA ADMISSION

REVIEW OF SYSTEMS No headache No alopecia, rash, photophobia No night sweats No oral ulcers No cough, colds, dyspnea No chest pain, palpitations (+) weight loss of 10 lbs No bleeding tendencies

PAST MEDICAL ILLNESS (+) HPN – 5 months, on Losartan 50 mg OD UBP 120 -130/80 HBP 150/80 (-) DM, BA, PTB Post colonoscopy , November 2006 - normal Post appendectomy – 15 years old

FAMILY HISTORY (+) HPN, CVA, CA (breast) – mother (+) DM – paternal side

PERSONAL & SOCIAL HISTORY Non smoker Non alcoholic beverage drinker No history of travel

PHYSICAL EXAMINATION Conscious, coherent, not in cardio-respiratory distress BP 120/70 CR 89 bpm RR 18 T 37. 7 0 C Wt: 57 kg Ht: 156 cm BMI 23. 4 kg/m 2 Pink palpebral conjunctivae, anicteric sclerae Moist buccal mucosae, non- hyperemic posterior pharyngeal walls, tonsils not enlarged Supple neck, no palpable cervical lymphadenopathies

PHYSICAL EXAMINATION Symmetrical chest expansion, no retractions, clear lungs Adynamic precordium, AB 5 th LICS MCL, no murmurs Flabby abdomen, normoactive bowel sounds, soft, non -tender, no hepatosplenomegaly, no CVA tenderness No edema, no cyanosis, pulses full and equal

IMPRESSION Fever of Unknown Origin

LABORATORY Hgb 11. 2 Hct 35 WBC 9750 Segmenters 70 Lymphocytes 20 Monocytes 10 Platelets 464, 000 CRP Positive up to 1: 16 dilution ESR 125

LABORATORY Urinalysis: rbc 3. 4 WBC 6. 3 epi cells 0. 7 bacteria: 323. 9 Urine C/S: no growth Fecalysis: color: brown consistency: soft Pus cells: 8 -10/hpfmucus: moderate Ova/parasite: none Stool C/S: normal flora Blood C/S: no growth

LABORATORY ANA Negative LE panel Negative VDRL Negative CA 125 20. 447 CA 19 -9 0

2 -D ECHO Normal left ventricular dimension with normal wall thickness, wall motion and contractility. Normal EF 65%. No preicardial effusion nor evidence of vegetation.

CT SCAN OF THE CHEST Minimal fibrosis, both apices otherwise normal CT of the chest

MRI OF THE WHOLE ABDOMEN Diverticulitis, ascending and recto-sigmoid colon. Complex pelvic fluid collections as described. Consider pelvic abscess probably secondary to ruptured diverticulitis.

CT SCAN OF THE WHOLE ABDOMEN Primary consideration is sigmoid diverticulitis with fistula formation. No discrete abscess formation but no intravenous contrast given.
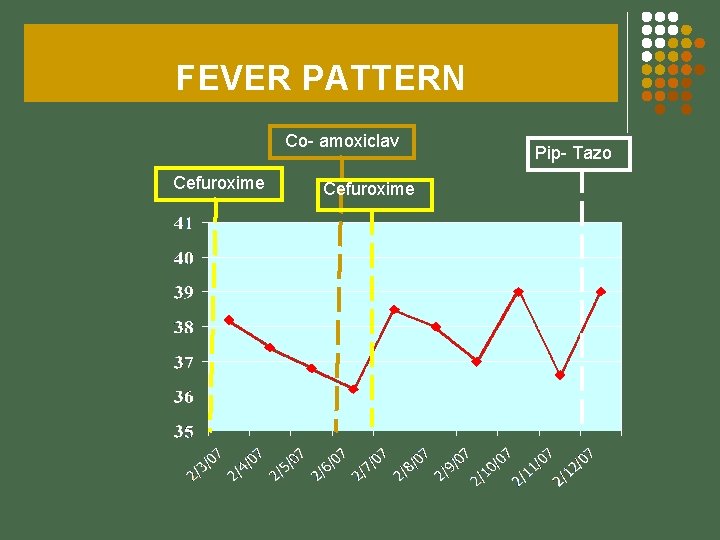
FEVER PATTERN Co- amoxiclav Cefuroxime Pip- Tazo
FEVER OF UNKNOWN ORIGIN DISCUSSION

FEVER OF UNKNOWN ORIGIN l Definition: l l l Fever higher than 38. 3ºC (100. 9°F) on several occasions Duration of fever for > 3 weeks Failure to reach a diagnosis despite 1 week of inpatient investigation …by Petersdorf and Beeson from a prospective analysis of 100 cases, which has become the clinical standard • Petersdorf, RG, Beeson, PB. Fever of unexplained origin: report on 100 cases. Medicine (Baltimore) 1961; 40: 1.

Classification of Fever of Unknown Origin

FEVER OF UNKNOWN ORIGIN l Minimal diagnostic work ups to qualify as FUO: l l l l History Physical examination Complete blood count, including differential and platelet count Routine blood chemistries, including liver enzymes and bilirubin Hepatitis serology (if liver tests abnormal) Urinalysis, including microscopic examination, and urine culture Chest radiograph

FEVER OF UNKNOWN ORIGIN l Risk Factors l l l History of travel Current medications (including antimicrobials) Immunocompromised state l l (Collagen vascular disease /Cancer/ HIV/AIDS) Current or recent hospitalization
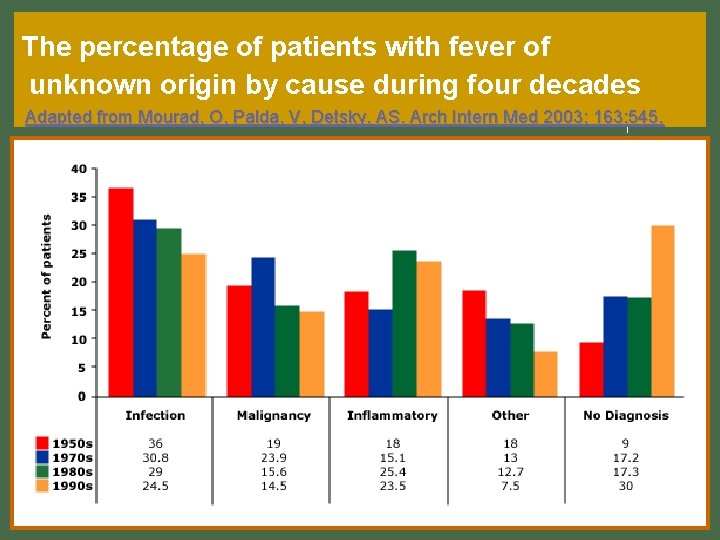
The percentage of patients with fever of unknown origin by cause during four decades Adapted from Mourad, O, Palda, V, Detsky, AS. Arch Intern Med 2003; 163: 545.

Common Etiologies of Fever of Unknown Origin Infections l l l l Tuberculosis (especially extrapulmonary) Abdominal Abscesses Pelvic Abscesses Dental Abscesses Endocarditis Osteomyelitis Sinusitis l l l l Cytomegalovirus Epstein Barr Virus Human immunodeficiency virus Lyme disease Prostatitis Sinusitis Fungal disease

Common Etiologies of Fever of Unknown Origin l l l l l Malignancies Chronic Leukemia Lymphoma Metastatic cancers Renal cell carcinoma Colon carcinoma Hepatoma Myelodysplastic syndromes Pancreatic carcinoma Sarcomas l l l l l Collagen-Vascular Dse Adult Still’s disease Polymyalgia rheumatica Temporal arteritis Rheumatoid arthritis Rheumatoid fever Inflammatory bowel dse Reiter’s syndrome SLE Vasculitides

Common Etiologies of Fever of Unknown Origin Miscellaneous Drug-induced fever * l Complications from cirrhosis l Factitious fever l Hepatitis (alcoholic, granulomatous or lupoid) l Deep venous thrombosis l Sarcoidosis l

DRUG FEVER

DIAGNOSTIC APPROACH FEVER OF UNKNOWN ORIGIN

DIAGNOSIS OF FEVER OF UNKNOWN ORIGIN Fever > 38. 30 C x 3 weeks; 1 week of “intelligence and invasive investigation” Physical Exam CBC, ESR, CRP, urinalysis, liver function tests, electrolytes, blood culture, urine culture, PPD skin test, chest radiograph Positive NO Order appropriate follow up and diagnostic testing CT scan of the chest/ abdomen/pelvis With contrast

DIAGNOSTIC APPROACH l Erythrocyte sedimentation rate — l One study reviewed elevations above 100 mm/h among 263 patients with FUO: l 58 percent had malignancy, most commonly lymphoma, myeloma or metastatic colon or breast cancer l 25 percent had infections such as endocarditis, or inflammatory diseases like rheumatoid arthritis or giant cell arteritis Zacharski, LR, Kyle, RA. Significance of extreme elevation of erythrocyte sedimentation rate. JAMA 1967; 202: 264
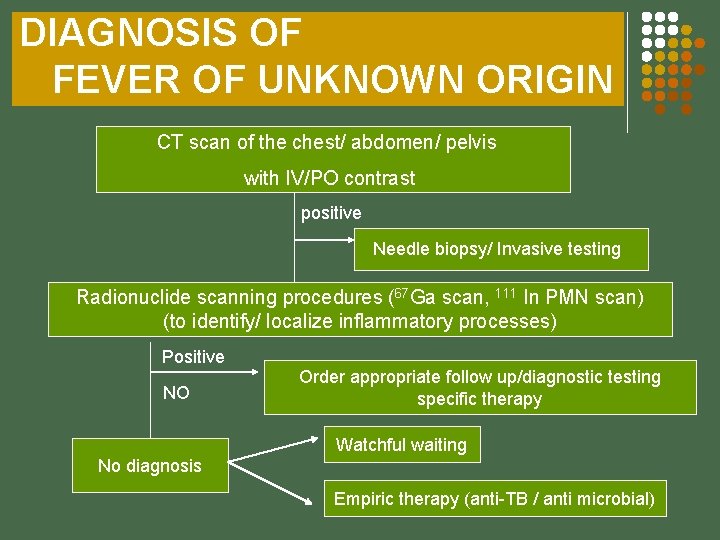
DIAGNOSIS OF FEVER OF UNKNOWN ORIGIN CT scan of the chest/ abdomen/ pelvis with IV/PO contrast positive Needle biopsy/ Invasive testing Radionuclide scanning procedures (67 Ga scan, 111 In PMN scan) (to identify/ localize inflammatory processes) Positive NO Order appropriate follow up/diagnostic testing specific therapy Watchful waiting No diagnosis Empiric therapy (anti-TB / anti microbial)
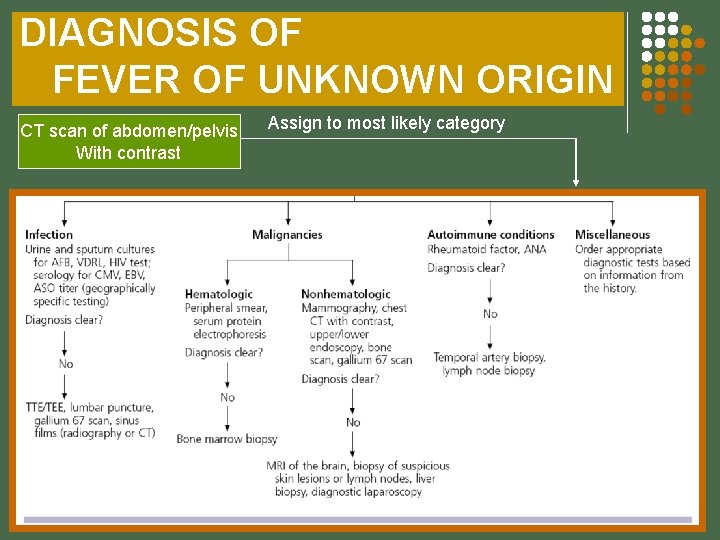
DIAGNOSIS OF FEVER OF UNKNOWN ORIGIN CT scan of abdomen/pelvis With contrast Assign to most likely category
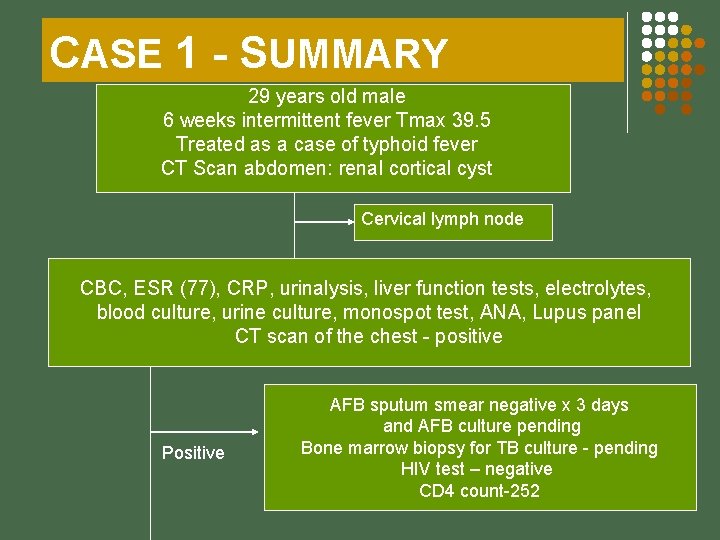
CASE 1 - SUMMARY 29 years old male 6 weeks intermittent fever Tmax 39. 5 Treated as a case of typhoid fever CT Scan abdomen: renal cortical cyst Cervical lymph node CBC, ESR (77), CRP, urinalysis, liver function tests, electrolytes, blood culture, urine culture, monospot test, ANA, Lupus panel CT scan of the chest - positive Positive AFB sputum smear negative x 3 days and AFB culture pending Bone marrow biopsy for TB culture - pending HIV test – negative CD 4 count-252
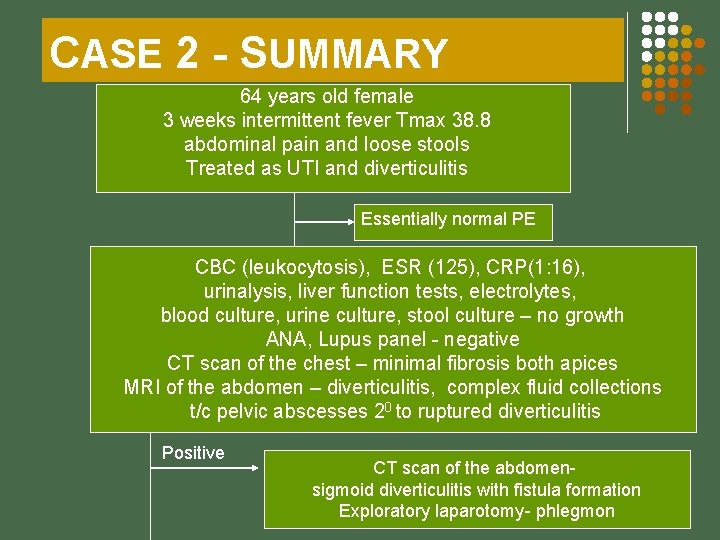
CASE 2 - SUMMARY 64 years old female 3 weeks intermittent fever Tmax 38. 8 abdominal pain and loose stools Treated as UTI and diverticulitis Essentially normal PE CBC (leukocytosis), ESR (125), CRP(1: 16), urinalysis, liver function tests, electrolytes, blood culture, urine culture, stool culture – no growth ANA, Lupus panel - negative CT scan of the chest – minimal fibrosis both apices MRI of the abdomen – diverticulitis, complex fluid collections t/c pelvic abscesses 20 to ruptured diverticulitis Positive CT scan of the abdomensigmoid diverticulitis with fistula formation Exploratory laparotomy- phlegmon

FEVER OF UNKNOWN ORIGIN l Among infections, tuberculosis and abscesses are the most common etiologies. l Tuberculosis l single most common infection in most FUO series. l Presentations of TB, which escape early detection, are either extrapulmonary, miliary, or occur in the lungs of patients with significant preexisting pulmonary disease.

FEVER OF UNKNOWN ORIGIN l Abscess l Usual location of occult abscesses -abdomen or pelvis l Underlying conditions which predispose to abscess formation –cirrhosis, steroid or immunosuppressive medications, recent surgery, and diabetes. l Abscesses arise when there has been disruption of a barrier such as the bowel wall in appendicitis or diverticulitis. The rupture often seals off spontaneously and local peritonitis is converted to an abscess by host defense mechanisms.

FEVER OF UNKNOWN ORIGIN l Therapeutic trials of antimicrobials or corticosteroids, rarely establish a diagnosis. l Antimicrobial agents could be expected to suppress, but not cure, an infectious process such as an occult abscess since adjunctive drainage would usually be required. l A trial of corticosteroids for an inflammatory process should not replace relevant biopsies for steroid responsive diseases; and a careful evaluation for infection should precede such a trial

SUMMARY l Fever of unknown origin (FUO) is defined as fever higher than 38. 3ºC on several occasions lasting for at least three weeks without an established etiology despite intensive evaluation and diagnostic testing l Three general categories of illness account for the majority of "classic" FUO cases and have been consistent through the decades. l These categories are infections, malignancies, and collagen vascular diseases.

SUMMARY l The most important aspects of the evaluation of a patient with FUO are to take a careful history, perform a detailed physical examination, and to reassess the patient frequently. l We recommend the following minimum diagnostic evaluation: blood cultures, erythrocyte sedimentation rate, lactate dehydrogenase, HIV antibody test and viral load, rheumatoid factor, heterophile antibody test, antinuclear antibodies, tuberculin skin test, and CT scan of abdomen and chest

SUMMARY AND RECOMMENDATIONS l Diagnostic workup may fail to identify an etiology in as many as 30 to 50 percent of patients. l Most adults who remain undiagnosed have a good prognosis.

References l l l De Kleijn, EM, Vandenbroucke, JP, van der, Meer JW. Fever of unknown origin (FUO). I A. prospective multicenter study of 167 patients with FUO, using fixed epidemiologic entry criteria. The Netherlands FUO Study Group. Medicine (Baltimore) 1997; 76: 392. Knockaert, DC, Vanneste, LJ, Bobbaers, HJ. Fever of unknown origin in elderly patients. J Am Geriatr Soc 1993; 41: 1187. Miller, RF, Hingorami, AD, Foley, NM. Pyrexia of undetermined origin in patients with human immunodeficiency virus infection and AIDS. Int J STD AIDS 1996; 7: 170. Mourad, O, Palda, V, Detsky, AS. A comprehensive evidence-based approach to fever of unknown origin. Arch Intern Med 2003; 163: 545 Petersdorf, RG, Beeson, PB. Fever of unexplained origin: report on 100 cases. Medicine (Baltimore) 1961; 40: 1. 2. Vanderschueren, S, Knockaert, D, Adriaenssens, T, et al. From prolonged febrile illness to Fever of unknown origin: the challenge continues. Arch Intern Med 2003; 163: 1033. 12
- Slides: 77