Monthly Webinar 2019 Pediatric Services August 28 th

Monthly Webinar – 2019 Pediatric Services August 28 th at 12: 15 pm 1

Webinar Coversheet Tri. Health Physician Hospital Organization(TPHO)Value-based Care Date: 8/28/2019 Location: Web. Ex Topic: Value Adds: Pediatrics Service Line and Measures Speakers: Line΄ Elder-Moore, Julia Mc. Cormick, Lorraine Stephens, MD Additional Speakers: Joseph Bailey, MD, Pamela Coyle-Toerner, Executive Director Primary Care/Pediatric Service Line & Practice Operations Elizabeth Berter, RN, MSOL, BSN; Executive Director Medical Management and Ambulatory Care Coordination for Tri. Health. Objectives (specific or global) At the end of this session, participants should be able to understand: 1. Learn the type of services or support are provided through Pediatric Service Line 2. Understand the PSL quality measures for the Value Based Programs 3. Know tactics being used to meet Value Based Quality program goals Disclosure: No one in a position to control content has any relationships with commercial interests. Tri. Health is accredited by the Ohio State Medical Association (OSMA) to provide continuing medical education for physicians. Tri. Health designates this live activity for a maximum of. 5 AMA Category 1 Credit(s)TM Physicians should only claim credit commensurate with the extent of their participation in this activity. For further information on Continuing Medical Education at Tri. Health, please contact the CME Office at (513) 865 -1625. 2

Meet Our Speakers Guest Expert Presenter: Joseph M Bailey, MD; Board Certified Pediatrician with direct oversight for the Pediatric Service Line. Dr. Bailey is also active under Tri. Health Primary Care Institute. Guest Expert Presenter: Pamela Coyle-Toerner, MHHA; CEO of Tri. Health Q, Queen City Physicians. Coyle- Toerner provided the leadership to design, implement and integrate within the QPC EMR, chronic disease support analysis that allowed eleven physicians in the group to achieve Diabetic Recognition from the National Committee on Quality Assurance in 2004. Coyle-Toerner has a Masters Degree in Hospital and Health Administration from Xavier University and Bachelor of Science Degree from The Ohio State University. Pam has served as Executive Director of Tri. Health Primary Care/Pediatric Service Line & Practice Operations since September 2018. Guest Expert Presenter: Elizabeth Berter, RN, MSOL, BSN; Executive Director Medical Management and Ambulatory Care Coordination for Tri. Health. Beth has been a nurse with Tri. Health over 26 years. She began her nursing career as a perioperative nurse for Good Samaritan Hospital where she had the opportunity to fulfill various roles in Perioperative Services. After 20 years with Good Samaritan Hospital, Beth transited to the practices as a Director of Operations at Group Health and since 2017 she has fulfilled the role of Executive Director for Medical Management and Ambulatory Care Coordination. Expert Presenter: Lorraine Stephens, MD: TPHO Medical Director, Dr. Stephens has served as the Medical Director for TPHO since 2016. She is also the System Chief for Family Medicine at Tri. Health. She has worked with TPP Primary Care Quality since 2008 and currently practices at Bethesda Family Medicine and serves as faculty for the Family Medicine Residency at Tri. Health. Her special interests include programs focusing on improving population health and provider education. Current projects includes improving osteoporosis management in women, system strategy for colon cancer screening and lung cancer screening. Facilitator/Presenter: Line’ Elder-Moore-TPHO Clinical Integration Manager, Line’ has been with the TPHO since October 2018. She has the primary responsibility to ensure engagement, support and education on VBA for TPHO independent PCP’s and specialist. Her previous role was with Anthem where she was Ohio’s Sr. Manager for Provider Network Management, working in step with key providers groups who participated in Valued Bases Agreements and had a goal of moving towards Risk. 3

Agenda • Welcome, Reflection, Celebration of Wins • Pediatric Services/Service Line – Building a Pediatric System of Care • Locations and access to • Services – Key services: Radiology, Anesthesia, ENT & Ortho • Tri. Health has Pediatrics – Quality Metrics Review • 2018 and 2019 – Gap Closure Tactics • Questions 4

Reflection 5

Celebration of Wins TPHO = Tri. Health Population Health Organization! In an attempt to make our core function concise and direct, The TPHO Board decided to change its name from “Physician Hospital Organization” to “Population Health Organization”. With this deliberate change, the TPHO wants our mission crystal clear- ensuring your patients and your practice thrive in the era of value-based care delivery. 6

Webinar Objectives 1. 2. 3. Learn what Tri. Health has done to build a Pediatric System of Care Understand the Pediatric Services quality measures for the Value Based Programs Know the tactics that are being used to meet Pediatric Services Quality program goals By the end of our discussion you will understand: • PSL services, locations and access • Quality Measures related to Pediatric Services • 2018 and 2019 review • Tri. Health’ s gap closure tactics • Your Role 7

Tri. Health Pediatric Services “To every child – I dream of a world where you can laugh, dance, sing, learn, live in peace and be happy. “ Malala Yousafzai 8
Tri. Health has Pediatrics Tri. Health Pediatrics 51 Pediatricians 7 APC 13 Sites All Sites Accepting New Patients 9

Building a Pediatric System of Care 1. Location and Access = Care Retention ü In addition to 51 Pediatricians at 13 sites there are more than 70 primary care Family Medicine physicians at more than 45 sites. ü There is location offering Pediatric Services open 364 days a year. • Pediatric visits fiscal YTD 130, 000 • 2. 3. 4. 5. 30, 000+ flu shots given & offered to parents this year Creating awareness that Tri. Health does PEDS. (copy of ads located in appendix) ü Tri. Health Pediatrics Radio ü Signature Patient Experience through advertisements Target initial key services: Radiology, Anesthesia, ENT & Ortho ü Follow specific guidelines that have been approved by radiologist. (general list below) • General x-rays no age restrictions • CT Scan ages 12 and up for spine, orthopedics, sinus and head without contrast • MRI for MSK ordered by any Tri. Health physician or Orthopedic and Spin Institute have no age restrictions Driving care to our specialists Nurture a culture of care in pediatrics ü Pediatric Monthly meetings 12 times a year lead by Dr. Bailey 10
Pediatric ’s Services Quality Measure Review VBC Data 11
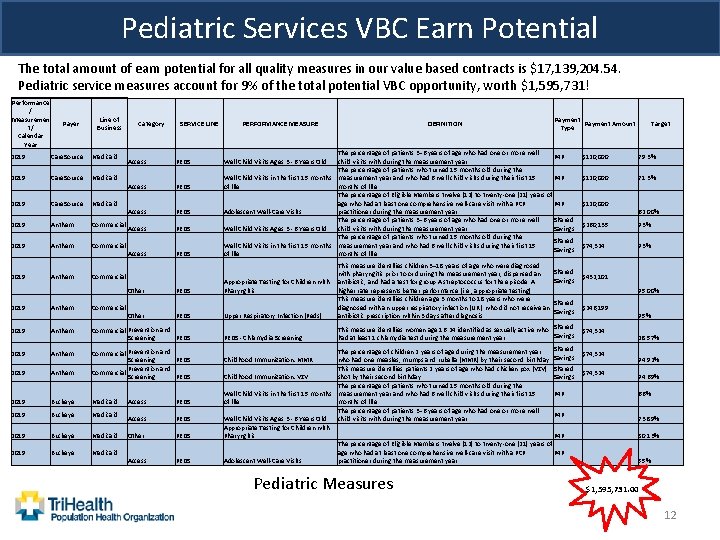
Pediatric Services VBC Earn Potential The total amount of earn potential for all quality measures in our value based contracts is $17, 139, 204. 54. Pediatric service measures account for 9% of the total potential VBC opportunity, worth $1, 595, 731! Performance / Measuremen t/ Calendar Year Payer Line of Business 2019 Care. Source Medicaid 2019 Anthem Commercial Category SERVICE LINE Access PEDS Access PEDS PERFORMANCE MEASURE DEFINITION Payment Amount Type The percentage of patients 3– 6 years of age who had one or more well. P 4 P child visits with during the measurement year. The percentage of patients who turned 15 months old during the Well Child Visits in the first 15 months measurement year and who had 6 well-child visits during their first 15 P 4 P of life months of life The percentage of Eligible Members twelve (12) to twenty-one (21) years of P 4 P age who had at least one comprehensive well-care visit with a PCP Adolescent Well-Care Visits practitioner during the measurement year. The percentage of patients 3– 6 years of age who had one or more well. Shared Well Child Visits Ages 3 - 6 Years Old child visits with during the measurement year. Savings The percentage of patients who turned 15 months old during the Shared Well Child Visits in the first 15 months measurement year and who had 6 well-child visits during their first 15 Savings of life months of life Well Child Visits Ages 3 - 6 Years Old Anthem Commercial PEDS This measure identifies children 3– 18 years of age who were diagnosed Shared with pharyngitis prior to or during the measurement year, dispensed an Savings Appropriate Testing for Children with antibiotic, and had a test for group A streptococcus for the episode. A Pharyngitis higher rate represents better performance (i. e. , appropriate testing). This measure identifies children age 3 months to 18 years who were Shared diagnosed with an upper respiratory infection (URI) who did not receive an Savings Upper Respiratory Infection (Peds) antibiotic prescription within 3 days after diagnosis. 2019 Anthem Commercial Prevention and Screening PEDS This measure identifies women age 16 -24 identified as sexually active who Shared Savings had at least 1 chlamydia test during the measurement year. 2019 Anthem Commercial Prevention and Screening PEDS Prevention and Commercial Screening PEDS 2019 Buckeye Medicaid 2019 Other PEDS Other Access PEDS Other PEDS Access PEDS - Chlamydia Screening Shared The percentage of children 2 years of age during the measurement year Childhood Immunization: MMR who had one measles, mumps and rubella (MMR) by their second birthday. Savings This measure identifies patients 2 years of age who had chicken pox (VZV) Shared Childhood Immunization: VZV shot by their second birthday. Savings The percentage of patients who turned 15 months old during the Well Child Visits in the first 15 months measurement year and who had 6 well-child visits during their first 15 P 4 P of life months of life The percentage of patients 3– 6 years of age who had one or more well. P 4 P Well Child Visits Ages 3 - 6 Years Old child visits with during the measurement year. Appropriate Testing for Children with Pharyngitis P 4 P The percentage of Eligible Members twelve (12) to twenty-one (21) years of P 4 P age who had at least one comprehensive well-care visit with a PCP Adolescent Well-Care Visits practitioner during the measurement year. Pediatric Measures Target $120, 000 79. 3% $120, 000 71. 3% $120, 000 62. 00% $260, 135 93% $74, 324 93% $432, 101 95. 00% $246, 199 $74, 324 95% 28. 57% 94. 92% 94. 69% 66% 73. 89% 80. 13% 55% $1, 595, 731. 00 12
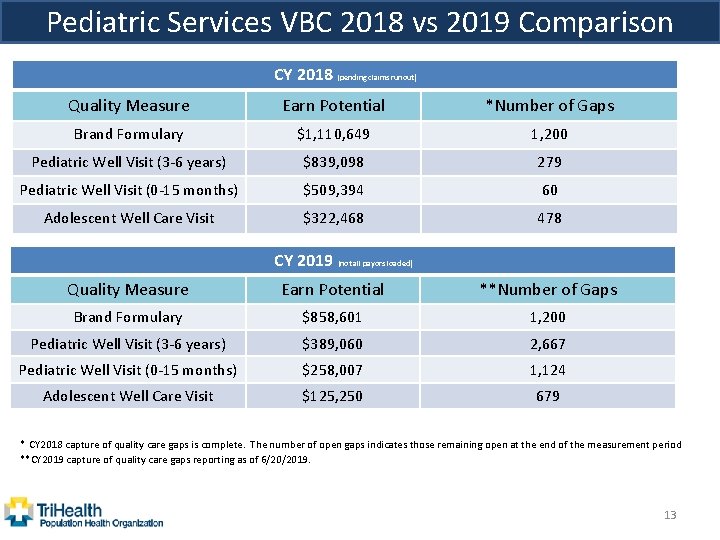
Pediatric Services VBC 2018 vs 2019 Comparison CY 2018 (pending claims runout) Quality Measure Earn Potential *Number of Gaps Brand Formulary $1, 110, 649 1, 200 Pediatric Well Visit (3 -6 years) $839, 098 279 Pediatric Well Visit (0 -15 months) $509, 394 60 Adolescent Well Care Visit $322, 468 478 CY 2019 (not all payors loaded) Quality Measure Earn Potential **Number of Gaps Brand Formulary $858, 601 1, 200 Pediatric Well Visit (3 -6 years) $389, 060 2, 667 Pediatric Well Visit (0 -15 months) $258, 007 1, 124 Adolescent Well Care Visit $125, 250 679 * CY 2018 capture of quality care gaps is complete. The number of open gaps indicates those remaining open at the end of the measurement period **CY 2019 capture of quality care gaps reporting as of 6/20/2019. 13

Population Health: Pediatric Service Measures Tactics • • : Align service line quality measures with VBC measures Obtain access to attributed TPHO patients. Implement operations to support closures of gaps in care in the Pediatric and Family Medicine Practices. Utilize payer reports to make outreach calls to parents of patients with gaps in care. Mail Campaigns Telephonic Outreach Pre-visit Planning 14
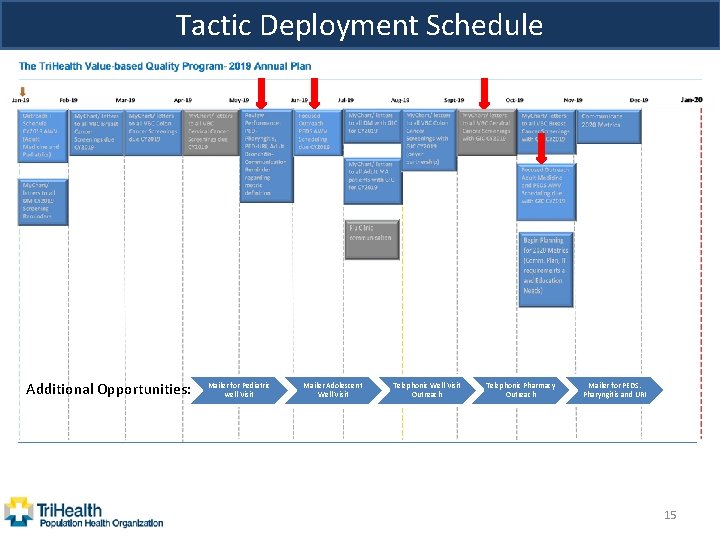
Tactic Deployment Schedule Additional Opportunities: Mailer for Pediatric well Visit Mailer Adolescent Well Visit Telephonic Well Visit Outreach Telephonic Pharmacy Outreach Mailer for PEDS. Pharyngitis and URI 15
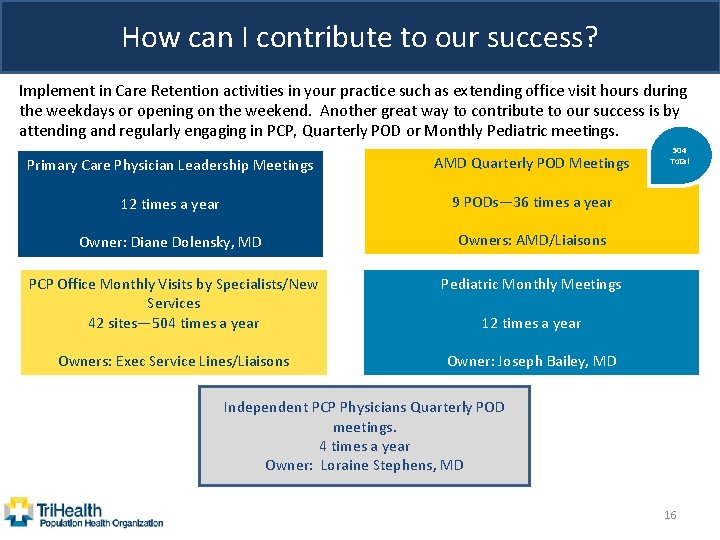
How can I contribute to our success? Implement in Care Retention activities in your practice such as extending office visit hours during the weekdays or opening on the weekend. Another great way to contribute to our success is by attending and regularly engaging in PCP, Quarterly POD or Monthly Pediatric meetings. Primary Care Physician Leadership Meetings AMD Quarterly POD Meetings 12 times a year 9 PODs— 36 times a year Owner: Diane Dolensky, MD Owners: AMD/Liaisons PCP Office Monthly Visits by Specialists/New Services 42 sites— 504 times a year Pediatric Monthly Meetings Owners: Exec Service Lines/Liaisons Owner: Joseph Bailey, MD 504 Total 12 times a year Independent PCP Physicians Quarterly POD meetings. 4 times a year Owner: Loraine Stephens, MD 16
How can I contribute to our success? To ensure that care is maintained within TPHO utilize Kyrus on the Tri. Health. com home page to search for TPHO providers. 46% of care for all TPHO attributed lives happens outside of the network which results in lower continuity of care, patient experience and higher unmanaged cost. 17

Questions? 18

What’s next: • Next webinar: September 25 th at 12: 15 pm • Topic: Care Retention • Questions regarding today’s topic: Pediatric Services • Pamela Coyle-Toerner, Executive Director of Tri. Health Primary Care/Pediatric Service Line & Practice Operations • Pamela_Coyle-Toerner@trihealth. com • Line’ Elder-Moore , Clinical Integration Manager, • Line’_Elder-Moore@Trihealth. com • Elizabeth Berter, RN, MSOL, BSN, • Elizabeth_Berter@trihealth. com 19

Pediatric Presentation Appendix • Tri. Health Pediatrics Radio • Signature Patient Experience – Three Ad’s 20

Tri. Health Pediatrics Radio: 21

Signature Patient Experience 22

Signature Patient Experience 23

Signature Patient Experience 24

Appendix 25

2019 Provider Webinar Topics The goal of the monthly webinar series is to ensure that our Physician partners are knowledgeable on the standards of operation for the valued based arrangements with key payors, understand the resources available through their relationship with the TPHO, well-versed in the use of reports/tools provided to improve performance outcomes and much more. This is a reoccurring event scheduled for the 4 th Wednesday of each month. Listed below is the 2019 topic schedule: MONTH: TOPIC: February 2019 Contract overview March VBC/Population Health 101/22 Core VBC measures April Attribution and Specific Initiatives (breast cancer, colorectal screenings)/Calendar of outreach) May Women’s Services June Pharmacy measures July Data and Analytics August Pediatric service line measures September Care Retention October Down side risk/Care Coordination/ Delegated services/Care Management November Funds Distribution December 2020 Contract Overview Note: Please be advised that monthly topics may be adjusted to accommodate resource challenges. You will be notified in advance on any changes. 26
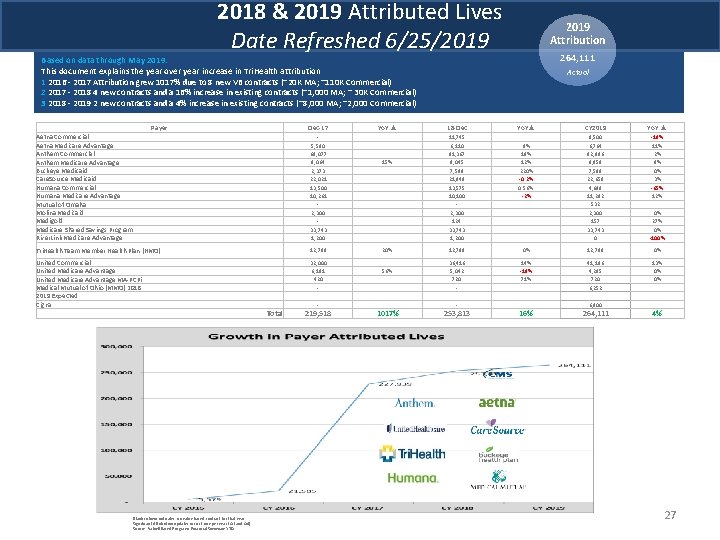
2018 & 2019 Attributed Lives Date Refreshed 6/25/2019 Attribution 264, 111 Based on data through May 2019: This document explains the year over year increase in Tri. Health attribution 1 2016 - 2017 Attribution grew 1017% due to 8 new VB contracts (~20 K MA; ~110 K Commercial) 2 2017 - 2018 4 new contracts and a 16% increase in existing contracts (~1, 000 MA; ~ 30 K Commercial) 3 2018 - 2019 2 new contracts and a 4% increase in existing contracts (~8, 000 MA; ~2, 000 Commercial) Payer Actual Dec-17 Yo. Y ▲ 18 -Dec Yo. Y▲ CY 2019 Yo. Y ▲ Aetna Commercial Aetna Medicare Advantage Anthem Commercial Anthem Medicare Advantage Buckeye Medicaid Care. Source Medicaid Humana Commercial Humana Medicare Advantage Mutual of Omaha Molina Medicaid Medigold Medicare Shared Savings Program River. Link Medicare Advantage 5, 590 69, 077 8, 064 2, 373 22, 021 13, 500 10, 261 2, 300 33, 743 1, 200 15% 11, 745 6, 110 81, 367 9, 045 7, 589 21, 949 13, 575 10, 100 2, 300 124 33, 743 1, 200 9% 18% 12% 220% -0. 2% 0. 56% -2% 9, 500 6, 764 82, 896 9, 859 7, 589 22, 659 4, 699 11, 282 532 2, 300 157 33, 743 0 -19% 11% 2% 9% 0% 3% -65% 12% 0% 27% 0% -100% Tri. Health Team Member Health Plan (HMO) 12, 788 20% 12, 788 0% United Commercial United Medicare Advantage MA-PCPi Medical Mutual of Ohio (MMO) 2018 2019 Expected Cigna 32, 000 6, 181 420 56% 36, 416 5, 042 720 14% -18% 71% - - 41, 186 4, 285 720 6, 252 6, 900 13% 0% 0% 264, 111 4% Blank column indicates no value based contract for that year Significant Attribution updates occur twice per year (Q 1 and Q 4) Source: Value 0 Based Programs Financial Summary YTD Total 219, 518 1017% 253, 813 16% 27
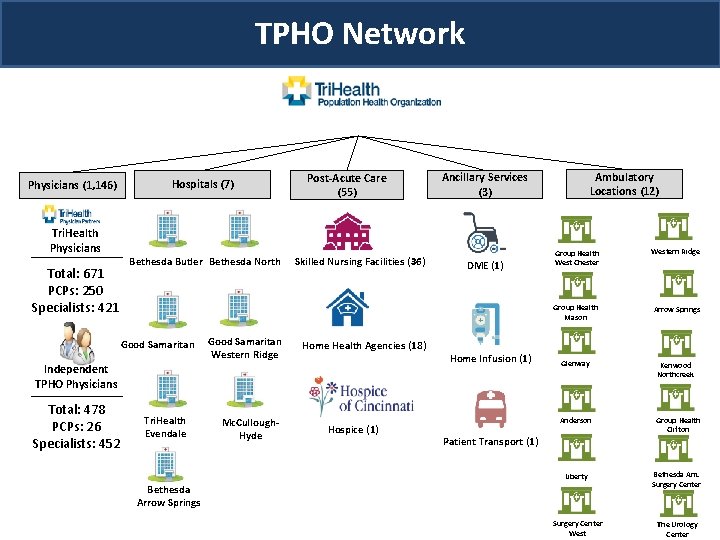
TPHO Network Physicians (1, 146) Tri. Health Physicians Total: 671 PCPs: 250 Specialists: 421 Hospitals (7) Bethesda Butler Bethesda North Good Samaritan Western Ridge Post-Acute Care (55) Skilled Nursing Facilities (36) Home Health Agencies (18) Independent TPHO Physicians Total: 478 PCPs: 26 Specialists: 452 Tri. Health Evendale Mc. Cullough. Hyde Hospice (1) Ambulatory Locations (12) Ancillary Services (3) DME (1) Home Infusion (1) Group Health West Chester Western Ridge Group Health Mason Arrow Springs Glenway Kenwood Northcreek Anderson Group Health Clifton Patient Transport (1) Liberty Bethesda Arrow Springs Surgery Center West Bethesda Am. Surgery Center The Urology Center
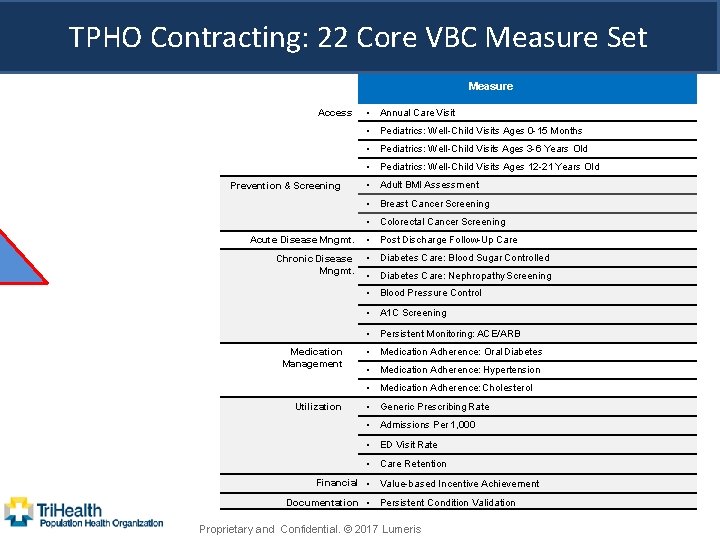
TPHO Contracting: 22 Core VBC Measure Set Measure Access • Annual Care Visit • Pediatrics: Well-Child Visits Ages 0 -15 Months • Pediatrics: Well-Child Visits Ages 3 -6 Years Old • Pediatrics: Well-Child Visits Ages 12 -21 Years Old Prevention & Screening • Adult BMI Assessment • Breast Cancer Screening • Colorectal Cancer Screening Acute Disease Mngmt. Chronic Disease Mngmt. • Post Discharge Follow-Up Care • Diabetes Care: Blood Sugar Controlled • Diabetes Care: Nephropathy Screening • Blood Pressure Control • A 1 C Screening • Persistent Monitoring: ACE/ARB Medication Management • Medication Adherence: Oral Diabetes • Medication Adherence: Hypertension • Medication Adherence: Cholesterol Utilization • Generic Prescribing Rate • Admissions Per 1, 000 • ED Visit Rate • Care Retention Financial • Value-based Incentive Achievement Documentation • Persistent Condition Validation Proprietary and Confidential. © 2017 Lumeris

• Definitions-Commonly used terms • Value Based program revenue structure • Healthcare dollars breakdown

Value Based Contracting Definitions Accountable Care Organization (AC)-ACOs are groups of doctors, hospitals, and other health care providers, who come together voluntarily to give coordinated high-quality care to their Medicare patients. The goal of coordinated care is to ensure that patients get the right care at the right time, while avoiding unnecessary duplication of services and preventing medical errors. Care Coordination Dollars: A per member/per month payment from the payor to the physician/system to provide funds to assist in building the infrastructure for coordinated care. Gap in Care or Care Gap: A “Gap In Care” is defined as the discrepancy between recommended best practices and the care that is actually provided. This can manifest itself in several different ways, but the most common include: Individuals missing agebased or seasonal screenings or vaccines. Hierarchical Condition Category (HCC): HCC is defined as a risk adjustment model that is used to calculate risk scores to predict future healthcare costs. The Centers for Medicare and Medicaid Services' (CMS) CMS-HCC model is used to predict healthcare spending for Medicare Advantage Plan enrollees.

Value Based Contracting Definitions Value Pay for Performance in healthcare (P 4 P): this is also known as value-based payment, comprises payment models that attach financial incentives/disincentives to provider performance. P 4 P is part of the overall national strategy to transition healthcare to value-based medicine. Population Health-Population health has been defined as "the health outcomes of a group of individuals, including the distribution of such outcomes within the group". It is an approach to health that aims to improve the health of an entire population. Quality Dollars: A per member/per month payment from the payor to the physician/system for successfully participating in quality activities to improve the health of the patient population. Often times these are Hedis measures. (Breast cancer screening, Colorectal screening, annual visits) When these quality activities haven’t yet been completed, they are often referred to as a “Gap in Care. ” Risk Adjustment Factor (RAF). A statistical process that takes into account the underlying health status and health spending of the enrollees in an insurance plan when looking at their health care outcomes or health care costs. 32

Value Based Contracting Definitions Shared Savings Dollars: A payment strategy that offers incentives for providers to reduce health care spending for a defined patient population by offering them a percentage of net savings realized as a result of their efforts. The Shared Savings Program is an important innovation for moving CMS' payment system away from volume and toward value and outcomes. It is an alternative payment model that: • Promotes accountability for a patient population. • Coordinates items and services for Medicare FFS beneficiaries. • Encourages investment in high quality and efficient services. Value Based Population-Patient allocation to PCP processes: • Attribution: Payor assigns a patient to a PCP based on claims history • Assignment: The patients selects their PCP 33
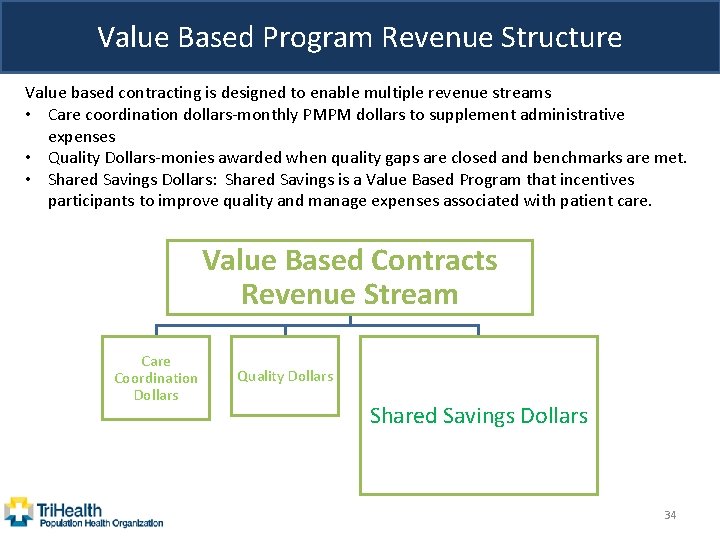
Value Based Program Revenue Structure Value based contracting is designed to enable multiple revenue streams • Care coordination dollars-monthly PMPM dollars to supplement administrative expenses • Quality Dollars-monies awarded when quality gaps are closed and benchmarks are met. • Shared Savings Dollars: Shared Savings is a Value Based Program that incentives participants to improve quality and manage expenses associated with patient care. Value Based Contracts Revenue Stream Care Coordination Dollars Quality Dollars Shared Savings Dollars 34
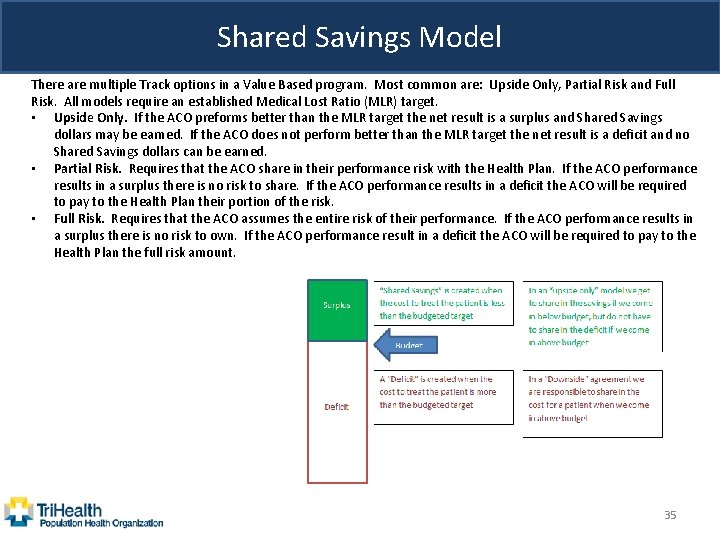
Shared Savings Model There are multiple Track options in a Value Based program. Most common are: Upside Only, Partial Risk and Full Risk. All models require an established Medical Lost Ratio (MLR) target. • Upside Only. If the ACO preforms better than the MLR target the net result is a surplus and Shared Savings dollars may be earned. If the ACO does not perform better than the MLR target the net result is a deficit and no Shared Savings dollars can be earned. • Partial Risk. Requires that the ACO share in their performance risk with the Health Plan. If the ACO performance results in a surplus there is no risk to share. If the ACO performance results in a deficit the ACO will be required to pay to the Health Plan their portion of the risk. • Full Risk. Requires that the ACO assumes the entire risk of their performance. If the ACO performance results in a surplus there is no risk to own. If the ACO performance result in a deficit the ACO will be required to pay to the Health Plan the full risk amount. 35
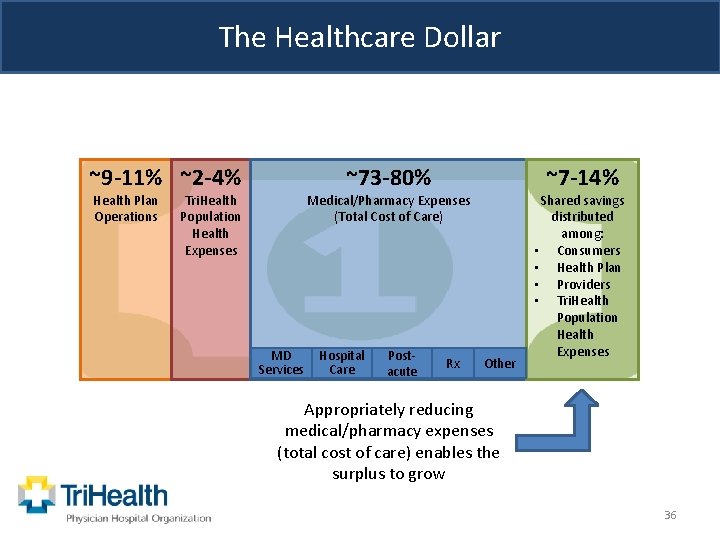
The Healthcare Dollar ~9 -11% ~2 -4% Health Plan Operations ~73 -80% Tri. Health Population Health Expenses ~7 -14% Medical/Pharmacy Expenses (Total Cost of Care) MD Services Hospital Care Postacute Rx Other Shared savings distributed among: • Consumers • Health Plan • Providers • Tri. Health Population Health Expenses Appropriately reducing medical/pharmacy expenses (total cost of care) enables the surplus to grow 36
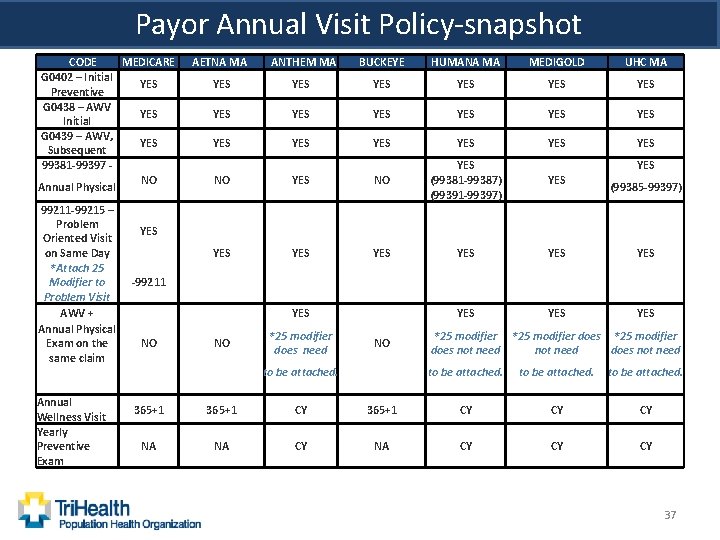
Payor Annual Visit Policy-snapshot CODE MEDICARE G 0402 – Initial YES Preventive G 0438 – AWV YES Initial G 0439 – AWV, YES Subsequent 99381 -99397 NO Annual Physical 99211 -99215 – Problem YES Oriented Visit on Same Day *Attach 25 -99211 Modifier to Problem Visit AWV + Annual Physical NO Exam on the same claim Annual 365+1 Wellness Visit Yearly NA Preventive Exam AETNA MA ANTHEM MA BUCKEYE HUMANA MA MEDIGOLD UHC MA YES YES YES YES YES NO YES (99381 -99387) (99391 -99397) YES YES YES NO *25 modifier does need NO to be attached. YES (99385 -99397) *25 modifier does not need does not need to be attached. 365+1 CY CY CY NA CY CY CY 37
- Slides: 37