Monoamine neurotransmitters Acetylcholine and Histamine Paul Glue Biogenic

Monoamine neurotransmitters (+ Acetylcholine and Histamine) Paul Glue
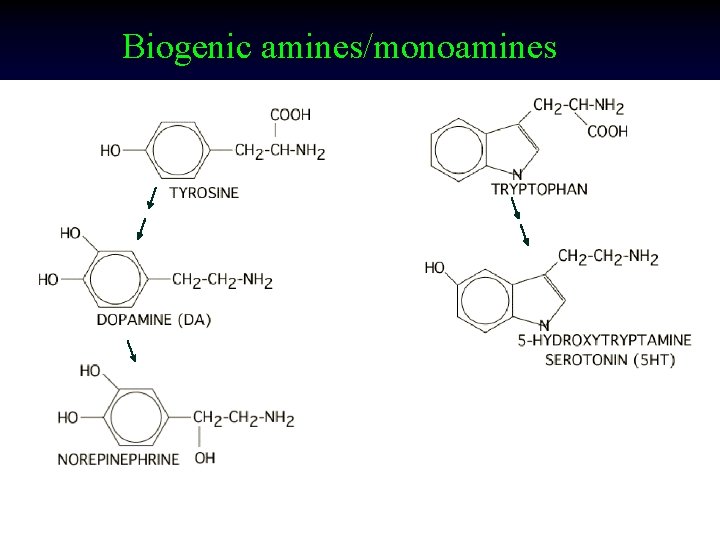
Biogenic amines/monoamines
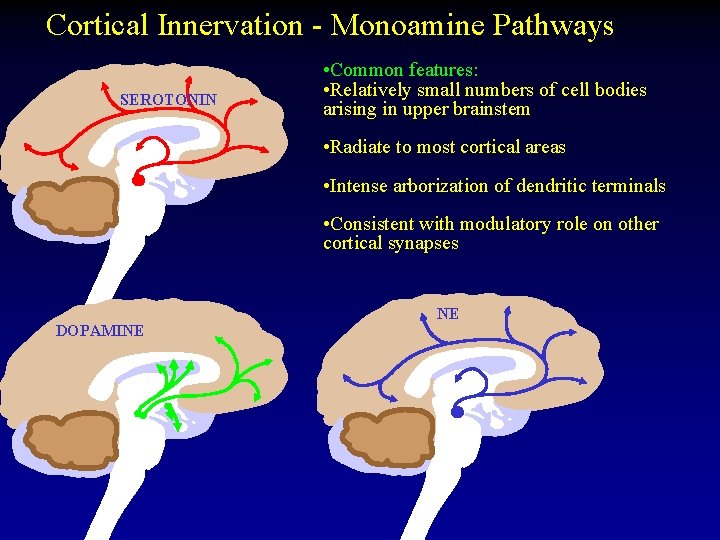
Cortical Innervation - Monoamine Pathways SEROTONIN DOPAMINE NOREPINEPHRINE DOPAMINE • Common features: • Relatively small. Common numbers of cell bodies features: Common features: arising in upper brainstem Cell bodies arising in in upper brainstem • Radiate to most cortical areas Radiate to to most cortical areas • Intense arborization of dendritic terminals Intense arborization of of dendritic terminals role on other • Consistent with modulatory cortical synapses Consistent with modulatory role NE Ventral Tegmental Substantia Nigra Area Substantia Nigra DOPAMINE
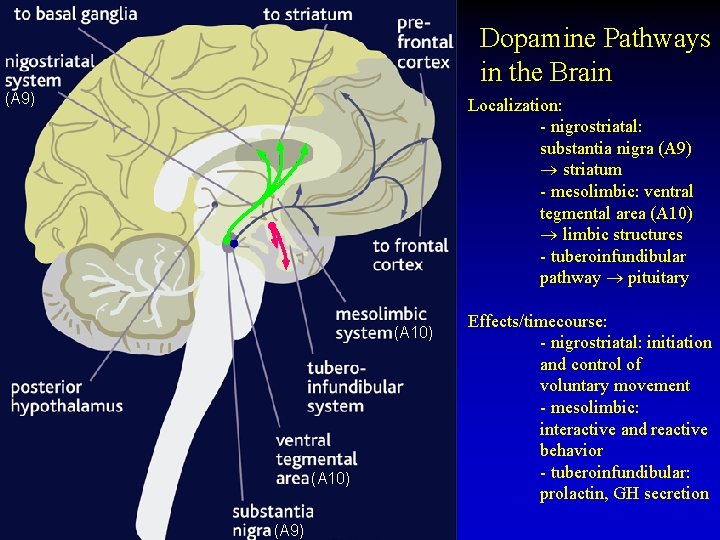
Dopamine Pathways in the Brain (A 9) Localization: - nigrostriatal: substantia nigra (A 9) striatum - mesolimbic: ventral tegmental area (A 10) limbic structures - tuberoinfundibular pathway pituitary (A 10) (A 9) Effects/timecourse: - nigrostriatal: initiation and control of voluntary movement - mesolimbic: interactive and reactive behavior - tuberoinfundibular: prolactin, GH secretion

Dopamine receptors • • Density in CNS: D 1>D 2>D 3>D 4>D 5 D 1, D 5 linked to adenylate cyclase D 2, D 3, D 4 (not linked to AC) Functions: – Only D 2 antagonism linked to antipsychotic effects – D 2/3 agonists for Parkinson’s Disease – D 1 antagonists ? anticraving effects – No known function for D 4/5 ligands •

Functions of DA in the brain • Motor control: movement initiation and cessation • Reward/Motivation: dependence liability of compounds correlated with degree of DA release in Nucleus Accumbens • Endocrine: Inhibition of prolactin release • Mood: DA releasers/reuptake inhibitors (e. g. cocaine, amphetamine) cause euphoria; D 2 antagonists – anhedonia in HVs • Psychosis: DA releasers/reuptake inhibitors may produce psychotic symptoms (paranoid delusions; hallucinations; etc); all antipsychotics are D 2 antagonists • Sleep: VTA inhibits ventrolateral preoptic area • Attention/Learning/Working memory

Peripheral DA activity – Blood vessel smooth muscle beds (vasorelaxation) – Atria ( myocardial contractility, cardiac output) – Kidneys (nephrons, prox tubule epithelium) – sodium excretion – Gut wall plexus – Lymphocytes
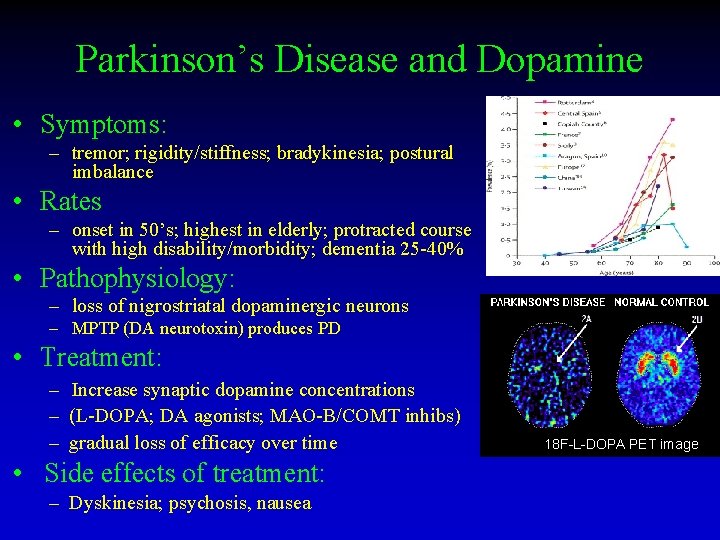
Parkinson’s Disease and Dopamine • Symptoms: – tremor; rigidity/stiffness; bradykinesia; postural imbalance • Rates – onset in 50’s; highest in elderly; protracted course with high disability/morbidity; dementia 25 -40% • Pathophysiology: – loss of nigrostriatal dopaminergic neurons – MPTP (DA neurotoxin) produces PD • Treatment: – Increase synaptic dopamine concentrations – (L-DOPA; DA agonists; MAO-B/COMT inhibs) – gradual loss of efficacy over time • Side effects of treatment: – Dyskinesia; psychosis, nausea 18 F-L-DOPA PET image

Schizophrenia and Dopamine • Symptoms: delusions; hallucinations; disturbances of thought; bizarre behavior; personality change; apathy; withdrawal; etc; episodic or progressive patterns • Rates: peak onset in late teens-early 30’s; ~ 1% lifetime prevalence • Pathophysiology: – mesolimbic dopaminergic dysfunction/overactivity (hypothesized) • cocaine/amphetamine produce psychotic symptoms • increased DA release relative to controls (no differences in brain DA concs, DA receptor density, etc. ) • Treatment: – All effective drugs are dopamine D 2 antagonists (+ other pharmacological effects); potency correlates with daily dose • Side effects: – Tremor, stiffness; restlessness; akathisia Laruelle M, Biol Psych 1999
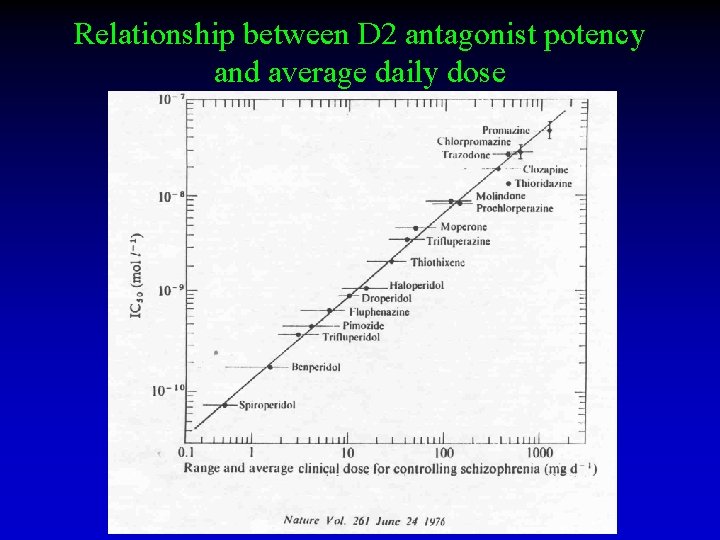
Relationship between D 2 antagonist potency and average daily dose

Dopaminergic Effects/Side Effects • Drugs that increase DA neurotransmission ( synaptic DA) • most are effective symptomatic treatments for PD • may precipitate/worsen psychosis/dyskinesia • potentially addictive • other s/e: nausea, GI symptoms – Postsynaptic agonists (DA from L-DOPA; bromocriptine, pramipexole) – Inhibitors of enzymes which degrade DA (MAOIs (selective MAO-B-I: deprenyl); COMT inhibitors (entocapone) – Inhibitors of DA reuptake or inducers of DA release (cocaine, damphetamine - not yet shown to help PD) • Block DA neurotransmission (postsynaptic antagonism) • worsen PD; may induce reversible Parkinsonian sx • improve psychotic symptoms • antiemetic, prokinetic – Typical neuroleptics - D 2 antagonists (haloperidol etc plus newer agents) – Atypical neuroleptics (D 2 antagonism + ? : clozapine)
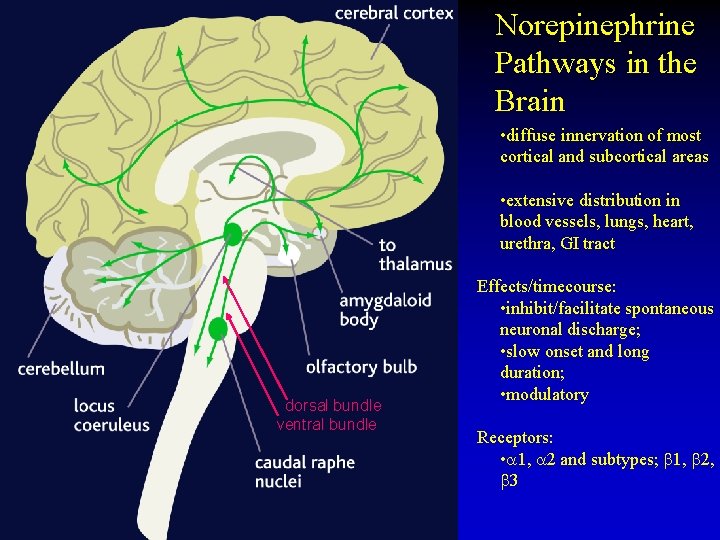
Norepinephrine Pathways in the Brain • diffuse innervation of most cortical and subcortical areas • extensive distribution in blood vessels, lungs, heart, urethra, GI tract dorsal bundle ventral bundle Effects/timecourse: • inhibit/facilitate spontaneous neuronal discharge; • slow onset and long duration; • modulatory Receptors: • 1, 2 and subtypes; 1, 2, 3

Agonist effects at NE receptors • 1: • 2: • 3: – Smooth muscle contraction (blood vessels, urethra, bronchioles, etc) – Central autoreceptor (presynaptic inhibition of NE release) – Endocrine ( insulin, glucagon release in pancreas) – GI (sphincter contraction) – Platelet aggregation – Increased cardiac output (contractility, – Endocrine (ghrelin, renin secretion) – Smooth muscle relaxation (uterus, bladder, blood vessels, bronchi – Lipolysis NE in the periphery: sympathetic nervous system (fight or flight)

Functions of NE in the brain • Alertness/Arousal/Sleep: – LC inhibits ventrolateral preoptic area • Memory • Mood • Attention/Learning/Working memory Disorders associated with altered central NE • Depression • Anxiety/panic disorder – NE= anxiety; MHPG concs (NE metabolite) correlate with anxiety • ADHD • Schizophrenia – Akathisia (+); negative symptoms (-)

NE Effects/Side Effects • Increase NE neurotransmission by increasing synaptic NE • most are effective symptomatic treatments for major depression • may cause adrenergic side effects (increased blood pressure, heart rate, dry mouth, tremor) – Presynaptic reuptake blockers (imipramine; venlafaxine; etc; cocaine is not!) – Indirect effects on NE neurotransmission (fluoxetine and other SSRIs - neuronal crosstalk; lithium and ECT) – Enzyme inhibitors (MAOIs: phenelzine etc) • Decrease NE neurotransmission • risk of inducing or worsening depression • adrenergic side effects sedation, bradycardia, hypotension (esp. postural), bronchoconstriction – Inhibit NE formation/release (reserpine; a-methyldopa) – Post-synaptic -adrenoceptor antagonists (e. g. propranolol - uncommon)
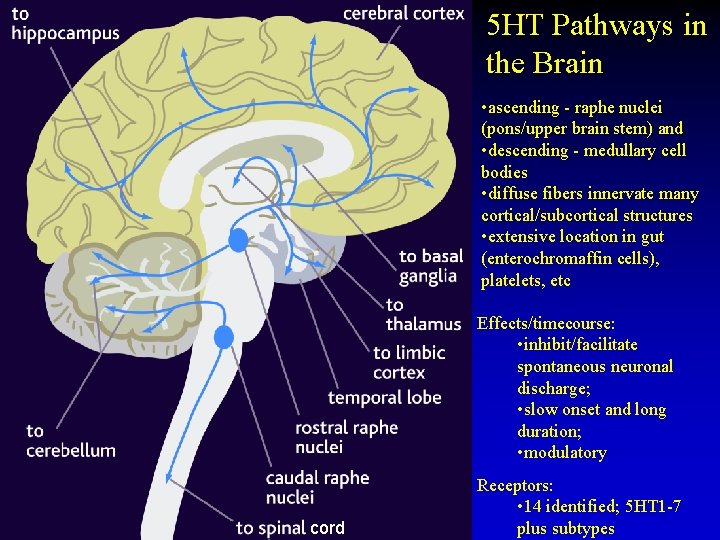
5 HT Pathways in the Brain • ascending - raphe nuclei (pons/upper brain stem) and • descending - medullary cell bodies • diffuse fibers innervate many cortical/subcortical structures • extensive location in gut (enterochromaffin cells), platelets, etc Effects/timecourse: • inhibit/facilitate spontaneous neuronal discharge; • slow onset and long duration; • modulatory cord Receptors: • 14 identified; 5 HT 1 -7 plus subtypes

14 serotonin receptors in 6 families Family 5 -HT 1 5 -HT 2 5 -HT 3 5 -HT 4 5 -HT 5 5 -HT 6 5 -HT 7 Type Gi/Go-protein coupled. Gq/G 11 -protein coupled. Ligand-gated Na+ and K+ cation channel. Gs-protein coupled. Gi/Go-protein coupled. Gs-protein coupled. Mechanism Decreases c. AMP. Increases IP 3 and DAG. Depolarizing plasma membrane. Increases c. AMP. Decreases c. AMP. Increases c. AMP. Potential Inhibitory Excitatory Inhibitory Excitatory

Serotonin 1/2 receptors • 5 HT 1 a: buspirone (partial agonist) – • 5 HT 1 b: triptans (agonists) – (5 HT 1 c – no such receptor) • 5 HT 1 d: triptans (agonists) – • 5 HT 1 e: methysergide • 5 HT 1 f: triptans (agonists) – anxiolytic, antidepressant vasoconstriction; antimigraine • 5 HT 2 a: LSD, psilocybin (agonists) – SGAs (antagonists) • 5 HT 2 b: Fenfluramine (agonist) Tegaserod (antagonist) • 5 HT 2 c: Mirtazapine (antagonist) - perception ? reduced EPSE anorexia reduced GI motility/IBS anxiolytic. antidepressant vasoconstriction; antimigraine ? effect vasoconstriction; antimigraine

Serotonin 3 -7 receptors • • • 5 HT 3: ondansetron (antagonist) – 5 HT 4: cisapride, tegaserod (agonists) 5 HT 5 a: ? function 5 HT 6: ? function 5 HT 7: ? function anti-nausea, vomiting altered GI motility

Drugs that modulate 5 HT • Increase 5 HT neurotransmission by increasing synaptic 5 HT • most are effective symptomatic treatments for major depression • may cause serotonergic side effects (nausea/GI discomfort; anxiety; tremor; insomnia) – – Selective presynaptic reuptake blockers ( SSRIs fluoxetine; paroxetine; etc) Nonselective presynaptic reuptake blockers (imipramine etc) Indirect effects on 5 HT neurotransmission (lithium and ECT) Enzyme inhibitors (MAOIs: phenelzine etc) • Decrease 5 HT neurotransmission – Most serotonin antagonists have no obvious side effects – Subtype selective effects may affect GI motility, nausea, vomiting, EPSE – General 5 HT depletion risk of inducing or worsening depression • experimental depletion of brain 5 HT (L-tryptophan-free amino acid drink)

Monoamine transporters (Example - SERT) A brief history: - 1961: Axelrod: presynaptic uptake of neurotransmitter first reported - 1979: Raisman: SERT is a target for antidepressant drugs - 1981: Langer: linking of SERT to depression - 1991: Blakely: sequence of the transporter gene from rats published
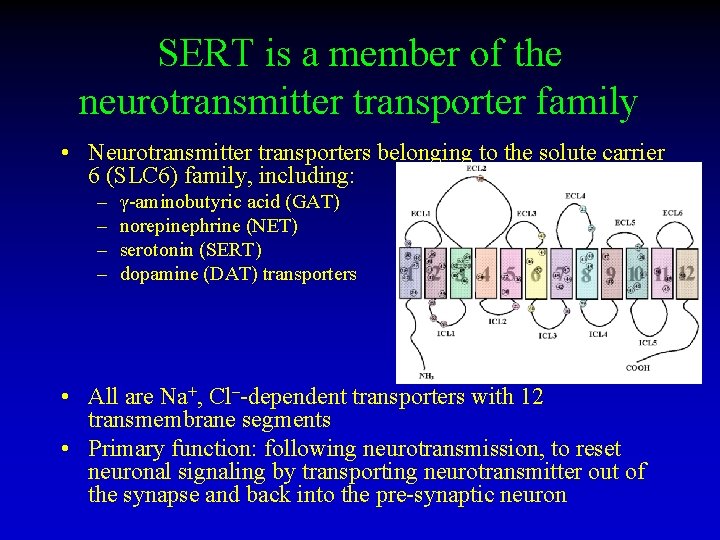
SERT is a member of the neurotransmitter transporter family • Neurotransmitter transporters belonging to the solute carrier 6 (SLC 6) family, including: – – γ-aminobutyric acid (GAT) norepinephrine (NET) serotonin (SERT) dopamine (DAT) transporters • All are Na+, Cl–-dependent transporters with 12 transmembrane segments • Primary function: following neurotransmission, to reset neuronal signaling by transporting neurotransmitter out of the synapse and back into the pre-synaptic neuron
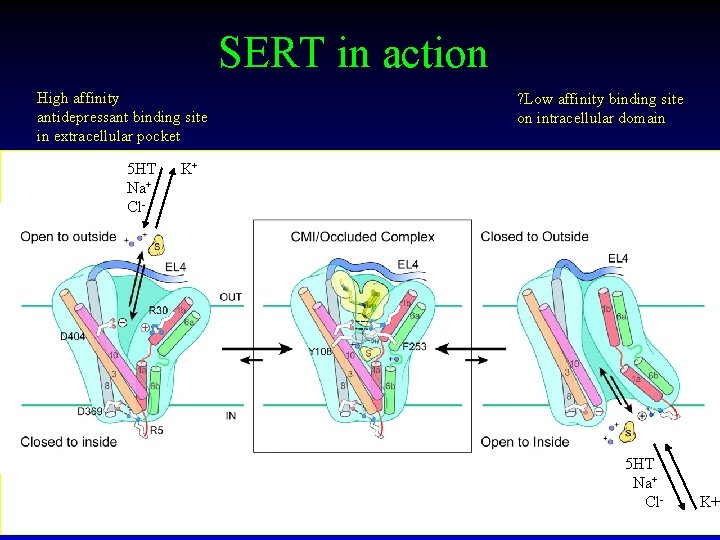
SERT in action High affinity antidepressant binding site in extracellular pocket 5 HT Na+ Cl- ? Low affinity binding site on intracellular domain K+ 5 HT Na+ Cl- K+

Monoamine transporters and psychotropics Reuptake Inhibitors: (not substrates for the transporter) SSRIs Mixed monoamine reuptake inhibitors Psychostimulants Substrates: (release 5 HT after being taken up by SERT) Amphetamine Fenfluramine Ecstacy/MDMA m. CPP (trazodone metabolite)
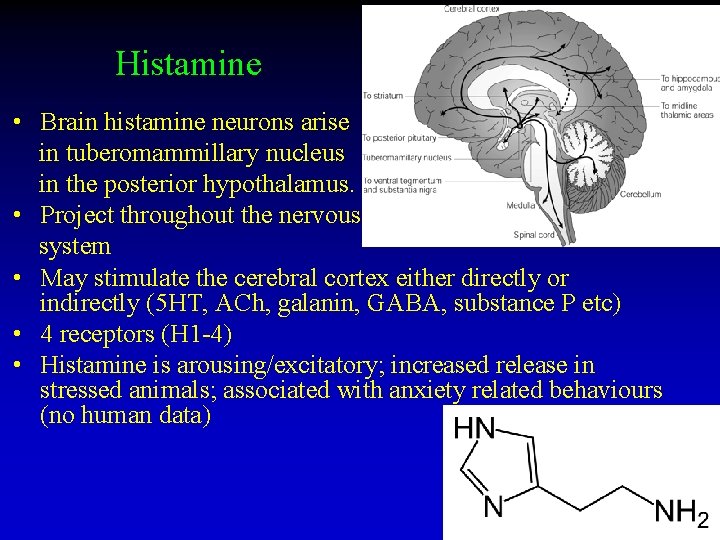
Histamine • Brain histamine neurons arise in tuberomammillary nucleus in the posterior hypothalamus. • Project throughout the nervous system • May stimulate the cerebral cortex either directly or indirectly (5 HT, ACh, galanin, GABA, substance P etc) • 4 receptors (H 1 -4) • Histamine is arousing/excitatory; increased release in stressed animals; associated with anxiety related behaviours (no human data)

Histaminic drugs • H 1 antagonists: antiallergy/ local antiinflammatory effects • H 2 antagonists: reduced gastric acid secretion • H 3 (antagonists) – may enhance transmission of monoamines, histamine – experimental • H 4: ? ?
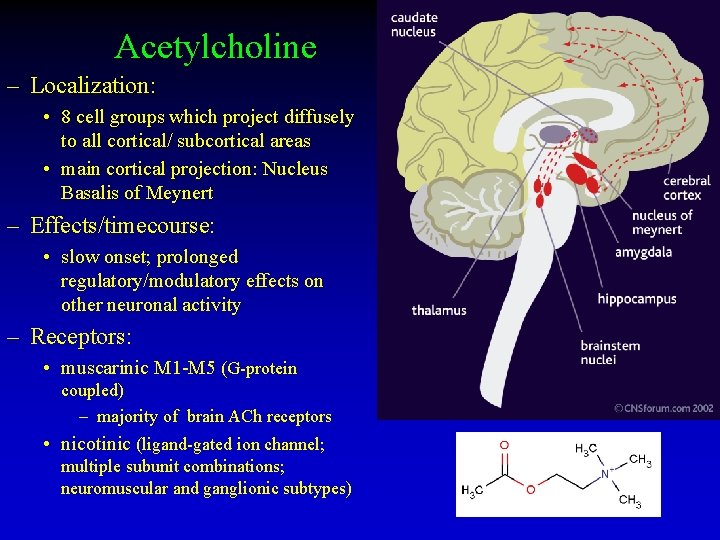
Acetylcholine – Localization: • 8 cell groups which project diffusely to all cortical/ subcortical areas • main cortical projection: Nucleus Basalis of Meynert – Effects/timecourse: • slow onset; prolonged regulatory/modulatory effects on other neuronal activity – Receptors: • muscarinic M 1 -M 5 (G-protein coupled) – majority of brain ACh receptors • nicotinic (ligand-gated ion channel; multiple subunit combinations; neuromuscular and ganglionic subtypes)

ACh receptor localization Brain (m 1 -5) Autonomic ganglia (m 1) Heart (m 2) Smooth muscle (m 2, m 3) Exocrine glands (m 3) Lung (m 4) Autonomic NS (n) Skeletal muscle (n) Brain (n) Agonists Learning/memory GI motility, nausea HR ( vagal tone) vasodilation; bladder contraction salivation broncho-constriction +/- (dose dependent) attention, performance; tremor Antagonists memory impairment GI motility, constipation HR urinary hesitancy; blurred vision dry mouth paralysis

Functions of ACh in the brain • Learning and memory • anticholinergics and ACh lesions impair learning and memory • Attention/arousal • Pain (? ) • Schizophrenia (? sensory gating) • (peripherally) – striated muscle activation – autonomic innervation • parasympathetic NS
![Cholinergic Side Effects • Muscarinic antagonists [nonselective neuroleptics, antidepressants] – impair memory – symptoms Cholinergic Side Effects • Muscarinic antagonists [nonselective neuroleptics, antidepressants] – impair memory – symptoms](http://slidetodoc.com/presentation_image_h/17cea5a88405f250e71f8cc54ef91e60/image-32.jpg)
Cholinergic Side Effects • Muscarinic antagonists [nonselective neuroleptics, antidepressants] – impair memory – symptoms of peripheral cholinergic blockade – – constipation urinary hesitancy blurred vision dry mouth • Muscarinic agonists – nausea, diarrhea – drooling – improved attention, memory
![Therapeutic ACh Compounds • Cholinesterase inhibitors (donepezil; rivastigmine; galanthamine) • increase brain [ACh]; improves Therapeutic ACh Compounds • Cholinesterase inhibitors (donepezil; rivastigmine; galanthamine) • increase brain [ACh]; improves](http://slidetodoc.com/presentation_image_h/17cea5a88405f250e71f8cc54ef91e60/image-33.jpg)
Therapeutic ACh Compounds • Cholinesterase inhibitors (donepezil; rivastigmine; galanthamine) • increase brain [ACh]; improves memory, attention in Alzheimer’s dis. • [organophosphorus insecticides (e. g. Malathion) and nerve gas (Sarin)] • Muscarinic antagonists • orphenadrine, procyclidine, others - tremor in Parkinson’s disease • scopolamine - pre-anesthesia • Muscarinic agonists • pilocarpine - glaucoma; • (experimental for Alzheimer’s disease) • Nicotinic agonists (nicotine) • improves memory; addictive (via DA) • Nicotinic neuromuscular blocking agents • tubocurarine; pancuronium, others - surgical paralysis
- Slides: 33