Monitoring in Critical Care Dr AbdulMonim Batiha General

Monitoring in Critical Care Dr. Abdul-Monim Batiha

General Guidelines n n n Monitoring ensures rapid detection of changes in the clinical status Allows for accurate assessment of progress and response to therapy When clinical signs and monitored parameters disagree, assume that clinical assessment is correct Trends are generally more important than a single reading Use non-invasive techniques when possible Alarms are crucial for patient safety
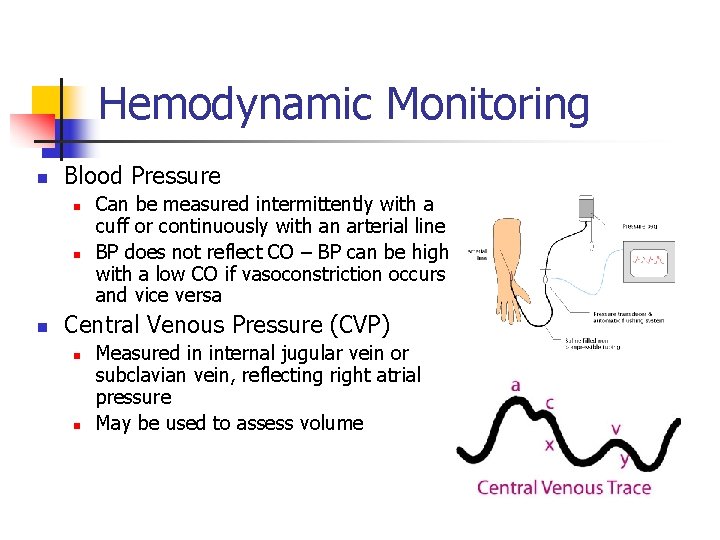
Hemodynamic Monitoring n Blood Pressure n n n Can be measured intermittently with a cuff or continuously with an arterial line BP does not reflect CO – BP can be high with a low CO if vasoconstriction occurs and vice versa Central Venous Pressure (CVP) n n Measured in internal jugular vein or subclavian vein, reflecting right atrial pressure May be used to assess volume

Hemodynamic Monitoring, cont… n Pulmonary Artery Wedge Pressure (PAWP) n n n Cardiac Output (CO) n n n Reflects left atrial pressure Normal is 6 -12 mm Hg Usually measured by thermodilution PA catheter Can also be measured by dye dilution, transesophageal Doppler, echo, or impedence plethysmography EKG n Monitors rate and rhythm of heart

Respiratory Monitoring n ABG n n Monitors acid-base balance, Pa. O 2, and Pa. CO 2 Oxygen Saturation n Sp. O 2, using a finger or other probe, measures the proportion of saturated to desaturated hemoglobin Requires adequate perfusion for accuracy Oxygenatio is OK if Sp. O 2 >90%

Respiratory Monitoring, cont… n Mixed venous O 2 saturation (Sv. O 2) n n Measured with PA catheter Normal is 65 -75% Low Sv. O 2 may indicate inadequate tissue O 2 delivery (even if arterial O 2 is OK) Lung Function n n Aa gradient and Pa. O 2/Fi. O 2 ratio measure the adequacy of gas exchange Arterial to end-tidal CO 2 gradients indicate the adequacy of ventilation PF, FEV 1, and FVC help assess patients with lung dx MIP/NIF is used to determine readiness for extubation

Respiratory Monitoring, cont… n Respiratory compliance n n Vt/PIP-PEEP A measure of the ease of inflation High airway pressures during mechanical ventilation may be caused by low compliance Capnography n n End-tidal CO 2 concentration is close to artrial Pa. CO 2 levels Indicates the adequacy of alveolar ventilation

Organ and Tissue Oxygenation n Global measures n n n Reflect the adequacy of total tissue perfusion but could be normal with local perfusion abnormalities Increased lactate concentration and metabolic acidosis suggests anaerobic metabolism and inadequate tissue oxygenation…lactate also increases with liver failure and sepsis, though Sv. O 2 <55% indicates global tissue hypoxia

Organ and Tissue oxygenation n Organ-specific Measures n Urine flow n n n A sensitive indicator of renal perfusion provided the kidneys aren’t damaged Normal is 1 ml/kg Core-peripheral temperature n n The gradient between peripheral (skin) temp and core (rectal) is often used as an index of peripheral perfusion The less perfusion, the colder the periphery

Organ and Tissue Oxygenation n Organ-specific Measures n Gastric tonometry n n Used to detect shock-induced splanchnic ischemia by measure gastric luminal PCO 2 and deriving the mucosal p. H Neurological monitoring n Utilizes GCS, ICP measurement, and jugular venous bulb saturation
- Slides: 10