Monitoring in Anesthesia Medical Student Lecture Series Introductory












- Slides: 16

Monitoring in Anesthesia Medical Student Lecture Series Introductory Anesthesiology Clerkship Canvas Department of Anesthesiology University of Minnesota

Objectives • Understand the American Society of Anesthesiology Standard Monitors • Understand what organ systems/ functions need to be monitored • Gain a basic appreciation of what information monitors provide and how this information is obtained

ASA Standard Monitors • Pulse Oximetry • Non-invasive and invasive BP • ECG • Capnography • Temperature

Standards for Basic Anesthetic Monitoring • Oxygenation Adequate O 2 concentration in the inspired gas AND blood. - Inspired gas Oxygen analyzer WITH a low O 2 concentration limit alarm in use, to measure the Fi. O 2 in the breathing system - Blood oxygenation Pulse oximetry with variable tone and low threshold alarm

Standards for Basic Anesthetic Monitoring • Ventilation Chest excursion, fogging of mask/endotracheal tube, inflation/ deflation of the breathing bag, breath sounds Capnography (monitors end-tidal CO 2) Monitors end-tidal CO 2 (capnography) Monitors volume of expired gas (tidal volume) Features alarm that detects breathing circuit disconnection

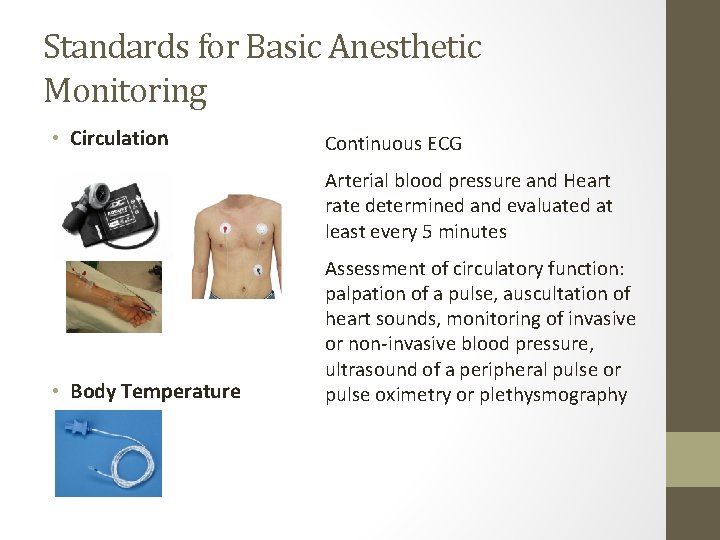
Standards for Basic Anesthetic Monitoring • Circulation Continuous ECG Arterial blood pressure and Heart rate determined and evaluated at least every 5 minutes • Body Temperature Assessment of circulatory function: palpation of a pulse, auscultation of heart sounds, monitoring of invasive or non-invasive blood pressure, ultrasound of a peripheral pulse or pulse oximetry or plethysmography

Pulse Oximetry • Measures two wavelengths: 660 nm red light (well absorbed by oxyhemoglobin) and 940 nm, infrared light (well absorbed by deoxyhemoglobin) • Provides information about: • Hear rate (beats per minute) • Heart rhythm (regular, irregular) • Oxygenation (sp. O 2)

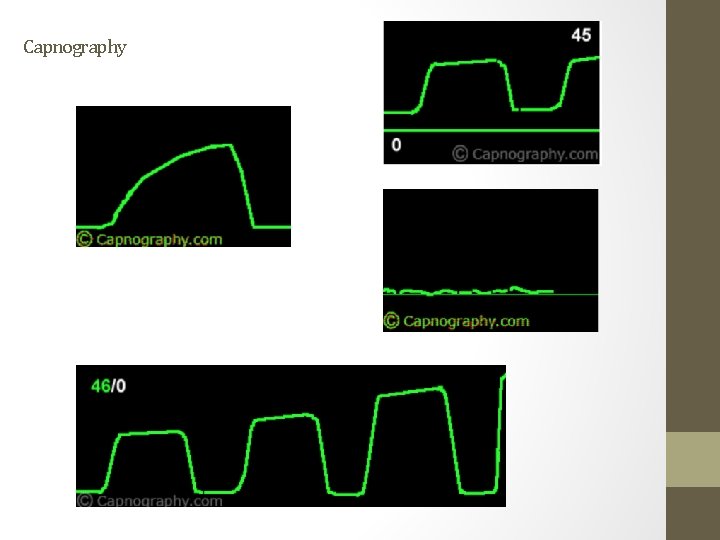
Capnography To determine if ventilation is, in fact, taking place Estimator of Pa. CO 2 Dead space assessment Sustained CO 2 waveform > 30 mm. Hg confirms tracheal placement of an ETT • Esophageal intubation may give a waveform that quickly vanishes (within 3 TV breaths) and will become flat • May be used during cardiopulmonary resuscitation to ensure adequate chest compressions (ETCO 2 should be >20 mm. Hg) • •

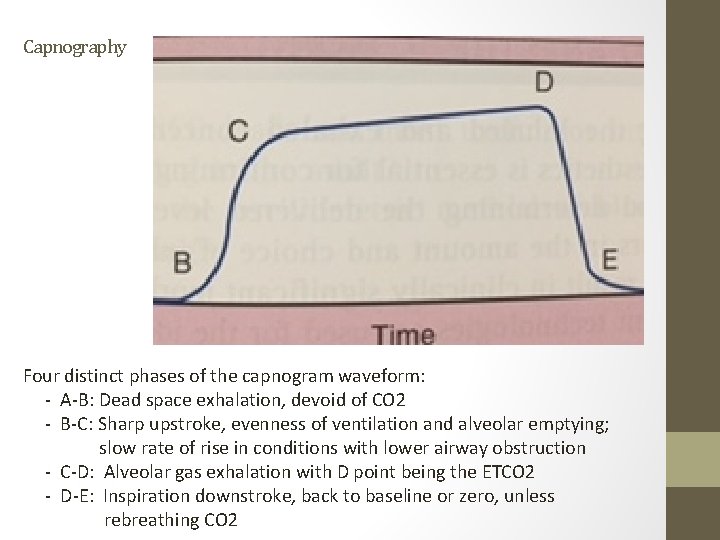
Capnography Four distinct phases of the capnogram waveform: - A-B: Dead space exhalation, devoid of CO 2 - B-C: Sharp upstroke, evenness of ventilation and alveolar emptying; slow rate of rise in conditions with lower airway obstruction - C-D: Alveolar gas exhalation with D point being the ETCO 2 - D-E: Inspiration downstroke, back to baseline or zero, unless rebreathing CO 2

Capnography

NIBP • In the past, frequently performed manually using a stethoscope • In perioperative period, automatic non-invasive blood pressure cuffs are used (oscillometric method) • Blood pressure cuff size is important • Width should be 40% of arm circumference • If too small: measured BP is too high • If too large: measured BP is too low

Direct Arterial Pressure Monitoring • Direct BP monitoring: Invasive measurement by placing a catheter in a peripheral artery which is connected to a transducer system and display. • Indications: CPB, wide swings in BP are expected, when rigorous control of BP is required, need of frequent analysis of ABG’s • Possible cannulation sites: - Radial, Ulnar, Axillary, Brachial, Femoral, Dorsalis Pedis, Posterior Tibial

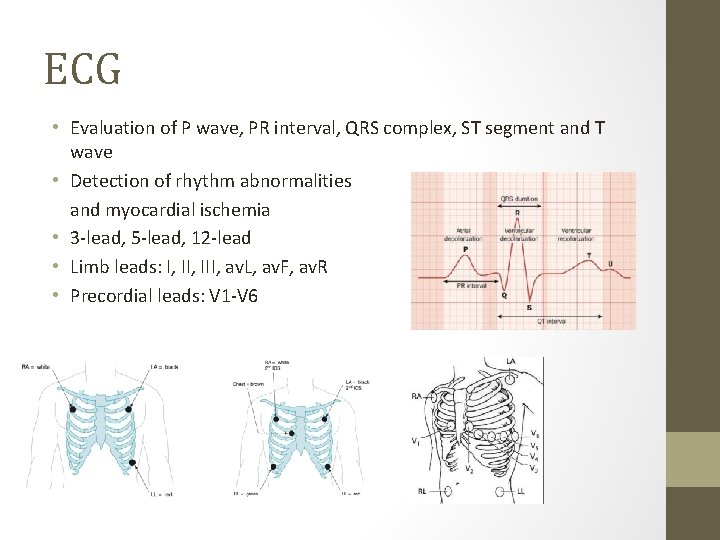
ECG • Evaluation of P wave, PR interval, QRS complex, ST segment and T wave • Detection of rhythm abnormalities and myocardial ischemia • 3 -lead, 5 -lead, 12 -lead • Limb leads: I, III, av. L, av. F, av. R • Precordial leads: V 1 -V 6

Temperature monitoring • Decreases in body temperature are frequent during surgical procedures related to • • Radiation Conduction Convection Evaporation • Effects of hypothermia: delayed recovery from anesthesia; shivering, increases O 2 consumption, dysrhythmias, impairment of coagulation and wound healing • Possible monitoring sites: esophageal, nasopharyngeal, tympanic, oral, bladder, rectal, skin

Neuromuscular monitoring • Peripheral nerve stimulator (“twitch monitor”) is used to monitor depth of neuromuscular blockade (paralysis) when non-depolarizing neuromuscular blockers are being used (rocuronium, vecuronium, cis-atracurium) • “Train of Four”: nerve stimulator applies 4 stimuli and measures the muscular response • Aim for TOF ratio of at least 0. 9 for extubation

Other monitors that may be used • Central Venous Catheter • Pulmonary artery catheter • Echocardiography (TEE) • Evoked Potentials (SSEP, MEP, visual and auditory) • Brain Electrical Activity Monitoring (BIS) • Cardiac Output Monitoring • Intracranial Pressure Monitoring • Cerebral Oximetry