Monitoring in Anesthesia Done by Heba Abu Khalaf

Monitoring in Anesthesia Done by : Heba Abu Khalaf

Objectives • 1. Guidelines to the practice of anesthesia and patient monitoring • 2. Anesthesia depth • 3. Elements to monitor ( Oxygenation, Ventilation, Circulation, Temperature) • • 2. 1. ECG 2. 2. Pulse Oximetry 2. 3. Blood Pressure 2. 4. central venous line and pressure 2. 5. Capnography and Et. CO 2 2. 6. How to identify Cyanosis 2. 7. The oxyhemoglobin dissociation curve 3. Normal values for a healthy adult undergoing anesthesia

Guidelines to the practice of anesthesia and patient monitoring: • 1. an anesthetist present: “the only indispensable monitor” The doctor should present in the room & monitor the conduct of all general or regional anesthetics • 2. A completed pre-anesthetic checklist. • (ASA class, Hx &physical exam, investigations, NPO policy )

Con’t. . . • 3. perioperative anesthetic record: HR and BP every 5 min, O 2 saturation, End Tidal CO 2, dose and route of drugs and fluids • 4. continuous monitoring: patient’s oxygenation, ventilation, circulation and temperature.
Elements to Monitor : • I. Anesthetic Depth: • Patients with local or regional anesthesia provide verbal feedback regarding well being. • • Onset of general anesthesia signaled by lack of response to verbal commands, in addition to loss of blink reflex to light touch. • Inadequate anesthesia can be signaled by : Facial grimacing or movement of arm or leg. //blink reflex present when eyelashes lightly touched, • But with muscle relaxants ( fully paralysis), it can be signaled by : Hypertension, tachycardia, tearing or sweating. { Due to pain }

Con’t. . . • Excessive anesthesia can be signaled by : Cardiac depression, bradycardia, and Hypotension. also may result in hypoventilation, hypercapnia and hypoxemia when muscle relaxants is not given.

2. Oxygenation >> inspired Oxygen • we monitor it Clinically through observation of patient / skin color also by : • 1) pulse oximetry ( Sa. O 2 ) • 2) Blood gas analysis ( Pao 2 ) • 3) fraction of inspired O 2 (Fi. O 2) • Quantitavely monitored by using oxygen analyzer, equipped with an audible low oxygen concentration alarm.

• Pulse Oximetry: • ** mandatory monitor for any anesthetic , , including cases of moderate sedation • **measure { non invasively} pt’s Sp. O 2 ( arterial oxy saturation) • And blood flow fluctuation by plethysmograph (waveform of pulse oximeter “arterial waveform “ >> indicates that pulse oximeter is reading the arterial oxy saturation

• Technique >> sensor containing light sources (Red and Infra-red light) & light detector is placed across finger tip , toe , earlobe or any other perfused tissue that can be transillumintaed • processing >>analyze amount of light absorbed by the 2 wavelengths, , then determining concentrations of oxygenated and deoxygenated forms through only arterial blood • light absorption is differ between oxy. Hb and deoxy. Hb. • analysis of oxygenation in each beat

Also it provides an indication of tissue perfusion & measure heart rate • Inaccurate measurements , , causes of oximetry artifact : • 1) poor tissue perfusion (shock & hypotension) • 2) movement • 3)dysrhythmias • 4) hypothermia ( cold extremities ) • 5) cardiac arrest • • Pulse oximetry (Sp. O 2) measures oxy-, deoxy-, met-, and carboxy. Hb.

• Pulse oximetry is never used for rapid diagnosis of hypoxia ( that may occur in unrecognized esophageal intubation ) • It used for monitoring oxygen delivery to vital organs • Also in recovery room , it helps identify post op pulmonary problems such as hypoventilation / bronchospasm / atelactasis • So timing of Spo 2 monitoring >> before intubation , through the surgery , , after extubation & recovery

• Pulse oximeter tone changes with desaturation from high to low(deep) sound • So just by listening to the monitor , , you can recognize the • 1) HR. 2) O 2 saturation • Healthy patient under GA (O 2= 100%) >> Spo 2 96 -100%

• Rules : • # pay attention to the sound of pulse oximetry • # Always remember that your clinical judgment is much more superior to the monitor , , check pt’s color for cyanosis , , lips , , nails

4. Temperature • ** should be monitored for patients under anesthesia • ** post op temp. >> used as quality anesthesia indicator • ** hypothermia associated with : • 1) delay drug metabolism, 2) impaired coagulation • ** hyperthermia has bad effects peri operatively leading to : • 1) tachycardia 2) vasodilation 3) neurological injury • So temp. Must be measured & recorded peri operatively

• Hypothermia (<36°C) • Normal heat loss during anesthesia averages 0. 5 - 1 C per hour, but usually not more that 2 -3 C • Temperature below 34 C may lead to significant morbidity • Hypothermia develops when thermoregulation fails to control balance of metabolic heat production and environment heat loss • Normal response to heat loss is impaired during anesthesia • • Those at high risk are elderly, burn patients , spinal cord injuries

• Causes of Hypothermia (<36°C) • **intraoperative temperature losses are common (e. g. 90% of intraoperative heat loss is transcutaneous) • >> due to: • 1) OR environment (cold room, IV fluids, instruments) • 2) open wound • ## prevented with forced air warming blanket and warmed IV fluids

• Impact of Hypothermia • 1) Increased risk of wound infections >> due to impaired immune function • 2) Increases the period of hospitalization by delaying healing • • 3) Reduces platelet function and impairs activation of coagulation cascade increasing blood loss and transfusion requirements • 4) Decreases the metabolism of anesthetic agents prolonging postoperative recovery

• Causes of Hyperthermia (>37. 5 -38. 3ºC) • 1) malignant hyperthermia • 2) drugs (e. g. atropine) • 3) blood transfusion reaction • 4) infection/sepsis • 5) • Increases in metabolic rate secondary to: • –Thyrotoxicosis • –Pheochromocytoma • 6) Excessive environmental warming

• Continuous temperature measurements monitoring (Thermometry) is mandatory if changes in temperature are suspected. • ** intra op , , temp measured by thermistor or thermocouple • Monitoring sites : • >> esophagus • >> tympanic membrane • >> nasopharynx. • >> Peripheral sites axilla & rectal.

2. Ventilation • Clinically, monitored through a correctly positioned endotracheal tube, also observing chest expansion and breath sounds over both lungs. • • Quantitavely by ETCO 2 analysis, equipped with an audible disconnection alarm. • • Arterial blood gas analysis for assessing both oxygen and ventilation.
3. Circulation • Clinically monitored by pulse palpation, heart auscultation & monitoring intra-arterial pressure (MAP normally between 70 - 100 mm. Hg) or oximetry. • Quantitively using ECG & blood pressure measurements every 5 min.
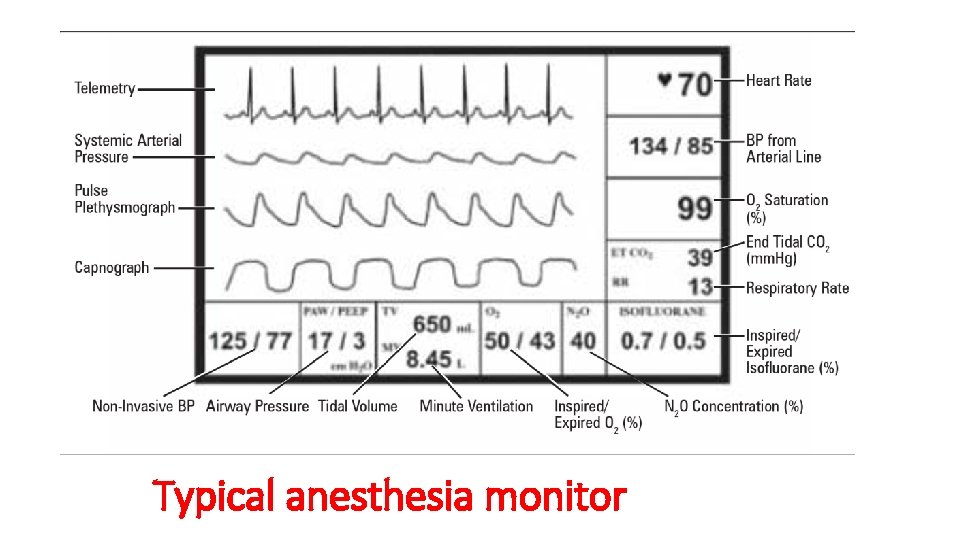
Typical anesthesia monitor

Always remember that your clinical judgment is much more superior to Any monitor • monitor is present to help you not to be ignored and not to cancel you brain.

Thank You
- Slides: 24