Monitoring and Evaluation of MDR TB Kstutis Mikinis

Monitoring and Evaluation of MDR TB Kęstutis Miškinis, Medical officer, WHO Ukrainian country office

What is multidrug-resistant tuberculosis (MDR-TB)? • TB bacilli resistant to at least two of the most powerful anti-TB agents: isoniazid and rifampicin; • One of the main aims of any national TB program is to minimize the development of drug (multidrug) resistance;

Effectiveness of National TB Programme • High cure rate of new TB cases; • Low (and constantly decreasing) MDR-TB rate; • Ultimately, high case-detection rate; Potential criteria: • Ability to analyze cohort data; • Default and transfer rates less than 10%; • Continual supply of 1 st line anti-TB drugs; • Application of DOT in 90% of all cases;

Effectiveness of National TB Programme (con’t. ) • Surveillance of anti-TB drug resistance is an essential tool for monitoring the effectivness of TB control programme in any country; • The use of drug-sensitivity tests (DST) was recommended many years ago;

Cause of anti-TB drug resistance • (M)DR-TB is man-made! Naturally drugresistant organisms arising through spontaneous mutations are selected by inadequate drug regimens; • Reasons – exposure to a single drug due to: ü Poor adherence; ü Inappropriate prescription; ü Irregular drug supply; ü Poor drug quality;

MDR-TB • Problems: • longer to treat (up to 24 months); • more expensive (up to 100 x); • more side-effects; • demanding follow-up mechanism; • requires complex diagnostics;
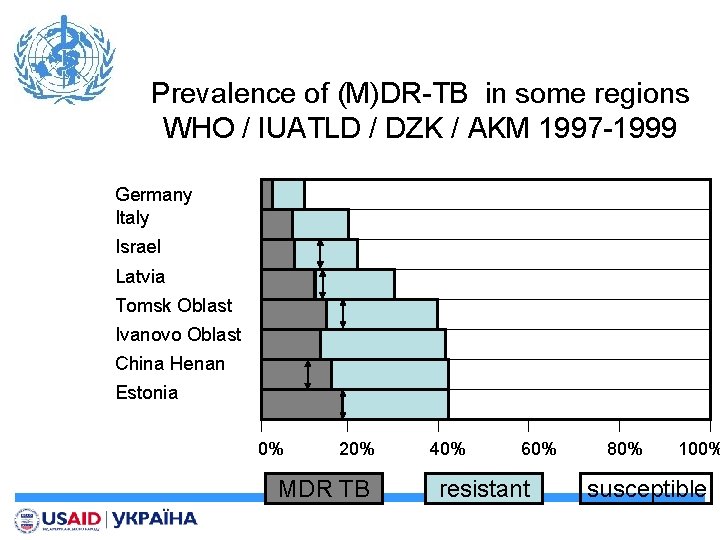
Prevalence of (M)DR-TB in some regions WHO / IUATLD / DZK / AKM 1997 -1999 Germany Italy Israel Latvia Tomsk Oblast Ivanovo Oblast China Henan Estonia 0% 20% MDR TB 40% 60% resistant 80% 100% susceptible
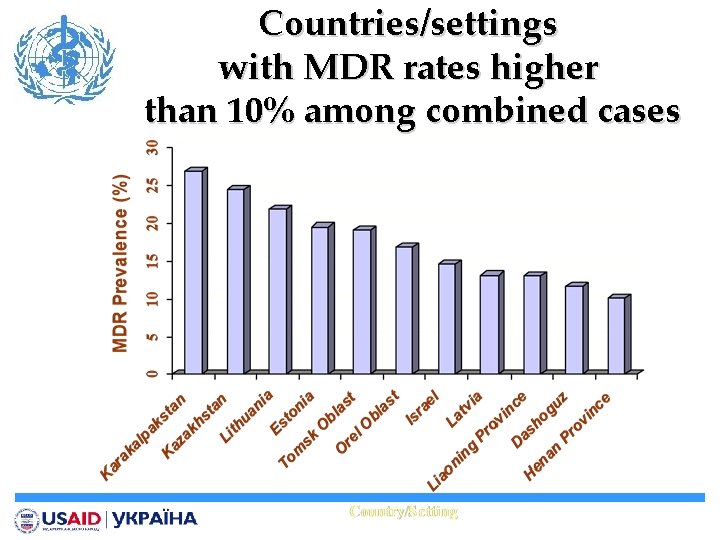
Countries/settings with MDR rates higher than 10% among combined cases
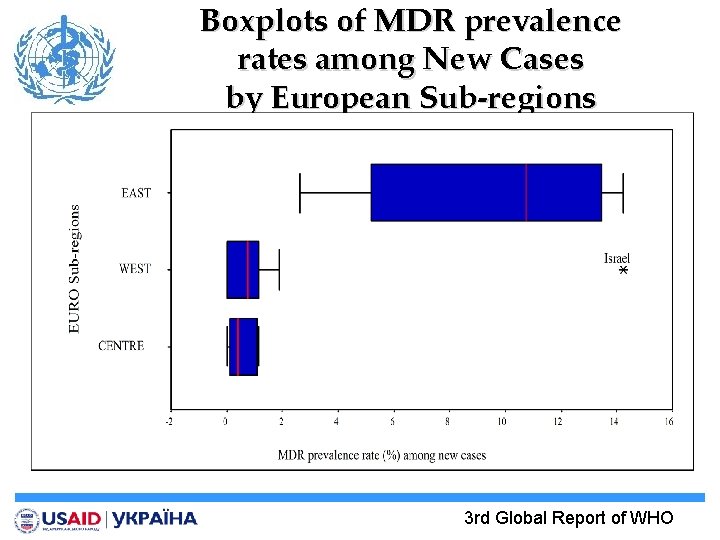
Boxplots of MDR prevalence rates among New Cases by European Sub-regions 3 rd Global Report of WHO
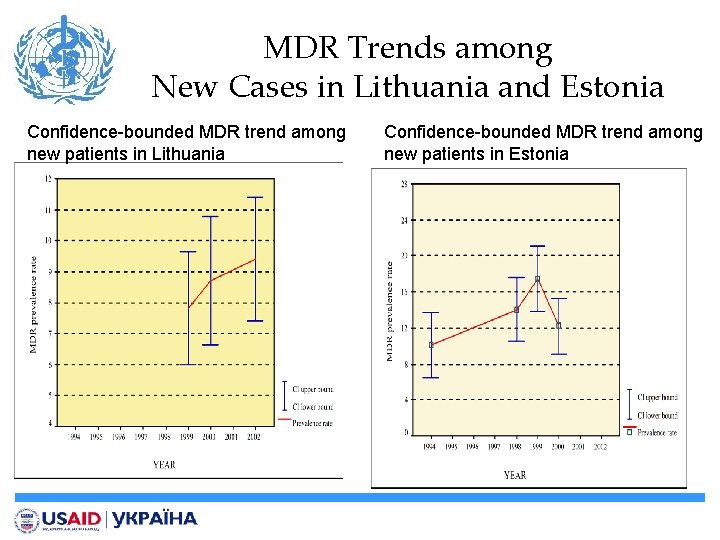
MDR Trends among New Cases in Lithuania and Estonia Confidence-bounded MDR trend among new patients in Lithuania Confidence-bounded MDR trend among new patients in Estonia

Establishment of drug-resistance surveillance system • The sample of specimens should be representative of the TB patients; • The patient’s history should be carefully obtained (available to determine whether the patient has previously received anti-TB drugs); • The laboratory methods should meet internationally recommended standards;

DST methods • Proportion; • Resistance ratio; • Absolute concentration; • BACTEC 460 radiometric; Comparability of data is assured by: • Quality assurance; • Proficiency testing performed by Supranational Reference Laboratories

Choice of drugs Four out of six 1 st line drugs: • Isoniazid (H); • Rifampicin (R); • Streptomycin (S); • Ethambutol (E); Why these four? • Widely used; • Resistance can be reliably measured by standardized techniques;

Definitions of resistance • Resistance among previously treated cases (having been treated for tuberculosis for one month or more); • Resistance among new TB cases (denies having had prior anti-TB treatment); • Multi-drug resistance;

National Reference Laboratory Is a reference institution on MDR surveillance. It: • Prepares cultures; • Undertakes identification of Mycobacteria; • Undertakes DST; • Ensures quality of DST performed by regional labs; • Establishes a regular “on-site” supervision;

Organizing of surveillance • Laboratories and diagnostic centers; • Sample size and sampling strategies; • Organization and survey outline (preparation, sampling, training, logistics); • Intake of patients (inclusion criteria, sputum-collection, registration, transport); • National Reference laboratory; • Data management and analysis;

Ukraine • NRL is established, but not functioning; • QA is not implemented; • Proficiency testing hasn’t started yet; • Laboratory standards are defined, but not strictly followed; • Equipment is poor, purchase of new equipment and necessary supplies is often delayed; • Staff needs retraining and rejuvenation;

Trends in Anti-TB-Drug. Resistance in Ukraine Feshchenko et al. , Ukraine Chemotherapeutical Journal, 2000/3 Year No of Isolates Number of stains tested susceptible % Number of strains % with resistance(s) 1990 748 400 53, 5 348 46, 5 1991 799 419 52, 4 380 47, 6 1992 839 437 52, 1 402 47, 9 1993 1051 534 50, 8 517 49, 2 1994 762 387 50, 8 375 49, 2 1995 814 393 48, 3 421 51, 7 1996 744 366 49, 2 378 50, 8 1997 731 359 49, 1 372 50, 9 1998 957 432 45, 1 525 54, 9 1999 961 372 38, 7 589 61, 3
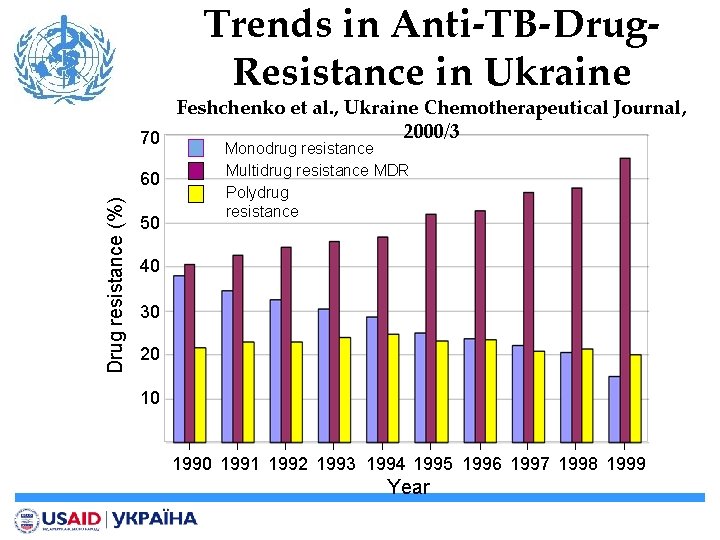
Trends in Anti-TB-Drug. Resistance in Ukraine Feshchenko et al. , Ukraine Chemotherapeutical Journal, 2000/3 70 Monodrug resistance Drug resistance (%) 60 50 Multidrug resistance MDR Polydrug resistance 40 30 20 10 1991 1992 1993 1994 1995 1996 1997 1998 1999 Year
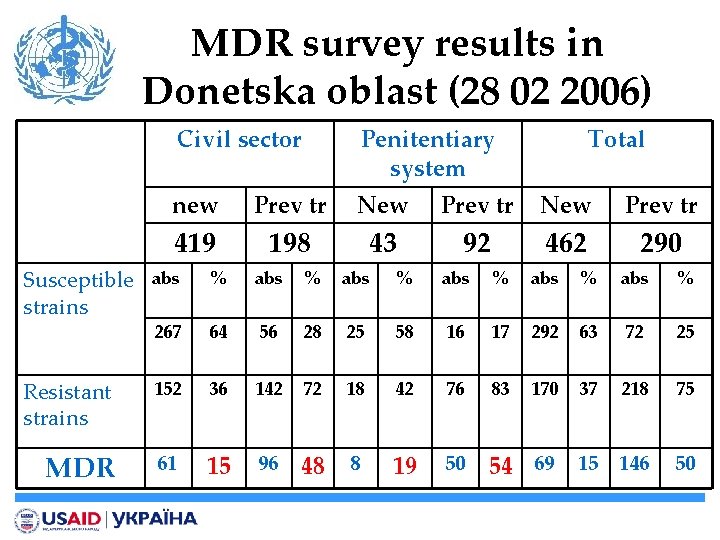
MDR survey results in Donetska oblast (28 02 2006) Civil sector Penitentiary system new Prev tr New Prev tr 419 198 43 92 462 290 Susceptible abs strains Total % abs % abs % 267 64 56 28 25 58 16 17 292 63 72 25 Resistant strains 152 36 142 72 18 42 76 83 170 37 218 75 MDR 61 15 96 48 8 19 50 54 69 15 146 50

Drug Resistance Surveillance • Magnitude and trend of drug resistance prevalence among new and re-treatment cases; • Useful parameter to evaluate current and past treatment programme; • Useful information for selection of effective initial treatment and retreatment regimens;

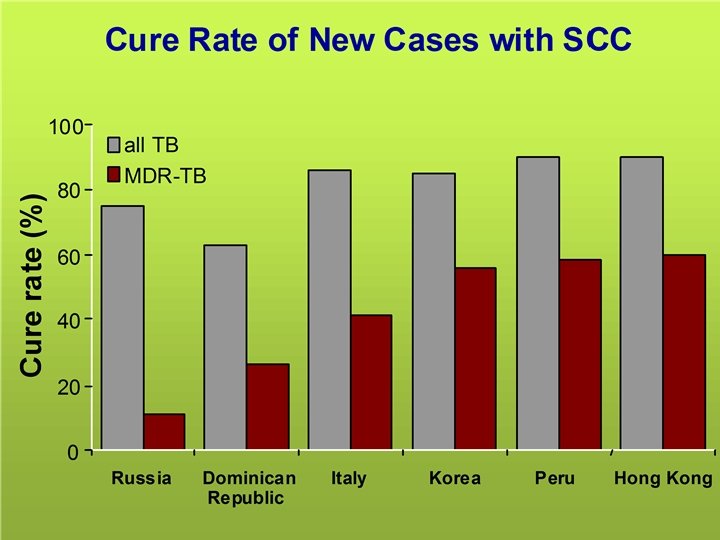
Should we treat persons with MDR-TB? • Yes…for humanitarian reasons • But health policy is not only driven by values, facts also matter No. . . unless it is proven that it is feasible and cost-effective • But can we afford not to respond?

DOTS-Plus: working definition • DOTS-Plus is a case-management strategy under development designed to manage MDR-TB using 2 nd line drugs within the DOTS strategy in low- and middle-income countries; DISCLAIMER: DOTS-Plus means DOTS first

Prevention of MDR TB Correct operations of the TB programme: • Diagnosis based on bacteriological examination; • Standard treatment under strict observation (DOT); • Uninterrupted supply of good-quality TB drugs (recommended FDC); • Proper recording and reporting;
- Slides: 25