Molecular epidemiology of multidrug resistant tuberculosis in Mongolia

Molecular epidemiology of multi-drug resistant tuberculosis in Mongolia Ulziijargal Gurjav Sydney Medical School, The University of Sydney
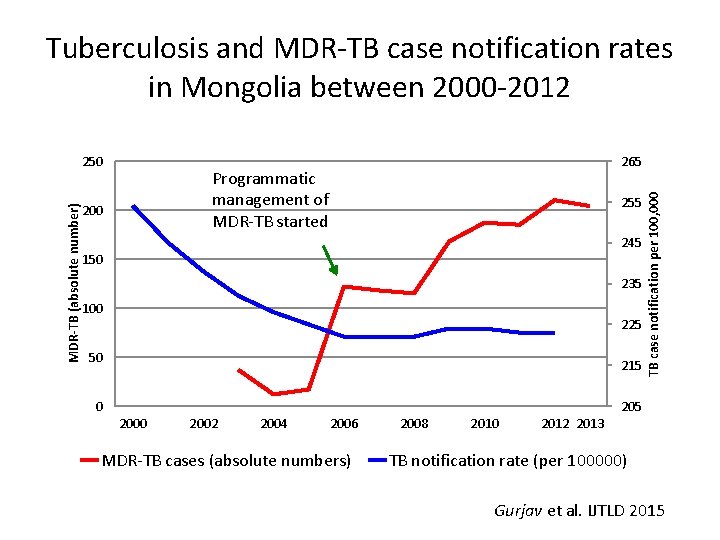
Tuberculosis and MDR-TB case notification rates in Mongolia between 2000 -2012 265 Programmatic management of MDR-TB started 200 255 245 150 235 100 225 50 215 0 TB case notification per 100, 000 MDR-TB (absolute number) 250 205 2000 2002 2004 2006 MDR-TB cases (absolute numbers) 2008 2010 2012 2013 TB notification rate (per 100000) Gurjav et al. IJTLD 2015
![Tuberculosis incidence rate in Australia Department of Health, Australia [www. health. gov. au] Tuberculosis incidence rate in Australia Department of Health, Australia [www. health. gov. au]](http://slidetodoc.com/presentation_image_h/fa7e03914a639f0a9a31811a0284141a/image-3.jpg)
Tuberculosis incidence rate in Australia Department of Health, Australia [www. health. gov. au]
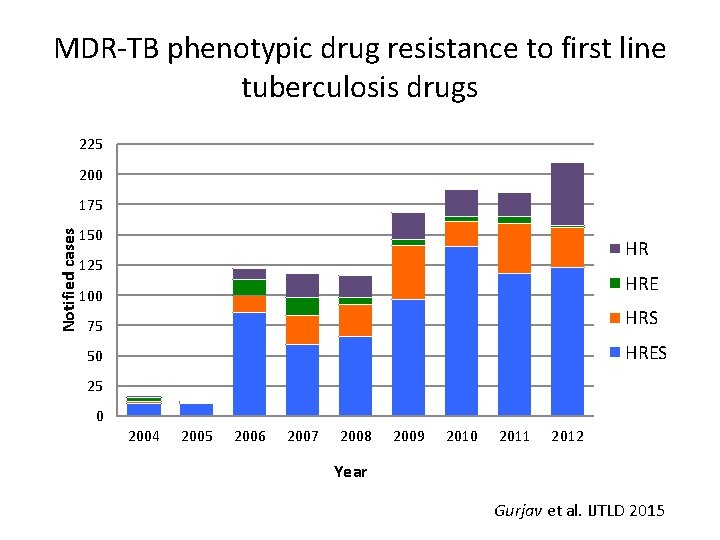
MDR-TB phenotypic drug resistance to first line tuberculosis drugs 225 200 Notified cases 175 150 HR 125 HRE 100 75 HRS 50 HRES 25 0 2004 2005 2006 2007 2008 2009 2010 2011 2012 Year Gurjav et al. IJTLD 2015
2004 2005 2006 2007 2008 2009 2010 2011 2012 Gurjav et al. IJTLD 2015
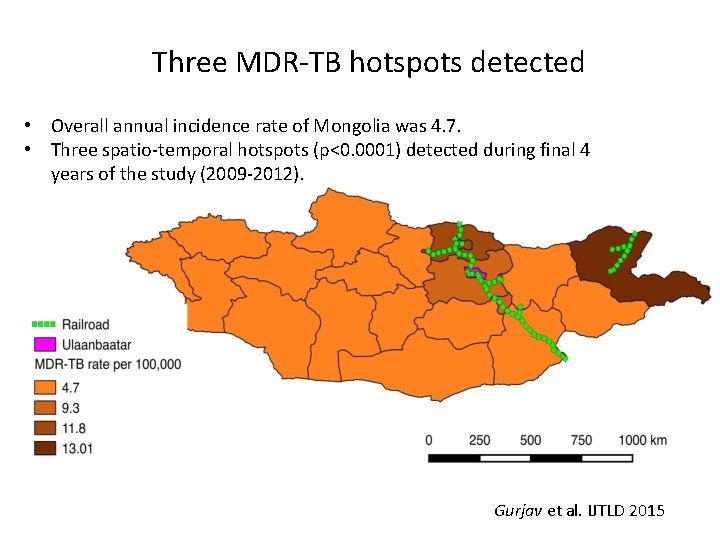
Three MDR-TB hotspots detected • Overall annual incidence rate of Mongolia was 4. 7. • Three spatio-temporal hotspots (p<0. 0001) detected during final 4 years of the study (2009 -2012). Gurjav et al. IJTLD 2015
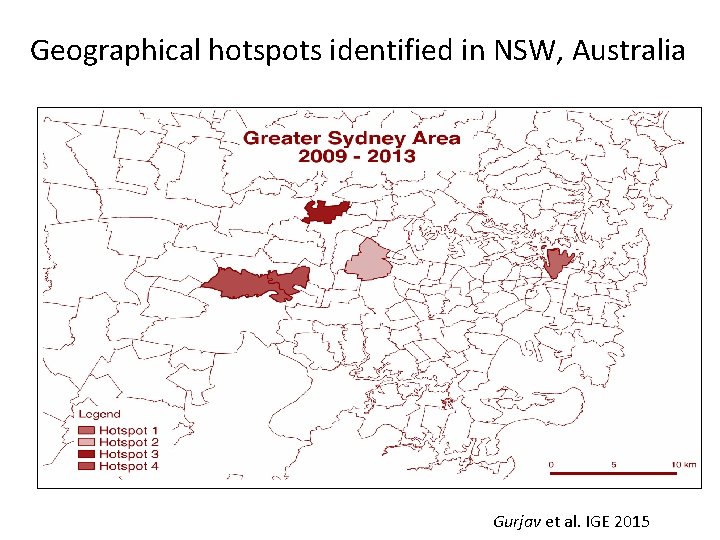
Geographical hotspots identified in NSW, Australia Gurjav et al. IGE 2015

MIRU typing revealed possible high local transmission of MDR-TB • Mycobacterium tuberculosis isolates collected during 2012 indicated that 42% (28/66) of MDR-TB cases clustered by 24 -loci mycobacterium interspersed repetitive unit (MIRU) typing. – – Beijing 86. 4% (57/66) LAM 7. 6% (5/66) Haarlem 4. 5% (3/66) New-1 1. 5% (1/66) Clustered 61. 4% (35/57) Clustered 40% (2/5) Gurjav et al. Tuberculosis 2016

Minimum spanning tree of Beijing lineage strains isolated from (regimen 1) treatment failed MDR-TB patients diagnosed during 2012 Single loci difference Two locus difference Three locus difference More than 4 locus difference *24 -loci MIRU used to create the tree and 3 largest nodes include 7 -15 isolates; Gurjav et al. Tuberculosis 2016

Summary of MDR-TB molecular epidemiology of Mongolia • The MDR-TB incidence in Mongolia is high and has not shown any decline, despite PMDT implementation since 2006 • Among MDR-TB cases, resistance to all first line drugs is high (>60%) • Clear spatial expansion of MDR-TB is observed across the country • Three MDR-TB hotspot areas are identified in provinces that are traversed by Trans-Siberian Railroad • Mongolian National Tuberculosis Program (NTP) needs to scale up its MDR-TB case detections and interventions in these hot spot areas.

Acknowledgement The University of Sydney Assoc. Prof. Vitali Sintchenko Assoc. Prof. Ben Marais Dr. Grant Hill-Cawthorne Nadine Mc. Callum Mycobacterium Reference Laboratory, NSW, Australia Peter Jelfs Andrea Bustamante Basil Suliman Fangrong Kong Funding: TB-CRE Grant 2013 -2016 Marie Bashir Institute
- Slides: 11