Module Health Psychology Lecture Health Behaviours and Beliefs

Module: Health Psychology Lecture: Health Behaviours and Beliefs Date: 26 January 2009 Chris Bridle, Ph. D, CPsychol Associate Professor (Reader) Warwick Medical School University of Warwick Tel: +44(24) 761 50222 Email: C. Bridle@warwick. ac. uk www. warwick. ac. uk/go/hpsych

Aims and Objectives n n Aim: To provide an overview of the psychological determinants of health-related behaviours and beliefs Objectives: The student should be able to provide a basic description of the … n n meaning of health-related behaviours, and provide examples of different types of health behaviour psychological processes that influence health behaviours and a framework for their organisation common psychological components of health behaviour theories core constructs relevant to understanding, predicting and changing health-related behaviours
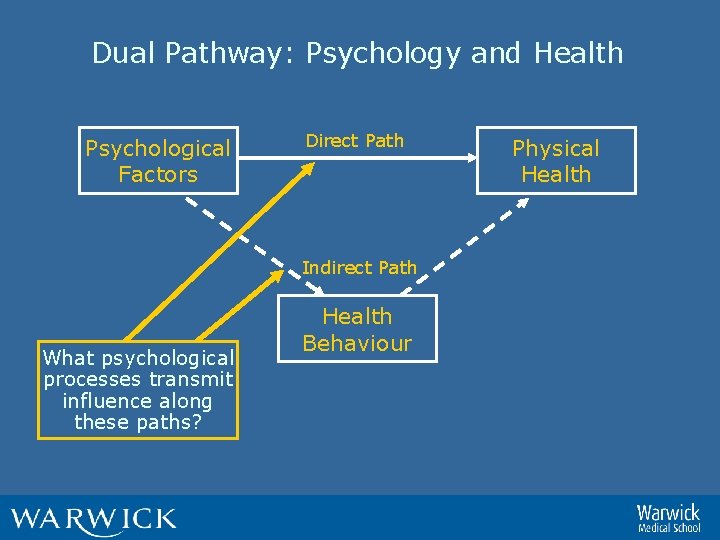
Dual Pathway: Psychology and Health Psychological Factors Direct Path Indirect Path What psychological processes transmit influence along these paths? Health Behaviour Physical Health

Recap n Psychoneuroimmunology (PNI) n Physiological reactivity = mechanism of action n Stress & negative affect = influence being transmitted n Interpretation = process generating the influence n Negative physical effects = chronic stable exposure
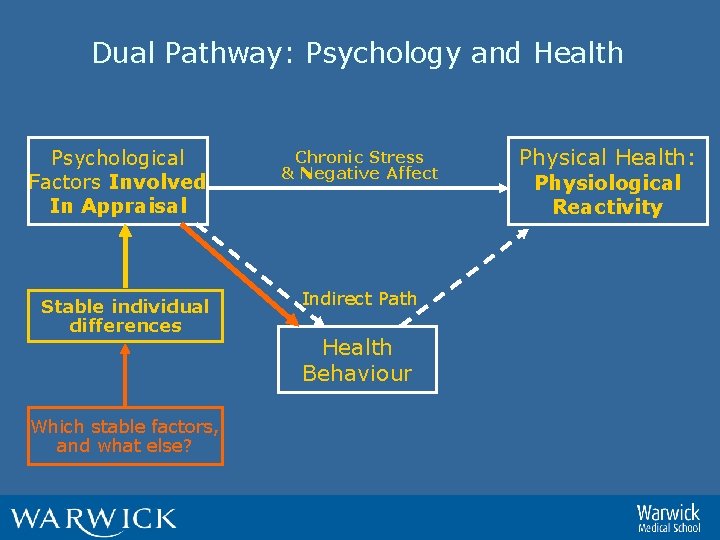
Dual Pathway: Psychology and Health Psychological Factors Involved In Appraisal Stable individual differences Which stable factors, and what else? Chronic Stress & Negative Affect Indirect Path Health Behaviour Physical Health: Physiological Reactivity
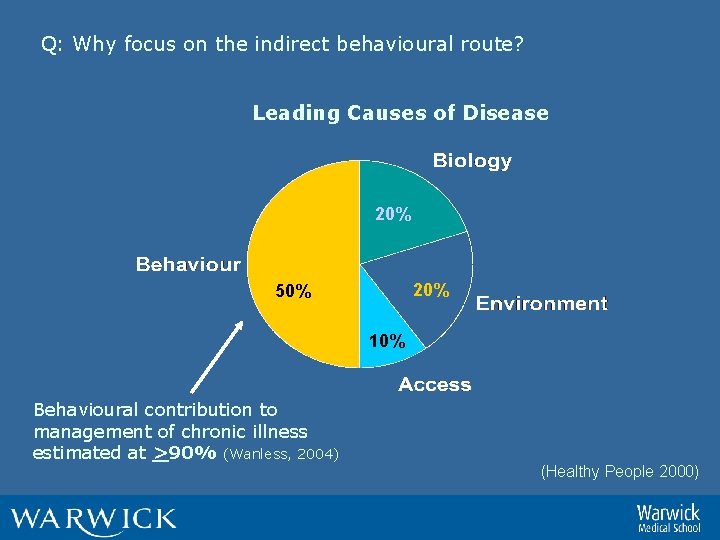
Q: Why focus on the indirect behavioural route? Leading Causes of Disease 20% 50% 10% Behavioural contribution to management of chronic illness estimated at >90% (Wanless, 2004) (Healthy People 2000)

Key Questions n What psychological factors influence health behaviour? n n n What do we know about the determinants of health behaviour? To what extent are we able to sufficiently explain and predict health behaviour? Can our understanding of psychological processes be used to change health behaviour? n Will interventions that change health behaviour yield benefits for physical health?

Defining Behaviour n Behaviour: the actions or reactions of an individual to a situation – can be conscious or unconscious, voluntary or involuntary n But … what specifically? Health behaviour Illness Adaptive behaviour Maladaptive Prevention behaviour Detection behaviour Public behaviour Service-use behaviours Private Self-care behaviours Health behaviour: Behaviour that may have implications for health

Determinants of Health Behaviour A framework n n Background factors: Characteristics that define the context in which people live their lives; shared understanding and ways of knowing the world Stable factors: Individual differences (personality) in psychological activity that are stable over time and context Social factors: Social connections in the immediate environment; mostly stable, but can be fragile, e. g. when in conflict with background factors Situational factors: Appraisal of personal relevance that shape responses in a specific situation
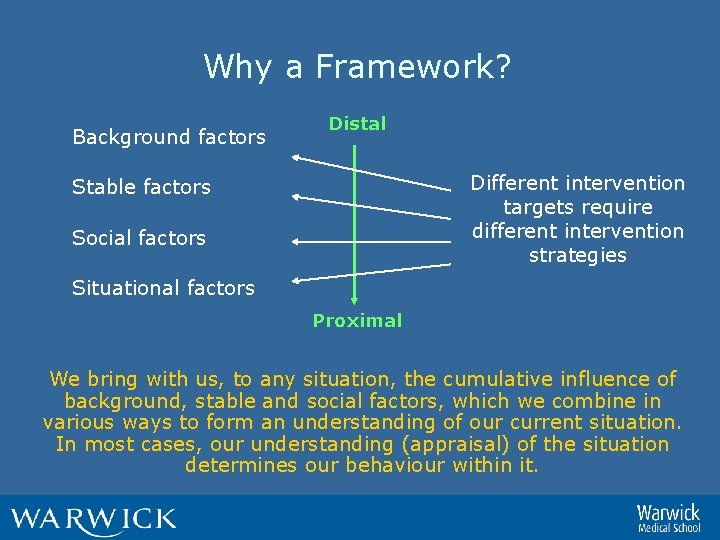
Why a Framework? Background factors Distal Different intervention targets require different intervention strategies Stable factors Social factors Situational factors Proximal We bring with us, to any situation, the cumulative influence of background, stable and social factors, which we combine in various ways to form an understanding of our current situation. In most cases, our understanding (appraisal) of the situation determines our behaviour within it.

Stable Factors n Stable factors: i. e. individual differences, dispositions, personality n Refer to variations, between people, in psychological activities that, within people, produce responses that are stable across time and context n Influence appraisal in three key ways: n n n they determine if, and to what extent, an event is salient, i. e. sensitivity towards particular types of event they provide a generalised framework for understanding and evaluating the event, e. g. as threat or challenge they make available, or suggest, potential responses, i. e. initial response options

Individual Differences and Health n Three broad types of individual differences: n n n Emotional dispositions: Psychological processes involved in both the experience and expression Generalised expectancies: Psychological processes involved in formulating expectations in relation to future outcomes Explanatory styles: Psychological processes involved in explaining the causes of negative events Temporal dimension: Present Future Past

Emotional Dispositions n Negative affect: Tendency toward the experience of negative affective states, e. g. hostility, depression, anxiety n n n Appraisal bias for heightened arousal and increased frequency Evidence for causal role in development of physical disease health behaviour impeded as a function of fatigue and apathy. Emotional expression: The (low) expression of (negative) emotional experience, both unconscious repression and conscious suppression n n Appraisal bias for neutralising threat or extreme intensity, both leading to maladaptive responses Risk factor for recovery (post-MI) and cancer progression

Generalised Expectancies n Locus of control: Expectations that future outcomes will be determined by factors that are either internal (self) or external (powerful others, and chance) n n Internal loci generally associated with more favourable outcomes, and performance of health behaviours, but VERY dependent situational factors Self-efficacy: Belief in one’s own ability to organise and execute a course of action, and the expectation that the action will result in, or lead to, a desired outcome n Heuristic belief in the beneficial effects of higher self-efficacy, deriving from appraisal bias for challenge rather than threat and expectation of success

Explanatory Styles n Optimism (Pessimism): Expectation of positive future outcome (however achieved) despite current negative event n n n Appraisal bias for brief, low levels of physiological reactivity, and promoting active coping responses Optimism, vis-à-vis pessimism, associated with better physical health, illness recovery, and health behaviour performance Attributional style: Causal explanations of negative events as internal (self), stabile (time), and global (situation) n n Generally better if attributions are external, unstable and specific, rather than internal, stable and global Causal attributions influence expectations about controllability of future outcomes, i. e. the relevance of health behaviours

Social Cognition Theories n n Social cognition theories attempt to explain the relationship between social cognitions (e. g. beliefs, attitudes, goals, etc. ) and behaviour Some examples: n Health Belief Model n Protection Motivation Theory of Reasoned Action n Theory of Planned Behaviour n Transtheoretical Model (Rosenstock, 1966) (Rogers, 1975) (Fishbein & Ajzen, 1975) (Ajzen, 1988) (Prochaska and Di. Clemente, 1983)
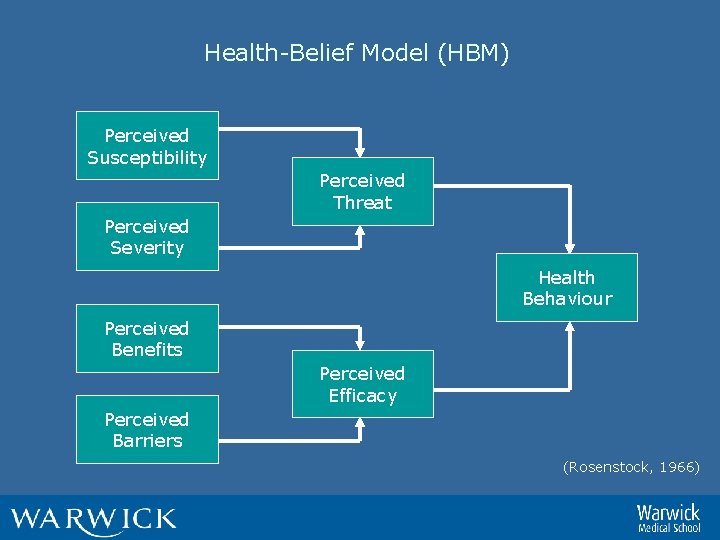
Health-Belief Model (HBM) Perceived Susceptibility Perceived Threat Perceived Severity Health Behaviour Perceived Benefits Perceived Efficacy Perceived Barriers (Rosenstock, 1966)
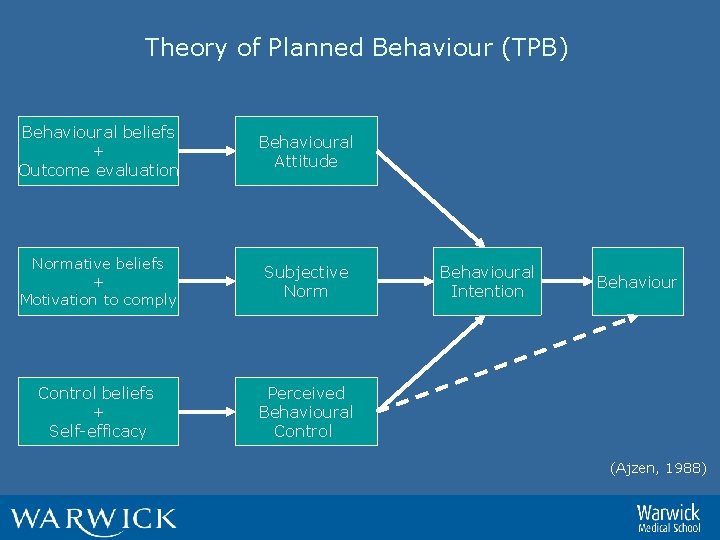
Theory of Planned Behaviour (TPB) Behavioural beliefs + Outcome evaluation Behavioural Attitude Normative beliefs + Motivation to comply Subjective Norm Control beliefs + Self-efficacy Perceived Behavioural Control Behavioural Intention Behaviour (Ajzen, 1988)
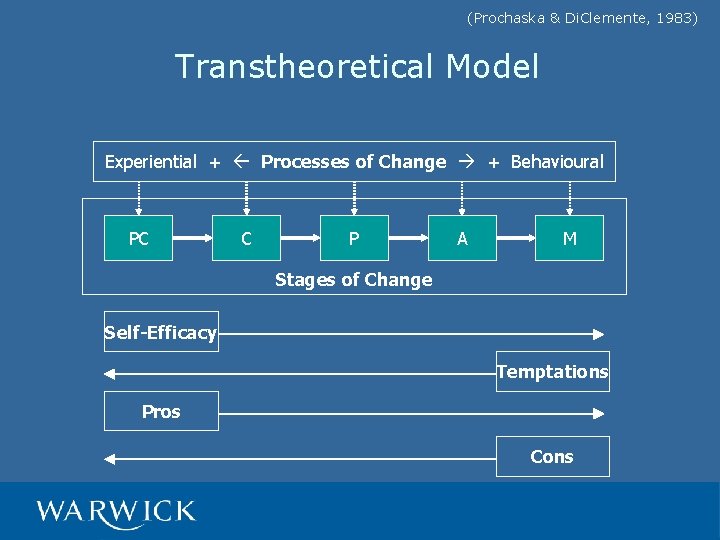
(Prochaska & Di. Clemente, 1983) Transtheoretical Model Experiential + Processes of Change + Behavioural PC C P A M Stages of Change Self-Efficacy Temptations Pros Cons

Health Behaviour Models / Theories Which model / theory is best? n At the end of every ‘theory’ chapter in every health psychology text, you’ll receive the following expert advice: n ‘Models are not in competition … … they offer different perspectives on the relationship between social cognitions and (health) behaviour … …’ … blar, blar …

Which ‘perspectives’, on which ‘relationships’ and between what cognitions, etc. , will help us to … understand … … predict …. … and change … … the health damaging behaviours in which so many people habitually engage?
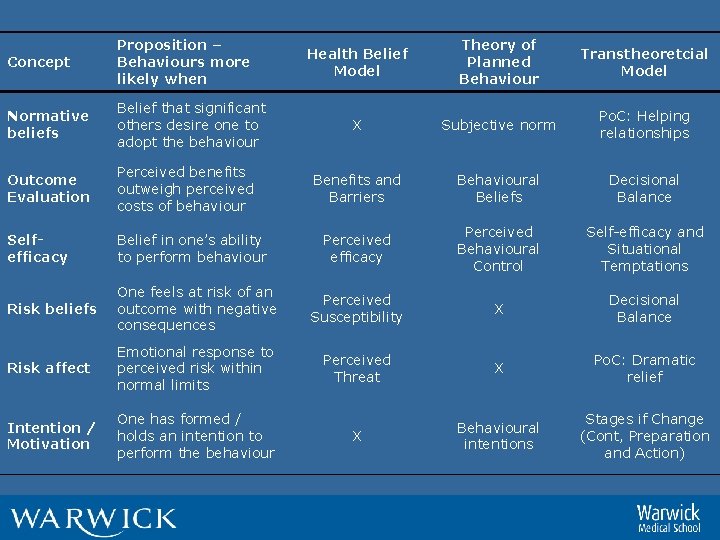
Concept Proposition – Behaviours more likely when Health Belief Model Theory of Planned Behaviour Transtheoretcial Model Normative beliefs Belief that significant others desire one to adopt the behaviour X Subjective norm Po. C: Helping relationships Outcome Evaluation Perceived benefits outweigh perceived costs of behaviour Benefits and Barriers Behavioural Beliefs Decisional Balance Selfefficacy Belief in one’s ability to perform behaviour Perceived efficacy Perceived Behavioural Control Self-efficacy and Situational Temptations Risk beliefs One feels at risk of an outcome with negative consequences Perceived Susceptibility X Decisional Balance Risk affect Emotional response to perceived risk within normal limits Perceived Threat X Po. C: Dramatic relief Intention / Motivation One has formed / holds an intention to perform the behaviour X Behavioural intentions Stages if Change (Cont, Preparation and Action)

Conceptual Framework n Determinants of health behaviours and beliefs n n Background factors: Cultural norms; SES; Gender; Ethnicity; Genes; Chronic health status Stable factors: Emotional disposition, Generalised expectancies; Explanatory styles Social factors: Perceived support (family, friends, peers, etc. ); Subjective norm; Helping relationships Situational factors: Situation-specific self-efficacy; Perceived risk; Emotional response; Intention (motivation); Outcome evaluation;

Conclusions n n n There are many determinants of health-related behaviours Determinants can be usefully grouped to form a conceptual framework Background, stable and social factors shape beliefs and situational appraisals Behaviour (typically) is most strongly influenced by situational beliefs / appraisals Psychological models attempt to explain the relationship between beliefs and behaviour Changing beliefs promotes long-term behaviour change

Summary n This session would have helped the student to understand the … n n range of behaviours that can be described as being health-related different types of determinants of health-related behaviours and the level at which they operate common psychological components of health behaviour theories core constructs relevant to understanding, predicting and changing health-related behaviours

Next Week n Illness Behaviours & Beliefs n n Common sense would suggest that people who seek medical help have more severe symptoms than those who do not seek help. Research demonstrates that this is incorrect. Peoples interpretation of their symptoms and their helpseeking behaviour is determined by many factors aside from the presence or severity of physical symptoms. These factors will be the examined in next week’s session.

Any questions? n What now? n n Obtain / download one of the recommended readings In your small groups consider today’s lecture in relation to next week’s tutorial tasks: a) integrated template b) ESA question
- Slides: 27