Module 7 Outbreak Investigation Disease Control Outbreak Investigation

Module 7: Outbreak Investigation & Disease Control Outbreak Investigation Developed through the APTR Initiative to Enhance Prevention and Population Health Education in collaboration with the Brody School of Medicine at East Carolina University with funding from the Centers for Disease Control and Prevention

Acknowledgments APTR wishes to acknowledge the following individuals that developed this module: Kristina Simeonsson, MD, MSPH Department of Public Health Brody School of Medicine at East Carolina University Julie Daugherty, MPH Department of Public Health Brody School of Medicine at East Carolina University This education module is made possible through the Centers for Disease Control and Prevention (CDC) and the Association for Prevention Teaching and Research (APTR) Cooperative Agreement, No. 5 U 50 CD 300860. The module represents the opinions of the author(s) and does not necessarily represent the views of the Centers for Disease Control and Prevention or the Association for Prevention Teaching and Research.


Foodborne Outbreaks in the News

Presentation Objectives Define the terms outbreak, epidemic and pandemic Discuss reasons that outbreaks occur Understand the rationale for investigating outbreaks 4. Describe the steps of an outbreak investigation 1. 2. 3.

Is Their a Difference between an Epidemic and an Outbreak? EPIDEMIC Occurrence of more cases of disease than expected in a given area or among a specific group of people over a particular period of time OUTBREAK Epidemic limited to localized increase in the incidence of disease CLUSTER Aggregation of cases in a given area over a particular period without regard to whether the number of cases is more than expected

What is a Pandemic? An epidemic occurring over a widespread area and usually affecting a substantial proportion of the population Influenza Severe acute respiratory syndrome (SARS) Tuberculosis Acquired immunodeficiency syndrome (AIDS)
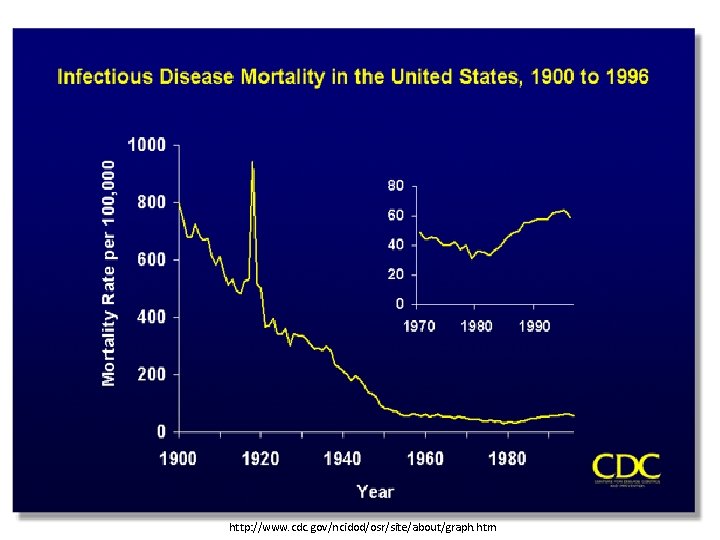
http: //www. cdc. gov/ncidod/osr/site/about/graph. htm
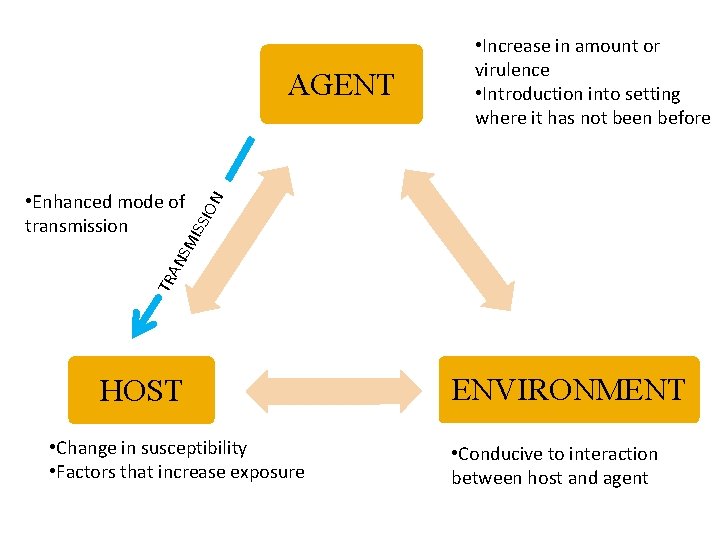
TR AN SM I SSI • Enhanced mode of transmission ON AGENT • Increase in amount or virulence • Introduction into setting where it has not been before HOST • Change in susceptibility • Factors that increase exposure ENVIRONMENT • Conducive to interaction between host and agent

Why Investigate Outbreaks? Prevention and control Research Public concern Political interest Program considerations Training http: //www 2 a. cdc. gov/TCEOnline/

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Establish Existence of Epidemic Determine if observed numbers exceed the expected level Be aware of artifactual causes of increases or decreases of reported cases Change in reporting practices Change in case definition New diagnostic test available

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Verify the Diagnosis Confirm clinical diagnosis with laboratory techniques Not every reported case needs to be laboratory confirmed

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Case Definition Consists of standard elements Clinical information Time Place Person Can have varying degrees of certainty Suspect Probable Confirmed
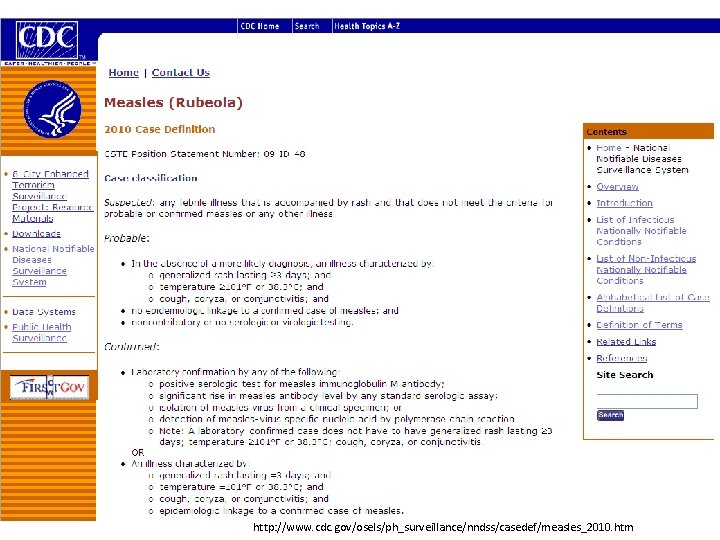
http: //www. cdc. gov/osels/ph_surveillance/nndss/casedef/measles_2010. htm

Case Definition Can vary depending on the purpose Characterize the extent of the outbreak Determine risk factors or find a cause

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings
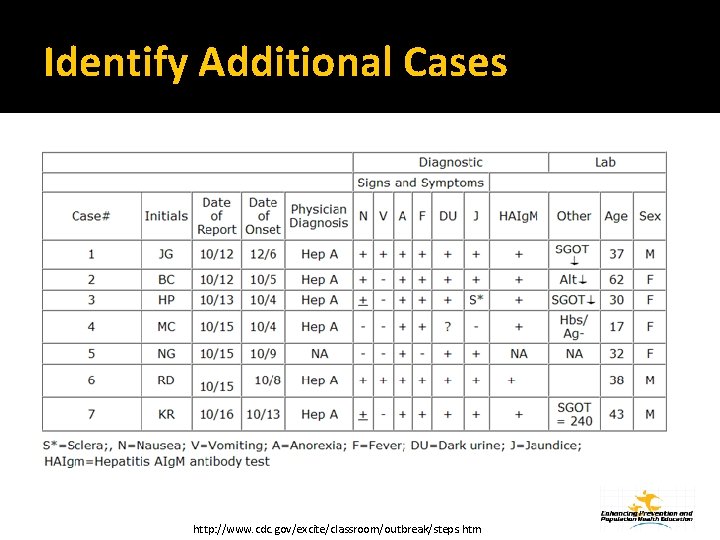
Identify Additional Cases http: //www. cdc. gov/excite/classroom/outbreak/steps. htm

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Perform Descriptive Epidemiology Orient data in terms of time Orient data in terms of place Orient data in terms of person

Orient by Time Characterize the cases by plotting a graph or epidemic curve that shows the number of cases (y-axis) over the time of onset of illness (x-axis) using an appropriate interval
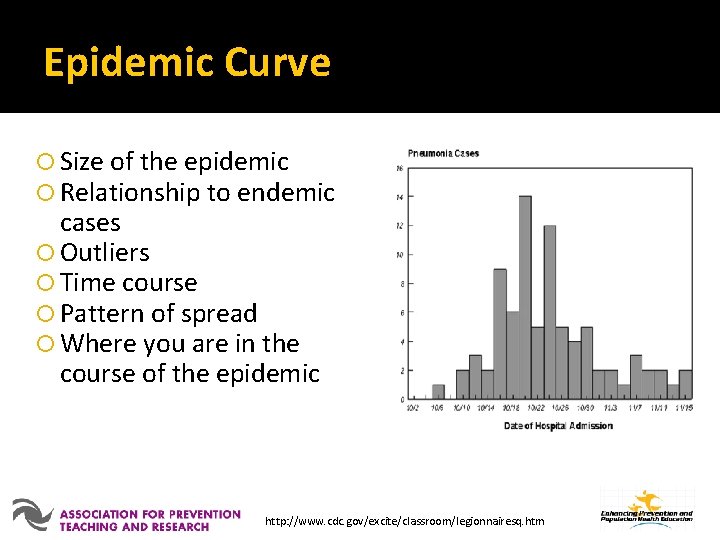
Epidemic Curve Size of the epidemic Relationship to endemic cases Outliers Time course Pattern of spread Where you are in the course of the epidemic http: //www. cdc. gov/excite/classroom/legionnairesq. htm
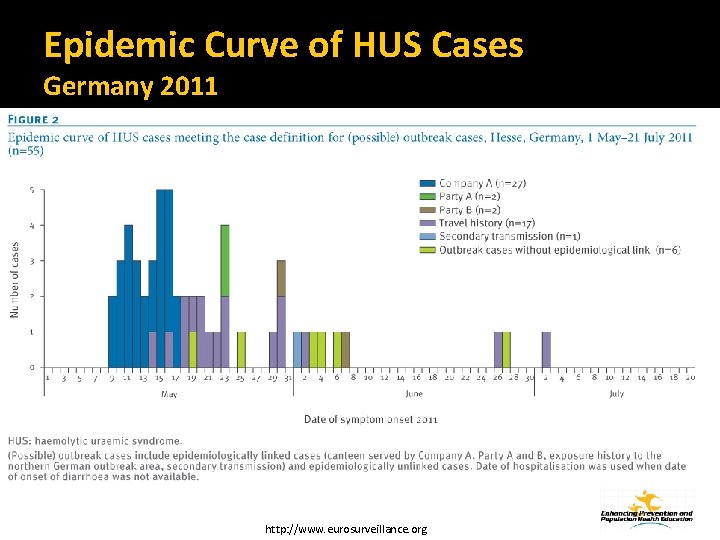
Epidemic Curve of HUS Cases Germany 2011 http: //www. eurosurveillance. org
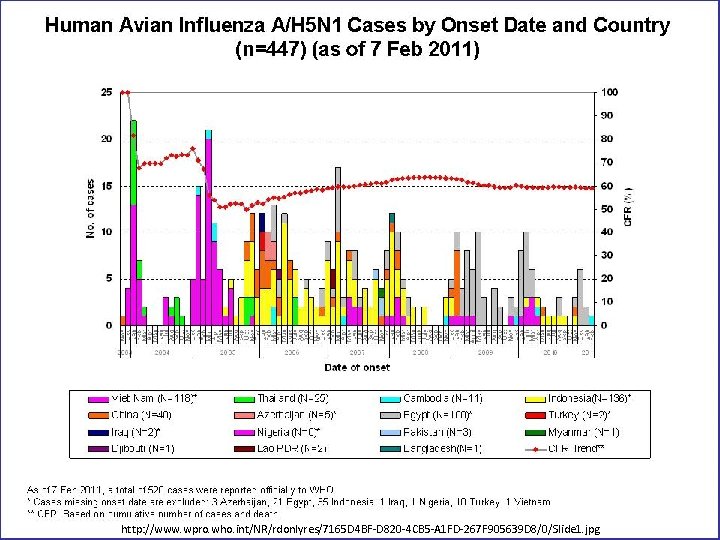
http: //www. wpro. who. int/NR/rdonlyres/7165 D 4 BF-D 820 -4 CB 5 -A 1 FD-267 F 905639 D 8/0/Slide 1. jpg

Orient by Place Geographic distribution of cases can provide clues to source of the epidemic Water supplies Air flow patterns in buildings Ecologic habitat of vectors May help identify the vehicle or mode of transmission
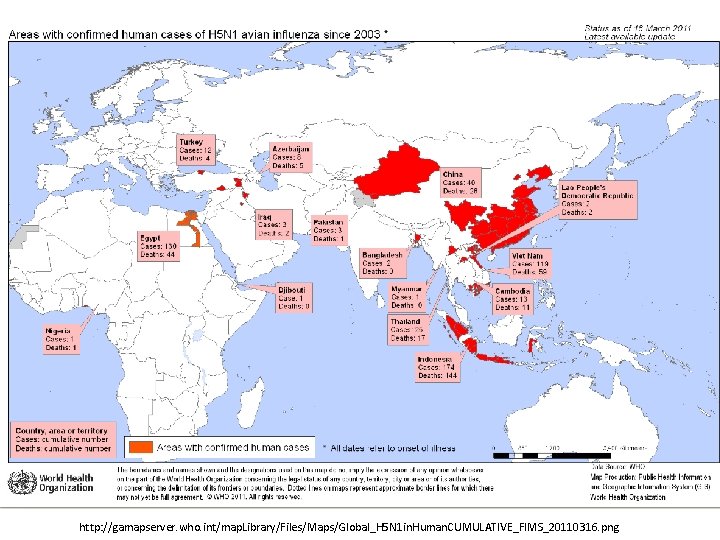
http: //gamapserver. who. int/map. Library/Files/Maps/Global_H 5 N 1 in. Human. CUMULATIVE_FIMS_20110316. png

Orient by Person Examine characteristics of cases Personal characteristics Exposures
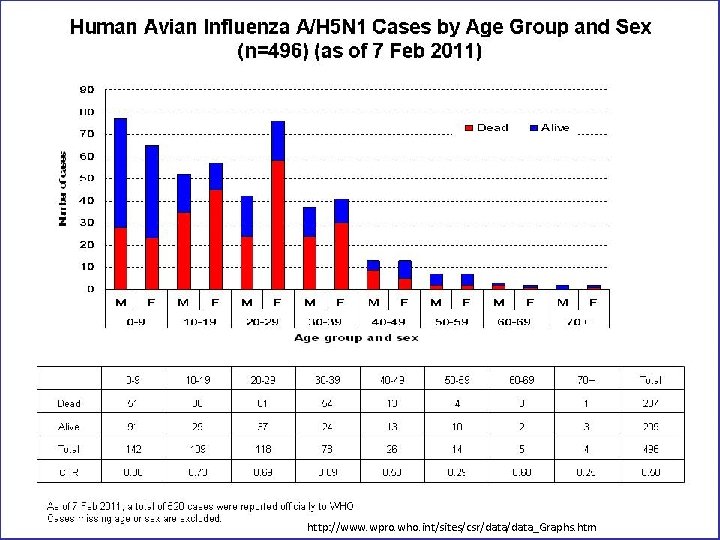
http: //www. wpro. who. int/sites/csr/data_Graphs. htm

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Develop and Test Hypothesis Develop hypothesis using descriptive epidemiology Person, place and time Clinical and laboratory findings Test hypothesis using analytic epidemiology Identify exposures significantly associated with illness Analytic epidemiologic study designs ▪ retrospective cohort study ▪ case-control study

(Retrospective) Cohort Study Enrolled after the disease has occurred Enrolls everyone in a given population regardless of disease status Technique of choice for acute outbreak in well- defined population Church picnic

(Retrospective) Cohort Study Directly measure risk of disease because the population at risk is known Outcome measure is relative risk Risk in the exposed group divided by the risk in the unexposed group (relative risk) Also known as the attack rate ratio

Case-Control Study Begins conceptually with disease and looks backward at prior exposures Useful when the population at risk is unknown Group of people with disease (cases) and group of people without disease (controls) are enrolled and prior exposures are ascertained Differences in exposure between groups indicates an association between exposure and disease

Case-Control Study True size of exposed and unexposed groups is unknown No denominator to calculate attack rate or relative risk Outcome measure is odds ratio (OR) Odds of developing disease based on exposure Odds ratio can approximate relative risk When the cases are representative When the controls are representative When the disease being studied is rare
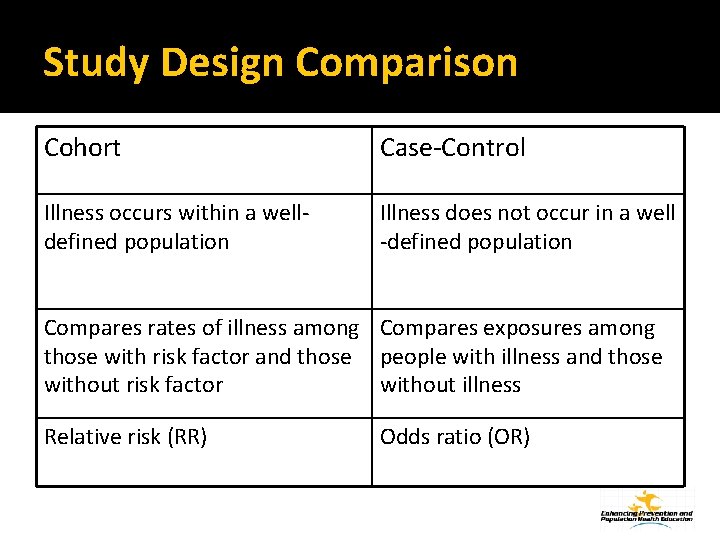
Study Design Comparison Cohort Case-Control Illness occurs within a welldefined population Illness does not occur in a well -defined population Compares rates of illness among Compares exposures among those with risk factor and those people with illness and those without risk factor without illness Relative risk (RR) Odds ratio (OR)

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Reconsider Hypothesis “Square” the hypothesis to clinical, laboratory and epidemiologic facts If exposure histories for ill versus well are not significantly different, develop a new hypothesis

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Perform Additional Studies Find more cases Define better the extent of the epidemic Evaluate new laboratory method Evaluate case-finding technique Improve sensitivity and specificity of case definition Degrees of exposure / dose response Environmental investigation

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Implement Control Measures Prevent exposure Prevent infection Prevent disease Prevent death

Control Measures for Influenza

Steps of an Outbreak Investigation 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Establish existence of an outbreak Verify the diagnosis Define a case Identify additional cases Perform descriptive epidemiology Develop and test hypothesis Reconsider hypothesis Perform additional studies if needed Implement control measures Communicate findings

Communicate Findings Outbreak investigation staff Public health personnel Government officials Healthcare providers Media Community

Risk Communication Developed from the need to find more effective ways to communicate health risks Goal is to provide information about expected type and magnitude of an outcome from a behavior or exposure The purpose of the message is to empower decisionmaking

Risk Communication Pitfalls Mixed messages from multiple experts Messages that are over-reassuring Leaving myths, rumors, and doomsayers unchallenged or uncorrected Public spokespersons who lack affect

http: //www. bt. cdc. gov/CERC/

Emergency Risk Communication Principles Stop trying to allay panic Emphasize there is a process in place Don’t over reassure Acknowledge uncertainty Acknowledge people’s fears Express wishes Give people things to do Acknowledge the shared misery Give anticipatory guidance Address dreaded “what if” questions Be a role model and ask more of people Be regretful Crisis and Emergency Risk Communication Centers for Disease Control and Prevention, September 2002

Challenges in Outbreak Investigations Data sources Small numbers Specimen collection Publicity Reluctance to participate Gregg Field Epidemiology 3 rd edition

Summary Steps of an outbreak investigation are a guide Not to be used as a “one size fits all” model Some steps may happen simultaneously Clear and consistent communication is key

Collaborating Institutions Center for Public Health Continuing Education University at Albany School of Public Health Department of Community & Family Medicine Duke University School of Medicine

Advisory Committee Mike Barry, CAE Lorrie Basnight, MD Nancy Bennett, MD, MS Ruth Gaare Bernheim, JD, MPH Amber Berrian, MPH James Cawley, MPH, PA-C Jack Dillenberg, DDS, MPH Kristine Gebbie, RN, Dr. PH Asim Jani, MD, MPH, FACP Denise Koo, MD, MPH Suzanne Lazorick, MD, MPH Rika Maeshiro, MD, MPH Dan Mareck, MD Steve Mc. Curdy, MD, MPH Susan M. Meyer, Ph. D Sallie Rixey, MD, MEd Nawraz Shawir, MBBS

APTR Sharon Hull, MD, MPH President Allison L. Lewis Executive Director O. Kent Nordvig, MEd Project Representative
- Slides: 56