Module 5 Additional Complications of CKD Hyperkalemia Metabolic

Module 5: Additional Complications of CKD Hyperkalemia, Metabolic Acidosis, Malnutrition, Depression & Acute Kidney Injury Andrew Narva, MD, FASN & Amy Barton Pai, Pharm. D, MHI, FASN, FCCP, FNKF

Faculty Disclosure Information Andrew Narva, MD, FASN No financial disclosures/conflicts of interest Amy Barton Pai, Pharm. D, MHI, FASN, FCCP, FNKF Disclosure: Consultant for Keryx Slide 2 of 64

About NKDEP This professional development opportunity was created by the National Kidney Disease Education Program (NKDEP), an initiative of the National Institute of Diabetes and Digestive and Kidney Diseases of the National Institutes of Health. With the goal of reducing the burden of chronic kidney disease (CKD), especially among communities most impacted by the disease, NKDEP works in collaboration with a range of government, nonprofit, and health care organizations to: • • raise awareness among people at risk for CKD about the need for testing; educate people with CKD about how to manage their disease; provide information, training, and tools to help health care providers better detect and treat CKD; and support health system change to facilitate effective CKD detection and management. To learn more about NKDEP, please visit: http: //www. nkdep. nih. gov. For additional materials from NIDDK, please visit: http: //www. niddk. nih. gov. Slide 3 of 64

Meet our Presenters Amy Barton Pai, Pharm. D, MHI, FASN, FCCP, FNKF Dr. Barton Pai is Chair of the National Kidney Disease Education Program’s Pharmacy Working Group Dr. Amy Barton Pai, Pharm. D. , MHI, FASN, FCCP, FNKF is Associate Professor of Clinical Pharmacy at the University of Michigan College of Pharmacy. She obtained her Bachelor of Science in Pharmacy from Albany College of Pharmacy in 1996 and then completed a Pharmacy Practice Residency at St. Peter’s Hospital in Albany, New York. She received her Doctor of Pharmacy from Albany College of Pharmacy in 1999. From 1999 -2001 she was a Nephrology Research Fellow at the University of Illinois at Chicago. Dr. Pai was on faculty at the University of New Mexico College of Pharmacy and School of Medicine from 2001 to 2008 and at Albany College of Pharmacy and Health Sciences from 2008 to 2016. She earned a Master's degree in Healthcare Innovation in 2018. Slide 4 of 64

Meet our Presenters Andrew S. Narva, M. D. , F. A. C. P. Dr. Narva is the Director of the National Kidney Disease Education Program (NKDEP) at the National Institutes of Health. Prior to joining the NKDEP in 2006, he served as Director of the Kidney Disease Program for the Indian Health Service (IHS). Dr. Narva continues to serve as the Chief Clinical Consultant for Nephrology for IHS and to provide care for patients at Zuni Pueblo through a telemedicine clinic. Dr. Narva is a member of the American Board of Internal Medicine Nephrology Subspecialty Board. He has served as a member of the Eighth Joint National Committee (JNC 8) Expert Panel, the National Quality Forum Renal Steering Committee, the Kidney Disease Outcomes Quality Initiative Work Group on Diabetes in Chronic Kidney Disease, and the Medical Review Board of End Stage Renal Disease Network 15. Slide 5 of 64

After this module, you will be able to: • Recognize hyperkalemia, metabolic acidosis, malnutrition, depression & acute kidney injury (AKI) as important complications of CKD. • Evaluate patient clinical data to identify appropriate treatments for hyperkalemia and metabolic acidosis. • Identify laboratory data that is used to assess and monitor metabolic acidosis, malnutrition and AKI in CKD. • Describe important implications of depression in CKD patients. Slide 6 of 64

HYPERKALEMIA Slide 7 of 64
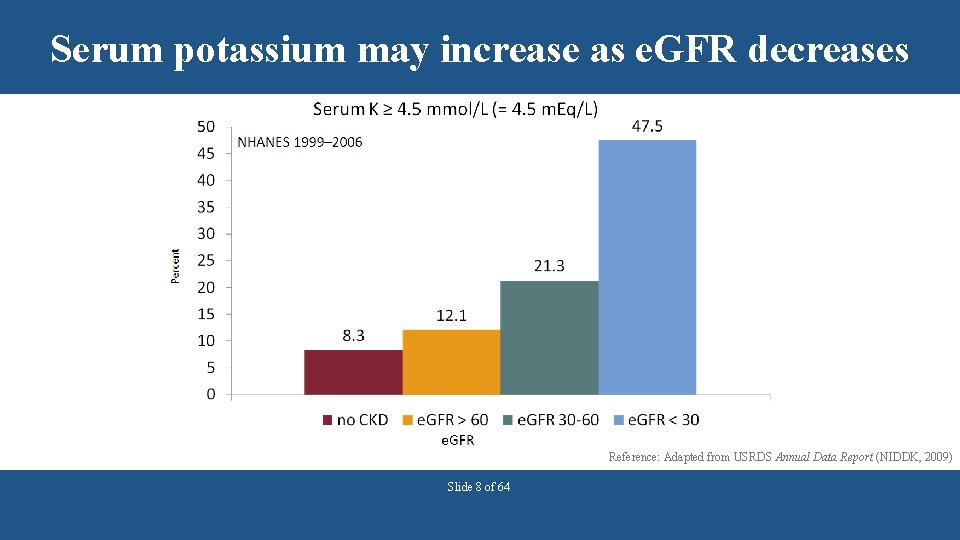
Serum potassium may increase as e. GFR decreases Reference: Adapted from USRDS Annual Data Report (NIDDK, 2009) Slide 8 of 64
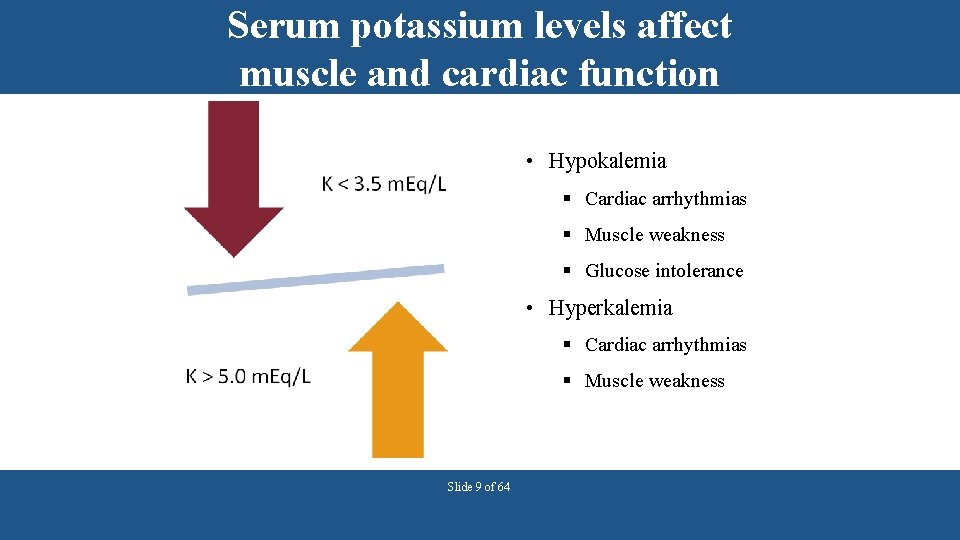
Serum potassium levels affect muscle and cardiac function • Hypokalemia § Cardiac arrhythmias § Muscle weakness § Glucose intolerance • Hyperkalemia § Cardiac arrhythmias § Muscle weakness Slide 9 of 64

Hyperkalemia is potentially life threatening • Susceptibility to hyperkalemia depends on serum calcium and other factors determining transmembrane potential. • Cardiac arrhythmias and cardiac arrest are possible if severe hyperkalemia is not recognized and treated. Slide 10 of 64

Potassium Balance • About 85% of dietary potassium is absorbed. • Proximal tubules reabsorb 70– 80% of potassium. • Potassium secretion occurs in distal tubule and collecting duct and may be an “adaptation” to high intake. • A small amount may be excreted in the feces. Gennari & Segal, Kidney Int 2002; 62(1): 1– 9. Slide 11 of 64

Renin-angiotensin-aldosterone system (RAAS) affects potassium excretion • Activation of RAAS increases potassium excretion via aldosterone. • Medications that inhibit RAAS increase risk for hyperkalemia. Palmer, N Engl J Med 2004; 351(6): 585 -592 Slide 12 of 64

Medication-induced hyperkalemia is a concern in CKD Medication Mechanism Beta-blockers (non-selective) Decreased Na+/K+-ATPase pump activity and renin release Digoxin intoxication Decreased Na+/K+-ATPase pump activity and renin release ACE inhibitors Blockade of angiotensin II synthesis and decreased aldosterone secretion ARBs Competitive binding of the angiotensin II receptor and decreased aldosterone synthesis NSAIDs Decreased prostaglandin-mediated renin release Calcineurin inhibitors Decreased aldosterone synthesis and Na+/K+-ATPase pump activity Aldosterone antagonists Blockade of mineralocorticoid receptors Potassium-sparing diuretics/trimethoprim Blockade of luminal sodium channels Ben Salem, C. Drug Saf. 2014 37: 677 -692 Slide 13 of 64
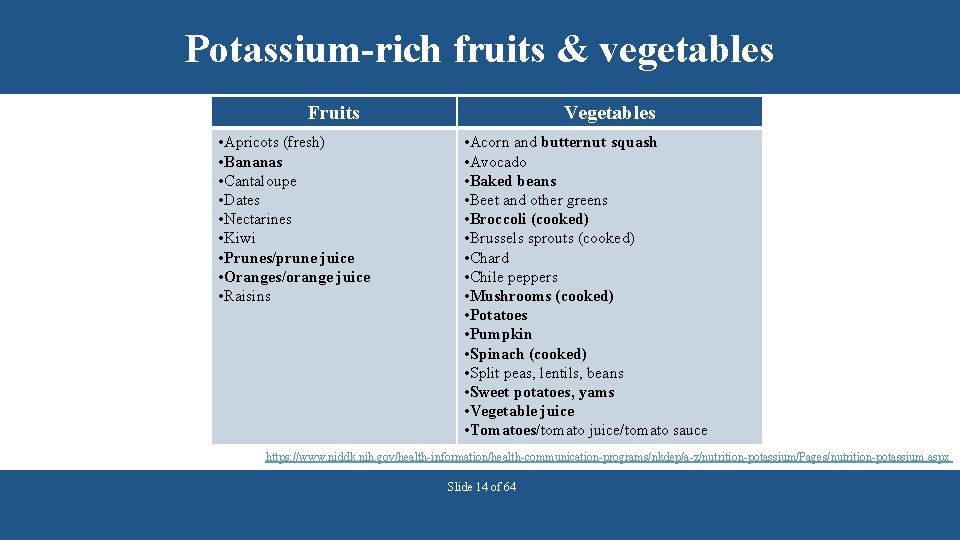
Potassium-rich fruits & vegetables Fruits • Apricots (fresh) • Bananas • Cantaloupe • Dates • Nectarines • Kiwi • Prunes/prune juice • Oranges/orange juice • Raisins Vegetables • Acorn and butternut squash • Avocado • Baked beans • Beet and other greens • Broccoli (cooked) • Brussels sprouts (cooked) • Chard • Chile peppers • Mushrooms (cooked) • Potatoes • Pumpkin • Spinach (cooked) • Split peas, lentils, beans • Sweet potatoes, yams • Vegetable juice • Tomatoes/tomato juice/tomato sauce https: //www. niddk. nih. gov/health-information/health-communication-programs/nkdep/a-z/nutrition-potassium/Pages/nutrition-potassium. aspx Slide 14 of 64

Potassium restriction is not indicated in the absence of hyperkalemia • Specific level of e. GFR does not determine need for potassium restriction. • Restrict dietary potassium to help achieve and maintain safe level. • Level of potassium restriction should be individualized. Slide 15 of 64

Question A patient with an e. GFR of 35 m. L/min/1. 73 m 2 presents with a serum potassium of 5. 8 m. Eq/L. His medications include labetalol 100 mg BID, lisinopril 40 mg once daily and acetaminophen 500 mg every 4 hours for osteoarthritis. He was started on Bactrim DS 5 days ago. Which of following is not likely contributing to his hyperkalemia? a) b) c) d) labetalol lisinopril acetaminophen Bactrim DS Slide 16 of 64

Answer A patient with an e. GFR of 35 m. L/min/1. 73 m 2 presents with a serum potassium of 5. 8 m. Eq/L. His medications include labetalol 100 mg BID, lisinopril 40 mg once daily and acetaminophen 500 mg every 4 hours for osteoarthritis. He was started on Bactrim DS 5 days ago. Which of following is not likely contributing to his hyperkalemia? a) b) c) d) labetalol lisinopril acetaminophen Bactrim DS Answer: C The answers A B and D are incorrect because nonselective beta-blockers, ACE inhibitors and trimethoprim can all induce hyperkalemia via renin, aldosterone or luminal sodium channel mechanisms. Acetaminophen does not decrease prostaglandins and does not decrease renin release. Slide 17 of 64

Potassium shifts between intracellular and extracellular compartments • 98% of potassium is intracellular. § 75% in muscles • 2% is extracellular (65– 70 m. Eq). • Transcellular electrical potential generated by sodiumpotassium exchange is responsible for voltage gradient across cell membranes. • Gradient difference is needed for muscle and nerve function. Slide 18 of 64

Factors affecting potassium shifts between compartments • Insulin concentration and hyperglycemia § Insulin moves potassium into cells. § Insulin deficiency may lead to hyperkalemia. • Acid-base status § Metabolic acidosis may drive potassium out of cells, as hydrogen ion is buffered intracellularly. Slide 19 of 64

Treating hyperglycemia and acidemia may lower serum potassium • Control hyperglycemia with adequate insulin. § Potassium follows glucose into the cells. • Treating acidosis may lower serum potassium. § Treatment may allow continued use of RAAS inhibitors that lower urine albumin and slow progression. Palmer, N Engl J Med 2004; 351(6): 585– 592 Slide 20 of 64

Treatments for hyperkalemia • Severe hyperkalemia (> 6. 0 m. Eq/L): § Intravenous calcium § Agents to induce intracellular shift: insulin and glucose, sodium bicarbonate and beta-2 agonist (albuterol) § Removal of potassium: Loop diuretics or Dialysis • Mild hyperkalemia (5. 5 -6. 0 m. Eq/L): § Sodium polystyrene sulfonate § Patiromer § Sodium zirconium cyclosilicate Slide 21 of 64

Sodium Polystyrene Sulfonate • Mechanism of action: Cation exchange resin, exchanges sodium for potassium • Dosage: § Adult dose: 15 g to 60 g (divided into 15 g one to four times daily) § In CKD: 30 g orally daily for up to 7 days • Side effects: nausea, vomiting, anorexia, constipation, hypomagnesemia, hypocalcemia § Fecal impaction has been reported in children § GI concretions with oral administration has been reported § GI tract ulceration or necrosis leading to intestinal perforation has been reported http: //www. accessdata. fda. gov/drugsatfda_docs/label/2009/011287 s 022 lbl. pdf Slide 22 of 64
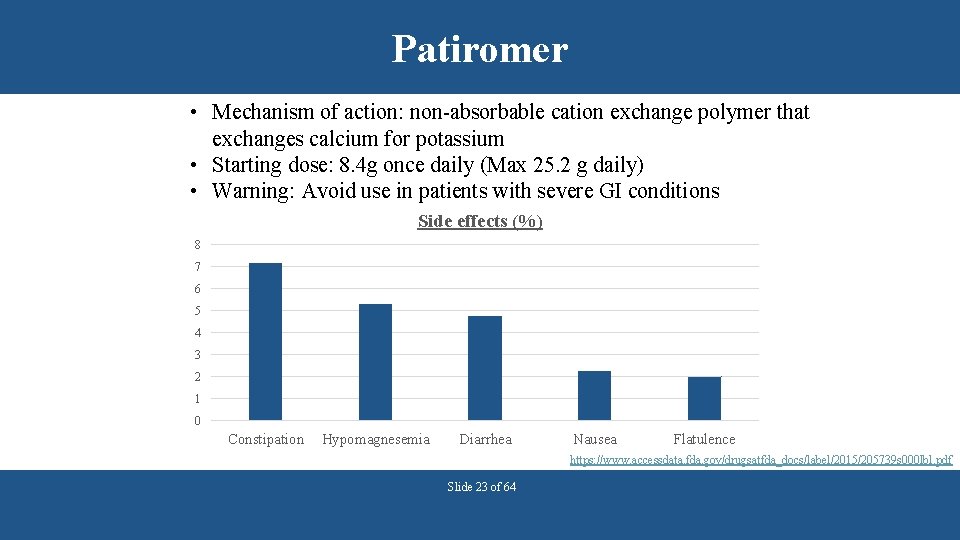
Patiromer • Mechanism of action: non-absorbable cation exchange polymer that exchanges calcium for potassium • Starting dose: 8. 4 g once daily (Max 25. 2 g daily) • Warning: Avoid use in patients with severe GI conditions Side effects (%) 8 7 6 5 4 3 2 1 0 Constipation Hypomagnesemia Diarrhea Nausea Flatulence https: //www. accessdata. fda. gov/drugsatfda_docs/label/2015/205739 s 000 lbl. pdf Slide 23 of 64

Sodium Zirconium Cyclosilicate • Mechanism of action: Cation exchange resin, exchanges sodium/hydrogen for potassium • Dosage: § 10 g TID for 48 hours, then 10 g once daily • Side effects: less gastrointestinal side effects than other agents § Can reduce serum potassium within 1 hour with proposed dosing, more rapid than other agents § Sodium absorption can be significant (800 mg/dose) Slide 24 of 64

Considerations for pharmacists • Drug preparation § All available potassium binding resins are available in powder form. • Symptoms of hypokalemia § Irritability, confusion, muscle weakness, hyporeflexia • Drug interactions § SPS: antacids, non-absorbable cation-donating antacids and laxatives, digoxin, sorbitol, lithium, thyroxine § Patiromer: Other drugs should be taken 3 hours before or after patiromer. § Sodium Zirconium Cyclosilicate: Separate other medications by 2 hours https: //www. accessdata. fda. gov/drugsatfda_docs/label/2015/205739 s 000 lbl. pdf Slide 25 of 64

Summary: Hyperkalemia • • • The reference range for serum K level is 3. 5– 5. 0 m. Eq/L Hyperkalemia is potentially life threatening RAAS affects potassium excretion Medication-induced hyperkalemia is a significant concern in CKD Hyperkalemia treatment includes: § Acute treatment: Insulin + beta agonist + calcium or dialysis § Chronic treatment: SPS, patiromer, sodium zirconium cyclosilicate § Choice of potassium resins should be based on risk of sodium absorption and gastrointestinal intolerance Slide 26 of 64

METABOLIC ACIDOSIS Slide 27 of 64
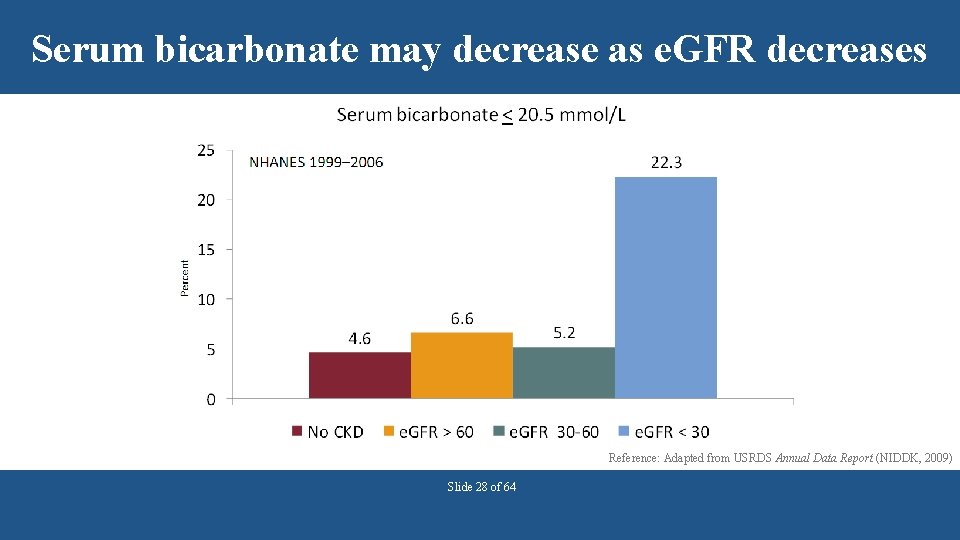
Serum bicarbonate may decrease as e. GFR decreases Reference: Adapted from USRDS Annual Data Report (NIDDK, 2009) Slide 28 of 64

Serum bicarbonate may decrease as e. GFR decreases • Metabolic acidosis is usually defined as serum bicarbonate concentration <22 m. Eq/L. • Approximately, 2. 3% to 13% of CKD Stage 3 patients are estimated to have metabolic acidosis • Approximately, 19% to 37% CKD Stage 4 patients are estimated to have metabolic acidosis Eustace JA et al. Kidney Int 2004; 65: 1031 -1040 Slide 29 of 64

Metabolic acidosis = excessive hydrogen ions in the blood • Acid production exceeds acid elimination • CO 2 + H 2 O HCO 3 + H+ • The reference range for serum bicarbonate (HCO 3) is 21– 28 m. Eq/L. • Maintaining normal serum HCO 3 may be beneficial. Bailey JL. Kidney Int. 2005; 68(suppl 96): S 15–S 23. de Brito-Ashurst I et al. J Am Soc Nephrol. 2009; 20(9): 2075– 84. Slide 30 of 64

Kidney tubules help maintain normal acid-base balance • Tubules reabsorb filtered HCO 3 and synthesize HCO 3 to neutralize acid load. § About 80– 85% is reabsorbed within the proximal tubules. • Patients with CKD have fewer functioning nephrons. § Less hydrogen ion (acid) is excreted. § Capacity to reabsorb and synthesize HCO 3 is reduced. § Condition may lead to chronic metabolic acidosis. Slide 31 of 64

Chronic metabolic acidosis • Accelerates muscle degradation • Reduces albumin synthesis • Exacerbates pre-existing bone disease • May impair glucose tolerance due to interference with insulin actions • May accelerate CKD progression • May stimulate inflammation Slide 32 of 64

Interventions for chronic metabolic acidosis • Adequate, not excessive, intake of animal protein • Supplemental base may be prescribed to balance the acid § Sodium bicarbonate may be prescribed, 650 mg tablet has 179 mg sodium § Re-emphasize dietary salt restriction § May require higher dose of diuretic Kraut & Madias, Nat Rev Nephrol 2010; 6(5): 274– 285 Slide 33 of 64

Sodium Bicarbonate • Contraindication: § Any medication or disease state that would induce hypochloremia (example. NG suction or severe vomiting) • Chronic metabolic acidosis dose: initial, 650 mg orally 3 times daily or calculated bicarbonate requirement; increase to maintain serum bicarbonate level at 22 -24 m. Eq/L • Side effects: § Flatulence/feeling of fullness § Fluid retention § Metabolic alkalosis Kraut & Madias, Am J Kidney Dis. 2016 Feb; 67(2): 307 -17 Slide 34 of 64

Summary: Metabolic acidosis • Animal protein may increase acid load. • Reducing protein intake may improve serum HCO 3. • Supplemental base may be prescribed to treat metabolic acidosis. • Sodium bicarbonate will increase daily sodium intake. Review salt restriction, if prescribed. • Treatment may improve serum albumin levels by improving nutritional status. Slide 35 of 64

Serum albumin is a marker for nutritional status and inflammation HYPOALBUMINEMIA Slide 36 of 64

Serum albumin • Maintains oncotic pressure and blood volume • Acts as buffer • Binds: § Calcium, magnesium § Hormones § Vitamins (e. g. , A, riboflavin, B 6, C, and folate) § Medications (e. g. , furosemide) • Serum albumin is a marker for nutritional status and inflammation Slide 37 of 64

Changes in drug binding to albumin in CKD • Metabolic acidosis changes protein confirmation, reduces binding, and increases free drug plasma concentration • Uremic toxins compete for binding to albumin • Reduced albumin increases the volume of distribution of water soluble drugs (third spacing) Slide 38 of 64

Serum albumin at dialysis initiation is an independent risk factor for mortality • Serum albumin ≥ 4. 0 g/d. L at initiation of dialysis is associated with reduced mortality risk. • Only 11% of incident dialysis patients had serum albumin ≥ 4. 0 g/d. L (1999– 2005). Reference: Kaysen et al. J Renal Nutr 2008; 18(4): 323– 331. Slide 39 of 64

Hypoalbuminemia in CKD is multi-factorial • Inflammation § Acute or chronic, e. g. , foot ulcer, infected tooth • Albuminuria • Metabolic acidosis • Insulin resistance • Reduced appetite particularly for foods high in protein Slide 40 of 64
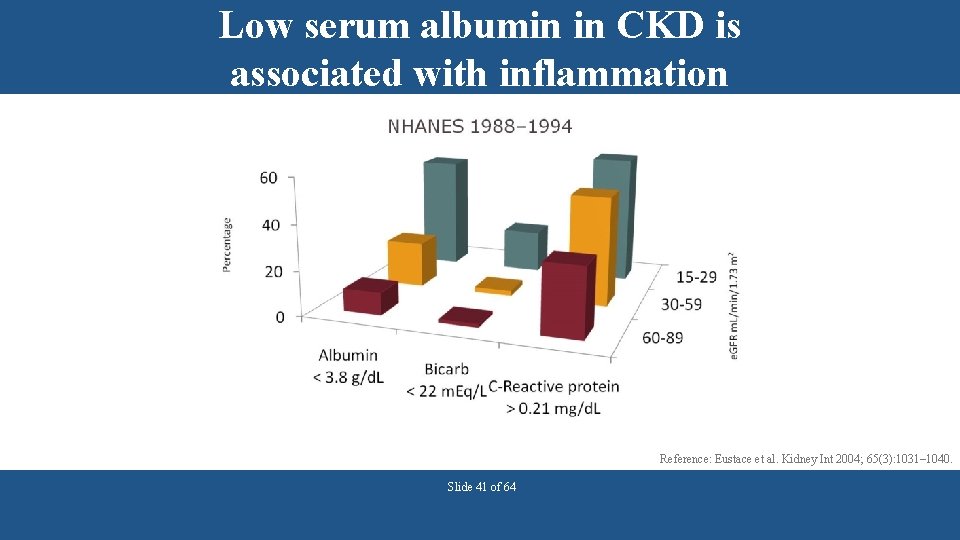
Low serum albumin in CKD is associated with inflammation Reference: Eustace et al. Kidney Int 2004; 65(3): 1031– 1040. Slide 41 of 64

Summary: Hypoalbuminemia in CKD • Reduce inflammation, treat infections • Serum albumin ≥ 4. 0 g/d. L at initiation of dialysis associated with lower risk of mortality • Control blood pressure and use ACE inhibitor to reduce proteinuria • Provide adequate protein and calories • Treat metabolic acidosis § Eating less protein may reduce acid load § May be treated with sodium bicarbonate Slide 42 of 64

DEPRESSION Slide 43 of 64
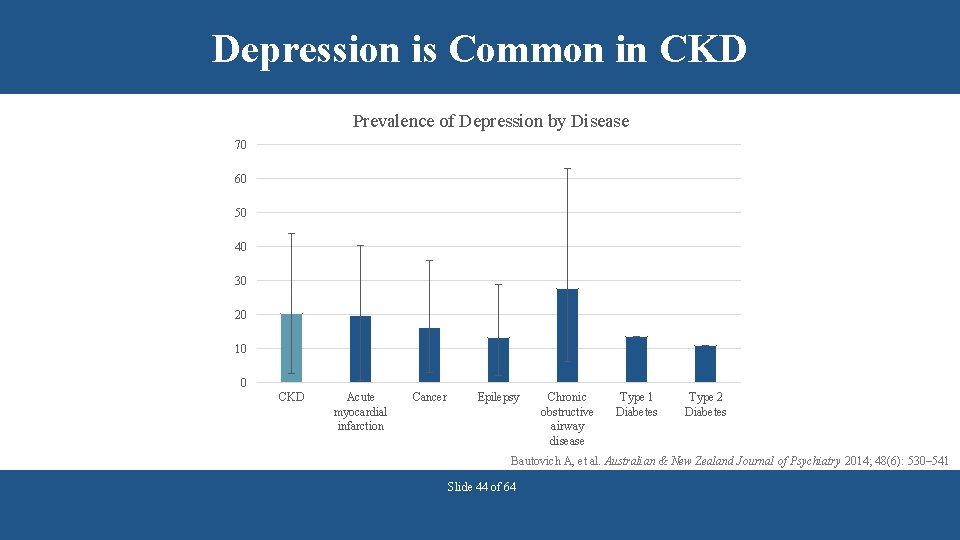
Depression is Common in CKD Prevalence of Depression by Disease 70 60 50 40 30 20 10 0 CKD Acute myocardial infarction Cancer Epilepsy Chronic obstructive airway disease Type 1 Diabetes Type 2 Diabetes Bautovich A, et al. Australian & New Zealand Journal of Psychiatry 2014; 48(6): 530– 541 Slide 44 of 64

Assessing Depression in CKD is Complex • Medications used to treat patients with CKD might also cause depression or have side effects that mimic its symptomatology § Clonidine § Propranolol • Uremia—which is common in advanced CKD—results in symptoms that may overlap with those of depression (e. g. , weight change, sleep disturbances, decreased appetite) Cukor D, et al. Psychosocial Aspects of Chronic Disease: ESRD as a Paradigmatic Illness 2007; 18(12): 3042 -55; Kimmel PL. Depression in patients with chronic renal disease: What we know and what we need to know 2002; 53(4): 951 -6. Slide 45 of 64
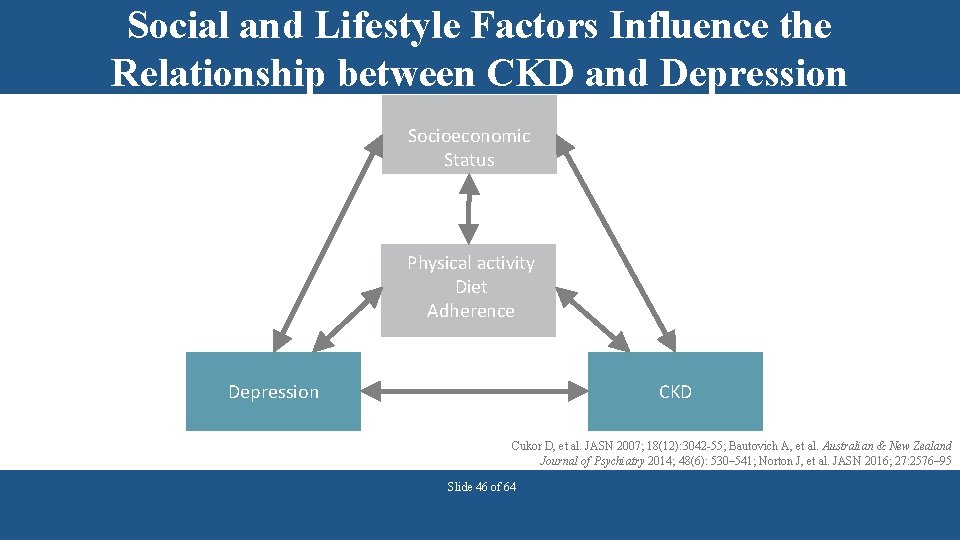
Social and Lifestyle Factors Influence the Relationship between CKD and Depression Socioeconomic Status Physical activity Diet Adherence Depression CKD Cukor D, et al. JASN 2007; 18(12): 3042 -55; Bautovich A, et al. Australian & New Zealand Journal of Psychiatry 2014; 48(6): 530– 541; Norton J, et al. JASN 2016; 27: 2576– 95 Slide 46 of 64

Biopsychosocial consequences of CKD and depression • Biological consequences: Increased inflammation and dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis as a consequence of depression and often reported in those with CKD • Barrier to healthy behaviors: Depression is a barrier to maintaining medical, dialysis and diet regimens. CKD is associated with a sedentary lifestyle, which is an independent risk factor for depression Cukor D, et al. JASN 2007; 18(12): 3042 -55; Bautovich A, et al. Australian & New Zealand Journal of Psychiatry 2014; 48(6): 530– 541 Slide 47 of 64

Biopsychosocial consequences of CKD and depression • Symptom burden: CKD patients have increased fatigue and sleep disturbance which all increase the risk of subsequent depression • Loss: Those with CKD report loss of role, identity, body image and employment, which all increase the risk of depression Bautovich A, et al. Australian & New Zealand Journal of Psychiatry 2014; 48(6): 530– 541 Slide 48 of 64

Negative outcomes are associated with depression in CKD • Higher all-cause mortality • Increased risk for hospitalization and length of stay • Barrier to adherence to medical and nutritional regimens • Reduced quality of life Palmer S, et al. Kidney Int. 2013; 84: 179– 191; Lopes AA, et al. Kidney Int. 2002; 62: 199– 207. Hedayati SS et al. JAMA 2010; 303: 1946– 1953; Chilcot J, et al. Sem Dial. 2010; 23: 74– 82 Kimmel PL, et al. Kidney Int. 2000; 57: 2093– 2098 Slide 49 of 64

Summary • Depression is a very common but complex problem among people with CKD • Depression has been associated with higher rates of mortality, increased hospitalization, reduced treatment adherence and lower QOL. • Screening and treatment of depression in those with CKD should be prioritized along with evidence-based pharmacotherapy Slide 50 of 64

ACUTE KIDNEY INJURY (AKI) Slide 51 of 64

Community-acquired acute kidney injury (CA-AKI) • Rapid decline of kidney function in the outpatient setting • Most commonly hemodynamically mediated • Outcomes are similar to patients who develop hospitalacquired AKI • Early patient-reported symptoms can include fatigue, reduced urine output and edema • CA-AKI may be more insidious, subtle signs/symptoms may be more important to glean from patient interview Mehta RL et al. Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury, ” Critical Care. 2007; 11 (2): R 31 Slide 52 of 64

CA-AKI is common and preventable • Drug induced AKI accounts for 18% of AKI hospital admissions from the outpatient setting. § Most cases are hemodynamically-mediated • There is a 3 -8 fold age-dependent increase in the frequency of CA-AKI in patients >60 years old • History of AKI is a strong risk factor for both new-onset CKD and accelerated progression of existing CKD Coca SG et al. Acute kidney injury in the elderly: predisposition to chronic kidney disease and vice versa. Nephron Clin Pract. 2011; 119 Suppl 1: c 19 -24. , Feest TJ et al. Incidence of severe acute renal failure in adults: results of a community-based study. BMJ 306: 481– 483, 1993 Slide 53 of 64

Who is at highest risk for CA-AKI? • Patients with: § existing CKD are at highest risk § diabetes and/or hypertension § renin-dependent comorbid conditions which are acquired with age (e. g. congestive heart failure, renal artery disease, severe liver disease) § comorbid conditions that require the use of drugs that affect renal hemodynamics (ACE Inhibitors, ARBS, diuretics, NSAIDs) Slide 54 of 64

Hemodynamically-mediated AKI • This video details the hemodynamic effects of RAASi, and NSAIDs with concurrent illness Renal Hemodynamics • Please also see this separate CE program focused on NSAID-induced AKI Slide 55 of 64

NSAIDs and CA-AKI • In a retrospective study of Medicaid enrolled patients, use of NSAIDs increased the risk of and AKI hospitalization by 58% (relative risk [RR] = 1. 58; 95% CI = 1. 34 -1. 86), and higher doses of ibuprofen (the most commonly used NSAID) were associated with a higher risk of developing AKI • The most relevant risk factors for AKI associated with NSAIDs from observational data are preexisting CKD, older age (ie, >65 years), concomitant use of diuretics and RAAS inhibitors, and recent initiation of an NSAID. Pai AB et al. Need for a Judicious Use of Nonsteroidal Anti-inflammatory Drugs to Avoid Community-Acquired Acute Kidney Injury. Ann Pharmacother. 2018; Slide 56 of 64
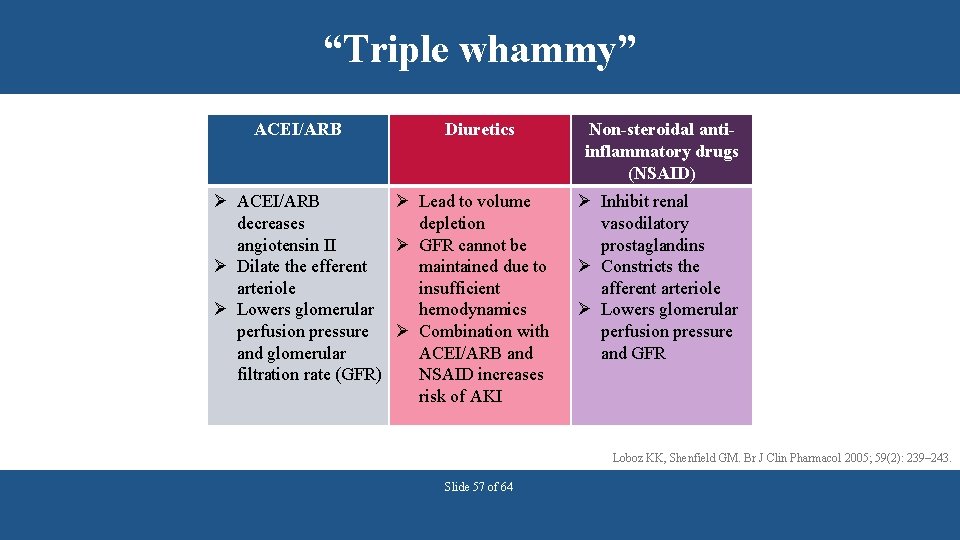
“Triple whammy” ACEI/ARB Diuretics Ø ACEI/ARB Ø Lead to volume decreases depletion angiotensin II Ø GFR cannot be Ø Dilate the efferent maintained due to arteriole insufficient Ø Lowers glomerular hemodynamics perfusion pressure Ø Combination with and glomerular ACEI/ARB and filtration rate (GFR) NSAID increases risk of AKI Non-steroidal antiinflammatory drugs (NSAID) Ø Inhibit renal vasodilatory prostaglandins Ø Constricts the afferent arteriole Ø Lowers glomerular perfusion pressure and GFR Loboz KK, Shenfield GM. Br J Clin Pharmacol 2005; 59(2): 239– 243. Slide 57 of 64

Case The patient is a 60 -year-old (110 kg) male who presents to urgent care with confusion, shortness of breath and edema. His past medical history includes hypertension, diabetes and back pain. His wife states that he had been taking naproxen multiple times per day for back pain that developed a couple weeks before admission. He stated he has not made much urine for the past few days. Today his labs reveal BUN 77 mg/dl, and SCr 3. 9 mg/d. L (baseline 1. 2 mg/d. L), potassium 5. 9 m. Eq/L. Home medications: Lisinopril 40 mg once daily, Hydrochlorothiazide 50 mg once daily, Humulin 70/30, Naproxen 220 mg 2 tablets q 12 h PRN Slide 58 of 64

Question Which of the following is most likely the cause of acute kidney injury in this patient? a) b) c) d) Humulin + Lisinopril + Humulin + Hydrochlorothiazide Lisinopril + Naproxen + Hydrochlorothiazide Humulin + Naproxen Slide 59 of 64

Answer Which of the following is most likely the cause of acute kidney injury in this patient? a) b) c) d) Humulin + Lisinopril + Humulin + Hydrochlorothiazide Lisinopril + Naproxen + Hydrochlorothiazide Humulin + Naproxen Answer: D Concurrent use of ACEI/ARB, NSAID and diuretic has been associated with risk of community acquired acute kidney injury. Slide 60 of 64

What are “Sick Day Rules”? • Dehydration can be a significant risk for people taking certain medicines. • Health care professionals can provide advice to patients who are at increased risk of AKI (e. g. patients with CKD / heart failure) that certain drugs should be temporarily discontinued during acute intercurrent illnesses(vomiting, diarrhea and fever), particularly where there is disturbed fluid balance. • This is commonly described as ‘sick day rules’ https: //www. thinkkidneys. nhs. uk/aki/wp-content/uploads/sites/2/2018/01/Think-Kidneys-Sick-Day-Guidance-2018. pdf Slide 61 of 64

https: //ihub. scot/media/1290/20170814 -medicines-sick-day-rules-card-v 2 -0 -print. pdf Slide 62 of 64

https: //ihub. scot/media/1290/20170814 -medicines-sick-day-rules-card-v 2 -0 -print. pdf Slide 63 of 64

Summary • Community-acquired AKI is becoming better defined and the prevalence rate may be higher than previously described. • The majority of CA-AKI cases are hemodynamically mediated and can be prevented. • CA-AKI is associated with long-term consequences on kidney function and clinical outcomes. • Use of ACEI, ARBs, diuretics and NSAIDs concomitantly has been associated with increase risk of CA-AKI in high risk patients Slide 64 of 64

- Slides: 65