MODULE 2 FOODBORNE DISEASE SURVEILLANCE AND OUTBREAK DETECTION

MODULE 2 – FOODBORNE DISEASE SURVEILLANCE AND OUTBREAK DETECTION FOODBORNE DISEASE OUTBREAK INVESTIGATION TEAM TRAINING

AT THE END OF THIS MODULE, YOU WILL BE ABLE TO 1. Describe the surveillance of foodborne illness through complaint systems. 2. List ways to improve the accuracy of a food history obtained in a foodborne illness complaint. 3. Describe the surveillance of foodborne illness through pathogen-specific surveillance. 4. Recognize a possible outbreak using a complaint system or pathogen-specific surveillance. 5. Describe the role of local public health in national pathogen-specific surveillance. 2

FOODBORNE DISEASE SURVEILLANCE Many ways to find out about cases of foodborne illnesses and outbreaks Two primary means § Foodborne illness complaint systems § Pathogen-specific surveillance (notifiable disease reporting) 3

FOODBORNE ILLNESS COMPLAINT SYSTEMS 4

COMPLAINT SYSTEMS § Complaints of illness among individuals and groups reported by affected members of the community (and others) § Includes any illness thought to be related to food § Common exposures used to link cases together 5
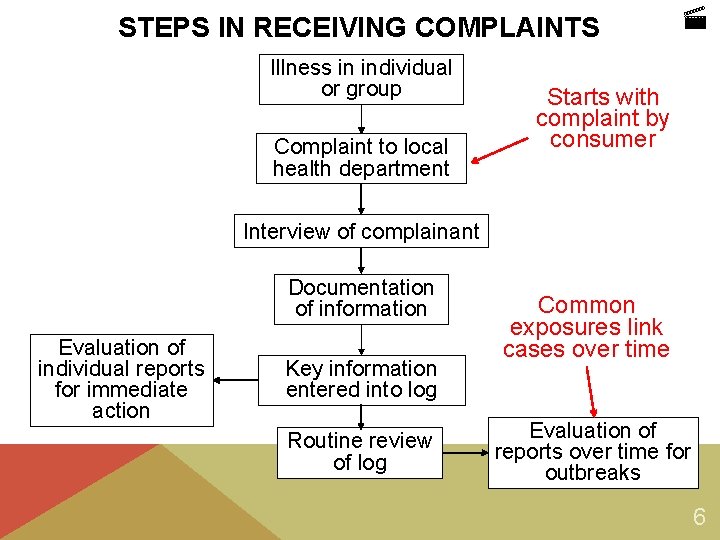
STEPS IN RECEIVING COMPLAINTS Illness in individual or group Complaint to local health department Starts with complaint by consumer Interview of complainant Documentation of information Evaluation of individual reports for immediate action Key information entered into log Routine review of log Common exposures link cases over time Evaluation of reports over time for outbreaks 6
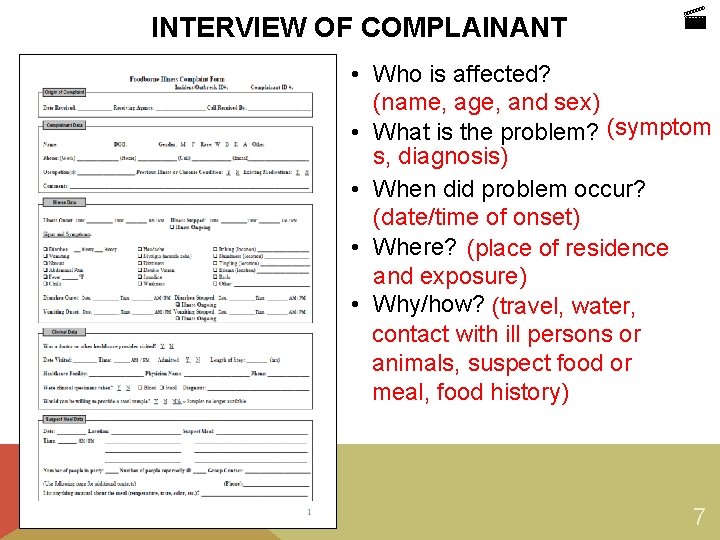

INTERVIEW OF COMPLAINANT • Who is affected? (name, age, and sex) • What is the problem? (symptom s, diagnosis) • When did problem occur? (date/time of onset) • Where? (place of residence and exposure) • Why/how? (travel, water, contact with ill persons or animals, suspect food or meal, food history) 7

COLLECTING FOOD HISTORIES Complete food history including § Foods eaten in 5 days before onset of illness − If norovirus likely, focus on 24 -48 hours before illness. − If >1 ill person, focus on shared foods/meals. § ALL foods eaten during time period of interest (unless focusing on shared foods/meals) § Details of named events, food establishments, or suspect food products Information on non-food exposures 8

SMALL GROUP EXERCISE Divide into groups of three. One person will be the interviewer; one, the complainant; and one, an evaluator. 1. The interviewer should solicit a 5 -day food history from the complainant. 2. The complainant should respond to questions as if they just developed symptoms that day and based on what they really ate in the last 5 days. 3. Was it easy or difficult? Did you get a complete history? What approaches were helpful? Be prepared to share with class. Time: 10 minutes 9

IMPROVING FOOD HISTORIES Have complainant: § Look at a calendar § Describe each meal in time period § Identify key events to jog memory § Review receipts or menus § Enlist help of dining partners § Consider specific list of foods § Think about food preferences § Rule out or rule in specific foods 10
ENTERING INFORMATION INTO LOG § Extract key information from the complaint to facilitate examination of reports over time − Date of illness onset − Predominant signs and symptoms − Name of food thought to have caused illness − Names of eating places or gatherings − Source of water and type − Other exposures § Transfer information carefully § Use consistent abbreviations and codes 11

EVALUATION OF COMPLAINTS Individual reports of concern: § Symptoms suggestive of serious illnesses § Laboratory-confirmed diagnoses § Reports of obvious food safety problems § Group illnesses thought to be due to an identified, shared exposure 12
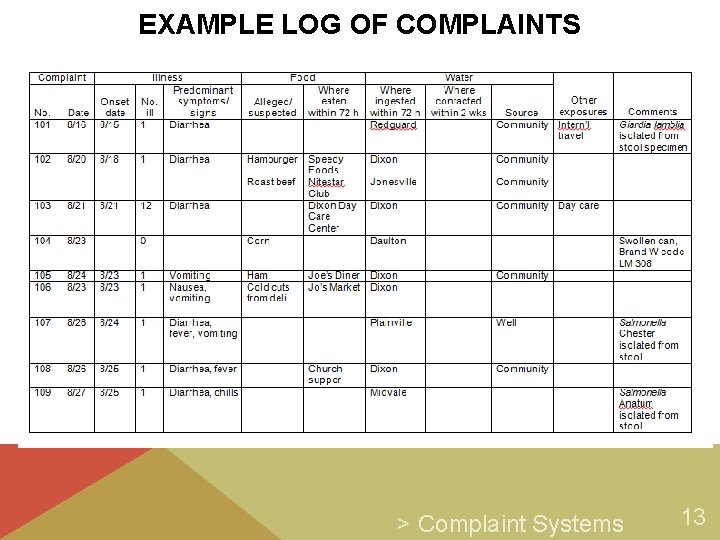
EXAMPLE LOG OF COMPLAINTS > Complaint Systems 13

GROUP ILLNESSES DUE TO IDENTIFIED, SHARED EXPOSURE Illnesses are likely to be related to an identified, shared exposure, if group members have: § Similar signs and symptoms § Shared a food or meal prior to onset of illness and had no other common exposures § Onset and nature of illness is consistent with identified shared exposure 14

QUESTION Which of the following group illnesses are likely to be Due to due to the identified restaurant exposure? Person developed diarrhea after eating at a restaurant. Neighbors who ate at the restaurant also are sick but complainant does not know their symptoms. Four friends develop nausea and vomiting, facial flushing, headache, and itching skin within an hour of eating fish at a restaurant. Family members develop bloody diarrhea within hours of eating at a restaurant. Exposure Unknown Likely Unlikely 15

EVALUATION OF COMPLAINTS (CONT’D) Looking at reports over time § Multiple individual complaints with same exposure (e. g. , same food establishment or food) § Multiple individual complaints with clustering by time, place, or person § Overall increase in complaints 16

RESPONSE TO COMPLAINTS § Notify epidemiology unit/communicable disease staff of laboratory-confirmed diagnoses. § Refer food safety problem to agency with regulatory authority. § Alert appropriate persons if possible outbreak detected. § Prioritize follow-up of commercial establishments. 17

FOLLOW-UP OF COMMERCIAL ESTABLISHMENTS Rational approach to follow-up § As required by local law/statute or § If complainant observed food safety problem or § If two or more persons (not from same household) − Have similar illness − Shared history of eating at establishment − Onset and nature of illness with shared foods 18

SMALL GROUP EXERCISE Study the foodborne illness log at the end of this module spanning a 2 -week period and determine: 1. Is the number of complaints what you would expect for the period covered? 2. Are there individual complaints of concern? 3. Are there common exposures (e. g. foods, establishments) across complaints signaling an outbreak? Be prepared to share with class. Time: 10 minutes 19

STRENGTHS OF COMPLAINT SYSTEMS Primary means to detect outbreaks that are § Localized (involving only one jurisdiction) § Due to diseases with a short incubation period 20

COMPLAINT SYSTEM ISSUES Inaccurate and incomplete food histories Large numbers of complaints Anonymous complaints Complaints with unknown causative agent § Inability to exclude unrelated cases § Inability to link cases based on illness unless symptoms very unique or cases report similar exposure 21

PATHOGEN-SPECIFIC SURVEILLANCE 22

PATHOGEN-SPECIFIC SURVEILLANCE § Also called “reportable diseases, ” “notifiable diseases, ” or “laboratory-based reporting” § Reports of individual lab-confirmed cases of foodborne disease by medical and laboratory staff with submission of clinical isolates, where requested § Only covers diseases selected by public health agency § Cases linked to each other by common pathogen 23
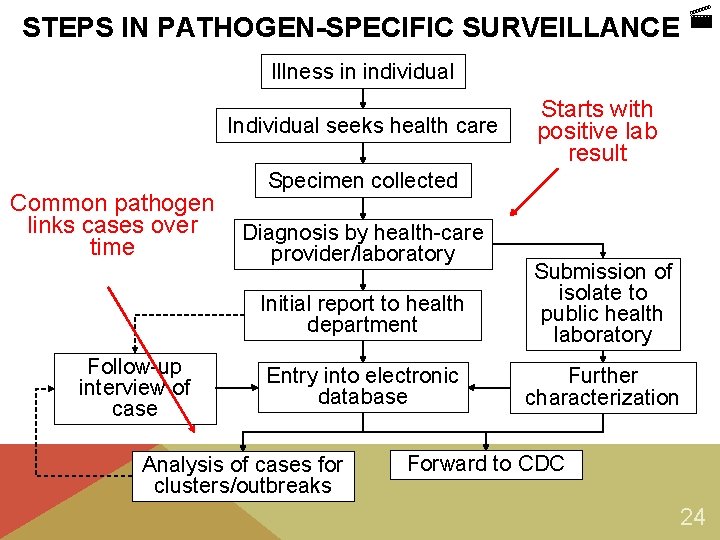
STEPS IN PATHOGEN-SPECIFIC SURVEILLANCE Illness in individual Individual seeks health care Common pathogen links cases over time Follow-up interview of case Starts with positive lab result Specimen collected Diagnosis by health-care provider/laboratory Initial report to health department Submission of isolate to public health laboratory Entry into electronic database Further characterization Analysis of cases for clusters/outbreaks Forward to CDC 24

INITIAL REPORT § From health-care provider or laboratory § Standardized form (often pathogen-specific) § Information of interest − Patient identifiers − Basic demographic information − Clinical information − Laboratory results 25

FOLLOW-UP INTERVIEW OF CASE § To identify potential exposures leading to illness § Similar to interview for complaint system but tailored to specific pathogen − High-risk food exposures for agent − Other exposures related to agent (e. g. , contact with ill people, animals, water) § Often occurs weeks after exposure leading to illness resulting in poor recall 26

LABORATORY CHARACTERIZATION OF PATHOGEN § Submission of patient isolate to public health laboratory for confirmation and subtyping § Increased detail about the pathogen (e. g. , serotyping, PFGE) improves − Recognition of clusters − Linking an outbreak with an exposure § Most critical with common pathogens 27

ANALYSIS FOR CLUSTERS Examine cases by pathogen over time using § Different levels of specificity of pathogen (e. g. , species, selected subtypes) § Subgroups of population (certain time, place, or person characteristics) Look for increase in number of cases over expected or baseline, indicating a cluster 28

ANALYSIS BY CAUSATIVE AGENT Number of Case Lab-confirmed salmonellosis cases by month of diagnosis, 2010 All Salmonella Month of Diagnosis 29
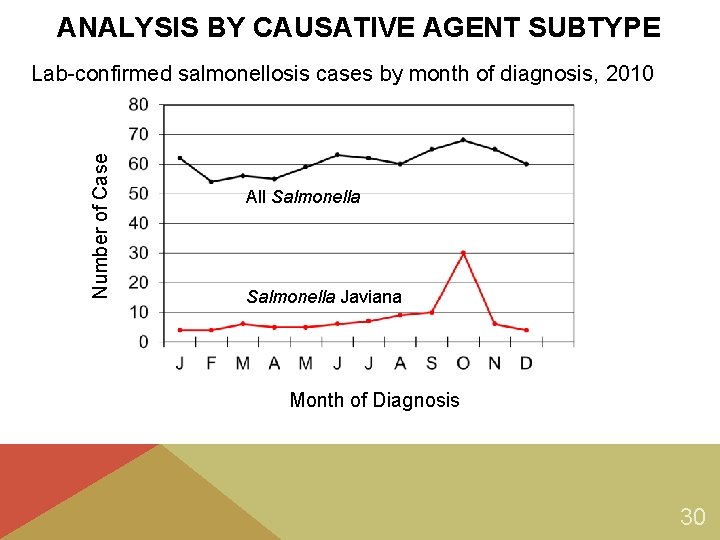
ANALYSIS BY CAUSATIVE AGENT SUBTYPE Number of Case Lab-confirmed salmonellosis cases by month of diagnosis, 2010 All Salmonella Javiana Month of Diagnosis 30

Number of Case ANALYSIS BY CAUSATIVE AGENT AND AGE Lab-confirmed salmonellosis. GROUP cases by month of diagnosis, 2010 All Salmonella Javiana among persons <5 yrs. Salmonella Javiana Month of Diagnosis 31

STRENGTHS OF PATHOGEN-SPECIFIC SURVEILLANCE Primary means to detect outbreaks that are § Wide-spread (i. e. , multijurisdictional), § Due to prolonged low-level food contamination, or § Due to diseases with a long incubation (e. g. , hepatitis A) 32

PATHOGEN-SPECIFIC SURVEILLANCE ISSUES § Incomplete detection and reporting Reported Culture-confirmed Case Lab Tests for Organism Specimen Obtained Person Seeks Care Person Becomes Ill Population 33

PATHOGEN-SPECIFIC SURVEILLANCE ISSUES § Incomplete detection and reporting § Elapsed time Elapsed Time for Salmonella Reporting Patient eats food Incubation period=1 -3 d Time to contact with health Patient care=1 -5 d becomes ill Stool sample collected Time to diagnosis=1 -3 d Shipping time=0 -7 d Salmonella identified Isolates received by Serotyping and PFGE=2 -10 d public Case health lab confirmed as part of cluster 34

PATHOGEN-SPECIFIC SURVEILLANCE ISSUES § Incomplete detection and reporting § Elapsed time § Availability of isolate for further characterization 35
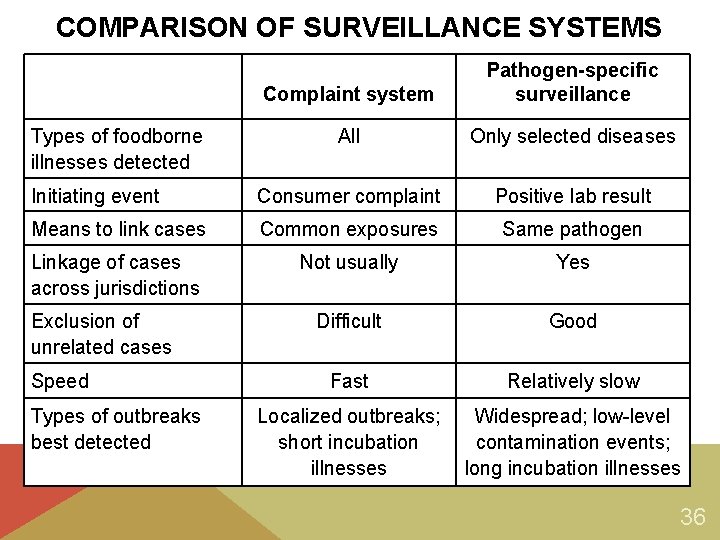
COMPARISON OF SURVEILLANCE SYSTEMS Complaint system Pathogen-specific surveillance All Only selected diseases Initiating event Consumer complaint Positive lab result Means to link cases Common exposures Same pathogen Linkage of cases across jurisdictions Not usually Yes Difficult Good Fast Relatively slow Localized outbreaks; short incubation illnesses Widespread; low-level contamination events; long incubation illnesses Types of foodborne illnesses detected Exclusion of unrelated cases Speed Types of outbreaks best detected 36

NATIONAL PATHOGEN-SPECIFIC SURVEILLANCE SYSTEMS 37

NATIONAL PATHOGEN-SPECIFIC SURVEILLANCE NNDSS (National Notifiable Disease Surveillance System) § Data from pathogen-specific surveillance forwarded to CDC (minimal case information) § Statistical algorithm used to identify increases Pulse. Net (National Molecular Subtyping Network for Foodborne Disease Surveillance) § Lab network that uses standardized PFGE methods § PFGE patterns uploaded by labs for STEC, Salmonella, Shigella, Listeria, Campylobacter § Comparisons of patterns to identify clusters 38

NATIONAL PATHOGEN-SPECIFIC SURVEILLANCE Calici. Net (National Electronic Norovirus Outbreak Network) § Laboratory network that subtypes/sequences norovirus isolates related to outbreaks § Data uploaded to CDC allows linkage of outbreaks and identification of new variants NARMS (National Antimicrobial Resistance Monitoring System—enteric bacteria) § Submission of Salmonella, Shigella, E. coli O 157, Campylobacter, and non-cholerae Vibrio to CDC § Determines trends in antimicrobial resistance 39

ROLE OF LOCAL HEALTH DEPARTMENTS Local pathogen-specific case reports and lab results feed into national surveillance Important for local health departments to § Collect data in format consistent with other investigators. § Streamline reporting and isolate submission. § Share case reports with state and submit patient isolates as quickly as possible. § Use national systems to learn about outbreaks in other jurisdictions. 40

WHAT DIFFERENCE DOES ONE LOCAL CASE MAKE? § Two E. coli O 157: H 7 infections in MN with same PFGE pattern; both ate tenderized steaks § Through Pulse. Net, single cases identified in KS and MI; both ate tenderized steaks § Steaks eaten by cases from same plant § Recall of 739, 000 lbs. of beef § Outbreak generated concern about needle/ blade tenderized steaks 41

QUICK QUIZ 42

QUICK QUIZ 1. Typically common exposures are used to detect outbreaks through a foodborne illness complaint systems whereas a common pathogen is used to detect outbreaks through pathogen-specific surveillance systems A. True B. False 43

QUICK QUIZ 2. Illnesses in a group are likely to be related to an identified, shared exposure (e. g. particular meal, event, or establishment), if group members have which of the following? A. Ill persons all have the same symptoms. B. Ill persons shared food or a meal prior to onset of illness and had no other common exposures. C. Onset of the illness is consistent with the timing of the exposure. D. All of the above 44

QUICK QUIZ 3. Which of the following can improve the accuracy of a food history solicited during a foodborne illness complaint? A. Have case look at a calendar and identify key events to jog memory. B. Have case review credit card or cash register receipts to identify where or what they ate. C. Enlist help of dining partners. D. All of the above 45

QUICK QUIZ 4. All of the following are true of pathogen-specific surveillance EXCEPT A. Detects all types of foodborne illness. B. Relies on reports from health-care providers and clinical laboratory staff. C. Is the primary means to detect widespread outbreaks such as multistate outbreaks. D. Has an inherent lag in reporting due to time necessary to confirm pathogen through laboratory testing. 46

QUICK QUIZ 5. All of the following are important roles for local health departments in national pathogenspecific surveillance EXCEPT A. Collect information on local cases in a format consistent with other investigators. B. Share case reports with state health department in a timely fashion. C. Be alert to outbreaks in other jurisdictions. D. Submit all patient isolates directly to CDC. 47
- Slides: 47