Module 1 Kidney Disease Basics Andrew Narva MD

Module 1: Kidney Disease Basics Andrew Narva, MD, FASN & Amy Barton Pai, Pharm. D, MHI, FASN, FCCP, FNKF

Faculty Disclosure Information Andrew Narva, MD, FASN No financial disclosures/conflicts of interest Amy Barton Pai, Pharm. D, MHI, FASN, FCCP, FNKF Disclosure: Consultant for Keryx Slide 2 of 74

About NKDEP This professional development opportunity was created by the National Kidney Disease Education Program (NKDEP), an initiative of the National Institute of Diabetes and Digestive and Kidney Diseases of the National Institutes of Health. With the goal of reducing the burden of chronic kidney disease (CKD), especially among communities most impacted by the disease, NKDEP works in collaboration with a range of government, nonprofit, and health care organizations to: • raise awareness among people at risk for CKD about the need for testing; • educate people with CKD about how to manage their disease; • provide information, training, and tools to help health care providers better detect and treat CKD; and • support health system change to facilitate effective CKD detection and management. To learn more about NKDEP, please visit: http: //www. nkdep. nih. gov. For additional materials from NIDDK, please visit: http: //www. niddk. nih. gov. Slide 3 of 74

Meet our Presenters Amy Barton Pai, Pharm. D, MHI, FASN, FCCP, FNKF Dr. Barton Pai is Chair of the National Kidney Disease Education Program’s Pharmacy Working Group Dr. Amy Barton Pai, Pharm. D. , MHI, FASN, FCCP, FNKF is Associate Professor of Clinical Pharmacy at the University of Michigan College of Pharmacy. She obtained her Bachelor of Science in Pharmacy from Albany College of Pharmacy in 1996 and then completed a Pharmacy Practice Residency at St. Peter’s Hospital in Albany, New York. She received her Doctor of Pharmacy from Albany College of Pharmacy in 1999. From 1999 -2001 she was a Nephrology Research Fellow at the University of Illinois at Chicago. Dr. Pai was on faculty at the University of New Mexico College of Pharmacy and School of Medicine from 2001 to 2008 and at Albany College of Pharmacy and Health Sciences from 2008 to 2016. She earned a Master's degree in Healthcare Innovation in 2018. Slide 4 of 74

Meet our Presenters Andrew S. Narva, M. D. , F. A. C. P. Dr. Narva is the Director of the National Kidney Disease Education Program (NKDEP) at the National Institutes of Health. Prior to joining the NKDEP in 2006, he served as Director of the Kidney Disease Program for the Indian Health Service (IHS). Dr. Narva continues to serve as the Chief Clinical Consultant for Nephrology for IHS and to provide care for patients at Zuni Pueblo through a telemedicine clinic. Dr. Narva is a member of the American Board of Internal Medicine Nephrology Subspecialty Board. He has served as a member of the Eighth Joint National Committee (JNC 8) Expert Panel, the National Quality Forum Renal Steering Committee, the Kidney Disease Outcomes Quality Initiative Work Group on Diabetes in Chronic Kidney Disease, and the Medical Review Board of End Stage Renal Disease Network 15. Slide 5 of 74

After completing this module, you will be able to: • Describe kidney anatomy and physiologic functions • Define and discuss the pathophysiology of chronic kidney disease (CKD) • Calculate estimated glomerular filtration rate (e. GFR) and urine albumin -to-creatinine ratio (UACR) to assess kidney function and kidney damage and to determine diagnosis • Describe the burden of chronic kidney disease in the US and how pharmacists can improve outcomes for patients Slide 6 of 74
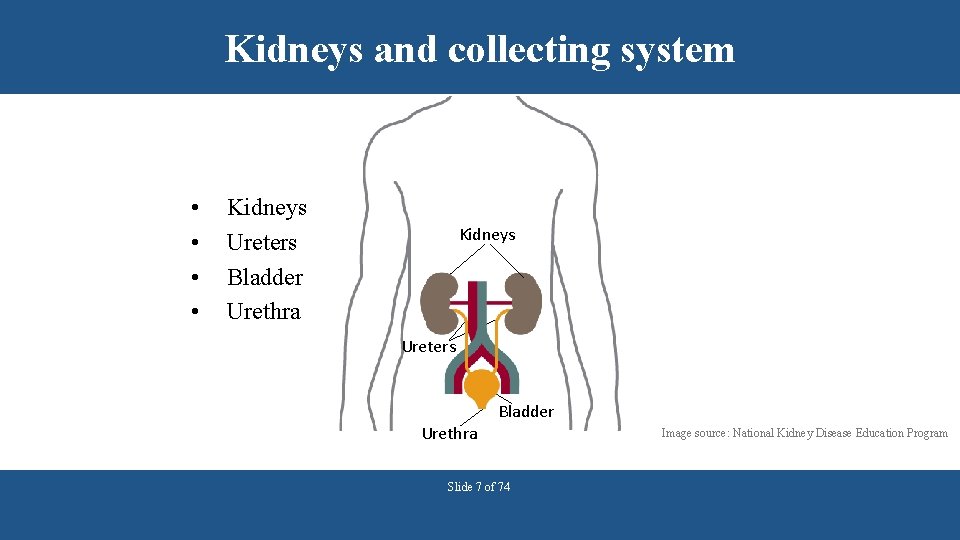
Kidneys and collecting system • • Kidneys Ureters Bladder Urethra Slide 7 of 74 Image source: National Kidney Disease Education Program
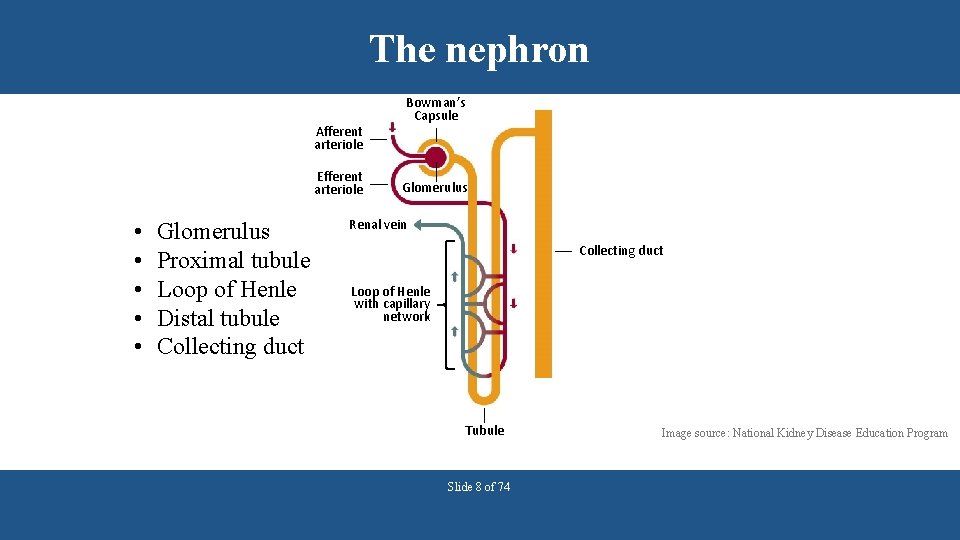
The nephron Afferent arteriole Efferent arteriole • • • Glomerulus Proximal tubule Loop of Henle Distal tubule Collecting duct Bowman’s Capsule Glomerulus Renal vein Collecting duct Loop of Henle with capillary network Tubule Slide 8 of 74 Image source: National Kidney Disease Education Program
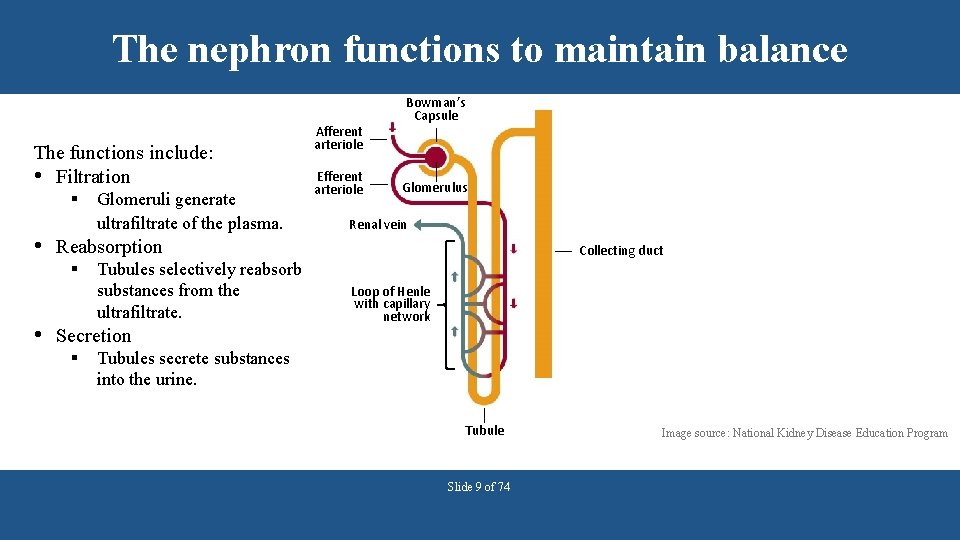
The nephron functions to maintain balance The functions include: • Filtration § Glomeruli generate ultrafiltrate of the plasma. • Reabsorption § Tubules selectively reabsorb substances from the ultrafiltrate. • Secretion § Afferent arteriole Efferent arteriole Bowman’s Capsule Glomerulus Renal vein Collecting duct Loop of Henle with capillary network Tubules secrete substances into the urine. Tubule Slide 9 of 74 Image source: National Kidney Disease Education Program
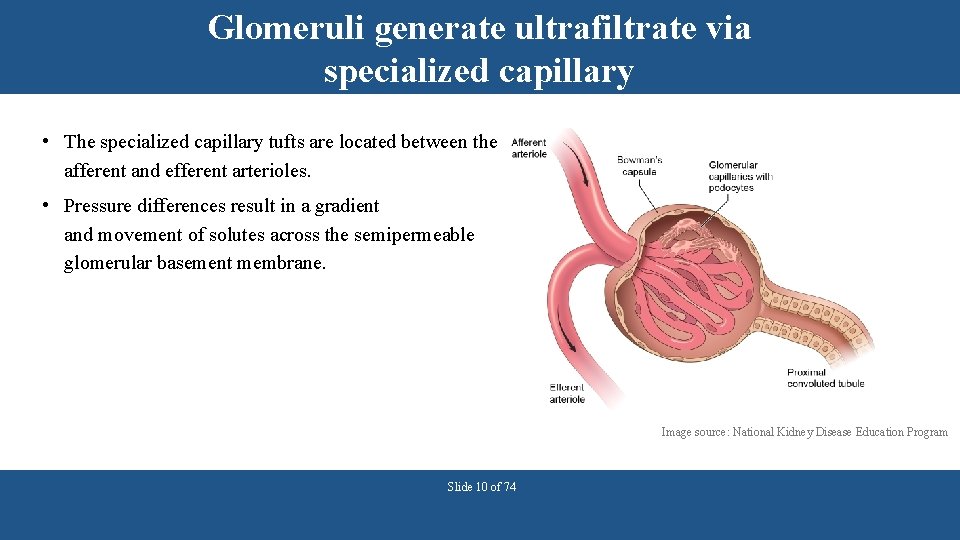
Glomeruli generate ultrafiltrate via specialized capillary • The specialized capillary tufts are located between the afferent and efferent arterioles. • Pressure differences result in a gradient and movement of solutes across the semipermeable glomerular basement membrane. Image source: National Kidney Disease Education Program Slide 10 of 74
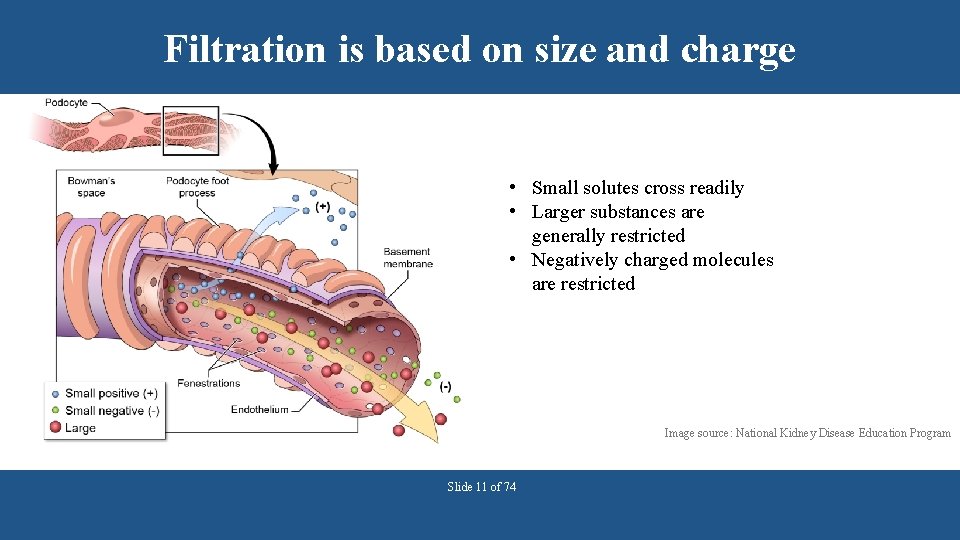
Filtration is based on size and charge • Small solutes cross readily • Larger substances are generally restricted • Negatively charged molecules are restricted Image source: National Kidney Disease Education Program Slide 11 of 74

Ultrafiltration of plasma is the main function of the glomeruli • Volume of ultrafiltrate = 135– 180 liters(L)/day • 99% water reabsorbed -> 1– 1. 5 L urine excreted Slide 12 of 74

The ultrafiltrate is modified by the tubules • Reabsorption and secretion of substances occurs within the tubules. Examples: • Potassium (K) is reabsorbed from and secreted into the urine • Sodium (Na) is generally reabsorbed • Organic acids are secreted into the urine. • Many drugs are actively secreted (e. g. cephalexin, renal clearance rate 252 m. L/min) or reabsorbed (e. g. levofloxacin, renal clearance rate 96 m. L/min) Slide 13 of 74

What happens in the tubules? • Reabsorption and secretion of substances occurs within the tubules. Proximal Tubule Loop of Henle Sodium 67% reabsorbed 25% reabsorbed Potassium 80 -90% reabsorbed - Slide 14 of 74 Distal Tubule Collecting Duct 5% reabsorbed 3% reabsorbed Actively secreted when high K+ intake occurs Reabsorption mediated by aldosterone

The kidneys have many functions • Regulatory function § Control composition and volume of blood § Maintain stable concentrations of inorganic anions such as sodium (Na), potassium (K), and calcium (Ca) § • Maintain acid-base balance Excretory function § § Produce urine Remove metabolic wastes § Including nitrogenous waste Slide 15 of 74
The kidneys have many functions • Endocrine function § Produce renin for blood pressure control § Produce erythropoietin which stimulates bone marrow production of red blood cells § Activate 25(OH)D to 1, 25 (OH)2 D (active vitamin D) • Metabolic function § Gluconeogenesis § Metabolize drugs and endogenous substances (e. g. , insulin) Slide 16 of 74
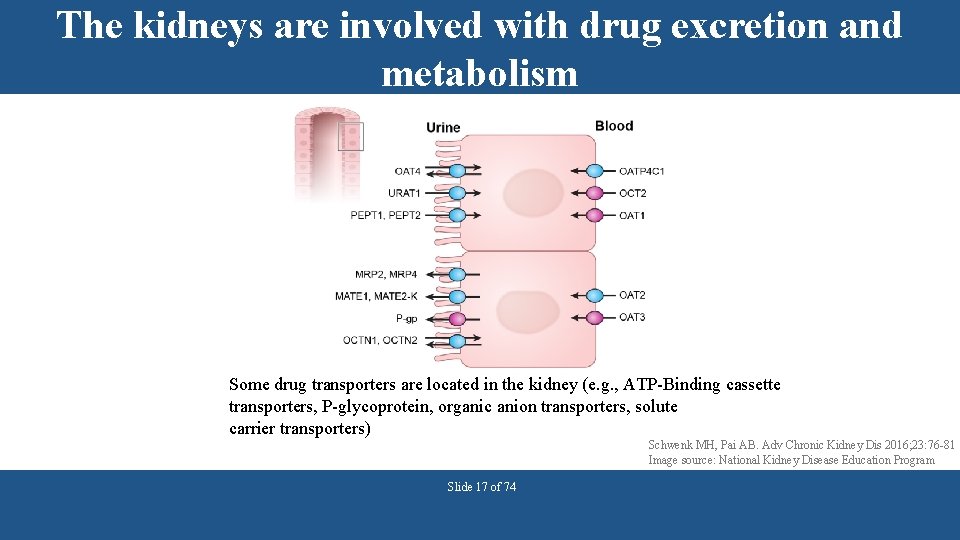
The kidneys are involved with drug excretion and metabolism Some drug transporters are located in the kidney (e. g. , ATP-Binding cassette transporters, P-glycoprotein, organic anion transporters, solute carrier transporters) Schwenk MH, Pai AB. Adv Chronic Kidney Dis 2016; 23: 76 -81 Image source: National Kidney Disease Education Program Slide 17 of 74
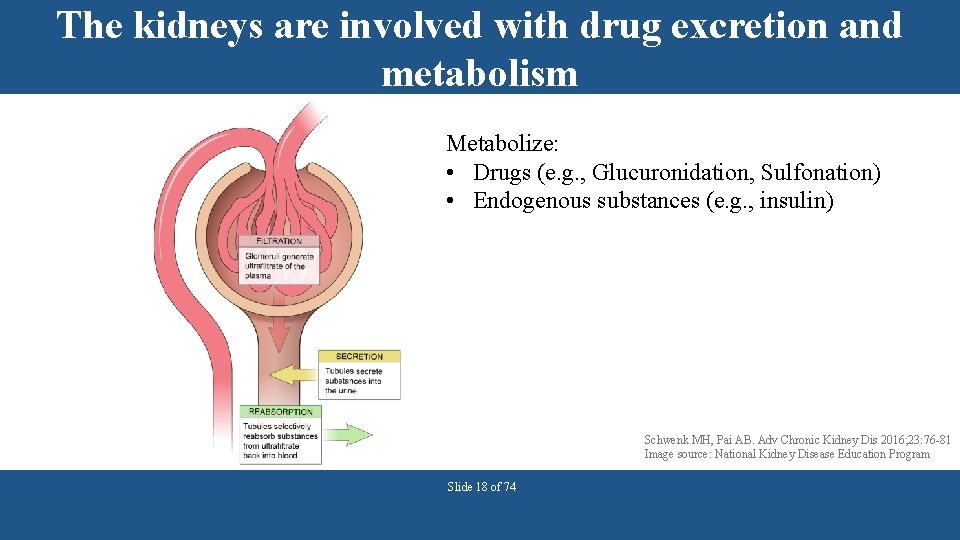
The kidneys are involved with drug excretion and metabolism Metabolize: • Drugs (e. g. , Glucuronidation, Sulfonation) • Endogenous substances (e. g. , insulin) Schwenk MH, Pai AB. Adv Chronic Kidney Dis 2016; 23: 76 -81 Image source: National Kidney Disease Education Program Slide 18 of 74
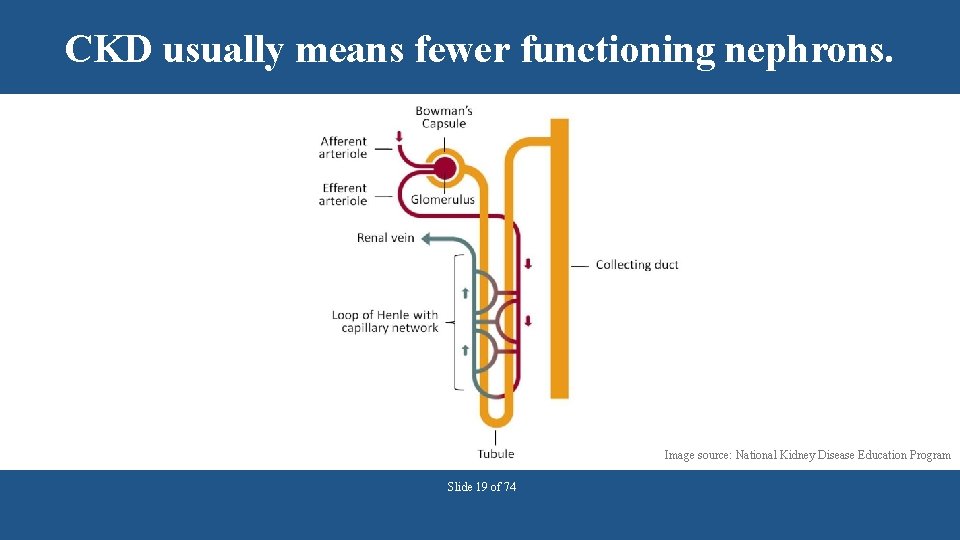
CKD usually means fewer functioning nephrons. Image source: National Kidney Disease Education Program Slide 19 of 74

Fewer nephrons disrupt the balance • Urine volume may not change § Composition of the urine changes • Reduced waste excretion § May not be apparent until CKD is advanced • Altered hormone production § Anemia (erythropoietin) and mineral & bone disorders (vitamin D) • Reduced catabolism § Examples: Insulin, glucagon, drugs Slide 20 of 74

Fewer nephrons disrupt the balance • Reduced renal clearance and accumulation of § § Advanced glycation end products Pro-inflammatory cytokines Reactive oxygen species (oxidation) Metabolic acids • Insulin resistance (even in non-diabetics) § Reduces insulin-mediated glucose uptake in skeletal muscles § May be associated with inflammation as well Slide 21 of 74
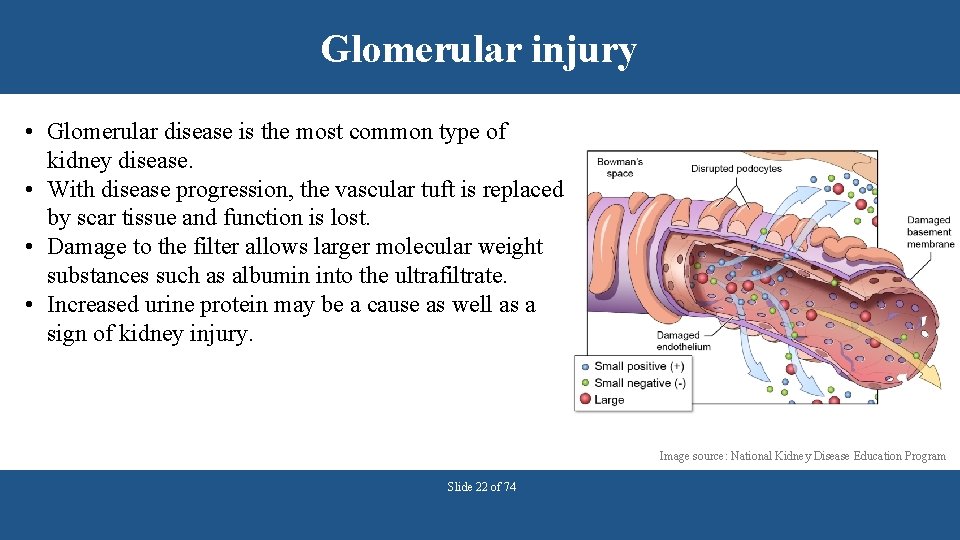
Glomerular injury • Glomerular disease is the most common type of kidney disease. • With disease progression, the vascular tuft is replaced by scar tissue and function is lost. • Damage to the filter allows larger molecular weight substances such as albumin into the ultrafiltrate. • Increased urine protein may be a cause as well as a sign of kidney injury. Image source: National Kidney Disease Education Program Slide 22 of 74

Risk factors for CKD • Diabetes • Hypertension • Family history of kidney disease • Cardiovascular disease • Obesity • Acute kidney injury Slide 23 of 74

Terms Used to Described States of Reduced GFR 1998 and 1999 ASN Abstracts 1. Chronic renal failure 2. Chronic renal insufficiency 3. Mild renal insufficiency 4. Moderate chronic renal insufficiency 5. Moderate or advanced renal insufficiency 6. Severe renal insufficiency 7. Renal dysfunction 8. Severe renal dysfunction 9. Decreased renal function 10. Pre–end-stage renal disease 11. Low clearance (predialysis) patients 12. Pre-uremic 13. Renal failure 14. Renal disease 15. Renal insufficiency 16. Predialysis 17. Mildly elevated serum creatinine 18. Chronic renal failure patients not on dialysis 19. Pre–end-stage chronic renal failure 20. Pre–end-stage renal disease chronic renal failure 21. Mild renal failure 22. Chronic renal disease 23. Chronic renal failure requiring dialysis AJKD 2000; 36: 415 -418 Slide 24 of 74

CKD, regardless of etiology, is reduced kidney function and/or kidney damage • Chronic Kidney Disease § Kidney function § Glomerular filtration rate (GFR) < 60 m. L/min/1. 73 m 2 for > 3 months with or without kidney damage AND/OR § Kidney damage § > 3 months, with or without decreased GFR, manifested by either § Pathological abnormalities § Markers of kidney damage, i. e. , proteinuria (albuminuria) § Urine albumin-to-creatinine ratio (UACR) > 30 mg/g Slide 25 of 74

Each kidney has about 1 million nephrons; slow loss may not be noticeable • Large physiologic reserve. • Slow, progressive loss of functioning nephrons may not be noticeable. • Often, there are no symptoms until more than threequarters of kidney function is lost. Slide 26 of 74

Importance of inflammation • Inflammation may contribute to: § § § Decline in kidney function with aging Albuminuria Cardiovascular disease Malnutrition Anemia Metabolic acidosis • Causes reduced clearance and/or increased production of pro-inflammatory cytokines • Obesity may be an inflammatory state Slide 27 of 74

People with CKD still make urine • The composition of the urine changes. • Most people do notice any difference in urine volume. • Slow, progressive loss of function may not be noticeable. Slide 28 of 74

FUNCTIONAL ASSESSMENT Identify and Monitor CKD. Slide 29 of 74
CKD is reduced kidney function and/or kidney damage • Chronic Kidney Disease § Kidney function § Glomerular Filtration Rate (GFR) < 60 m. L/min/1. 73 m 2 for § > 3 months with or without kidney damage • AND/OR § Kidney damage § > 3 months, with or without decreased GFR, manifested by either § Pathological abnormalities § Markers of kidney damage, e. g. , albuminuria § Urine albumin-to-creatinine ratio (UACR) > 30 mg/g Reference: National Kidney Foundation, 2002 Slide 30 of 74

What is the GFR? • GFR is equal to the sum of the filtration rates in all of the functioning nephrons. • GFR is not routinely measured in clinical settings. • Estimation of the GFR (e. GFR) gives a rough measure of the number of functioning nephrons. • Cardiac output (CO) = 6 L/min § x 20% of CO goes to kidneys = 1. 2 L/min § x Plasma is 50% blood volume = 600 m. L/min § x Filtration Fraction of 20% = 120 m. L/min Slide 31 of 74

Approaches to Estimate Kidney Function • Cockcroft-Gault estimates creatinine clearance • Modification of Diet in Renal Disease (MDRD) • Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) Slide 32 of 74

“Normal” serum creatinine may not be normal • • Serum creatinine levels reflect muscle mass, age, gender and race • A 28 -year-old African American man with serum creatinine of 1. 2 has an e. GFR > 60. • A 78 -year-old white woman with serum creatinine of 1. 2 has an e. GFR of 43. A typical “normal” reference range of 0. 6– 1. 2 mg/d. L listed on many lab reports does not account for muscle mass, age, gender, and race. Slide 33 of 74

Cockcroft-Gault Background • Developed to predict creatinine clearance (Cr. Cl) using 24 -hour creatinine excretion per weight (kg) • Used actual body weight • Based on 249 men (aged 18 -92) • Cr. Cl ranged between 30 -130 m. L/m 2 (not adjusted for body surface area) • The equation “assumes” females would be 15% lower creatinine clearance at the same level of serum creatinine (s. Cr) Cockcroft DW, Gault MH. Nephron 1976; 16: 31 -41 Demirovic JA, Pai AB, Pai MP. Am J Health Syst Pharm. 2009; 66(7): 642 -8. Slide 34 of 74

Estimating Equations for e. GFR • The Modification of Diet in Renal Disease (MDRD) and CKDEPI study equations are most widely used for estimating GFR. • The variables are serum creatinine, age, race, and gender. • MDRD e. GFR = 175 x (Standardized Scr)-1. 154 x (age)-0. 203 x (0. 742 if female) x (1. 212 if African American) • CKD-EPI e. GFR = 141 × min (Scr /κ, 1)α × max(Scr /κ, 1)-1. 209 × 0. 993 Age × 1. 018 [if female] × 1. 159 [if African American] • The estimate is normalized to body surface area. Slide 35 of 74

e. GFR estimates the measured GFR • e. GFR is not the measured GFR. • Estimating equations are derived from population-based studies. • The performance measurement of the estimating equation is the P 30 • P 30 refers to the percent of GFR estimates that are within 30% of m. GFR Slide 36 of 74

What does this mean? MDRD: There is an 77. 2% chance that the estimated GFR (for patients with e. GFR <60) is +/- 30% of the measured GFR § e. g a patient with an e. GFR of 59 has an 77. 2% chance of having a measured GFR between 42 and 78 vs CKD-Epi: There is an 79. 9% chance that the estimated GFR (for patients with e. GFR <60) is +/- 30% of the measured GFR § e. g a patient with an e. GFR of 59 has an 79. 9% chance of having a measured GFR between 42 and 78 Slide 37 of 74

Decreased Kidney Function vs Kidney Disease • Estimating equations are less reliable at higher GFR • Kidney function declines with age • While there is an association between decreased e. GFR and morbidity, even in elderly, this association does not mean causality • Use diagnostic terms denoting disease with caution, especially in older people without evidence of kidney damage (e. g. elderly with e. GFR 55) Slide 38 of 74

Creatinine-based estimates of kidney function have limitations • Do not use with: § Rapidly changing creatinine levels § § § Example: acute kidney injury Extremes in muscle mass, body size, or altered diet patterns Medications that interfere with the measurement of serum creatinine Slide 39 of 74
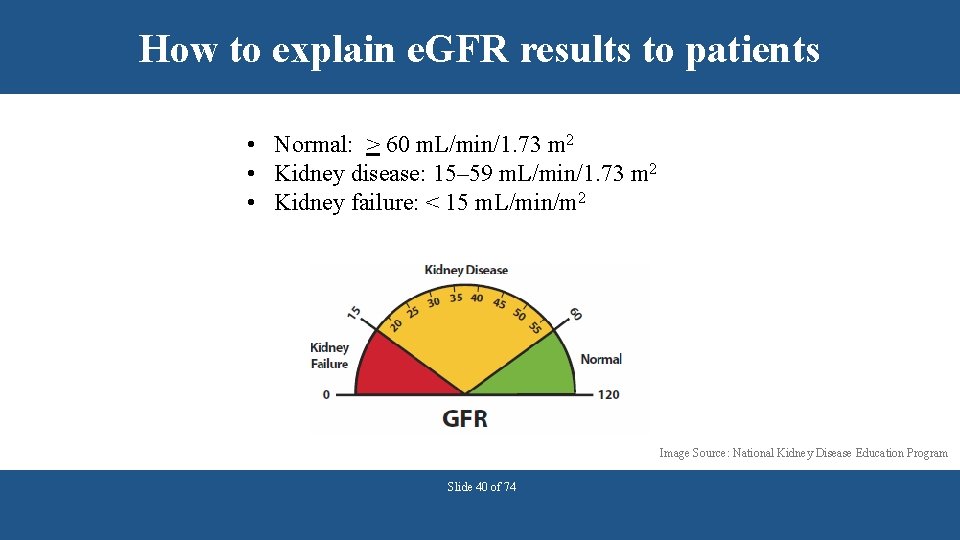
How to explain e. GFR results to patients • Normal: > 60 m. L/min/1. 73 m 2 • Kidney disease: 15– 59 m. L/min/1. 73 m 2 • Kidney failure: < 15 m. L/min/m 2 Image Source: National Kidney Disease Education Program Slide 40 of 74

KIDNEY DAMAGE Use urine albumin-to-creatinine ratio (UACR) to assess and monitor. Slide 41 of 74
CKD is reduced kidney function and/or KIDNEY DAMAGE • Chronic kidney disease § Kidney function § GFR < 60 m. L/min/1. 73 m 2 for > 3 months with or without kidney damage AND/OR § Kidney damage § > 3 months, with or without decreased GFR, manifested by either § Pathological abnormalities § Markers of kidney damage, e. g. , albuminuria § Urine albumin-to-creatinine ratio (UACR) > 30 mg/g Slide 42 of 74

Urine albumin results are used for screening, diagnosing, and treating CKD • An abnormal urine albumin level is often the earliest marker for kidney disease complicating diabetes • Important prognostic marker, especially in diabetes • Used to monitor and guide therapy • Tool for patient education and self-management (such as A 1 C or e. GFR) Slide 43 of 74

Proteins are filtered based on size and electrical charge • Low-molecular-weight proteins cross the glomerulus. • High-molecular-weight proteins do not cross the glomerulus normally. • Negatively charged molecules usually are restricted from crossing the glomerulus. • Drugs bound to albumin are not filtered into urine • Reduced albumin from albuminuria reduces drug binding sites and can increase free drug concentrations Slide 44 of 74

Damaged kidneys allow albumin to cross the filtration barrier into the urine • Increased glomerular permeability allows albumin (and other proteins) to cross the glomerulus into the urine. • Higher levels of protein within the tubule may exacerbate kidney damage. § Proteins may exceed tubules’ ability to reabsorb. Slide 45 of 74

Very little albumin or protein is normally excreted into urine • Currently accepted “normal” level ≤ 30 mg/g § § Albumin is a medium-size molecular-weight protein with a negative charge. Most is reabsorbed by the tubules. • Normal urine protein is < 150 mg/day § Includes albumin and other proteins. Reference: Danziger J. Mayo Clinical Proceedings, 2008 Slide 46 of 74

Use urine albumin-to-creatinine ratio (UACR) for urine albumin assessment • UACR uses a spot urine sample. • In adults, ratio of urine albumin to creatinine correlates closely to total albumin excretion. • Ratio is between two measured substances (not dipstick). Urine albumin (mg/d. L) = UACR (mg/g) Albumin excretion in mg/day Urine creatinine (g/d. L) • UACR of 30 mg/g is generally the most widely used cutoff for “normal. ” Reference: http: //nkdep. nih. gov/resources/uacr_gfr_quickreference. htm Slide 47 of 74

UACR quantifies all levels of urine albumin • UACR is a continuous variable. • The term albuminuria describes all levels of urine albumin. • The term microalbuminuria describes abnormal urine albumin levels not detected by dipstick test. § 30 mg/g – 300 mg/g • The term macroalbuminuria describes urine albumin > 300 mg/g. Slide 48 of 74
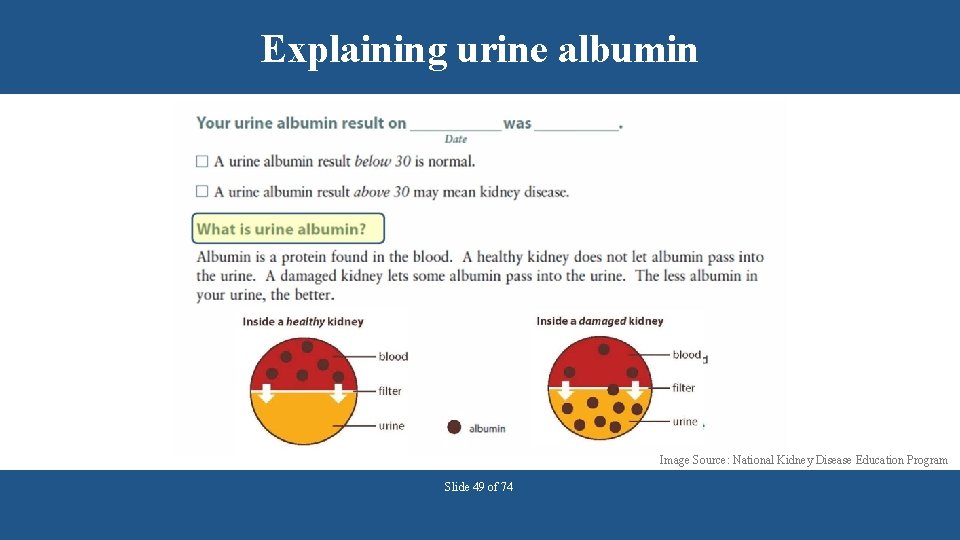
Explaining urine albumin Image Source: National Kidney Disease Education Program Slide 49 of 74

DESCRIBING THE BURDEN OF CKD Slide 50 of 74
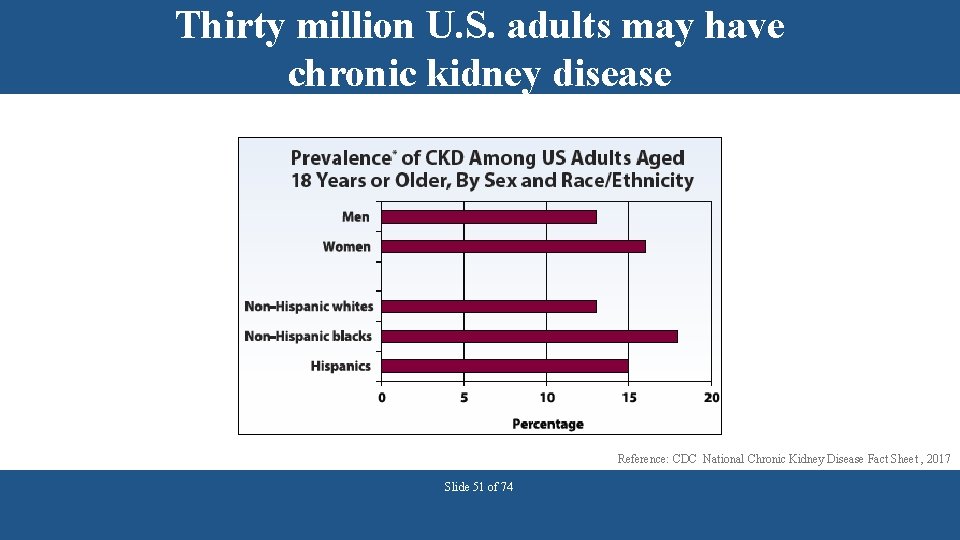
Thirty million U. S. adults may have chronic kidney disease Reference: CDC National Chronic Kidney Disease Fact Sheet , 2017 Slide 51 of 74
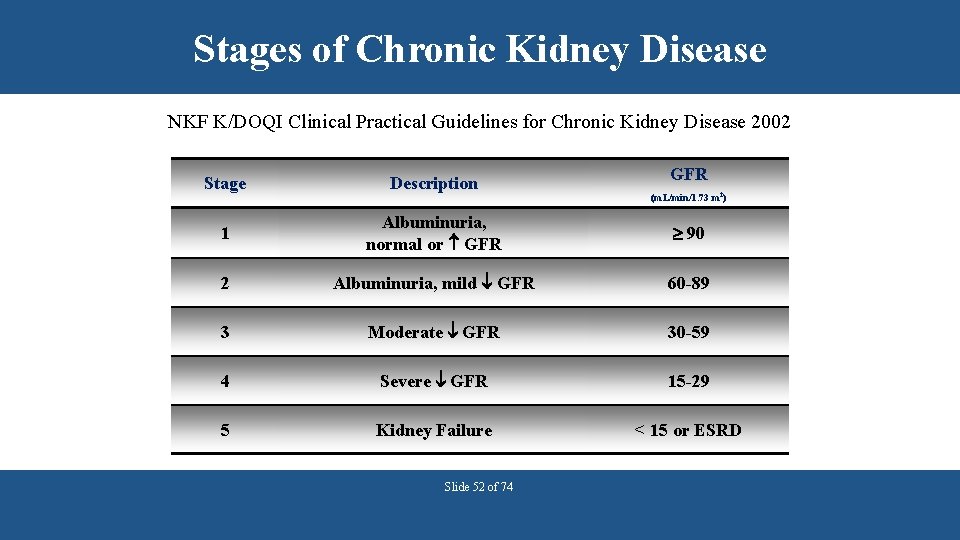
Stages of Chronic Kidney Disease NKF K/DOQI Clinical Practical Guidelines for Chronic Kidney Disease 2002 GFR Stage Description 1 Albuminuria, normal or GFR 90 2 Albuminuria, mild GFR 60 -89 3 Moderate GFR 30 -59 4 Severe GFR 15 -29 5 Kidney Failure < 15 or ESRD Slide 52 of 74 (m. L/min/1. 73 m 2)
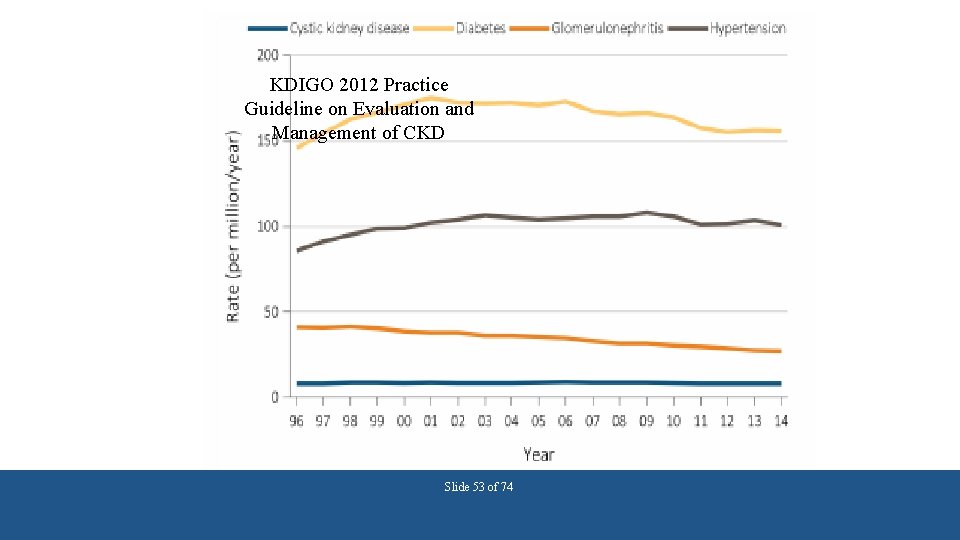
KDIGO 2012 Practice Guideline on Evaluation and Management of CKD Slide 53 of 74

Uses of CKD Staging System • • • Determining incidence and prevalence of CKD Association with cardiovascular risk Risk prediction for end stage kidney disease US and global burden of kidney disease Public health messaging Population health management Slide 54 of 74
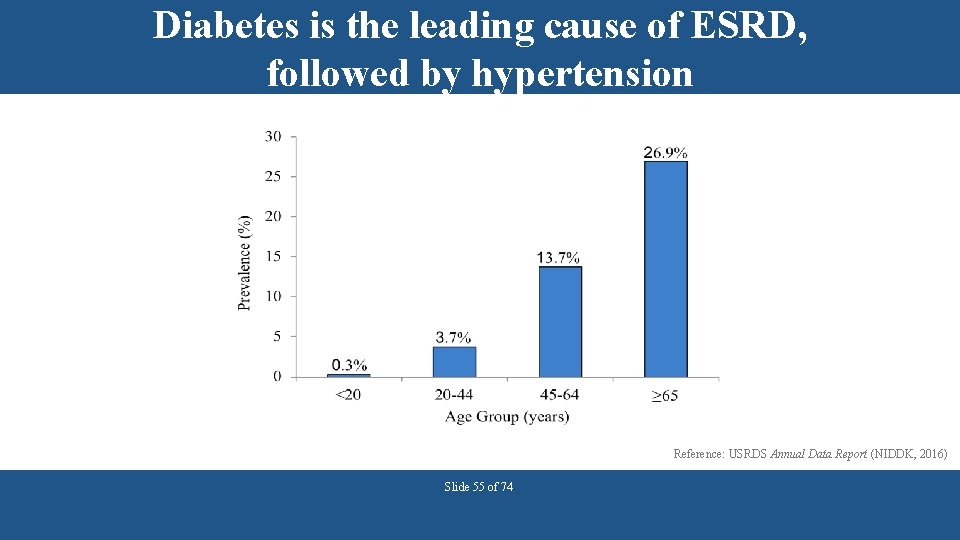
Diabetes is the leading cause of ESRD, followed by hypertension Reference: USRDS Annual Data Report (NIDDK, 2016) Slide 55 of 74
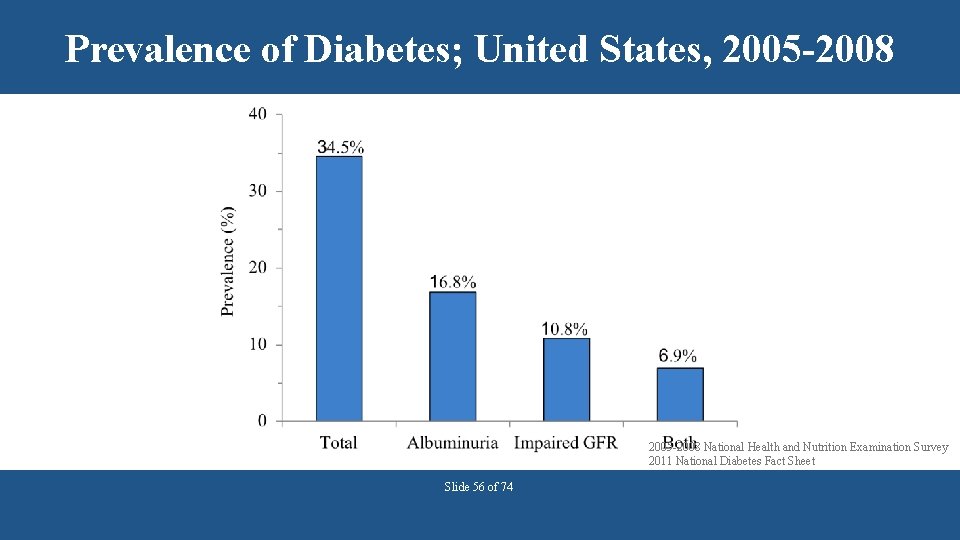
Prevalence of Diabetes; United States, 2005 -2008 National Health and Nutrition Examination Survey 2011 National Diabetes Fact Sheet Slide 56 of 74
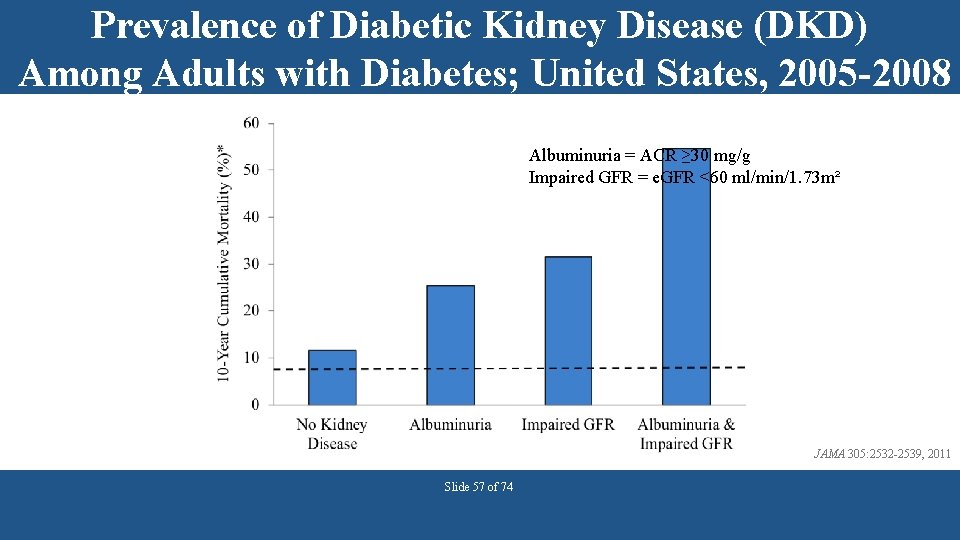
Prevalence of Diabetic Kidney Disease (DKD) Among Adults with Diabetes; United States, 2005 -2008 Albuminuria = ACR ≥ 30 mg/g Impaired GFR = e. GFR <60 ml/min/1. 73 m² JAMA 305: 2532 -2539, 2011 Slide 57 of 74
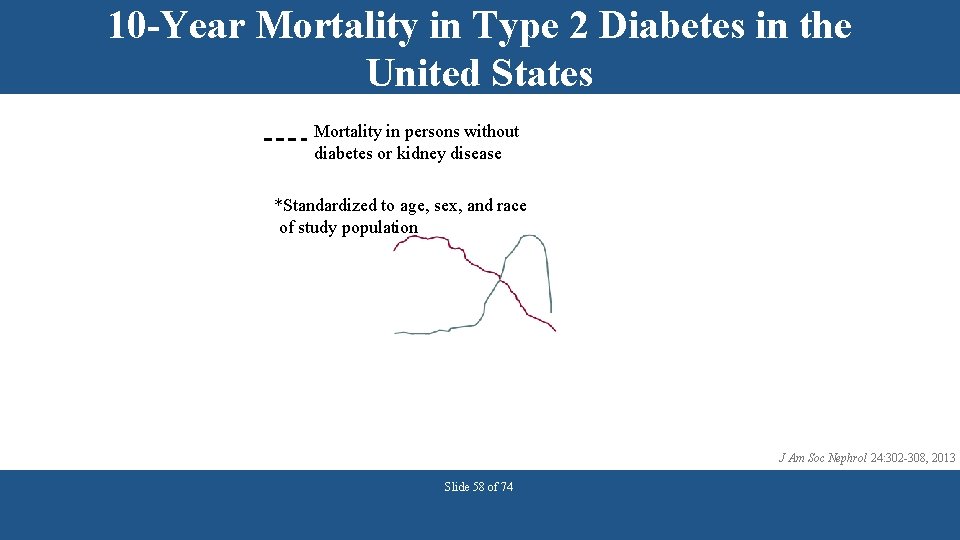
10 -Year Mortality in Type 2 Diabetes in the United States Mortality in persons without diabetes or kidney disease *Standardized to age, sex, and race of study population J Am Soc Nephrol 24: 302 -308, 2013 Slide 58 of 74
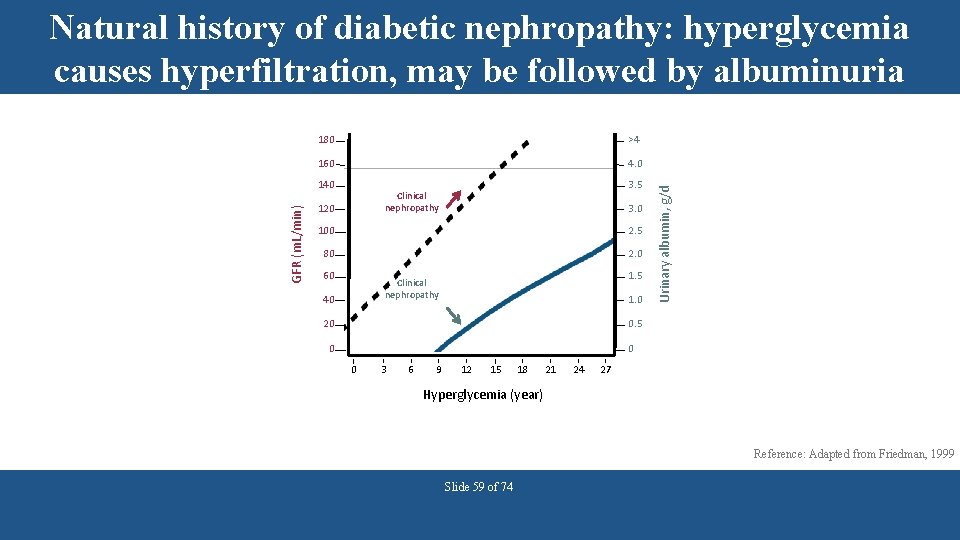
180 >4 160 4. 0 GFR (m. L/min) 140 3. 5 Clinical nephropathy 120 3. 0 100 2. 5 80 2. 0 60 1. 5 Clinical nephropathy 40 1. 0 20 Urinary albumin, g/d Natural history of diabetic nephropathy: hyperglycemia causes hyperfiltration, may be followed by albuminuria 0. 5 0 0 0 3 6 9 12 15 18 21 24 27 Hyperglycemia (year) Reference: Adapted from Friedman, 1999 Slide 59 of 74

…however • Microalbuminuria can regress § de Boer IH et al, Arch Int Med 2011 • Impaired GFR can develop without albuminuria § Molitch M et al, Diabetes Care 2010 • Disease heterogeneity often not reflected by GFR § Bohle et al. American Journal of Nephrology, 1987 Slide 60 of 74
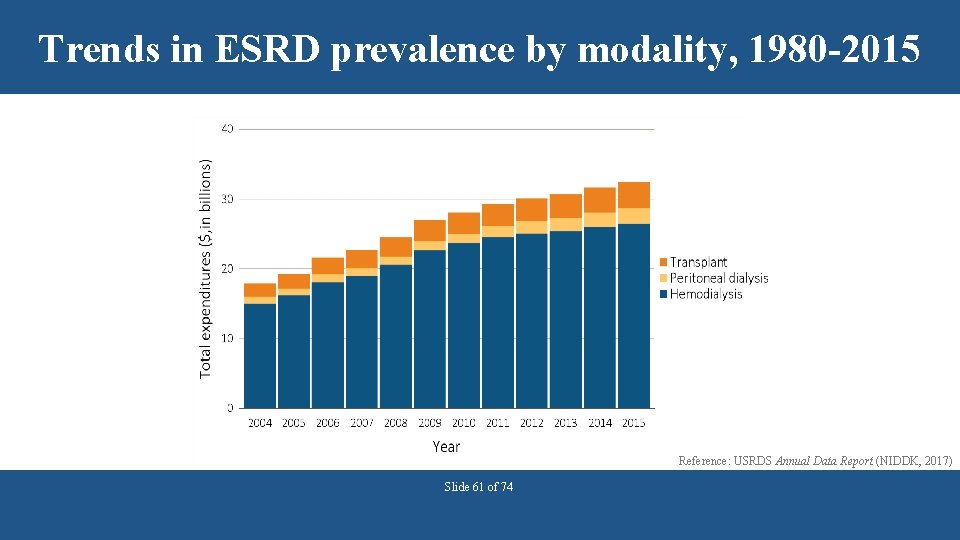
Trends in ESRD prevalence by modality, 1980 -2015 Reference: USRDS Annual Data Report (NIDDK, 2017) Slide 61 of 74

Delaying the need for Renal Replacement Therapy (RRT) may be cost-effective. • • • Hemodialysis $26. 7 billion ($88, 195 per patient) Peritoneal Dialysis $ 2. 1 billon ($75, 140 per patient) Transplantation $ 3. 3 billion ($34, 800 per patient) • ESRD data do not include Medicare Part D cost Slide 62 of 74 Reference: USRDS Annual Data Report (NIDDK, 2017)

IMPORTANCE OF THE PHARMACIST’S ROLE IN CHRONIC KIDNEY DISEASE Slide 63 of 74

Key Issues in Managing CKD • • • Ensure the diagnosis is correct Monitor progression Implement appropriate therapy to slow progression Screen for CKD complications Treat CVD risk Avoid acute kidney injury (e. g. NSAIDs) Refer to a dietitian Educate the patient about CKD Begin the conversation about renal replacement therapy Slide 64 of 74

Challenges to Improving CKD Care • CKD remains under diagnosed • Implementation of recommended care is poor • Many clinicians feel inadequately educated § Uncertain about how to interpret diagnostic tests § Unclear about clinical recommendations § Low confidence in their ability to successfully manage CKD § Indications for, and process of, referral poorly defined Slide 65 of 74

Awareness & Knowledge about CKD in Patients Seen by Nephrologists Low Self-Rating Perceived Knowledge N=676 No Knowledge of Hemodialysis / Peritoneal Dialysis Little or No Knowledge Re: Diagnosis 43% / 57% 35% Finkelstein, et al. Kidney International, 2008 Limited Awareness & Objective Knowledge N=401 Unaware of CKD diagnosis 31% Do not understand CKD implications, e. g. heart disease 34% Do not understand kidney functions, e. g. urine production 34% Do not understand terminology, GFR 32% Wright, et al. AJKD 2011 Slide 66 of 74

Pharmacists are Pivotal Members of the Multi-disciplinary Team! “The clinician will need to adopt an appropriate system for monitoring individual patients… Pharmacists are a valuable resource for identifying potential drug interactions, interpreting the clinical relevance of known interactions and developing monitoring plans based on pharmacodynamic and pharmacokinetic characteristics of individual agents” http: //www 2. kidney. org/professionals/KDOQI/guidelines_bp/guide_7. htm Slide 67 of 74

Why is it important to have pharmacists on board? • The prevalence of medication-related problems (MRPs) increases as CKD progresses because the medication usage increases. • Patients with stage 3 and 4 CKD are prescribed approximately 6 to 8 medications. • Stage 5 patients are prescribed an average of 12 medications to treat on an average 5 to 6 chronic medical conditions • These patients are at a high risk for MRPs and it is associated with significant costs to the healthcare system. Cardone KE et al. Adv Chronic Kidney Dis. 2010 Sep; 17(5): 404 -12. Slide 68 of 74

Medication-related Problems Problem Description Example(s) Indication without drug therapy (IWD) Patient is not receiving medication therapy for a diagnosed medical condition A patient with an elevated LDL level not taking a lipid lowering medication Drug use without indication (DWI) Use of a medication without a medically valid indication Failure to discontinue diuretic therapy in an anuric patient Improper drug selection (IDS) Medication of choice is not being used Initiating a calcium-based phosphate binder in a hypercalcemic hemodialysis patient Subtherapeutic dosage Patient has a medical problem that is A hemodialysis patient continues to receive (UD) being treated with too little of a the same dose of sevelamer carbonate despite correct medication serum phosphorus levels of 6. 3 Overdose (OD) Patient has a medical problem that is Not adjusting the dose of renally cleared being treated with too much of the medications in patients with CKD correct medication Adverse drug reaction Drug effects that are unwanted, (ADR) unpleasant, or harmful • Nonproductive cough associated with ACE inhibitor therapy • Rhabdomyolysis resulting from statin use Cardone KE et al. Adv Chronic Kidney Dis. 2010 Sep; 17(5): 404 -12. Slide 69 of 74
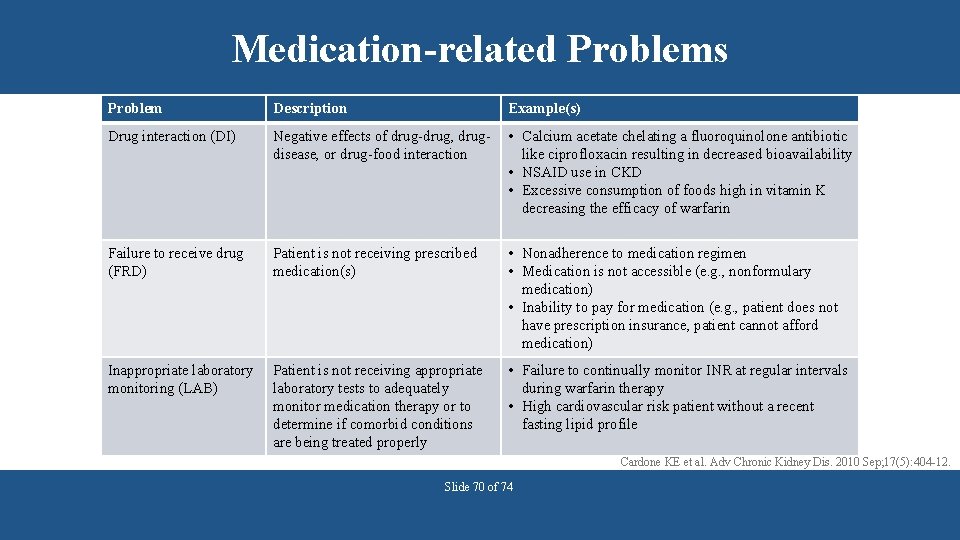

Medication-related Problems Problem Description Example(s) Drug interaction (DI) Negative effects of drug-drug, drugdisease, or drug-food interaction • Calcium acetate chelating a fluoroquinolone antibiotic like ciprofloxacin resulting in decreased bioavailability • NSAID use in CKD • Excessive consumption of foods high in vitamin K decreasing the efficacy of warfarin Failure to receive drug (FRD) Patient is not receiving prescribed medication(s) • Nonadherence to medication regimen • Medication is not accessible (e. g. , nonformulary medication) • Inability to pay for medication (e. g. , patient does not have prescription insurance, patient cannot afford medication) Inappropriate laboratory monitoring (LAB) Patient is not receiving appropriate laboratory tests to adequately monitor medication therapy or to determine if comorbid conditions are being treated properly • Failure to continually monitor INR at regular intervals during warfarin therapy • High cardiovascular risk patient without a recent fasting lipid profile Cardone KE et al. Adv Chronic Kidney Dis. 2010 Sep; 17(5): 404 -12. Slide 70 of 74

Trials on Medication-related Problems in CKD/ESRD Author(s) Year Result Pai and colleagues 2009 HD patient group who had the drug regimen reviewed by a clinical pharmacist was associated with fewer drug use, fewer all-cause hospitalizations and shorter cumulative time of hospitalization compared with patient group who had the drug regimen reviewed by a nurse. Hug and colleagues 2009 Of ADE that occurred in 900 patients with acute or chronic kidney damage, 91% were preventable and 51% were significant. All preventable events could have been detected by renal dosing checking. Pai and colleagues 2009 Quality of Life at 1 -year was significantly worse in several domains in the patient group who had the drug regimen reviewed by a nurse compared with patient group who had the drug regimen reviewed by a clinical pharmacist. Cabello-Muriel and colleagues 2014 Study showed significant improvement in Cr. Cl among patients with advanced CKD and taking nephrotoxic medications in the pharmacist intervention group (Renal dose adjustments in nephrotoxic med). ADE: adverse drug events; Cr. Cl: Creatinine Clearance; HD: hemodialysis; MRP: Medication-related problems; RQLP: Renal Quality of Life Profile Slide 71 of 74 Pai AB et al, Pharmacotherapy 2009; 29: 1433 -40. Hug BL et al. Kidney Int 2009; 76: 1192 -98. Pai AB, et al. Hemodial Int 2009; 13: 72 -9. Cabello-Muriel A, et al. Int J Clin Pharm. 2014; 36(5): 896 -903.

Population Health and CKD • CKD is best addressed through population management • Improvement in care results from changes implemented by in the community and in the clinic by all health professionals • Implemented through diabetes care delivery system; not specialty clinic based Slide 72 of 74

Integrated Approaches Reduce Burden of CKD Slide 73 of 74

Pharmacists in Team-based care • In a report to the Surgeon General from the Office of the Chief Pharmacist four key focal points were outlined to expand the scope of pharmacy practice: § Pharmacists integrated as healthcare professionals in federal programs (e. g. Indian Health Service and Veterans Affairs) improve quality and access to care. § Pharmacists need to be recognized as providers § Compensation mechanisms need to be expanded to support growth of pharmacist in team-based care. § The evidence is supporting pharmacists in team based care models improving preventative medicine and reducing total cost of care is strong Giberson S, Yoder S, Lee MP. Improving Patient and Health System Outcomes through Advanced Pharmacy Practice. A Report to the U. S. Surgeon General. Rockville, MD: Office of the Chief Pharmacist, US Public Health Service; 2011. Slide 74 of 74

- Slides: 75