MODULE 1 INTERAGENCY GENDERBASED VIOLENCE CASE MANAGEMENT TRAINING

MODULE 1 INTERAGENCY GENDER-BASED VIOLENCE CASE MANAGEMENT TRAINING

MODULE 12 STEP 2: ASSESSMENT

Use supportive communication to facilitate disclosure OBJECTIVES Develop an understanding of the survivor’s situation and context Conduct a thorough assessment of a survivor’s needs
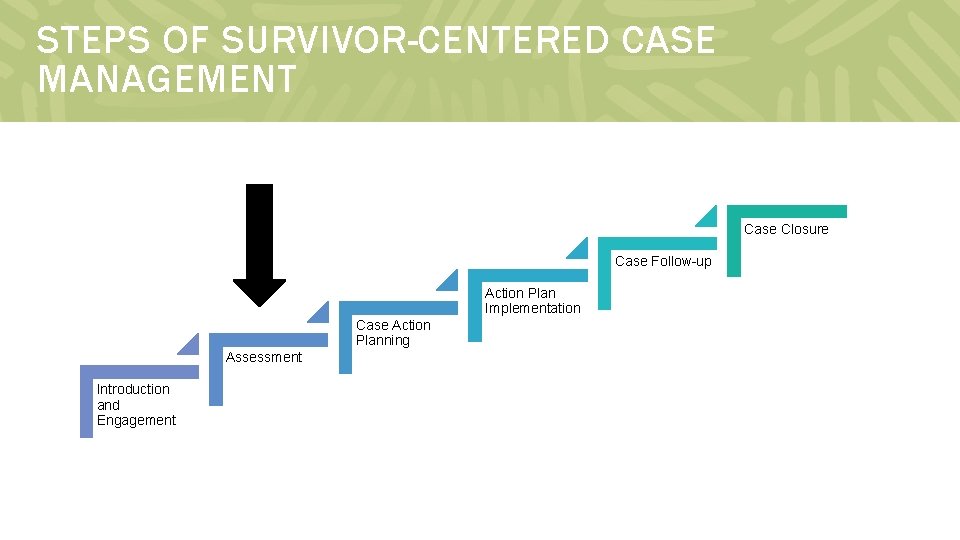
STEPS OF SURVIVOR-CENTERED CASE MANAGEMENT Case Closure Case Follow-up Action Plan Implementation Case Action Planning Assessment Introduction and Engagement

STEP 2 Purpose: Good case management relies on conducting a good assessment Step 2: Assessment ü Determine if other responders are involved ü Understand who the survivor is ü Invite the survivor to tell you what happened ü Listen well ü Respond with validation, compassion and information ü Identify the survivor’s concerns and key needs ü Document relevant information on a form or in case notes if you have a safe case documentation and storage

ACTIVITY: ASSESSMENT In small groups, discuss: What is assessment? What makes for a good assessment? Be prepared to share with the larger group.

ASSESSMENT – WHAT IS IT? The act of gathering information or data from a client and evaluating it for the purpose of making decisions with the client about her/his care. • Safely and slowly assess the survivor’s situation and her/his experience of violence • The focus of the assessment is listening, not asking

The facilitator and a volunteer will role play a scenario between a caseworker and a survivor who is having an emergency. ACTIVITY: PRE-ASSESSMENT Watch the role play individually. Think about: What did the caseworker do well? What did the caseworker not do well? Did anything surprise you? After, we will discuss as a larger group.

PRE-ASSESSMENT ACTIVITIES • Ask the survivor about their immediate safety • Address any urgent medical needs • Determine if other service providers have already been involved Does the survivor feel safe here? Does the perpetrator know where to find her now? If safety is in question, take immediate action If there are immediate emergency medical needs (severe bleeding, extreme pain) take action to get medical help with the survivor’s verbal consent. Has the survivor already reported her case to another organization? If so, give them the option of telling you again or giving consent for you to speak with the organization.
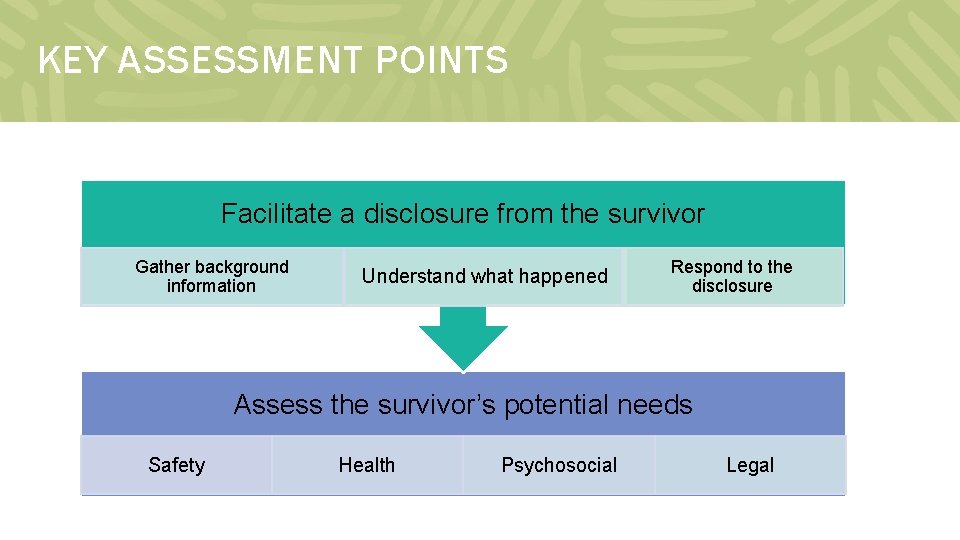
KEY ASSESSMENT POINTS Facilitate a disclosure from the survivor Gather background information Understand what happened Respond to the disclosure Assess the survivor’s potential needs Safety Health Psychosocial Legal

FACILITATING DISCLOSURE ØBegin the conversation with basic questions ØListen carefully to the story as the survivor tells it ØWatch the survivor’s body language closely for any signs of discomfort ØEncourage and empathize through non-verbal and verbal communication ØActively check in with her along the way ØRespect the survivor’s desire to stop sharing information ØAsk clarifying questions once the survivor has finished or has paused ØAvoid unnecessary questions and interruptions ØTake notes if needed, but focus on the survivor

BACKGROUND INFORMATION- WHO IS THE SURVIVOR? • Understand who the survivor is • Basic, essential information, less threatening topics: • The survivor’s age (approximate) • Current living situation • Family situation • Occupation or role in the community Don’t ask the person a list of questions, instead, begin the conversation with an open-ended question that invites the person to tell you about her/himself.

UNDERSTAND WHAT HAPPENED • Nature of the violence/abuse • • Do not need to have all of the details about the violence Important to know if physical force and weapons were used Know if there is severe pain, bleeding, and if there was vaginal/anal penetration *Immediate medical treatment is highly recommended in these cases* Who the perpetrator is and their access to the survivor • • • Relationship of the perpetrator to the survivor and her family Where the perpetrator is now If the perpetrator can access the survivor easily The occupation of the perpetrator or his role in the community The number of perpetrators

UNDERSTAND WHAT HAPPENED • When the last incident took place • • • Urgency of a medical referral Accurately informing the survivor about medical options Frequency • • History of recurring abuse, focus on most recent to understand current needs * this does not mean that the most recent incident is the most significant* Survivors do not need to recount every incident of abuse during an initial interview

ACTIVITY: FACILITATING DISCLOSURE § In groups of four, select one person to be the caseworker and one person to be the survivor. The caseworker and survivor will each be given a handout with a script/background. § Role play the scenario of “bad interviewing. ” Observing group members should take notes. As a group, discuss: what you would do differently? § Be prepared to share with the larger group.
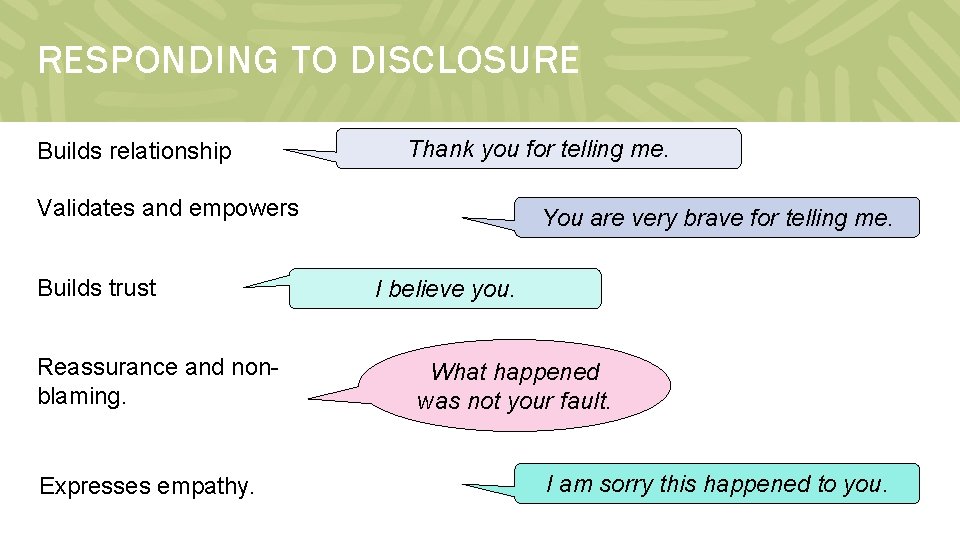
RESPONDING TO DISCLOSURE Builds relationship Thank you for telling me. Validates and empowers Builds trust Reassurance and nonblaming. Expresses empathy. You are very brave for telling me. I believe you. What happened was not your fault. I am sorry this happened to you.
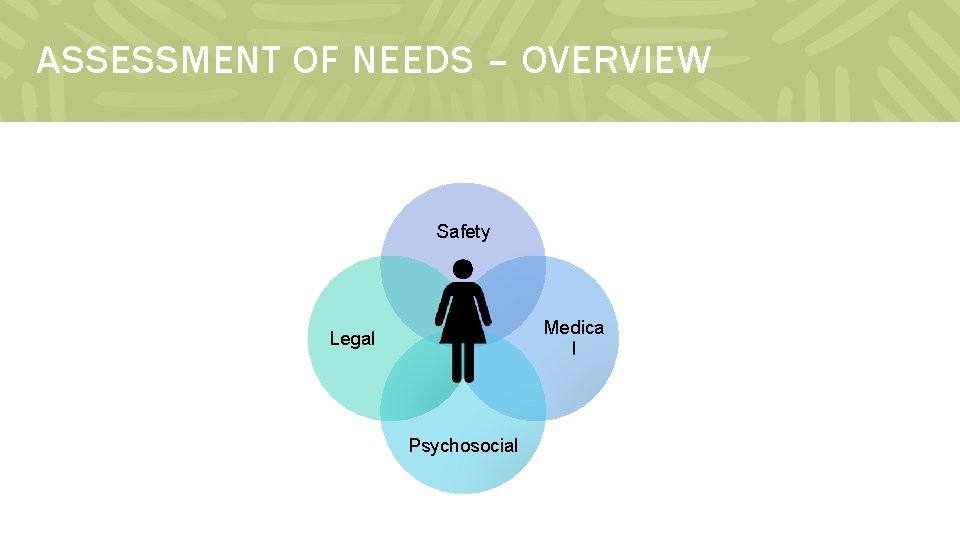
ASSESSMENT OF NEEDS – OVERVIEW Safety Medica l Legal Psychosocial

SAFETY ASSESSMENT Determine the level of the survivor’s safety by understanding: • Survivor’s sense of safety in the home • Survivor’s sense of safety in the community • Survivor’s identified safety/support systems

SAFETY NEEDS – HOW TO ASSESS • Listen for situations, circumstances, and people that are harming the survivor • If it will be understood in your context, use a scale (1 -5) to gauge the survivor’s sense of safety in different situations • Identify who the survivor does not feel safe with and why • Identify what places they do not feel in and why • In cases of Intimate Partner Violence, assess perpetrator-specific safety and risks • Safety assessment Safety plan

HEALTH ASSESSMENT Identify if a medical referral is needed by evaluating: • The survivor’s willingness or desire to receive a medical check-up • The survivor’s desire to have counselling about her options in case of pregnancy (if available) • The survivor’s desire to undergo voluntary HIV/STI counseling and testing (if available)

HEALTH NEEDS – HOW TO ASSESS • Listen for potential medical implications while the survivor is telling her story • Understand the nature of the incident (rape/sexual assault, physical abuse) • Obtain the date/timing of the last incident • Find out if the survivor is in pain or has any injuries

HEALTH ASSESSMENT – LEVEL OF URGENCY EMERGENCY NEEDS: Non-Urgent Needs: • If the incident was within the last 120 • STIs including chlamydia, gonorrhea, hours and/or the survivor is injured or in syphilis can be treated with antibiotics pain: • Hepatitis B vaccinations can be given up • Prevention of HIV (within 72 hours) to 14 days after exposure • Prevention of pregnancy (within 120 hours) • Medical stabilization/treatment • Incontinence of urine or stool may indicate severe complications (fistula, rectal-sphincter damage) • Physical and genital exams and • Forensic evidence collection (within 6 -48 laboratory tests are recommended hours)

PSYCHOSOCIAL ASSESSMENT Determine the survivor’s emotional state and functioning by: • Observing the survivor’s communication and behavior • Conducting a basic assessment of the survivor’s functioning • Asking the survivor about changes in their thinking and behavior since the abuse occurred

PSYCHOSOCIAL NEEDS – HOW TO ASSESS Get a basic sense of how the survivor Do they look frazzled or disorganized? is feeling Assess any changes in their feelings Use a scale from 1 -5, pictures, or emotion or behavior faces Look/listen for indicators the survivor: Observe appearance and behavior Assess the person’s ability to maintain normal functioning Has stopped doing daily activities Has stopped leaving the house Has stopped talking with or seeing family and friends Is having trouble sleeping Has changed eating habits Feels sad most of the time Complains of physical aches Expresses that they feel hopeless

PSYCHOSOCIAL NEEDS – HOW TO ASSESS Assess opportunities for education and livelihoods: • Source of income and/or education can provide important avenues for both emotional and practical support for the survivor. • First- understand if/how existing education or livelihoods activities were a source of or related to the GBV they experienced. • Understand if education and livelihoods are part of the survivor’s life goals. • Identify range of activities as options for the survivor • Discuss and address barriers to accessing these opportunities

PSYCHOSOCIAL NEEDS – HOW TO ASSESS Identify protective factors and strengths Listen to their story for: Family and living situation Social support Spiritual/religious Positive coping mechanisms Ask direct questions: What do you do when you are scared? What do you do when you are sad? What do you do to make yourself feel safe? Who are some people you feel safe with? Who are people that give you hope and strength? What are your interests?

LEGAL ASSESSMENT Determine the survivor’s interest in pursuing legal action through the available justice systems by: • Understanding the survivor’s interest in pursuing a justice response • Know the options for pursuing justice in a particular setting (formal or informal) Unless a survivor raises the issue of reporting a case to the police or wanting to prosecute the case, we usually do not conduct a legal needs assessment in the initial assessment with a survivor. It is not our role to pressure the survivor into any services

ACTIVITY: PUTTING IT ALL TOGETHER In you pairs #1 s will carrying out Health and Psychosocial assessment. #2 s will carry out Safety and Legal assessments using the case study provided.

SUICIDE ASSESSMENT AND RESPONSE Survivor may express feeling of wanting to die, or to never wake up, or to want their life to end. It is normal. Our job = • Normalize the person’s feelings • Determine if these are just thoughts/feelings or if there is an immediate risk that this person my ACT on the feeling they are having • Plan for how to keep the person safe • We do not judge or tell the person that they shouldn’t have these thoughts/ feeling.

RISK FACTORS FOR SUICIDE • Previous suicide attempt(s) • Family history of suicide • History of experiencing violence • History of mental disorders, particularly clinical depression • History of alcohol and substance abuse • Feelings of hopelessness • Impulsive or aggressive tendencies • Local epidemics of suicide • Isolation, a feeling of being cut off from other people • Loss (relational, social, work, or financial)

SUICIDE RISK ASSESSMENT Step 1: Assess current/past suicidal thoughts Step 2: Assess risk: lethality and safety needs Step 3: Address feelings and provide support

SUICIDE RISK ASSESSMENT: STEP 1 Step 1: Assess current/past suicidal thoughts • Ask the person questions that can help you assess their current and past suicidal thoughts. • Based on the person’s responses, you may or may not need to continue with the suicide risk assessment. Ø If “no”, and there are no signs that they intend to harm or kill themselves, it is likely the risk of suicide or self-harm is low. ØIf the survivor answers “yes” to either of the questions, proceed to the next step.

SUICIDE RISK ASSESSMENT: STEP 2 Step 2: Assess risk: lethality and safety needs • Determine if the person has a plan for how they would harm themselves • Assess past suicide attempts • These indicate higher risk that the person will act on their thoughts Ø If person able to explain a plan and / or there are past suicide attempts proceed to Step 3. Ø If person is unable to explain a plan, support the person by exploring strategies for coping and if needed go to Step 4 (develop a safety agreement)

SUICIDE RISK ASSESSMENT: STEP 3 Step 3: Address feelings and provide support • Acknowledge their courage for sharing with you • Normalize their feelings -- express that you understand that they are in a lot of pain • Reiterate that you are here to support them • Be explicit that it is important to you that they do not hurt themselves • Communicate that you would like to come up with a plan together for helping the person not to do this

SUICIDE RISK ASSESSMENT: STEP 4 Step 4: Develop a safety agreement • Helps the person come up with mitigation and prevention strategies • Identify warning signs with them • Identify strategies the person can use to feel better when recognize these warning signs. Be practical and feasible. • Can they agree that they will use these strategies when they start to feel this way in order to help them feel better. • Explore – what might get in the way of them using these strategies. • Identify a safety person – someone who can be on “watch” for the next 24 hours

CLOSING QUESTIONS? CONCERNS? REFLECTIONS?
- Slides: 36