Modifiable Major Risk Factors 1 Hyperlipidemia more specifically

Modifiable Major Risk Factors 1. Hyperlipidemia— more specifically hypercholesterolemia - The major component of serum cholesterol associated with increased risk is low-density lipoprotein (LDL) cholesterol (“bad cholesterol”). - LDL is the complex that delivers cholesterol to peripheral tissues

- In contrast, high-density lipoprotein (HDL) is the complex that mobilizes cholesterol from the periphery and transports it to the liver for excretion in the bile - Consequently, higher levels of HDL (“good cholesterol”) correlate with reduced risk

- High dietary intake of cholesterol and saturated fats (present in egg yolks, animal fats, and butter) raises plasma cholesterol levels. - Conversely, diets low in cholesterol and/or high in polyunsaturated fats lower plasma cholesterol levels

- Omega-3 fatty acids (abundant in fish oils) are beneficial, whereas (trans)unsaturated fats produced by artificial hydrogenation of polyunsaturated oils (used in baked goods and margarine) adversely affect cholesterol profiles. - Exercise and moderate consumption of ethanol raise HDL levels whereas obesity and smoking lower it

2. Hypertension - Is another major risk factor for atherosclerosis; both systolic and diastolic levels are important. - On its own, hypertension can increase the risk of ischemic heart disease by approximately 60% versus normotensive populations

3. Cigarette smoking - Is a well-established risk factor in men and likely accounts for the increasing incidence and severity of atherosclerosis in women. - Prolonged (years) smoking of one pack of cigarettes or more daily doubles the death rate from ischemic heart disease.

4. Diabetes mellitus - The incidence of myocardial infarction is twice as high in patients with diabetes than in those without. - There is also an increased risk of stroke and a 100 -fold increased risk of atherosclerosis-induced gangrene of the lower extremities.

Additional Risk Factors - As many as 20% of all cardiovascular events occur in the absence of overt risk factors - More than 75% of cardiovascular events in previously healthy women occur with LDL cholesterol levels below 160 mg/d. L (levels connote low risk). - Clearly, other factors also contribute to risk; among those that are proven or suspected are the following:

1. Inflammation. - Inflammation is present during all stages of atherogenesis and is intimately linked with atherosclerotic plaque formation and rupture - With the increasing recognition that inflammation plays a significant causal role in ischemic heart disease, assessment of systemic inflammation has become important in overall risk stratification.

- While a number of circulating markers of inflammation correlate with ischemic heart disease risk, C-reactive protein (CRP) has emerged as one of the simplest to measure and one of the most sensitive

- However, it is well established that plasma CRP is a strong, independent marker of risk for myocardial infarction, stroke, Gangrene and sudden cardiac death, even among apparently healthy individuals - CRP is also a useful marker for gauging the effects of risk reduction measures, such as smoking cessation, weight loss,

2. Metabolic syndrome. - Associated with central obesity - This entity is characterized by insulin resistance, hypertension, dyslipidemia (elevated LDL and depressed HDL), and hypercoagulability.
![3. Lipoprotein a [Lp(a)] - Is an altered form of LDL that contains the 3. Lipoprotein a [Lp(a)] - Is an altered form of LDL that contains the](http://slidetodoc.com/presentation_image_h2/44f990a4a493e88fabdcaade925ca0d4/image-13.jpg)
3. Lipoprotein a [Lp(a)] - Is an altered form of LDL that contains the apolipoprotein B-100 portion of LDL linked to apolipoprotein A (apo A); - Lp(a) levels are associated with coronary and cerebrovascular disease risk, independent of total cholesterol or LDL levels

• Other factors. - Factors associated with a less pronounced risk include 1. lack of exercise; 2. competitive, stressful life style (“type A” personality); 3. and obesity

morphology - Atherosclerotic lesions are patchy, usually involving only a portion of any given arterial wall and are rarely circumferential; -
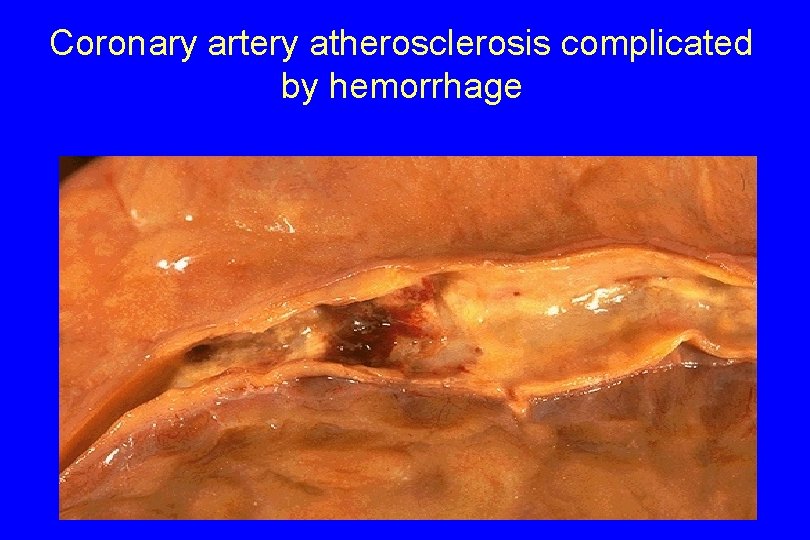
Coronary artery atherosclerosis complicated by hemorrhage
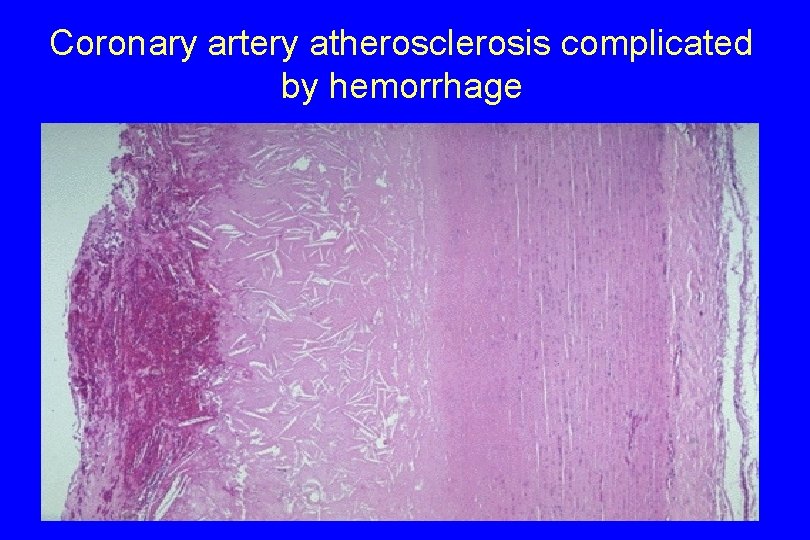
Coronary artery atherosclerosis complicated by hemorrhage
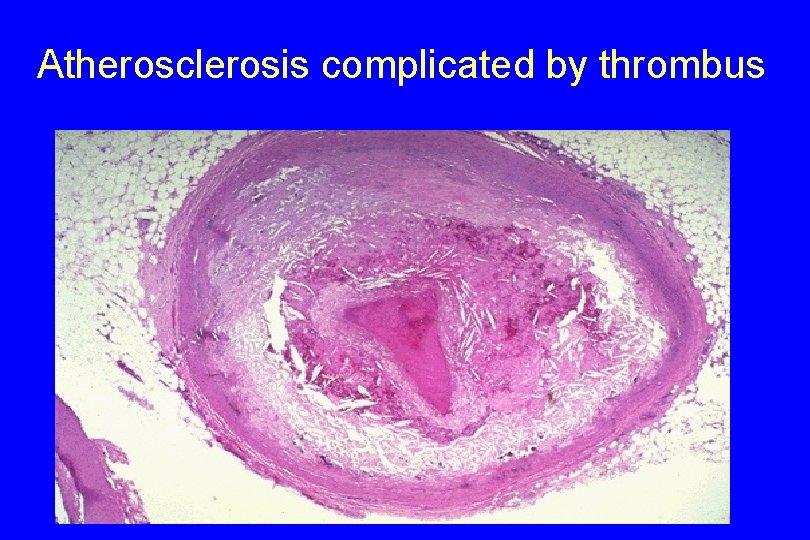
Atherosclerosis complicated by thrombus
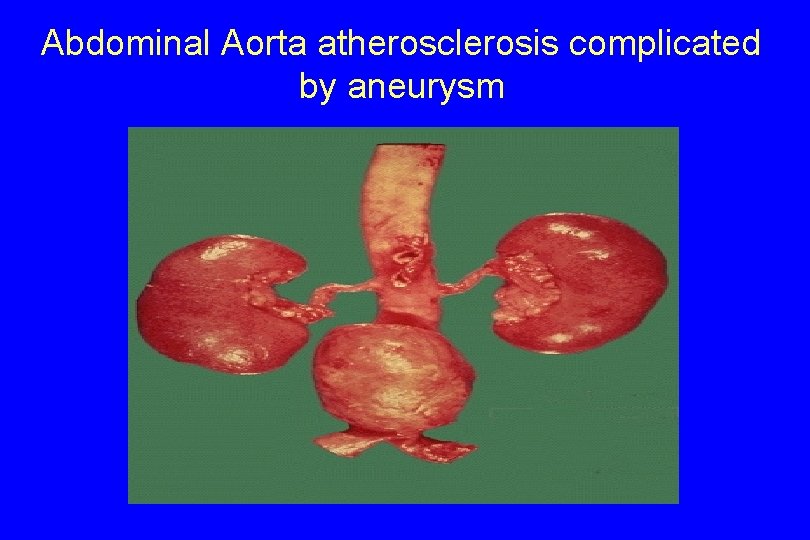
Abdominal Aorta atherosclerosis complicated by aneurysm

In descending order, the most extensively involved vessels are a. the lower abdominal aorta, b. the coronary arteries, c. the popliteal arteries, d. the internal carotid arteries, e. and the vessels of the circle of Willis -

Notes - In humans, the abdominal aorta is typically involved to a much greater degree than the thoracic aorta. - Vessels of the upper extremities are usually spared, as are the mesenteric and renal arteries, except at their ostia.

- Atherosclerotic plaques are susceptible to the following clinically important pathologic changes: 1. Rupture, ulceration, or erosion of the surface of atheromatous plaques - Exposes highly thrombogenic substances and leads to thrombosis, which may partially or completely occlude the vessel lumen

2. Hemorrhage into a plaque. - Rupture of the overlying fibrous cap, can cause intraplaque hemorrhage; - A contained hematoma may expand the plaque or induce plaque rupture. - Plaque rupture can discharge atherosclerotic debris (cholesterol) into the bloodstream, producing Atheroemboli

3. Aneurysm formation. - Atherosclerosis-induced pressure or ischemic atrophy of the underlying media, with loss of elastic tissue, causes weakness and potential rupture

Consequences of Atherosclerotic Disease a. b. c. d. Myocardial infarction (heart attack), Cerebral infarction (stroke), Aortic aneurysms, and Peripheral vascular disease (gangrene of the legs)
- Slides: 25