MODERN Health LABOR Economics ECONOMICS 12 6 TH

MODERN Health LABOR Economics ECONOMICS 12 6 TH EDITION THEORY ANDCharles PUBLIC E. POLICY Phelps CHAPTER 11 Health Insurance Supply and Managed Care 06 March 2021 1

Learning Goals • Discover how “managed care” can help resolve the tension between risk reduction and control of health care costs. • Acquire a working understanding of the alphabet-soup menagerie of managed care plan types. • Learn what mechanisms managed care plans have to control health care costs and the extent to which these do (or do not) work well. • Digest the effects of managed care market penetration on health care providers, and consider the long-run market equilibrium consequences of these changes. 06 March 2021 2

11. 1 The Supply of Insurance • Insurance companies perform two primary tasks • Processing of claims • Bearing and spreading risk. • By pooling risks, insurance companies can actually reduce average risk. • If the risks are completely independent, the average risk (the risk person in the group) of an insured group with N members is 1/N times the variance that each individual confronts. • If the risks are correlated across persons, then the risk can’t be reduced as much. • In health care, the presence of contagious diseases such as colds and influenza contribute to the correlation of risks, but overall, the correlations across people are very small, and risk spreading can work quite well. 06 March 2021 3

11. 1 The Supply of Insurance The Production Function of Health Insurers • The operating costs of insurance companies include the tasks of processing insurance claims and making appropriate payments. • These tasks primarily involve people and computers, which are the main inputs, along with buildings, in the production of health insurance claims. • These costs are paid for by the loading fee charged by the insurance company. • The loading fee for the insurance company rises and falls with its costs. • The structure of an insurance policy itself also affects the loading fee. • If the insurance plan has complicated provisions that require many human decisions before a payment can be made, the loading fee will of necessity be higher. • Number and complexity of claims filed by insured people affect loading fees. • Insurance plans with large deductibles, for example, generate fewer claims because people don’t bother filing small claims on the policy. 06 March 2021 4

11. 1 The Supply of Insurance The Production Function of Health Insurers, continued. • The other relevant cost of insurance companies is the “cost” of money. • Insurance companies collect a premium at the beginning of a year and pay claims throughout the year. • Hold the money in the interim, earning a return on their investment. • For a typical health insurance contract, the average time between payment of the premium and payment of the “typical” benefit can be as large as six months if the premium is paid annually. • The higher the “real” return on capital for the insurance company, the lower its loading fee. • Over the past several decades, the real return for insurance companies has averaged about 5 percent. • The “real” rate of earnings is approximately the actual rate of interest earned minus the rate of inflation. • Health insurance companies pay out most of the premium in terms of health care costs. 06 March 2021 5

11. 1 The Supply of Insurance Flavors of Insurance Companies • Many health insurers in the United States operate as not-for-profit (NFP) organizations, but the for-profit (FP) model now dominates the market. • The NFP companies, most commonly “Blue” plans (Blue Cross and Blue Shield), were organized under special enabling legislation passed during the first half of the twentieth century. • NFP plans operate with several advantages over their FP competitors. • Exempt from taxation. • States levy a special “premium tax” on all insurance sales. • Also exempt from federal and state corporate taxes, etc. • NFP plans do not face the extent of regulation in many states that other insurers do, including regulations about minimum cash reserves that are imposed upon other insurers. 06 March 2021 6

11. 1 The Supply of Insurance Flavors of Insurance Companies, continued. • The FP model now dominates the U. S. health insurance market. • The largest, United. Health Group, had $87 billion in revenue in 2010 and $3. 8 billion in profits. The second-largest of these, Wellpoint, consists mostly of what were originally NFP Blue Cross and Blue Shield plans. • The first combination of these plans (and conversion to FP status) formed the Anthem group (including plans from California, Connecticut, Indiana, Kentucky, Maine, New Hampshire, and Virginia). Wellpoint Health Networks, Inc. , became the new name of what was Blue Cross of California in 1996, at which time they became FP. Anthem, which arose out of the Blue plans in Indiana, converted to FP status in 2001. • Wellpoint Health Networks and Anthem merged in 2004 to form Wellpoint, Inc. , which in 2010 had $65 billion in revenues and $4. 75 billion in profits, the largest profit total of any U. S. health insurer. • The other top-five health insurers (and their 2010 revenues and profits) were Aetna ($35 billion, $1. 3 billion), Humana ($31 billion, $1 billion), and Cigna ($18 billion, $1. 3 billion). • These profits represent a significant proportion of these firms’ revenues, particularly when we account for the fact that only about 15 percent represent something other than payments to health care providers for covered services (see Table 11. 1). For example, consider Wellpoint’s profits as a percentage of their revenues, excluding insurance benefit payments. Of their $65 billion revenue, approximately $55 billion were payments to health care providers, leaving $10 billion of other revenue. Of that, reported profits were $4. 75 billion, thus representing almost one-half of revenues minus claims payments to health care providers. 06 March 2021 7

11. 1 The Supply of Insurance Flavors of Insurance Companies, continued. • The FP model now dominates the U. S. health insurance market. • The largest, United. Health Group, had $87 billion in revenue in 2010 and $3. 8 billion in profits. • The second-largest of these, Wellpoint, consists mostly of what were originally NFP Blue Cross and Blue Shield plans. • The first combination of these plans formed the Anthem group (including plans from California, Connecticut, Indiana, Kentucky, Maine, New Hampshire, and Virginia). • Wellpoint Health Networks and Anthem merged in 2004 to form Wellpoint, Inc. , which in 2010 had $65 billion in revenues and $4. 75 billion in profits, the largest profit total of any U. S. health insurer. • The other top-five health insurers (and their 2010 revenues and profits) were Aetna ($35 billion, $1. 3 billion), Humana ($31 billion, $1 billion), and Cigna ($18 billion, $1. 3 billion). 06 March 2021 8

11. 1 The Supply of Insurance Flavors of Insurance Companies, continued. • Profits represent a significant proportion of these firms’ revenues. • For Wellpoint, of their $65 billion revenue, $55 billion were payments to health care providers, leaving $10 billion of other revenue. • Of that, reported profits were $4. 75 billion, almost one-half of revenues minus claims payments to health care providers. • The pressure for conversion from NFP status to FP status for the Blue plans (and other NFPs) came from three sides. • The Blues had maintained regional monopolies and were limited in how well they could capture economies of scale. • The Blues emphasized traditional health insurance with full coverage for a specific number of days, fee-for-service insurance, which has fallen out of favor. • Finally, as the optimal size increased and managed care became more prevalent, the need for capital to invest in new claims-management systems increased to the point where it could not be funded “from operations, ” and without access to equity capital markets, the NFP organizations could not keep pace with the modern insurance world. 06 March 2021 9

11. 1 The Supply of Insurance Group Insurance • Group insurance offers two benefits over individual insurance: economies of scale and a way to avoid adverse selection. • Economies of scale make the loading fee smaller as firms get larger. • Logic says that as the price of a fringe benefit falls, it will become more attractive to employees, and hence more employers will offer it. • In the most recent data, the percentage of all workers covered by employer-based plans rose steadily from 38 percent (in plans with 3– 24 workers) to about 65 percent (in plans with over 1, 000 workers). • Most of these differences come through the rate at which employers offer the coverage—“takeup” rates do not differ much by firm size when employees are offered coverage, although the takeup rates are modestly smaller in small firms (78 percent) than larger firms (83 percent). • In addition, studies of demand for insurance have commonly found a strong link between group size and overall demand for insurance. 06 March 2021 10
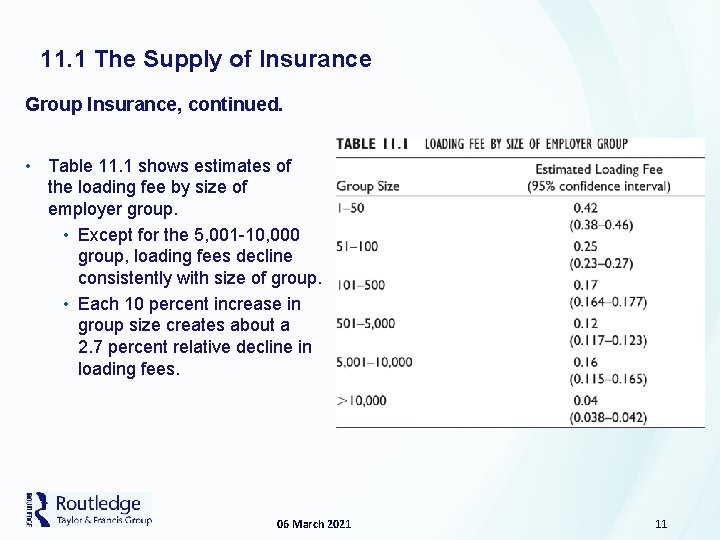

11. 1 The Supply of Insurance Group Insurance, continued. • Table 11. 1 shows estimates of the loading fee by size of employer group. • Except for the 5, 001 -10, 000 group, loading fees decline consistently with size of group. • Each 10 percent increase in group size creates about a 2. 7 percent relative decline in loading fees. 06 March 2021 11

11. 2 Insurance Changes in the PPACA • The PPACA established a set of regional “insurance exchanges, ” one for small employer groups (under 100 employees), and the other set for individuals. • Only 12 states established their own exchanges, and a federal exchange (healthcare. gov) served as the primary exchange in 28 states (including the District of Columbia); another 11 states worked with the federal program in a federal–state partnership. • Four levels of plans: 1. 2. 3. 4. Bronze plan, the minimum acceptable coverage defined in the law (at least 60 percent of costs covered, on average); Silver plan (at least 70 percent of health costs covered); Gold plan (at least 80 percent of costs covered); and Platinum plan (at least 90 percent of costs covered). All of these plans must adhere to the out-of-pocket limits used in defining HSA-eligible plans (e. g. , $6, 550 for individuals, twice that for families, in 2017). 06 March 2021 12

11. 2 Insurance Changes in the PPACA • The insurance exchanges also offer income-related coverage, linked to the maximum out-of-pocket expenditures the plans include before reaching full coverage. • In addition, the PPACA had a requirement that individuals acquire at least a Bronze plan, or they would face a tax penalty. • Tax penalty was set very low initially, and phased in over the years so that 2016 was to be the first year with a full penalty in place. • The total annual penalty is calculated in two ways: person and per family. On the per-person basis, the penalty was set at $695 per adult, but with a maximum family payment of $2, 085 per family (3× the per-person rate). • On the family basis, it was set at 2. 5 percent of family income. Then people would pay the maximum of those two methods of calculating the penalty. • In no case could the penalty exceed national average of the cost of a Bronze plan. • In 2016, the average premiums by age were: 30– 39 = $3, 092; 40– 49 = $3, 479; 50 – 59 = $4, 863; 60– 65 = $7, 382. 06 March 2021 13

11. 2 Insurance Changes in the PPACA • Consider a single 30 -year-old person. • The penalty would be the maximum of two numbers: $695 (for a single person) or 2. 5 percent of family income above the reporting threshold ($10, 300 in 2016). Thus the rule for the 30 -year-old single person: Income under $38, 100 Penalty = $695 Income between $38, 100 and $133, 980 Penalty = 2. 5% of (income – 10, 300) Income over $133, 980 Penalty = Bronze plan cost ($3, 092) • Now consider the decision to insure: • In 2016, the average cost of a Bronze plan nationally was $3, 092. • Suppose this person’s annual income is $50, 000 (about the average per capita GDP in 2016). • Penalty would be approximately $1, 000 (since only the portion of income above $10, 300 is used in the calculation). • Some people in the U. S. choose not to buy the coverage, but rather to pay the penalty. • The decision is quite different for people who envision a year of higher medical costs, such as childbearing or risky activities. 06 March 2021 14

11. 2 Insurance Changes in the PPACA • In general, the model of demand for insurance would suggest that an individual would evaluate their expected payout from the insurance plus the risk premium they would be willing to pay to avoid financial risk. • Compare the premium charged to them in the Exchange, their estimated value of the insurance, and the penalty, and choose the best course of action. • The ratio of premium to expected benefits creates an implicit value of the loading fee, and if that estimated loading fee exceeds the risk premium plus the penalty, they will rationally choose to pay the penalty rather than buying the insurance. • • Finally, the decision is linked to a person’s age, since the Bronze premium (which caps the 2. 5 percent of income penalty) rises with age. In approximate numbers, the incomes at which the Bronze plan premium sets an upper cap on the amount of the penalty are: Age 30– 39 $134, 000 Age 40– 49 $150, 000 Age 50– 59 $205, 000 Age 60+ $306, 000 For most persons above the low-income threshold, their penalty is 2. 5 percent of income, and thus sometimes this leads to a decision to pay the penalty rather than buy the insurance. 06 March 2021 15

11. 2 Insurance Changes in the PPACA • The net effects of these incentives was lower enrollment into the Exchange plans for loweraged persons, the people needed in the pools to bring down the average cost of the premiums. TABLE 11. 2 HERE • In 2015 the data show a strong age effect for those remaining without insurance 06 March 2021 16

11. 3 Managed Care: A Response to the Incentives of Traditional Insurance • Managed care spans a wide variety of organizations, but the key idea is that MCOs are actively involved both in the delivery of health care and in the provision of health insurance. • HMO: health maintenance organization • The essential feature of the pure “staff model” HMO is that the plan is paid on a “capitation” basis (“per head”), which means that the HMO receives a fixed sum of money each year to provide all of the medical care the enrollee needs, no matter what. • This offers the greatest incentive for cost control and cautious use of medical interventions. • FFS: Fee-for-serve, the opposite of HMOs. • Traditional insurance offered defined coverage for billed charges. • Least constraints on both provider and consumers and higher costs for a given level of financial protection. 06 March 2021 17

11. 3 Managed Care: A Response to the Incentives of Traditional Insurance • IPA: independent practice association • Doctors work as independent doctors in their own offices, and normally have a mix of patients enrolled in traditional FFS plans as well as capitated or “managed” patients. • PPO: preferred provider organization • Patients steered to preferred providers by the PPO insurance plan in exchange for a lower price. • The lower price allows the PPO to offer a lower total insurance premium, which attracts enrollees, which in turn creates a larger patient base that the PPO can use to negotiate with providers. • Doctors are paid on a fee-for-service system, usually with a set of negotiated fees for each service offered. • POS: point of service plans • Usually an agreement with providers, but the doctors are spread around in their own offices as in an IPA or PPO. • Compensation is per patient per year rather than FFS. 06 March 2021 18

11. 3 Managed Care: A Response to the Incentives of Traditional Insurance • HDHP: high-deductible health plan • Large front-end deductibles, typically with a health saving account (HSA) attached. • Individuals can made tax-exempt contributions to HSAs up to $3, 100 annually or $6, 250 for families. • ACO: accountable care organization • Newly defined by the PPACA. • Resembles an HMO but need not have the entire range of services. • Receives payments directly related to both levels of and improvements in measurable quality of care. 06 March 2021 19

11. 4 Why Managed Care? • Traditional forms of health insurance (FFS) altered people’s behavior in choosing medical care, leading to overconsumption. • Managed care limits consumer access to medical care in a way that offsets some of the incentives for overuse. • Incentives and constraints that reduce the quantity of care and shift care to lower-cost alternatives if possible. • The real value to a consumer of an MCO is in its ability to reduce premiums while retaining the elimination of financial risk offered by FFS plans. • When consumers decide to enroll in an MCO, they in effect precommit to a plan that they know in advance will constrain their choices because such precommitment can actually improve their overall expected utility. 06 March 2021 20

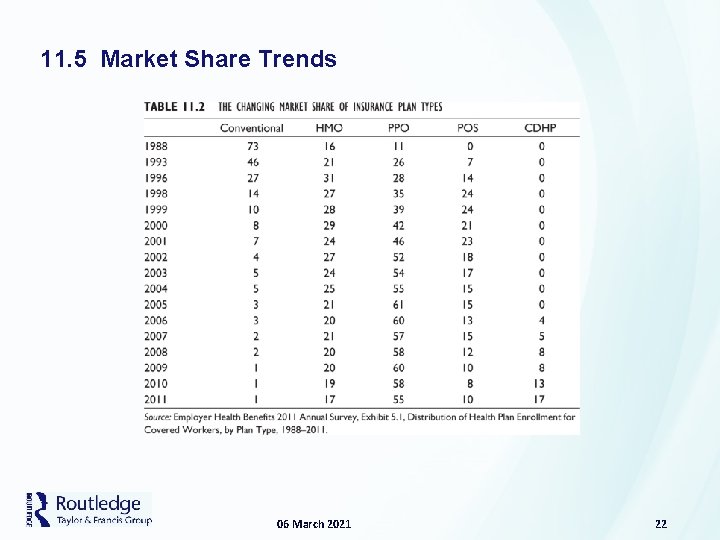
11. 5 Market Share Trends • As in Table 11. 3 (next slide), conventional FFS plans that once dominated the market now barely exist. • The HMO model was briefly popular, but is now only 15 percent of the market. • The HDHP is the fastest gaining plan, at the expense of HMO, PPO, and POS plans. • Declining plan types all limit providers. • HDHPs offer unlimited access but patients share a greater portion of the costs. • Consumers seem to prefer a plan that controls costs but does not interfere much with medical treatment. • New CDHPs (consumer-directed health plans) with HSAs offer a high deductible, 20 percent copay up to a catastrophic cap, and then full coverage. 06 March 2021 21
11. 5 Market Share Trends 06 March 2021 22
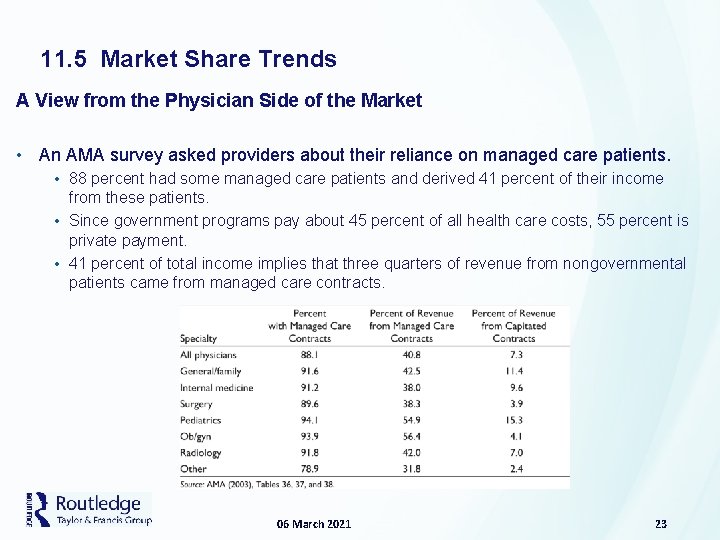
11. 5 Market Share Trends A View from the Physician Side of the Market • An AMA survey asked providers about their reliance on managed care patients. • 88 percent had some managed care patients and derived 41 percent of their income from these patients. • Since government programs pay about 45 percent of all health care costs, 55 percent is private payment. • 41 percent of total income implies that three quarters of revenue from nongovernmental patients came from managed care contracts. 06 March 2021 23

11. 6 Types of Interventions Consumer Side • Copayments • Fixed amount per visit, typically $10 -$40 for office visit, more for specialists, more for emergency room visits. • Second-Opinion Programs • Usually a patient choice, but sometimes required prior to surgery • Insurance pays for the second opinion but the second doctor will not be the treating doctor, if the procedure is approved. • Attempts to reduce the financial incentive for doctors to recommend procedures that may not be necessary. • Have not worked well and are now rarely required. • Patients reluctant to challenge doctors. • Second doctor is likely to be in the same area and thus may have the same practice style, reducing the chance of a dissenting second opinion. 06 March 2021 24

11. 6 Types of Interventions Consumer Side, continued. • Gatekeeper Models • Primary care provider (PCP) must refer to specialist. • Idea is that some procedures can be done by the lower-cost PCP. • Little data on effectiveness is available, and thus mostly not required today. Provider Side • Salary Versus Fee-for-Service • “Capitation” plans where payment comes on a per patient basis rather than per service. • Changes incentive from increasing volume of procedures to preventing the use of care. • Legal provisions to prevent undertreatment. • The major cost savings is in limiting hospitalization, which doctors largely control. 06 March 2021 25
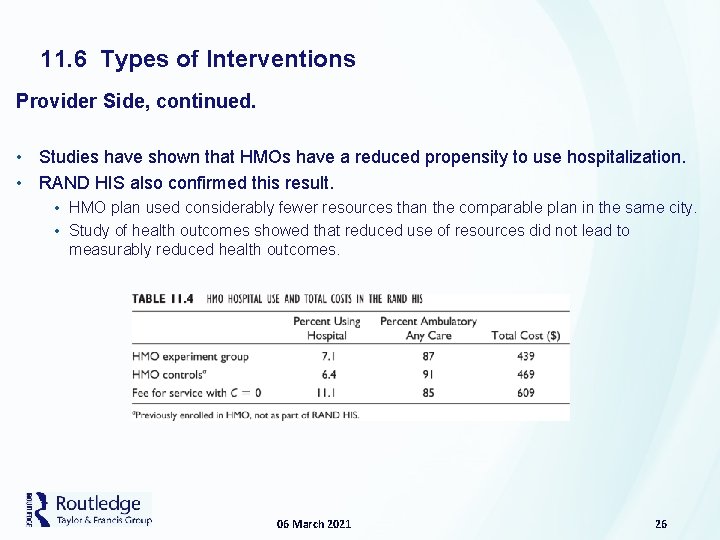

11. 6 Types of Interventions Provider Side, continued. • Studies have shown that HMOs have a reduced propensity to use hospitalization. • RAND HIS also confirmed this result. • HMO plan used considerably fewer resources than the comparable plan in the same city. • Study of health outcomes showed that reduced use of resources did not lead to measurably reduced health outcomes. 06 March 2021 26

11. 6 Types of Interventions Provider Side, continued. • The Proper Balance of Incentives • FFS plans have an incentive to overtreat; HMOs have an incentive to undertreat. • A balanced plan might do better, depending on which of the negative effects is likely to be largest. • Difficult to determine the relative strengths of demand inducement and shirking, and thus difficult to determine optimal balance. • Holdbacks • Insurance plans may “hold back” part of the payments to physicians until the end of the year, to see if total treatment costs within the plan have come within targets. • If costs are unusually high, the holdback is kept, giving doctors a stake in controlling costs. • But unclear that this actually lowers costs due to weak incentives. 06 March 2021 27

11. 6 Types of Interventions Payment Strategies for Hospitals and Related Organizations • Hospitals have distinct characteristics about their services that make them eligible for a particular form of payment that lies in between FFS and capitation, payment by “the case. ” • A hospital “event” has clearly defined boundaries—the admission and discharge of the patient—insurance plans can pay hospitals for single hospitalization events in a lump sum. • The quintessential case-based payment system emerged from the federal government’s desires to control hospital costs under the Medicare program, creating a “prospective payment system” (PPS) involving nearly 500 “diagnostically related groups” (DRGs). • Discussed further in Chapter 12. 06 March 2021 28

11. 6 Types of Interventions Provider Selection • MCOs rely on careful selection of providers to control costs of care. • If intrinsic differences between the costs of various providers actually exist, then finding the low-cost providers makes good sense. • Whatever the actual cost structure of providers, if they have been pricing above their actual costs of treatment, then negotiating the price downward is beneficial. • One reason why PPOs might not achieve their full possible benefit is that they seldom actually use available information to select among providers carefully. • In a study of primary-care physicians in Rochester, NY, there were large and systematic differences in the total costs of treating patients among doctors in a very “open” IPA panel of physicians. • The top 10 percent of doctors had charges per patient per year that were twice those of the lowest 10 percent. • Yet neither of the competing IPA insurance plans in the community opted to limit their panel of physicians to the relatively lower-cost providers. • Their choices embraced the philosophy of bringing into the “panel” of allowed providers all those who wished to participate, apparently on the hypothesis that more doctors meant more patients and hence a larger market share. 06 March 2021 29

11. 6 Types of Interventions Provider Selection, continued. • One study provides some evidence that MCOs may select doctors on the basis of quality of care as well as cost of treatment, at least when quality can be measured. • Blue Cross of California (and then others) abandoned rewards linked to cost control in its HMO MCO plans and structured a new set of bonus payments to physicians directly tied to patient satisfaction with the plan. • Offered incentive payments of up to 10 percent bonuses for the highest satisfaction scores, as measured by random surveys of patients enrolled in the plan. • MCOs also select hospitals as well as individual doctors. • In a study utilizing California data from 1983 to 1997, the consequences of California’s introduction of selective contracting both through the state’s Medicaid program (“Medi. Cal”) and by introducing legislation allowing selective contracting in private insurance markets was considered. • Based on measures of competition among hospitals and the rate of cost growth and how it changed due to selective contracting entering the market • Found a strong negative relationship between market concentration and the rate of cost growth after selective contracting emerged—more competitive markets had less cost growth. 06 March 2021 30

11. 6 Types of Interventions Prices and Fee Schedules • A PPO enrolls a group of people with the promise of a low premium (based on the expectation of low prices from providers) and negotiates with providers (doctors, hospitals, nursing homes, etc. ) by promising to bring them a high volume of patients (those they have enrolled) in exchange for a favorable price. • If a PPO is successful in recruiting more patients, it can negotiate better with providers. • If a PPO successfully negotiates with providers, it can lower premiums and attract more patients. • Price negotiations affect the quality of services. • Lower payments may result, for example, in less time per visit. • Price negotiations affect the mix of services by changing relative prices. • For services that are not quality-sensitive (like emergency care), lower prices will reduce the quality and thus lower cost, while keeping higher quality in other areas where demand is sensitive (such as predictable events, like childbirth). 06 March 2021 31

11. 6 Types of Interventions Intervention in Specific Treatment Choices • Prior Authorization • Especially for expensive treatments, prior authorization may be required. • Alternately, treatment may be approved with limits requiring further authorization. • Denial of Payment • Occurs after the treatment has taken place. • Physicians, hospitals, or the patient must pay the costs of treatment. • Source of considerable conflict with MCOs, providers, and patients. 06 March 2021 32

11. 7 Which Interventions Work Best for Managed Care? Intervention in Specific Treatment Choices • A study of tools used to control costs for acute myocardial infarctions (AMI) and ischemic heart disease (IHD, a milder form of heart disease) found that patients under different regimes received about the same type of treatment in all cases. • The cost savings from the managed care approach came almost entirely from the price per unit of service negotiated. • Average payment from traditional indemnity plans for AMI patients was $38, 500. • For PPO plans (which basically have only the price tool at their disposal), the average was $26, 500 (about 70 percent of the indemnity plan level). • For HMO (more aggressively managed) plans, the average was $23, 600 (about 60 percent of the indemnity plan level), despite the higher actual use of invasive procedures (bypass surgery and angioplasty). • Similar patterns for treatment of patients with IHD. • Two facts stand out. 1. 2. Given the already widespread growth of managed care plans in the market, it would appear that managed care has already squeezed out a considerable level of “fat” in the prices for health care. About three-quarters of the possible gains from “managing” care come from simple price negotiation and the remaining quarter from actual “management. ” 06 March 2021 33
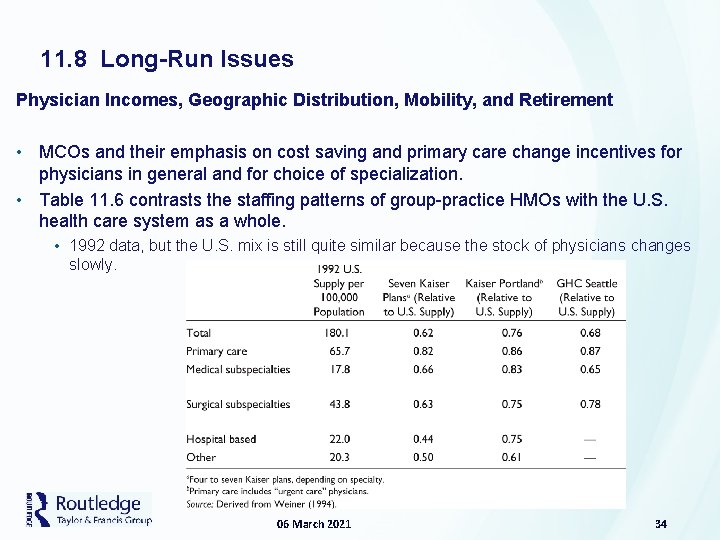
11. 8 Long-Run Issues Physician Incomes, Geographic Distribution, Mobility, and Retirement • MCOs and their emphasis on cost saving and primary care change incentives for physicians in general and for choice of specialization. • Table 11. 6 contrasts the staffing patterns of group-practice HMOs with the U. S. health care system as a whole. • 1992 data, but the U. S. mix is still quite similar because the stock of physicians changes slowly. 06 March 2021 34

11. 8 Long-Run Issues Physician Incomes, Geographic Distribution, Mobility, and Retirement • Table 11. 6 shows an important decline in employment of specialists of all types. • Incomes for specialists should thus be falling. • Medicare’s payment schemes, discussed in the next chapter, will enhance these trends. • Studies have shown: • Managed care penetration into a market increases primary care physicians’ earnings. • Also cuts into the earnings of hospital-based specialists (such as radiologists) • Each 1 percent increase in MCO market share added $2, 263 to the earnings of primarycare doctors in the study. • During the time period studied, 15 percent increase in MCO market share led to a 50 percent increase in the earnings of primary care physicians. • Effects on location of physicians suggests that there is less growth in the supply of doctors in areas in which there is a higher MCO market share, although studies conflict. • May also cause some physicians to retire earlier. 06 March 2021 35

11. 8 Long-Run Issues Market Segmentation • Health insurance markets might segment into submarkets for low- and high-risk consumers. • See Chapter 10. • The gatekeeping function of MCOs might also have this effect. • A review of studies on the selection of MCOs suggested that managed care plans generally have a 20 -30% prior utilization advantage over conventional indemnity plans. • A primary outcome of MCOs may not be so much to control costs as to create a viable mechanism by which insurance carriers can identify relatively healthy people and attract them to a plan that relatively sickly people will find undesirable. 06 March 2021 36

11. 8 Long-Run Issues Accountable Care Organizations (ACOs): New Entrant from the PPACA • ACOs (as defined in the PPACA) will resemble traditional HMOs, most likely with a primary-care group at the core, and either providing or collaborating with other physicians, hospitals, home health care, and other providers, most typically under a capitation payment system. • If care is delivered for less than the predetermined amount, the ACO can share the savings under the new Medicare Shared Savings Program (which began operation on January 1, 2012). • The Center for Medicare and Medicaid Services (CMS) has defined a significant number of quality indicators to be applied to ACO performance (and the set of these will increase through time). • To share in cost savings, the ACOs must also meet these quality standards. • Thus, in concept, ACOs cannot simply reduce cost by reducing quality. 06 March 2021 37
- Slides: 37