Mobile Pharmacy An Innovative Community Pharmacy and Primary

Mobile Pharmacy: An Innovative Community Pharmacy and Primary Care Collaboration for Co-morbid & Chronic Pain Patients Scott V. Monte, Pharm. D Chester Fox, MD

Disclosures • Scott V. Monte, Pharm. D declares an equity interest in Mobile Pharmacy Solutions

Learning Objectives • First Objective: To identify common barriers to appropriate medication use and interdisciplinary strategies to overcome these barriers. • Second Objective: To identify improvement opportunities in workflow and communication through direct primary care and community pharmacy collaboration. • Third Objective: To provide experience implementing a realworld community pharmacy primary care collaboration for complex and pain management patients.

What is the Role of the Community Pharmacist? • Fulfill orders written by the provider • Adjudicate insurance claims for coverage • Review drug interaction and ensure safety • Counsel on proper medication use • Provide OTC recommendations
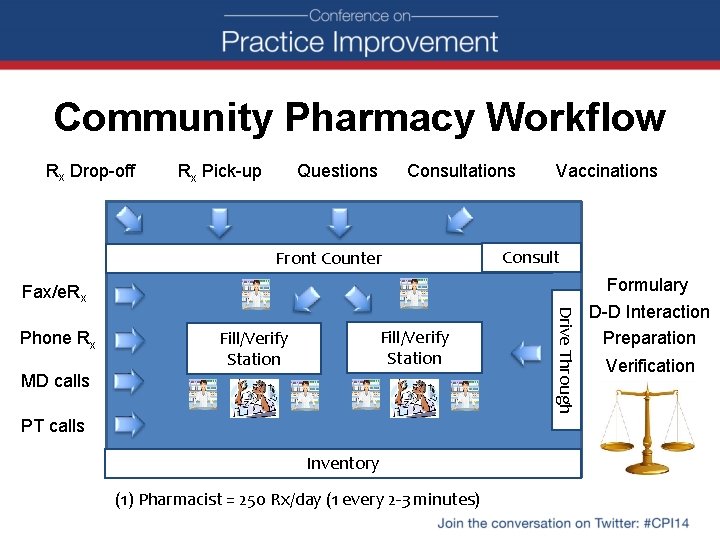
Community Pharmacy Workflow Rx Drop-off Consultations Questions Rx Pick-up Front Counter Vaccinations Consult Fax/e. Rx Fill/Verify Station MD calls PT calls Inventory (1) Pharmacist = 250 Rx/day (1 every 2 -3 minutes) Drive Through Phone Rx Formulary D-D Interaction Preparation Verification

Workflow is efficient for… • • • Pharmacist-patient access Brief clinical interactions Maximizing prescription volume Minimizing workforce requirements Cost control

Workflow is inefficient for… • Pro-active intervention on medication-related problems • Extended patient care interactions • Interdisciplinary interactions • Introduction of new pharmacy services (innovation) • Physician office communication – Silo mentality – Medical and pharmacy staff are strangers

Pharmacy is at a crossroad ph ic ide al Diminished health plan reimbursements Delayed payment cycles Increased cost of goods (generic costs) Expansion of closed networks Div ilo How do we hold on to our volume and reimbursement? so Traditional Paradigm Ph • • Advancing Care Models Where is pharmacist value to the healthcare system?

What Value is Community Pharmacy to the Medical Community? Proper Medication Use (Adherence) Medical Provider & Staff Efficiency Significant Change in Pharmacy Workflow Creation of New Services Medical Provider & Staff Communication

Interacting Dimensions of Adherence Trends in Medication Non-adherence • Up to 50% are patients non-adherent • Those w/ chronic illness take ~½ of meds Poor Outcomes & Care Transition • 30 -50% of treatment failures • 10 -25% of hospital admissions • 40% of nursing home admissions Cost American College of Preventative Medicine (www. acpm. org) • $100 -300 Billion annually • $2, 000 per patient annually in MD visits

Predictors of Medication Non-adherence American Society of Consultant Pharmacists. Adult Meducation. Improving medication adherence in older adults. http: //www. adultmeducation. com/downloads/Adult_Meducation. pdf.

Mobile Pharmacy Solutions

Mobile Pharmacy Service Model Home prescription delivery: – Medications are delivered by vehicle to the patient’s home Prescription mailing: – Medications are mailed to the patient’s home Adherence reminder calls: – The pharmacy dispensing system creates an automated queue for pharmacy staff to prioritize outbound adherence reminder phone calls. – The reminder call system includes up to (3) phone calls in the 7 -10 day period before a chronic medication comes due. Thereafter, a designated caregiver or provider is contacted to check on the patient.

Mobile Pharmacy Service Model Pharmacist Home Visit: – A clinical pharmacist visits the house or other desired setting to reconcile the medication regimen and teach appropriate use Accounts Receivable (Payment Planning): – In-house accounting staff creates payment planning for patients with financial limitations or no insurance coverage for required medications Medication Synchronization: – Pharmacist and technical staff reconcile all chronic medications and obtain updated prescription refills from each of the patient’s providers – Prescription refills are aligned to occur at a regular intervals to permit for consistent insurance billing and single delivery (i. e. monthly)

Mobile Pharmacy Service Model Adherence Packaging: – Second stage to medication synchronization – Distinct from Blister Packaging (one medication to one card) – Commingling of medication (more than one medication per cell) – Organize the daily medication regimen • 4 Weekly packages (pillbox feel) • Monthly packages (morning, evening)

Adherence Packaging Technical and Clinical Process Medication Adherence Packaging: • Reconcile the chronic medication regimen with the patient and their physicians • Identify controlled substances and prn medications to be dispensed in traditional vials • Determine an optimal daily schedule (i. e. once, twice, three times daily) • Agree on a preferred packaging method with patient (i. e. weekly or monthly package) • Communicate with the insurance company and physician for early refills • Utilize coupons or short-fill prescriptions to overcome insurance barriers • Document the medication regimen and packaging mechanism for next refill • Schedule adherence calls 7 -10 days before next packaging is to be prepared • Schedule a face-to-face or telephonic pharmacist visit for explanation of use • Educate the patient on e-prescribing and use of one pharmacy

Mobile Pharmacy Service Model Impromptu Compounding: – Dedicated compounding laboratory space within the pharmacy to create custom formulations of medications (non-sterile preparations) • Liquid Preparations - Solutions - Suspensions • Capsules • Rapidly Dissolvable Tablets • Effervescent Powders • Troches (buccal administration) • Lollipops • Topical Preparations - Creams and ointments - Gels and foams • Lip Balms • Poly-ox Bandages (wound barrier) • Rectal Suppositories (“rockets”) • Nasal Sprays • Shampoos

Medication Adherence Community Pharmacy Service Opportunities Service Adherence Barrier Addressed Home delivery Burdensome schedule, lack of transportation or mobility (access), stigma w/ therapies, discharge plan Adherence reminder phone calls Forgetfulness, refill obtainment Pharmacist home visit Low health literacy, lack in insight into illness, lack of belief in treatment, belief that meds are harmful, motivation, mastery of techniques, fear of side effects or dependence, regimen impact on lifestyle Accounts receivable (payment plans) Medication cost, pay-check timing, no insurance Medication synchronization & packaging Low literacy/language proficiency, low cognitive function or impairment, anxiety, depression, psychiatric disease, substance abuse, forgetfulness, complexity of medication regimen, inconvenience Impromptu Compounding Swallowing problems, dexterity, formulation needs
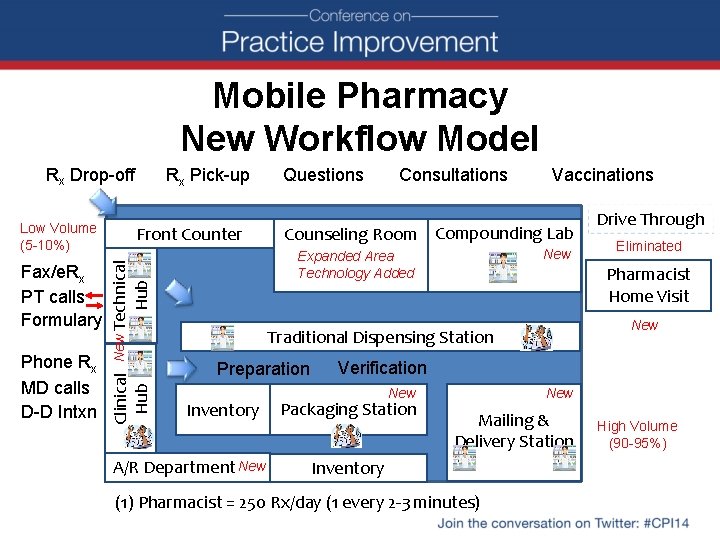
Mobile Pharmacy New Workflow Model Rx Drop-off Low Volume (5 -10%) Questions Consultations Vaccinations Counseling Room Compounding Lab New Expanded Area Technology Added Hub New Technical Phone Rx MD calls D-D Intxn Front Counter Clinical Hub Fax/e. Rx PT calls Formulary Rx Pick-up Inventory A/R Department New Eliminated Pharmacist Home Visit New Traditional Dispensing Station Preparation Drive Through Verification New Packaging Station Mailing & Delivery Station Inventory (1) Pharmacist = 250 Rx/day (1 every 2 -3 minutes) High Volume (90 -95%)

Early Experience on Adherence Sustain a community pharmacy practice model that we believe will promote patient adherence to medications 54 32 153 216 49 110 106 65 Early Experience 241 patients >1 -year in MPS 3+ disease state 7+ medications

Mobile Pharmacy Medical Community Collaboration IDENTIFY OPPORTUNITY Incoming or outreach Executive Team INITIAL MEETING Medical Leadership CEO / CCO Legal OFFICE MEETING Key Office Personnel COO Pharmacy Manager Clinical Pharmacist

Primary Care Office Community Pharmacy Opportunities • Reduced or streamline pharmacy refill requests • Reduced patient phone calls / office Rx pick-up • Easier communication – Direct contact information for clinical and non-clinical – Secure email / text messaging • Build workflow for specialized practice-based needs • Improve medication and formulary knowledge

Primary Care Community Pharmacy Pilot Jefferson Family Medicine (JFM) • A safety net patient centered medical home • Teaching site of the UB Department of Family Medicine • Provides comprehensive health care to a predominantly low-income, African-American patient population. • Located on the east side of Buffalo, NY • 1. 7 miles from Mobile Pharmacy

Pilot Timeline • September 2013: Introductory meeting (Dr. Fox & Dr. Monte) • October 2013: Dr. Monte site visit and shadowing with Dr. Fox • October 2013: 1 st patient referral and on-site staff meeting – MPS Clinical Pharmacist – JFM Nursing Staff • January 2014: General Provider Meeting – MPS presentation of services and referral process • September 2014: Community Pharmacy Resident Shadowing
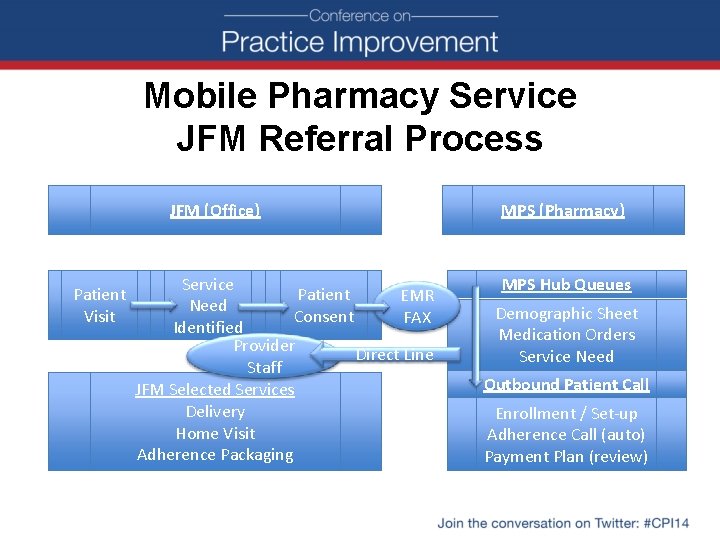
Mobile Pharmacy Service JFM Referral Process JFM (Office) Patient Visit Service Patient EMR Need Consent FAX Identified Provider Direct Line Staff JFM Selected Services Delivery Home Visit Adherence Packaging MPS (Pharmacy) MPS Hub Queues Demographic Sheet Medication Orders Service Need Outbound Patient Call Enrollment / Set-up Adherence Call (auto) Payment Plan (review)

JFM-Mobile Pharmacy Custom Workflow Builds • Medication discontinuation notification – Notes section in the e-Rx – “ 0” quantity in the sig of the e-Rx • Controlled Substance Prescriptions – Once monthly batch of new prescription sent to pharmacy • In the event of expiration pharmacy has direct line to a nurse – MPS activated C 2 adherence reminder call capability – Ability to maintain precise refills at the 30 -day mark – Mitigates pharmacy shopping – Provides MPS ability to have medication in stock and be firm on refill dates – Reduce patient call volume to JFM; peace of mind • Electronic Medical Record (Integration)
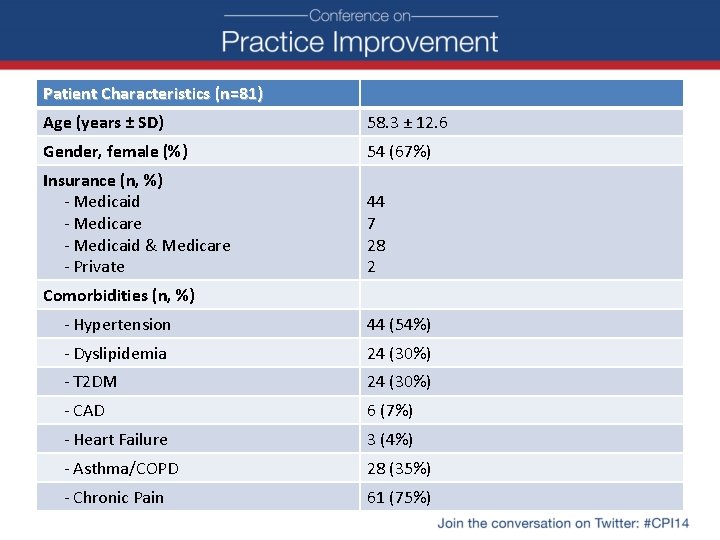
Patient Characteristics (n=81) Age (years ± SD) 58. 3 ± 12. 6 Gender, female (%) 54 (67%) Insurance (n, %) - Medicaid - Medicare - Medicaid & Medicare - Private 44 7 28 2 Comorbidities (n, %) - Hypertension 44 (54%) - Dyslipidemia 24 (30%) - T 2 DM 24 (30%) - CAD 6 (7%) - Heart Failure 3 (4%) - Asthma/COPD 28 (35%) - Chronic Pain 61 (75%)
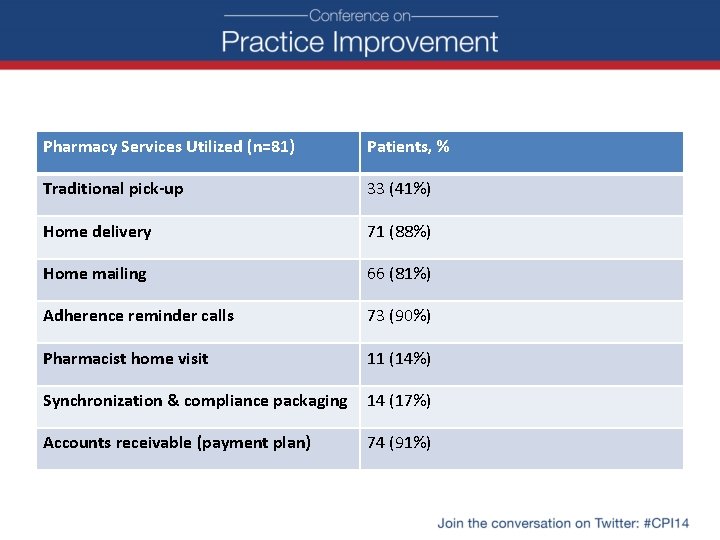
Pharmacy Services Utilized (n=81) Patients, % Traditional pick-up 33 (41%) Home delivery 71 (88%) Home mailing 66 (81%) Adherence reminder calls 73 (90%) Pharmacist home visit 11 (14%) Synchronization & compliance packaging 14 (17%) Accounts receivable (payment plan) 74 (91%)

Medical and Pharmacy Program Metrics Total PCP’s referring into the program 10 Patients declining participation after PCP referral 13/94 (14%) Patients discontinuation from the program 5/81 (6%) Average time in the program 7. 3 ± 3. 5 months Number of chronic medications at enrollment 7. 0 ± 4. 6 Average monthly medication fills 8. 4 ± 5. 5 Total medication fills 5, 301

Physician Perspective • Role of Community Pharmacy • Impact of the pilot on JFM • Patient response
Please evaluate this session at: stfm. org/sessionevaluation
- Slides: 31