MLT 242 Medical Microbiology 242 Week 4 Ch

MLT 242: Medical Microbiology 242 Week 4

Ch. 44: Obligate Intracellular Bacteria • • • Obligates intracellular bacteria. Is similar to gram-negative bacteria. Contains lipopolysaccharide in the cell wall. Exhibits little endotoxic activity. Causes of human infections are: • Chlamydia trachomatis • Chlamydophila pneumoniae • Chlamydophila psittaci Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 2
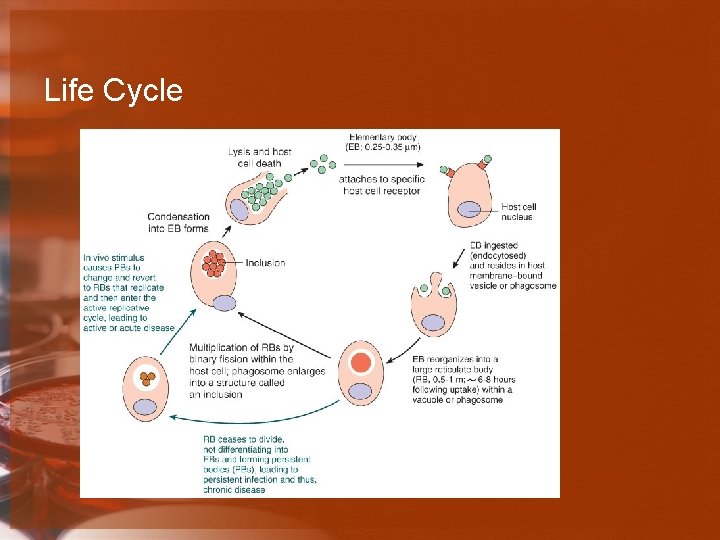
Life Cycle

Chlamydia pneumoniae • Important respiratory pathogen (acute respiratory disease, pneumonia, and pharyngitis) • Common (50% of adults have antibodies) • College age students most susceptible • Implicated in asthma

Chlamydia pneumoniae (cont’d) • Reinfection common • Biphasic clinical picture • Prolonged sore throat and hoarseness, followed by flu-like lower respiratory symptoms • Pneumonia and bronchitis

Chlamydia trachomatis • Most commonly sexually transmitted bacterial pathogen in U. S. • Only HPV is a more commonly sexually transmitted disease • Major cause of sterility in U. S. • May be transmitted to newborns during delivery • Results in conjunctivitis

Chlamydia trachomatis (cont’d) • Other sites of infection • Trachoma – infection of the conjunctiva, resulting in scarring and blindness (Mostly in India and Egypt) • Lymphogranuloma venereum • Infects lymph nodes • STD found in immigrants from the tropics

Laboratory Diagnosis • If cultured, must be in cells • Direct microscopic examination to find EB’s – visualized with fluorescein-conjugated antibodies • Enzyme immunoassay • Nucleic acid probes with and without amplification (PCR) • Serologic tests are method of choice for detection (Fourfold rise in titer)
Chlamydophila pneumoniae Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 9

Rickettsia • • • Intracellular, gram negative organism Requires host to replicate and survive Cause febrile illness through the bite of an arthropod Patient often presents with a rash Posses a cell wall

Rickettsia • Rickettsia are transmitted by arthropod vectors: • Ticks • Lice • Fleas • Chiggers • Three major groups: • Spotted fever group • Rickettsia conorii • R. rickettsii (Rocky Mountain spotted fever) • Typhus group • R. prowazekii • R. typhi • Scrub typhus group • Orientia tsutsugamushi Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 11
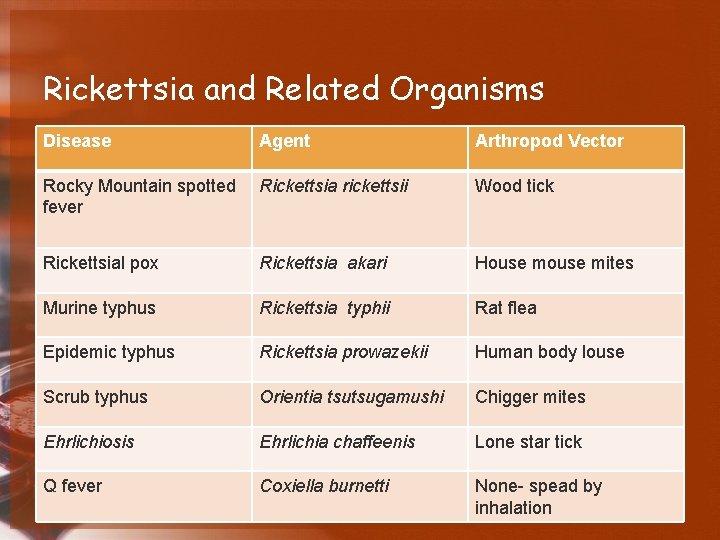
Rickettsia and Related Organisms Disease Agent Arthropod Vector Rocky Mountain spotted fever Rickettsia rickettsii Wood tick Rickettsial pox Rickettsia akari House mites Murine typhus Rickettsia typhii Rat flea Epidemic typhus Rickettsia prowazekii Human body louse Scrub typhus Orientia tsutsugamushi Chigger mites Ehrlichiosis Ehrlichia chaffeenis Lone star tick Q fever Coxiella burnetti None- spead by inhalation

Ehrlichia, Anaplasma, and Neorickettsia • All genera are transmitted by ticks. • Ehrlichia • Has two major species: Ehrlichia chaffeensis and E. ewingii • E. chaffeensis causes human monocytic ehrlichiosis. • Morulae are observed in monocytes. • Anaplasma • Causes human granulocytic anaplasmosis. • Morulae are observed in granulocytes. • Neorickettsia sennetsu • Causes sennetsu fever. Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 13

Laboratory Diagnosis of Rickettsial Disease • Immunohistochemical detection • Serological tests • PCR
Ch 45: Cell-Wall Deficient Bacteria • Highly fastidious • Slow growing • Facultative anaerobes • Very small cell size (0. 3 x 0. 8 μm) • No cell wall • Small genome

Mycoplasma and Ureaplasma Species • General Characteristics • Once thought to be viruses because of size • Mycoplasmas are the smallest free-living organism in nature • Four human pathogens • Mycoplasma pneumoniae - respiratory • Mycoplasma hominis - urogenital • Ureaplasma urealyticum – urogenital • Ureaplasma parvum- urogenital

Mycoplasma and Ureaplasma Species • Pathogens of respiratory and urogenital tracts • Transmission • • Direct sexual contact Mother-child exposure during delivery or in utero Respiratory secretions/aerosols Nosocomial (transplanted tissues)

Clinical Manifestations • Mycoplasma pneumoniae • Asymptomatic infection • Upper and lower respiratory tract infections • Ureaplasma urealyticum and M. hominis • Systemic infections in neonates • Invasive disease in patients who are immunosuppressed • Urogenital tract infections • M. genitalium • Nongonococcal urethritis in men • Cervicitis and endometritis in women • Ureaplasma spp. • Has been isolated from tissue (e. g. , chorioamnion) of neonates Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 18

Diagnosis • Direct detection methods are not recommended. • Molecular diagnostics (Most detected) • Polymerase chain reaction (PCR) amplifies clinical relevant species. • Cultivation • Glucose is used to detect Mycoplasma pneumoniae. • Urea and arginine media are used to isolate Ureaplasma urealyticum and M. hominis. • Identification • M. pneumoniae appears spherical, grainy, and yellow. • U. urealyticum appears as dark, brownish clumps. • M. hominis has a “fried egg” appearance. Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 19

Ch. 43 Mycobacterium • Aerobic • Non–spore forming (except Mycobacterium marinum) • Intracellular pathogens • Nonmotile • Very thin, slightly curved or straight rods • Slow growing (2 to 60 days) • Acid-fast cell wall • N-glycolylmuramic acid • Very high lipid content

Mycobacterium tuberculosis • Primary tuberculosis • Spread by coughing, sneezing, or talking • Inhalation of droplets • Inhaled into alveoli, where the organisms are phagocytized • If the organism does not cause immediate infection, the organism can be “walled off” in a granuloma • Granulomas can break down in future and the organisms can cause infection later
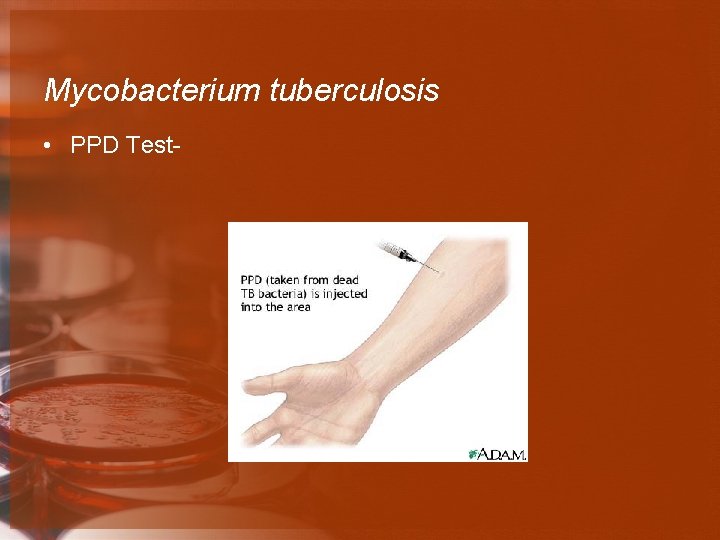
Mycobacterium tuberculosis • PPD Test-
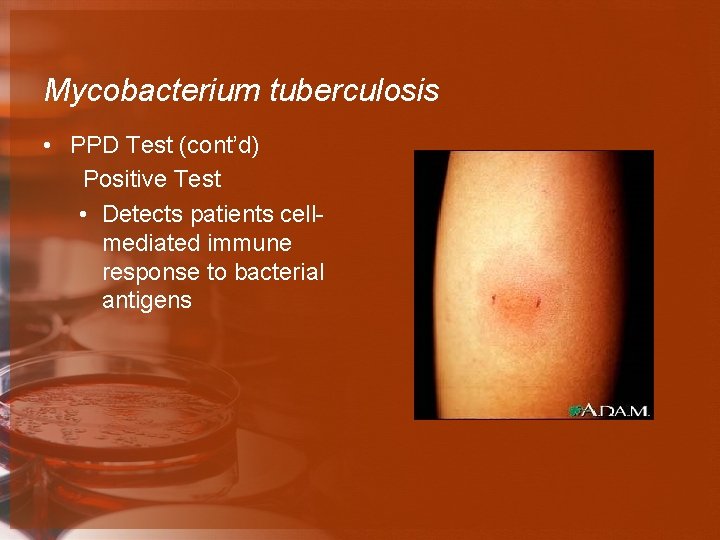
Mycobacterium tuberculosis • PPD Test (cont’d) Positive Test • Detects patients cellmediated immune response to bacterial antigens

Mycobacterium bovis • Is associated with the ingestion of milk from infected cows. • Penetrates gastrointestinal mucosa or invades the oropharynx. • Similar to M. tuberculosis • Nonpigmented • Slow grower

Nontuberculous Mycobacteria • Is widely distributed in nature. • Infections are acquired by trauma, inhalation, or ingestion. • Runyon classification of cultivatable organisms: Slow growers • Group I—Photochromogens • Group II—Scotochromogens • Group III—Nonphotochromogens • Group IV—Rapid growers (less than 7 days) • Mycobacterium leprae is the only noncultivatable organism. Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 25

Photochromogens • Are slow growing. • Colonies become pigmented when exposed to light. • • • M. kansasii M. asiaticum M. marinum M. intermedium M. novocastrense Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 26

Scotochromogens • Are slow growing. • Colonies are pigmented when grown in the dark or the light. • Are rarely recovered. • • • M. szulgai M. scrofulaceum M. interjectum M. heckeshornense M. tusciae M. kubicae M. gordonae M. cookii M. hiberniae Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 27

Nonphotochromogens • Are slow growing. • Produce no pigment, regardless of whether they are grown in the dark or the light. • Most are pathogenic microorganisms. • • • M. avium complex M. xenopi M. ulcerans M. malmoense M. genavense M. haemophilum M. heidelbergense M. shimoidei M. simiae M. celatum M. conspicuum Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 28

Mycobacterium avium Complex • Most commonly isolated nontuberculous mycobacteria (NTM) species. • Incidence is higher in patients who are immunosuppressed. • Infections include: • Respiratory disease in adults • Lymphadenitis in children • Disseminated infection in patients with HIV • Consists mainly of M. avium and M. intracellulare. Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 29

Rapid Growers • Appear on solid media within 7 days. • Can grow on routine media. • Appear weakly gram positive on Gram stain. • Common species: • Mycobacterium abscessus subsp abscessus • M. fortuitum • M. chelonae • Most common infections are posttraumatic wound infections. Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 30

Mycobacterium leprae • Causes leprosy (Hansen disease). • • • Not cultivatable in vitro. Can be cultivated in armadillo or mice footpads. Two major forms: • Chronic disease of the skin, mucous membranes, and nerve tissue • Bacilli multiplying in peripheral nerves to cause sensory impairment • Tuberculoid • No immune defect • Localized to skin and nerves • Few organisms present in lesions • Lepromatous • Extensive skin lesions • Numerous acid-fast bacilli • May disseminate Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 31

Safety Considerations • Proper Ventilation • Separate from other parts of lab • Nonrecirculating ventilation systems • Negative air pressure • Air flows from clean areas to less clean areas • 6 to 12 room air changes/hour • Biological Safety Cabinet

Specimen Collection and Processing • Variety of clinical specimens, including respiratory, urine, feces, blood, CSF, tissues, and aspirations • Should be collected before antibiotic therapy and processed ASAP • Swabs are discouraged due to decreased recovery

Digestion & Decontamination of Specimens • Decontamination • Specimen from non-sterile site is mixed with an agent that will kill non-mycobacterium bacteria • Common decontamination agents • Na. OH is most common • Benzalkonium chloride (Zephiran) • Oxalic acid (used with Ps. aeruginosa) • After decontamination, the agent must be neutralized so that it will not eventually kill the Mycobacterium

Digestion & Decontamination of Specimens • Digestion • Liquefying mucus enables the mycobacterium to contact and use the nutrients in the agar medium • Common digestion agents • N-acetyl-L-cysteine – most common • Trisodium phosphate (Z-TSP) – used with Zephiran

Concentration • After decontamination and digestion, the specimen is centrifuged in a closed, vented centrifuge for 15 minutes @ 3000 g to concentrate the organisms

Acid Fast Stains • After centrifugation, the button at the bottom of the tube is used to make a smear and to inoculate media • Acid Fast Stains • Ziehl-Neelsen – uses heat to drive the color into the lipids of the cell wall; decolorized with acid-alcohol • Kinyoun – cold stain • Auramine or auramine-rhodamine fluorochrome stain – more sensitive • After staining, a minimum of 300 oif are examined

Culture Media and Isolation Methods • • Mycobacterium are strictly aerobic 5 -10% CO 2 35 -37 o. C Slow growers; cultures held for 6 weeks before calling negative

Culture Media and Isolation Methods • Media- 3 types • Egg-Based with Malachite green (inhibits bacteria) • Lowenstein-Jensen (LJ) • Agar based • Promotes early growth • Middlebrook 7 H 10 and 7 H 11 agar – serum based • Liquid Media • Middlebrook 7 H 9 Broth

Culture Media and Isolation Methods (cont’d) • Labs with large volumes of Mycobacterium cultures use an automated reader (BACTEC) • Used for blood, body fluids, bone marrow • BACTEC broth contains 14 C-labeled substrate • When organisms grow, 14 C in the form of 14 CO 2 is released and detected radiometrically

Direct Detection • Antigen-protein detection • Immunodiagnostic testing • Genetic sequencing and nucleic acid amplification • DNA microarrays • Chromatographic analysis

Biochemical Identification • • • Niacin accumulation Nitrate reduction Catalase Iron uptake Arylsulfatase Pyrainamidase Telluride reduction Urease Hydrolysis of Tween 80
- Slides: 42