MLT 131 Medical Microbiology I Week 3 Ch

MLT 131: Medical Microbiology I Week 3 Ch. 15 Streptococci

General Characteristics • Catalase negative • Facultatively anaerobic • Varying hemolytic patterns (alpha, beta, and gamma) • Nonmotile • Colonies—Most are small to medium, circular and entire, and range from transparent to off white or gray

Gram Reaction • Gram-positive cocci appearing singly or in pairs and chains

Streptococcus and Enterococcus: Habitat and Clinical Infections • Habitat • Normal Flora • Respiratory tract • Gastrointestinal tract • Urogenital tracts • Clinical Infections • Upper and lower respiratory tract infections • Urinary tract infections • Wound infections • Endocarditis
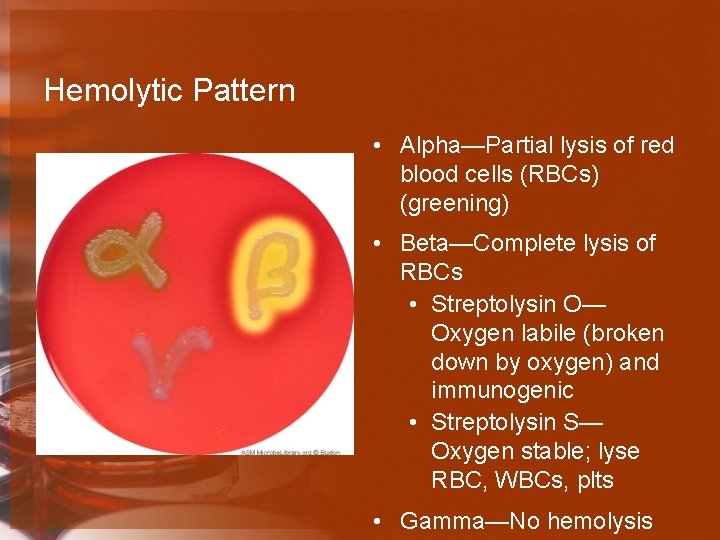
Hemolytic Pattern • Alpha—Partial lysis of red blood cells (RBCs) (greening) • Beta—Complete lysis of RBCs • Streptolysin O— Oxygen labile (broken down by oxygen) and immunogenic • Streptolysin S— Oxygen stable; lyse RBC, WBCs, plts • Gamma—No hemolysis

Serological Grouping • Lancefield grouping • Based on presence of carbohydrates in cell wall • Typing done on beta-hemolytic colonies • Groups A, B, C, and D most significant • Staphylococcus pyogenes (group A) • S. agalactiae (group B) • Commercially available kits allow for the rapid detection of the Lancefield classification in beta-hemolytic streptococci.

Streptococcus pyogenes Group A Strep • Virulence Factors • M protein: Antiphagocytic • Hyaluronic acid capsule: Inhibits phagocytosis • Streptokinase : prolongs clotting • F protein: attachment and adherence • Hyaluronidase: prevents phagocytosis; spreading factor • Streptococcal pyrogenic exotoxins (SPEs): mediate production of rash or multisystem effects (scarlett fever); erythrogenic toxins; heat-liable; activate powerful immune response to induce shock and organ failure

Streptococcus pyogenes Group A Strep • Virulence Factors • Hemolysins • Streptolysin O (O 2 labile: broken down by oxygen) • detected in ASO titers (immunogenic) • Will also cause hemolysis on plates anaerobically • Streptolysin S (O 2 stable) • Causes hemolysis on plates; can also lyse WBCs and plts
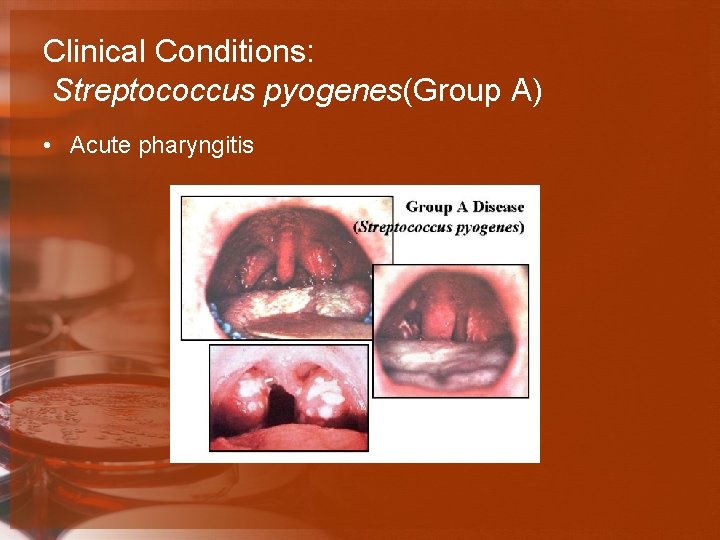
Clinical Conditions: Streptococcus pyogenes(Group A) • Acute pharyngitis
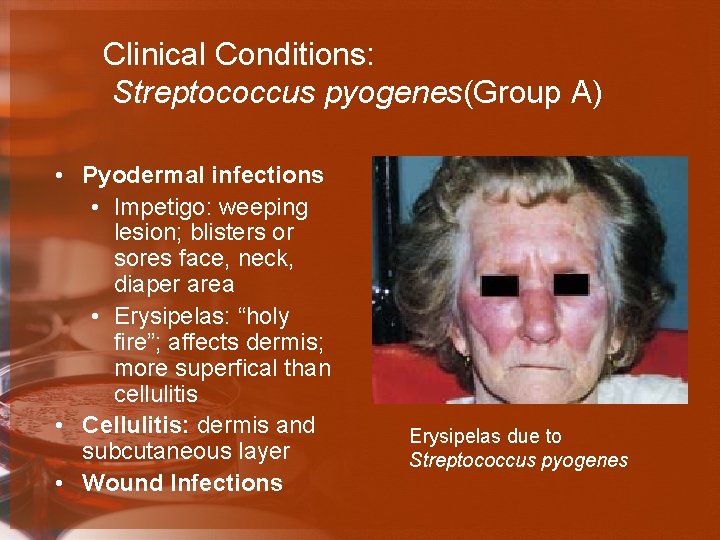
Clinical Conditions: Streptococcus pyogenes(Group A) • Pyodermal infections • Impetigo: weeping lesion; blisters or sores face, neck, diaper area • Erysipelas: “holy fire”; affects dermis; more superfical than cellulitis • Cellulitis: dermis and subcutaneous layer • Wound Infections Erysipelas due to Streptococcus pyogenes

Clinical Conditions: Streptococcus pyogenes(Group A) • Scarlet Fever • Starts with pharyngitis and causes rash on trunk and extremities • Due to untreated Group A infections • Streptococcal pyrogenic exotoxins being released

Invasive Group A Streptococcal Infections • Streptococcal toxic shock syndrome • Multi-organ system failure similar to staphylococcal toxic shock • Initial infection may have been pharyngitis, cellulitis, peritonitis, or other wound infections • Due to a potent amount of streptococcal pyrogenic exotoxin
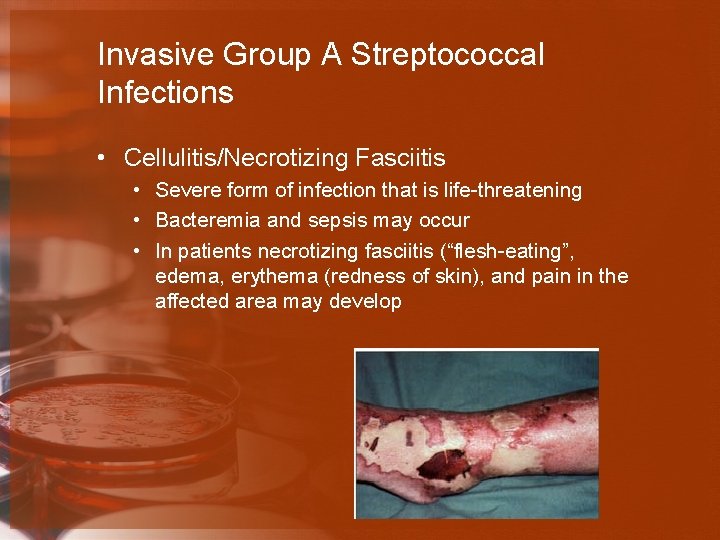
Invasive Group A Streptococcal Infections • Cellulitis/Necrotizing Fasciitis • Severe form of infection that is life-threatening • Bacteremia and sepsis may occur • In patients necrotizing fasciitis (“flesh-eating”, edema, erythema (redness of skin), and pain in the affected area may develop

Post–Group-A Streptococcal Infections • Rheumatic fever • Caused by antibodies made against the M protein • Fever • Inflammation of the heart, joints, blood vessels, and subcutaneous tissues • Chronic, progressive damage to the heart valves (most evidence favors cross-reactivity between Strep. antigens and heart tissue) • ASO titer will be elevated

Post–Group-A Streptococcal Infections • Acute glomerulonephritis (AGN) • Follows either cutaneous or pharyngeal infections • More common in children than adults • Antigen-antibody complexes deposit in the glomerulus • Inflammatory response causes damage to the glomerulus and impairs the kidneys
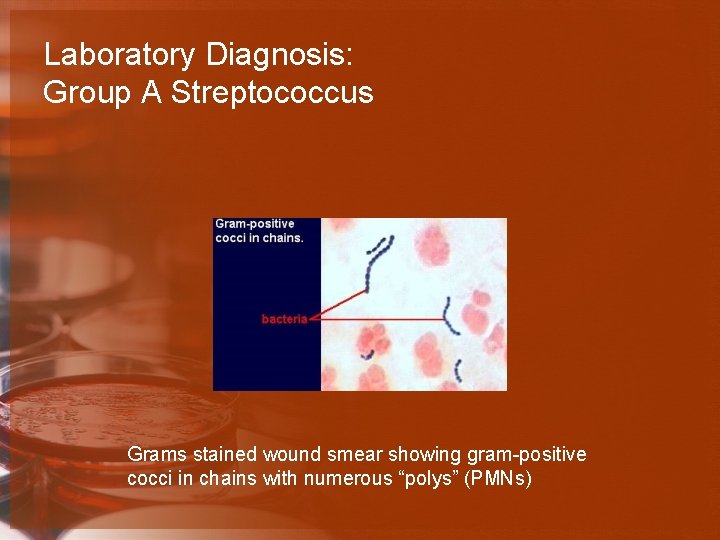
Laboratory Diagnosis: Group A Streptococcus Grams stained wound smear showing gram-positive cocci in chains with numerous “polys” (PMNs)
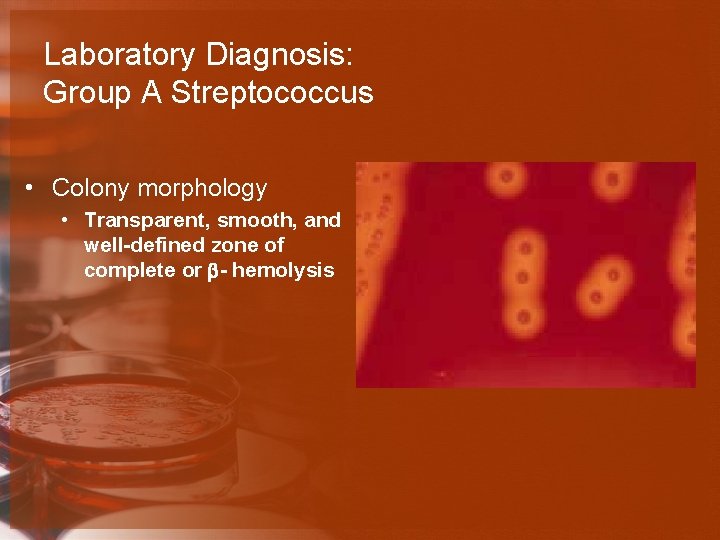
Laboratory Diagnosis: Group A Streptococcus • Colony morphology • Transparent, smooth, and well-defined zone of complete or b- hemolysis

Group B b-Hemolytic Streptococcus (Streptococcus agalactiae) • Group B streptococcal infections are associated with neonates. • Colonize the urogenital tract of pregnant women (10 -30% rate – can cause OB complications such as premature rupture of membranes and premature delivery) • Mother fails to pass protective antibodies to fetus • Cause invasive diseases in newborns • Early onset—Symptoms occur within first 5 days of life. • Late onset—Symptoms occur 1 week to 3 months after birth.

Group B b-Hemolytic Streptococcus (Streptococcus agalactiae) • Newborns • Sepsis • Meningitis • Respiratory distress • pneumonia • Adults (postpartum) • Pelvic abscess • Septic shock
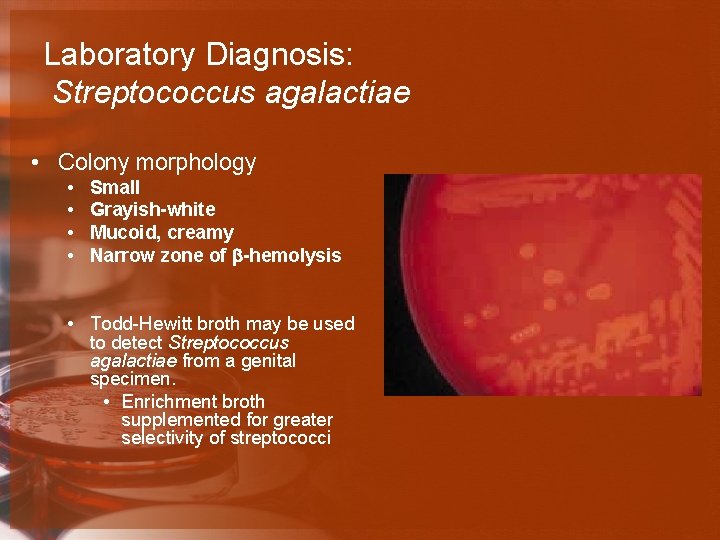
Laboratory Diagnosis: Streptococcus agalactiae • Colony morphology • • Small Grayish-white Mucoid, creamy Narrow zone of b-hemolysis • Todd-Hewitt broth may be used to detect Streptococcus agalactiae from a genital specimen. • Enrichment broth supplemented for greater selectivity of streptococci
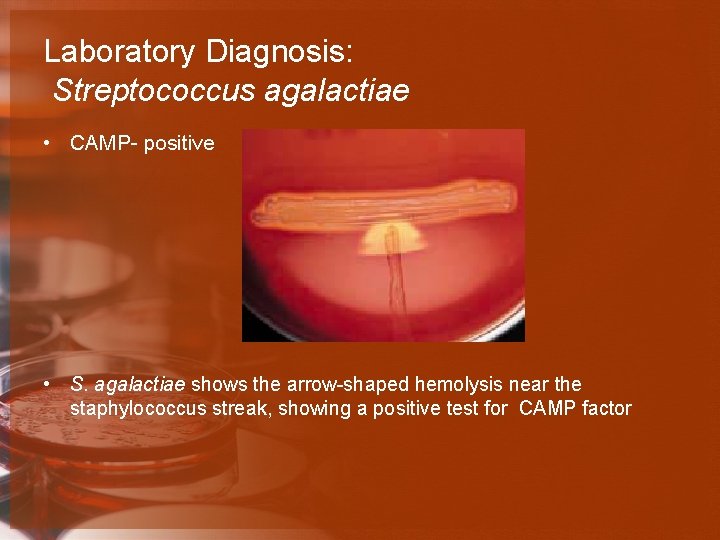
Laboratory Diagnosis: Streptococcus agalactiae • CAMP- positive • S. agalactiae shows the arrow-shaped hemolysis near the staphylococcus streak, showing a positive test for CAMP factor

Streptococcus pneumoniae • General characteristics • Inhabits the nasopharyngeal areas of healthy individuals • Typical opportunist • Leading cause of bacterial pneumonia, meningitis, and otitis media • 2 major virulence factors • Possess C polysaccharide capsule (NOT Lancefield related) • Inhibits phagocytosis • Pneumolysin: suppresses the internal action of phagocytes
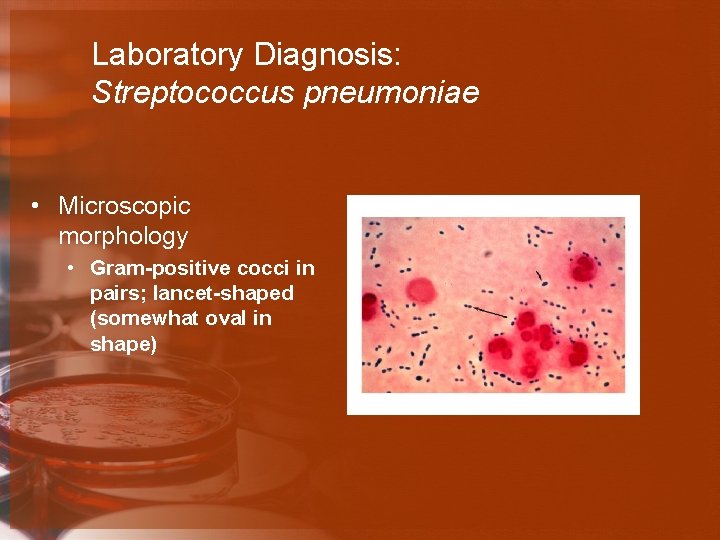
Laboratory Diagnosis: Streptococcus pneumoniae • Microscopic morphology • Gram-positive cocci in pairs; lancet-shaped (somewhat oval in shape)
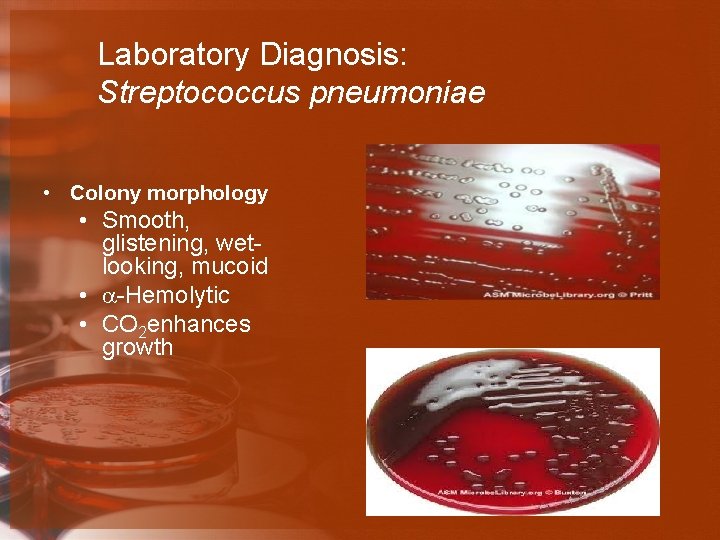
Laboratory Diagnosis: Streptococcus pneumoniae • Colony morphology • Smooth, glistening, wetlooking, mucoid • -Hemolytic • CO 2 enhances growth

Enterococcus Species (previously Group D) • Clinically Significant Isolates • E. faecalis • E. faecium • Opportunistic pathogens • In the GI tract, genitourinary tract and oral cavity • Associated infections • • • Bacteremia Urinary tract infections Wound infections: intra-abdominal infections Endocarditis Hospital-acquired Infections

Laboratory Diagnosis: Enterococcus Species • Colony morphology • Small, grey • Most are non-hemolytic, although some may show - or, rarely, bhemolysis

Other Streptococcal Species • Viridans group (Viridans means “green”) • Members of the normal oral, nasopharyngeal flora, GI tract and female genital tract • Most are hemolytic but also includes nonhemolytic species • The most common cause of subacute bacterial endocarditis (SBE) • Also involved with gingivitis and dental carries

Abiotrophia & Granulicatella • Once referred to as Nutritionally variant streptococci (NVS) • Causes endocarditis and otitis media • Normal flora of oral cavity • Requires pyridoxal (vitamin B 6) to grow • Will not grow on BAP or Choc agar alone
- Slides: 28