MLT 131 Medical Microbiology I Week 2 Taxonomy
MLT 131: Medical Microbiology I Week 2

Taxonomy • Family: Micrococcaceae • Genus: • Staphylococcus • Coagulase positive • Coagulase negative • Micrococcus

Genus Staphylococcus Coagulase positive • S. aureus Coagulase negative • S. epidermidis • S. saprophyticus • S. haemolyticus

Staphylococcus • Gram positive cocci • Arrangement: • clusters

Staphylococcus: General Characteristics • Nonmotile • Non–spore-forming • Nonencapsulated • Catalase-producing • Oxidase: negative • Glucose fermenters • Primarily aerobic, some facultatively anaerobic

Media • 5% sheep blood agar • Routine medium • Mannitol salt • High concentration of salt, sugar mannitol, and phenol red dye • S. aureus ferments mannitol, yellow halo = acid production • PEA (Phenylethyl Alcohol Agar) • Grow gram positive only • Columbia CNA agar • Grow gram positive only • CHROMagar: cefoxitin • Used for the identification of MRSA • Mauve colonies Copyright © 2014, by Mosby, an imprint of Elsevier Inc. 6
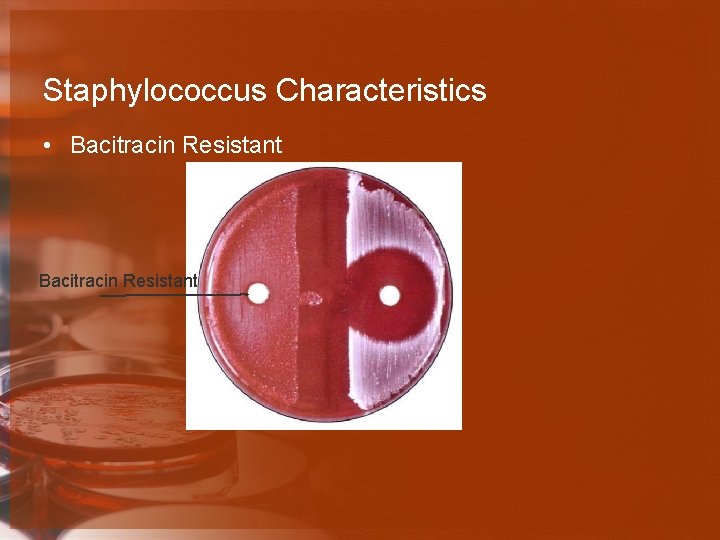
Staphylococcus Characteristics • Bacitracin Resistant

Staphylococcus aureus • Primary pathogen of the genus • Habitat: • Anterior nares (carriers) • Colonization: axilla, vagina, pharynx • Produce superficial to systemic infections • Skin • Bacterial sepsis • Hospital acquired infections

Staphylococcus aureus • Mode of transmission • Traumatic introduction • Direct contact with infected person • Inanimate objects • Predisposing conditions • Chronic infections • Indwelling devices • Skin injuries • Immune response defects

Virulence Factors of S. aureus • capsule: resist phagocytosis • Enterotoxins: damage tissues; Toxic shock syndrome • Cytolytic toxins: • Alpha: Disrupt smooth muscle in blood vessels • Beta: works with alpha; cell lysis • Delta: damages RBCs • Gamma: leukocidin • Deep tissue wounds • Enzymes: coagulase; hyaluronidase • Protein A: ability to bind Ig. G and Complement and preventing them from clearing organism
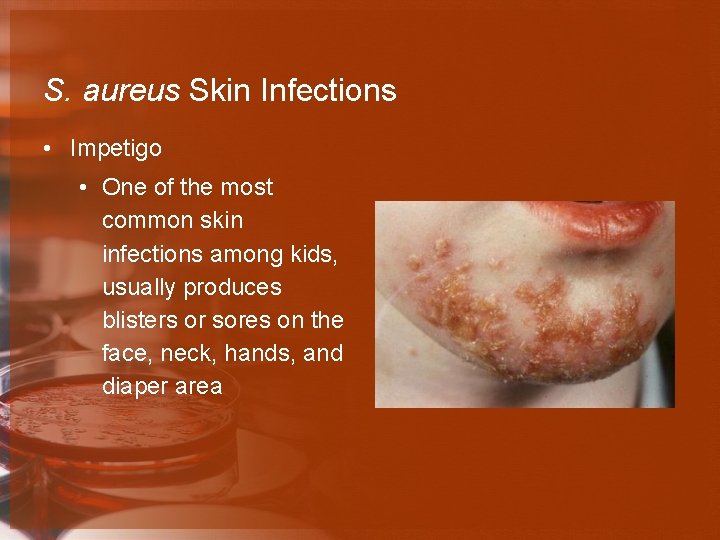
S. aureus Skin Infections • Impetigo • One of the most common skin infections among kids, usually produces blisters or sores on the face, neck, hands, and diaper area
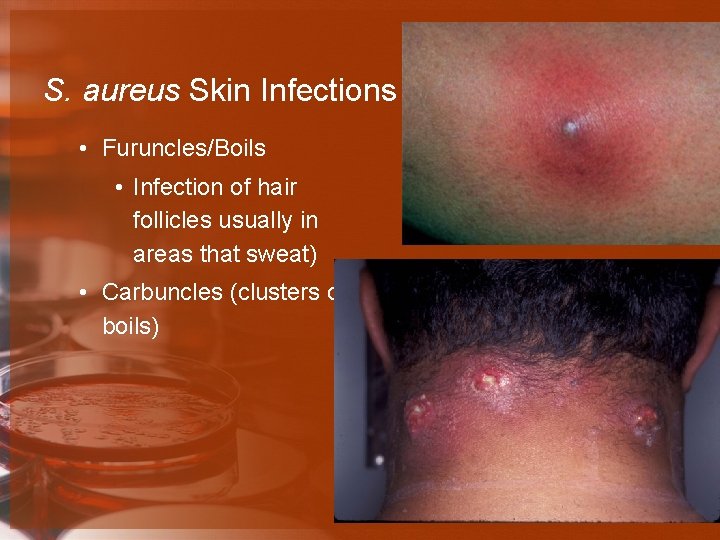
S. aureus Skin Infections • Furuncles/Boils • Infection of hair follicles usually in areas that sweat) • Carbuncles (clusters of boils)
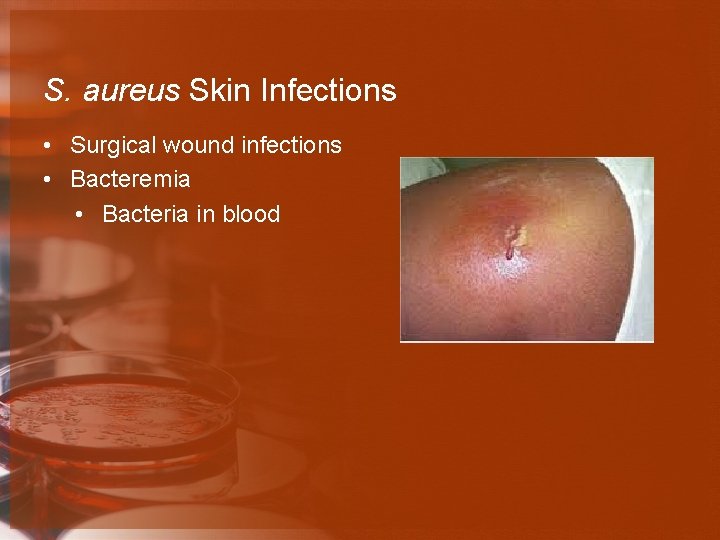
S. aureus Skin Infections • Surgical wound infections • Bacteremia • Bacteria in blood
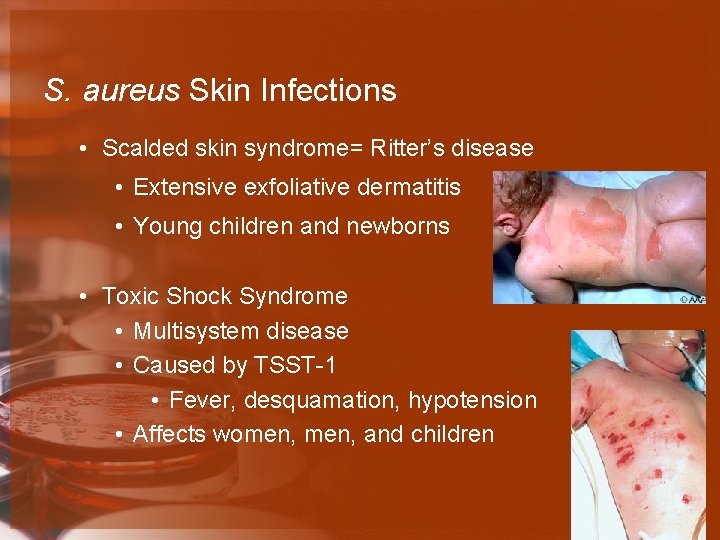
S. aureus Skin Infections • Scalded skin syndrome= Ritter’s disease • Extensive exfoliative dermatitis • Young children and newborns • Toxic Shock Syndrome • Multisystem disease • Caused by TSST-1 • Fever, desquamation, hypotension • Affects women, and children

Staphylococcus aureus: Clinical Infections • Food poisoning • Source is infected food handler • Enterotoxin A the most common cause • Foods affected include meat, dairy products, bakery goods with cream fillings, and salads made with eggs and mayonnaise.

Coagulase negative Staph • • Abbreviated CNS or Co. NS Found as indigenous flora Presence can indicate contamination Seeing an increase due to prosthetic devices, catheters and immunocompromised • Most common S. epidermidis (opportunistic pathogen

Coagulase-Negative Staphylococci: Staphylococcus epidermidis • Predominantly hospital acquired infections • Skin flora gets introduced by catheters, heart valves, CSF shunts • Produces a slime layer that helps adherence to prosthetics and avoidance of phagocytosis • UTIs are a common result

Coagulase-Negative Staphylococci: Staphylococcus saprophyticus • UTIs in young sexually active women • Rarely present in other skin areas or mucous membranes • Clinically significant in any amounts if isolated in urine

Laboratory Diagnosis • Specimen Collection and Handling • Actual site of infection • Prevent delay in transport to the lab • Transport in appropriate device to minimize drying and growth of contaminating organisms
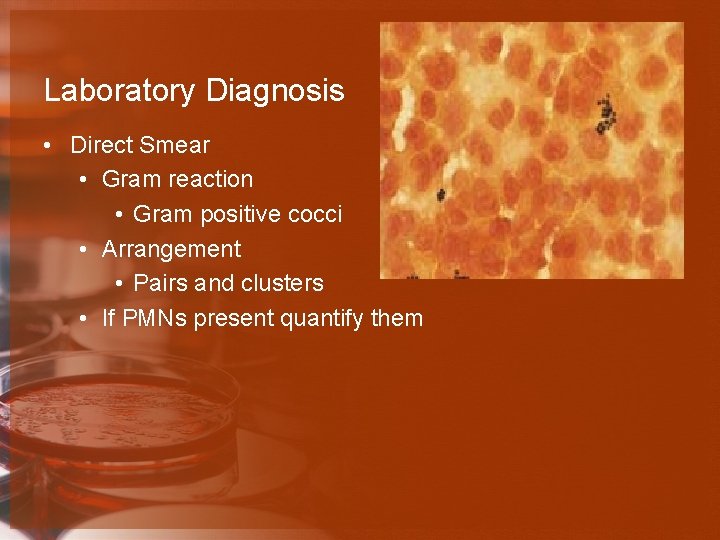
Laboratory Diagnosis • Direct Smear • Gram reaction • Gram positive cocci • Arrangement • Pairs and clusters • If PMNs present quantify them
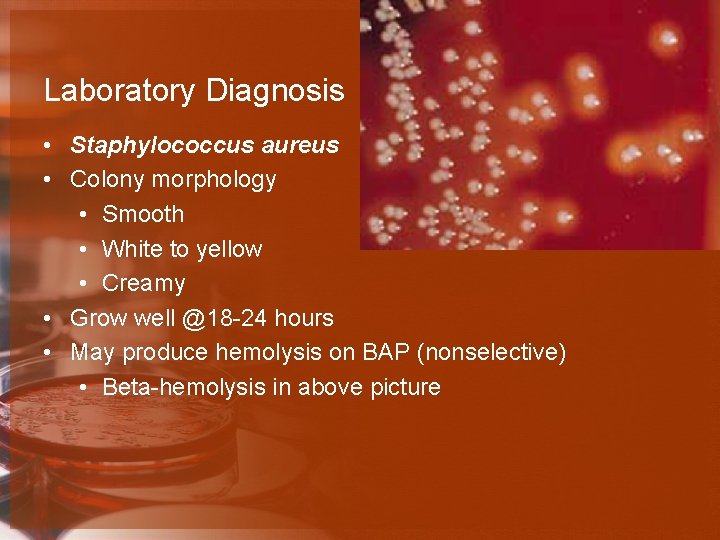
Laboratory Diagnosis • Staphylococcus aureus • Colony morphology • Smooth • White to yellow • Creamy • Grow well @18 -24 hours • May produce hemolysis on BAP (nonselective) • Beta-hemolysis in above picture

Laboratory Diagnosis • S. epidermidis • Smooth, creamy, white • Small-to medium- sized, usually non-hemolytic • S. saprophyticus • Smooth, creamy, may produce a yellow pigment
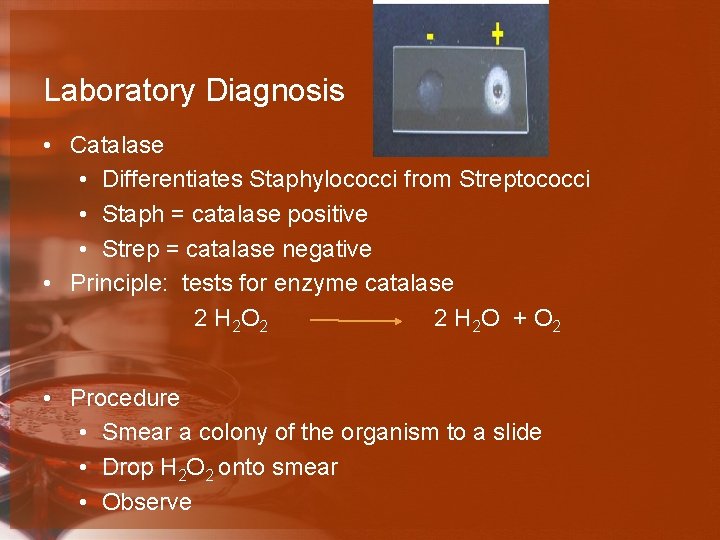
Laboratory Diagnosis • Catalase • Differentiates Staphylococci from Streptococci • Staph = catalase positive • Strep = catalase negative • Principle: tests for enzyme catalase 2 H 2 O 2 2 H 2 O + O 2 • Procedure • Smear a colony of the organism to a slide • Drop H 2 O 2 onto smear • Observe
Laboratory Diagnosis • Coagulase • Differentiate members within Staphylococci • Slide: Detects clumping factor found on the surface of S. aureus • Clumping factor causes agglutination with rabbit plasma by converting fibrinogen to fibrin

Laboratory Diagnosis • Tube Coagulase • Detects “free coagulase” or staphylocoagulase which is not bound to S. aureus • Causes a clot when bacterial cells are incubated with rabbit plasma at 35 -37°C • Clot = positive = S. aureus
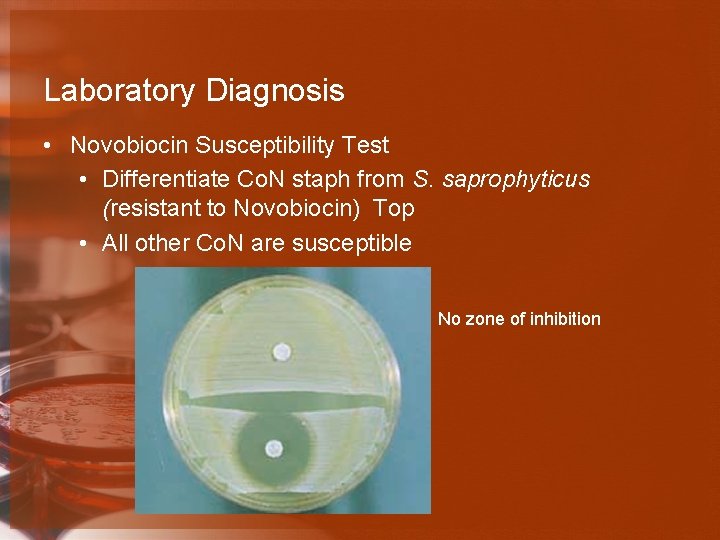
Laboratory Diagnosis • Novobiocin Susceptibility Test • Differentiate Co. N staph from S. saprophyticus (resistant to Novobiocin) Top • All other Co. N are susceptible No zone of inhibition
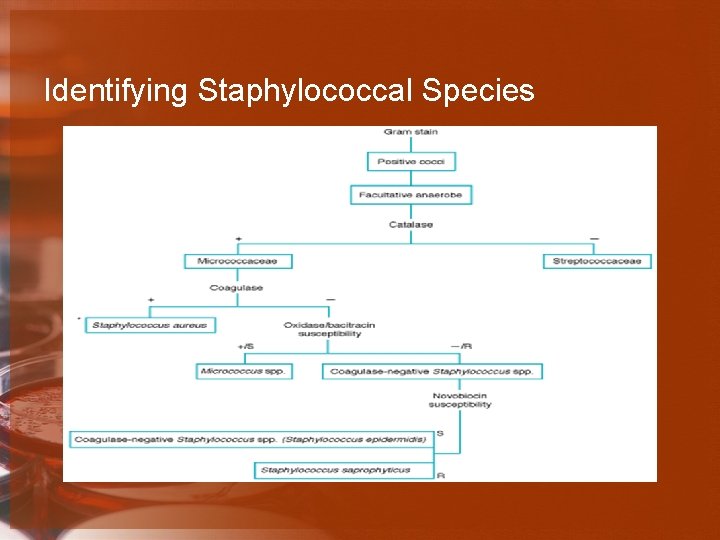
Identifying Staphylococcal Species

Methicillin-Resistant Stephylococci • MRSA • MRSE: Methicillin-resistant S. epidermidis • Infection control • Barrier protection • Contact isolation • Handwashing • Treat with vancomycin • Test for susceptibility with cefoxitin disk

Vancomycin-resistant Staphylococci • VRSA • VISA: Vancomycin intermediate S. aureus

Antimicrobial Susceptibility • Macrolide Resistance • Clindamycin sensitivity often requested by physician to treat Staph skin infection. Referred to as “D” test • Clindamycin resistance is often inducible meaning it only is detectable when bacteria are also exposed to erythromycin
- Slides: 30